Abstract
Introduction
This paper estimates the effectiveness and cost-effectiveness of a Hospital in the Home (HITH) service using virtual care technology to provide home-based care for COVID-19 patients with moderate symptoms in Queensland, Australia.
Methods
A cohort study was conducted to analyse data of all patients admitted to the virtual COVID-19 HITH service between December 2021 and November 2022. A decision tree model was developed to compare of the cost-effectiveness of this service with a hypothetical usual care cohort admitted to a conventional physical ward from the perspective of the Australian health system. Comparator cohort data were sourced from published literature. Base-case analysis employed a 3-month time horizon with an additional lifetime scenario analysis. Quality-adjusted life-years (QALYs) were used as the measure of effectiveness. Sensitivity analyses were performed to assess the robustness of the model.
Results
The virtual COVID-19 HITH service saved 15,273 bed days. The cost-effectiveness analysis indicated the virtual COVID-19 HITH model was dominant, resulting in an additional 0.015 QALYs and a cost saving of $201 per patient compared to usual care. The incremental cost-effectiveness ratio was most sensitive to the cost of operating the virtual HITH. When all uncertainties were considered, there was 74% likelihood that the virtual HITH model of care was cost-effective, assuming a willingness to pay of $28,033/QALY.
Discussion
HITH services incorporating virtual care modalities replicating the systems, staffing, and daily routines of a hospital ward are likely to be an effective and cost-effective intervention to expand inpatient care capacity.
Introduction
Hospital in the Home (HITH) is an evidence-based model of care that provides home-based care for patients requiring clinical governance that would otherwise necessitate treatment in a traditional inpatient hospital bed. 1 It aims to address challenges related to bed blockage and hospital overcrowding, as receiving care at home may replace the need for admission or facilitate early discharge.2,3 The need for home-based healthcare delivery programs has escalated since the onset of the COVID-19 pandemic, which has seen increasing strain on hospital resources.4,5 Consequently, adopting a model of care that allows for the provision of symptomatic management at home for COVID-19 patients is important to mitigate nosocomial spread and reduce inpatient capacity strain.
The potential for HITH to increase health system capacity was explored during the COVID-19 pandemic, often through concepts such as ‘virtual wards’ and ‘remote home monitoring’.6–8 These services employed virtual care modalities to replicate the systems, staffing, and daily routines of a traditional hospital ward in treating COVID-19 patients. 9 However, there is limited evidence regarding patient safety and economic analyses for those services.3,6,9 To date, there have been no studies investigating the cost-effectiveness of a virtual HITH service for treating COVID-19 patients. Given the current policy emphasis on providing care closer to home10,11 and concerns about the increasing demand for hospital bed-based care,12,13 coupled with the substantial resources needed to establish home-based acute treatment services with virtual care technologies, it is important to understand the costs relative to health outcomes associated with these models of care.
This paper reports on patients’ health outcomes and an economic evaluation of a virtual COVID-19 HITH service in Queensland, Australia. We aimed to determine the effectiveness and cost-effectiveness of this virtual HITH service. Findings from this study may inform planning, implementation, and expansion of this virtual care-enabled HITH model into other clinical areas to increase inpatient care capacity.
Methods
This paper presents an observational retrospective cohort study of patients admitted to a virtual COVID-19 HITH service, and a modelled cost-utility analysis comparing this service to conventional inpatient care for a comparable cohort of patients. The study protocol was approved by West Moreton Human Research Ethics Committee (HREC/2023/QWMS/91529). We followed the ‘Consolidated Health Economic Evaluation Reporting Standards’ (CHEERS) checklist 14 for reporting.
The virtual COVID-19 HITH service
A virtual COVID-19 HITH service was provided by West Moreton Hospital and Health Service in Southeast Queensland, Australia as a scalable response to demand from COVID-19 surges. This service streams dedicated to support COVID-19 positive patients who had additional health concerns such as pregnancy or chronic conditions. Admission criteria followed Queensland Health HITH: During a pandemic Guideline. 15 In Queensland, HITH provides a comparable level of care to what provided in the inpatient in-hospital admitted care, which means without a HITH service, the patient would be admitted to a bed within the hospital setting for treatment as an inpatient. Admitted patients had to be medically stable, able to safely self-isolate at home, have an appropriate residence for home-based care (e.g. not cohabitating with individuals at high risk of complications), and have access to a telephone.
The service was rolled out on 19 December 2021, in preparation for the Queensland border opening amid the emerging surge of cases presenting with the Omicron variant. Admitted patients were contacted daily via phone or videoconference by a team of doctors and nurses to discuss the symptoms and any medications required. Oximeters and thermometers were provided to patients as needed. Patients were required to upload their observations into an online coordinator system, which were reviewed daily by a nurse for quick responses to any signs of deterioration. If an in-person review was necessary, patients were transferred to a physical ward at the hospital. The service also implemented a ‘whole family’ model, allowing parents and children to be supported under a single service.
Model structure
A decision tree model was developed using TreeAge Pro software 16 to perform a cost-utility analysis comparing the cost and health outcomes of the virtual COVID-19 HITH service with a clinically comparable, hypothetical usual care cohort. Usual care was defined as admission to a conventional physical ward for in-person acute care. A decision tree was considered the most appropriate model structure to reflect the relatively linear care pathway of COVID-19 hospital admissions, with a limited number of health states over a relatively short duration. 17
The model structure is outlined in Figure 1. Patient care pathways were modelled from an initial index admission to either a HITH ward or usual care ward, with potential outcomes including discharge, transfer to a physical ward (for HITH only), transfer to intensive care unit (ICU) (with subsequent transfer back to general ward included within this event), and death. The potential for 28-day readmissions was also accounted for. The model adopted a 3-month time horizon that was considered adequate to account for the course of the admission and any subsequent 28-day readmissions.
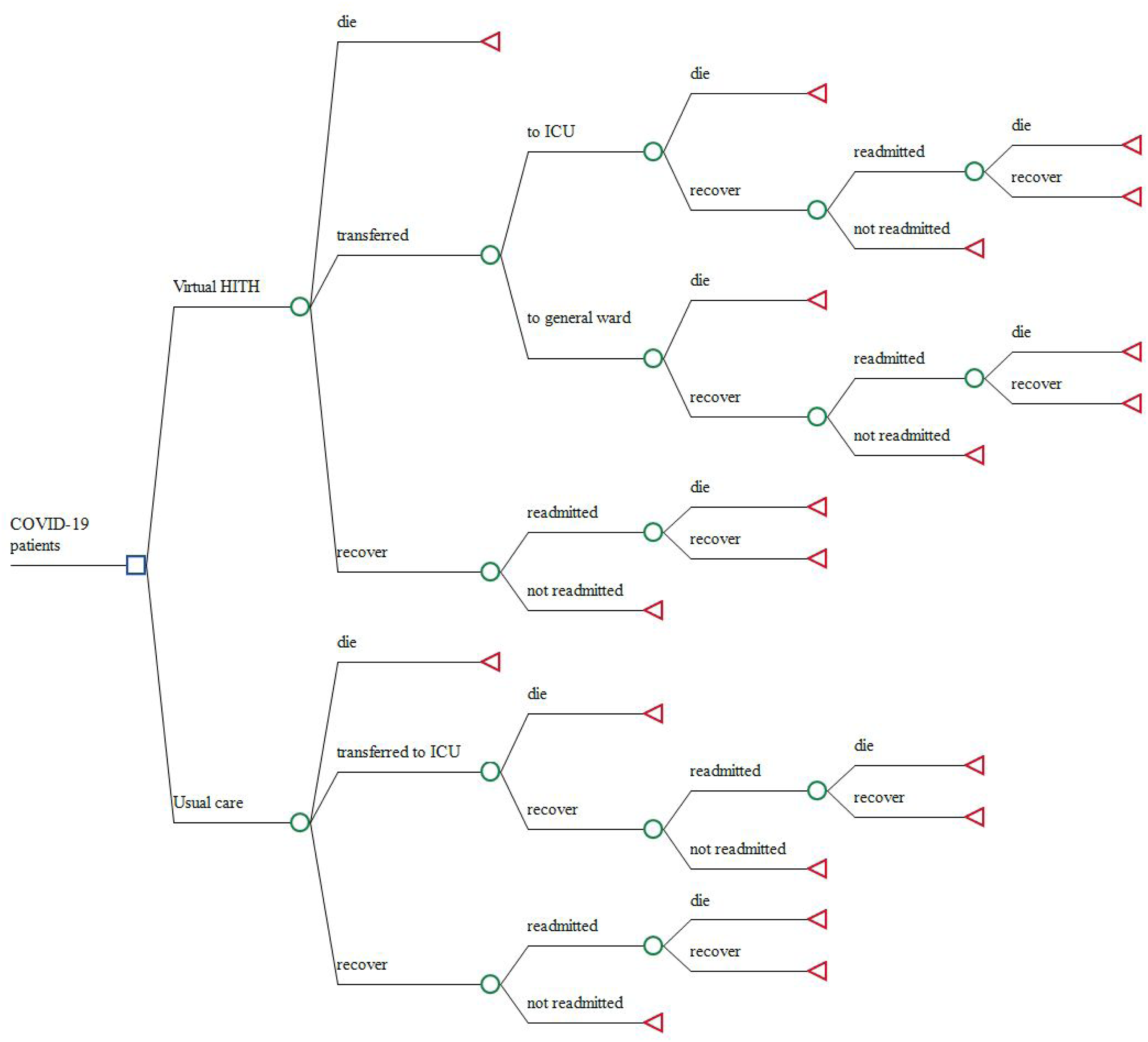
Decision tree of the virtual hospital in the home service and usual care for treating patients with COVID-19. HITH: Hospital in the Home; ICU: intensive care unit. Usual care is defined as admissions to a conventional physical ward for in-person acute care.
Data collection for the virtual COVID-19 HITH cohort
All patients admitted to the virtual COVID-19 HITH service from 19 December 2021 to 28 November 2022 were included in the cohort study. This period covers the initial rollout of the service until the last patients were discharged, as this dedicated service stream was subsequently decommissioned and absorbed into the regular workflows of the standard HITH service due to a decrease in COVID-19 referrals after the peak periods. De-identified patient data including demographic characteristics, service utilisation and clinical outcomes were extracted from routinely collected electronic health record system and hospital finance documentation. Outcomes included the length of stay (LOS), admission cost, ward transfer rate, discharge rate, readmission rate, and in-hospital mortality. Readmissions were defined as subsequent admissions to any hospital ward within 28-day of being discharged from the index admission to the HITH ward.
Total admission cost was estimated from program financial records, which included costs associated with general clinical and domestic supplies, computer-related services and equipment, pathology, and clinician time. An average cost per HITH bed day was assigned by dividing the annual program cost by the total number of patient bed days within a 12-month period. Individual HITH admissions were then costed by assigning the average bed day cost to the HITH episode LOS.
Model input parameters
The full set of model inputs along with their respective distribution and data sources are outlined in Table 1. Cost, LOS, and probabilities of transition between events in the HITH arm were informed by the cohort study described above. A literature review was conducted to inform parameter inputs in the usual care arm and utility values for each event in the whole patient care pathway. The search strategies (Supplementary 1, Table 1) were guided by the PICO (population/intervention/comparison/outcome) framework, aiming to identify a comparable cohort of COVID-19 patients admitted to a physical ward. To ensure relevance, the search was restricted to studies reporting outcomes for moderate-severity COVID-19 patients hospitalised during the Omicron waves. Australian-based cohorts were prioritised to reflect a comparable health system context. Where Australian studies were not available, studies with strong methodological quality were selected, including meta-analyses and studies with large sample sizes. A detailed justification for the selection of data sources used to populate model inputs not directly available from primary data is provided in Supplementary 1, Table 2.
Parameters applied in the cost-utility model.
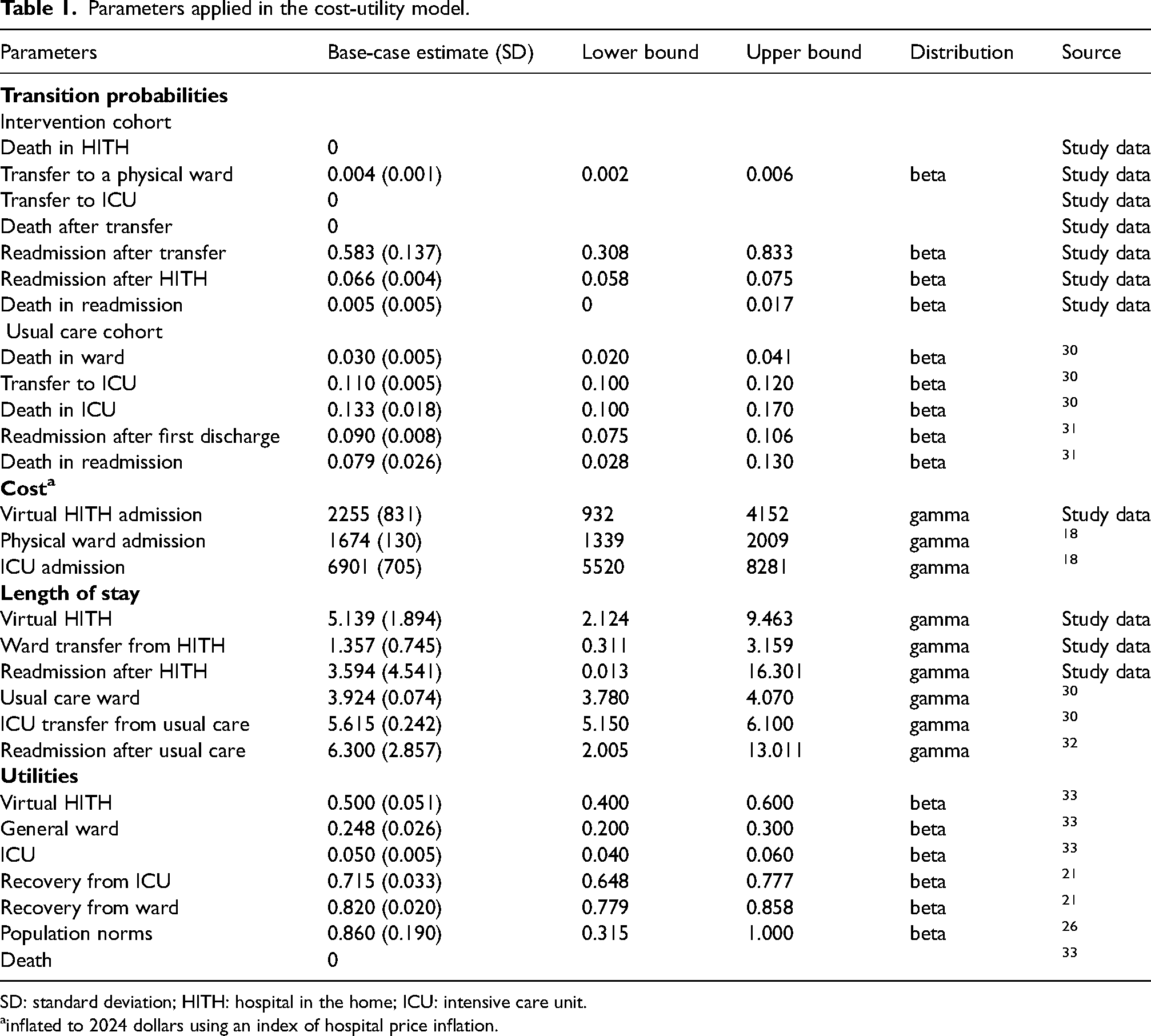
SD: standard deviation; HITH: hospital in the home; ICU: intensive care unit.
inflated to 2024 dollars using an index of hospital price inflation.
Costs associated with physical ward or ICU stays were calculated using National Efficient Price determination 2023-24 18 and admission-level Australian Refined Diagnosis Related Groups (AR-DRG) version 11.0. 19 Ward stay costs were based on code D63B (Otitis Media and Upper Respiratory Infections, Minor Complexity), while ICU costs were derived from code E75A (Other Respiratory System Disorders), reflecting the most common diagnoses for all admissions to the virtual HITH ward in this study (Supplementary 1, Table 4). The same cost estimates of ward and ICU stays were applied uniformly across all physical ward and ICU admissions in both arms.
Health outcomes were measured in quality-adjusted life-years (QALYs). At the time of analysis, there were no published utility values specific to COVID-19 hospitalisation. Therefore, utility values for each event in the patient care pathway (i.e. at-home monitoring, hospitalisation, in ICU) were assumed to be equal to previously published lower bound utility estimates for SARS patients. 20 These values were selected based on their inclusion of acute respiratory distress syndrome symptoms and isolation during infection. Utility values for recovery were derived from pooled estimates for hospitalised and ICU patients from a scoping review summarising the impact of COVID-19 on health utility post-discharge. 21 QALYs gained from each strategy were calculated by weighting the time spent in each event by the utility associated with that event.
Data analysis
Descriptive statistics were used to analyse patient characteristics and outcomes in the cohort study. Categorical variables are presented as frequencies and percentages. LOS is presented as median with interquartile ranges. RStudio version 4.3.1 was used for all analyses. 22
Costs were estimated from the perspective of the Australian health care system in which public hospital admissions are government funded. All costs are reported in 2024 Australian dollars using an index of hospital price inflation. 23 Total cost and health outcomes were estimated for each patient care pathway and aggregated to determine the expected cost and outcomes for each strategy. No discounting was applied due to the time horizon being less than 1 year. The Incremental Cost-Effectiveness Ratio (ICER) was then calculated by comparing the incremental differences in costs and health outcomes between the intervention cohort relative to the usual care cohort. Cost-effectiveness of the intervention was also interpreted based on net monetary benefit (NMB), using a recently published study that set the optimal willingness to pay (WTP) for a QALY in Australian setting at $28,033 per QALY. 24 NMB provides a measure of the value of the intervention in monetary terms when the WTP for a QALY is known. A positive NMB indicates that the intervention is cost-effective.
Scenario and sensitivity analyses
A scenario analysis adopting the lifetime time horizon was conducted by extrapolating the QALYs gained to the remaining life expectancy of patients. Median survival estimates were calculated by comparing the mean age of the cohort to the average Australian life expectancy in 2020–2022. 25 As there is currently no evidence to suggest that the HITH model would impact longer term costs or health outcomes, this scenario analysis made the simplifying assumptions that no differences in follow-up costs were associated with recovery, and that any patients discharged would recover from COVID-19 without experiencing long-term impacts on quality or duration of survival time. Utility values for recovery return to Australian population averages health-related quality of life 26 in this extrapolated lifetime model. Because all direct costs were modelled to occur within the first year after being infected by COVID-19, a 5% discount rate was applied only to future health outcomes.
A series of sensitivity analyses were conducted to test the robustness of the base-case analysis. One-way deterministic sensitivity analyses were conducted to assess the relative impact of each individual parameter on the ICER. All parameters were varied by applying upper and lower limits from the base-case values based on their 95% confidence intervals, or by ±20% from the point estimate if no information on standard deviations or confidence intervals were reported. A probabilistic sensitivity analysis was performed to estimate the impact of simultaneous uncertainty across all parameters in the model. Gamma distributions were applied to cost and LOS parameters, while beta distributions were fitted to the transition probability and utility estimates. Distribution for parameters from the cohort study was calculated based on their mean and standard deviation using the ShinyPrior application. 27 Since no deaths and no ICU transfers were observed in HITH, the standard deviation of the probability of death, transfer to ICU, and death in ICU from the Usual Care arm was assumed for these parameters in the HITH arm to account for any potential risks of mortality and ICU transfers. Other parameters’ distributions were derived from their sources or assumed to be a variation of 20% above and below the base-case estimate if no information on standard deviations or confidence intervals were reported. A Monte Carlo simulation was performed with 10,000 randomly drawn samples taken from each of the parameter distribution. 28 Finally, a sensitivity analysis using data from a randomised controlled trial (RCT) comparing remote hospital care for COVID-19 patients to standard in-hospital case 29 was conducted to validate the base-case results from a better-defined, comparable RCT cohorts (Supplementary 3).
Results
Virtual COVID-19 HITH patient outcomes
Between 19 December 2021 and 28 November 2022, a total of 3909 COVID-19 patients were admitted to the HITH service. After excluding 622 patients with severe symptoms who received only in-person treatments during their HITH admission and 95 patients with missing or unknown data, 3192 patients were included in the analysis. The demographic characteristics of the cohort are described in Table 2. The relatively high levels of socio-demographic disadvantage of HITH patients are representative of the broader geographical jurisdiction of the service (Supplementary 1, figure 1).
Demographic characteristics of virtual COVID-19 hospital in the home patients.
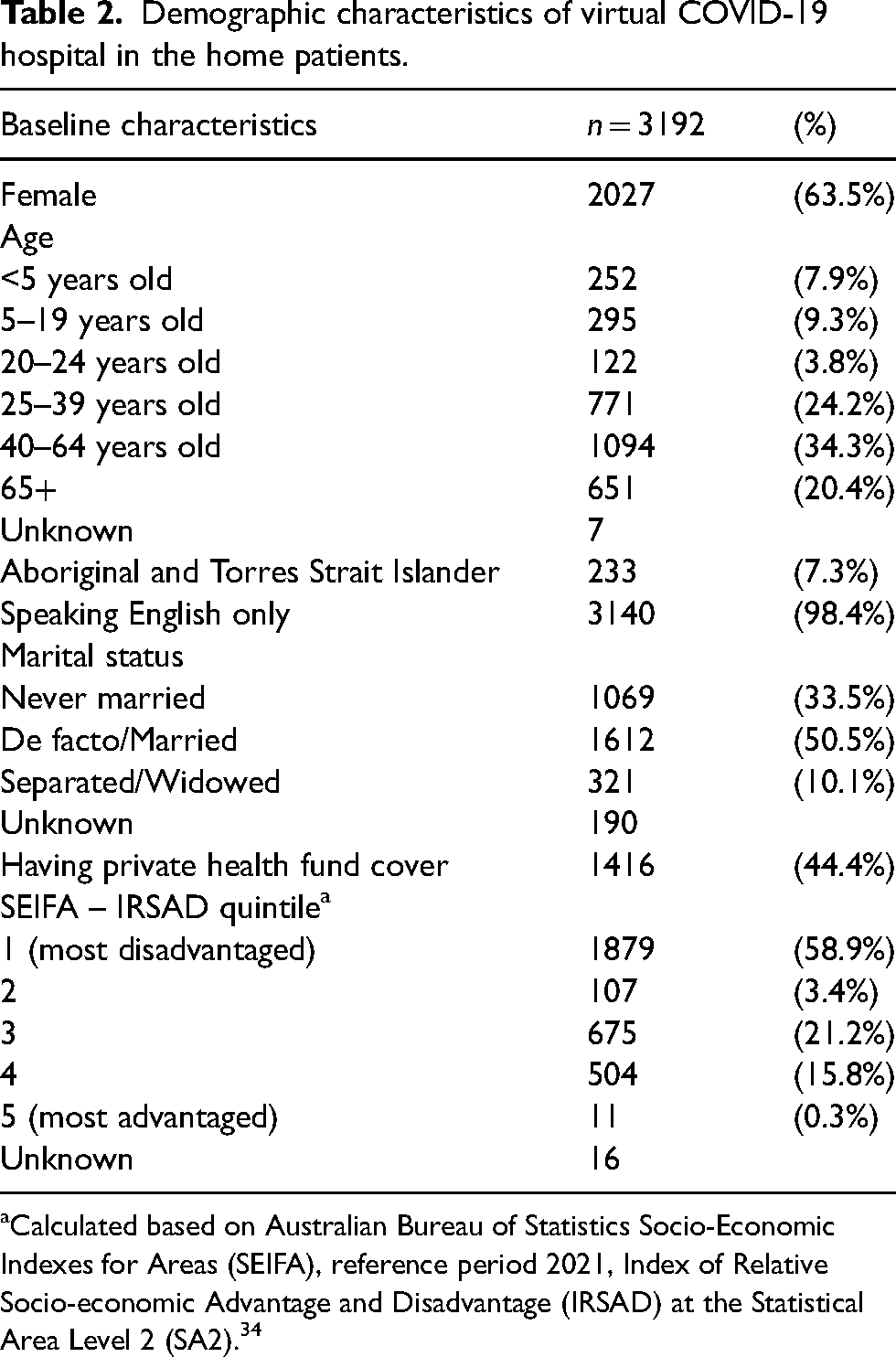
Calculated based on Australian Bureau of Statistics Socio-Economic Indexes for Areas (SEIFA), reference period 2021, Index of Relative Socio-economic Advantage and Disadvantage (IRSAD) at the Statistical Area Level 2 (SA2). 34
Table 3 summarises the outcomes of all admissions to the virtual COVID-19 HITH service. During the index admission, 12 patients (0.4%) were transferred to a physical hospital bed. No patients were transferred to ICU and there were no deaths either in the HITH ward or in the physical ward after transfer. The median LOS was 5.0 days (IQR 4.0–6.0). The 28-day readmission rate was 6.8% (n = 217). Of these, 16 patients were re-admitted to the virtual COVID-19 HITH ward and recovered, while 201 patients were readmitted into other wards with 1 subsequent in-hospital death occurring. These findings are consistent with previous studies evaluating virtual wards for COVID-19 during a similar wave, including high-risk populations (Supplementary 1, Table 3).
Patient outcomes of the virtual COVID-19 hospital in the home service.
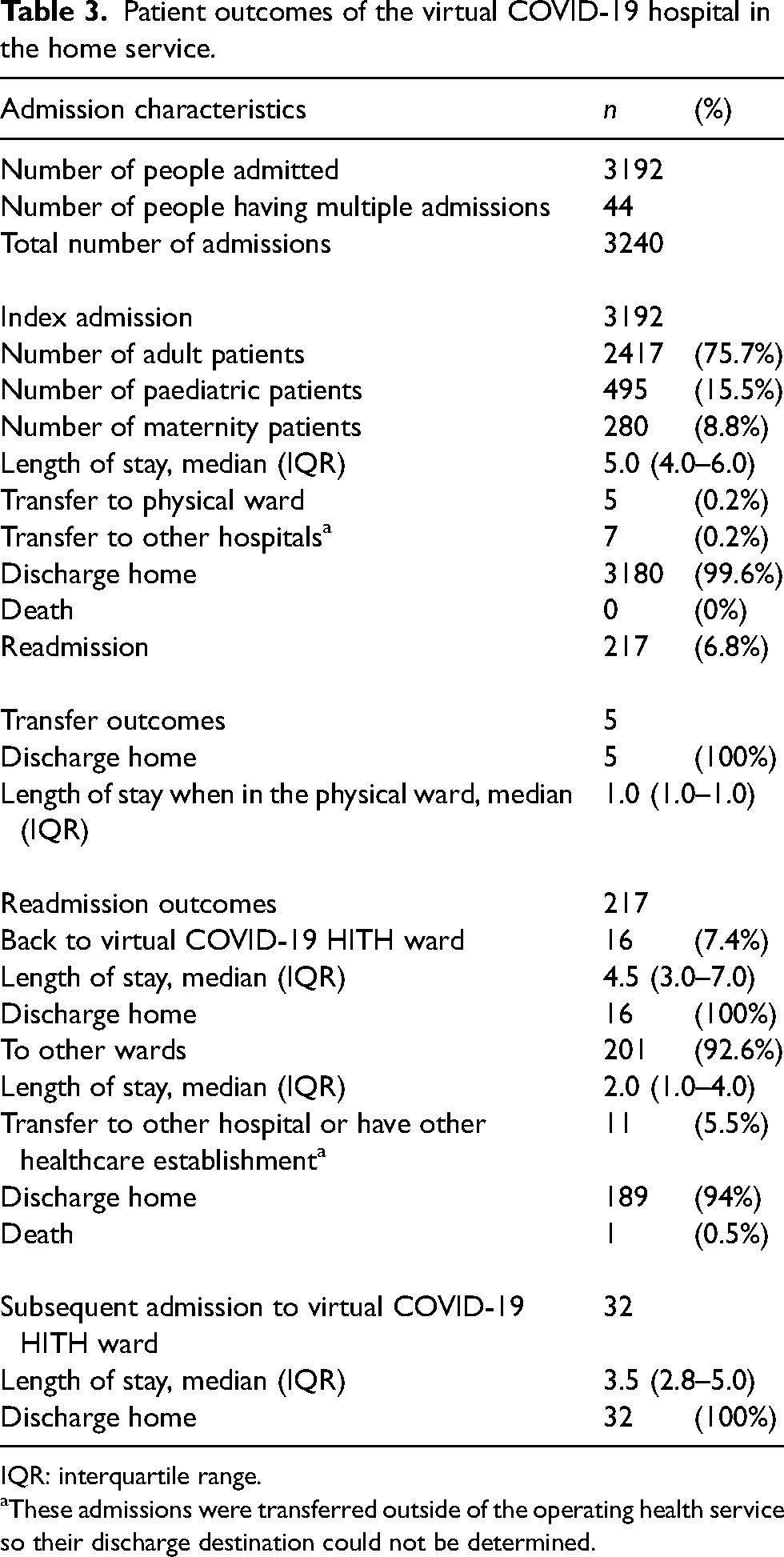
IQR: interquartile range.
These admissions were transferred outside of the operating health service so their discharge destination could not be determined.
The total cost for the service operating period was $5,369,381, with labour costs contributing to 93% of expenditure ($4,988,471). Costs fluctuated in response to the volume of admitted patients over time and subsequent staffing required to operate the ward. The average cost per patient bed day was $439 and the average cost per separation was $2255.
Modelled cost-utility analysis
Results of the cost-utility base-case analysis are summarised in Table 4. The virtual COVID-19 HITH service saved an estimated 15,273 inpatient bed days relative to usual care. The HITH strategy was dominant, resulting in an additional 0.015 QALYs and a cost saving of $201 per patient. The incremental NMB of the service was $3153. The extrapolated lifetime model confirmed that the virtual COVID-19 HITH service remains a dominant strategy with incremental NMB increasing to $854,106.
Modelled cost-utility analysis results.
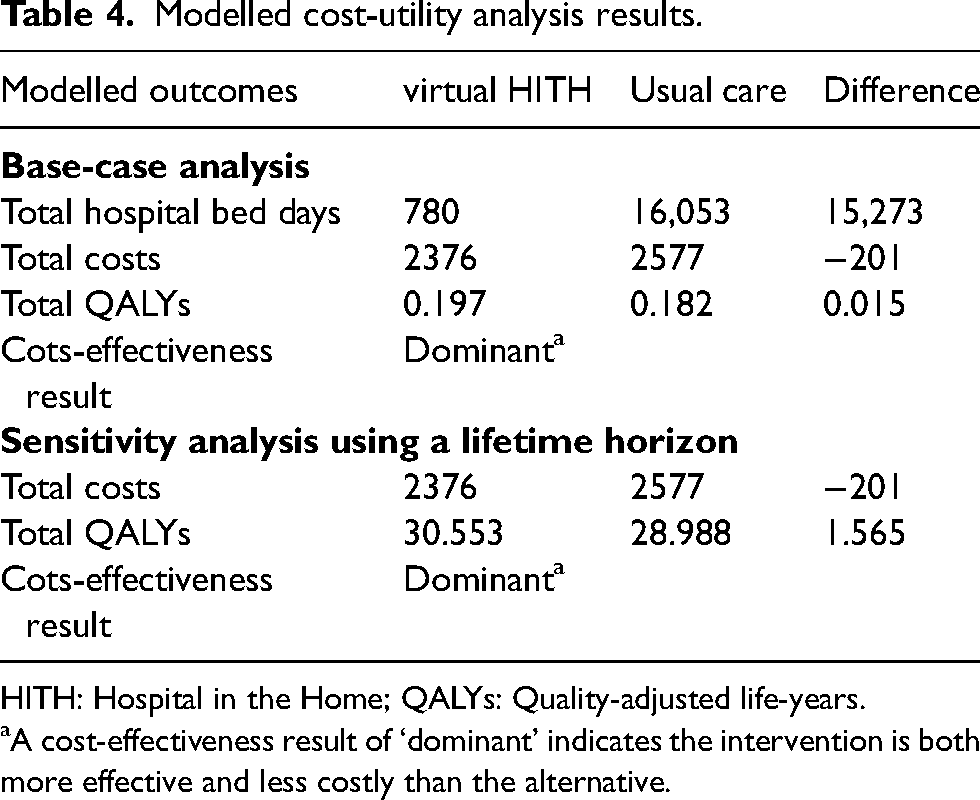
HITH: Hospital in the Home; QALYs: Quality-adjusted life-years.
A cost-effectiveness result of ‘dominant’ indicates the intervention is both more effective and less costly than the alternative.
The one-way sensitivity analysis results indicated that the ICER was most sensitive to the cost of operating the virtual HITH service (Figure 2). HITH was no longer a cost-effective strategy if its operational cost exceeded $2,882, assuming a WTP threshold of $28,033. However, the overall cost-effectiveness results are robust across other parameter ranges, with HITH remaining dominant over usual care.
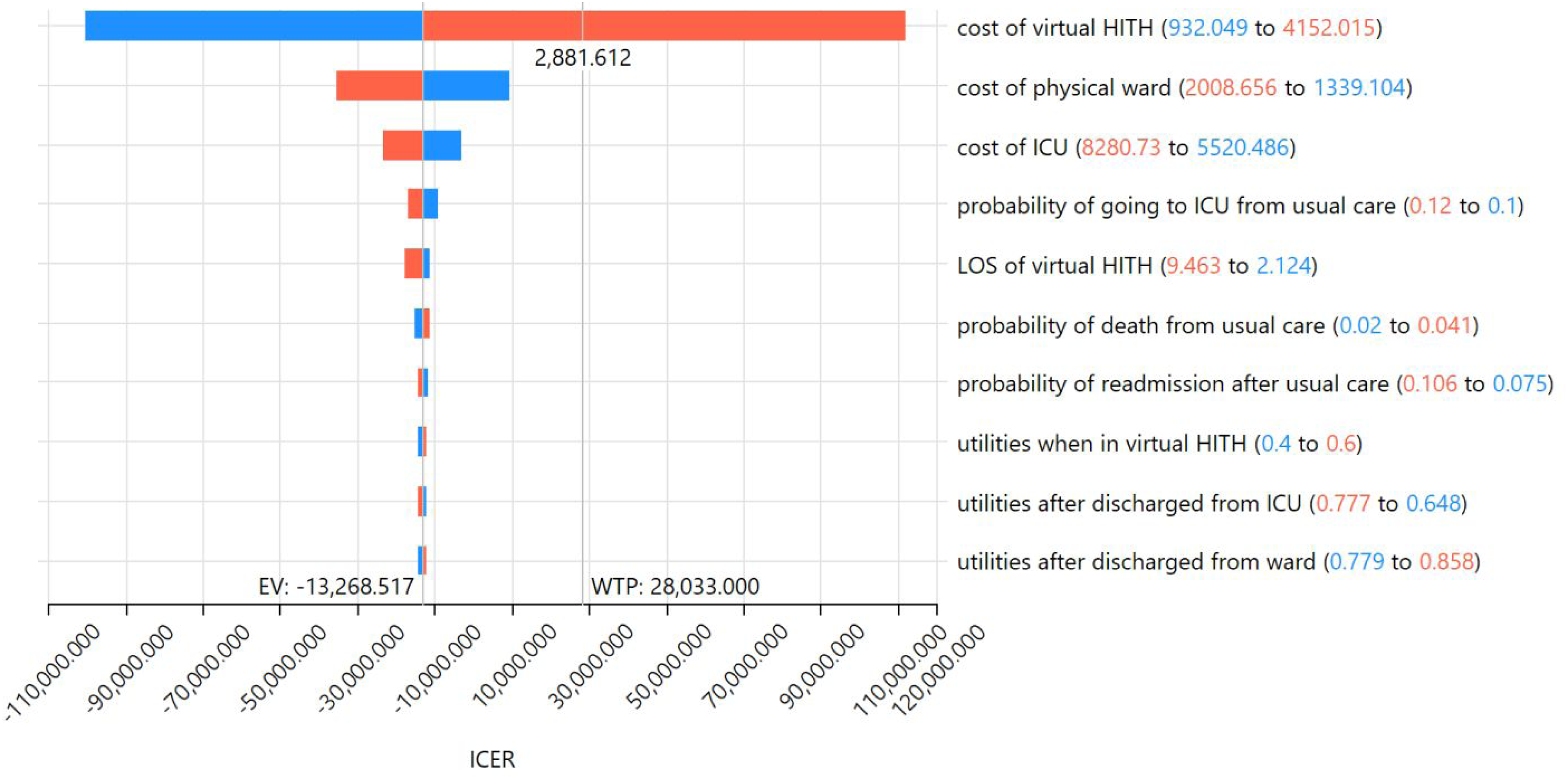
Tornado diagram of incremental cost-effectiveness ratio (ICER) between virtual HITH service and usual care for treating patients with COVID-19. HITH: Hospital in the Home; LOS: length of stay; ICER: incremental cost-effectiveness ratio; WTP: willingness to pay.
Results of the probabilistic sensitivity analysis indicated that the likelihood of the HITH strategy being cost-effective was 74%. Figure 3 presented a cost-effectiveness plane, where 63.13% of simulations fall in the southeast quadrant and to the right of the $28,033 threshold dashed line (i.e. HITH is less costly and more effective), further supporting the cost-effectiveness of the virtual COVID-19 HITH service.
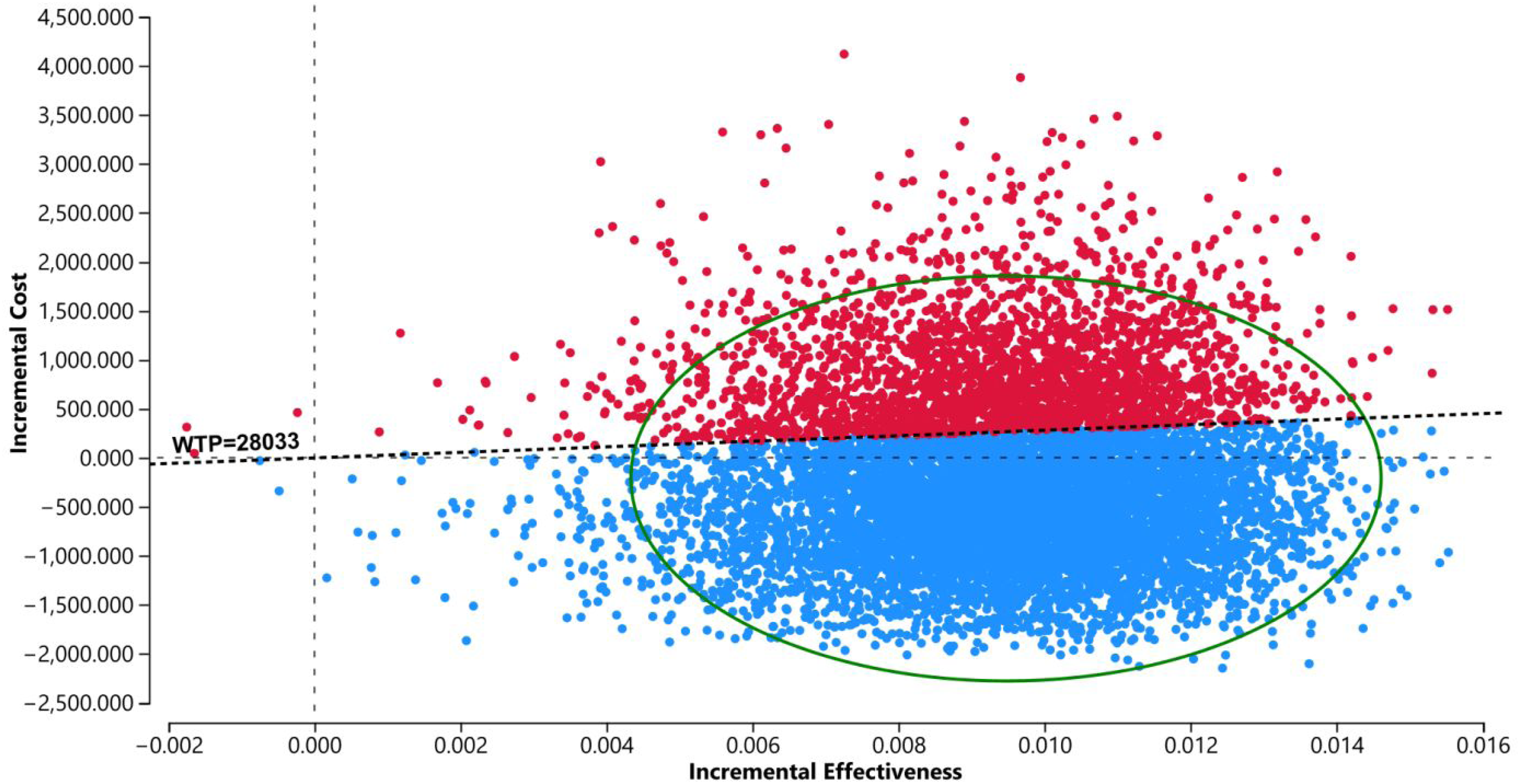
Monte Carlo simulation incremental cost-effectiveness scatterplot (with 95% confidence ellipse) between virtual HITH service vs usual care for treating patients with COVID-19. WTP: willingness to pay: QALYs: quality-adjusted life-years, scatterplot), each iteration represents incremental cost and incremental QALYs when model parameters take random values from a pre-specified range and probability distribution.
Discussion
This observational study and modelled economic evaluation found a virtual COVID-19 HITH service to be effective and cost-effective. The analysis demonstrated substantial benefits, with 15,273 hospital bed days saved over 3-month time horizon. This translated to modelled savings of $201 per patient with additional 0.015 QALYs generated when compared with usual care. After accounting for plausible uncertainty in the model, there was 74% probability of HITH being cost-effective when adopting a WTP threshold of $28,033.
Despite extensive research emerging from the COVID-19 pandemic, this study is the first to conduct a modelled economic evaluation of a virtual ward utilising telecommunication technology for treating COVID-19 patients. While several studies have explored the implementation of virtual wards for COVID-19, most included only simple descriptive costing analyses and did not go beyond reporting the amount spent per patient. 6 Our study fills this gap by providing a cost-utility analysis, offering more robust evidence to support the economic viability of this virtual HITH model of care. While potential cost reduction may fluctuate depending on equipment used and the typologies of condition treated in HITH,35,36 our findings demonstrate that this model has the potential to increase inpatient care capacity and allow for continuous access to hospital care for those at high risk of infection. These findings may also be relevant in other situations where the risks of in-person visits outweigh the benefits, such as for immunosuppressed patients, and individuals with transportation issues.
Additionally, in Australia, HITH programs are growing, accounting for 3.7% of admissions from 2011 to 2017, which highlights the importance of systematic monitoring and oversight. 37 Global systematic reviews and meta-analyses have demonstrated that HITH could reduce mortality, readmission rates,3,38,39 and cost2,5,38,40,41 when compared with traditional hospitalisation. However, limited research has addressed healthcare resources and cost of HITH in Australia.41–43 Existing studies are also often dated from the 1990s or early 2000s where no virtual care modalities were implemented. Our findings align with previous research, indicating that HITH is a safe model of care, and further support the body of evidence that HITH, incorporating virtual care technology in a public Australian health setting, is cost-effective.
Our analysis has several limitations. First, the usual care group in this study is hypothetical, as randomisation of the intervention was not feasible. This limited our ability to attribute causality to the observed differences in patient outcomes between cohorts. A hypothesis could be that outcomes for patients selected for the usual care arm, drawn from the literature, may comprise a different case mix with more complex health needs compared to those opting for HITH. Alternatively, both cohorts may have been broadly similar in baseline risk profile, and the observed differences could reflect the benefits of receiving care at home, including reduced exposure to hospital-acquired complications, 44 and improved psychological wellbeing from being in a familiar environment.2,3,38 While these uncertainties had been addressed through careful selection of data sources and our series of sensitivity analyses, future research should collect prospective health outcomes data for the control arm to enable a more comparable set of parameters used to populate the model.
A second limitation is the lack of specific utility values for COVID-19 hospitalisation, which led us to rely on data derived from another acute respiratory infection. We also assumed that any patients discharged would recover without further hospitalisations until death, due to the lack of data on long-term impact of virtual versus physical wards on patients’ outcomes. Although this assumption is consistent with our 1-year follow-up data showing minimal post-COVID symptoms and deaths among survivors (Supplementary 1, Table 5), the analysis would have been further strengthened by having more utility and health outcome data for both arms over a longer follow-up period, which might be more sensitive to changes. There is also a need for more data on different characteristics of COVID-19 survivors post-discharge including age, comorbidities, sex, and ethnicity. This would allow future research to account for the heterogeneity in subgroup analyses and potential disease progression over time for different subgroups, thereby enhancing the robustness of our findings.
Future research should also consider context-specific factors that may impact the scale-up and sustainability of the virtual HITH model of care. For example, analysing costs from a societal perspective is important in the concept of HITH and virtual care, which often involves both patients and caregivers’ time, and potential avoidance of travel costs. Furthermore, caregiver opportunity cost and cost of purchasing resources can also be important for fairly attributing cost to the HITH model from an equity perspective. Caregivers from lower income households may find it more burdensome to give up work than those from higher income household. Similarly, the cost of teleconsultation equipment is more burdensome for people with low socio-economic status. These differences should be considered when assessing the total program's costs and determining subsequent patient out of pocket costs. A time-driven activity-based costing study that tracks costs by analysing time spent on each unit of activity, including referral, labour, equipment, implementation, transport, and caregiver opportunity costs, would allow for a more comprehensive assessment of costs.
Conclusion
Recent advancements in remote monitoring technology, coupled with the pressure on health systems caused by the COVID-19 pandemic, have motivated many countries to prioritise HITH services. This study serves as an exploratory cost-effectiveness analysis to understand the viability of a HITH service incorporating virtual care modalities to replicate the systems, staffing, and daily routines of a hospital ward in the Australian public healthcare setting. Outcomes from this study support the effectiveness and cost-effectiveness of the virtual HITH service, providing compelling evidence that HITH models can address funding and resource allocation issues. These findings highlight the potential for scaling HITH to other clinical areas to expand inpatient care capacity.
Supplemental Material
sj-docx-1-jtt-10.1177_1357633X251340262 - Supplemental material for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis
Supplemental material, sj-docx-1-jtt-10.1177_1357633X251340262 for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis by Linh K Vo, Michelle J Allen, Steven M McPhail, Shannon Wallis, Kelly McGowan, Kate Atkinson and Hannah E Carter in Journal of Telemedicine and Telecare
Supplemental Material
sj-docx-2-jtt-10.1177_1357633X251340262 - Supplemental material for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis
Supplemental material, sj-docx-2-jtt-10.1177_1357633X251340262 for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis by Linh K Vo, Michelle J Allen, Steven M McPhail, Shannon Wallis, Kelly McGowan, Kate Atkinson and Hannah E Carter in Journal of Telemedicine and Telecare
Supplemental Material
sj-docx-3-jtt-10.1177_1357633X251340262 - Supplemental material for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis
Supplemental material, sj-docx-3-jtt-10.1177_1357633X251340262 for The effectiveness and cost-effectiveness of a virtual Hospital in the Home service for COVID-19 infection: A cohort study and modelled decision analysis by Linh K Vo, Michelle J Allen, Steven M McPhail, Shannon Wallis, Kelly McGowan, Kate Atkinson and Hannah E Carter in Journal of Telemedicine and Telecare
Footnotes
Acknowledgements
We would like to acknowledge the contributions of all West Moreton Hospital and Health Services staff for their assistance in data collection for this study.
Author contributions
LKV contributed to the concept and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, critical revision, statistical analysis, obtaining funding, and administrative support. MJA contributed to the concept and design, acquisition of data, critical revision, and supervision. SMM contributed to the concept and design, analysis and interpretation of data, critical revision, and supervision. SW contributed to the concept and design, critical revision, administrative support, and supervision. KM contributed to the concept and design, critical revision, administrative support, and supervision. KA contributed to the acquisition of data, analysis and interpretation of data, critical revision, provision of study materials, and administrative support. HEC contributed to the concept and design, analysis and interpretation of data, critical revision, and supervision. All authors read and approved the final version of the manuscript.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research for this paper was made possible by the first author's PhD program, which is supported by the Australian Government Research Training Program Stipend (Domestic), Queensland University of Technology Faculty of Health Excellence top-up Scholarship and West Moreton Health top-up Scholarship.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
This study received ethical approval from the West Moreton Human Research Ethics Committee (HREC/2023/QWMS/91529). A waiver of consent was obtained to access patient data on the health service use and cost retrospectively, consistent with the Australian National Statement on Ethical Conduct in Human Research section 2.3.6. A waiver of consent is justified in this case as it is impracticable to retrospectively collect individual consent from the >3000 patients who have accessed the service, and many of whom may no longer be in active contact with the service. In addition, there is no reason to believe these patients would not consent if requested, as there is no active patient participation required, and all data were already collected through routine health service data collection processes and was de-identified prior to analysis. Approval to access data without consent under the Public Health Act (Grant 91529) was also obtained following ethical approval.
Data availability statement
The data supporting the findings of this study are sourced from the Hospital Based Corporate Information System (HBCIS) and the integrated electronic medical record (ieMR) at West Moreton Hospital and Health Service. Access to data was granted under Public Health Act approval (Grant 91529) by Queensland Health. Due to the sensitivity and confidentiality of patient information, the datasets used and/or analysed during the study are not publicly available. However, they may be made available upon reasonable request from the corresponding author, subject to approval by the West Moreton Hospital and Health Service and compliance with relevant ethical guidelines.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
