Abstract

A 73-year-old woman with a history of recurrent deep vein thrombosis of the left lower extremity, which occurred approximately 7 and 5 years previously, was admitted for placement of a caval filter prior to surgery to repair a left femur fracture. Physical examination revealed edema and swelling of the left leg, and color Doppler ultrasonography (US) documented a floating oval lesion in the left common femoral vein (online supplementary video).
Subsequently, computed tomography (CT) of the abdomen demonstrated a filling defect in the left femoral vein, supported by an oval formation with sharp margins and fat attenuation, with axial dimensions of 19 × 16 mm (Panel A, arrows).
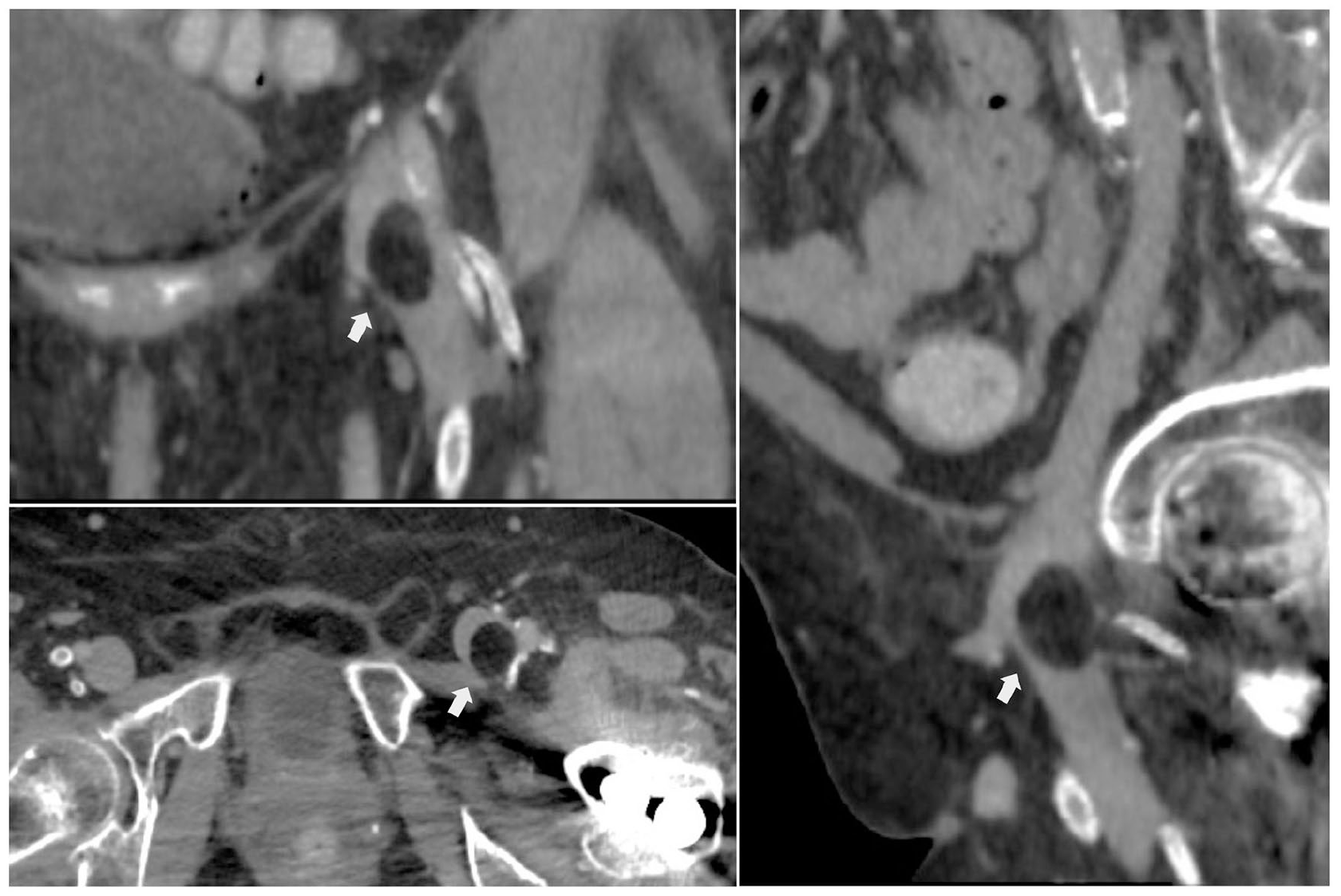
A multistep therapeutic approach, including caval filter placement, anticoagulation with subcutaneous low-molecular-weight heparin and surgical excision, was performed to reduce the risk of thromboembolism, establish the pathologic diagnosis, and prevent complications arising from this tumor.
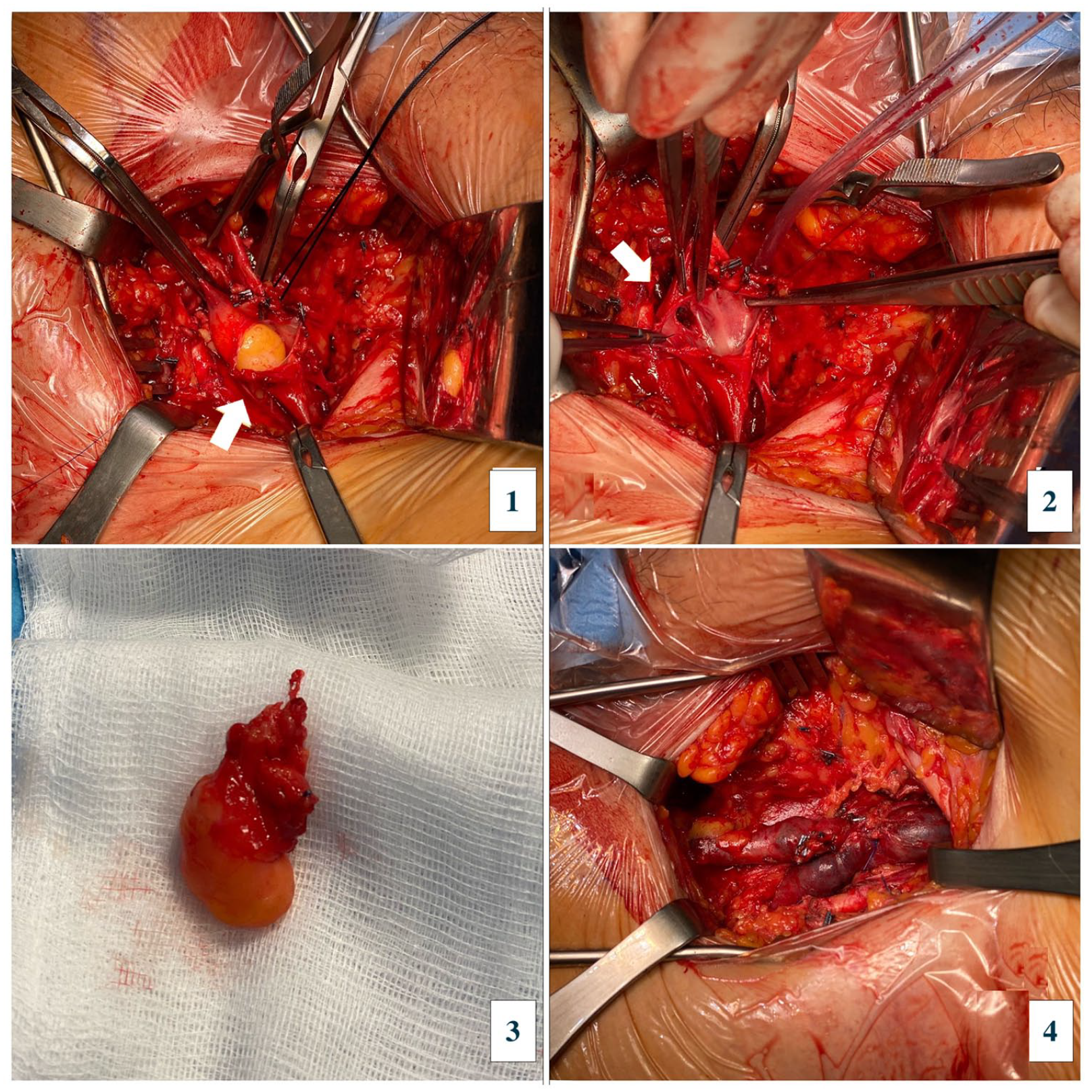
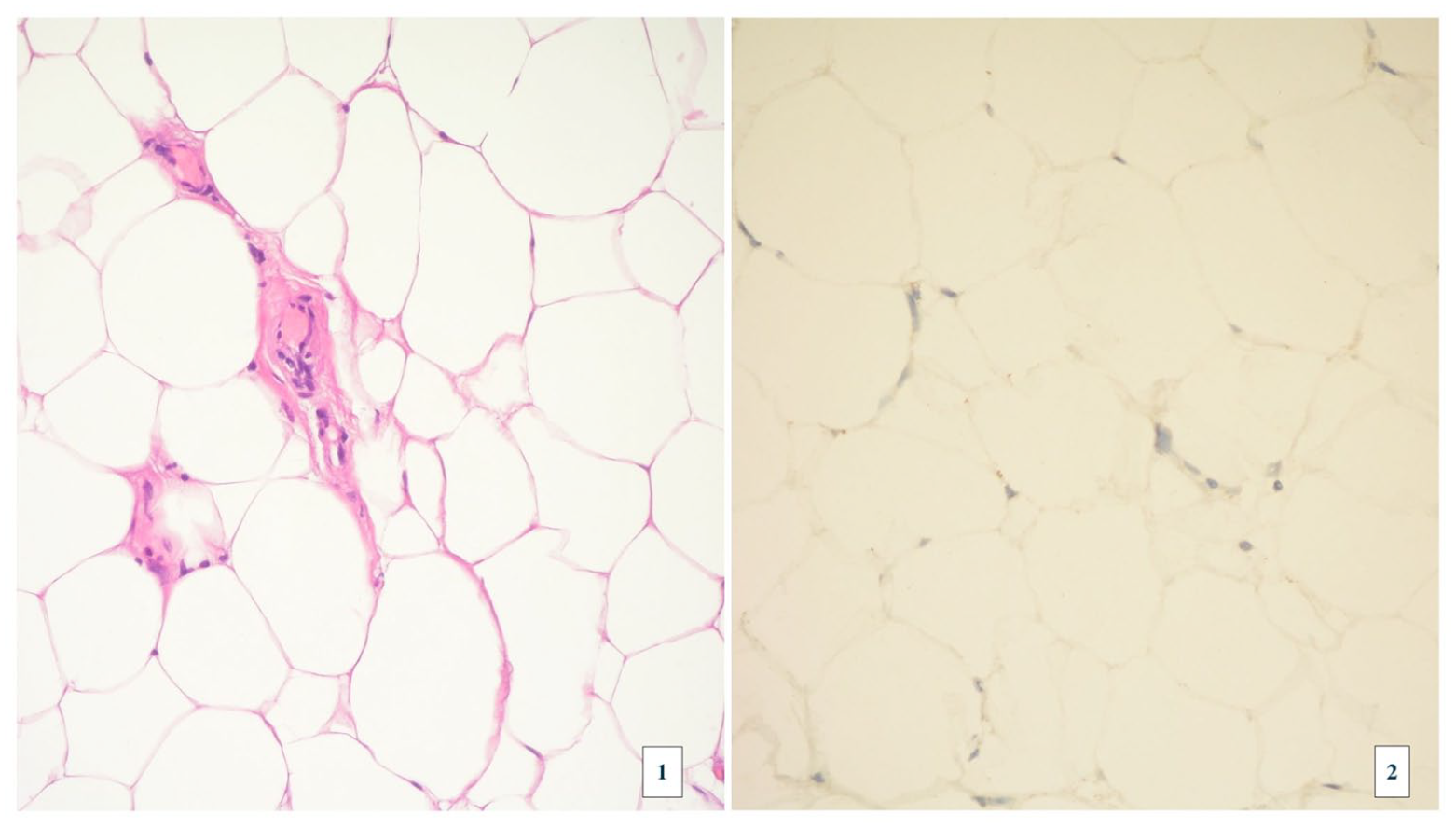
After placement of the caval filter, surgical excision was performed, and the patient was found to have an extrinsic adipose formation infiltrating the postero-lateral wall of the femoral vein, in continuity through a wall breach with an adipose mass occluding the venous lumen (Panels B-1 and B-2). The mass was resected, and the venous breach was repaired with a Prolene 6/0 continuous suture (Panels B-3 and B-4). Histologic examination revealed a lipomatous, partially capsular lesion without evidence of cellular atypia, consistent with lipoma (Panels C-1 [hematoxylin-eosin stain] and C-2 [immunohistochemical stain for murine double minute 2 or MDM2 expression]).
One month after surgery, the caval filter was removed. At 3 months’ follow-up, the patient had no swelling or symptoms, and US showed patency of the left femoral vein in the absence of residual formations.
Lipomas are benign tumors composed of well-differentiated adipocytes and usually arising from the inferior vena cava, superior vena cava, brachiocephalic veins, and sporadically from lower-extremity veins. 1 Intravascular lipomas are often asymptomatic and are considered an incidental finding during abdominal CT, with a frequency of 0.35%. 2 If they occur, vascular complications of lipomatous lesions usually manifest as signs and symptoms of venous compression, including limb swelling. Deep vein thrombosis may be a complication, although rare. 3
Indications for surgical excision of lipomas are expansive growth, cosmetic reasons, or, rarely, transformation into liposarcomas. 4 Some authors consider surgical excision mandatory to differentiate benign lipomas from malignant liposarcomas and to treat obstructive symptoms of the deep venous system. 5
We chose a multistep therapeutic approach, including caval filter placement and anticoagulation to reduce the risk of thromboembolism, and surgical excision to prevent complications that may arise from this tumor, and exclude the presence of a liposarcoma. Removal of the mass also allowed subsequent removal of the caval filter and discontinuation of anticoagulant therapy.
Only five cases of lipoma of the common femoral vein are described in the literature, with a single case of localized thrombosis of the femoral vein, and venous obstruction in all other cases. This is the second case of intravascular lipoma causing deep vein thrombosis reported in the literature.
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Daniella Kadian-Dodov, Images in Vascular Medicine Section Editor, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplementary material
The supplementary material is available online with the article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
