Abstract
Physical restraint is regularly used in children and adolescent mental health care, often as a reactive behaviour management strategy. Physical restraint has been associated with physical injury, but psychological consequences are poorly understood. The aim of this systematic review was to examine physical restraint of children and adolescents in inpatient mental healthcare services. Healthcare databases were searched to identify English language publications discussing anyone aged ≤18 years who had experienced physical restraint as a mental health inpatient. No date restrictions were applied. Sixteen quantitative studies are included within this review. Most studies are retrospective in nature. Publications were appraised using the Critical Appraisal Skills Programme quality assessment tool. Common characteristics associated with children and adolescents who experience physical restraint include age, gender, diagnosis, and history. Most studies associate physical restraint with the management of aggression. Findings suggest that it may be a combination of patient (intrinsic) and environmental (extrinsic) factors which ultimately lead to children and adolescents experiencing restraint. This review confirms that little is known about children and adolescents’ first-hand experiences of physical restraint. Future research should address children and adolescents’ perceptions and first-hand experiences of physical restraint.
Keywords
Introduction
Restrictive interventions, which include restraint, have a long history within mental healthcare services. Physical restraint in mental health care means ‘…the use of physical contact which is intended to prevent, restrict, or subdue the natural movement of any part of the patient’s body’ (Mental Health Units (Use of Force) Act, 2018). Despite the potential risk of physical injury as a result of being physically restrained (Department of Health, 2014), its implementation in mental healthcare practice is sometimes deemed necessary to maintain safety (Wilson et al., 2015) and protect children and adolescents and/or people around them from harm (National Institute for Health and Care Excellence, 2017). However, there are ethical, moral, and legal considerations associated with its implementation in all fields of health care (Hollins, 2017), including disproportionate use (Georgieva et al., 2012), unnecessary exposure to injury (Hollins and Stubbs, 2011), and death (Barnett et al., 2012; Scheuermann et al., 2016; United Nations Convention on the Rights of the Child, 1989). The focus on physical risks can result in psychological harm being overlooked (Bray et al., 2014; Ridley and Leitch, 2019).
In the United Kingdom, ‘…physical interventions should only ever be used as a last resort…’ (Department of Health, 2014: 9) and broad guidelines, targeted at health, social care, and educational providers, as well as local authorities and clinical commissioning groups, aim to eliminate the inappropriate use of physical restraint with children and adolescents who are ‘…still developing both physically and emotionally and for whom trauma…could be very damaging…’ (Department of Health, 2017: 5). However, historically, not all healthcare guidelines have provided evidence-based frameworks of how to implement standards (Wilson et al., 2015).
Understanding the consequences of physical restraint on a child’s mental and physical well-being is important (Ridley and Leitch, 2019). Further, research indicates that adults (patients and staff) can also experience distress (Tolli et al., 2017), anger, fear (Merineau-Cote and Morin, 2013), anxiety (Laugharne et al., 2012), and traumatic psychological damage (Mohr et al., 2003) resulting from restraint implementation. There are also reports that the use of restraint within mental health services can damage therapeutic rapport (Steinert et al., 2010) and contribute to increased staff turnover (Department of Health, 2017). An important resource for service providers and policy-makers, both in the United Kingdom and internationally, would be access to a contemporary systematic literature review on the use of physical restraint with children and adolescents within mental health settings. Currently, this does not exist, and this review aims to address this deficit.
Aim of the review
The aim of this review was to systematically locate, appraise, analyse, and synthesise literature pertaining to the physical restraint of children and adolescents in inpatient mental healthcare services. The objectives are to explore which children and adolescents are being physically restrained in inpatient mental health services, critically examine the reasons why children and adolescents are being physically restrained in inpatient mental health services, and critically examine the consequences for children and adolescents of reported physical restraint use in inpatient mental health services.
Method
Selection of a narrative approach
Due to the heterogeneity of the combination of sample populations and settings (Popay et al., 2006) as well as the poorly understood nature of physical restraint of children and adolescents in mental health care, a narrative synthesis approach was chosen (Campbell et al., 2018), informed by Popay et al. (2006), to ‘tell the story’ of findings from the included quantitative studies (page 5).
Search criteria
Key search terms.

Note: CAMH: child and adolescent mental health.
Inclusion and exclusion criteria
The eligibility criteria included empirical studies, availability in English, and reporting on physical restraint use with children and adolescents admitted to mental health services. Studies were excluded if physical restraint was not independently reported from seclusion (a restrictive intervention which falls beyond the remit of the current study). Due to the paucity of the literature, no date restrictions were applied.
Screening
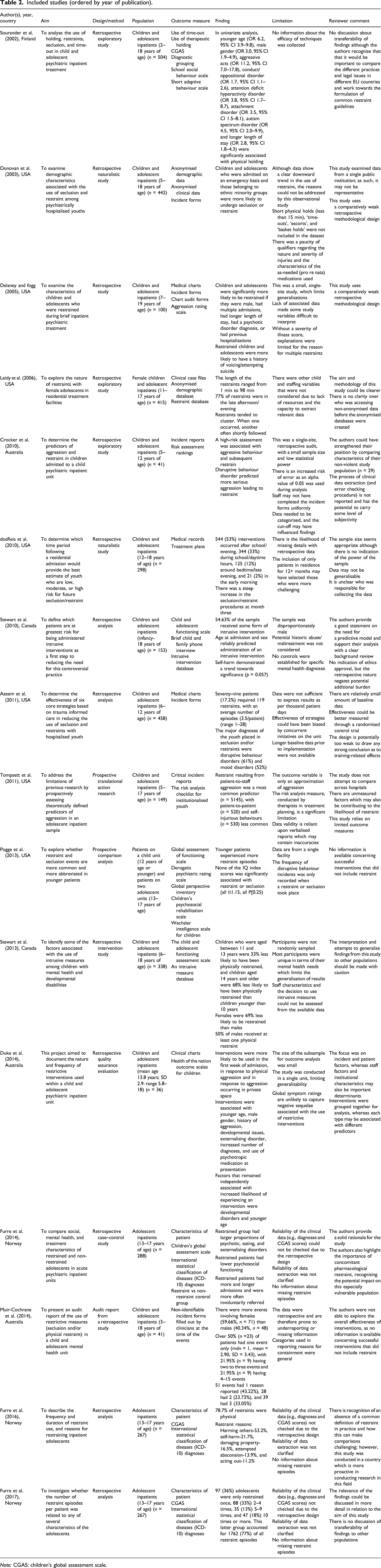
The initial searches retrieved 1727 publications. Of those, 455 duplicates were removed. Titles, keywords, and abstracts of all remaining publications (n = 1272) were screened for relevance, and 1231 publications were excluded (Figure 1). Reference lists and lead authors of the remaining publications (n = 41) were examined to identify relevant additional studies. Full-text screening resulted in a further 24 publications being excluded. Data were then extracted from the remaining publications (n = 17); in Table 2, these studies are presented in order of publication. Preferred reporting items for systematic reviews and meta-analyses flowchart. Included studies (ordered by year of publication). Note: CGAS: children's global assessment scale.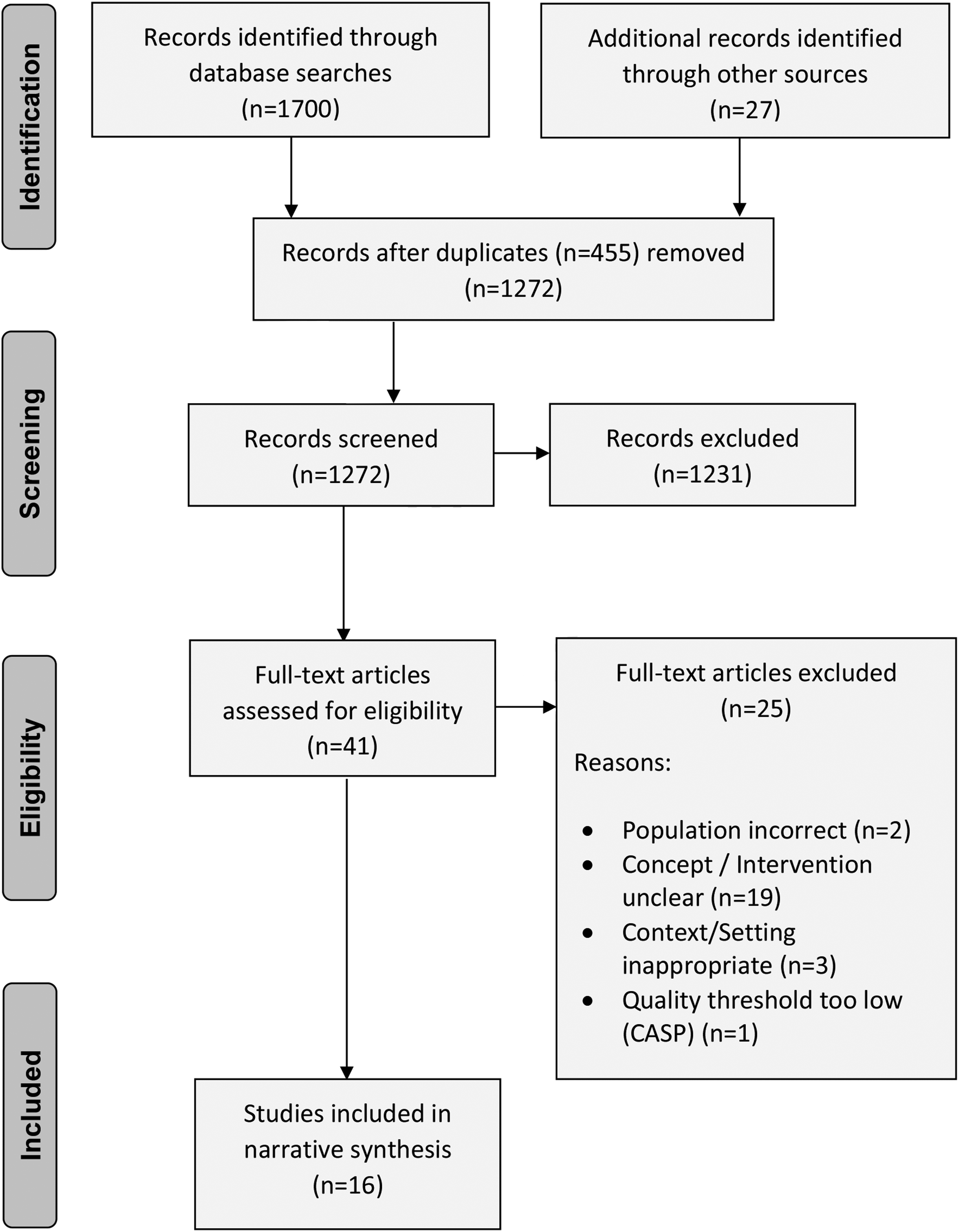
Quality appraisal
Critical appraisal skills programme quality of evidence.
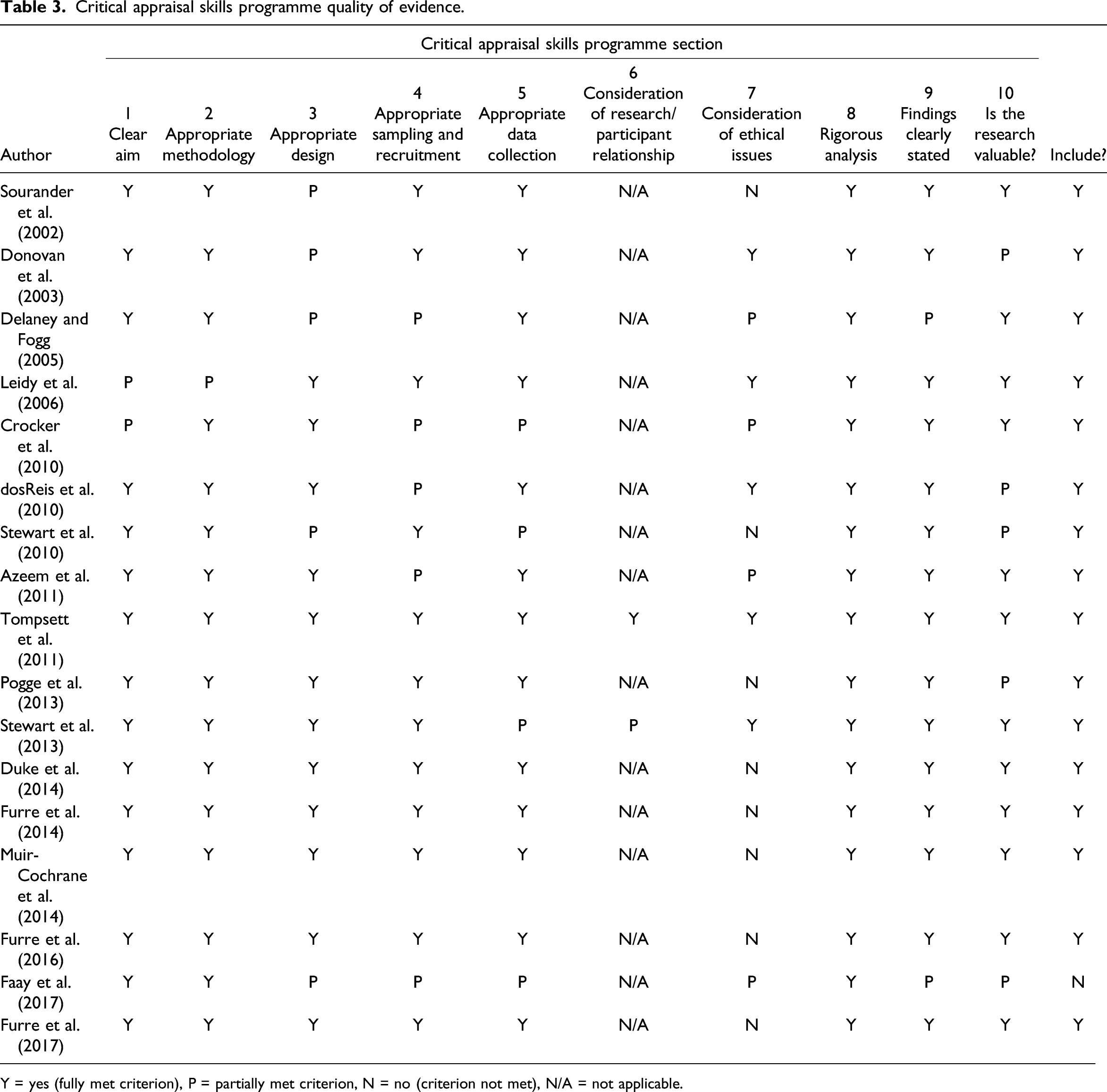
Y = yes (fully met criterion), P = partially met criterion, N = no (criterion not met), N/A = not applicable.
Data synthesis
Narrative synthesis, informed by Popay et al. (2006), facilitated the identification of patterns across the data. Studies were tabulated to allow for preliminary comparison. Relationships within and between the reviewed studies were explored to identify similarities, differences, and potential effects of background variables. Subgroups were derived that best illustrate the emergent themes from within the study findings. Accordingly, these are presented and discussed in respect of the objectives of this review.
Results
Study characteristics
Sixteen studies are included in this review representing research conducted across America (n = 6), Australia (n = 3), Norway (n = 3), Canada (n = 2), Belgium (n = 1), and Finland (n = 1). Settings comprise psychiatric inpatient environments (acute and secure units and residential services). Services are representative of both private and state-funded facilities, serving urban and rural populations. Studies were conducted across child and adolescent settings (n = 10), adolescent-only environments (n = 5; one of which is female only), with one study focussing exclusively on a child-oriented service. Most designs (n = 13) are retrospective. All included studies were quantitative in nature, reflecting the paucity of empirical qualitative research in the current literature reporting on the physical restraint of children and adolescents in mental health care. There is evidence of total population sampling (n = 5). Two publications provide weak descriptions of sampling and recruitment. Most (n = 15) do not acknowledge the relationship between researcher and participant.
Summary of key factors.
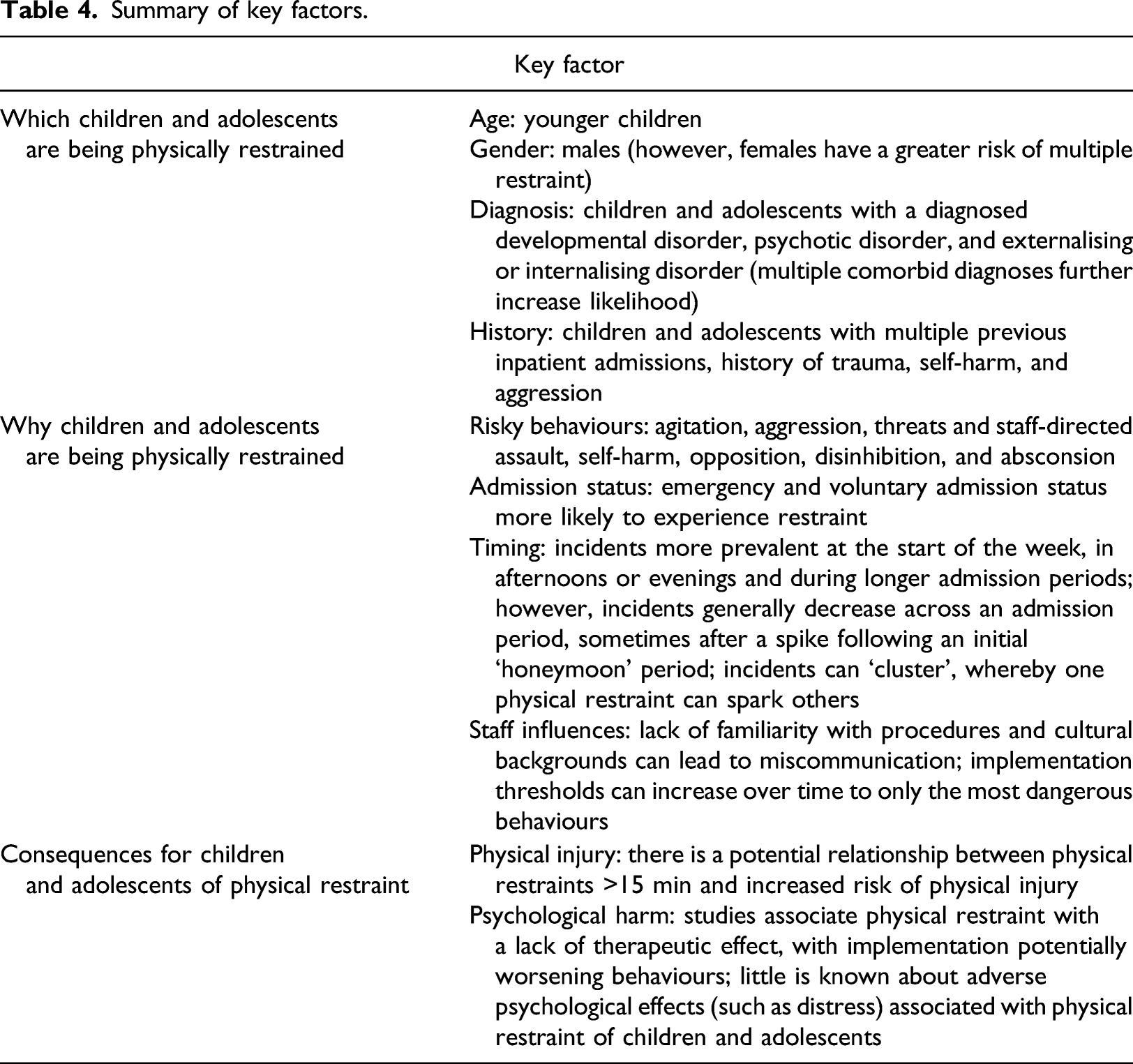
Which children and adolescents are being physically restrained in inpatient mental health services?
Five studies cite that between 27% and 44% of their demographic experienced some type of physical restraint during treatment: 27% (Tompsett et al., 2011), 36.3% (Furre et al., 2016), 38% (Leidy et al., 2006), 40% (Sourander et al., 2002), and 44% (Muir-Cochrane et al., 2014). However, most studies recognise that some incidents of physical restraint use remain underreported (Crocker et al., 2010; Donovan et al., 2003; dosReis et al., 2010; Furre et al., 2014, 2016, 2017; Leidy et al., 2006; Muir-Cochrane et al., 2014; Pogge et al., 2013; Tompsett et al., 2011). dosReis et al. (2010) report that 60% of physically restrained children (n = 156) experienced, on average, 14 physical restraints each, potentially identifying a group of children who may be at relatively high risk of physical restraint– and/or psychological restraint–related harm.
Association between a child or adolescent’s age and being physically restrained
Younger age (<13 years) is associated with an increased likelihood of physical restraint experience in 10 studies (Azeem et al., 2011; dosReis et al., 2010; Duke et al., 2014; Furre et al., 2014; Leidy et al., 2006; Muir-Cochrane et al., 2014; Pogge et al., 2013; Sourander et al., 2002; Stewart et al., 2010, 2013). Younger children are reported to be more overtly aggressive (Duke et al., 2014; Pogge et al., 2013; Sourander et al., 2002), with aggression being strongly associated with physical restraint. Four studies cite no association between age and physical restraint (Crocker et al., 2010; Delaney and Fogg, 2005; Donovan et al., 2003; Tompsett et al., 2010), although methodological weaknesses are identified in each study (see Table 1). The earliest study (Donovan et al., 2003) excluded interventions lasting less than 15 min, a time period which has subsequently been identified as most common for physical restraint of younger children in this environment (Pogge et al., 2013).
Association between a child or adolescent’s gender and being physically restrained
Five studies report that males (regardless of age) are physically restrained significantly more often than females (Delaney and Fogg, 2005; Duke et al., 2014; Stewart et al., 2010, 2013 Sourander et al., 2002), with reported figures of 70% of male children and adolescents being restrained (Duke et al., 2014), whereas three studies report females as having a greater risk of multiple physical restraints than males (dosReis et al., 2010; Furre et al., 2017; Muir-Cochrane et al., 2014). However, the variation in demographics (e.g., age of children and proportion of males to females) means that interpretation is challenging. Crocker et al. (2010) found no identifiable association between gender and physical restraint in their relatively small (n = 41) majority male population (78%; n = 32).
Association between diagnosis/psychosocial functioning and being physically restrained
Restraint incidence is positively associated with children and adolescents with developmental disorders (Azeem et al., 2011; Duke et al., 2014; Sourander et al., 2002), psychotic disorder (Delaney and Fogg, 2005; Furre et al., 2014; Sourander et al., 2002), externalising disorders (conduct/oppositional/disruptive disorders) (Azeem et al., 2011; Crocker et al., 2010; Furre et al., 2014; Leidy et al., 2006; Sourander et al., 2002), and internalising disorders (mood, and depression and anxiety) (Azeem et al., 2011; Delaney and Fogg, 2005; dosReis et al., 2010; Leidy et al., 2006). Crocker et al. (2010), Delaney and Fogg (2005), and Duke et al. (2014) report that having multiple (comorbid) diagnoses further increases the likelihood of the use of physical restraint (comorbidity indicating conditions which coexist in the context of the index condition (Yancik et al., 2007)). Three studies present findings which suggest that it is psychosocial functioning, rather than diagnostic status, which reliably predicts physical restraint experiences (Furre et al., 2014, 2016; Stewart et al., 2013).
Association between a child or adolescent’s history and being physically restrained
Physical restraint incidence is positively associated with multiple previous inpatient admissions (Delaney and Fogg, 2005; Furre et al., 2014, 2016), past trauma (Azeem et al., 2011; Delaney and Fogg, 2005; dosReis et al., 2010; Duke et al., 2014; Furre et al., 2014; Tompsett et al., 2011), and history of aggression (Crocker et al., 2010; Duke et al., 2014; Tompsett et al., 2011). Four studies associate a history of self-harm with increased likelihood of physical restraint (Delaney and Fogg, 2005; Furre et al., 2016; Sourander et al., 2002; Stewart et al., 2010).
Reasons why children and adolescents are reported as being physically restrained in inpatient mental health services
Intrinsic factors associated with children and adolescents being physically restrained
Crocker et al. (2010) identify how an increase in a child or adolescent’s risky behaviour (presentations associated with aggression and disruptive behaviour disorder) is linked to them being more likely to be physically restrained. Delaney and Fogg (2005) report the most prevalent risky behaviours as agitation, threats, and staff-directed assault (most of which were extremely violent). A child or adolescent’s aggressive acts (defined as harmful behaviour which may include deliberate intent to harm or injure another person (Bandura, 1973, cited in Suris et al., (2004)) most frequently trigger the use of physical restraint (Crocker et al., 2010; Delaney and Fogg, 2005; dosReis et al., 2010; Duke et al., 2014; Furre et al., 2016; Muire-Cochrane et al., 2014; Pogge et al., 2013; Sourander et al., 2002; Stewart et al., 2010, 2013; Tompsett et al., 2011), with child-to-staff aggression being identified as a common precursor (Sourander et al., 2002; Tompsett et al., 2011). Studies also associate the use of physical restraint with ‘lower level’ behaviours (opposition, disinhibition, and absconsion) (Duke et al., 2014; Furre et al., 2016; Muir-Cochrane et al., 2014) as well as destruction of property (Furre et al., 2016; Muir-Cochrane et al., 2014). Self-harming behaviours significantly increase the likelihood of a child or adolescent being physically restrained (Furre et al., 2016; Muir-Cochrane et al., 2014; Stewart et al., 2010), whereas suicidal acts decrease this likelihood in favour of alternative management approaches (Sourander et al., 2002).
Extrinsic factors associated with children and adolescents being physically restrained
Leidy et al. (2006) found that children and adolescents whose admissions were mandated were twice as likely to experience multiple physical restraints. However, this is contradicted by three studies which report that mandatorily admitted children and adolescents experienced fewer physical restraints than their voluntarily admitted peers (Azeem et al., 2011; Donovan et al., 2003; Furre et al., 2016). Donovan et al. (2003) report that children and adolescents admitted on an emergency basis (52%; n = 111) were 4.6 times more likely to experience physical restraint than planned admission peers. Similarly, Crocker et al. (2010) report that 82% of children and adolescents (n = 9) admitted as an emergency experienced physical restraint. No article which discussed the status of emergency admission included a clear definition of what constituted an emergency. Although the Department of Health (2013) defines emergency admissions as those which are unpredictable and unplanned, it is not possible to ascertain if this definition aligns with the terminology used in the individual studies within this review.
The literature indicates that the day of the week and the time of the day may influence the prevalence of physical restraint within inpatient mental health settings. Crocker et al. (2010) and Leidy et al. (2006) indicate that physical restraints are more prevalent at the beginning of the week, before steadily decreasing towards Friday. Crocker et al. (2010) identify that fewer incidents occur Friday–Sunday (when most children and adolescents were on home leave), whereas Leidy et al. (2006) report an increase again over the weekend, reinforcing how trends bear relevance only in respect of individual service provision. Four studies (Delaney and Fogg, 2005; dosReis et al., 2010; Furre et al., 2016; Leidy et al., 2006) found that physical restraint is more likely to occur in the afternoon or evening. Two studies found an overall decrease in physical restraints during an admission period (Furre et al., 2016; Leidy et al., 2006), whereas dosReis et al. (2010) reported the opposite, perhaps identifying the existence of an initial ‘honeymoon’ period (where more communicative and/or behavioural effort is expended by children, adolescents, and staff earlier in an admission).
Eight studies claim that longer admission periods are linked to an increase in the likelihood of physical restraint being used (Delaney and Fogg, 2005; dosReis et al., 2010; Furre et al., 2016; Leidy et al., 2006; Pogge et al., 2013; Sourander et al., 2002; Stewart et al., 2013; Tompsett et al., 2011). Whilst the length of stay is an important factor, Leidy et al. (2006) report that its association with physical restraint is not straightforward. Tompsett et al. (2011) offer a practical explanation, suggesting that children and adolescents simply have more time in which to aggress as the length of stay increases. Leidy et al. (2006) identify potential ‘clustering’, 75% of physical restraints (n = 794) occurred on less than 20% of the days, with 25% (n = 265) occurring on just 3% of the days, potentially highlighting a ‘chain reaction’, whereby one physical restraint has the potential to ‘spark’ others.
Four studies report how multiple interventions were attempted prior to physical restraint (Delaney and Fogg, 2005; Muir-Cochrane et al., 2014; Pogge et al., 2013; Sourander et al., 2002). Delaney and Fogg (2005) report that ‘as-needed’ medication (typically antipsychotic and/or sedative) was used before 38% (n = 45) of physical restraint incidents, although the authors report that no further information was available to explore the reasons why physical restraint was subsequently implemented. Five studies show how the use of physical restraint is partly determined by the familiarity of staff with policies (dosReis et al., 2010; Donovan et al., 2003; Furre et al., 2014, 2016, 2017). dosReis et al. (2010) and Donovan et al. (2003) describe how, as time progresses, the threshold for staff using physical restraint increases, with intervention implementation becoming selectively focused on the most dangerous behaviours. Staff members’ lack of familiarity with non-native cultural backgrounds may also lead to misperceptions that some children and adolescents are dangerous, leading to miscommunication and mistrust from both perspectives (dosReis et al., 2010; Furre et al., 2014). Children and adolescents from minority communities have a higher proportion of unmet mental health needs and have often developed more serious symptoms at the point of admission, placing them at a higher risk of physical restraint (Donovan et al., 2003).
Reported consequences for children and adolescents of physical restraint use in inpatient mental health services
Physical consequences of children and adolescents being physically restrained
dosReis et al. (2010) draw attention to the potential for children and adolescents to be exposed to physical (and psychological) harm through increased restraint incidences. Two studies discuss a relationship between longer duration of physical restraint and increased risk of physical harm (Duke et al., 2014; Furre et al., 2016), with Furre et al. (2016) highlighting how restraint duration should be as short as possible to reduce any potentially harmful effects. Donovan et al. (2003) note a reduction of physical restraint frequency (by 26%) and duration (by 38%) over the two-year period of their naturalistic retrospective study. However, there was a proportional increase in the number of children and adolescent’s restraint-related physical injuries (from 4% to 8%) over the same time, suggesting that reduced physical injury risk may not be directly proportional to reduced physical restraint frequency or duration. It is difficult to interpret findings further as physical restraints <15 min were excluded from the study.
Psychological consequences of children and adolescents being physically restrained
None of the reviewed studies reported child-reported psychological consequences of physical restraint. Pogge et al. (2013) suggest that some interventions could provide therapeutic benefits, although this is not drawn from empirical evidence. Two studies associate physical restraint with a lack of therapeutic effect (Duke et al., 2014) and a potential to worsen behaviours (Crocker et al., 2010; Duke et al., 2014). Health of the Nation Outcome Scale scores (measuring general health and social functioning) were available for 35% of admitted children (n = 47) in the study by Duke et al. (2014), with scores suggesting global improvements across children and adolescent’s admission periods, with no differences between those who did and did not experience physical restraint. However, the authors do not specify if scores were self-rated (by the children or adolescents), parent-rated, or clinician-rated. Further, the authors note that the retrospective dataset did not allow investigation of more immediate adverse effects associated with physical restraint (such as distress). Therefore, this finding should be viewed with some caution.
Discussion
This is the first systematic review which synthesises research reporting which children and adolescents are being physically restrained in mental health inpatient services, the reasons why, and any potential associated consequences. This review addresses recommendations from an earlier review (DeHert et al., 2011), which called for a focus on indications and predictors, clinical outcomes, and effectiveness of physical restraint of children. Previous systematic reviews have been conducted examining restraint use with adults in mental health care (Dahm et al., 2017; Wilson et al., 2015) and general health care (Mohler et al., 2016) as well as with children in general paediatric care (Bray et al., 2014; Kirwan and Coyne, 2016). There has also been a tendency to approach this subject through examination of the perspectives of nursing staff (Demir, 2007; Kirwan and Coyne, 2016).
The implementation of physical restraint results from complex, dynamic, and reactive decision-making by front-line care providers and can be based upon a combination of patient (intrinsic) and environmental (extrinsic) factors. Some of the more frequently reported characteristics include a child or adolescent’s age, gender, diagnosis, and history, with males restrained significantly more often than females (Delaney and Fogg, 2005; Duke et al., 2014; Stewart et al., 2010, 2013; Sourander et al., 2002) although females can have a greater risk of multiple restraints (dosReis et al., 2010; Furre et al., 2017; Muir-Cochrane et al., 2014). Having a formal diagnosis regularly emerges as a predictor of physical restraint (Azeem et al., 2011; Crocker et al., 2010; Delaney and Fogg, 2005; dosReis et al., 2010; Duke et al., 2014; Furre et al., 2014, 2016; Leidy et al., 2006; Sourander et al., 2002; Stewart et al., 2013). Organisational factors, a child or adolescent’s admission status, longer length of stay, miscommunication, and mistrust of staff (and children) can also contribute to the reasons for physical restraint implementation.
Physical restraint is generally more likely to be used earlier in an admission (dosReis et al., 2010; Furre et al., 2016; Leidy et al., 2006), in the afternoons or evening (Delaney and Fogg, 2005; dosReis et al., 2010; Furre et al., 2016; Leidy et al., 2006). There is also some potential ‘clustering’ of incidents (Leidy et al., 2006). Individually, these characteristics can have predictive merits. In combination, some stronger predictive traits potentially emerge. Several studies reported that multiple interventions were attempted prior to the implementation of restraint, although information concerning positive behavioural interventions (negating restraint use altogether) was rarely reported in the identified literature included within this review. One study excluded interventions lasting less than 15 min (Donovan et al., 2003), although no clear reason was reported for only including interventions where physical restraint lasted longer than 15 min. Contemporary evidence (Mental Health Commission, 2013) shows that 90% of physical restraints (both with children and adult inpatients) last 15 min or less, meaning that if Donovan’s cut-off point was used in current research, most episodes of restraint would be missed. Most studies discuss the physical consequences associated with physical restraint, including physical injury. A focus on physical harm can result in psychological harm (rarely discussed in depth) being overlooked (Bray et al., 2014). There is anecdotal mention of potential therapeutic benefits of physical restraint (Pogge et al., 2013), although the evidence supporting this claim is weak.
DeHert et al. (2011) highlight the importance of the development of restraint guidelines which take into account the input of children. Whilst restraint reduction remains high on the agenda (Department of Health, 2014, 2017), guidelines exist (Ridely and Leitch, 2019), and evaluation of initiatives is important (Caldwell et al., 2014; Valenkamp et al., 2014; Wilson et al., 2015), but the evidence shows that restraint reduction training alone does not necessarily negate the risk of physical injury (Challenging Behaviour Foundation, 2019; Ridely and Leitch, 2019). Restraint implementation with children and adolescents can be enhanced through a richer understanding of the impact of the intervention (Demir, 2007), with credibility existing in the words of those who experience mental health services first-hand (Caldwell et al., 2014). This review has identified that there are no published UK studies focussing on children’s first-hand reported experiences of physical restraint within inpatient child and adolescent mental health services. Services must be able to take into account the individual needs voiced by the children under their care (Caldwell et al., 2014). Therefore, more research is needed to better understand the variables that can lead to restraint (Kirwan and Coyne, 2016) and to listen to what children and adolescents say about their experiences of physical restraint in mental health care.
Limitations
This review is subject to limitations within the available evidence base. Services are representative of both clinical and residential settings. Although the context and culture of service provision were examined, this was not consistently or effectively reported. However, of those articles (n = 11) that did report context, it was clear that some provision was delivered more intensively (dosReis et al., 2003; Leidy et al., 2006; Stewart et al., 2010, 2013) than others (Crocker et al., 2010; Donovan et al., 2003; Furre et al., 2014, 2016, 2017; Sourander et al., 2002; Tompsett et al., 2011). Where resources were available, residential providers appeared positioned to provide more personalised, intensive treatment (Stewart et al., 2010). Some data from clinical providers were reported as more nationally representative (Furre et al., 2017; Sourander et al., 2002), although there is recognition that within both contexts, there is room for improvement on how clinical information is recorded (Furre et al., 2014, 2016, 2017; Leidy et al., 2006), which has the potential to impact review findings. Additionally, there remains a reliance on proxy reporting of physical restraint outcomes for children and adolescents admitted to mental health services. The results of this review rely on a small number of empirical studies, most of which relied on retrospective data which can be prone to missing or unreported data. The study populations differed in terms of age, setting characteristics, and duration of admission periods making some comparisons challenging.
Recommendations
There is a need to explore children and adolescents’ perceptions about physical restraint and the impact of physical restraint frequency on health outcomes. Future research should continue to assess the use of physical restraint with children and adolescents. Studies should specifically focus upon understanding the effect that physical restraint has upon children and adolescents in mental health care. Studies should also focus on determining, through collaboration with children, the most appropriate use of physical restraint, including the most appropriate approaches for using the intervention when alternative strategies may be more beneficial to the well-being of children, adolescents, and staff.
Conclusion
This review highlighted some common characteristics associated with children and adolescents who have experienced physical restraint in inpatient mental health care, as well as common reasons for implementation. There remains a reliance on retrospective data, single-centre studies, and proxy reporting of outcomes. This review has identified the absence of first-hand reported accounts of children and adolescents who have experienced physical restraint in inpatient mental healthcare services.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
