Abstract

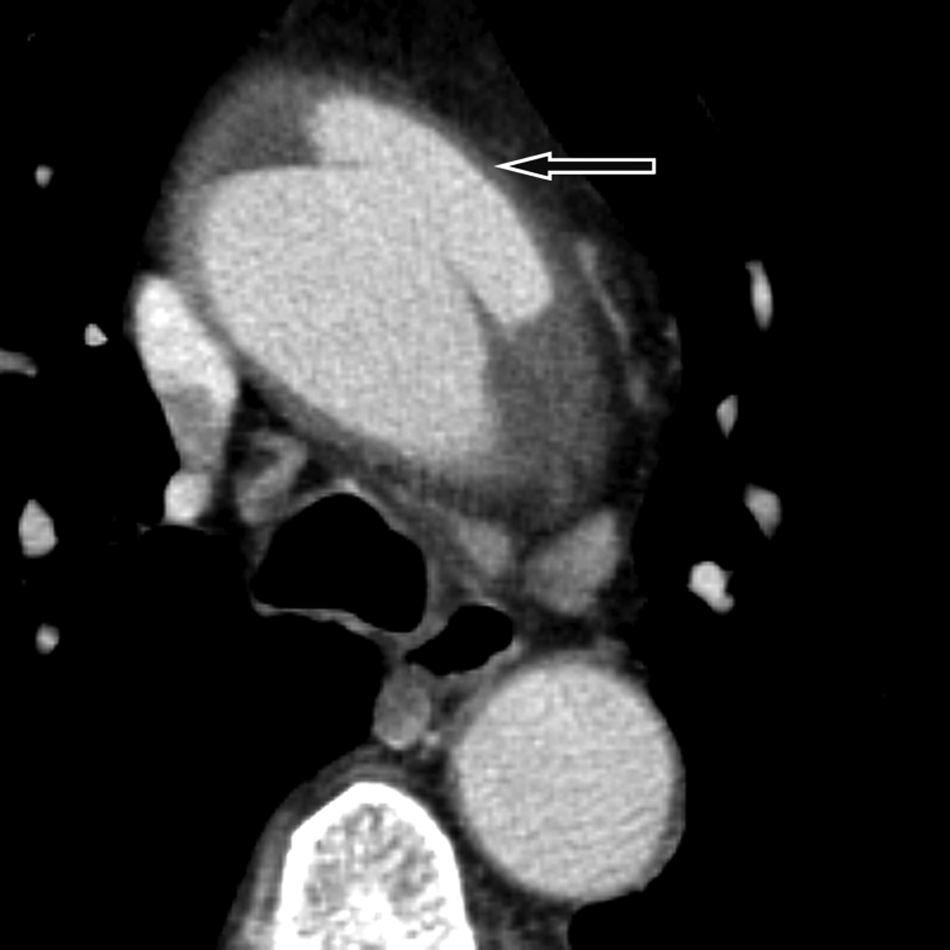
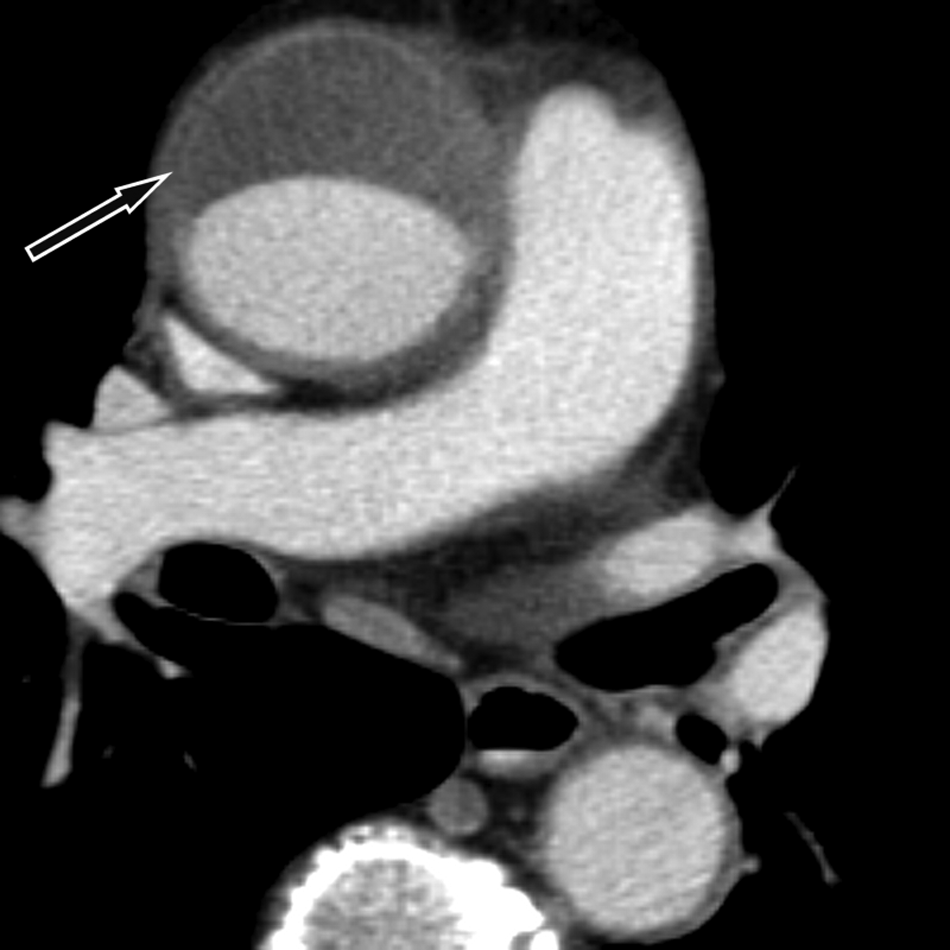
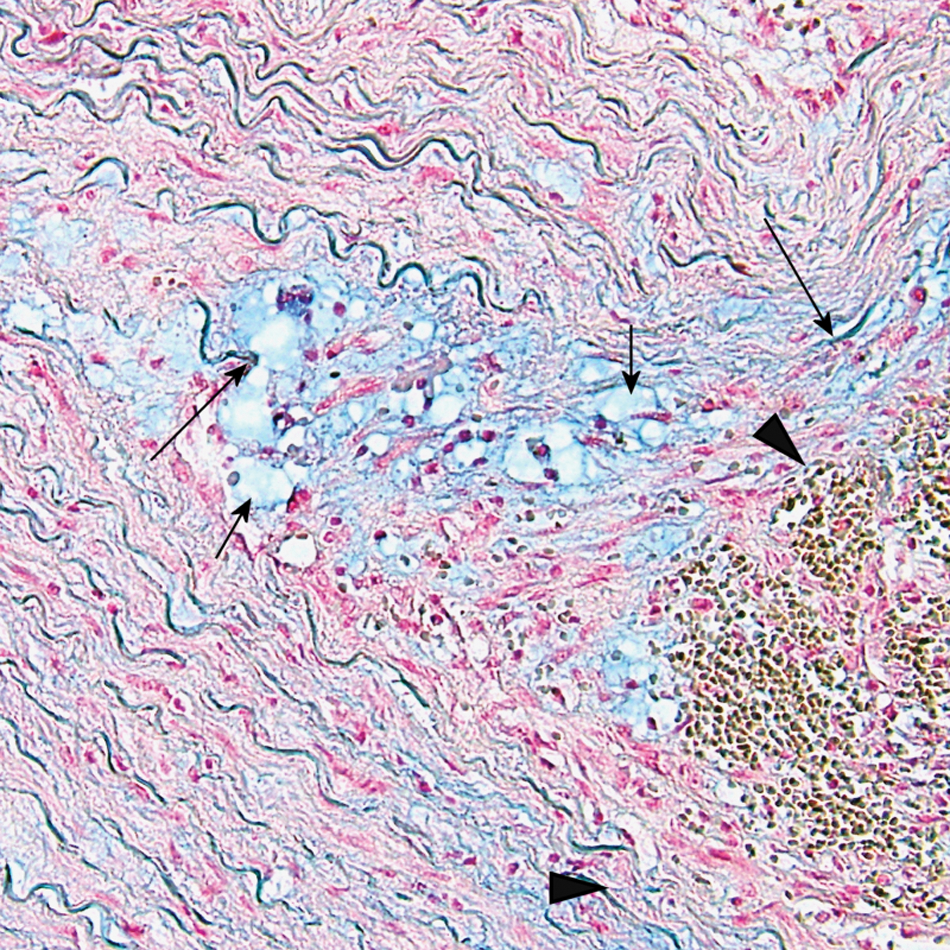
A 67-year-old man presented to the hospital after acute onset of chest pain. Echocardiography showed a pericardial effusion and an aortic dissection was suspected. Contrast-enhanced computed tomographic angiography depicted aneurysmal dilation of the ascending aorta measuring 5.5 cm in diameter. Furthermore, it revealed an intimal tear with outflow of contrast medium into the dissected anterior wall of the upper ascending aorta (Panel A1; arrow). This tear extended into an anterior intramural hematoma, reaching from the aortic arch to the aortic root (Panel A2; arrow). Pericardial effusion was also present. The arch vessels were not involved. Catheter angiography ruled out coronary artery disease and confirmed that the coronary arteries were neither dissected nor compressed by the intramural hematoma. The imaging findings were confirmed intraoperatively, including the intimal tear of the aortic dissection. On visual inspection, the aortic valve and orifices of the coronary arteries were normal. The supracoronary ascending aorta and inferior wall of the aortic arch were replaced by a vascular prothesis. Histology of the resected aortic wall revealed a medial degeneration (previously termed ‘cystic medial necrosis’). 1 Tissue staining with Alcian-blue (Panel B) showed a hematoma within the dissected medial layer (arrowheads) and adjacent accumulation of extracellular proteoglycans (short arrows) with fragmentation of some elastic fibers (long arrows). The patient fully recovered without significant disability.
These images of an aortic dissection demonstrate that, on the basis of a pre-existing aortic wall disease, an intramural hematoma may be closely associated with an intimal tear. 1
‘Images in vascular medicine’ is a regular feature of Vascular Medicine. Readers may submit original, unpublished images related to clinical vascular medicine. Submissions may be sent to: Mark A Creager, Editor in Chief, Vascular Medicine, via the web-based submission system at http://mc.manuscriptcentral.com/vascular-medicine
Footnotes
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
