Abstract
Living with a chronic illness or condition that impacts physical functioning, appearance, or both, may have unique implications for positive body image (PBI), which research suggests is associated with higher quality of life, and thus an outcome of interest in this population. Therefore, the present study systematically reviewed and synthesized the current data on PBI among people with chronic conditions or illnesses (PwCC/I). A total of 36 articles were included. Facets of PBI in this population include illness-related factors, positive social support, caring for the body and symptom management, rejection of sociocultural appearance ideals, illness acceptance, meaning making, broader conceptualization of beauty and functionality, having a multidimensional view of body image, self-compassion, positive mood and outlook, and assimilation. Additional work is needed to develop models that capture sociocultural influences of PBI among PwCC/I, as well as specifically tailored assessments and interventions.
Introduction
According to the CDC, chronic illnesses are conditions that last 1 year or more and require ongoing medical attention, limit activities of daily living, or both (Center for Disease Control and Prevention, n.d). Chronic illnesses and conditions are prevalent, affecting up to one in three adults globally (Hajat and Stein, 2018), and often negatively impact body image (Byrne et al., 2023; Levenig et al., 2019; Özbay et al., 2025). The current body of literature primarily explores negative body image among people with chronic conditions or illnesses (PwCC/I; Pinquart, 2013; Trindade et al., 2018). Although positive body image (PBI), a relatively newer construct, has gained traction in the broader body image literature (Tylka, 2012), research on this topic within populations with chronic illnesses remains limited. Despite emerging interest in this area, no systematic review has yet examined factors associated with PBI in the context of chronic illness. Therefore, the present study sought to systematically review the literature on PBI and chronic illness.
Given that PwCC/I may be at greater risk for negative body image, cultivating PBI may be more challenging for this population. PBI is conceptually distinct from negative body image and reflects an overarching love and respect for the body (Wood-Barcalow et al., 2010). It is characterized by body appreciation, body acceptance and love, a broad conceptualization of beauty, inner positivity, and the ability to filter information in a body-protective manner (Wood-Barcalow et al., 2010). There may be unique nuances to the development and maintenance of PBI among individuals whose chronic conditions affect appearance, physical functioning, or both. Applying the PBI tenets to individuals with congenital visible differences and other stigmatized conditions, Tiggemann (2015) suggested that PBI may be fostered by minimizing the centrality of the visible difference in their lives. However, this may be difficult in Western societies that idealize appearances unmarked by chronic illness. Moreover, PBI may be harder to cultivate for individuals experiencing illness-induced physical limitations.
A core aspect of PBI is functionality appreciation, which involves valuing the body’s capabilities across physical, sensory, creative, communication, and self-care domains (Alleva and Tylka, 2021). Franzoi (1995) conceptualized body functionality as “body-as-process,” which he argued fosters more positive attitudes toward the body compared to the esthetic-focused “body-as-object” attitude. However, prioritizing body functionality may be unhelpful for individuals whose illnesses impair physical functioning, particularly for body appraisal (Alleva and Tylka, 2021). For example, one systematic review suggested that women with cancer-related lymphedema who reported stronger body integrity beliefs and functional and sensory changes reported greater body image concerns (Byrne et al., 2023). Consequently, it may be more helpful to adopt a holistic definition of body functionality that acknowledges both capabilities and limitations (Alleva and Tylka, 2021) and avoids reinforcing idealized notions of physical functioning (Sündermann et al., 2020) among PwCC/I. Accordingly, characteristics of PBI, such as functionality appreciation, may still be promoted for those with chronic illnesses or conditions, especially if framed to resonate with their unique experiences.
Outcomes of PBI include improved physical and mental well-being through self-care engagement (Avalos et al., 2005; Tylka, 2012). Therefore, those with chronic illnesses or conditions may particularly benefit from its cultivation. In fact, a qualitative study assessing the characteristics associated with PBI development among individuals whose bodies deviated from social norms suggested that the subgroup with medical conditions engaged in more self-care practices through shifting their life priorities away from appearance (Alleva et al., 2023). Additionally, increasing functionality appreciation may be associated with greater awareness and honoring of bodily needs (Avalos and Tylka, 2006), which has been described as promoting increased physical activity and consumption of foods that may aid those with medical conditions (Alleva et al., 2023). Taken together, PBI may increase quality of life for PwCC/I.
Although PBI may contribute to better mental and physical health outcomes for PwCC/I, existing research has primarily focused on the population’s negative body image. Moreover, emerging PBI literature has yielded relatively inconsistent findings across chronic illnesses (Markey et al., 2020; Matusik et al., 2025). To date, no studies have systematically synthesized the literature on PBI in chronic illness. Therefore, the present study aimed to systematically review the literature that measured and discussed positive body image among individuals with chronic conditions or illnesses.
Methods
Ethics and eligibility
As per Northeastern University’s Institutional Review Board’s guidelines, secondary research that analyzes articles with de-identified datasets, such as this review, meets criteria for IRB review exemption. The PRISMA guidelines (Moher et al., 2009) were utilized to conduct this review.
Studies were eligible to be included in this review if the study: (a) was empirical; (b) had a sample that included only individuals with a chronic illness; (c) the study measured positive body image; and (d) the study reported a positive body image outcome. Studies were excluded if they did not meet the inclusion criteria.
Data sources and search strategy
A systematic search was conducted using the following databases: PsycINFO, PubMed, and ScienceDirect. The following search string was used to screen for articles within each database: (“Positive body image” OR “self-image” OR “body perception” OR “appearance satisfaction” OR “body positive” OR “body confidence” OR “body acceptance” OR “body appreciation” OR “functionality appreciation” OR “positive embodiment”) AND (“chronic illness” OR “chronic disease” OR “chronic conditions” OR “chronic disorder” OR “chronic health problem” OR “disability”). Fifteen studies were manually searched and screened. All articles were imported into and screened using Covidence, a web-based software platform.
Study selection and quality
Articles were first screened by title and abstract, followed by full-text screening. The following data were extracted from each article: year, country, study design, sample size, gender, mean age and standard deviation, chronic illness or condition, positive body image measure, and factors associated with positive body image. An adapted 12-item version of the Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies (National Heart, Lung, and Blood Institute, n.d.) was used to conduct the quality assessment for all studies. All criteria were scored as either “yes” or “no.” The maximum study quality score was 12 if all criteria were coded as “yes.” Data were synthesized according to the identified factors associated with positive body image within each study.
Results
Study and sample characteristics
The literature searches yielded 1428 articles. After removing 257 duplicates, 1170 studies were selected for title and abstract screening, and 64 articles were selected for full-text screening. Ultimately, the authors identified 36 articles (32 peer-reviewed, 4 dissertations) that assessed PBI among our selected sample (See flow diagram in Figure 1). Study designs included 32 cross-sectional studies, 3 longitudinal studies, and 1 randomized control trial. Data collection method designs were comprised of 15 qualitative, 18 quantitative, 2 mixed methods, and 1 quasi-experimental. See Table 1 in Supplemental Materials for all extracted data. The study quality assessment scores ranged from 6 to 12 and were overall of fair to good quality. Sample sizes ranged from n = 4 to n = 1239, and mean participant ages ranged from 10 to 67.9. Samples were primarily female, with four studies including less than 50% female participants.
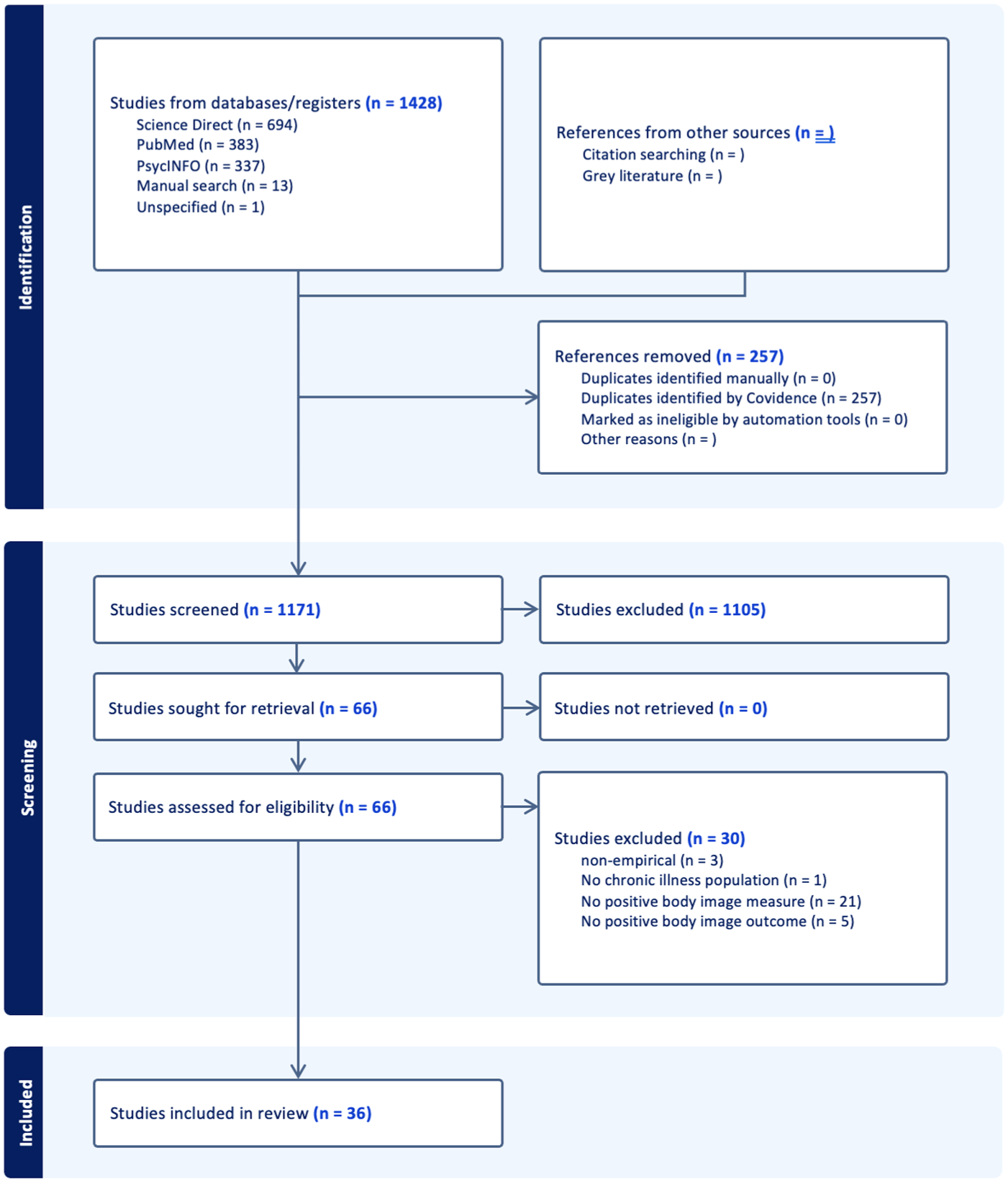
Study selection process.
Illness-related factors
Illness-related factors, such as onset and severity, were associated with PBI in 15 studies. Both quantitative and qualitative evidence suggested that a greater number of years post-illness onset was associated with PBI (Bassett et al., 2009; Sengul et al., 2019; Taleporos and McCabe, 2002; Watson, 1988). Similarly, an inverse relationship was found between illness severity and PBI, with lower illness severity correlating with greater PBI. For example, low sexual distress (Price and Brunet, 2024), fewer appearance-related effects (Feragen and Borge, 2010; Lawrence et al., 2006), lower symptom intensity (Argyrides et al., 2023; Matusik et al., 2025; Sengul et al., 2019), and increased global health and functional status (Boman et al., 2013) were associated with greater PBI. Taken together, an earlier illness onset, along with symptoms that have minimal to no impact on appearance and functioning, are associated with greater PBI among PwCC/I.
Sociodemographic factors appeared to influence the relationship between illness characteristics and PBI. Across several studies, males with chronic illnesses generally reported more PBI than females (Boman et al., 2013; Feragen and Borge, 2010; Kaminsky and Dewey, 2013; Lawrence et al., 2006). Findings on age were mixed. Some studies suggested that older adults, particularly individuals with gynecologic or breast cancer, polycystic ovarian syndrome, and chronic pain reported greater PBI than their younger counterparts (Brunet et al., 2022; Markey et al., 2020; Price and Brunet, 2024; Soucie et al., 2021; Thornton and Lewis-Smith, 2023). In contrast, other studies reported higher PBI among younger individuals with chronic illnesses compared with their older counterparts, including those with multiple sclerosis, adult survivors of central nervous system cancer, children with a cleft lip, and general physical disabilities (Argyrides et al., 2023; Boman et al., 2013; Feragen and Borge, 2010; Matusik et al., 2025).
Positive social support
Positive social support was identified as a facet of PBI in 12 studies. Qualitative evidence suggested that external appearance validation, independent of having a close personal relationship with the person providing feedback, was associated with a greater PBI within this population (Pope et al., 2007; Price and Brunet, 2024; Wade, 2007). Additionally, both quantitative and qualitative evidence suggested that positive social reactions promoting the inclusion of PwCC/I were associated with greater PBI (Argyrides et al., 2023; Bailey et al., 2015; Brunet et al., 2022; Price and Brunet, 2024; Taleporos and McCabe, 2002; Watson, 1988), regardless of the illness’s impact on appearance (Feragen and Borge, 2010). Therefore, positive social reactions to PwCC/I may facilitate PBI. Moreover, providing consistent and positive support during periods of body-related distress in the community was associated with more positive feelings toward one’s body (Bailey et al., 2015; Price and Brunet, 2024), especially if the support was received earlier in life (Watson, 1988).
Six studies explored the mechanisms through which social support may increase PBI in PwCC/I. Four qualitative studies highlighted the role of social support from close relationships or loved ones in fostering PBI for these individuals through acceptance, compassion, and positive body image role-modeling (Bailey et al., 2015; Brunet et al., 2022; Price and Brunet, 2024). Two studies examined the role of receiving care from others on PBI. Quantitative evidence suggested that higher perceived authoritative figure control over health for adolescents with Type 1 diabetes facilitated PBI (Kaminsky and Dewey, 2013), which was supported in qualitative evidence suggesting that increased support from others with illness management may increase PBI among breast cancer survivors (Thornton and Lewis-Smith, 2023). Lastly, moderate to high levels of perceived social support may also enhance the efficacy of avoidance- and problem-focused coping strategies for increasing PBI (Almeida et al., 2025). Taken together, the literature consistently supports the role of positive social support in fostering PBI for PwCC/I independent of the provider, type, or timing of the support.
Caring for the body and symptom management
Caring for the body and symptom management was identified as a facet of PBI in 10 studies. Six studies suggested that taking care of the body, particularly when it resulted in symptom reduction, was associated with greater PBI. For example, two qualitative studies found tending to bodily needs through self-care was associated with greater PBI when it resulted in functional improvements (Bailey et al., 2015; Thornton and Lewis-Smith, 2023). Specific symptom improvements, such as pain reduction, were found to be associated with greater PBI over others according to both quantitative and qualitative evidence (Bailey et al., 2015; Markey et al., 2020; Thomas et al., 2019; Volker and Mills, 2022). In addition, one qualitative study found that recognizing the body for surviving hardship, such as being in remission from cancer, may increase gratitude for the body, suggesting that appreciating functional improvement may facilitate PBI (Thornton and Lewis-Smith, 2023).
Symptom management was associated with PBI when physical functionality was prioritized over appearance and weight. Three qualitative studies suggested that regaining function by promoting health goals over appearance goals (Brunet et al., 2022; Thornton and Lewis-Smith, 2023) and utilizing weight-neutral treatment methods (Soucie et al., 2021) were associated with greater PBI among PwCC/I. Independence through symptom management was also associated with PBI within the population. One qualitative study indicated that, among individuals with a spinal cord injury, being attentive and caring for the body for symptoms management may increase one’s sense of independence and PBI (Bailey et al., 2015). Qualitative research also suggested that adaptive clothing, excluding mobility aids, may promote a sense of independence, which may therefore enhance PBI among PwCC/I (Thomas, 2019; Thomas et al., 2019).
According to the literature, exercise may improve physical functioning which was associated with PBI among individuals whose chronic illness or condition symptoms impacted their ability to be active. For example, both quantitative and qualitative evidence suggested that physical activity appropriate for an individual’s current physical status was associated with greater PBI in an adult chronic illness population, provided that weight loss was not the goal (Brunet et al., 2022; Price and Brunet, 2024). The association between increased physical activity and greater PBI also extended to children with chronic conditions (Greguol et al., 2014). Furthermore, qualitative evidence among a sample of women treated for non-metastatic breast cancer suggested that accepting and accommodating functional limitations during activity may support PBI (Price and Brunet, 2024). Taken together, taking care of and listening to one’s body as a means of self-care and improving illness-related symptoms may promote PBI among individuals whose physical functioning is impacted by their chronic illness or condition.
Rejection of sociocultural appearance ideals
Rejection of sociocultural appearance ideals was identified as a facet of PBI in six studies. Overall, qualitative findings suggested that rejecting mainstream body ideals and embracing the natural body were associated with greater PBI among PwCC/I (Bailey and Gammage, 2020; Brunet et al., 2022; Grogan and Mechan, 2017). Specifically, two qualitative studies found that increased media literacy and using protective filtering to reject sociocultural appearance ideals and recognize beauty in all body types was associated with greater PBI within the population (Bailey et al., 2015, 2021; Thornton and Lewis-Smith, 2023). Taken together, rejection of sociocultural appearance ideals, especially via increased media literacy, was associated with increased PBI among PwCC/I.
Illness acceptance
Illness acceptance was identified as a facet of PBI in nine studies. Qualitative findings from Grogan et al. (2019) revealed that women who were treated for cancer generally accepted their outward bodies (appearance). Both quantitative and qualitative evidence suggested that accepting perceived negative, illness-related body features was associated with a more positive body image among individuals with chronic illnesses (Bailey and Gammage, 2020), regardless of illness severity (Matusik et al., 2025). Qualitative findings also suggested that illness acceptance may be more likely to occur over time and therefore facilitates PBI with increasing age (Brunet et al., 2022; Grogan and Mechan, 2017; Price and Brunet, 2024; Taleporos and McCabe, 2002; Watson, 1988). Conversely, one study found that increased illness acceptance in individuals with multiple sclerosis was associated with both lower age and positive attitudes toward the body (Matusik et al., 2025). Additionally, qualitative evidence suggested that accepting illness-related limitations, whether through mindful activities like yoga or through religion and spirituality, may help PwCC/I engage positively with their bodies (Bailey et al., 2015; Price and Brunet, 2024). Regardless of the pathway through which acceptance was achieved, it was consistently associated with a more positive body image.
Meaning making
Engaging in meaning making was consistently linked to greater PBI in seven studies. Qualitative evidence suggested that reframing illness appearance effects, such as scars, as evidence of the body’s resilience, may assist with increasing pride for the body (Grogan et al., 2019; Grogan and Mechan, 2017). Additionally, meaningfully engaging with life (i.e. through hobbies, career, education) was associated with greater PBI (Taleporos and McCabe, 2002). Meaningfully engaging with life prior to illness onset may also be associated with PBI, especially if the individual feels satisfied with how they utilized their functional capabilities (Thornton and Lewis-Smith, 2023). Lastly, meaning making through religion and spirituality was also associated with an increase in PBI (Bailey et al., 2015; Brunet et al., 2022; Thomas et al., 2019). Overall, finding meaning and purpose in one’s body and overall life was consistently associated with positive body image among the population.
Broader conceptualization of beauty and functionality
Broader conceptualization of beauty and functionality was identified as a facet of PBI in three qualitative studies. A more holistic understanding of body image was more associated with PBI in this population. Specifically, expanding the definition of body image to encompass meaningful functions and capabilities, rather than focusing solely on appearance, was associated with greater PBI (Alleva et al., 2018; Bailey and Gammage, 2020). These findings extend to exposure to body positive social media content, with one experimental study suggesting that brief exposure to chronic illness-inclusive body positive social media content may increase state broad conceptualization of beauty (Longhurst et al., 2024).
Having a multidimensional view of body image
Having a multidimensional view of body image was identified as a facet of PBI in four qualitative studies. Qualitative evidence suggested that viewing the body image as multidimensional, encompassing physical function and health rather than appearance-only, was associated with higher PBI (Bailey et al., 2015; Thomas, 2019; Thomas et al., 2019), Participants with physical disabilities reported greater functionality appreciation after receiving a PBI intervention that included psychoeducation on this expansive definition of body image (Bailey and Gammage, 2020). Therefore, acknowledging that body image is dynamic and multi-faceted may facilitate positive body image for PwCC/I.
Self-compassion
Self-compassion was identified as a facet of PBI in four studies. Overall, evidence suggested that increased self-compassion was associated with greater PBI in this population (Bailey and Gammage, 2020; Brunet et al., 2022; MaGee and Gammage, 2025; Thornton and Lewis-Smith, 2023). One qualitative study suggested that greater self-compassion may be achieved through downward comparisons to individuals “worse off” (Brunet et al., 2022) or through receiving care (Thornton and Lewis-Smith, 2023), which may enhance PBI.
Positive mood and outlook
Positive mood and outlook was identified as a facet of PBI in four studies. Both qualitative and quantitative evidence suggested that greater positive mood and positive life outlook among PwCC/I can either be directly associated with greater PBI (Brunet et al., 2022; Hajj-Moussa et al., 2024; Thomas et al., 2019) or indirectly associated with greater PBI via improved social relationships (Price and Brunet, 2024). Therefore, achieving a positive mood or life outlook may serve as an avenue for PwCC/I to engage in positive body image behaviors.
Assimilation
Assimilation was identified as a related factor of PBI in 12 studies. A greater PBI was associated with factors that resulted in minimal or no appearance-related side effects. For instance, treatment modalities such as surgery alone for individuals with scoliosis and chemotherapy with minimal esthetic impact for individuals with cancer were associated with greater PBI (Wade, 2007; Wu and Chin, 2003). Among those who experienced illness-related appearance effects, findings were mixed regarding the association between concealing these effects and PBI. For example, two qualitative studies suggested that individuals who successfully concealed illness-related appearance changes through clothing reported a higher PBI (Thomas, 2019; Thomas et al., 2019). Conversely, two additional studies suggested that concealing illness-related appearance changes through clothing in women treated for cancer were associated with negative perceptions of their natural bodies (Grogan et al., 2019; Grogan and Mechan, 2017). Similar findings were observed in three qualitative studies, which suggested that concealing functionality impairments in day-to-day life, or “appearing capable,” when engaging in day-to-day activities was associated with greater PBI in samples of PwCC/I (Thomas, 2019; Thomas et al., 2019; Watson, 1988). Finally, both quantitative and qualitative data suggested that greater PBI may be more prevalent among individuals who concurrently have a chronic illness or condition and meet sociocultural appearance ideals, such as having a lower BMI, smaller waist circumference, and lower body fat percentage (Bassett et al., 2009; Greguol et al., 2014; Markey et al., 2020). This was further confirmed by evidence suggesting that individuals reported greater body and functionality appreciation for aspects of their bodies least impacted by symptoms (Taleporos and McCabe, 2002; Thomas, 2019; Thomas et al., 2019), which may be facilitated through downward comparisons to individuals with more severe chronic illness impacts on their function and appearance (Price and Brunet, 2024).
Outcomes of positive body image
Eight studies examined PBI as an outcome variable for PwCC/I. Overall, both qualitative and quantitative evidence suggested that increased PBI may be associated with quality of life outcomes for the population. Specifically, increased PBI was associated with dimensions of psychological well-being outcomes, such as higher optimism, lower pessimism, and greater self-esteem, better emotional and cognitive function, increased perception of a meaningful life, and increased psychological flexibility (Ettridge et al., 2022; Hajj-Moussa et al., 2024; Policardo et al., 2025; Teixeira, 2022; Wade, 2007). Increased PBI was also associated with dimensions of physical quality of life outcomes, such as higher perceived reporting of physical well-being and increased engagement in intuitive eating (Bailey and Gammage, 2020; Teixeira, 2022). Quantitative evidence suggested that positive body image, specifically appearance acceptance, was associated with an enhanced ability to accept one’s illness or condition (Matusik et al., 2025; Teixeira, 2022) and situational body dysphoria (body dissatisfaction triggered by specific contexts) reduction (Argyrides et al., 2023). Lastly, evidence among PwCC/I suggested that greater knowledge and experience with having a more positive body image may increase the likelihood that those individuals will become advocates for positive body image (Bailey and Gammage, 2020).
Discussion
The aim of this systematic review was to summarize the literature on (PBI) among samples of people with chronic conditions or illnesses (PwCC/I). The review findings identified 11 themes, including illness-related factors, positive social support, caring for the body and symptom management, rejection of sociocultural appearance ideals, illness acceptance, meaning making, broader conceptualization of beauty and functionality, having a multidimensional view of body image, self-compassion, positive mood and outlook, and assimilation. Additionally, increased PBI was found to be a predictor of physical and psychological quality of life outcomes, such as higher optimism, lower pessimism, greater self-esteem, better emotional and cognitive function, increased perception of a meaningful life, increased psychological flexibility, higher perceived reporting of physical well-being, and increased engagement in intuitive eating (Bailey and Gammage, 2020; Ettridge et al., 2022; Hajj-Moussa et al., 2024; Policardo et al., 2025; Teixeira, 2022; Wade, 2007). Illness acceptance, reduced situational body dysphoria, and becoming an advocate for positive body image also emerged as outcomes of increased PBI (Argyrides et al., 2023; Bailey and Gammage, 2020; Matusik et al., 2025; Teixeira, 2022). Generally, these findings aligned with those originally developed in the literature among non-disabled populations (Wood-Barcalow et al., 2010). A unique facet of PBI identified in this review was assimilation, whereby individuals with chronic illnesses reported greater PBI when their appearance and functional status more closely resembled those of non-disabled populations (Thomas, 2019; Thomas et al., 2019). The facets associated with PBI were fairly consistent with current evidence, although there were some differences in PBI expression among chronically ill populations.
This review identified consistent chronic illness-specific facets of positive body image: illness acceptance, caring for the body and symptom management, illness-related factors, and meaning making. Illness acceptance’s association with PBI (Bailey and Gammage, 2020; Price and Brunet, 2024) may be explained by its ability to counteract illness-related shame associated with body dissatisfaction (Trindade et al., 2018). Illness acceptance may also enhance quality of life and reduce symptom intensity, as reported by women with breast cancer (Jankowska-Polańska et al., 2020), which may, in part, explain illness acceptance’s relation to higher PBI. Caring for the body and symptom management were also associated with greater PBI. This finding extends the literature on honoring bodily needs and its association with greater body appreciation in college women (Avalos and Tylka, 2006; Wood-Barcalow et al., 2010), which may be relevant for individuals experiencing illness since it may reduce appearance-related values (Alleva et al., 2023). As for symptom management, pain reduction was consistently associated with greater PBI (Bailey et al., 2015; Markey et al., 2020; Vinoski Thomas et al., 2019; Volker and Mills, 2022). Symptoms that heighten interoceptive awareness, such as pain, may unintentionally draw more attention to the body in a likely unpleasant way. When symptom intensity is difficult to manage, individuals may begin to appraise their bodies negatively, thus shifting focus to aspects they can control such as their appearance, a pattern similarly theorized by Sündermann et al. (2020) in their cognitive behavioral model of body image and chronic pain. However, engaging with the body in adaptive or non-appearance-focused ways rooted in acceptance and self-care to accommodate physical limitations (Brunet et al., 2022; Price and Brunet, 2024), such as in exercise (Greguol et al., 2014) or using adaptive clothing (Thomas et al., 2019), may draw positive attention to the body or increase perceived control over one’s body, fostering a sense of independence. Alternatively, making meaning out of one’s experience, whether through reframing negative thoughts about illness-related appearance and physical effects or through religion and spirituality, may enhance one’s ability to accept and cope with living with a chronic illness or condition, thereby fostering greater comfort in the body. However, focusing solely on matching the physical capabilities of those who do not have chronic illness may increase ableist stigma (Thomas, 2019), which could in turn have implications for body image. Therefore, accepting every function, rather than attempting to reduce symptoms or ignore their presence, may enhance PBI. Taken together, accepting illness, caring for the body, and making meaning out of the illness experience may promote PBI for PwCC/I.
Certain illness-related factors, such as longer time post-illness onset and lower illness severity, were consistently associated with PBI. The buffering effect of long-term adjustment to the illness or condition may stem from the gradual development of coping strategies and supportive social networks, which may help individuals with chronic illnesses feel more at ease in their bodies and foster key aspects of PBI, such as appreciation and positive mood. Furthermore, while some studies found that older individuals reported greater PBI (Brunet et al., 2022; Markey et al., 2020; Price and Brunet, 2024; Soucie et al., 2021; Thornton and Lewis-Smith, 2023), others found the opposite, with younger individuals reporting greater PBI (Argyrides et al., 2023; Boman et al., 2013; Feragen and Borge, 2010; Matusik et al., 2025; Sengul et al., 2019). Mixed findings on age-related outcomes may be explained by the fact that older adults may experience less pressure to conform to youthful beauty ideals (Alleva et al., 2023; Tiggemann and McCourt, 2013), whereas younger individuals with chronic illnesses reported higher global health and functional statuses, which are associated with greater PBI (Argyrides et al., 2023; Boman et al., 2013). Therefore, younger individuals with less severe illnesses may not require intensive strategies to cope with their illness and are at a greater advantage to foster PBI. Lastly, males with chronic illnesses consistently reported higher PBI than females (Boman et al., 2013; Feragen and Borge, 2010; Kaminsky and Dewey, 2013; Lawrence et al., 2006), reflecting broader gender differences in PBI among chronically ill pediatric and adolescent populations (Pinquart, 2013). Although no research has examined sociocultural influences on PBI, recent studies have suggested males are less likely to have a chronic illness (Boersma et al., 2020) and experience less healthcare-related stigma (Samulowitz et al., 2018). Broader societal messaging about living with a chronic illness as a female may reflect less acceptance and greater stigma (Samulowitz et al., 2018). Therefore, individuals who identify as female, are older, or experience more severe chronic illnesses or conditions may struggle most to maintain PBI and benefit from earlier, targeted efforts to promote PBI and support it.
This review identified additional PBI facets and related factors that are also supported in the broader literature on non-chronically ill populations. These include broader conceptualizations of beauty, having a multidimensional view of body image, self-compassion, rejection of sociocultural ideals, positive mood and outlook, positive social support, increased engagement in intuitive eating, and improved physical and psychological quality of life (Alleva and Tylka, 2021; Avalos et al., 2005; Avalos and Tylka, 2006; Ettridge et al., 2022; Linardon et al., 2023; Policardo et al., 2025; Siegel et al., 2020; Teixeira, 2022; Tylka and Iannantuono, 2016; Wood-Barcalow et al., 2010). Although, several factors of PBI have been supported in the broader literature, some appeared to exhibit illness-specific characteristics among PwCC/I. For example, extending the view of body image as encompassing factors beyond appearance to include functionality may increase attention toward how one feels, thereby increasing self-care behaviors. Regarding positive social support, women with breast cancer reported that receiving physical care during recovery provided them with more time to heal and appreciate their bodies (Thornton and Lewis-Smith, 2023), which may also be explained through symptom reduction’s positive effect on body image (Thomas et al., 2019). Additionally, PwCC/I receiving positive social support may feel more accepted despite mainstream appearance and functional ideals, which may enhance overall positive feelings toward their bodies.
Of note, individuals whose appearances aligned more closely with sociocultural ideals, such as having minimal illness-related appearance changes, lower BMI, or smaller waist circumference, reported higher PBI. This suggests that there is a desire to adopt non-chronically ill appearance norms to assimilate, potentially to avoid being recognized as chronically ill outside of healthcare settings. This may explain why concealing illness-related appearance changes (Grogan et al., 2019; Grogan and Mechan, 2017) and “appearing capable” (Thomas et al., 2019) were associated with higher PBI. This contradicts literature suggesting that adaptive appearance investment or engaging in appearance-related self-care and grooming in a way that enhances natural features rather than external standards of beauty, is associated with positive body image (Tylka and Wood-Barcalow, 2015). Additionally, although meaning making emerged as a factor associated with greater PBI, it was often facilitated by comparing oneself to individuals with greater illness-related appearance and functional effects (Price and Brunet, 2024). These findings highlight ongoing issues of limited representation and societal acceptance of diverse appearance, functional abilities, and internalized ableism. One study assessing brief exposure to chronic illness-inclusive body positive content suggested it may reduce state negative affect and increase state broader conceptualization of beauty (Longhurst et al., 2024). However, more research on the benefits of and continued advocacy for increased representation of chronic illness beyond the media is needed.
The findings from this systematic review have several important implications for future research and clinical practice. In terms of research, although efforts have been made to assess sociocultural influences of PBI among a disabled population (Longhurst et al., 2024), the findings from this review highlight a need for theoretical models that incorporate said sociocultural influences (i.e. media, societal norms, healthcare stigma), on PBI in chronic illness. Developing and testing such models would provide researchers with a solid framework for future studies and offer clinicians evidence-based foundations for designing interventions that support body image in this population. Additionally, the inconsistency in how PBI is conceptualized and measured within chronically ill populations also signals a need for scales specifically developed for this group and the validation of other existing scales within populations with chronic illnesses. While the Body Appreciation Scale-2 (BAS-2; Tylka and Wood-Barcalow, 2015) is widely used and validated across various genders, age groups, and cultural contexts, it has yet to be validated among individuals with chronic illnesses. Although many PBI outcomes identified in this review align with findings from non-chronically ill populations, several unique patterns also emerged. These unique elements further underscore the importance of using tailored assessments, both in research and clinical settings, to more accurately capture the lived experiences of PwCC/I. Lastly, although few articles assessed PBI as a predictor variable, the cross-sectional study designs of the majority of the referenced studies limit the causal inferences that can be made between increased PBI and its associated outcomes among PwCC/I. PBI was also not assessed as a moderator or mediator within our selected articles. Future studies should strengthen methodological rigor by incorporating such designs to better identify the mechanisms of PBI among PwCC/I, particularly if assessed near the time of diagnosis and continuing over time.
The findings identified in this review have important implications for intervention development, resource creation, and clinical practice. Notably, there is a lack of broad and inclusive interventions aimed at promoting PBI among PwCC/I. Although some studies have examined programs designed for this purpose (Alleva et al., 2018; Bailey and Gammage, 2020; MaGee and Gammage, 2025), these efforts have primarily targeted older adults, with only one study employing a randomized control trial (RCT) design. Future research should prioritize the inclusion of gender-diverse individuals with chronic illnesses when evaluating intervention efficacy, particularly through methodologically rigorous designs such as RCTs. Doing so would increase the applicability and validity of such interventions across a wider range of clinical populations with chronic illness. Additionally, the findings from this review may inform the development of clinician training programs to focus on supporting patients with chronic illnesses or conditions who struggle with body image concerns. Recent evidence suggests that targeting PBI may be more effective than focusing solely on reducing negative body image (Tylka, 2012). Therefore, identifying and strengthening specific components of PBI within PwCC/I conditions may offer clinicians more targeted, affirming, and empowering tools in their therapeutic work.
This review is the first to summarize the literature on PBI among individuals with a diverse chronic illnesses and conditions in both males and females across a wide range of ages. It is important, however, to note the review’s limitations. First the studies in this review did not provide consistent definitions nor measures of PBI. Studies developed prior to the introduction of the PBI construct in research (Watson, 1988; Wu and Chin, 2003) broadly defined what is now coined “positive body image” as being generally satisfied with one’s body. Later models defined PBI as encompassing more specific core features such as functionality appreciation (Thomas, 2019), body appreciation (Matusik et al., 2025), rejecting sociocultural ideals (Thornton and Lewis-Smith, 2023), and having a broader conceptualization of beauty (Longhurst et al., 2024). Additionally, at the time of this review, no research has been conducted on PBI within fully gender expansive or male samples who have chronic illnesses or conditions. There is a specific need for research on PBI among minoritized identities with chronic illnesses or conditions. For example, Morris et al. (2025) reported that living with a disability may significantly limit their engagement in activities for improving body image, such as exercise and gender-affirming care, for non-binary individuals. Similarly, living with a chronic illness and having a higher BMI or being of a lower socioeconomic status may pose an increased threat to body image, which has yet to be explored within the literature.
Conclusion
The findings of this review support and extend existing literature on positive body image (PBI) by highlighting both shared and unique factors among individuals with chronic conditions or illnesses. Specifically, positive actions and feelings toward the body (i.e. meaning making, self-compassion) and illness-specific body-image related factors (i.e. symptom management) may both contribute to fostering PBI in this population. Enhancing positive body image may also increase physical and psychological quality of life, enhance illness acceptance, reduce situational body dysphoria, and foster positive body image advocacy. These results underscore the distinct ways chronic illness may shape body image experiences and behaviors. As such, future research should focus on developing tailored assessments and interventions for PwCC/I and incorporate longitudinal designs to better capture and promote PBI over time.
Supplemental Material
sj-docx-1-hpq-10.1177_13591053261418744 – Supplemental material for Positive body image and chronic illness: A systematic review
Supplemental material, sj-docx-1-hpq-10.1177_13591053261418744 for Positive body image and chronic illness: A systematic review by Isabel M. Cunha, Samantha Nett, Arabella Jarvie and Rachel F. Rodgers in Journal of Health Psychology
Footnotes
Ethical considerations
As per Northeastern University’s Institutional Review Board’s guidelines, secondary research that analyzes articles with de-identified datasets, such as this review, meet criteria for IRB review exemption.
Consent to participate
Consent to participate is not applicable to this review article as no data were collected from participants.
Consent for publication
Consent for publication is not applicable to this review article as no identifiable participant data are included.
Author contributions
I.C. co-developed the research question, screened articles for inclusion, extracted data, performed the quality assessment, and drafted and reviewed the manuscript. S.N. and A.J. screened articles for inclusion and performed a quality assessment. R.R. supervised the review, developed the research question and search strategy, screened articles for inclusion, and reviewed the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Extracted data of included articles in this review are included as a Supplemental Material in Table 1.
Supplemental material
Supplemental material for this article is available online.
