Abstract
Building on research on the critical role of laypeople in medicalization and the multi-dimensional character of this process, this study explores the effects and meanings of the ADHD category for mothers and teachers of diagnosed children. Based on interviews with 27 schoolteachers from two different schools and 42 mothers of children diagnosed with ADHD, we show that despite the growing acceptance of ADHD as a medical diagnosis, it exhibits only minor narrative, institutional, and moral effects in school and family arenas. The diagnostic label attributed to children does not resolve blame games and uncertainty about the source of children’s difficulties and does not provide many pragmatic benefits for either mothers or teachers. We argue that these limited narrative, moral and institutional effects are shaped by the moral positionings available to mothers and teachers, the institutional status of ADHD as a category of disability, and educational policy. We distinguish medicalization’s institutional and interpersonal dimensions and explore their complex interrelations. Our analysis resonates with recent moves in medical sociology toward more pragmatic and practice-based analyses of the effects of medical categories, particularly when enacted outside traditional healthcare settings.
Introduction
Understandings of self and personhood are increasingly influenced by scientific discourses about the brain (O’Connor and Joffe, 2013), particularly for conditions perceived to be intimately linked with personhood, such as Attention Deficit/Hyperactivity Disorder (ADHD). In sociology, ADHD has served as a paradigmatic case of medicalization, the process “by which nonmedical problems become defined and treated as medical problems, usually in terms of illness and disorders” (Conrad, 2007: 4). This study explores the effects and meanings of ADHD—the most common neurodevelopmental disorder diagnosed in children (Bergey and Filipe, 2018) among parents and teachers of diagnosed children. We ask how the category is perceived and deployed by adults who play important roles in children’s lives, focusing on the institutional and moral-interactional dimensions of medicalization.
Such a perspective is particularly timely due to the recognition that non-medical actors increasingly participate in promoting medicalized answers to problems of living (Bergey, 2024; Conrad, 2005). Furthermore, social research on childhood medicalization shows that the expectation that ADHD diagnosis transfers moral blame for children’s unwanted behaviors to their brain and hence “blame[s] none of the victims: neither parents, children, nor society” (Lakoff, 2000: 166), is not borne out in ethnographic and interview-based research (Singh, 2004). Nor does the inclusion of ADHD as a protected disability category—an increasing trend in recent years in Israel and in other countries—ensure institutional recognition and resources to diagnosed school children in practice (Bergey and Conrad, 2018).
Based on interview research with mothers and teachers of ADHD-diagnosed children, and building on and integrating literature from the sociology of education, medicine, and family life, we show that despite its broad acceptance in the medical field, the ADHD label has relatively limited power in family and school arenas. Focusing on the narrative, moral and institutional effects of medical diagnosis on teachers and mothers, we argue that these effects are shaped by moral positionings available to mothers and teachers, the institutional status of ADHD as a category of disability, and related educational policy. Our analysis resonates with recent moves in medical sociology toward more pragmatic and practice-based analyses of health and medicine, calling for closer attention to the multifaceted and uneven effects that medical categories generate (Brown and Tavory, 2024; Halfmann, 2012; Showalter, 2019), particularly when enacted outside traditional healthcare settings (Bergey, 2024).
Medicalization: From discursive to multidimensional social process
Conrad and Schneider (1992) theorized medicalization as process that can occur at a conceptual, institutional, or interpersonal level. The key threshold for determining whether a problem is “medicalized” is whether it is discursively framed as medical in nature, usually by medical experts. In the past two decades, studies of medicalization have pointed to the distributed character of this process and the critical role of laypeople in it (Bergey, 2024; Conrad, 2005). More recently, scholars have also called for a more multidimensional approach that examines the identities, practices and effects that enact medicalized realities (Bergey, 2024; Halfmann, 2012; Showalter, 2019), in contrast to the traditional focus on the motivations and social factors leading up to medicalization (Brown and Tavory, 2024:2). For example, medicalization can reveal different effects depending on the dimensions where such effects are examined (such as the discourses, practices, and identities of different actors), or the observed level of analysis (micro, meso, macro) (Halfmann, 2012). Exploring the history of psychopathy, Showalter shows that defining “psychopathy” as a diagnostic psychiatric category and classifying people as such did not bring about medical effects in terms of actual treatment (Showalter, 2019). Thus, contra authors who view medicalization as a more total, society-wide process (e.g. Conrad, 2007), Showalter argues that medicalization is not a unified social phenomenon, and that conceptualizing a problem as “medical” does not necessarily change the logic and practices through which a condition is addressed. Similarly, Halfmann (2012) also shows that the conceptual, institutional and practical effects of “medicalization” are distinct from one another and can even contradict each other. Building on Conrad and Schneider’s (1992) typology of the dimensions of medicalization, Halfmann (2012) describes the institutional level as referring mainly to organizations that adopt a medical approach to a problem, and the interactional level as addressing interpersonal relations and communication among various actors.
In this paper, we address medicalization in two dimensions: institutional (top-down imperatives of educational policy and institutional status of ADHD at school) and moral-interpersonal (the moral positioning and “blame games” of teachers versus parents). By including the experiences of both mothers and teachers, we are able to highlight similarities in meanings and practices, which draw from the uneven effects of ADHD as a medical category in schools and family settings.
Narrative, moral, and institutional effects of ADHD diagnosis
Our analysis of the specific effects of the medical category of ADHD on mothers and teachers departs from earlier critical accounts of medicalization, which emphasized its broad and dominating influence, such as Timimi’s (2010) examination of the impact of market-driven healthcare policies on childhood mental health in a neoliberal context. We are informed by studies that investigate how ADHD is enacted by professionals and laypeople, revealing a complex interplay between medical discourse and everyday life (Pickersgill, 2013), and highlighting local concerns as “bottom-up factors in the introduction and adoption of ADHD diagnoses” (Slagboom et al., 2021: 114400). Diagnostic categories have profound effects on “making up people” (Hacking, 2004), suggesting an etiology of suffering, and hence implying hidden moral assumptions (Jutel and Nettleton, 2011; Plotkin-Amrami, 2016). Yet, authors have also found that diagnoses differ in their supposed medical legitimacy, in their associated stigma, in their centrality to the child’s self (Francis, 2012; O’Connor et al., 2022), as well as in their meanings, which “derive from social interaction and are modified by interpretations in practice” (Brown, 1995: 46). In other words, defining a problem as biomedical does not overshadow cultural notions of selfhood and moral responsibility, which interact in diverse ways with different diagnoses and contexts (Jutel and Nettleton, 2011; McLeod, 2023; O’Connor and Joffe, 2013).
Although medical diagnosis can potentially diminish attribution of moral responsibility and disapproval of the diagnosed person (Honkasilta et al., 2016; Wienen et al., 2019), this is less evident in the case of childhood ADHD. Scholarship shows that despite a major cultural and medical shift to classifying ADHD as a brain-based neurodevelopmental disorder, biomedical understandings do not “eclipse. . . nonpathological interpretations” of children’s unwanted behaviors (Carpenter-Song, 2009: 66; cf., Malacrida, 2003; Rafalovich, 2004). Mothers are particularly held to account for children’s misbehavior, as Singh (2004) has shown, elaborating the failure of potential “brain blame” to replace “mother blame” in the case of ADHD. Singh’s findings resonate with the perseverance of maternal culpability for a variety of children’s health conditions (Blum, 2015).
Several compelling ethnographic works on childhood ADHD in family and school settings evoke the intense moral work by adults surrounding children with ADHD. They show that in managing children’s stigmatized behaviors, adults continuously interpret and classify children’s actions, seeking to distinguish those for which the child is culpable, versus those that can be attributed to the disorder (Garro and Yarris, 2009; Versteeg and Te Molder, 2018). Frigerio et al. (2013: 598) extended such observations of everyday moral positioning to show how teachers, parents and physicians can be drawn into a mutual “blame game” (cf., Malacrida, 2003; Rafalovich, 2004). For example, parents and mental health professionals may blame teachers for their outdated teaching practices and the child’s lagging school performance, while teachers may try to displace responsibility for children’s school difficulties onto parents and medical professionals (Frigerio et al., 2013). Indeed, the controversial etiology of ADHD exacerbates interpretive conflicts between schools and families (Gwernan-Jones et al., 2015; cf., Ewe, 2019; Malacrida, 2003; Rafalovich, 2004); scholarship shows that adults take diverse positions on the biomedical dimension of ADHD to advance their moral positioning, sometimes arguing for a more biomedical understanding of ADHD, and sometimes arguing against it (Bröer and Heerings, 2013; Carpenter-Song, 2009; Horton-Salway and Davies, 2015; Simoni, 2021; Slagboom et al., 2021). By discussing the moral effects of the ADHD category on mothers and teachers of diagnosed children, we build on blame dynamics while moving beyond them to show that both sides often identify with each other and feel a personal responsibility for the child’s functioning and unrealistic expectations to control it.
In educational institutions, disability categories vary substantially in the institutional resources they afford and in their degree of associated stigma (Fish, 2019). In the case of childhood ADHD, attention to the institutional effects of medicalization is especially significant since the “politics of care” are distributed among medical and school arenas, often with little coordination between them (Akrich and Rabeharisoa, 2018). ADHD is increasingly included in protected categories of disability in many countries (Bergey and Filipe, 2018), including in Israel; diagnosis can be a vehicle to institutional recognition, and a means of channeling resources and increasing social acceptance of the diagnosed person (Farrugia, 2009; Jutel and Nettleton, 2011; Ryan and Cole, 2009). Yet, in the contemporary landscape, ADHD characteristically “falls through the cracks” between health and school institutions, and diagnosis does not easily translate into school resources and accommodations (Prosser and Graham, 2018: 61; cf., Akrich and Rabeharisoa, 2018). The Israeli situation is similar, including at schools serving relatively privileged communities (Plotkin-Amrami and Fried, 2024; Plotkin-Amrami et al., 2024). These problems are exacerbated by chronic understaffing and budget crises across the system, which is highly centralized; and by cultural understandings of children’s distress that feed ambivalence toward ADHD as a medical category (Fried and Plotkin-Amrami, 2023).
Exploring childhood ADHD in schools can shed light on the interrelated social and material dimensions of disability, a critical empirical task since schools are often discussed as a main institution driving medicalization (Wienen et al., 2019), and are responsible for meeting children’s diverse needs outside the family.
ADHD in the Israeli context
Rates of ADHD diagnosis and treatment have increased rapidly in Israel in the past two decades (Davidovitch et al., 2017). Public health officials have prioritized early diagnosis and treatment of childhood ADHD (Israel Ministry of Health, 2008), for example by granting every child a free ADHD evaluation and subsidized pharmaceutical treatment.
The rising rates of diagnosis of ADHD and other childhood disabilities is related to two major education reforms in recent years that aim to promote the mainstreaming of pupils with disabilities. “From Disabilities to Learning” was launched in 2017 in response to the marked increase in students seeking formal recognition for “common” special educational needs (SEN) such as learning disabilities and ADHD. This reform aims to improve teacher training in identifying and teaching students with learning differences, so as to reduce schools’ reliance on pupil-specific accommodations. The “Inclusion and Integration” reform was enacted in 2019 to facilitate the inclusion of students with SEN in mainstream classrooms, by strengthening parents’ rights to choose mainstream as opposed to special education school placement for children with SEN. Both reforms espouse a social model of disability, promoting teaching practices that are adaptive to heterogeneous classrooms, and express ideals of social equality and inclusion. Teachers are at the forefront in carrying out such inclusive education practices and are “responsible. . . for providing the best possible response to the needs of pupils” with variable needs (Israel Ministry of Education, 2021: 22).
In Israel, most students with ADHD are enrolled in mainstream classrooms and, ideally, should receive “adjustments in teaching methods and testing” (Monnickedem-Givon, 2021), such as simply-worded instructions during lessons, or extra time on exams. However, these adjustments are not always fulfilled due to schools’ lack of staff and resources, and to the absence of professional training. Moreover, ADHD is institutionally defined as a “common” and mild SEN (to contrast with those classified as “uncommon” and more severe such as autism or intellectual disability). Accordingly, the supports available for ADHD-diagnosed pupils—such as tutoring or short-term psychotherapy—come out of schools’ general operating budget and are not mandated specifically for children with ADHD (Weissblei, 2023). In other words, while some resources are available, there is no requirement that a child with ADHD receive them. Thus, while recent educational reforms have called more attention to the needs of pupils with SEN, ADHD in itself has limited institutional power with respect to making resources and supports available to diagnosed pupils in Israeli schools (Akrich and Rabeharisoa, 2018; Prosser and Graham, 2018).
We wish to expand previous research insights on how the diagnostic category of ADHD shapes the interpretations and moral positioning of proximal adults. Focusing on the institutional and interactional levels of medicalization (Conrad and Schneider, 1992; Halfmann, 2012), we explore how teachers and parents deploy the diagnostic category of ADHD to explain children’s troubles and cope with them daily. Based on our findings, we show that despite the growing legitimacy of ADHD as a neurodevelopmental disorder and its recognition as a disability category, the diagnostic label does not resolve blame games and uncertainty about the source of children’s difficulties and does not provide many pragmatic benefits for either mothers or teachers. In other words, we point to a disconnection between the medical status of ADHD and its indeterminate effects in the family and school arenas. We argue that the dynamic effects of an ADHD diagnosis are shaped by the moral positioning it enables for teachers and mothers, its institutional status as a disability category, and discursive and policy imperatives to accommodate a diversity of children’s needs.
Research context and methodology
This article builds on a broad study of the medicalization of childhood in family and school arenas in the Israeli context. In this article, we integrate the analysis of mothers’ and teachers’ accounts, which we have previously analyzed separately (Fried and Plotkin-Amrami, 2023; Plotkin-Amrami and Fried, 2024; Plotkin-Amrami et al., 2024). We specifically recruited mothers, rather than parents, because mothers are pragmatically and symbolically held more responsible for managing children’s health (Ryan and Cole, 2009; Singh, 2004); this is especially relevant in Israeli society, where childcare and paid work are divided along traditional gender roles (Mann and Schechner, 2024).
Given that attitudes, experiences and practices surrounding ADHD diagnosis and treatment are significantly shaped by socioeconomic location (Carpenter-Song, 2009; Owens, 2020), we diversified both samples socioeconomically. We did not aim to compare social contexts but to achieve greater representativeness of our sample (Patton, 2014).
The study was carried out with IRB approval, and ethical permission to interview teachers was attained from the Israeli Ministry of Education.
Parts of the study have been presented to the Ministry of Education, and inform a teacher training course taught by the first author.
Data collection
The study used a stratified, purposive sampling strategy (Patton, 2014). Teachers were recruited via contacts with school principals, and mothers were recruited by word-of-mouth and via online posts. Mothers were compensated for their time with a prepaid shopping card. We predetermined a minimum sample size of 24 teachers and 36 mothers, which is considered sufficient for analytical comparison among two and three subsamples, respectively (Hennink and Kaiser, 2022). We predetermine a larger minimum sample size for mothers due to the greater expected variation in interviewee variables such as gender and ages of diagnosed children.
Interviewees received a transparent explanation of the nature of the project, emphasizing that the purpose was not to judge or evaluate their functioning as teachers or as mothers. Transcripts were anonymized using random pseudonyms and omitting identifying details. All interviewees provided written informed consent.
The semi-structured questionnaires for teachers and parents aimed to capture interviewees’ experiences, interpretations and practices regarding children and ADHD. We began with broad questions about the interviewees’ background and experience, and moved to more specific questions on key topics that were relevant to the study, such as the emergence of the suspicion of ADHD in the family and at school; the perceived importance and effects of diagnosis and treatment; issues of labeling and stigma; and parental or professional challenges and practices. After completing the first 12 interviews, we modified the interview prompts in response to emerging data (for example, interviewees’ own ADHD diagnosis).
Interviews were conducted in person or over Zoom between February 2019 and September 2022. In addition to the interview protocol described above, mothers were encouraged to trace the broad arc of their parenting experience, from the child’s babyhood through the present. Thus, interviews with mothers were longer (ranging from 1 to 3 hours, mean 1h:44m) than teachers (1/2 to 1 hour, mean 41m). Interviews were conducted by the second author and two trained graduate students, recorded and transcribed verbatim. Both authors translated and crosschecked the transcripts for accuracy.
Participants
Teachers
The research team interviewed 27 schoolteachers from two different schools. One was an elementary school (ages 6–13) that serves mostly low-income families, including a large immigrant community. Of 13 teachers interviewed from the school, all were women, and four shared that they were also parents of children diagnosed with ADHD. The other school was a junior high school (ages 12–15) in a suburban town that served a community of mostly middle- to upper-middle income families. Of the 14 teachers interviewed at this school (13 female, 1 male), 10 had a child or immediate relative diagnosed with ADHD.
The different socioeconomic background and age range of the schools—which would be confounding variables in a comparative study—serve our aim to find “important shared patterns that cut across cases and derive their significance from having emerged out of heterogeneity,” based on the rationale of maximum variation sampling (Patton, 2014: 429).
Mothers
We interviewed 42 mothers of children diagnosed with ADHD from across Israel, ages 32–52 yo (mean 42 yo). Twenty-four mothers had the equivalent of a high school education, and 18 were college-educated; we deliberately recruited mothers with different education levels in order to diversify the sample socioeconomically.
The mothers’ children included 35 boys and 9 girls, ages 7–15 yo at the time of the interview (mean age 11). All children had been diagnosed at least a year prior to the interview and had tried pharmaceutical treatment. All mothers were Jewish and in heterosexual partnerships.
Table 1 lists the pseudonyms of interviewees quoted in this article.
List of interviewees by pseudonym.
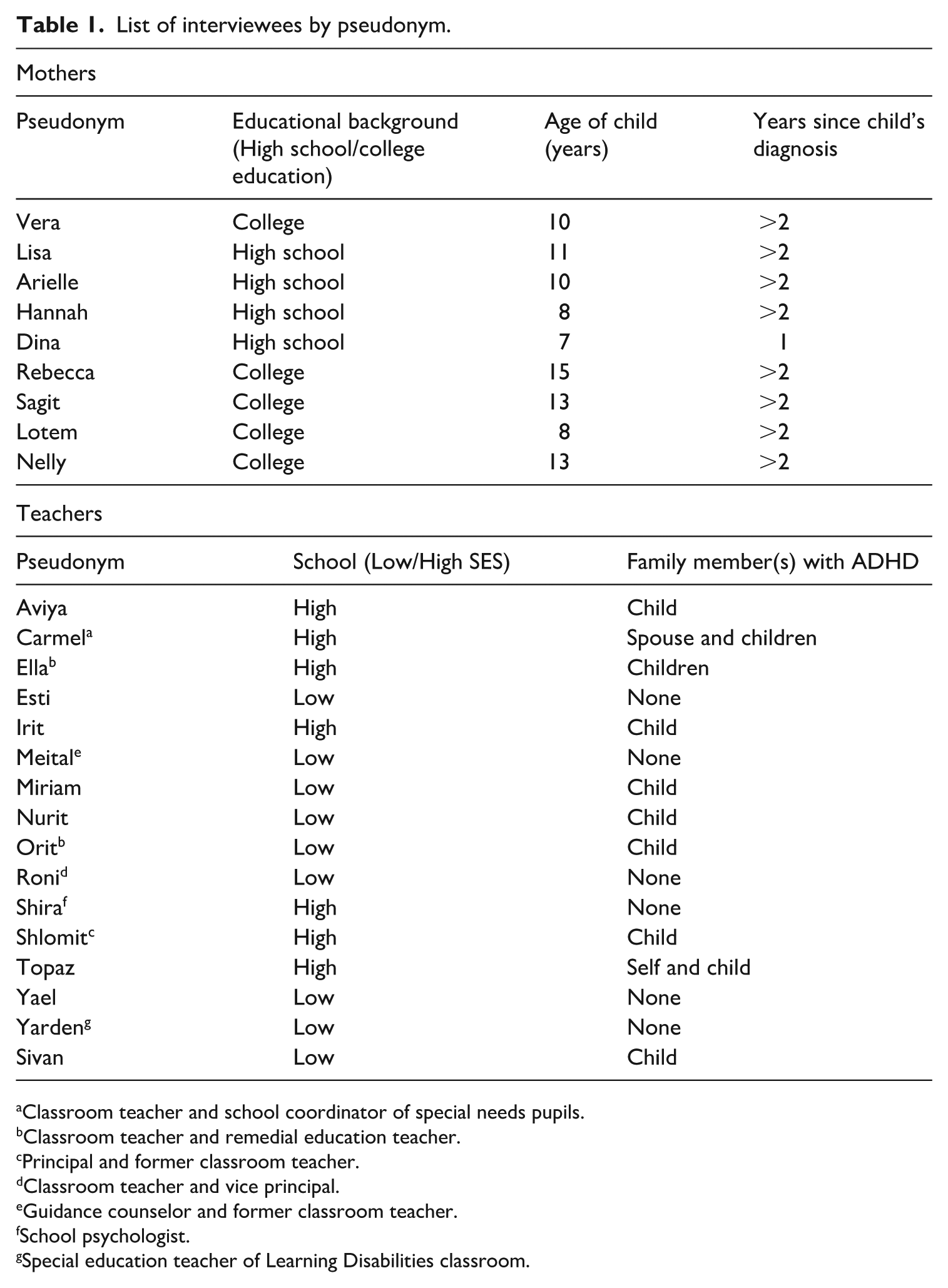
Classroom teacher and school coordinator of special needs pupils.
Classroom teacher and remedial education teacher.
Principal and former classroom teacher.
Classroom teacher and vice principal.
Guidance counselor and former classroom teacher.
School psychologist.
Special education teacher of Learning Disabilities classroom.
Analysis
We used principles from constructivist grounded theory to analyze the interviews (Charmaz, 2014), beginning from a preliminary set of sensitizing concepts that we recursively refined and elaborated in the course of ongoing interviewing and analysis (e.g. stigma, knowledge). To capture interviewees’ situated perspectives, explanations, assumptions and actions, as well as implicit meanings within the interview data, we applied a process of initial and then focused coding using the atlas.ti program. We developed the codes into concepts through iterative comparison within the data and between the findings and their emerging theorization, as well as through continuous memo-writing and reflection as a research team. As key analytical categories emerged from the data, we organized them to conceptualize how interviewees understood the ADHD label and their role in relation to the child, seeking similarities and differences between our interlocutors (Charmaz, 2014).
Findings
The narrative effects of ADHD: Framing the source and meaning of children’s troubles
Most teachers pointed to the existence of a biological dimension of ADHD: “The disorder is something physiological,” Carmel; it is a “short circuit in the brain” (Sivan). Yet, most also posited that ADHD is a consequence of various environmental factors, such as social media and the stressful pace of modern life. Several teachers combined conflicting narratives, such as Nurit, who said that ADHD is “a congenital disorder” that might be related to something “in the mother’s life, in pregnancy,” but that “the nutritional part can also have a lot of impact. . ..Of course, I’d add that it can also be an emotional issue, the student may have some problem. . . he’s dealing with at home.” Like many teachers, Ella said a child’s challenges “could have something to do with boundaries, with attention, with other emotional or social difficulties”; but, she observed, “we rush to label it and say they have ADHD.”
Most teachers believed that diagnosis could be beneficial: “You can. . . come help them. . . and not classify them as lazy, untalented” (Yarden). However, the label did not clarify the significance of children’s problems in particular cases. Teachers said that distinguishing general difficulties from those associated with ADHD was “confusing. . . sometimes I don’t know to say if it’s emotional. . . or attentional” (Meital). They also tended to couch particular children’ difficulties in reference to the child’s family background and social milieu, in ways that were at times judgmental or sympathetic. In the low-income neighborhood, teachers addressed the difficult circumstances of families (“They have no support at home,” Yarden; “They’re so troubled by daily life. . . They’re not in a situation where they can learn,” Yael). At the school where families were financially better off, teachers expressed disapproval of parents who “think money will solve every problem” or who are not willing to “give up their career for their children’s sake” (Irit). At both schools, the effect was to fortify the view that problems associated with ADHD are ultimately under parents’ control: “Even if there is a problem, I can still do many things to control it. . .. The parents don’t have the tools and they give in to the kids and allow them to do whatever they want” (Shlomit).
Similar to teachers, mothers also expressed ongoing uncertainty about the source and meaning of their children’s ADHD-associated difficulties. For some mothers, receiving the ADHD diagnosis made their child’s challenging behaviors seem more forgivable, and it empowered them to advocate more confidently for their child at school. These mothers said that the diagnosis made teachers take the child’s difficulties more seriously, and view parents as more “cooperative” and responsible. Yet, at the same time, the diagnosis did not introduce a static meaning around which the child’s “trouble” was easily reworked. Most mothers saw ADHD as a narrow neurological problem synonymous with lack of “concentration”; they did not think the ADHD diagnosis sufficiently explained the child’s troubles, which they often described as “emotional” in nature. Arielle was emphatic that her son’s extreme sensitivity and meltdowns at school were unequivocally separate from ADHD: “If you ask me, he has nothing. He just has an emotional problem, which is something that can be treated by a psychologist.” Hannah attributed her son’s angry outbursts to “some stage in life” that “went wrong” with the birth of a younger sister; “I didn’t prepare him.”
Some mothers saw their children’s emotional difficulties—such as lack self-confidence, and difficulty making friends—as a consequence of mistreatment and stigma for having ADHD: “They are children who are very, very hurt, also socially, because they know they are not equal” (Rebecca). Other mothers suggested the opposite causal direction, or were unsure. Dina mused that ADHD “accompanies” emotional difficulties: “It starts with emotional difficulties and then later develops into ADHD. . . If I had taken care of things then like I should have. . .” But she quickly corrected herself: “No, actually that’s not right because it [ADHD] is hereditary. So it wouldn’t have made a difference.”
In short, we found that ADHD diagnoses have limited narrative power for mothers in trying to make sense of the source of their children’s painful life experiences and challenges; and that the uneven interpretive effects of diagnosis were resonant with the uncertainties of teachers. In interviews with both mothers and teachers we saw ongoing attempts to “get to the bottom” of children’s genuine source of difficulty, which the ADHD diagnosis did not definitively settle. As we will show next, nor did it release mothers or teachers from a sense of responsibility, and even blame, for children’s struggles.
Moral effects and blame
Both mothers and teachers continued to experience and to cast blame for children’s difficulties following diagnosis. Mothers described being embarrassed and shamed for their child’s stigmatizing behavior in various social situations. Sagit said that gatherings with extended family were “very difficult. The stares. The advice. The feeling that they’d prefer it if we didn’t come over.” She describes her extended family’s ridicule and criticisms of her functioning as a mother: My father said, ‘if you give them Paracetamol, you’ll see it has the same effect’ [as stimulant medication]. He said to me once, that my children have problems because I’m fat. It’s not pleasant for them. So therefore they have behavioral problems. . .. And that I don’t enforce boundaries with them. . . My brother said, ‘if you stopped going to so many professionals, things would be much easier. . . You’re just wasting your money.’
Almost all mothers described feeling chronically judged and blamed for their children’s behavior in public, such as at the supermarket or the playground. Lotem summarized: Your surroundings don’t understand it, and that’s the real battle. . . . . . A child with intellectual delay, a child with autism, people see it on them . . . [But] people don’t understand that a child with an attention problem is a child who doesn’t have that self-restraint. . . You’re always getting dirty looks and comments.
These examples reflect the limited moral effects of ADHD to reduce stigma and judgment of mothers for their children’s undesirable behaviors. The child’s ADHD is perceived as not severe enough to elicit compassion toward mothers (as in the case of children with more visible disabilities), yet sufficiently socially disturbing to justify blaming mothers for the child’s unruly behavior (Blum, 2015; McLeod, 2023).
Blame was also prominent in interviews with teachers, who said they felt chastised by the public for being too quick to judge and medicate children, and of promoting their own, selfish motives at the expense of children’s wellbeing. Orit said: “The common perception. . . is that. . . teachers are quick to say that a child has it [ADHD]. . .. That the teacher just wants peace and quiet.” Miriam recalled a parent who told her, “I think the pill is for you.”
While many mothers felt pressured by schools to medicate their children, we also found that teachers were ambivalent about pharmaceutical treatment. Their responses ranged from great relief—“It works wonders” (Aviya)—to disappointment with medications that cause unbearable side-effects or failed to help: “Sometimes it’s hard, it’s not the same child, he loses his joyfulness. . . You want a child. A child who plays, who is active. . . It was very hard for me. [. . .] Your heart breaks. . .” (Yarden).
Roni explained that the idea that teachers push parents to diagnose and medicate children was often tied to accusations of incompetence: “They [parents] don’t want to label the child. . . so they say, ‘What do you mean, ADHD? It’s because you don’t know how to handle him in your classroom.’” Other teachers complained that parents “expect the teacher to do everything” (Irit) and place unrealistic demands on teachers to manage children’s inattention and impulsive behavior.
The interviews with teachers and mothers in our study revealed that children’s diagnosis with ADHD does not relieve them of blame for the child’s dysfunction, as expected in earlier sociological works on the medicalization of ADHD (Conrad and Schneider, 1992; Lakoff, 2000). Although the understanding of ADHD as a neurodevelopmental disorder is highly prevalent in the medical field, it has limited narrative and moral power within school and family arenas. The framing of ADHD as a brain disorder does not free mothers and teachers from responsibility for children’s emotional well-being and functioning. Moreover, our findings on the patchy moral and interpretive effects of the ADHD label are surprisingly similar for teachers and mothers, whose social roles are usually framed as opposed and even adversarial (Frigerio et al., 2013; Malacrida, 2003; Rafalovich, 2004). Both mothers and teachers express ongoing uncertainty about the source of children’s difficulties, are ambivalent about the appropriateness of pharmaceutical treatment, and express unrealistic expectations to control children’s challenging behaviors and experiences.
Institutional effects of ADHD, and responses of mothers and teachers
Our interviewees carried out various strategies and practices in light of the institutional weakness of the ADHD label. Mothers found that diagnosing their child brought surprisingly little material benefit at school, as parents were expected to provide necessary tutoring and therapies privately: “I didn’t get any help this way or that. . . They said, ‘there are children worse off than her’” (Lotem); “The school says. . . ‘it’s your problem, you deal with it’” (Nelly).
In this context, mothers actively sought to employ comorbid diagnoses to maximize their child’s academic and emotional resources at school. ADHD is characterized by “extraordinarily high levels” of comorbidity with other psychiatric conditions (Hinshaw, 2018: 1.10), including learning disabilities, anxiety and mood disorders. This was reflected in our sample: most mothers said their children had been diagnosed or treated for at least one other condition besides ADHD, and some with two or more, most commonly anxiety and learning disabilities. These comorbid diagnoses had an array of institutional and narrative consequences in mothers’ accounts (Fried and Plotkin-Amrami, 2023).
In the Israeli education system, anxiety disorders are classified as a “mental illness,” which is considered an “uncommon” and severe SEN that is grounds for significant resources, including a personal aide. Mothers rejected the implication that their children suffered from “mental illness,” but they embraced the pragmatic significance of the anxiety diagnosis, as a disability whose severity is recognized and that qualifies a child with significant and personalized support at school: We saw that the [ADHD] diagnosis does not qualify [my son] for an aide, but the child clearly needs an aide. He needs something. So we looked at [the codes]. . . Like, she [the psychiatrist] was actually looking at the book of diagnoses. . . ‘Okay then, I’ll write that one. . . anxiety disorder not otherwise specified.’ We got the aide. (Vera)
Mothers also found that schools’ response to children with learning disabilities was much more favorable, compared to ADHD: “He gets one-on-one tutoring. . . The school is really trying” (Lisa). To summarize, for mothers, ADHD diagnosis does not translate into concrete forms of social capital or significant material support.
The limited institutional effect of ADHD was also evident in interviews with teachers. Similar to mothers, teaching staff said the school system provided little response to children with ADHD: “Besides extra time [on exams], ADHD doesn’t get you anything” (Shlomit). In addition, teachers lamented their lack of relevant training, and said that implementing adaptive teaching methods—such as allowing children to leave their seats during class time, or having them sit close to the blackboard—was often unrealistic: “It sounds easy, but if you have a class of 25 children. and 8 have ADHD. . . It’s very hard” (Meital).
In this context, teachers developed various pragmatic and intuitive means of managing children’s everyday struggles and expressed a moral obligation of educational inclusion: “not to give up on any child” (Carmel), and to cope “with a pill or without it” (Ella). For example, Miriam said, “I have to ‘read’ the child. . . How did he wake up today?. . . Do I have the right to make demands of him. . . or not?” The commitment to including children with ADHD may reflect teachers’ uncertainty about the ADHD category; as expressed in the above quotes, they do not see a bright line distinguishing issues associated with an ADHD diagnosis from children’s everyday problems with attention and behavior. Thus, the diagnosis in itself is not grounds for differential treatment: “The point isn’t to. . . give in to them because of the difficulty. . . One has to learn to cope” (Aviya). Moreover, the ethic of universal inclusion is consonant with the rhetoric of recent changes to Israeli educational policy, which frames teachers as primarily responsible to carry out inclusive education practices. In the interviews, we indeed saw that teachers extensively used the term “inclusion” as a moral imperative, expressed in their commitment not to leave children behind. The imperative to “include” children was translated by teachers into semi-therapeutic practices of “containment” of troubled children. Topaz spoke of inclusion/containment in terms of “giving space to the emotional side” and “loving” the child; “I think it is very important to a child with ADHD to feel secure, and that they belong.” Aviya said she aimed “to really, truly include them.. . . I always remind myself, ‘What if they were your own children?’ . . . [I tell] myself [. . .] ‘Take a step back. . .. Breathe. Don’t lash out.’”
The teachers we interviewed felt obligated to make efforts to accommodate struggling children in the classroom and developed various emotional and pedagogical tools to do so (Plotkin-Amrami et al., 2024). Irit said she gave one-on-one tutoring sessions in her private time because “it’s worth it for me. . . I win the child back for another ten classroom periods”; Esti discussed some practices that she acquired over the years: “Small study groups. . . pairing him with a friend. . . giving them less open questions. . . Assigning tasks. . . [in smaller] “doses” because I don’t want him to suffer.”
As these quotes illustrate, the formal medical diagnosis of ADHD did not free teachers from a sense of responsibility for children’s successful functioning in the classroom. While diagnosis ostensibly points to an etiology of difference that is beyond the teacher’s control, the current educational policy of inclusion and teachers’ experiences reflect a sense of greater, rather than lesser, responsibility for the well-being and achievements of diagnosed children.
Discussion
Past research on childhood ADHD has found that parents/mothers generally distinguish between the pragmatic and the interpretive significance of a formal diagnosis, seeking to minimize blame and stigma while maximizing accommodations and empathy for their child (Blum, 2015; Frigerio et al., 2013; Malacrida, 2003; Singh, 2004; Versteeg and Te Molder, 2018). Our findings show that despite the growing acceptance of ADHD as a medical diagnosis and its formal recognition in education policy and school settings, it did not exhibit much narrative, institutional, or moral power for either mothers or teachers. For mothers, the diagnosis is perceived as a narrow problem of attention and does not fully explain children’s emotional and social difficulties. The diagnosis does not bring clarity about the child’s condition, and does not translate into significant material support and educational adjustments for child. Nor does it release mothers from blame or responsibility for the child’s difficulties; neglectful parenting persists as a fundamental explanation for children’s troubles at school, even if in a more diffused form (Blum, 2015; Singh, 2004).
Like mothers, teachers also take part in, and are on the receiving end of, “blame games.” Teachers feel that they are accused of pushing diagnosis and medication against children’s best interests, yet once children are formally diagnosed, teachers continue to be accused of incompetence by parents (“They say. . . ‘you don’t know how to handle him’”). Nor does diagnosis provide teachers with certainty about the source of children’s problems. Teachers hold competing explanations for children’s difficulties and are skeptical when interpreting the difficulties of the particular children they teach.
While previous research has pointed to the increasing role of schools, and particularly teachers, in medicalizing childhood troubles (Hjorne and Saljo, 2004; Wienen et al., 2019), we found that schools are a site of ambivalence and even skepticism about ADHD diagnosis, as well as criticisms of overdiagnosis (“we rush to label it”) and disappointment with the effects of pharmaceutical treatment (“You want a child,” not a “zombie”). Institutionally, teachers describe ADHD as a category that “doesn’t get you anything.” Thus, they develop pedagogical tools to cope with struggling children, against a backdrop of a growing imperative of inclusion in educational policy and discourses of children’s disability rights.
Our findings resonate with previous scholars’ arguments that medical discourses of ADHD are used in selective and hybrid ways by scientists, clinicals, and laypeople, in relation to local norms, social roles, and pragmatic concerns (Bröer and Heerings, 2013; Pickersgill, 2013; Singh, 2011). The limited moral, narrative and institutional effects of ADHD may result from the fact that ADHD is an ambiguous signifier of disability: it is invisible, it does not provide a strong causal explanation for children’s difficulties, and is almost completely normalized (in the sense of non-pathologized) condition, or in Blum’s words, a precarious normality (Blum, 2015). They can also be explained in relation to cultural meanings of ADHD-associated difficulties. As scholars of ADHD have noted, notion of personal responsibility and self-control are central Western values that structure fundamental assumptions about individual personhood and moral accountability (Carpenter-Song, 2009; Lakoff, 2000). As our findings show, ADHD was framed narrowly by teachers and especially mothers as a disorder that explains children’s difficulties with attention; emotional and behavioral difficulties are not contained by the medical label. Fault is displaced onto proximal adults—both teachers and mothers—who are expected to control children’s functioning in the pre-adolescent years. They are not only involved in “blame games” but feel a personal responsibility for the child’s functioning and unrealistic expectations to control it. While teachers and mothers share similar moral positions, mothers’ sense of personal responsibility for a child’s troubles is profoundly shaped by a cultural narrative of mother-blame, leaving mothers to experience embarrassment and shame in various social situations.
Bröer and Heerings (2013: 50) have argued that the dominance of medical discourses of ADHD can be evaluated by examining the extent that “knowledge is institutionalised through law, practice, policy or organization.” The limited institutional effects of ADHD in our case show a gap between the domains of policy and everyday practice, raising questions about the pragmatic value of medical categories. In a recent paper, Brown and Tavory (2024) asked if we can better understand medical phenomena through what people do rather than established definitions. They suggest “forgoing questions of what disease ‘really is’ in favor of understanding it according to how it is enacted,” allowing to “understand it beyond its textbook description and instead see its many—and sometimes contradictory—faces” (Brown and Tavory, 2024: 2). In our case, observing the real-world practices of mothers and teachers shows that ADHD is enacted in school and family arenas in accordance with its institutional status (Fish, 2019), accepted educational policy, and the interpretive possibilities open to our informants. Mothers and teachers make practical use of the diagnostic category in various ways, maneuvering between top-down policy imperatives and different actors’ expectations and interests. Mothers seek material resources and social capital at school by deploying supplementary diagnoses to ADHD, and teachers develop pedagogical practices and understandings that bridge the “perceived gap in care” (Bergey, 2024: 13). Our attention to the institutional dimension of medicalization highlights that this “gap in care” brings both teachers and mothers into heightened moral self-scrutiny. Both teachers and mothers encounter the expectations of moral control over a child’s dysfunction. These cultural expectations might explain why mothers and teachers adopt ambivalent positions to medicalization that resonate with Bergey’s (2024) concept of “liminal medicalization,” reflected in their only partial acceptance of ADHD as a medical label.
The analysis of institutional and moral-interpersonal dimensions of medicalization reveals that the assumptions, moral positioning, and practices of various social actors in the field may be contradictory, but they constantly interact and influence each other. To grasp their simultaneous occurrence, we need to examine medicalization as a dynamic, multi-agent, and multi-sited tendency—a fluid point of departure, rather than one of discursive and categorical closure. Such theoretical understandings should inform practices that support the rights and wellbeing of children, who are at the center of medicalizing processes.
Footnotes
Acknowledgements
We wish to thank Tal Tzadok and Yam Umansky for their assistance with the interviews and the teachers and mothers who were interviewed for their participation in the study.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was supported by the Israeli Science Foundation (ISF). Grant number 1434/20. PI: Galia Plotkin-Amrami
Ethical approval
The study was approved by Ben Gurion University Institutional Review Board (IRB). Interviewees provided informed consent.
Availability of data
The data supporting this study’s findings are available on request from the corresponding author. However, due to privacy or ethical restrictions, the data are not publicly available.
