Abstract

Keywords
Introduction
Hypertension, or high blood pressure, is a common health condition that increases the risk of heart attack, heart failure, stroke, abdominal aortic aneurysm, peripheral artery disease (PAD), and eye and kidney problems.
As blood flows through blood vessels, it exerts force against the vessel walls – that force is the blood pressure. Blood pressure is read as two numbers, in units of millimeters of mercury (mmHg): the systolic blood pressure (top number) and the diastolic blood pressure (bottom number). The systolic blood pressure is the higher number and indicates the blood vessel pressure when the heart muscle contracts. The diastolic blood pressure indicates the blood vessel pressure when the heart relaxes between beats.
The risk of developing hypertension at some point within one’s lifetime is about 90% in the US. 1 A single elevated blood pressure reading does not necessarily indicate hypertension; rather, hypertension is diagnosed when the blood pressure is elevated above goal on at least two separate occasions (using an average of at least two readings).
What causes hypertension?
Blood pressure tends to increase with age. Hypertension that develops over time without any particular known cause is called primary, or essential, hypertension. This primary (essential) hypertension is the most common type. However, there are multiple causes of hypertension, and patients frequently have more than one contributing factor.
When other known factors cause or worsen hypertension, these are called secondary causes. The secondary causes of hypertension include certain common medications, as shown in Table 1.
Hypertension: causes and contributing factors.
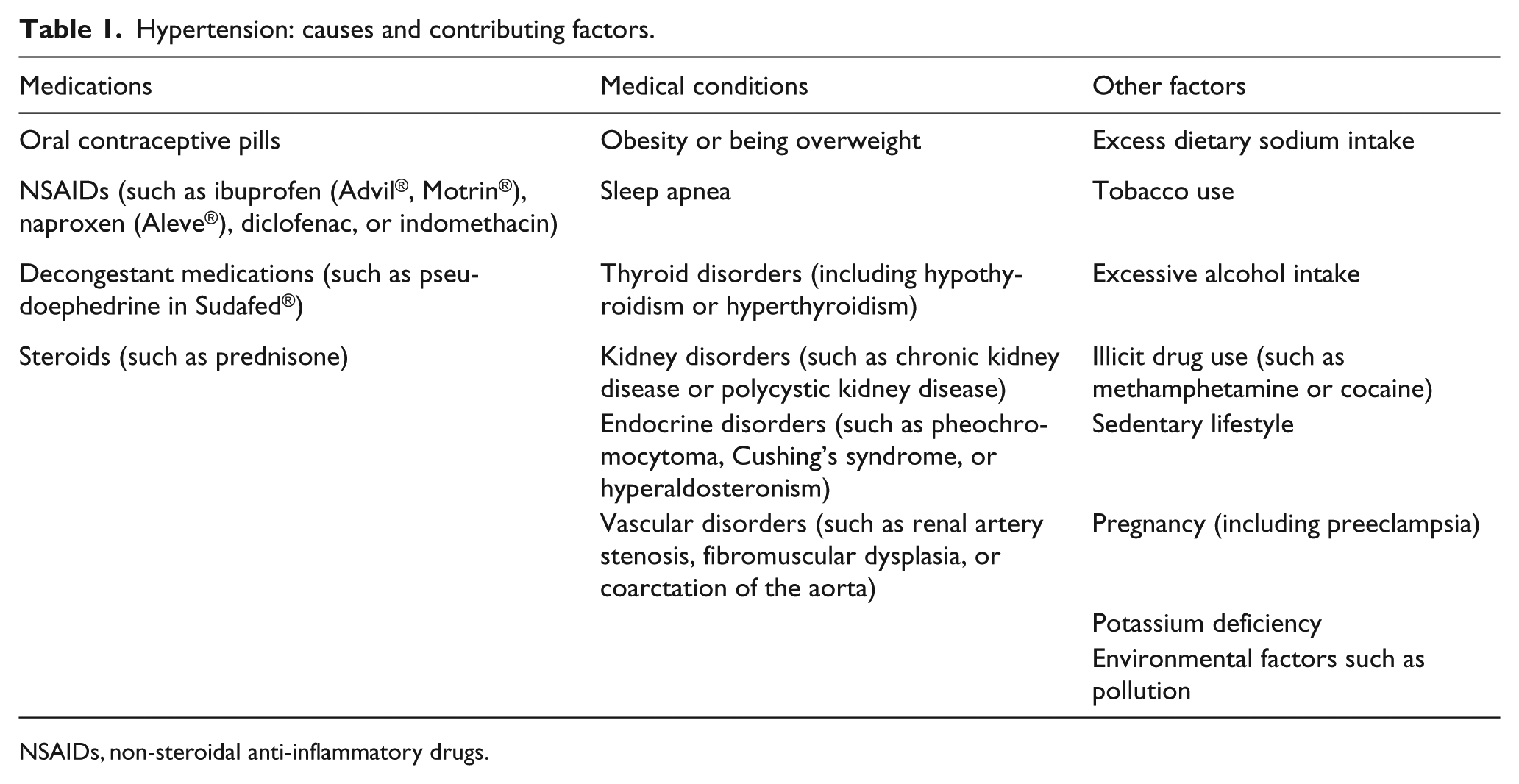
NSAIDs, non-steroidal anti-inflammatory drugs.
Having a family history, either of hypertension itself or of other contributing conditions, is also linked to the development of hypertension.
What other tests may be ordered when hypertension is diagnosed?
When a health care provider diagnoses hypertension, a few additional tests are commonly ordered to evaluate for related conditions.
Blood tests are usually checked, including electrolyte levels (sodium, potassium, chloride, and bicarbonate), as well as lipids (cholesterol), blood sugar, and basic kidney function and thyroid function tests. Urine tests are helpful to check for kidney damage.
An electrocardiogram (EKG) is a non-invasive test to evaluate the heart rhythm along with other features of heart function; it can be done in the office in a couple of minutes. If there is a strong suspicion for primary hypertension, these basic tests are usually all that is needed. If there is concern for secondary hypertension, additional tests may be ordered to find and treat the cause.
What are the risks of having hypertension?
Hypertension is sometimes called a ‘silent killer’ because although it increases the risk of heart attack, stroke, and other medical problems, the hypertension itself often causes no early warning symptoms. When there are no symptoms, measuring the blood pressure is the only way to know if it is too high.
High blood pressure affects blood vessels throughout the body, and can therefore cause problems in multiple areas. Hypertension increases the risk of heart disease, including coronary artery disease, which can lead to a heart attack. Pumping against elevated pressure can lead to abnormal thickening of the heart muscle (left ventricular hypertrophy), which can lead to heart failure.
The blood vessels in the brain are also affected by high blood pressure, increasing the risk of stroke. The kidneys carry many blood vessels, so another common result of ongoing hypertension is kidney disease or kidney failure. High blood pressure can affect the retina (the back of the eye) over time, leading to problems with vision.
Does salt (sodium) affect blood pressure?
Yes. Within the body, an increase in sodium intake leads to an increase in fluid retention. When excess fluid is retained in blood vessels, blood pressure tends to increase. High amounts of sodium can be found in packaged and processed foods, such as frozen foods, deli meats, canned soups, and in many restaurant meals. The intake of salt (which includes sodium) tends to be quite high in the average American diet; this increases blood pressure and can worsen hypertension.
What lifestyle changes can help lower blood pressure?
Leading a healthy lifestyle is vital in the prevention and treatment of high blood pressure. Lifestyle changes can be helpful regardless of whether a patient also requires medication to treat hypertension.
Quitting smoking is one of the most important steps toward controlling blood pressure and improving overall health. 2 Resources (including advice, support, and medications) are available through health care providers and the 1-800-QUIT-NOW hotline.
Regular exercise and avoiding a sedentary lifestyle both help maintain healthy blood pressure. All adults need a minimum of 30 minutes per day of brisk exercise based on current guidelines. Brisk walking, jogging, or biking are good options. Small steps, such as taking the stairs instead of the elevator daily, can help improve cardiovascular health. Scheduling exercise with a friend or family member may make a plan easier to maintain.
Nutrition and diet play an important role in maintaining a healthy blood pressure and weight. A research-based nutrition plan known as the DASH diet (Dietary Approaches to Stop Hypertension) is an overall healthy diet, and is especially recommended for patients with hypertension. The DASH diet emphasizes reduced sodium intake – between 1500 and 2300 mg per day at most. 3 As a reference, 1500 mg of sodium is about ¾ of a teaspoon. Checking nutrition labels (with close attention to the serving size per package) can be helpful to keep track of sodium intake. The DASH diet is high in vegetables, fruits, low-fat dairy, and whole grains, and is very limited in sugary foods and drinks, trans and saturated fats, and red meat. 3
If alcohol is consumed, it should be no more than one drink per day for women or two drinks per day for men. Excess alcohol intake can contribute to hypertension and cause other health problems; it also adds extra calories to the diet.
Maintaining a healthy weight can improve blood pressure. If a patient is overweight or obese (by body mass index), losing even 10% of body weight by modifying diet and increasing physical activity can improve blood pressure and health. Small daily changes, such as trading out sugary sodas for water, or taking a brisk, 30-minute walk after dinner, can add up to noticeable health benefits.
What are the medication options for hypertension?
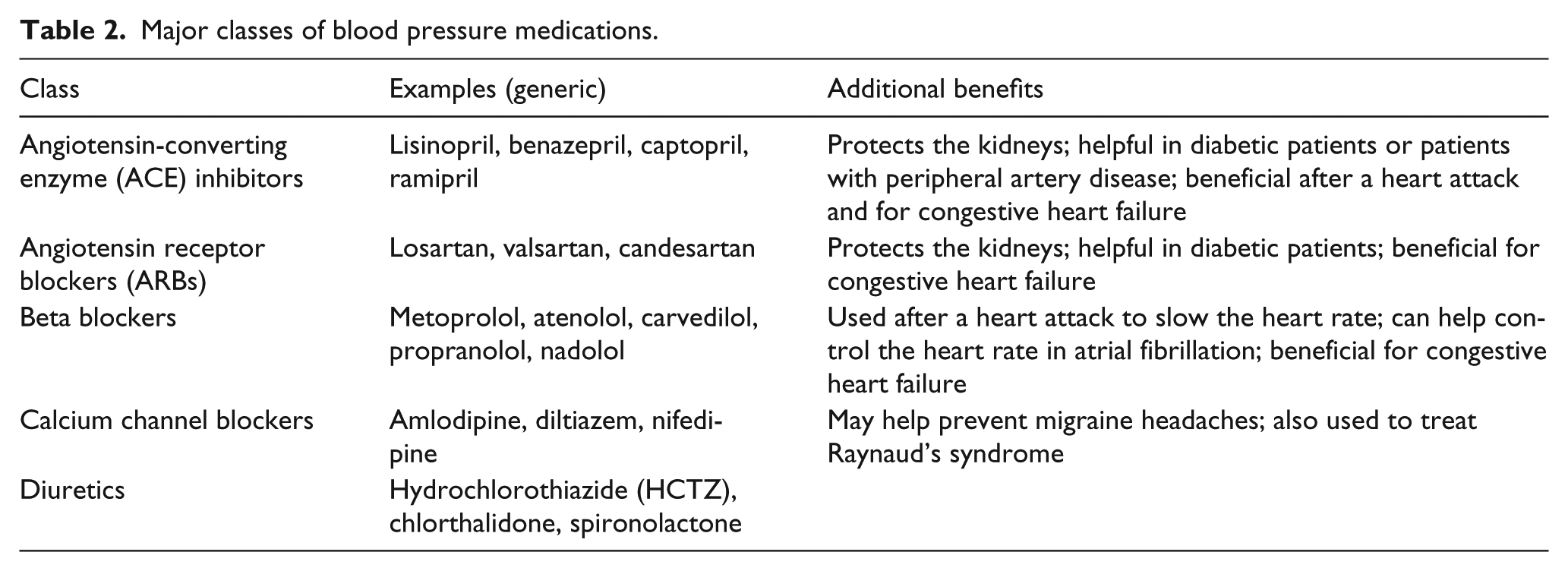
Several classes (types) of medications are used to treat hypertension, and they each work differently. There are a few similar medications within each class. The most commonly prescribed classes of blood pressure medications include diuretics (‘water pills’), angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), calcium channel blockers, and beta blockers, as shown in Table 2. Some of these medications have shown benefits beyond lowering blood pressure. ACE inhibitors and ARBs are closely related; sometimes patients are switched to an ARB if a cough develops with the ACE inhibitor. Other classes of medications, such as vasodilators or alpha blockers, are less commonly used.
Major classes of blood pressure medications.
Which medication is best for hypertension?
The most important consideration in the treatment of hypertension is simply to lower the blood pressure. Most patients require multiple medications in combination to achieve this goal – combining medications that act in different ways attacks the problem from multiple angles.
Adherence to the medication plan is extremely important, so medications with fewer side effects or that are taken just once a day may be preferable. The choice of medication is tailored to the individual patient. Response to the different medication classes can vary, and some blood pressure medications have additional benefits, shown in Table 2.
If a patient has a low potassium level, then supplementing this electrolyte under guidance from a health care provider may help. Otherwise, alternative treatments such as vitamins, minerals, and herbal supplements are not effective substitutes for lifestyle change and prescription medication for hypertension treatment. Some alternative treatments can cause harmful side effects or interfere with other medications. Dietary supplements are not reviewed by the US Food and Drug Administration (FDA) for efficacy, and are not regulated for safety by the same rigorous standards as medications. More research is needed to evaluate for potential benefits from herbal supplements in hypertension.
What are the most common side effects of hypertension medications?
Medications for hypertension are usually well tolerated, causing no side effects at all. Any blood pressure medication could cause the blood pressure to go too low, which may cause light-headedness. Beta blockers can worsen asthma, and could cause the heart rate to go too low, which may also cause light-headedness. About 10% of people who take ACE inhibitors may develop a dry cough. Calcium channel blockers can cause constipation or leg swelling. Diuretics increase urination (reducing sodium and fluid in the body), which could lead to dehydration, worsen gout, or cause leg cramps due to electrolyte changes.
If side effects occur, the prescribing provider should be notified so the medication can be adjusted or changed.
What is the ideal blood pressure goal?
A normal blood pressure is under 120/80 mmHg. However, the ideal goal blood pressure is somewhat controversial, and depends on each patient’s health and additional risk factors.
A few years ago, the JNC 8 (Joint National Committee) guidelines recommended slightly less strict control of blood pressure based on available research. JNC 8 recommended a goal of less than 150/90 mmHg for people aged 60 years or older. 4 They recommended a lower goal of 140/90 mmHg for patients under age 60 and for all patients with diabetes or chronic kidney disease. 4
In contrast, a more recent study called SPRINT looked at patients over age 50 who did not have diabetes, but who were at high risk for cardiovascular events such as heart attacks. The investigators found that treating patients to a lower systolic blood pressure of 120 mmHg (rather than 140 mmHg) showed a benefit in terms of fewer adverse outcomes, such as heart attacks or death. 5
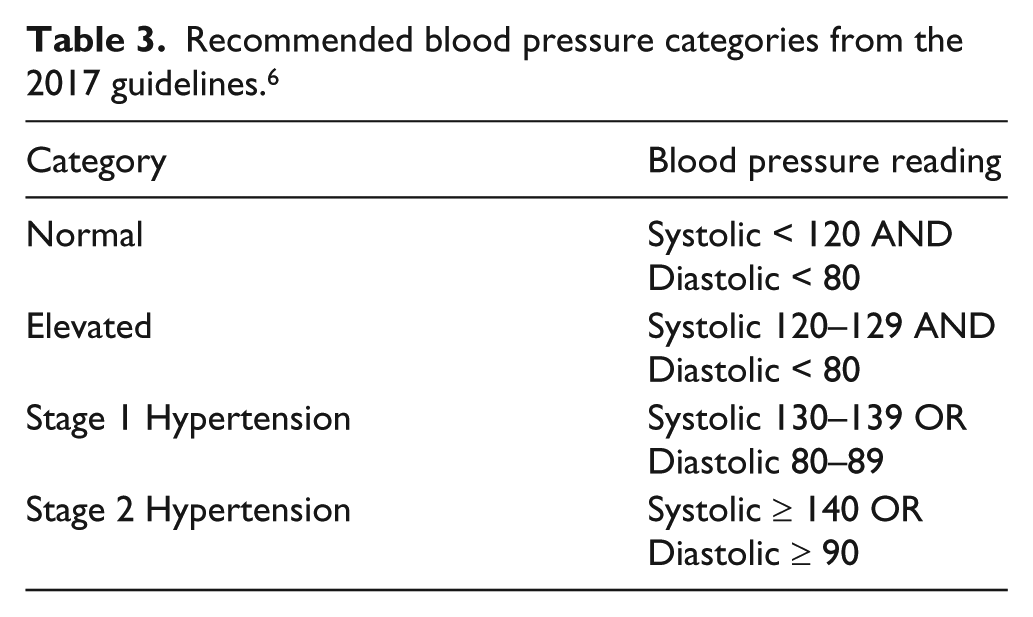
Taking into account prior research and the SPRINT study, new hypertension guidelines from collaborating medical societies were issued in 2017. 6 The new terminology for categorizing blood pressure is shown in Table 3. Based on the 2017 recommendations, the new target blood pressure is less than 130/80 mmHg for patients with cardiovascular disease, diabetes, or chronic kidney disease.
Recommended blood pressure categories from the 2017 guidelines. 6
While treating high blood pressure is important and reduces the risk of many adverse health outcomes, it is also important to avoid dropping the blood pressure too low, because overly low blood pressure may lead to dizziness or fainting.
Decisions about blood pressure goals should be made together with a health care provider, taking overall health and risk factors into consideration.
What about white coat hypertension? Should blood pressure be checked at home?
The term ‘white coat hypertension’ is used when the blood pressure is consistently high in the doctor’s office but is not elevated when checked at home or outside the office. White coat hypertension indicates an increased risk of developing hypertension.
Blood pressure can fluctuate throughout the day, and in-office readings may not reveal the pattern of blood pressures during an average day at home or work. Measuring blood pressure at home can be helpful for a more accurate assessment and can help with medication adjustments. For example, if medications are taken in the morning and the blood pressure drops low at 10:00 but then increases before bedtime, it may make sense to move one of the medications to the evening.
Keeping a log of home measurements to share with a health care provider, whether on paper or through a digital application, can help determine the blood pressure pattern and the best timing for medications.
What is the best method to check blood pressure at home?
Blood pressure measurements should be taken after at least a 5-minute period of quiet rest. Alcohol, caffeine, tobacco, and exercise should be avoided for 30 minutes prior to the measurement. As illustrated in Figure 1, both feet should be flat on the ground (not crossed) with the back supported in a chair and the arm resting on a table, with the upper arm at the level of the heart. Talking should be avoided while the measurement is being taken.

Correct positioning for blood pressure measurement.
It is important to use the correct blood pressure cuff size for a given patient’s arm size. Using a cuff that is too large or small can make the readings inaccurate. Taking at least two measurements, at least a minute apart, is helpful to ensure consistent readings, particularly when one measurement seems unusually high or low.
A small difference of less than 10–12 mmHg between the left and right arms is not a cause for concern. Differences in measurements are also common in patients with atrial fibrillation due to the variability in the heart rate. The higher of the two arm pressures should be used to guide the blood pressure medication management. If a large difference is noted, then a health care provider should be notified, as it may be a sign of PAD in the arms.
Blood pressure monitors that use a wrist cuff rather than an arm cuff are also available, but may be less reliable. The wrist must be kept at the level of the heart because these devices can produce more variable measurements based on body position. Bringing a home blood pressure device to a physician’s office is a good way to compare readings and determine whether they are consistent.
An even more accurate way to assess hypertension is with 24-hour ambulatory blood pressure monitoring (ABPM). ABPM is accomplished via a small device worn at home throughout the day and night and interpreted later by a physician. The cuff automatically measures blood pressure at certain intervals during daily life. Some patients have high blood pressure readings only in the office (‘white coat hypertension’) or only while at home (‘masked hypertension’). ABPM can provide a more detailed view of how the blood pressure varies at home to tailor treatment.
Summary
Hypertension is a common problem. Fortunately, it is treatable with lifestyle changes and with medication.
Leaving high blood pressure elevated without adequate treatment carries many health risks, including stroke, heart attack, heart failure, blood vessel disease, and kidney failure. Therefore, it is extremely important to take medications daily as prescribed. Keeping a log of home blood pressure measurements can be helpful, and may be more accurate than measurements taken in the clinic under stress.
Controlling blood pressure is key in maintaining good overall cardiovascular health.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
