Abstract

Keywords
Near-infrared spectroscopy (NIRS) is a noninvasive technique used to measure changes in oxyhaemoglobin (O2Hb), deoxyhaemoglobin (HHb), and total haemoglobin (THb) tissue concentrations, and thus in regional tissue oxygen saturation (Ox%). 1 Moreover, NIRS has been used to asses muscle oxygenation in clinical populations where O2 delivery and utilization are involved in muscle myopathies, muscle atrophy, heart failure, and peripheral arterial vascular disease. 2 Recently, NIRS has been also utilized in combination with vascular occlusion testing to explore muscle microcirculatory function in several clinical settings, 3 while only a few studies have used this technique to evaluate the effect of nicotine on microvascular responsiveness.4–6 In none of these cases was the vascular response evaluated after a 12-hour overnight nicotine abstinence.
This investigation was conducted as part of research exploring the ergogenic effects of snus on aerobic performance during exercise until exhaustion in two conditions: nicotine satiety and following nicotine abstinence. 7 Snus is a smokeless tobacco product which is administered in small sachets that are typically positioned between the gum and the lips for 30 minutes, then discarded. 8 The aim of this study, performed in nicotine (snus) users, was to investigate, by means of NIRS and a vascular occlusion test (VOT), the effect of overnight nicotine abstinence on microvascular responsiveness.
The hypothesis was that 12 hours of nicotine abstinence might be sufficient to restore muscle microvascular responsiveness after snus portion administration. Indeed, nicotine, due to its sympathomimetic action, stimulates epinephrine and norepinephrine release, and enhances vasoconstriction by impairing endothelium-dependent and endothelium-independent vasodilation; it may therefore hinder tissue perfusion.9,10
In this randomized, controlled, within-subject design experiment study, we recruited 16 healthy male subjects who declared that they were regular current snus users (one or more sachets daily in the last 30 days). 11 Their ages ranged from 18 to 45 years. Exclusion criteria were the presence of symptomatic cardiopathy, metabolic disorders such as obesity (body mass index > 30) or diabetes, chronic obstructive pulmonary disease, hormonal therapy, epilepsy, alcoholism, and medications that would alter cardiovascular function. The participants’ characteristics were: age = 21.1 ± 2.7 years; height = 177.3 ± 5.8 cm; body weight = 76.3 ± 6.1 kg; snus portion per day = 8.1 ± 4.1 sachets (mean ± SD). Moreover, the mean age of the first snus experience of the participants was 16.6 ± 2.6 years (mean ± SD). The Ethics Committee for Clinical Trials, University of Verona, Italy (Prot. No. 9922, 55CESC) approved the study, which complied with the principles of the 1964 Declaration of Helsinki. Informed consent was obtained for all participants. The study was a randomized, controlled, within-subject design, and the participants were tested in two separate sessions, under each of the following experimental conditions: nicotine satiety and after a 12-hour overnight nicotine abstinence.
Prior to each session, a 5 mL blood sample was taken from each participant on arrival at the lab, and the satiety or abstinence condition was confirmed by chromatographic analysis of nicotine and cotinine. Each participant was then administered a 1 g portion of Catch Eucalyptus White Portion Snus, a commercial snus produced by Swedish Match (Stockholm, Sweden),7,8 after which we immediately measured their dynamic Ox% response at the level of the thigh muscle. This was done by measuring, by means of NIRS, changes in O2Hb, HHb, and THb concentrations during a standardized VOT. 12 The VOT is an ischaemia–reperfusion test in which a pneumatic tourniquet is inflated rapidly (from 0 to 350 mmHg in < 1 second) in order to achieve transient vascular occlusion. Thereafter, Ox% is measured, for a fixed 5-minute interval, at a site distal to the occlusion. After the 5-minute period has elapsed, the occlusion is reversed through rapid deflation of the tourniquet (< 0.3 seconds) and the Ox% is allowed to recover. Several parameters are then measured, including the rate of deoxygenation (Slope 1), which reflects the local metabolic rate, and the rate of reoxygenation (Slope 2) (i.e. the time necessary to clear the accumulated blood metabolites). The post-obstruction hyperaemic response is shown by the Ox% peak value (Max) (Figure 1). The VOT involved applying an adult-size tourniquet cuff on the right thigh and the NIRS probe on the right vastus lateralis.
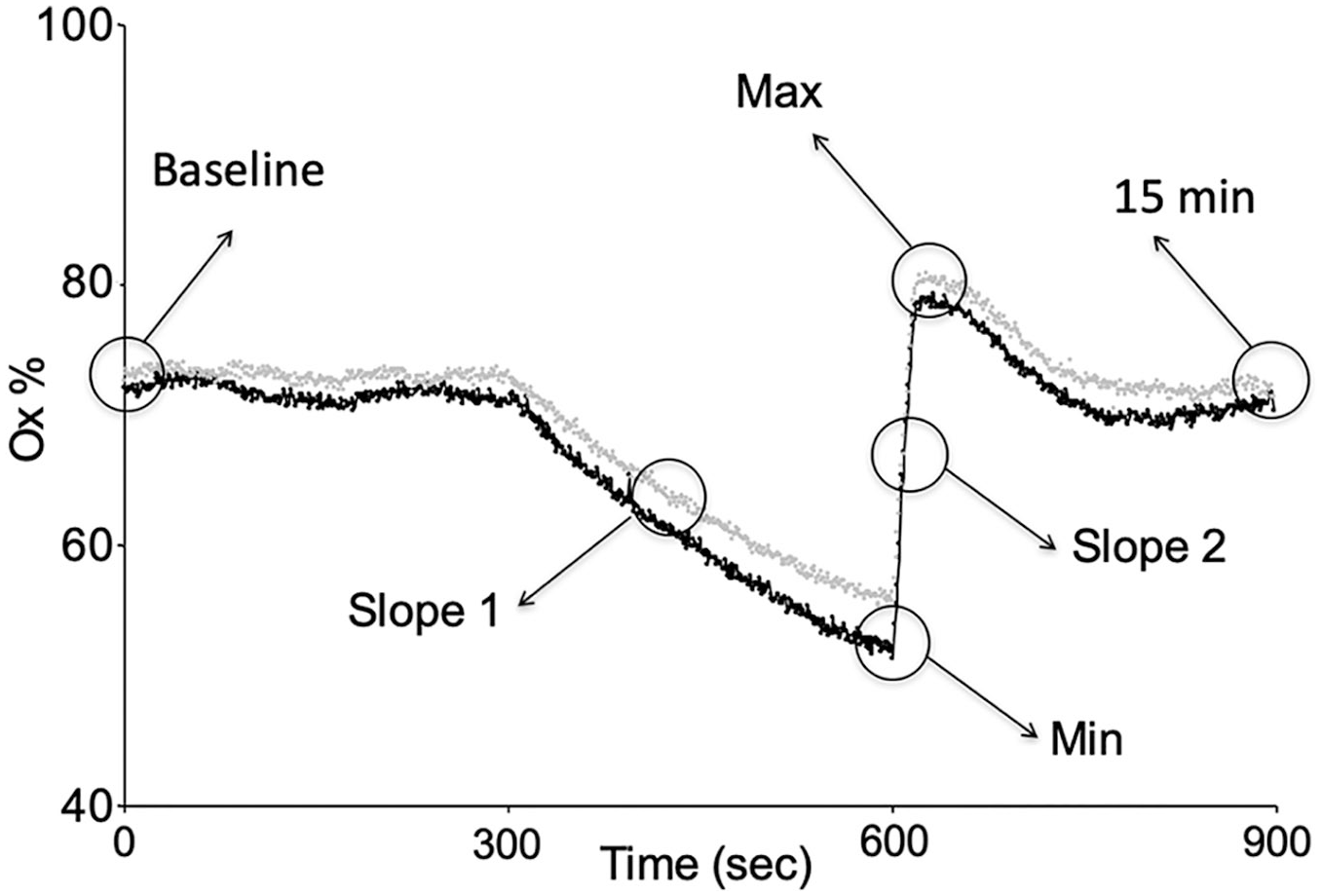
NIRS muscular values during the VOT.
The data are presented as mean values ± SD. All data were tested for normality using the D’Agostino–Pearson normality test. To compare the study variables, a paired Student’s t-test or Mann–Whitney U-test was applied as appropriate. A p-value < 0.05 was taken as the level of statistical significance. Data analysis was performed using GraphPad Prism 6 (GraphPad Software Inc., San Diego, CA, USA).
No significant difference in the average baseline Ox% value (T0) was found between the abstinence (72.55 ± 7.34%) and satiety (68.58 ± 6.40%) (p = 0.1475) conditions. Instead, the lowest Ox% value (Min) was, on average, significantly higher in abstinence (54.45 ± 11.30%) than in satiety (48.33 ± 10.03%) (p = 0.0146). Moreover, the average Ox% peak value (Max) was significantly higher in abstinence (81.90 ± 6.47%) than in satiety (77.37 ± 5.77%) (p = 0.0011). The average Ox% value at the VOT endpoint (15 minutes) was significantly higher in the abstinence (72.15 ± 7.12%) versus the satiety (67.45 ± 6.45%) condition (p = 0.0016).
The results of this study showed that a 12-hour overnight nicotine abstinence in snus users affected the post-obstruction hyperaemic response, given that the Ox% peak value was, on average, 6% higher in the abstinence condition, in which, moreover, Ox% remained elevated at the test endpoint. Conversely, the deoxygenation (Slope 1) and reoxygenation rates (Slope 1 vs Slope 2) did not differ significantly between the two conditions. The results of this novel study on vascular occlusion in smokeless tobacco users are important since they suggest that even a short period of abstinence from nicotine intake may improve the functional microvascular response in muscles, at least at rest.
Our participants consumed an average of eight por-tions daily. Each 1 g snus portion contains from 8.7 mg to 14.67 mg nicotine.13,14 Whereas only 10–20% of the nicotine existent in snus is absorbed via the mucous membrane and reaches the systemic circulation, participants used at least 10–15 mg of nicotine daily as a dose-dependent response. Moreover, at baseline, the chromatographic analysis confirmed the absence of nicotine in the abstinence condition (abstinence: 0.9 ± 0.4 ng/ml; satiety: 9.6 ± 2.8 ng/ml (mean ± SD); p = 0.0005). Therefore, if, according to Zamparini et al., 4 the absolute values of tissue oxygen saturation measured by NIRS in young healthy volunteers did not real any difference between smokers and non-smokers during a VOT, the improvement shown in our study on the functional microvascular response in muscles in the abstinence condition might be induced by a dose-dependent response.
This study is not free of limitations. First, our data should be taken with caution because we could not demonstrate a longer period of abstinence for vascular responsiveness due to the absence of complete nicotine washout (longer than 12 hours). Second, the absence of women in this study does not allow a comparison of the hyperaemic responses between sexes. Future research might clarify whether abstinence can restore microvascular responsiveness to vasoactive stimuli after a period of long-term nicotine abstinence – during exercise and in the female population. Were this found to be the case, it might encourage nicotine-addicted athletes to consider stopping the use of nicotine products in order to protect their health. 15
Footnotes
Acknowledgements
The authors warmly thank the volunteers without whom this study would not have been possible.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
