Abstract
Cranioplasty is one of the most common neurosurgical procedure performed to repair cranial defect. Many materials and fabrication technique are used to prepare cranial implant in cases where autologous bone is not available. Polymethyl Methacrylate (PMMA) is one of the most common polymer used as bone substitute. PMMA fabricated using 3D printed models have shown better fit, symmetrical shape, and restore esthetic looks of patients. The use of 3D printed implants in medical procedures has several advantages over traditional manufacturing methods. 3D printing allows for greater precision, customization, and quicker implant time.
Introduction
The advancement of science and technology has led to great leap in medical technology. Medical technology has revolutionized medical science and has greatly improved the ability of healthcare professionals to diagnose, treat, and manage various medical conditions. One of the modern medical technologies is 3D (three dimensional) printing and patient specific treatment. 1 3D printing technology has been extensively researched to develop and replace human organs, speed up surgical procedures, produce cheaper versions of required surgical tools, and improve the lives of those reliant on artificial organ or prosthetic limbs.2,3 3D printed implants are a promising area of medical technology that has the potential to improve patient outcomes and revolutionize the way we treat a variety of medical conditions.1,3
Cranioplasty is usually performed after decompressive craniectomy is aimed to provide cerebral protection, improve flow of cerebrospinal fluid and restore the cosmetic looks of the patient. 4 Cranioplasty for a large defect size (>5 inch by 5 inch) was a challenging task for the surgeon, both cosmetically and in terms of having better protection to the brain tissues. With additive printing technology, exactly fitting implant is prepared in laboratory which can be implanted intra-operatively which reduces the intra-operative implant preparation time, provides better cosmetic outcomes and safety with consistent bone thickness. 5
3D designed cranial defect repair is a medical procedure in which a patient’s skull defect is repaired using a 3D printed implant designed specifically for their unique cranial anatomy. This procedure is typically performed on patients who have suffered trauma to the head or have had a portion of their skull removed due to medical reasons. The process typically involves a team of medical professionals, including a neurosurgeon, and a biomedical engineer who specializes in 3D printing. 6 The patient’s cranial anatomy is first imaged using Computed Tomography (CT) or Magnetic Resonance Imaging (MRI) scans, which are then converted into a 3D digital model using specialized software. The biomedical engineer then designs a customized implant to fit the patient’s specific cranial anatomy. 7
Various other implant materials and procedures like titanium mesh, self-molded bone cement, and using allografts are the options available for repair of cranial defect. Although these techniques, provided safety and protection to underlying brain, the repair of defect did not promise to be symmetrical and perfect fit in defect.8,9 The introduction of 3D printing, repairing cranial defect has provided promising outcome to patient as well as neurosurgeons. 2
Out of all uses of medical 3D printing, its use in preparing cranial implant and defect repair has been discussed in this paper.
Designing and Printing
Patient specific cranial implant was designed using CT scan images of the patient. The plain CT scan of head taken with slice thickness of 1 mm or less was acquired in DICOM format (Digital Imaging Communication in Medicine). Thus obtained sequence of the CT image was reconstructed into 3D model and was exported as stereo-lithographic (STL) file. Thus obtained STL file was remodeled using a 3D manipulation application, meshmixer.
The open source designing software allows addition of new layers and models to fit in the defect of 3D model. With few steps of manipulation and designing a new object can be created that fits into the defects and has a symmetrical curvature compared to the normal side. The figure below depicts the 3D cranial model with a defect, which after manipulation is repaired to get a cranial implant.
The newly created object which covers the cranial defect is exported and is printed using a 3D printer. UPbox+, with a printing material of Acrylonitrile butadiene styrene (ABS), a kind of plastic, was used to create a 3D model of the implant (Figure 1).

(A) CT scan image, (B) 3D STL file, (C) remodeled defect, (D) 3D printed model of ABS, (E) PMMA based implant, and (F) intra-operative image.
Implant Preparation
First stage of implant is printed with ABS, a plastic material, which is not implantable in humans. Thus to acquire implantable material, the 3D printed model was molded using a mold-silicon under aseptic condition. The molding would take around 6 hours to set and harden. The mold is then cut out to extract the plastic 3D model, which is then filled with Polymethyl Methacrylate (PMMA), commonly known as bone cement. PMMA is a food and drug administration (FDA) approved substitute for bone and is available in powder form. It is required to mix with the hardening liquid, benzoyl peroxide and radio opacifier (contrast material), zicronium di-oxide (ZrO2), along with this powder of vancomycin (Antibiotic) is mixed and stirred together. The semi-solid mixture of PMMA is then poured into the mold. Fifteen to twenty minutes later, PMMA will set into a hard bone like material taking the shape of the 3D printed model, which eventually will be used as an implant to repair the cranial defect.
Result
One hundred eight cases of cranial implant have been done using the 3D printing technique (Table 1). The implantation was performed in multiple centers in Nepal. This technique has provided a customized implant to the patients with cranial defect, covering their defect with better fit, symmetricity, protection and overall at cheaper and affordable price.
Classification of cases based on diagnosis.

The cases included from June 2020 to April 2024 were classified as cranioplasty performed for decompressive craniectomy, Road traffic accident, and bone deformity. The Table 1 below shows the number of cases for each.
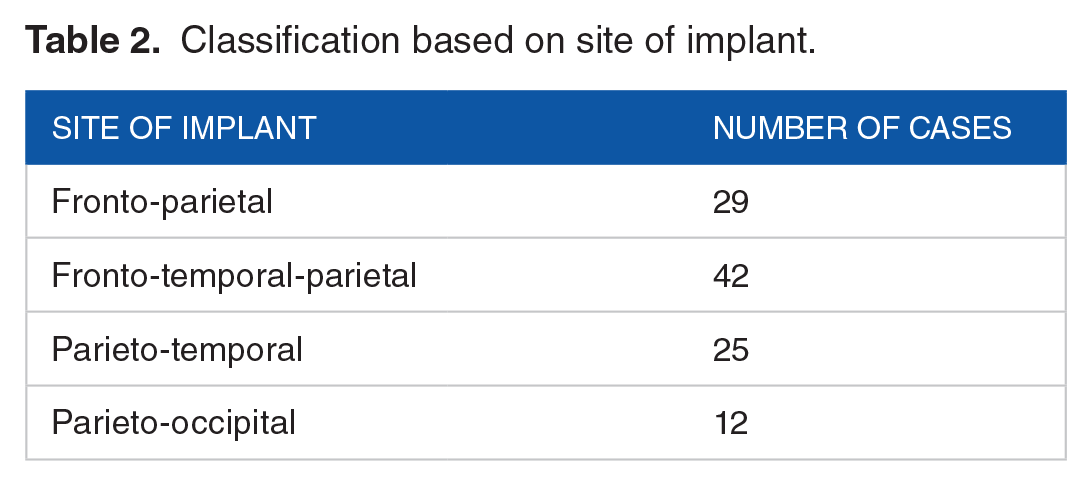
Table 2 shows the classification of cases based on area of the implant, where most of the implants were performed for fronto-temporal-parietal defect repair. Table 3 demonstrates the cases for unilateral versus bilateral implants.
Classification based on site of implant.
Unilateral versus bilateral cranioplasty.

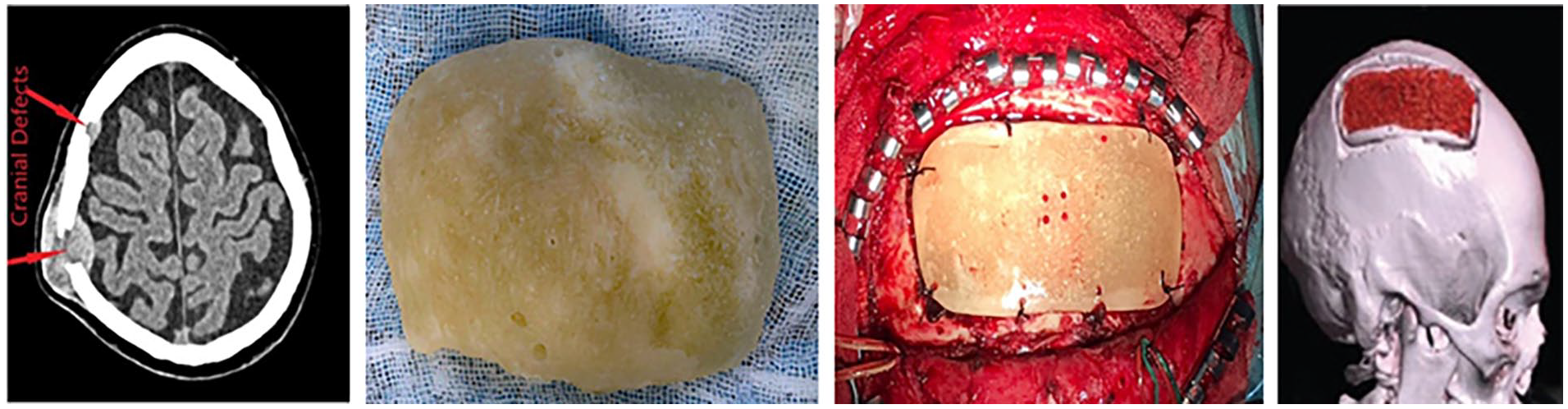
Figure 2 shows pre-operative 3d image of the patient’s skull on the left, the middle image shows the 3d printed model (Red), and the PMMA based implant (pink). The image on the right shows the post-operative scan where the cranial defect has been covered with 3d designed cranial implant.

Pre-operative, PMMA implant, 3D model, Post-Operative Images from left to right.
Figure 3 depicts the status of the patient before and after the implant was placed for his fronto-parietal defect.

Pre-operative and post-operative image of patient shown in case 1.
On 3 years’ post-operative follow up, there was no complications related to implant failure and rejection, except for a single case with the infection where it had to be explanted. The mechanical protection and esthetical looks was maintained with 3D printed implants. The patients had no complaint regarding symmetricity and protection. Most of the patients were able to continue to their previous job with the implants on. Some intra-operative case representation for PMMA based implants is depicted in Figure 4.

Intra-operative images for some cases with PMMA implants.
Figure 5 depicts the case of fibrous bone dysplasia treated with implanting a 3D printed PMMA based cranial implant.
Defect repair with 3D printed PMMA implant for fibrous dysplasia.
Discussion
Wide range of materials has been used and trailed for the reconstruction cranial defects; from human and non-human bones to metals, ceramics, and polymers. Some of the most commonly used polymers include, polyetheretherketone (PEEK), high-density polyethylene (HDPE), polypropylene (PP), PMMA, and poly(tetrafluoroethylene). 10 PEEK and PMMA represent the most widely used polymeric materials for the reconstruction of cranial defects. Both polymers are inert, biocompatible, and have adequate mechanical properties to be used as bone substitute. PEEK is superior to PMMA in terms of strength, stiffness, and durability. While on the other hand, PMMA is easily obtainable and affordable.11-13 However, PMMA needs to be molded by surgeons, intraoperative during the surgery. Hence to create an affordable implant having precise shape and size, the improvised technique to produce cranial implant is being used in many hospitals and countries.7,9 Comparing these molded PMMA to a 3D printed implant, they lack the homogenous thickness as of skull and are not bilaterally symmetrical, which leads to poor esthetic looks of a patient. On the other hand, a 3D printed implant has a homogenous thickness as skull and symmetrical shape is outlined through software, which leads with clinically and esthetically better results. 14
Metallic implants mostly made of titanium are available in fixed sized mesh. These are rectangular in shape and needs to be cut out in accordance to the defect of the patient. Though, the actual size of the defect can be achieved, however, the shape generating a good esthetic look and symmetrical outline of skull cannot be achieved with the use of mesh.6,11,15 Although, there are companies that have started designing and printing titanium based cranial implants, customized for each patient, those are quite expensive and are beyond reach for the patients in Nepal, where they have to pay out of pocket for surgery. However, directly printing the implant material (stainless steel, titanium, and PEEK) requires a high end, dedicated printer which is very expensive to purchase and setup, on the contrary the implants made with molding technique can be designed with simple home-based 3D printers capable of printing materials like PLA, ABS, and other plastic based material. Though it takes more time to prepare the implant, it’s very cheaper and affordable to get a regular printer for a hospital setup in a Low middle income country (LMIC) like Nepal.16,17
Regarding cost, accuracy, shape, esthetic and fit, PMMA based 3D printed cranial implant is one of the best alternative for the patient in low income countries, like Nepal. The implant is designed to fit snugly into the patient’s skull defect and is secured in place using screws or other fixation methods. The use of 3D printing technology in cranial defect repair has several advantages over traditional methods. It allows for greater precision and customization, as well as a quicker turnaround time from diagnosis to treatment. 18 Additionally, 3D printed implants can be lighter and more comfortable for the patient compared to traditional implants made from metals or other materials.
Conclusion
3D designed cranial defect repair is a promising field that has the potential to revolutionize the way we treat cranial injuries and defects. Fabricating PMMA using 3D models has been a good alternative for 3D printed metallic implant, which is not available in Nepal.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All the findings and related data has been published in this paper. For further data, contact corresponding author.
Statement of Ethics
The study has been approved by Institutional Review committee of Annapurna Neurological Institute and Allied Sciences. The approval reference number is IRB-2022/23-017-ANI. A written consent has been taken from each patient before surgical procedure, which can be provided upon request.
