Abstract

Keywords
What is medical genetics?
Medical genetics is a specialty in the health care field that focuses on the inheritance of disease. Remarkable breakthroughs have occurred in the past few decades, and now clinicians have a better understanding of the genetic basis of many conditions across multiple organ systems, including vascular disease. For example, the risk for aortic dissection (i.e., tears in the aorta, which is the main blood vessel that leaves the heart and provides oxygenated blood to the body) or for thoracic aortic aneurysms (i.e., dilations) is often inherited. Having a genetic diagnosis allows physicians to follow disease-specific guidelines for imaging follow up, thresholds for surgical repair, management of nonvascular manifestations of the disease, and medication therapy. 1 A genetic diagnosis also allows for targeted genetic testing for family members to aid in early diagnosis.
What is genetic testing?
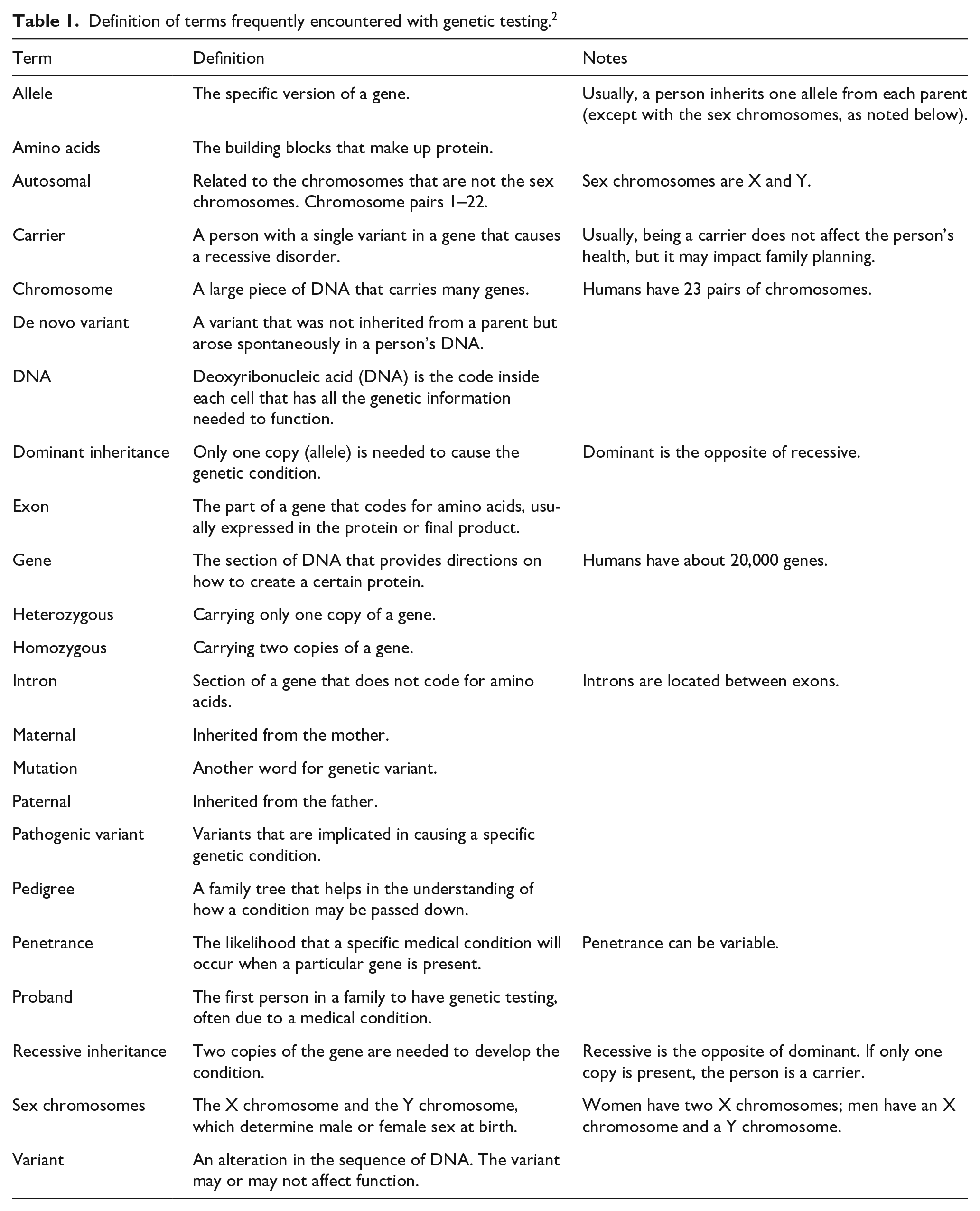
Genetic testing analyzes a person’s DNA to look for variants in his or her genes that may be associated with certain medical conditions. The results of this testing can help confirm or rule out a diagnosis. However, testing may detect a gene variant (DNA change) that is ambiguous, which is called a variant of uncertain significance (VUS). In this scenario, family member testing may be helpful to track the origin of the variant for a connection to the condition. The results may also help to predict the chances of developing a genetic disorder and passing it on to children. Table 1 provides a glossary of terms commonly used when discussing genetic testing.
Definition of terms frequently encountered with genetic testing. 2
What is genetic counseling?
Genetic counseling starts with an appointment with a health care provider (certified genetic counselor or a medical geneticist) who has specialized training in medical genetics. The provider can counsel, support, and help with understanding the process of genetic testing, the results of the tests, and the implications for the patient and family members.
What is the best way to prepare for a genetic counseling appointment?
Prior to the appointment, gathering the family medical history can assist the genetic counselor in determining the inheritance pattern. 3 Helpful information to obtain from relatives when looking for inherited vascular disorders of the aorta and other arteries includes:
History of aneurysm (a dilated blood vessel);
Location of the aneurysm (e.g., thoracic aorta in the chest, abdominal aorta, or brain);
History of dissection (tearing of an artery, such as the aorta or carotid artery);
Any rare vascular conditions, such as fibromuscular dysplasia (FMD);
Any relatives with sudden, unexpected cardiac death;
The age at time of event or death in anyone with a vascular condition;
Results from any family members who have already had genetic testing.
Figure 1 shows an example of a pedigree, a typical chart that is created illustrating the family history obtained during the visit. The genetics provider will also ask about other medical conditions occurring in a family, such as cancer or intellectual disability.
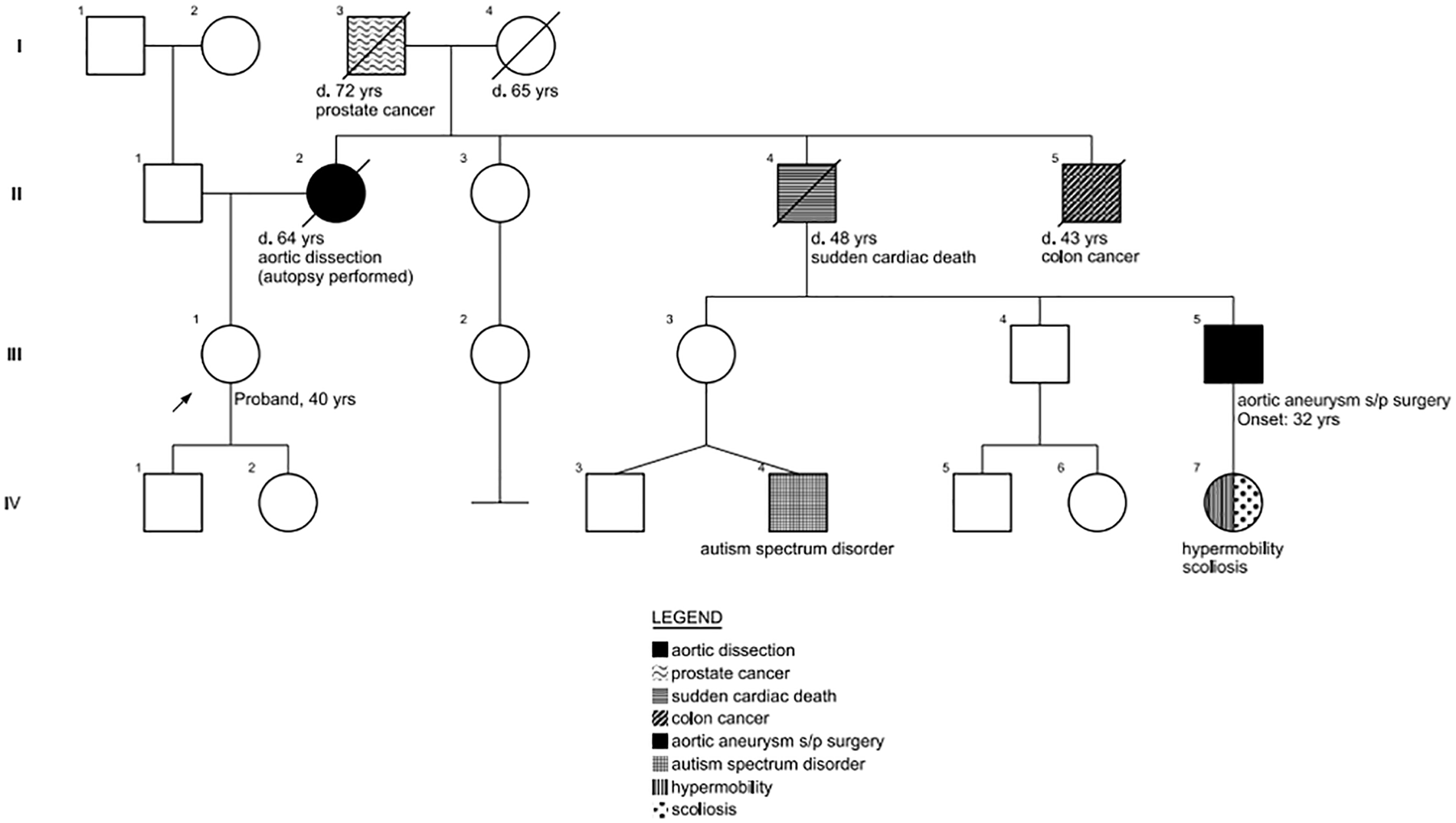
Sample pedigree showing the inheritance of aortic disease in a family. Circles represent women; squares represent men. The proband (III-1) is a 40-year-old woman who came for evaluation because her mother died suddenly at age 64 (II-2). An autopsy found an aortic dissection. The family history also revealed that maternal grandparents died from prostate cancer (I-3) and unknown causes (I-4). A maternal uncle (II-4) had sudden cardiac death. One of his children (the proband’s maternal cousin [III-5]) had aortic surgery in his 30s; he has a daughter with scoliosis and hypermobility (IV-7). An additional maternal uncle died of colon cancer (II-5). A maternal first cousin-once removed (IV-4) has autism.
Sometimes, a vascular disorder falls into the category of a connective tissue disorder, which can present with nonvascular features in other parts of the body. Examples of these disorders include Marfan, Loeys–Dietz, or Ehlers–Danlos syndromes.
Relevant issues include:
Eyes: lens dislocation, retinal detachment, or early eye muscle diseases;
Musculoskeletal: scoliosis (curvature of spine), flat feet, pectus deformities (chest wall protruding out or caving in), hypermobility (extremely flexible joints) or joint dislocations, or torn muscles, tendons, or ligaments;
Skin: easy bruising or abnormal-appearing scars;
Other medical issues: bleeding excessively with childbirth, hernias, or cleft palate.
What are the benefits of genetic testing?
Genetic testing can help confirm a suspected medical diagnosis. Confirmation of a specific diagnosis can help guide future monitoring and treatment, particularly if that diagnosis is a syndrome that is typically associated with other medical problems. For example, if Marfan syndrome is suspected and the genetic testing shows a pathogenic (disease-causing) variant (mutation) in the FBN1 gene, then the diagnosis is confirmed. Then, other people within the same family can undergo testing for that specific variant. This testing is easier and less expensive because each family member (parents, children, or siblings) only needs to be tested for the specific familial variant. Family members who have the variant then should be screened for aortic disease and counseled about other associated nonvascular issues. Family members who test negative for the familial variant do not need screening for aortic aneurysms, and unnecessary imaging can be avoided.
In some cases, a specific syndrome may have been suspected initially, but genetic testing may reveal a variant in a different gene. For example, Marfan syndrome can lead to thoracic aortic aneurysms, along with certain musculoskeletal and eye features. Loeys–Dietz syndrome (LDS) can also cause similar symptoms. Making this distinction is important because LDS puts people at high risk for aneurysms throughout the body and they may have a more severe aortic disease that may require surgery at smaller aortic diameters than in other conditions. Therefore, an accurate diagnosis can substantially impact medical care because the imaging and monitoring plans would differ.
Furthermore, the results of genetic testing can also be helpful for family planning. As an example, Marfan syndrome is an autosomal dominant condition, which means that only one copy of the altered gene is enough to lead to the disorder, resulting in a 50% chance that each child of an affected person will also be affected by the disorder. Parents may want to know about this risk prior to considering pregnancy. Options such as in vitro fertilization (IVF) and preimplantation genetic testing are available to avoid having a child with the condition; prenatal testing is also possible to test a pregnancy already in progress to plan for postnatal care. If the mother is the affected person, then pregnancy may increase the risk of health complications, and high-risk pregnancy care should be implemented.
What are the potential risks of genetic testing?
Many of the risks of genetic testing are emotional, and the results may lead to anxiety. Indeed, it can be stressful to learn about an inherited disorder. People may feel guilty or angry. A parent may feel guilty about passing a gene along to a child; another relative may feel guilty for not inheriting a disorder that affects other family members. Tension may arise within the family because the results may impact others who may or may not want to know the information. Moreover, testing may not answer all questions, leading to uncertainties in many cases.
The situation is further complicated because having a specific gene variant does not guarantee that the disorder will develop, nor does it predict the severity. Sometimes, a genetic condition has reduced penetrance, meaning that not every person with the gene variant (mutation) will develop a vascular issue. In addition, people with the same variant may have different degrees of severity of the disorder, called variable expression. For example, among four siblings who all carry the same genetic variant, one may have severe blood vessel problems with multiple aneurysms or dissections, two may have a slightly dilated aorta, and one may have completely normal imaging.
Can genetic testing lead to discrimination?
Discrimination based on genetic testing results is a concern for many people who are considering genetic testing or are participating in genetics research. The Genetic Information Nondiscrimination Act (GINA) went into effect in the United States in 2009. This legislation was designed to prevent discrimination based on genetic information in two areas: health insurance and employment. However, GINA does not protect against genetic discrimination for life, disability, or long-term care insurance. Fortunately, some state laws offer additional protection against discrimination based on genetic testing results.
Is genetic testing covered by insurance?
The cost of genetic testing has decreased significantly. Multiple labs offer genetic testing for vascular conditions, and many are in-network providers for major insurance companies. Genetic testing is frequently covered by insurance, but networks, deductibles, and copay costs can come into play. Many labs offer a ‘benefits investigation’ to help determine the range of out-of-pocket expenses, or they may have a reasonably low set-cost of $200–$400 for a panel of genes. People can also use a health savings account to cover the cost of testing. Lab choices and billing information are usually discussed in the genetics appointment prior to testing.
How is genetic testing performed and how long does it take?
Genetic testing can be performed on a biological sample, including blood, buccal cells (swab of inside the cheek), or saliva (spit). Once the genetics provider orders the test, he or she can send in the sample from the clinic, or the lab will send buccal or saliva kits directly to the patient in the mail to return via a prepackaged, prepaid courier service. Instructions for labeling samples and how to obtain the sample are included in the kits. Results typically take about 3–5 weeks to process and will be sent to the ordering genetics provider, who will then communicate and discuss results with the patient. Some labs will release results directly to the patient; however, results can be complicated to understand, so it is important to return to the genetics provider to ensure a correct interpretation.
What are the possible outcomes of genetic testing?
Genetic testing can lead to three possible outcomes:
The test results may be clearly positive, revealing a genetic basis for the medical findings. This result is called a pathogenic or likely pathogenic variant.
The test results may be clearly negative, revealing a normal DNA sequence based on the testing that is available today.
The test results may indicate a variant of uncertain significance (VUS).
A VUS means that a change in the genetic sequence was found, which may or may not be meaningful. The findings may be related to the observed medical condition or may simply be part of normal genetic diversity seen in the general population. It may not necessarily indicate a risk for health problems, and the variant may not be related to the patient’s vascular condition. If a specific variant is found, other family members with similar medical issues could also undergo genetic testing. For example, if a VUS is found in one family member with an aneurysm and a close relative (child or sibling) also has an aneurysm, the relative could be tested to see if the variant tracks with the aneurysm within the family.
If genetic testing is negative, what happens next?
The majority of individuals who undergo genetic testing are not able to obtain a specific genetic diagnosis despite a strong family history with multiple affected family members. In these cases, the inheritance pattern may suggest that the condition is genetic, but the genetic variant may remain undiscovered. Therefore, depending on the medical history, the genetic counselor may recommend additional testing in a few years when more information is available from ongoing gene discovery.
Researchers and clinicians are diligently working to understand the genetic basis of vascular diseases, and participation in research studies can help move the field forward, especially if there is an extensive family history of the vascular condition. In the future, gene-specific management based on the detected variant will increasingly allow a more personalized approach to medical care.
Summary
Widely available genetic testing for genetic variants associated with vascular diseases that cause aneurysm and dissection is the product of remarkable advances in the medical field over the past several decades. The genetics provider plays a critical role in shepherding the patient through an otherwise complex process. The test results can be combined with family history and diagnostic testing to confirm or rule out medical conditions, estimate risk, and assist with the development of individualized treatment approaches, including medication, type and frequency of vascular imaging, and testing of family members.
The ‘Vascular Disease Patient Information Page’ is a regular feature of Vascular Medicine. All articles in the collection are available for free online at http://journals.sagepub.com/vmjpatientpage.
The Vascular Disease Patient Information Page is provided for educational purposes only and is not a substitute for medical advice.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
Dr Elizabeth Ratchford’s work was supported in part by the generosity of David Kotick (1926–2021).
