Abstract
Non-urgent paediatric Emergency Department presentations contribute to overcrowding, poor patient health outcomes, and burden acute healthcare services. A study was conducted to explore motivations and factors that influence decision-making processes of parents who presented their child to ED for non-urgent conditions. An exploratory study using a qualitative descriptive design was undertaken to address research aims. Semi-structured interviews were conducted with a purposive sample of eight parents who presented their child (birth to 14 years of age), to ED for non-urgent conditions. Parental decision-making regarding ED presentations were influenced by a constellation of factors; however, three main themes emerged. These included Parental Anxiety, There is Only One Place, and Mitigating Perceived Delay or Inaccessibility. As such, centred on how parents addressed their anxiety when a child was ill, accessibility and capacity of EDs to provide immediate relief to parents and children, and parents’ perception that accessing other healthcare services impacted crucial time for treatment. EDs remain a preferred healthcare service to address non-urgent paediatric needs, despite adequate health literacy among participants. When improving models of care within EDs, non-urgent presentations must be considered, including management of parental anxiety, along with establishing non-urgent care adjacent to or integrated within an ED.
Introduction
Non-urgent Emergency Department (ED) presentations have increased globally, which includes non-urgent paediatric presentations (Alele et al., 2019). Any increase in presentations places additional pressure on acute healthcare services, leading to overcrowding of EDs and longer wait times (Coster et al., 2017). Such pressures have a propensity to lead to poorer patient health outcomes, increasing length of hospital stay, and potentially impacting patient morbidity and mortality (Carter et al., 2014; Wennman et al., 2019). Such outcomes lead to an increased burden on health consumers, healthcare system, and higher costs of care (Alele et al., 2019; Butun et al., 2019).
Internationally, research suggests that decision-making among parents for non-urgent paediatric ED presentations is a non-linear, diverse, complex, and an interconnected process. Although nuances exist between countries, these differences are based on the age of a child, having a general practitioner (GP), socioeconomic status, cultural background, and health insurance status, which are all considered as determinants of non-urgent ED presentations (Berry et al., 2008; Long et al., 2021; Salami et al., 2012). Common themes between countries are centred on accessibility, perceived urgency, and perceived efficiency of ED care (Farion et al., 2015; Grigg et al., 2013; Kua et al., 2016; Kurt et al., 2020; Long et al., 2021; Smith et al., 2015). Although current literature provides insights regarding parental decision-making for non-urgent ED presentations internationally, this issue has not been explored in depth across Australia (Cooper et al., 2003; Freed et al., 2016; Sharma and Usherwood, 2014; Williams et al., 2009; Woolfenden et al., 2000).
In Australia, GPs are often a first point of contact within the health system where fee for service is provided through Australia’s Medicare system, which reimburses for part or all consultation fees when care is provided. However, patient access may be limited by operating hours, waiting times, acceptability, and out or pocket or high costs to consumers (AIHW, 2024a). In contrast, EDs are an essential element of Australia’s healthcare system and provide services 24 hours a day and are available at little or no cost to consumers may be consider more accessible (AIHW, 2023). As such, one in three ED presentations in Australia are non-urgent, and children from birth to 14 years of age have the highest presentation rate among all age groups and account for 29% of all non-urgent ED presentations in 2018–2019 (AIHW, 2020).
A non-urgent ED presentation is defined as an ED presentation of a minor condition or illness that needs little or no medical treatment, and manageable in a primary healthcare setting (AIHW, 2024b). Australian Triage Scale in EDs use five categories to determine urgency, where category 1 is most urgent and 5 is least urgent, and where category 4 and 5 should be seen within 60 to 120 minutes (AIHW, 2024b). In this context, a high proportion of non-urgent paediatric ED presentations occur annually within Australia (Peck et al., 2021). In Victoria alone, an average of 67,500 non-urgent unintentional paediatric injury cases, who did not require hospital admission, present to EDs each year (Gafforini et al., 2016; Peck et al., 2021, 2024). As such, a high number of non-urgent paediatric ED presentations may appropriately be provided treatment through primary care services, such their GP, but choose to attend the ED.
Within this context, it is imperative to understand key factors involved in parental decision-making when presenting to EDs for non-urgent healthcare needs. Determining these factors will further enable the formulation of effective interventions or supports to address the challenges of ED overcrowding while enabling parents to receive accessible care when required. This study sought to investigate parents’ lived experiences in presenting their child to ED with a non-urgent condition.
Aim
To explore motivations and factors that influence decision-making processes of parents who presented their child to ED for non-urgent conditions.
Methods
An exploratory study using a qualitative descriptive design, and semi-structured interviews was undertaken, where guiding principles were phenomenological in nature (Gadamer, 2013). This approach enabled key experiences to be explored through voices of those who are embedded within the phenomena being studied. As such, these phenomenology principles enable description and interpretation of fundamental structures of participant lived experiences (Neubauer et al., 2019). Thus, this framework guided narrative collection that comprised of parents’ realities and supported multiple realities interpretation.
Sample
Recruitment was achieved using snowballing technique through both researcher and participant networks. Researcher responsible for recruitment is a registered nurse, where their own network were mostly colleagues; however, participant networks were broader. Several individuals declined or did not meet inclusion criteria.
Participants included parents of children, from birth to 14 years of age, who live in Victoria, Australia, and who presented their children to an ED with a non-urgent (Category 4 or 5) condition within the past five years. If participants had presented multiple times, they were to discuss their most recent ED presentation. Further, ED presentations needed to occur prior to coronavirus disease 2019 (COVID-19) pandemic being declared by World Health Organisation on 11th February 2020 (Srivastava and Saxena, 2020). This was vital, given healthcare seeking was challenged in association with COVID-19. As such, those who had presented their child during the pandemic did not meet inclusion criteria given the presentations to emergency departments may have been due to changes in parent decision-making and fear of COVID-19 at the time, and due to the highly altered healthcare access among within the various communities. Exclusion criteria also encompassed parents with children aged 15 years and older, those who live outside Victoria, and those who have children who presented with urgent (Category 1 to 3) conditions that required admission to the hospital.
Given differences between state health systems and geographical distances, it was determined recruiting participants from one state may limit extraneous factors that may contribute to parent decision-making. Each participant was coded and identified by means of a pseudonym and their child’s suspected condition and age. A rigid application of data saturation as a sample size measure is often questionable and to some extent inappropriate for qualitative description research, where this design emphasises an individual’s unique experience and where data saturation may never truly be reached (Bradshaw et al., 2017; Liamputong, 2019; O’Reilly and Parker, 2012). However, saturation was determined when new themes were no longer highlighted and new responses were not generating additional understanding (Kim et al., 2017; Polit and Beck, 2014).
Data collection
Data were collected between July and August 2021 using semi-structured interviews lasting between 15 and 40 minutes. An interview schedule was developed encompassing demographics questions regarding participant and child, followed by open-ended questions. Face validity of interview schedule was established by undertaking a pilot interview with a mother of a five-year-old who visited an ED for a non-urgent respiratory condition. Once tested, modified data collection commenced. Interviews were conducted using video conferencing technology and later transcribed verbatim.
Data analysis
Data were analysed using thematic analysis, as outlined by Braun and Clarke (2022), and transcripts were read and re-read for familiarisation. Data were identified and linked to the phenomena of interest and provided initial ideas to assist the researchers for coding. Codes were collated and organised to form provisional themes or subthemes. Themes were reviewed, refined, and finalised (Braun and Clarke, 2022).
Ethical considerations
Ethical approval was provided through Federation University Human Research Ethics Committee (#A21-027) and was conducted in adherence with the Declaration of Helsinki.
Findings
Participants’ demographic characteristics.
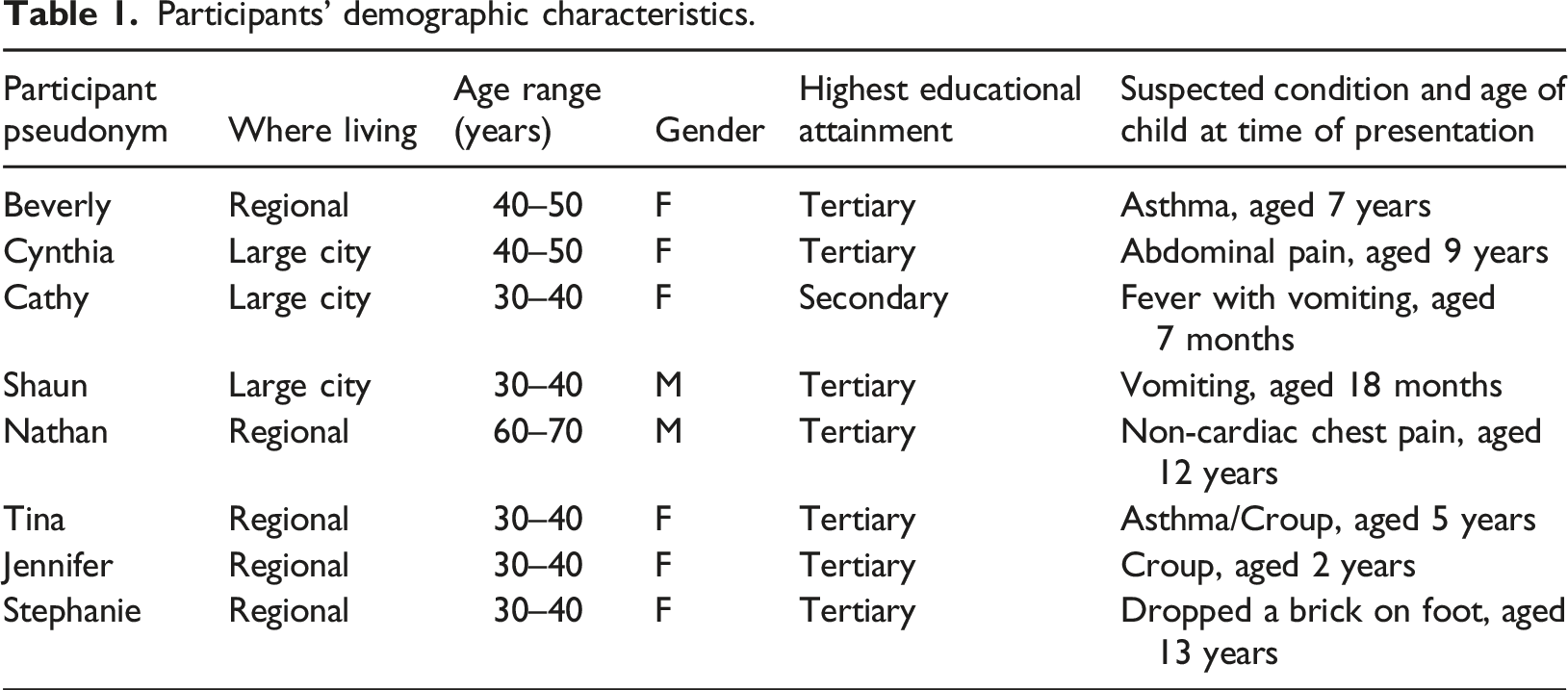
Among the findings, three major themes were identified to influence the decision-making process of parents and included Parental Anxiety, There is Only One Place, and Mitigating Perceived Delay or Inaccessibility, and are explored in detail.
Parental anxiety
Parental anxiety embodied a major factor among parents in their decision-making regarding taking their child to EDs for non-urgent conditions. Elements associated with anxiety and decision-making were centred around clinical signs of their child, past experiences, and ineffective home interventions. Overall, the clinical signs of a child contributed to parent’s anxiety that prompted immediate action. ‘My son… was complaining of abdominal pain. I monitored him throughout the day, and it seems to be getting worse…and it was a little bit low to the right. So, I was wondering myself if it could possibly be appendicitis?’ (Cynthia, Abdominal pain, aged 9 years)
Parents added not knowing exactly what their child was experiencing and their ability to gauge the severity of the symptoms was challenging. ‘It’s very difficult to work out how much pain the person is actually experiencing, so when you got a child saying, it hurts, it is impossible to gauge how much it really does hurt’. (Nathan, non-cardiac chest pain, aged 12 years)
More challenging, was when a child could not or did not have the capacity to verbalise symptoms. Specifically, one mother explained when her infant was vomiting with a high temperature: ‘When there is a baby involved…there’s a lot of uncertainty…there’s a lot of stress…you just don’t know what’s wrong with them and they can’t verbalise’. (Cathy, fever with vomiting, aged 7 months). Further, parental anxiety was also exacerbated by past experiences with children. ‘Both my children get croup during winter. I’m well-acquainted with croup because they’ve had croup all their lives… I know… if they don’t see a doctor within 24 hours, then the croup will be nasty… I have had to call an ambulance before’. (Tina, asthma/croup, aged 5 years).
In addition to their own children, it was experiences of friends or extended family that inform their own anxiety and decision-making. For example, a parent whose child was experiencing a high temperature stated: ‘We’ve had toddlers [relatives] that had high fevers that have passed away. So… in the back of my mind, I was just really scared… because I know how dangerous [fever] can be’. (Cathy, fever with vomiting, aged 7 months).
It was noted most parents initially provided home interventions to alleviate the symptoms based on successful past experiences. When interventions did not work or became ineffective, parental anxiety drove them to seek care. ‘I’d gone through all the normal steps you would do as a parent and as much as I could do at home… nothing seemed to be helping… so I decided to present to ED… ’cause from my perspective, he wasn’t getting any better’. (Jennifer, croup, aged 2 years).
Parents were driven to decide to go to EDs when they thought they had exhausted all possible avenues to improvement to their child’s condition at home with little effect.
There is only one place
Once parental anxiety had exacerbated to a point of deep concern, parental decision-making was that EDs were the only place to go. ‘I know that [the ED] is open. I don’t have to [call] them. I didn’t think of any other option, quite frankly. I was more interested [that]… the child should be seen and where could she be seen? Well, there’s only one place, [the ED], end of story’. (Nathan, Non-cardiac chest pain, aged 12 years). ‘I [didn’t] know what to do then… [we had] no other options…nothing in our hands…we had to take her to the hospital’. (Shaun, vomiting, aged 18 months)
Getting a child’s immediate needs addressed was also associated with ED accessibility and its capacity to provide immediate answers, interventions, and relief for the child, but also to alleviate parental anxiety. Parents gravitated towards EDs as it provided a sense of immediate ‘comfort’. ED accessibility, especially in terms of time, was found to be a main reason for this decision-making and behaviour. ‘I want the answer, I want something done now…I want an answer now of whatever the problem is…I didn’t want to go through like a four-week process of waiting for an x-ray result to come back or trying to get into my GP. I want to know then and there if she’s actually got a break instead of making her walk on it…all weekend’. (Stephanie, dropped a brick on foot, aged 13 years).
Some parents’ perceptions of EDs having highly trained staff with a complete suite of facilities and equipment had also contributed to ED accessibility, which may have provided comfort. Parents perceived diagnostic tests were required as part of assessing their child’s condition and felt EDs are the only place that can provide such procedures and services. ‘I wanted [my son] to be seen by someone who is very very medically trained, who has seen these sorts of things all the time… [and] ’cause they’ve got the facilities’. (Cynthia, abdominal pain, aged 9 years).
Conversely, another parent indicated attending EDs was not based on medical profession skill given there are often junior medical staff who attend to their care. ‘When you get to the hospital, the doctor that is seeing you is really no better or worse than a GP… because you got young interns and people like this on board’. (Nathan, non-cardiac chest pain, aged 12 years).
However, others indicated they prefer their GP as they are knowing their child’s history. This suggests that decision-making is not always based on expertise, but due to other factors such as facility accessibility, availability of resources for diagnostic procedures, and timeliness of service where diagnostic results are immediately known.
A parent highlighted that going directly to EDs also means being seen within hours rather than days, which may have been the case if trying to get to see their local family doctor. Comfort was received when immediate answers and solutions were provided. ‘We got looked at straight away and they gave us a lot of good information…our experience was so smooth, so quick… everyone was really lovely. We [the participant and her husband] left there feeling a lot better. I wasn’t stressed anymore. I wasn’t worried that he [son] wasn’t going to get better’. (Cathy, fever with vomiting, aged 7 months). ‘He’s seen straight away by a senior doctor and within 20 [or] 30 minutes they’ve assessed him…they’ve given him the medication that he needs. They’ve treated [his] asthma, and we go home with everything I need’. (Tina, asthma/croup, aged 5 years)
Medical interventions were administered, and their child’s clinical signs had improved. Thus, EDs has addressed the parents’ needs and, consequently, resolved their anxiety.
Mitigating Perceived Delay or Inaccessibility
Beyond EDs being a preferred place to received care, this theme embodies how EDs provided a source of comfort that could not be replaced by attendance at any other service. Participants discussed accessing other healthcare services and how doing so was found to impact critical time where decisions were about mitigating a perceived delay. This was due to the perceived inaccessibility of care or what they had deemed as GP services being unsuitable, unavailable, or inappropriate for their child’s condition. ‘I couldn’t have used the GP [for son’s condition]. It wouldn’t have been quick enough, and I do feel like [the other services] might just have sent me [to the ED] anyway’. (Beverly, asthma, aged 7 years).
Parents view utilising GP services leads to waiting ‘double’ the amount of for care, and they were certain they will only be referred to EDs in the end.
‘You do end up waiting a really really long time, probably similar amount of time as you would wait in the ED and I was worried that we’d wait for hours to see someone and they would have a little examination and say, “it could be appendicitis, go to the hospital” and once again we’d have to sit in ED and wait’. (Cynthia, abdominal pain, aged 9 years).
Often, this thinking was based on their lack of confidence in primary healthcare services or previous experiences. ‘In the end, they said, ‘look, if you’re that worried about your child, take him to the emergency department’. (Tina, asthma/croup, aged 5 years). In addition to parents being directed to EDs, some parents, although aware their GP is able to manage their child’s condition, still chose to go to the ED. In some cases, parents were even willing to pay additional money to access a private ED due to issues of overcrowding in public EDs. ‘The doctors in the ED [of a private hospital] are very kind but it costs money…almost $200 when you could’ve been to a GP for them to do exactly the same thing’. (Tina, asthma/croup, aged 5 years).
In other cases, inaccessibility was centred on a mismatch between what time services were available relative to health needs. It was noted GP clinics are closed outside of normal working hours, and if parents can contact clinics during working hours, they are unable to access same-day appointments. ‘The GP [clinic] is closed. They don’t operate at night-time. There are no home visits. There’s no one…, [sarcastically adding], I’m not going to ring up at 9 o’clock in the morning and they’ll say come straight in… I really had no other option... There’s nowhere else’. (Nathan, non-cardiac chest pain, aged 12 years). ‘[GP is] just hard to get into…you have to book a week in advance before you can see [him]. The reception will just say, well sorry, but we really can’t fit anybody in…you’ll have to find someone else or just go to the emergency department’. (Tina, asthma/croup, aged 5 years)
GP inaccessibility drove parents to bring their child to EDs, which was considered a more accessible healthcare service. Parents believed that EDs were the only place to go to. Despite the preference for GPs over EDs, and different views on regarding doctor competence, these same parents were satisfied in their decision of bringing their child to EDs. It was indicated that parents will, in fact, continue these same approaches in future. What was identified is a need for parents to immediately determine their child’s exact condition, ending their child’s poor health and suffering as soon as possible, while consequently relieving themselves of their anxiety.
Discussion
In-depth interviews with parents regarding their experiences presenting their child to ED for non-urgent conditions have aided in achieving study aims. For example, key motivating factors that influenced parental decision-making in presenting their child to ED for non-urgent conditions were centred on parental anxiety and ED accessibility. These findings are in consonance, while at times, divergent with the current literature (Berry et al., 2008; Farion et al., 2015; Grigg et al., 2013; Kua et al., 2016; Kurt et al., 2020; Long et al., 2021; Salami et al., 2012; Smith et al., 2015). Parental anxiety and their need to be reassured and comforted was a major contributor to perceived urgency. Anxiety felt by the parents in this study was principally caused by clinical signs and symptoms exhibited by their children, their own past experiences, and ineffective home interventions (Nicholson et al., 2020).
Clinical signs and symptoms exhibited by children were shown to influence parental anxiety and resonate with studies conducted elsewhere, wherein parents have brought their children to EDs with key symptoms that were of concern, suspecting a serious disease or condition (Burokienė et al., 2017; Kua et al., 2016). Other studies have suggested this natural reaction among parents is a demonstration of empathy for their child (Cook et al., 2015; Costet Wong et al., 2015). Empathy may also be couched within an anxiety-provoking inability to interpret information being exhibited by a child.
Another factor associated with parental anxiety was prior experiences that had influencing current perceptions. Participants identified a seasonal nature of an illness or prior death of a family member impacted their anxiety, which can have an influence upon their own capacity to assess their child’s condition objectively (Grigg et al., 2013). In some cases, parents’ previous experience of delaying care and leading to severe impairment or death was key in decision-making (Grigg et al., 2013).
Parents who sought to alleviate any signs and symptoms through ‘tried and tested’ home interventions demonstrated increased levels of anxiety when these were found to be less effective, leading to a perceived need for urgent medical attention. This finding was also demonstrated by Grigg et al. (2013) and Kua et al. (2016), wherein parents decided to bring their child to EDs when home remedies or over-the-counter medications had not resolved signs and symptoms. At this juncture, parents believed or were convinced their child was in a grave condition and needed to be urgently seen by a doctor. Parents within this study were not forthcoming or clear regarding how much time had passed between providing home interventions and deciding to bring their child to an ED. However, it was their child’s persistence clinical signs, rather than length of time that led decision-making to occur as has been demonstrated elsewhere (Conlon et al., 2021).
Studies have suggested decision-making regarding non-urgent ED presentation of a child is often due to low health literacy and inability to understand and interpret health needs of a child (Huang et al., 2021; Kua et al., 2016). Low health literacy among parents, especially regarding how to recognise and manage non-urgent conditions at home, also increases perception of urgency, thus increasing ED presentations (Fieldston et al., 2012; Huang et al., 2021; Kubiceck et al., 2012; Salami et al., 2012). An important finding from this study is most participants had a healthcare background. Despite their adequate knowledge of health, at a time of perceived crisis, decided to present their children to ED. Anxiety may have contributed to this decision-making process, where parents with a healthcare background, particularly nurses, have an increased level of anxiety due to stress brought about by their conflicting roles during a health crisis – being a parent and being a nurse (Lines et al., 2015).
Typically, knowledge of health among these parents enables an awareness of possible complications and potential diagnoses of their child’s condition, which further exacerbates their anxiety. This combination drives these parents’ desire to receive additional inputs from other healthcare providers (Lines et al., 2015). Providing educational instructions regarding how to manage non-urgent conditions of children in primary care settings increased parental health literacy, however, did not decrease ED utilisation (Fieldston et al., 2012). This suggests focussing on health literacy may not completely address the challenges associated with increasing non-urgent paediatric ED presentations, and it may instead exacerbate the issue.
Parents make decisions under extreme pressure, usually compounded with other stressors in life, which may impact their capacity to think rationally (Cook et al., 2015), and in these cases it is more likely to be intuitive rather than logical (Butun and Hemingway, 2018). However, as some parents indicated, they felt they were making rational decisions. Given they were highly risk averse, they preferred to act cautiously and seek ED treatment. Being confronted with something unfamiliar or something unknown makes a person feel unsafe and thus motivates to seek security (Maslow, 1943). Thus, parents witnessing their child suffer from worsening signs and symptoms of an unknown origin may have motivated them to seek help from the ED to satisfy their and their child’s need of security and safety, as demonstrated to be a fundamental need within Maslow’s hierarchy of needs (Maslow, 1943).
A further motivating factor for bringing a child to an ED with a non-urgent condition centred on EDs being considered a central place of care encompassing elements of healthcare accessibility. Parents stated that they brought their children to EDs as it is open 24 hours, unlike most GP clinics which are often closed outside normal working hours (McDonnell et al., 2022; Nicolson et al., 2020). In addition, appointments are not required to attend EDs and amongst participants, there was a perception there were shorter waiting times compared to GP clinics. These findings correspond with previous studies which have indicated that parents’ motivation to bring their children to EDs was due to the lack of timely access in GP clinics along with the unpredictability of child health issues that do not quite ‘fit’ the current GP model of care (Kurt et al., 2020; Long et al., 2021; McDonnell et al., 2022; Nicolson et al., 2020).
Among parents’ reasons for non-urgent ED presentations was the perceived efficiency of the ED. Parents perceived that EDs contain highly trained staff along with a full suite of healthcare facilities, equipment, and medications necessary to diagnose and treat their child’s specific condition, providing immediate answers and comfort. This finding echoed those of other studies which demonstrated that parents have felt that EDs are able to provide a higher quality of care than in primary care services (Burokienė et al., 2017; Farion et al., 2015). Despite this, some parents stated they prefer to see their GPs because they know their history. However, despite this familiarity and trust of their GP, they decided to attend the ED given its immediacy of access and is in harmony with other studies (Conlon et al., 2021).
According to Costet Wong et al. (2015), EDs immediately soothes parents’ anxiety and distress by their capacity to be accessible through timely and efficient care. This finding was similar to those of other studies wherein they have indicated parents find EDs a place of reassurance by providing them with much-needed ‘peace of mind’ (Conlon et al., 2021; Cook et al., 2015). EDs have been regarded by parents as a sanctuary where they can find refuge during times of health crises (Conlon et al., 2021; Cook et al., 2015). This finding suggests that a non-urgent clinical area may be a solution and could be incorporated in EDs to accommodate these cases. This is another opportunity for further research to specifically determine why the ED provides parents comfort immediately upon arrival. Whether it is a physical sense of being in a hospital, ED personnel presence, or a perception of being attended to and addressing child health issue immediately, such approaches provide parents with much-needed reassurance during a perceived health crisis.
Limitations of the study
Despite the findings, this study has several limitations. This study has a small sample size of eight participants due to recruitment difficulties and exclusion criteria which limited those who had presented their children during the time of the COVID-19 pandemic. Further participants had similar characteristics were recruited and therefore findings may not be transferrable to a wider population (Liamputtong, 2019). Given this outcome, snowball sampling of known contacts, including participant contacts, were utilised to obtain adequate participants, and referral quality is often dependent trust and cooperation referees has with the researcher, which is another potential source of bias. An additional limitation was recall bias, where participants relied on recall, which may have unintended inaccuracies as a significant period may have elapsed between crisis events prior to the COVID-19 pandemic and when interviews were conducted. In this case, this exploratory study identified new information, enabled the formulation of hypotheses, assessed feasibility, and prioritised future research. Thereby enhancing the effectiveness of our current prospective study designed to enable clearer understanding of parental decision-making that may enable the capacity for healthcare services to meet or triage the care needs of community members differently. Lastly, due to the qualitative nature of the study, demographic stratification was not possible, and the role of demographic variables as predisposing factors of non-urgent ED visits was not considered. However, future studies that are larger could explore their influence on decision-making.
Implications for practice
To reassure parents and address their anxieties by having children immediately, diagnosed and treated requires new approaches to healthcare that effectively decreases or mitigates non-urgent paediatric ED presentations. Parental level of health literacy is a predisposing factor of non-urgent paediatric ED presentation (Fieldston et al., 2012; Huang et al., 2021; Kua et al., 2016). Thus, various interventions may be implemented to improve health literacy despite being less effective in improving non-urgent paediatric ED presentations (Fieldston et al., 2012). In this study, participants were mostly practicing nurses who still took their child to the ED for non-urgent conditions despite their adequate knowledge and skills regarding healthcare, suggesting there are a constellation of other key factors that drive parents to seek help.
Challenges and implications for practice may not solely centred on how to address parental health literacy and behaviours that drive to the care and protection of offspring alone. It may also encompass the overarching infrastructure, funding, and design of healthcare which contributes to parental caring behaviour. Given this research along with previous studies, an extension of EDs specifically for non-urgent paediatric conditions may be necessary. An integrated primary healthcare service where patients may be triaged and seen on the same day within an ED may be required to divert non-urgent paediatric ED users. Nurse practitioners and other advanced clinicians may be appropriate to provide care and support among patients, educate, and guide them regarding the child’s condition and emphasise the importance of continuity of care.
Conclusion
As non-urgent paediatric ED presentations are identified as having a profound contribution to ED overcrowding, it is imperative to understand factors involved in decision-making of parents when presenting their child to EDs for non-urgent conditions. This study sought to understand why parents preferred ED services over other healthcare services. It has been established factors that influence parent decision-making is multifaceted and complex. However, it has been emphasised through this study that main driving force of this phenomenon is parental anxiety, and EDs are parents’ preferred option as they are a service that provides comfort and reassurance. Thus, moving forward, healthcare services and policy makers must design models of care within EDs which not only put focus on improved management of non-urgent conditions, but also on management of parental anxiety associated with paediatric needs. This includes establishing non-urgent primary healthcare, which may be adjacent to or integrated with an ED and staffed by nurse practitioners.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
