Abstract
This article explores the lived experience of informal caregivers in cancer care, focusing on the perceived burden and needs of individuals seeking support from an informal group for next of kin. A total of 28 individuals who were closely related to a patient with cancer participated in focus group interviews. Three themes were identified: setting aside one’s own needs, assuming the role of project manager, and losing one’s sense of identity. Together they form the framing theme: being co-afflicted. The characteristics of informal caregivers are shown to be similar to those of people with codependency, motivating development of targeted interventions from this perspective.
Background
It is estimated that by 2040 the disease burden from cancer in Europe will increase by 21 percent (from 4.2 to 5.2 million new cases annually) while the annual number of cancer deaths will increase by 31 percent (from 1.9 to 2.6 million) (Siegel et al., 2019). Every cancer diagnosis will also have some effect on the family members and close friends of the patient, for it is estimated that the contributions of informal caregivers account for one-third of the total costs of cancer care (Round et al., 2015). The impact and burden on informal caregivers will grow with the increasing incidence of cancer, the improved prognosis and increased life expectancy of patients, and the increasing reliance on outpatient care services (Goren et al., 2014; Haylock, 2010).
Cancer has been described as a “we-disease” (Kayser et al., 2007) in which informal caregivers are involved in both disease-related and everyday tasks. Informal caregiving can have positive consequences for the caregiver, including a sense of efficacy, of worth and purpose, of emotional closeness, and satisfaction and pleasure in preserving the patient’s dignity (Anderson and White, 2017; LeSeure and Chongkham-Ang, 2015). However, informal caregivers also carry a heavy burden and report stress, loneliness, isolation, a heavy workload, shame and guilt (Goren et al., 2014; Stenberg et al., 2010). The caregiver burden is defined as “the extent to which caregivers perceive that their emotional or physical health, social life and financial status are suffering as a result of caring for their relatives” (Zarit et al., 1986: 261). Informal caregivers have been described as experiencing psychological, social, relational, emotional, and financial burden (Halpern et al., 2017; Wang et al., 2018). Increased levels of distress and anxiety are reported by half of informal caregivers of patients with advanced-stage cancer (Reblin et al., 2016; Rumpold et al., 2016).
The support available to informal caregivers varies across health care organizations and cancer subtypes (Ferrell and Wittenberg, 2017). The general lack of such support in the public health care sector has led to the development of private or charity-based support initiatives. Most of these are however, targeted at optimizing the delivery of patient care by informal caregivers rather than at supporting these caregivers (Rowland et al., 2017; Ugalde et al., 2019). The limited implementation of support initiatives and measures is likely related to a weak evidence basis, difficulties in targeting caregivers’ specific and variable needs, and challenges in identifying a group for targeted intervention (Frambes et al., 2017; Kent et al., 2016). We accordingly set out to investigate the perceived burdens and needs of caregivers by conducting focus group interviews with individuals participating in a non-profit online community for peer-to-peer support. Thematic analysis of the interviews has enabled us to identify important themes for health professionals interacting with informal caregivers.
Aim
To explore the lived experience of informal caregivers in cancer care, focusing on the perceived burden and needs of individuals seeking support from an informal group for next of kin.
Methods
Setting
Swedish health care is strongly person-centered with a focus on shared decision-making based on the patient’s views and preferences (Pirhonen et al., 2017). The support offered to patients’ family members varies, and is mostly provided by primary care providers, local municipal groups, or charities such as churches and patient organizations. An example of such a group is the national non-profit community group known as Cancer buddies (www.cancerkompisar.se), which offers peer-to-peer support through an online forum and by matching informal caregivers who can share their experiences and offer personal, experience-based support (Kent et al., 2016). The community serves adults and young adults and is solely directed at family members and close friends of patients with cancers. It does not include the patients with cancers themselves.
Participants
Selection of participants was based on purposive criterion sampling with two fundamental criteria, having experience of being an informal caregiver in cancer care, and having sought support from a peer-to-peer network. Through the founders of Cancer buddies, the participants were recruited by email invitations and through a website post (in Swedish). To accommodate travels for the participants, groups were formed in three different cities throughout Sweden. Each group had between two and five participants. In total, there were 28 participants, 25 of whom were women while 3 were men. Their average age was 50 years (range: 25–71) and they identified themselves as partners (n = 19), siblings (n = 1), parents (n = 3), children (n = 4), and grandchildren (n = 1) of a person with cancer. Of the participants, 13 were current informal caregivers and 15 were bereaved informal caregivers. No financial compensation was provided, to participants, except to cover travel costs.
Study procedure
Data were collected through seven focus group interviews. Before each focus group began, all the participants gave written informed consent to being part of this study and to our audio-recording the group discussion. The interviews were conducted by research team members who were trained health care professionals and took place in three Swedish cities close to where the participants lived. Of the seven groups, four consisted of bereaved informal caregivers while the other three groups involved current informal caregivers. The interviews began with the participants sharing their story and discussion was initiated by asking “What needs do/did you have as an informal caregiver?” This question was followed by the question, “How are/were those needs being met?” The focus group discussions lasted on average 1.29 hours (range 1.16–1.47 hours). The discussions were digitally audio-recorded, transcribed verbatim by third party professional transcribers and validated by the first author. All focus groups were conducted in Swedish.
Data analysis
With the aim of the study in mind, we chose a thematic analysis (Braun and Clarke, 2006). Thematic analysis relies on depth of engagement to produce quality coding and allows for an organic approach to theme development (Clarke and Braun, 2018). The analyses focused on meanings of the perceived burdens of informal caregivers in cancer care and analyzed the data from all the focus groups as a whole. (1) Initially, research team members read the entire transcripts repeatedly to get a sense of the lived experience of being an informal caregiver in cancer care. (2) Next, the team members coded the transcripts individually, marking meaning units and noting how and where participants made sense of their own experiences. A meaning unit could be a few words, a sentence, or a whole paragraph related to the participants’ personal thought and feelings. (3) The resultant codes were compared, discussed, and developed into themes. (4) In the next step, the themes were reviewed in relation to the full text as well as the coded extracts in order to check their validity. (5) As a final step, we assembled and synthesized the themes to form a comprehensive understanding of the whole as a framing theme developing from and containing the initial three themes. In this article, we present the final themes that emerged from this analysis of the participants’ responses in the focus groups.
The study was performed in accordance with the principles of research ethics (General Assembly of the World Medical Association, 2014; Beauchamp and Childress, 2013), and was approved by the Regional Ethical Review Board in Lund, Sweden (2016/363).
Results
Setting aside one’s own needs
Being closely related to a person with cancer often meant setting aside one’s own needs and prioritizing the sick person’s needs and wishes. This reordering of priorities sometimes affected the participants’ own wellbeing, but was assumed by them to be a natural response, rather than something to be reflected up:
I’m not the one who’s sick; I’m a close relative. I’m supposed to handle it somehow. You’re the project manager, you’re supposed to endure. #24
Bowlby (1973) suggests that when we experience fatigue, pain or sickness, we seek proximity to a stronger, wiser, or protective person such as a spouse, friend, therapist, or physician, or from a support group. Our findings tend to indicate that despite being under strain, informal caregivers set their own needs aside and dedicated themselves to the sick person, without considering that they themselves also could be in need of support. This finding is also supported by other studies (Esbensen and Thomé, 2010; Fergus and Gray, 2009; Trudeau-Hern and Daneshpour, 2012). It has been suggested that informal caregivers fear that acknowledging their own needs could “detract attention from the patient” (Foster et al., 2015). The participants felt that even thinking about their own needs was to be avoided:
People ask, “How are you? How are you doing?” I don’t want to, and I don’t have time to think about how I’m doing, because I don’t dare to, actually. #3
Some participants said that the family member affected by cancer did not want the family to talk about the disease. In this type of situation, where the participants felt obliged to be there for their family member but were unable to talk about their experience, they experienced enhanced loneliness, isolation, and stress.
The experience of changing relationship roles evoked anxiety and fear and made it difficult for the caregivers to enjoy things and unwind, even when they were on their own:
I have to pull myself together because I’m so worried when I’m away. I never feel secure and if he doesn’t pick up (the phone) right away my heart races. I went to the movies once, and he hadn’t picked up before the movie started. I don’t remember anything from that movie, all I could see was him, dead at home. It was pointless to go to the movies. #4
Strategies to cope with stressful events include problem-focused confrontive coping and emotion-focused passive coping. Avoidance and denial are emotion-focused coping styles that are associated with burdening and an increased risk of depressive symptoms in caregivers (Papastavrou et al., 2012). Though opportunities for rest and recovery have been shown to be important for informal caregivers (Fergus and Gray, 2009; Trudeau-Hern and Daneshpour, 2012), several participants did not feel comfortable taking such opportunities. Several participants, both those bereaved and those whose family members were alive, focused so intensely on their family member that they developed depression or burnout syndrome. When this happened, some perceived it as a relief and as allowing them to care for themselves too:
I crashed in January and I’m still on sick leave for burnout syndrome. It was hard to make that decision, but at the same time a relief to be allowed to care for myself for a while. #24
Assuming the role of project manager
The perception of being the one who has to assume the role of being the project manager was a lonely experience throughout the course of the disease and aroused a multitude of conflicting emotions, with resultant strain on the participants:
I feel the responsibility to take care of him somehow, and I’m so ambivalent. I want to take care of him and at the same time I want to tell him to go to hell. It’s such a mix of love and hatred. #4
The feeling of overwhelming responsibility and love linked to helplessness and limited resources has been described as evoking feelings of guilt, shame, isolation, and even anger directed at the sick person (Duggleby et al., 2016). The participants described being responsible for everything running smoothly, including food, nutrition, medication, and health care appointments. The sense of responsibility, coupled with a suppression of the reality of the role of an informal caregiver, may add to the burden of caregiving and to the ambivalence related to the role (Ugalde et al., 2012). It can even influence sleep:
When he tiptoes off at night I lie in bed and listen. I don’t want to be his nurse or his mother or treat him like a child, so I pretend I’m sleeping so he can visit the bathroom in peace. #1
The sense of responsibility also related to managing health care appointments, including tracking the time and place of referrals, accessing information, and preparing questions for the physician. Some participants expressed distrust in health care:
If the doctor makes a suggestion, I go home and double-check it and then I call around and ask, “Is it really like this? Is this the right dose?” And I wish I didn’t need to. #26
This perceived need to supervise health care has been documented in previous studies that suggest that the perception of suboptimal communication with health care providers can contribute to psychological distress in caregivers, who feel responsible for bridging communication or knowledge gaps (Jolliffe et al., 2019).
The role of sole project manager carries a sense of moral duty that strongly parallels codependence:
You can leave a husband who is alcoholic or abusive, but people rarely do. My husband has cancer and will die. If I left him—you just don’t. But if someone drinks or uses drugs or hits you, then it’s your own fault if you don’t leave. #1
Some participants found consolation in the thought that 1 day they might be able to find a new partner. At the same time, even among the bereaved, getting a new partner was experienced as a form of betrayal:
I’m not a loner . . . but the children . . . my daughter hardly visits any longer, because there’s a new person there. She says: I will never see him as my dad. She visits the grave more often than she visits me. #28
Feelings of loneliness remained after the patient’s death, when the roles of caregiver and project manager were also lost: Since he passed I feel like, like there is nobody to take care of. I don’t know if taking care of is the right word but . . . you feel very lonely and yes—that’s what I feel. Loneliness. #8
Losing one’s sense of identity
Both patients and informal caregivers experience life-changing ordeals through the disease trajectory and have difficulty in readjusting to normal life at the end of treatment and follow-up:
I’ve felt very lonely, really lonely, and enormous grief. And now we’re supposed to find our way back to each other . . . I’m not the same person and my partner is definitely not the same person. We’re two new people, so to say, and yet not. #19
Research into life transitions shows that informal caregivers need to redefine “normal” to reduce the risk of negative effects such as anxiety, fear, anger, depression, guilt, and shame (Duggleby et al., 2016).
Several participants experienced a loss of their own identity. They were not being seen or heard when accompanying patients to hospital appointments. Thus, some stopped taking the patients to health care appointments. One participant commented on a meeting with a social worker:
I was there to meet my social worker but I had to use my partner’s social security number, because I didn’t exist anymore. It was on that level. #22
The perception of being invisible was not limited to the relationship with health care staff. After the death of a partner, many of the participants felt that neighbors and friends avoided them:
Sometimes when I was in my home town and I went in the store, it was really weird. Normally I know thousands of people, but it felt like the store was completely empty when I entered. Maybe they were hiding behind the shelves to avoid bumping into me. So I didn’t say hello to anyone, for the fourth time. #14
Some of the caregivers of a deceased person could see how they had faded during the course of the illness and had to reclaim their own sense of self after the death of their family member:
To be next of kin is special, you’re standing by. You shut down yourself a little, and you are just in it. Then suddenly you realize that you’re a person too, when it’s over. #5
To regain and maintain a sense of personhood requires recognition and uniqueness in relation to others (Duggleby et al., 2016). When health care workers and friends saw them only as an extension of a person with cancer, they lost that sense.
Being co-afflicted
The concept “co-afflicted” encapsulates an important aspect of being an informal caregiver to a person with cancer. It is interwoven with and synthesized from the three themes: “setting aside one’s own needs,” “assuming the role of project manager,” and “losing one’s sense of identity” (Figure 1). These three themes reoccurred throughout the interviews, and one participant summed up the experience:
We’re just as sick. About codependency, I was looking into that. It makes you into an addict somehow. We are co-afflicted, but nobody talks about it. #2
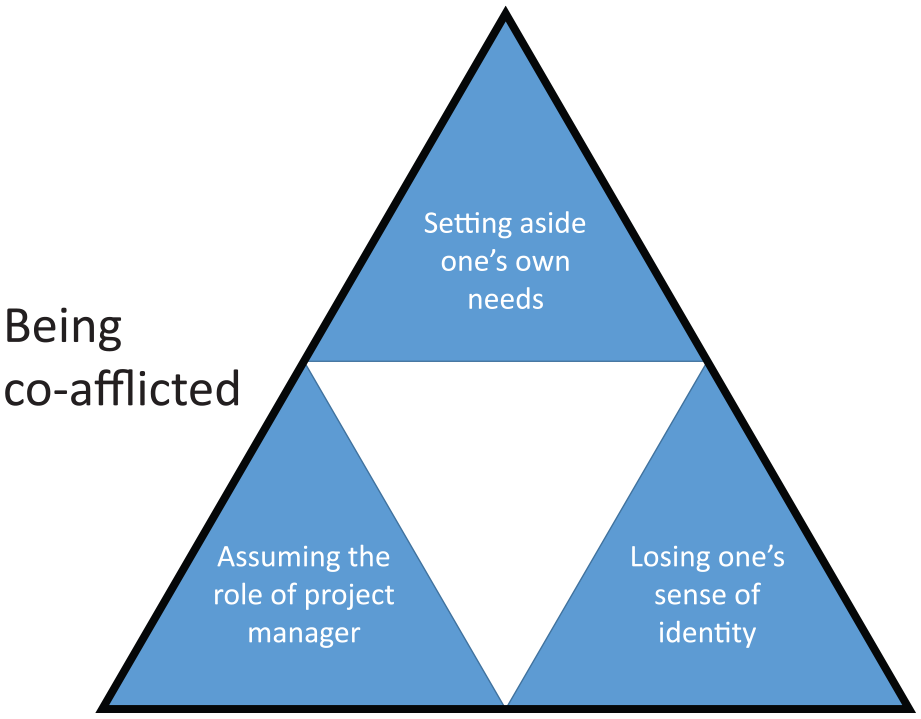
The three themes together form the framing theme “Being coafflicted”.
The idea of being co-afflicted came up as a result of reaching out and connecting online with others in the same situation. Through identification with others in the same situation the participants could see how the tendency to set their own needs aside and put all their efforts and attention to the sick persons needs led them to lose their own sense of identity and “just be co-afflicted” (#4). They were able to see in others what they were unaware that they were doing themselves. The participants said that the opportunity to join the focus group discussion and talk with others who shared similar experiences, feelings and thoughts was a great relief, and made them feel empowered:
It’s incredibly valuable for me to sit here . . . to realize that I’m not alone and I really appreciate that you . . . that I, can listen to other people share. #26
Just as in codependency, being able to identify with others seems to be very valuable to informal caregivers with a perceived high level of burden (Bacon et al., 2018).
Discussion
Informal caregivers make an important contribution to cancer care. Its importance is growing with increasing cancer prevalence and changing patterns of care with longer treatment times, a shift to outpatient services, and home-based care. The emphasis on person-centered health care has not been paralleled by an increased emphasis on the role of informal caregivers; they remain relatively invisible and unnoticed by health care professionals. With limited support from the health care system, many informal caregivers seek alternative support from community-based or municipal alternatives, charities, or private initiatives. We recruited informal caregivers from an online forum for peer-to-peer support for focus group interviews with a focus on lived experiences and perceived burdens. This is the first study of a small sample of Swedish informal caregivers belonging to an online support group for next of kin, and adds knowledge to a previously unexplored area.
As has been shown, the challenges and burdens can be summed up in terms of three themes: setting aside one’s own needs, assuming the role of project manager and, losing one’s sense of identity. These themes were united into the framing theme: being co-afflicted.
The very term “informal caregiver” may contribute to the perception that they are obliged to provide care rather than being entitled to receive support or care. The participants described how they refrained from meeting their own needs in order to take responsibility for, support and help the person with cancer, but in this process also lost themselves and became co-afflicted in a way that shows similarities to codependency (Bacon et al., 2018). Though group labeling may be stigmatizing, it may also provide support and relief, as has been demonstrated in relation to codependency (Bacon, 2015; Dear et al., 2005). The Composite Codependency Scale (CCS) was designed to provide empirical support for assessment of codependency based on the dimensions inter-personal control, self-sacrifice, and emotional suppression (Marks et al., 2012). These three dimensions were also recognized in our study in the themes setting aside one’s own needs and assuming the role of project manager. Codependency does not require chemical dependency in a significant other. Our data show that the wish to help and support may indeed be detrimental to a person’s own health (O’Brien and Gaborit, 1992).
The frequent descriptions of informal caregivers sacrificing their own needs to prioritize the needs of the patient show that for many of the participants such behavior came naturally and required little reflection. If these feelings of responsibility lead to insufficient rest and recovery, they may be detrimental and contribute to reduced quality of life and increased risk of secondary disease among the informal caregivers (Trudeau-Hern and Daneshpour, 2012). This risk has been connected to stress and lifestyle factors. In our study, the participants reported being stressed to the extent that some developed depression or burnout syndrome. They continued to care for their family members while they themselves were on sick leave. An increased risk of somatic diseases such as musculoskeletal disorders, cardiac disease and stroke, as well as psychiatric disease, has been documented among informal caregivers (Ji et al., 2012; Sjölander, 2012).
The project manager role described was identified as a sole and long-standing responsibility over the course of a long disease trajectory. It included a multitude of practical, coordinating, and investigatory tasks related to the responsibilities of daily life as well as to health care perspectives. Recognition in this role may be important to support the informal caregivers and to make their contributions transparent and accepted in order to minimize the impact on the relation with the patient (Bacon, 2015; Bacon et al., 2018).
Feelings of losing one’s identity were described as a major informal caregiver challenge. Participants felt that they were viewed as merely an extension of the sick person. These feelings were partly evoked by health care consultations that were strongly focused on the patient and ignored the caregiver. Interestingly, these feelings were also reported to remain after the loss of a family member to cancer. Our data suggest that health professionals can make a difference by acknowledging the accompanying persons’ uniqueness, and enquiring into their needs and awareness of support options.
Study limitations
The study is concerned with exploring the burden carried by informal caregivers. Thus, the results are idiographic rather than general. We used purposive sampling of members of, or people interested in, an online support community who volunteered to join the focus groups. The results might have been very different with a different sample of informal caregivers. Women were overrepresented among the participants, probably because they are overrepresented in the online community used, and because women may be more likely than men to reach out for support and are also most likely to become caregivers (Schrank et al., 2016). Half of the participants were bereaved caregivers, and one might suspect that the retrospective accounts of their lived experience would differ from current caregivers. However, the themes accurately captured the lived experience of both groups.
There is always a risk that the authors’ perspectives may color the findings. Three of the authors are women, two registered nurses with a research focus on older people and palliative care, and one medical doctor with focus on oncology. One author is male, registered psychologist with focus on serious illness. All four authors were involved in the analysis, constantly challenging the interpretation of the data, thus reducing the risk of a biased interpretation. The analysis was discussed continuously in the research group, and stakeholders validated the result.
The focus groups were conducted in Sweden, a country that endorses individual autonomy rather than relying on extended family and friends for support. In other countries, with different communal or cultural interaction patterns, the results might be different (Githaiga, 2017).
Future studies should focus on developing measures for early identification of “highly co-afflicted” informal caregivers as well as interventions suited to their needs. Further investigation into the similarities of the concepts of codependency and being co-afflicted might be helpful to develop and implement targeted interventions.
Clinical implications
Informal caregiving provides a considerable, but invisible, resource for health care. The support gained from informal caregiving should therefore be optimized and safeguarded to avoid negatively affecting the health of informal caregivers. It may be helpful to clarify support options and support informal caregivers in finding a personalized and suitable option. Further, health care professionals should be aware of the burdens of caregiving and avoid reinforcing maladaptive behaviors. They should be proactive in showing interest in the informal caregiver as a unique person and suggesting initiatives to make their burden manageable. In this regard the definition of informal caregivers as being co-afflicted may be helpful. Possible initiatives are support groups that include informal caregivers, psychoeducation with focus on the effects of caring for a person with cancer, and the provision of individualized and targeted support options for informal caregivers.
Conclusion
We demonstrate that the lived experience of being an informal caregiver can be understood through the concept of being co-afflicted with similarities to the concept of codependency. This recognition may help legitimize the experience of caregivers, entitle them to professional support, and help them navigate future behavior and decisions. Caregivers are carrying considerable strain and report disregarding their own needs. It is important that health professionals acknowledge caregivers sense of setting aside their own needs, assuming the role of project manager, and losing their sense of identity. Though evidence-based and personalized support initiatives are highly needed, part of the solution may be to pay attention to, affirm the perspectives of, and provide support to informal caregivers in cancer care.
Footnotes
Acknowledgements
The authors thank the participants in the focus group interviews, and Inga-Lill Lellky and Alexandra Lellky from Cancerkompisar.se for helping us recruit participants. The authors also thank Christina Landegren and Linn Rosell at the Regional Cancer Center South in Sweden for coordinating and participating in the focus group interviews.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data availability statement
The authors will provide access to the de-identified data on request.
