Abstract

What is carotid artery disease?
Carotid artery disease is narrowing of the large arteries of the neck (carotid arteries), which are the main blood vessels that supply oxygen-rich blood to the brain. The narrowing is usually caused by atherosclerotic plaque. Atherosclerosis, or hardening of the arteries, can affect arteries throughout the body. When the neck arteries are narrowed or blocked, the condition is called carotid artery disease or carotid artery stenosis.
Who is at risk for carotid artery disease?
The conditions that increase the chances of a disease are called risk factors. The risk factors for carotid artery disease are similar to the risk factors for coronary heart disease. Carotid artery disease becomes more common with age. Other risk factors for atherosclerosis include diabetes, smoking, high blood pressure (hypertension), and high cholesterol. Having atherosclerosis (plaque) in other areas of the body, such as in the coronary or leg arteries (known as peripheral artery disease), also increases the risk of carotid artery disease.
Does carotid artery disease cause symptoms?
The large majority of people with plaque in the carotid arteries have no symptoms. If the carotid arteries are severely narrowed, tiny pieces of plaque may break off and go to the brain, which can cause sudden vision loss, a stroke, or a transient ischemic attack (TIA). A TIA, often called a mini-stroke, is like a stroke except that the symptoms resolve within 24 hours.
If you suspect that you or someone you know is having a stroke, you should call an ambulance right away. Warning signs of a stroke can be remembered with the abbreviation
Signs and symptoms of stroke.
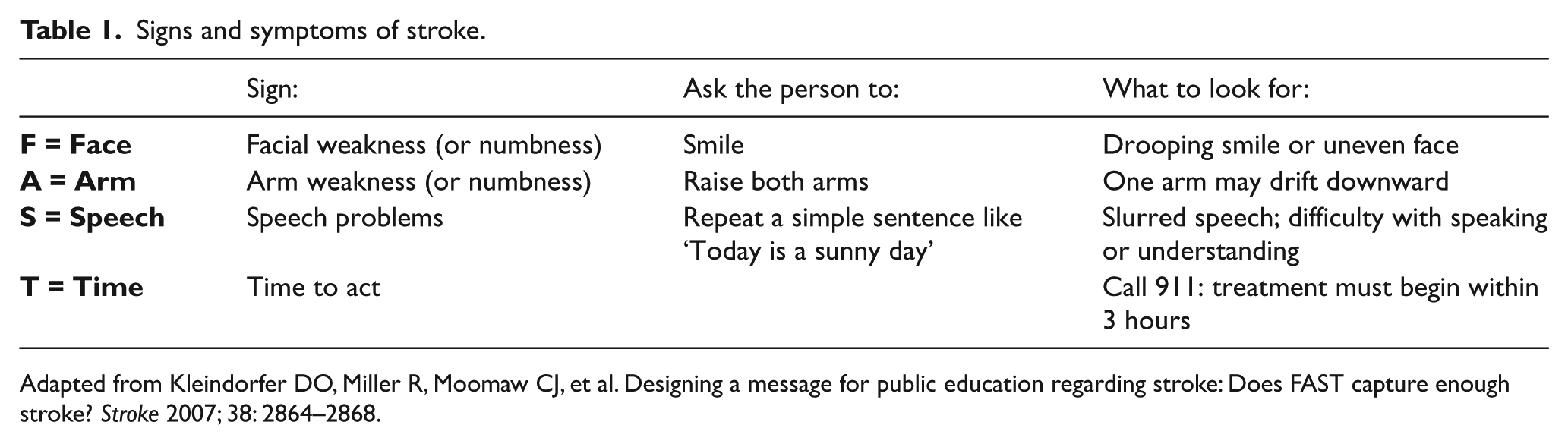

Adapted from Kleindorfer DO, Miller R, Moomaw CJ, et al. Designing a message for public education regarding stroke: Does FAST capture enough stroke? Stroke 2007; 38: 2864–2868.
How is carotid artery disease diagnosed?
Your health care provider may listen to your neck with a stethoscope (Figure 1). A whooshing sound heard over an artery is called a bruit (pronounced BREW-ee). Bruit is the French word for noise. If a bruit is heard in the neck, then a carotid ultrasound is often recommended. A bruit simply suggests that the blood flow may be turbulent but it does not necessarily mean the artery is blocked. It is possible to have carotid artery disease without having a bruit heard in the neck.
Listening for a bruit. Your health care provider may listen to the neck with a stethoscope.
The simplest way to diagnose carotid artery disease is with a carotid ultrasound (or ‘Doppler’). This non-invasive, painless test uses high-frequency sound waves to look inside the neck arteries. Conducting gel is applied to the skin. The sonographer then uses a hand-held transducer to record images of the carotid arteries (Figure 2). Ultrasound is used to visualize the atherosclerotic plaque and to determine if plaque is interfering with the blood flow through the arteries. When the artery is narrowed, the velocity of the blood flow increases just like when a thumb is placed over the end of a garden hose. With ultrasound, the degree of blockage (stenosis) can be estimated by measuring the speed of the blood flow. No special preparation is needed for a carotid ultrasound.
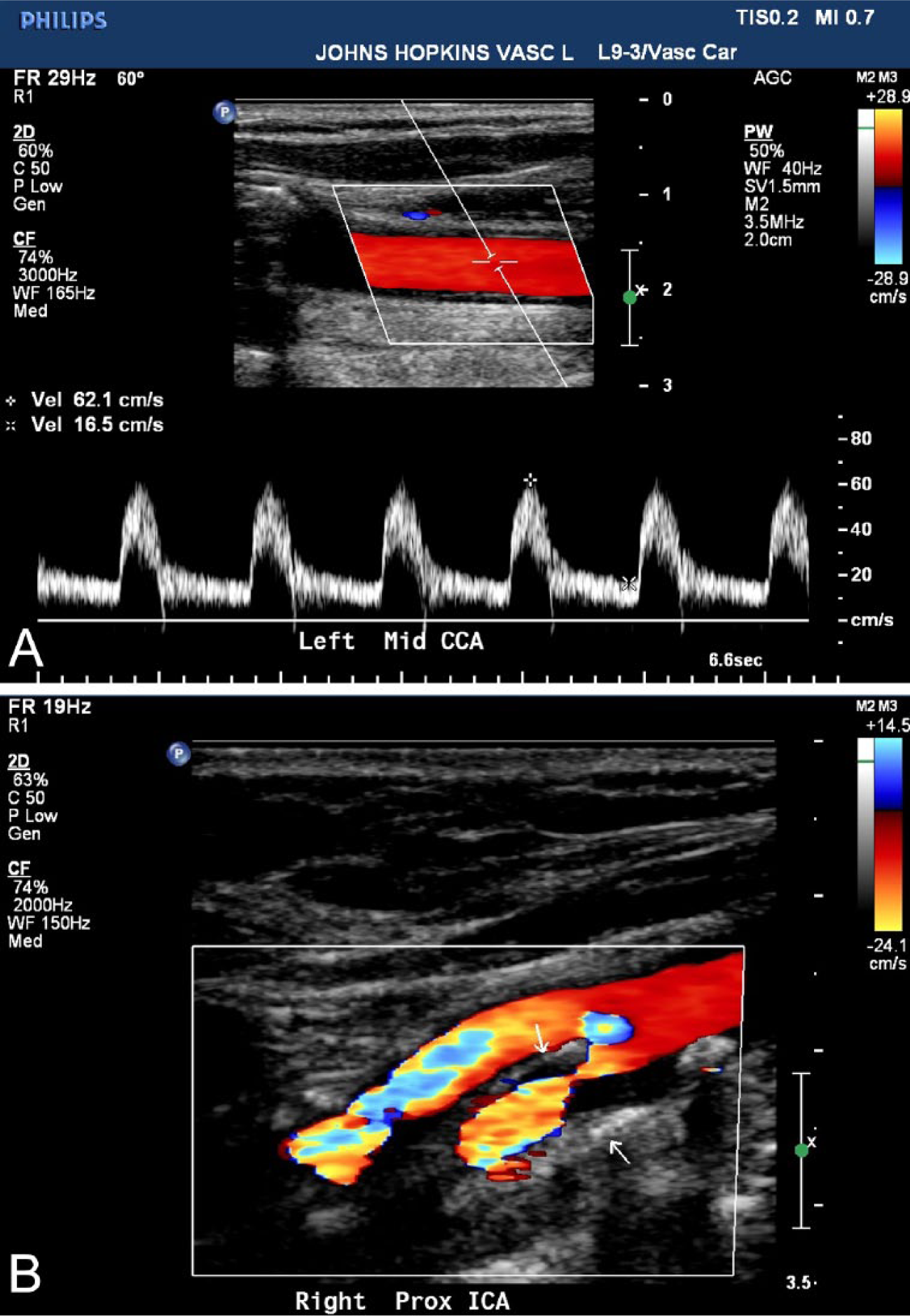
Carotid artery ultrasound. Panel A illustrates normal blood flow through the left common carotid artery. The patient’s head is to the left of the screen, and the feet are to the right. Panel B shows severe narrowing of the right internal carotid artery. There is plaque in the artery (arrows), and the flow is turbulent.
If significant blockage is seen on the carotid ultrasound, a vascular specialist may order other tests to confirm the location and severity of the carotid artery disease. These tests may include a CTA (computed tomographic angiography) or MRA (magnetic resonance angiography). An example of a CTA is shown in Figure 3.
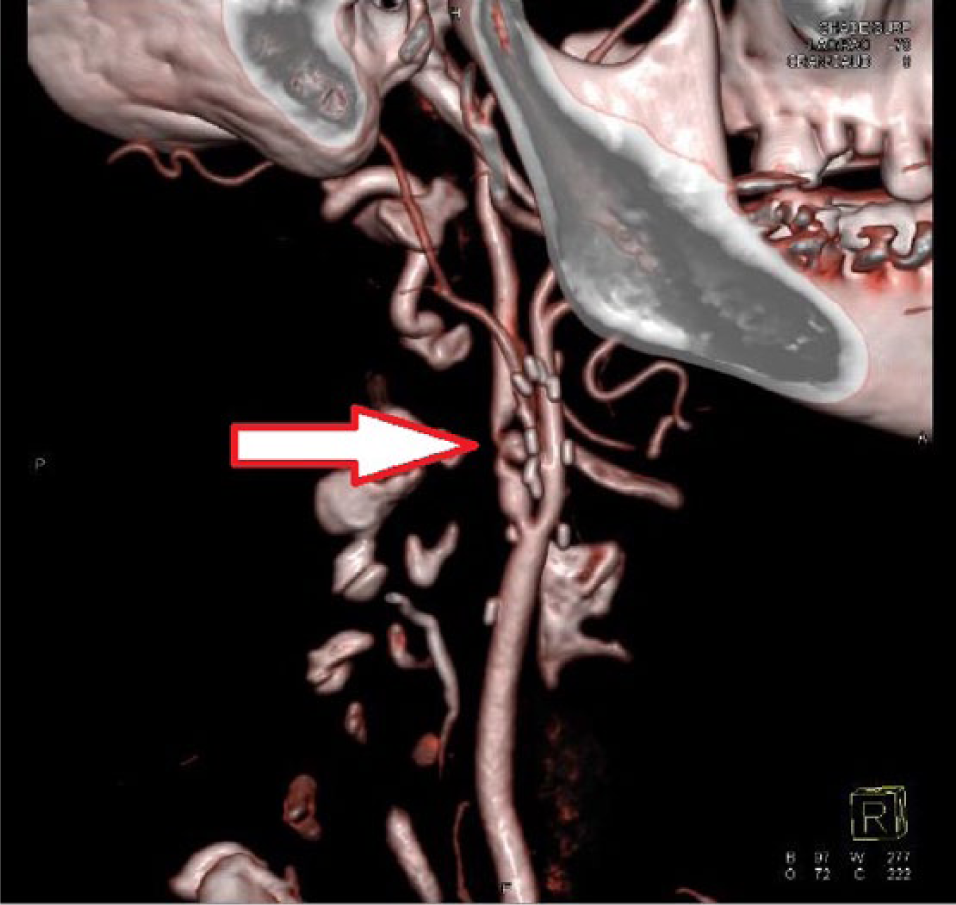
Computed tomographic angiography (CTA). Detailed images of the blood vessels are helpful when planning a procedure to treat severe carotid artery disease. This CTA image shows severe narrowing of the right internal carotid artery (arrow).
How is carotid artery disease treated?
The primary goal in treating carotid artery disease is prevention of stroke. Most of the time, carotid artery disease can be treated with a combination of medications which help stabilize the plaque and prevent further blockage, thus lowering the risk of stroke. If the carotid artery is severely narrowed, a vascular specialist may also recommend surgery or a stent, depending on the patient’s overall health status and other medical issues. Surgery on the carotid artery is called a carotid endarterectomy (CEA). An incision is made in the neck, and the plaque in the artery is removed. Carotid angioplasty with stenting is another alternative to restore the blood flow. Angioplasty with a balloon is used to clear the blockages, and a metal strut called a stent is inserted to prop open the vessel. Patients are typically in the hospital for one night after either procedure. Research studies have compared surgery (endarterectomy) versus a stent for carotid artery disease, and they are generally equivalent but may have different associated risks. Thus, the choice should be customized to the individual patient by a vascular specialist. Overall, the benefit of restoring carotid artery blood flow is much greater in patients who have had recent neurologic symptoms such as a TIA or stroke. After the surgery or stent, periodic ultrasounds are important to make sure the blockage does not recur and also to monitor the carotid artery on the other side.
What are the medical treatments for carotid artery disease?
Carotid artery disease indicates atherosclerosis, which means a higher risk of heart attack and stroke. Even if the blockage in the artery is not severe enough to require surgery or a stent, all patients with carotid artery disease need medical treatment for atherosclerosis. Medical treatment focuses on reducing cardiovascular risk. Table 2 lists key recommendations in the medical treatment of atherosclerosis.
Medical treatment of carotid artery disease.

A blood-thinning medication such as aspirin and a ‘statin’ cholesterol-lowering medication (such as atorvastatin, rosuvastatin, or simvastatin) are usually prescribed to reduce the risk of heart attack and stroke. Quitting smoking is absolutely essential. Smoking cessation resources include medications (varenicline or bupropion), nicotine replacement, counseling, and hotlines such as 1-800-QUIT-NOW (1-800-784-8669) in the US. High blood pressure and diabetes should be controlled. A blood pressure medication called an ACE-inhibitor (such as ramipril or lisinopril) or angiotensin receptor blocker may be prescribed. Studies suggest that statins, ACE-inhibitors, and regular exercise may also have beneficial effects on the walls of the carotid arteries, which could delay the progression of the plaque.
How can carotid artery disease be prevented?
Everyone can reduce their risk for cardiovascular disease by not smoking, maintaining a healthy body weight, and getting regular exercise: at least 30 minutes per day of exercise on most days of the week. Getting checked for high blood pressure, high cholesterol, and diabetes is also important.
Summary
Carotid artery disease, or narrowing of the neck arteries, is generally caused by atherosclerosis (plaque). Diagnosis is typically made by ultrasound. Medical treatment includes smoking cessation, medications aimed at preventing heart attack and stroke, and exercise. Patients with severe carotid artery disease (especially those with neurologic symptoms such as stroke or TIA) may need to undergo a procedure to restore the blood flow with either surgery or a stent.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
