Abstract

What is the first step in adjusting to a vascular disease diagnosis?
A new vascular disease diagnosis can be unexpected, life-changing, and frightening. Vascular disease can have both physical and psychosocial effects, potentially impacting mental health, finances, relationships, and beyond. 1 Therefore, it is important that patients learn coping strategies for positive adjustment to overcome these challenges. 2 Deciding to seek mental/behavioral health support during this process is a sign of strength and bravery, although it can also evoke feelings of vulnerability. Different problems demand different solutions. Some solutions focus directly on solving the problem, while others focus on managing thoughts, feelings, and behaviors related to the problem (Table 1).
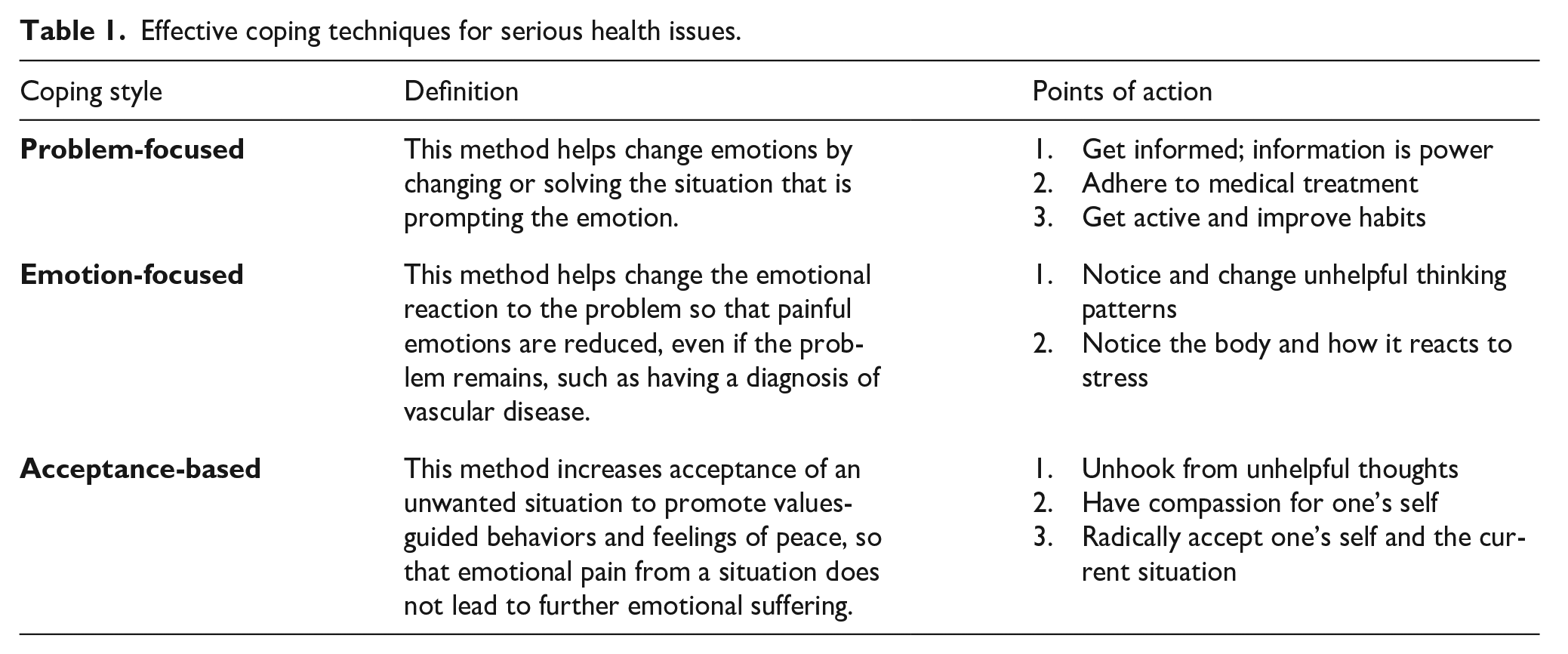
Effective coping techniques for serious health issues.
Problem-focused approaches for managing vascular disease
A problem-focused approach helps manage emotions by changing or resolving the situation that creates the feelings in the first place. This course of action is best when the problem can be identified, and patients can take active steps to solve it. Examples include the following approaches.
Get information about the diagnosis
Vascular disease is any condition that affects the blood vessels, including the arteries, veins, and lymphatics. Examples include peripheral artery disease (PAD), carotid artery and cerebrovascular disease, aneurysms (dilated vessels), dissections (torn arteries), and venous thromboembolism (e.g., pulmonary embolism, deep vein thrombosis, and other types of blood clots). Many patients with a serious vascular diagnosis fear the unknown; they may fear loss of control, future risk of vascular events, hospitalizations or procedures, and death. 3 This uncertainty can lead to uncomfortable emotions, such as chronic feelings of worry or anxiety. Sometimes, patients may try to avoid learning or thinking about their medical condition as a way to prevent negative feelings. However, this approach often backfires. Gaining more knowledge and becoming more certain (in other words, changing ‘unknowns’ into ‘knowns’) are good ways to feel more confident and comfortable.
Anyone can develop vascular disease, though some people have an increased risk due to lifestyle factors or genetics. Helpful steps include talking with the healthcare team and requesting educational materials. Free patient articles about many different vascular diseases are available at journals.sagepub.com/vmjpatientpage.
Adhere to medical treatment
The treatment of vascular disease depends on the particular disease itself (e.g., venous thromboembolism, aneurysm, PAD), though generally focuses on slowing disease progression, addressing underlying causes (including any other contributing medical conditions), and relieving symptoms. Treatment may involve lifestyle changes (e.g., quitting smoking, changing diet, exercising), prescription or nonprescription medications, and other medical or surgical interventions. Some ways to remain engaged with care include completing recommended testing (such as vascular imaging), 4 adhering to prescribed treatments, and attending follow-up appointments. Patients who have questions about their treatment plan should feel empowered to ask members of their healthcare team (e.g., physician, nurse, pharmacist) for clarification. When personal values, preferences, and concerns are openly discussed, patients are more likely to understand and follow the plan to improve their health. 5
Engage in lifestyle changes to optimize cardiovascular health
Regardless of the vascular issue, reducing risk factors and improving lifestyle habits make a tremendous difference. Exercising can help treat vascular disease symptoms while improving physical and mental health. 6 Depending upon the specific vascular disease, patients may have limitations on strenuous physical activity and should talk with their provider before beginning exercise plans. However, leading an active lifestyle (e.g., choosing to take the stairs or going for a walk) is typically more beneficial than harmful.
How can emotions be managed after a vascular disease diagnosis?
An emotion-focused solution helps change the gut reaction to a problem and reduce the associated negative emotions, even when the problem remains. After receiving the news of a vascular disease diagnosis, the body may react with the ‘fight, flight, or freeze’ response. 7 The first response may be to try to control uncomfortable emotions that arise. Unhelpful emotional reactions include excessive crying, hyperventilation, or self-isolation from loved ones. Some are less obvious, such as excessive worrying. Often, patients experience anxiety or worry while trying to anticipate dangerous events and preparing for the worst. Too much worrying can lead them to focus on the negative and dismiss the positive parts of life. Constantly thinking this way can stir up emotions and cloud judgment. Recognizing unhelpful thinking styles (see below) can lessen anxiety, improve mood, and lead to better reactions.
Catastrophizing and fortune telling: ‘time bomb thinking’
Catastrophic thinking happens when patients excessively focus on and imagine the worst possible outcomes of a situation. When patients wonder, ‘What if . . .?’, and then imagine the worst-case scenario (such as having a stroke and becoming paralyzed or dependent on care), or when patients make pessimistic guesses about the future (e.g., anticipating a traveling blood clot, a ruptured aorta, or a limb amputation), they are catastrophizing. Thinking this way may lead to strained relationships, poor judgment, or unhealthy behaviors.
Overgeneralizing: ‘first this, now that!’
Sometimes, it is tempting to make a broad conclusion based on a single incident or a single piece of evidence (e.g., thinking, ‘I should avoid the gym because that is where my dissection happened’). Even if something bad happens only once, patients may begin to expect it to happen over and over. A single, negative event may be viewed as a part of a never-ending pattern of defeat.
Personalization: ‘antihero thinking – it’s me; I’m the problem’
Personalization occurs when people blame themselves for events that are beyond their control. They may feel like they are the sole cause of some unwanted event that they were not responsible for, such as aortic disease. Personalization often occurs with ‘black-or-white thinking,’ or thinking that something is just one way or another – good or bad, a success or failure, a positive or negative. Approaching events from this ‘either/or’ perspective leaves out the gray area and prevents understanding of the complexity of most situations.
How can unpleasant feelings in the body be managed?
Patients with new or worsening vascular disease may feel increased stress or worry about managing their health. When left unmanaged, stress can start a spiral of anxiety that can be difficult to break. For example, acute periods of stress can bring about physical sensations such as muscle tension, headaches, chest pressure, stomach upset, and fatigue. The following strategies can be used to address stress and anxiety head-on. Practicing awareness and mindfulness can help change the physical reactions to stress and ultimately relieve anxiety. Experts suggest practicing these strategies regularly, even when not feeling anxious, to prepare the brain and body for times of stress.
Deep breathing
Deep breathing – sometimes referred to as diaphragmatic breathing – is a simple, effective, and easy-to-use technique for managing uncomfortable bodily sensations and unwanted emotions. There are many methods of deep breathing. One simple way is to breathe in through the nose for 4 seconds, hold for 2 seconds, and slowly breathe out through the mouth for 6 seconds, making the exhale longer than the inhale. Regular practice is needed so that this strategy can be easily implemented during stressful times.
Self-soothe with senses
Finding a way to use all five senses (seeing, hearing, touching, tasting, and smelling) is a good way to soothe the mind and body. Patients can use their current location or think of a comforting place and try to imagine the setting in detail. What can be seen? What can be heard? What smells are present?
Body scan
Body scan exercises encourage close attention to physical sensations. The goal is to increase self-awareness. Typically, patients start with one area of the body (such as the head or toes) and slowly work in order through the rest, addressing major areas such as the neck, shoulders, chest, back, arms, hands, and so on. If areas of tension are noticed, then squeezing those muscles tightly for a few seconds and releasing can help.
Is it possible to feel peace again after a serious vascular disease diagnosis?
Acceptance strategies 8 can help patients be at peace with who they are and their present situation. Acceptance is a willingness to acknowledge difficult events and allow them to be part of the experience. Examples of acceptance-based coping strategies include the following.
Cognitive defusion: ‘unhook from unhelpful thoughts’
Cognitive defusion is the practice of looking at the thoughts rather than from them. Patients with vascular disease may have thoughts such as, ‘I will never be able to live a normal life again.’ These thoughts may trick the mind into thinking they are facts and cause one to feel negative emotions more strongly. Once negative thoughts have been identified, they can be changed. Changing the thought, ‘I am not normal anymore,’ to ‘I’m only telling myself that I am not normal anymore, but that doesn’t make it true,’ helps a person realize that they have a choice in what they think and that feelings are only temporary experiences.
Mindfulness: have compassion, be present
Mindfulness practice can help decrease feelings of stress, anxiety, and depression and improve sleep, blood pressure, quality of life, overall feelings of wellbeing, and even sense of humor. 9 Much of life can be spent thinking about events in the past or what may happen in the future and attaching emotional significance. Being mindful involves being in the present moment (being nonjudgmentally aware of thoughts, feelings, and senses). There are many ways to be mindful: deep breathing, using the senses, body scanning, or doing a familiar activity (i.e., eating, walking, cooking, etc.) in a mindful manner – that is, paying attention to surroundings and enjoying the activity to the fullest.
Radical acceptance: rejecting reality causes suffering
Radical acceptance is a skill to help live life to the fullest despite challenging circumstances. Resisting reality leads to distress, so when patients radically accept reality for how it is – even if they do not like it – they confirm that life is still worth living. The goal of radical acceptance is to turn suffering that cannot be tolerated into pain that can be tolerated.
10
At first, accepting reality may lead to uncomfortable emotions; however, a deep sense of peace usually follows with practice. Examples of coping statements consistent with radical acceptance include:
I can’t control that I have an aortic aneurysm, but I can control how I respond to it.
I’ve dealt with difficulties before, so I can deal with the blood clot in my lungs.
The present moment is where I am supposed to be, even if I do not like it.
When is professional help needed?
Relying on a social network, such as family and friends, is a good approach to managing health-related quality of life. However, even with good support, patients might benefit from additional support. When problems in life stop someone from feeling good or functioning well (Figure 1), seeking professional help from a health psychologist or other mental health professional can make a big difference.
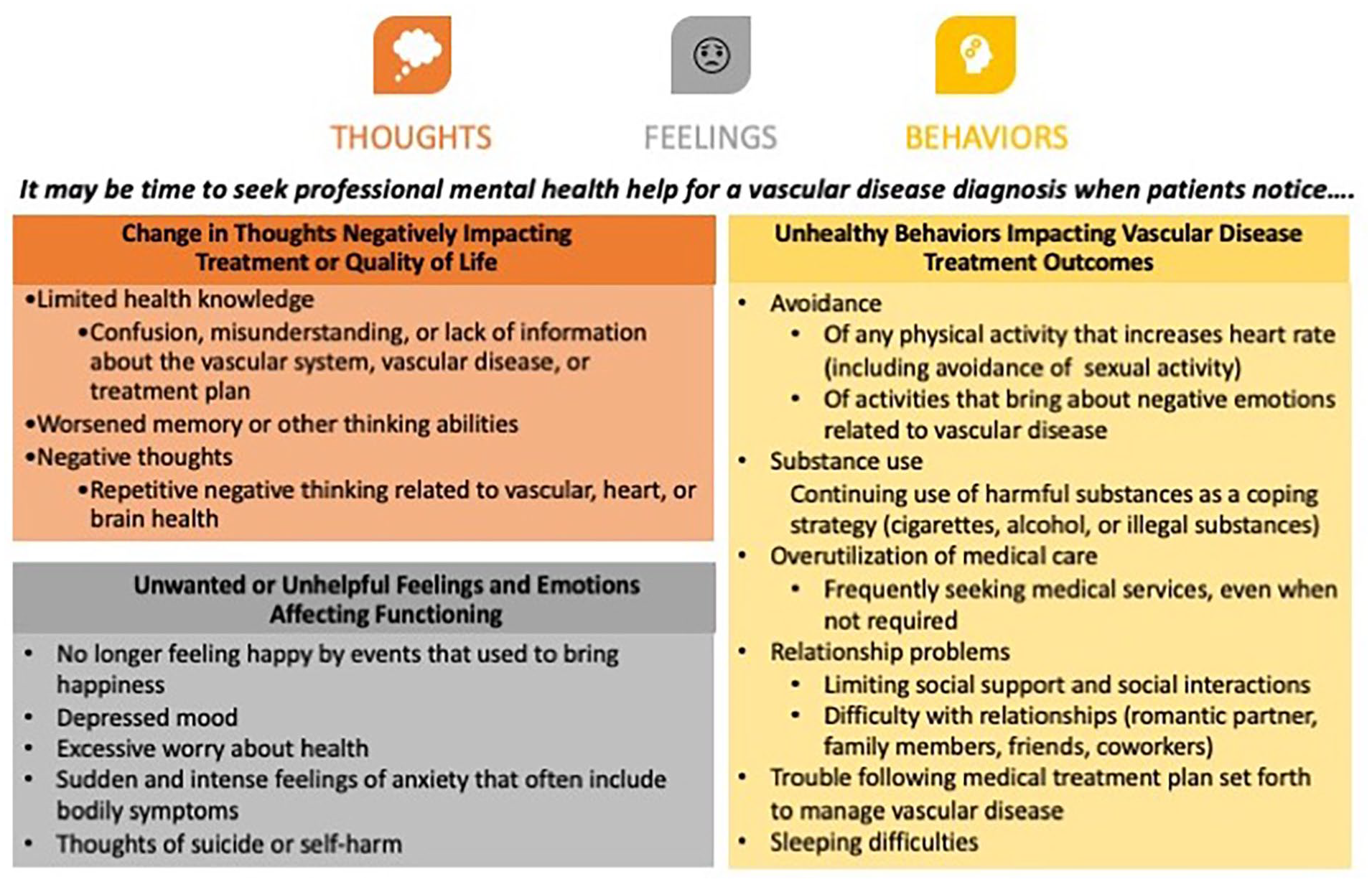
Tool for determining the need for psychological services.
Summary
Successful coping with a serious vascular diagnosis may include lifestyle changes, managing health, and adjusting to uncertainty regarding the future. Various problem-focused, emotion-focused, and acceptance-based coping strategies have been found to decrease feelings of stress, anxiety, and depression. By employing these tools, patients can feel empowered to play an active role in their vascular health and improve their quality of life.
The ‘Vascular Disease Patient Information Page’ is a regular feature of Vascular Medicine. All articles in the collection are available for free online at http://journals.sagepub.com/vmjpatientpage.
The Vascular Disease Patient Information Page is provided for educational purposes only and is not a substitute for medical advice.
Footnotes
Acknowledgements
The authors would like to thank the Cardiac Psychology Service team and the team of physicians, nurses, and staff at the East Carolina Heart Institute for their ongoing support and valuable role in comprehensive cardiac patient care.
Declaration of conflicting interest
Dr Samuel F Sears serves as a consultant to Medtronic and Abbott. He has received honoraria from Medtronic, Biotronik, and Zoll Medical in the past 12 months. All other authors have no conflicts of interest or disclosures regarding financial activities, relationships, and affiliations to report.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
