Abstract
Aim:
To explore the stigmatizing pattern in people living with HIV/AIDS (PLWHA) and assess coping strategies adopted for quality of life (QOL) appraisal.
Methods:
In the background of a descriptive, cross-sectional research design, PLWHA attending HIV (human immunodeficiency virus) outpatient clinic at Medical College, Kolkata (n = 120) were enrolled through “snowball sampling.” A brief semistructured interview schedule was used to elicit data on socio-demographics. Stigma was assessed using a 4-point scale (40-item). Quality of life was assessed using WHOQOL-BREF (World Health Organization Quality-of-Life) scale (26-item).
Results:
About 96.7% reported being stressed. Stigma was mostly confronted in socio-familial context. Fear of being stigmatized was much higher compared with those who actually faced stigma (69.2% vs 27.5%; P < .01). Quality of life negatively correlated with internalizing of stigma in the psychological domain (P < .01). Proportion experiencing actual stigma (women vs men: 79% vs 74%) experienced an above moderate QOL. Multiple defense mechanisms were identified. “Altruism,” “Anticipation,” and “Humor” were the most preferred defense strategies. However, such coping strategies appeared to be self-taught and only modestly helpful in managing perceived stigma.
Conclusions:
People living with HIV/AIDS should avoid internalizing stigmatized feeling and engage in social activities to work toward a better QOL.
Introduction
Nearly 36.7 million people worldwide were diagnosed with HIV/AIDS in 2015, which included 1.8 million (5%) young children (below 15 years).1,2 The HIV (human immunodeficiency virus) incidence rates have been so alarming that an estimated 2.1 million individuals became newly infected in 2015, 3 which included approximately 150 000 children, belonging mostly to sub-Saharan African areas. Most were infected through perinatal transmissions or breastfeeding. 4
However, apart from such a global crisis which was predicted way back in the 1980s, a relatively newer menace of “AIDS-related stigmatization” has been slowly gaining momentum. In fact, a few years ago, Jonathan Mann, Director of World Health Organization (WHO) Global Programme on AIDS (1987), had identified 3 distinct types of epidemic: (1) HIV infection, (2) AIDS epidemic, and (3) HIV/AIDS stigma. 5 The third entity (stigma) was not given due importance until the 1990s when AIDS-related stigma and discrimination was actually identified to be a greater concern for health care providers. The condition was referred to as prejudice, negative attitudes, abuse and maltreatment directed at people living with HIV/AIDS (PLWHA). 6 Stigma could be aggravated due to several reasons, which included being shunned by family and relatives, peers, and the wider community; poor health care delivery; inadequate health education; erosion of basic rights; and psychological damage which would ultimately lead to unsatisfactory patient compliance and treatment outcomes.7–11
It is very well known today that AIDS and stigma do coexist worldwide. Although there remain regional and ethnic variations in prevalence rates, the inherent growing trend remains comparable worldwide.12–14 They may occur alongside other forms of discrimination, such as racism, homosexuality or misogyny, prostitution, and drug abuse, and such associations complicate situation further because these are considered socially unacceptable in many parts of the world.15,16 The concern for the developing world seems even greater. For instance, India has the third largest HIV population in the world. 17 It is considered as a national epidemic because of very high prevalence rates in the country (in 2015, HIV prevalence in India was nearly 0.26%). 17 The Government of India (GoI) outlined its National AIDS Control Programme-IV (NACP-IV), which made elimination of stigma and discrimination with its major focus alongside therapy success. 17 In fact, the GoI had the HIV/AIDS Bill (2006) passed in 2014, which had one of several clear mandate: provisions for prohibiting discrimination in employment, education, health care, travel, and insurance among PLWHA.18,19 Moreover, it recognizes that PLWHA have the right to privacy and confidentiality about disease status.18,19 However, despite such clearly defined regulations, a major proportion of PLWHA continue to experience high levels of discrimination in households, community, and at workplaces. 20 Marfatia et al 20 showed that 25% HIV-infected individuals in India had been refused medical care due to strong evidence of stigma at workplace, and 74% of PLWHA did not disclose disease status for fear of discrimination and community retaliation. Surprisingly, stigma and discrimination have also been found to be very common in health setups as pointed by Ekstrand et al. 21
Given such a situation, it becomes imperative in many ways, for PLWHA to adopt defense strategies to cope with an inherent stress associated with stigmatization. Freud in his psychoanalytical theory defined defense mechanisms as unconscious psychological strategies brought into play by various entities to cope with reality and to maintain self-image. 22 Structural forms of defense mechanisms were defined as Id, Ego, and Super Ego 23 because it was suggested that defense or coping strategies work by distorting the Id impulses into acceptable forms or by unconscious or conscious blockade of these impulses. 24 Freud and Valliant even classified defense mechanism under various categories for qualitative assessment of such behavior. 25 However, it was also suggested that even normal individuals tend to use different defense mechanisms throughout life.
Rationale
Our study provides insights regarding as to how PLWHA attending our setup experience stigma. It provides estimates on proportion being stressed and assesses their coping strategies, to appraise the quality of life (QOL).
Methods
Ethics
The study was conducted in conformity to Helsinki II Declaration, and protocol approval was done by the Institutional Ethics Committee (IEC) at Medical College and Hospital, Kolkata, India. Oral and written informed consents of study participation were obtained. Strict confidentiality of subject data was maintained.
Study design
This study was an observational, descriptive study with a cross-sectional design. It enrolled subjects from a cohort of PLWHA attending HIV outpatient clinic at Medical College, Kolkata by snowballing method. The data were collected over a period of 8 weeks, thrice weekly (September-November, 2016). A brief semistructured interview schedule was used to elicit data on socio-demographics.
Stigma was measured using a scale discussed by Berger et al. 26 It is a 40-item 4-point scale which categorizes stigma into (1) actual stigma (personalized stigma), (2) perceived stigma (concern with public attitudes about people with HIV), (3) disclosure concerns, and (4) internalized stigma (negative self-image). The scores have demonstrated a positive correlation to stigma experience (the higher the score, the higher the stigma). A translated scale was pilot tested for reliability suited to our cultural setting. The internal reliability score was 0.95.
Quality of life was assessed using WHOQOL-BREF (World Health Organization Quality-of-Life) (1998) scale, 27 which is a 26-item scale with 4 domain scores. The domains are studied under physical, psychological, social relationships, and environmental aspects. The domain scores have a positive correlation (higher scores denoted higher QOL). It is basically a brief version of WHOQOL-100 (100-item scale).
Data collection from a respondent was carried in a one-to-one situation, in the total privacy of a consenting room adjoining outpatient clinic, and alternate arrangements were made for the supervision of young children or dependents of the respondents. On average, each interview required 30 to 40 minutes. Outcome assessment included (1) level of stigma-related stress among HIV-positive persons and (2) defense or coping strategies adopted to mitigate associated stress.
Statistical analysis
Descriptive data were represented as counts and percentages, if not stated otherwise. The Pearson correlation coefficient was calculated to assess associations between stigma and QOL. χ2 analysis was used for categorical data to determine the differences between the groups. Multivariate analysis was used to study the influence of some of the socio-demographic variables on stigma. The analysis was done using SPSS (version 16.0).
Results
In our study, HIV/AIDS was more prevalent in married women, mostly from urban areas belonging to lower socioeconomic status (Table 1). Most people were diagnosed within 6 months of HIV infection and received antiretroviral therapy. Disease communicability was rather high between spouse and near relatives (Table 2).
Baseline characteristics of subjects (n = 120).
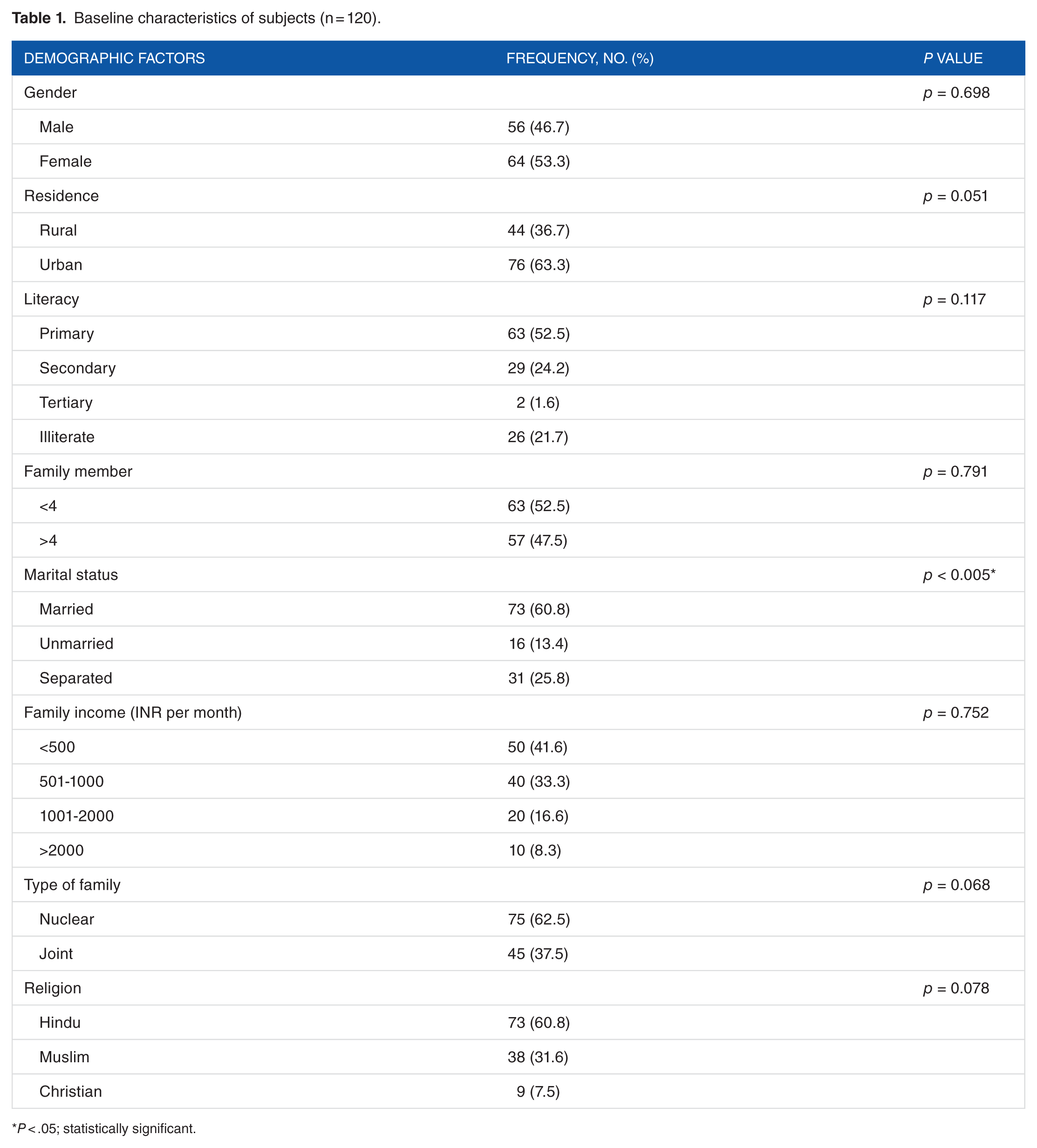
P < .05; statistically significant.
Distribution of study population as per HIV/AIDS-related information (n = 120).
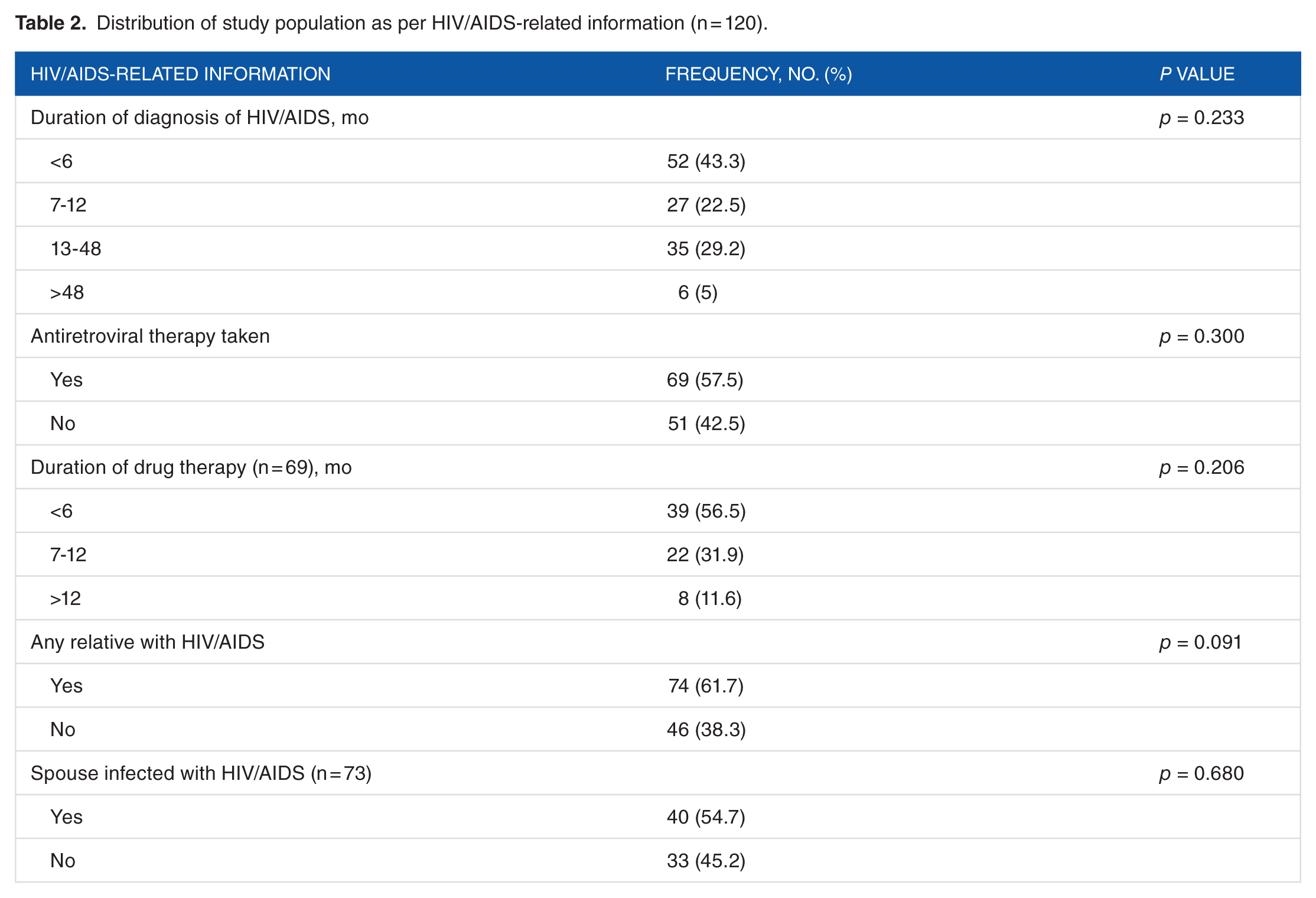
Most subjects reported that their HIV status was known to their family members, but relative anonymity was maintained for neighbors and workplace associates. As a result, stigma experiencing was mostly from family members and neighbors. However, the fear of being stigmatized was much higher compared with those who actually faced stigma (69.2% vs 27.5%; P < .01). A bivariate analysis revealed that proportion of women (79%) and men (74%) experiencing actual stigma seemed more determined to live and experienced an above moderate QOL. About 96.7% patients reported being stressed due to such reasons (Table 3). Internalizing of stigma showed a negative correlation with QOL in the psychological domain (r = −.265; P < .01). Proportion experiencing actual stigma seemed more determined to live and experienced an above moderate QOL (Table 4). Socio-demographic variables were tested for by multivariate analysis; however, none of the variables had a significant influence on stigma (data not tabulated).
Distribution of study population according to stigma-related factors (n = 120).
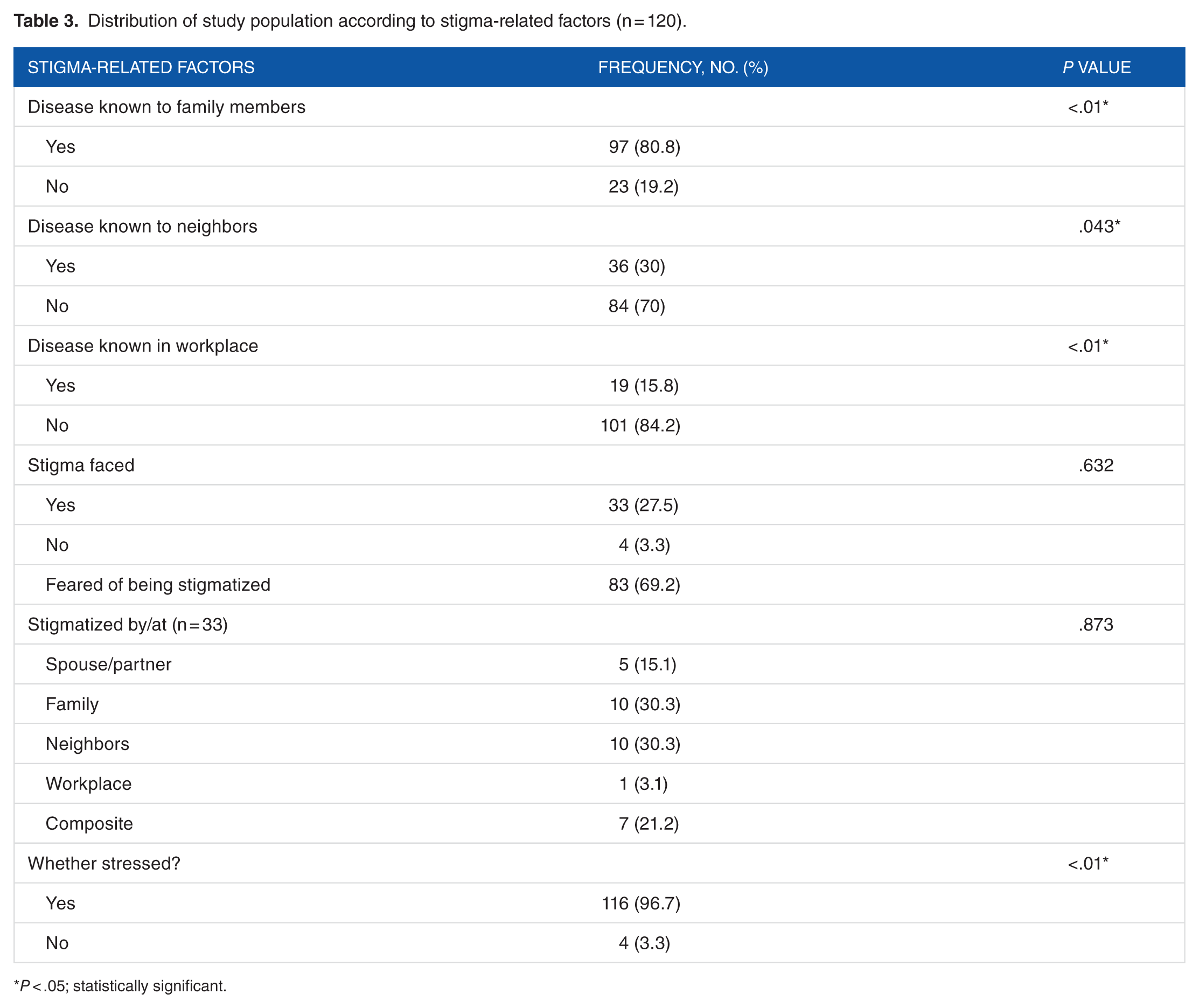
P < .05; statistically significant.
Correlation coefficient (r) between stigma and quality of life.
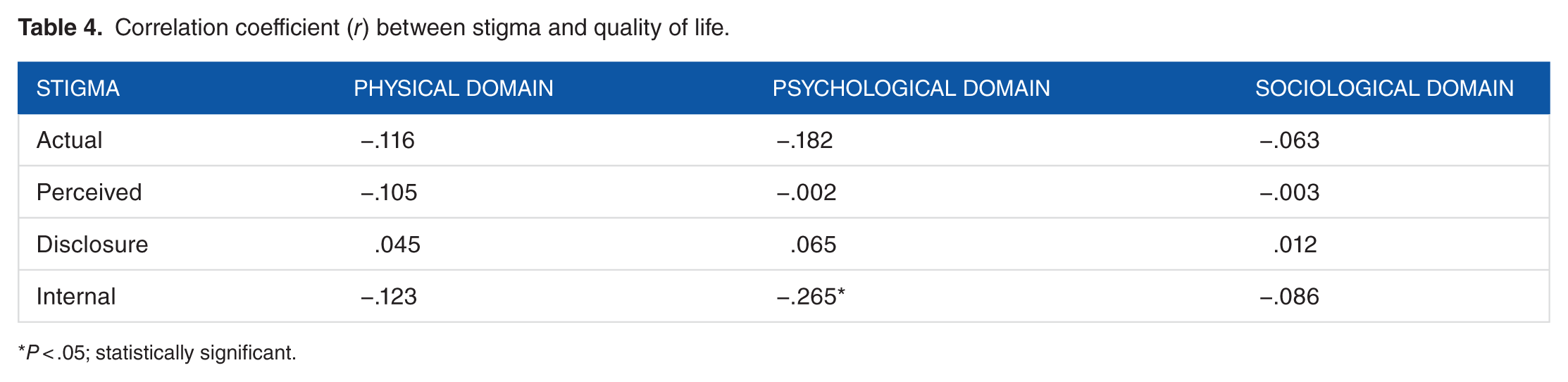
P < .05; statistically significant.
Multiple defense strategies adopted by PLWHA were identified and classified according to Vaillant’s Categorization of Defense Mechanism. Altruism (62.9%), Anticipation (94%), and Humor (78.4%) were the most preferred coping strategies (Level-IV). Coping appeared to be self-taught and only modestly helpful in managing perceived stigma.
Discussion
The study demonstrates that actual stigma experienced among PLWHA is far less as compared with the fear of being stigmatized or perceived stigma; however, this leads to increased stressful situations on part of the affected. As a result, various defense strategies are embraced, although such self-taught coping appears to be only modestly helpful in managing perceived stigma.
The study reported that stigma arises mostly from family members and neighborhood in directly stigmatized patients; however, such factors do not alter QOL significantly (Table 4). However, because impact on psychological domain and QOL is significantly correlated, a counseling process should go beyond PLWHA and include near relatives. An encouraging finding is that those individuals who experienced actual stigma had an above moderate QOL. This could be due to the fact that being stigmatized kindles in them a feeling of determination and zeal to counter the effect of stigma. It indicates that internalizing of stigmatized feelings accentuates the problem of stigma, as that study reveals a highly significant negative relationship between internalized stigma and QOL in the psychological domain. Stigma deprives an individual of social support, which in turn could negatively affect the QOL. The finding, where in conjunction with previous studies, reported that internalized stigma is likely to make an individual more sensitive to both actual and anticipated rejection and stigmatization by others which negatively affect disclosure. 28 Stigmatized individuals are also vulnerable to feelings of self-hatred, which can result when they internalize society’s negative views of them.29–32 Discrimination was also found to be prevalent among medical professionals. 33 Stigma can affect disclosure34–36; hence, hiding one’s status may not only preclude HIV-related social support. In 2003, a study from South India showed similar findings. 37
The findings of this study encourage PLWHA, therefore, to rise above stigma and live a QOL. Understanding and addressing moderating variables can inform health care provision, stigma reduction interventions, and public health policy. The findings also support the need for psychosocial counseling for the infected as well as the caregivers to cope with the illness positively. Increment in cultural and media exposure of people living with AIDS is the need of the hour. Fear-inculcating information about HIV/AIDS that emphasize the fatality of the condition or try to portray HIV as a result of moral decay and social deterioration does little to motivate people to change their behavior but cast infected individuals as immoral and deserving of discrimination.
Limitation(s)
(1) The generalizability of study findings may not be appropriate because it was a single center experience, (2) the cross-sectional design may have lent itself to retrospective bias, (3) limited study time frame to assess the defense mechanism for a long period was not an ideal approach, (4) assessment of defense mechanism was based on only Vaillant’s categorization, and (5) assessment was subjectively based on patient’s mood during interviewing, which could be affected in the wake of recent events.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
AnM conceived and designed the experiments, made critical revisions, and approved final version. SL analyzed the data. AM wrote the first draft of the manuscript. SC contributed to the writing of the manuscript. RS agree with manuscript results and conclusions. AM and SL jointly developed the structure and arguments for the paper. All authors reviewed and approved the final manuscript.
