Abstract
Study design:
Systematic literature review.
Objective:
This study provided a systematic review of randomized controlled trials which assessed the therapeutic effects of stem cell treatments, surgical interventions, and nonsurgical treatments on the outcomes of patients diagnoses with intervertebral disk degeneration (IDD).
Methods:
A MEDLINE (2000-2017), PubMed (2000-2017), and Google scholar (1995-2000) database search was performed to identify published articles reporting on patient-reported clinical outcomes. A total of 12 articles were identified and met the inclusion criteria.
Results:
Literature evaluating the comparative treatment outcomes between patients who underwent surgical versus nonsurgical interventions demonstrated mixed findings in treatment efficacy. Although studies involving the manipulation of endogenous stem cells in fibrocartilage suggested that this application could be a potentially noninvasive, stem cell–based strategy to treat fibrocartilage degeneration, especially in patients with IDD.
Conclusions:
The reviewed literature suggested that no clinical significance exists between surgical and nonsurgical treatment for IDD. The decision to undergo surgical or conservative treatment should depend on the patient’s state of health at the time of surgery, as well as any other potentially alarming factors (altered mental status, level of consciousness, comorbidities, etc) that could be exacerbated with the proposed treatment. Mesenchymal stem cells and fibrocartilage stem cells may also be an effective therapeutic option for the regeneration of a degenerated intervertebral disk. To move forward in finding an effective therapeutic treatment protocol for IDD, further research needs to be implemented that minimizes the limitation discussed in this review.
Keywords
Introduction
One of the most common structural abnormalities in the lumbar region of the spine is the degeneration of the intervertebral disk (IVD). 1 The IVD acts as a shock absorber during compressive loading of the spine. When the IVD degenerates, the ability of the spinal column to facilitate motion is limited, which results in the inability to maintain stress and compressive forces that are placed on the spine. When a disk is damaged, it has a limited ability for self-repair. This degenerative process involves the reduced synthesis of the extracellular matrix (ECM). 2 Studies have shown that aggrecan and collagen II are the most downregulated components of the ECM in IVD degeneration (IDD). 3 When this occurs, proteoglycans are lost from the tissue which will decrease the hydration and resilience of the joint accompanied with a loss of pressure within the fibrocartilage of the spine. 4 Matrix metalloproteinases (MMPs) can increase the presence of matrix-degrading enzymes (collagenase II). 5 Matrix metalloproteinases are thought to be the major degenerative enzymes in the IVD, which degrade a variety of substrates. These substrates include proteoglycans, gelatins, and collagens. 6 Haro et al support this study by suggesting that MMP-3 is directly involved in the physical degeneration of tissue within the IVD.
The nucleus pulposus (NP) of the healthy adult IVD is rich in proteoglycans, resulting in the tissue’s high water content and, thus, being able to distribute loads applied to the spine. NP cells ECM from the production of proteoglycans, mainly aggrecan and collagen. 7 Because the activity of NP cells underlies function of the disk, and their capacity to support the tissue declines with degeneration, we believe that treatments directed toward regenerating or replacing these cells would be the most effective for the restoration physical functioning.
Multiple studies have shown the efficacy of stem cell therapy in treating disk degeneration. The main action of this treatment is to focus on repopulating the IVD with cells that have the capability of reproducing the ECM and restoring tissue that had been damaged. 3 A systematic review from Wei et al provided a comprehensive outlook of recent advances in stem cell therapy that are directed toward treating disk degeneration. This review suggests that mesenchymal stem cells (MSCs) are effective in vitro for the treatment of disk degeneration as well as promoting cell survival following transplantation. This study seeks to strengthen the findings from Wei et al by providing more improved and up-to-date knowledge regarding the safety and efficacy of cell therapies in IVD regeneration. Embree et al discovered that fibrocartilage stem cells (FCSCs) localized within the superficial zone of the temporomandibular joint (TMJ) condyle has the efficacy to regenerate bone as well as cartilage.
In addition to stem cell therapy, conservative treatments have also been used in the treatment regimen of patients with degenerative disk diseases. These treatments are the least invasive and can include physical therapy, analgesics, anti-inflammatory medications, or lumbosacral orthoses. This method of treatment is a therapeutic option without major risks and can be acceptable for patients who cannot be operated on. 8 In a single-blinded randomized study from Brox et al, the researchers found that no significant difference exists in the outcomes of patients treated for IDD either surgically or by noninvasive treatment. However, additional literature reviewed in this article has produced mixed findings regarding the efficacy of conservative treatment.
Although nonsurgical (conservative) methods for treatment can be effective, a review from Rahman et al suggested that patients treated from IDD by surgical techniques responded with higher satisfactory rates at 4 years. This review highly advises surgical treatment for most patients; however, the outcome after surgical treatments could result in general complications such as deep venous thrombosis, pulmonary embolism, and urinary infections. 8
Unfortunately, there are no current treatments that directly focus on disk degeneration. Modern-day interventions are aimed toward the treatment of back pain (acute or chronic). These treatments are determined by the severity, degree, and persistence of pain. Intervertebral discs and ligaments can be endangered during bending moments after undergoing repetitive bending. This sustained bending can interrupt the normal protective functioning of the back muscles and can also exhaust the back muscles. This exhaustion can reduce the ability to protect the spine. 9 Treatment interventions such as surgery (ie, surgical disk treatment, invasive disk replacement) are effective in supporting the structural abnormality and improving this protective on the spine. However, these therapeutic options limit the further development of the vertebrae. 10 Studies have shown that patients undergoing conservative treatment for IDD have similar outcomes as patients following surgery.8,9,11 However, there still needs to be more investigation regarding conservative treatment on its long-term outcomes with respect to the patient’s quality of life.
Proactive efforts toward stem cell–based therapies for cartilage tissue regeneration have been made which involve stem cell growth and transplantation. 12 However, this approach has been limited by various contradictions that can include immune rejection, pathogen transmission, and potential tumorigenesis. 13 An alternative approach involves the regeneration of tissue by recruiting progenitor stem cells.14,15 Therefore, treatment strategies that use stem cells to restore adult fibrocartilage have the efficacy to become a cell-based treatment option for IDD. We believe that it is necessary to investigate the most effective therapeutic option for treating IDD that will result in the complete restoration of the patient both structurally and functionally. The present review could potentially lead to clinically significant findings that could result in improved treatment interventions for diseases involving the degeneration of the NP. Patients diagnosed with IVD degenerative conditions (eg, lumbar degenerative disk disease, low-back pain, spinal stenosis) could significantly benefit from the conceivable applications of the results of this review.
Methods
Selection of trials
Trials were reviewed using predetermined criteria. The trial must be a crossover study, a single-blinded or double-blinded randomized study, and the patients must be diagnosed with IDD. The studies are required to have stem cell, surgical, or conservation (physical therapy) approaches toward the treatment of each patient. Exclusion criteria include studies not pertaining to IDD treatment or ECM regeneration and studies that involve predisposing conditions or preventative measures for IDD (see Figure 1).
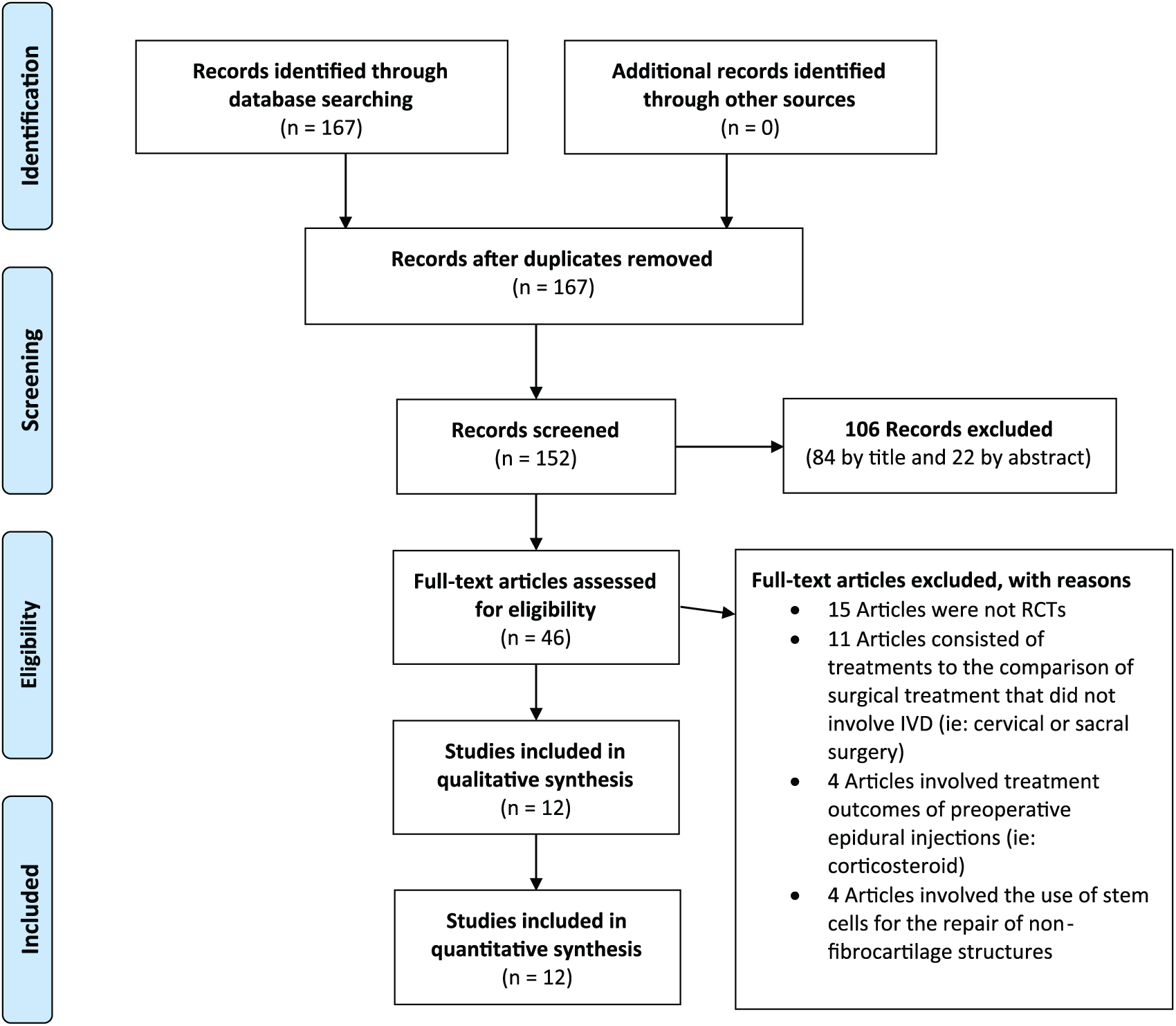
PRISMA flow diagram for the search, retrieval, and quality appraisal process. PRISMA indicates Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
A total of 167 total articles were identified through the search strategy performed by the researchers. Once 46 articles were identified for potential inclusion into the review, 34 of the full-text articles were then excluded due to failure to meet the inclusion criteria; 15 of the excluded articles were not randomized controlled trials (RCTs), 11 articles consisted of the comparison of surgical treatments that were not related to the IVD (ie, cervical or sacral surgery); 4 articles involved treatment outcomes of preoperative epidural injections (ie, corticosteroid); whereas 4 articles involved the use of stem cells for the repair of nonfibrocartilage structures.
Database and search strategy
Articles were obtained from the following sources: MEDLINE (2000-2017), PubMed (2000-2017), and Google scholar (1995-2000). Searches from each database included the search terms “Intervertebral Disk Degeneration,” “stem cell,” “physical therapy,” “treatment,” and “randomized trial” (see Table 1).
Chronological list of randomized controlled trials (RCTs) based on the search criteria given for this study: from PubMed, MEDLINE, and Google scholar.
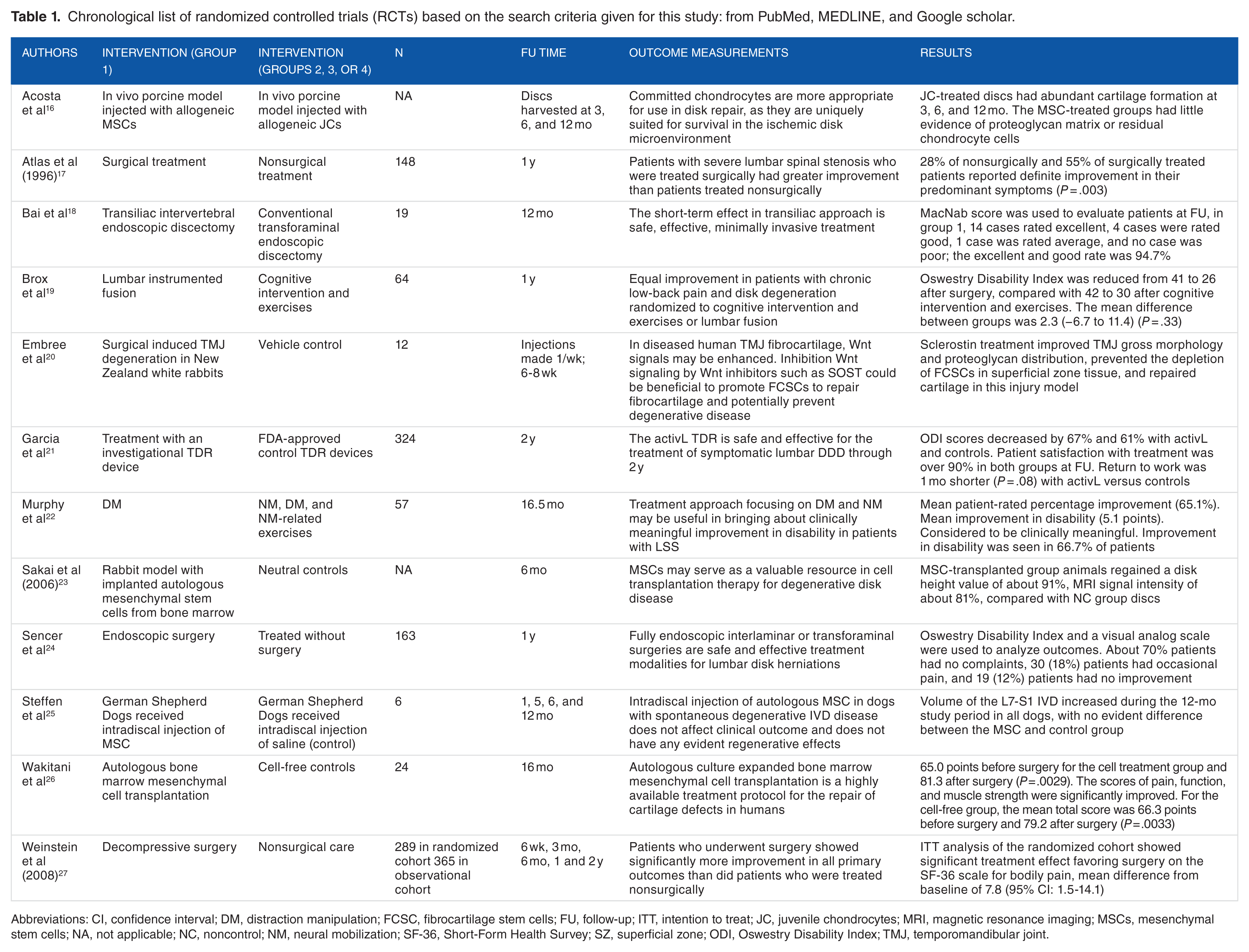
Abbreviations: CI, confidence interval; DM, distraction manipulation; FCSC, fibrocartilage stem cells; FU, follow-up; ITT, intention to treat; JC, juvenile chondrocytes; MRI, magnetic resonance imaging; MSCs, mesenchymal stem cells; NA, not applicable; NC, noncontrol; NM, neural mobilization; SF-36, Short-Form Health Survey; SZ, superficial zone; ODI, Oswestry Disability Index; TMJ, temporomandibular joint.
Data analysis
This study used a qualitative analysis to determine whether a clinically or statistically significant difference existed between each treatment group of the papers that were collected. This article used a flowchart for the search, retrieval, and quality appraisal process of the studies. In addition, the article has also included a chronological list of randomized trials based on the search criteria given for this study. This table was organized by the intervention, sample size, testing and follow-up (FU) time, outcome measurements, and results. Quality assessment of each randomized trial with the application of the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines was discussed in the review (see Table 2).
Quality assessment of each randomized controlled trial with the application of the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines.
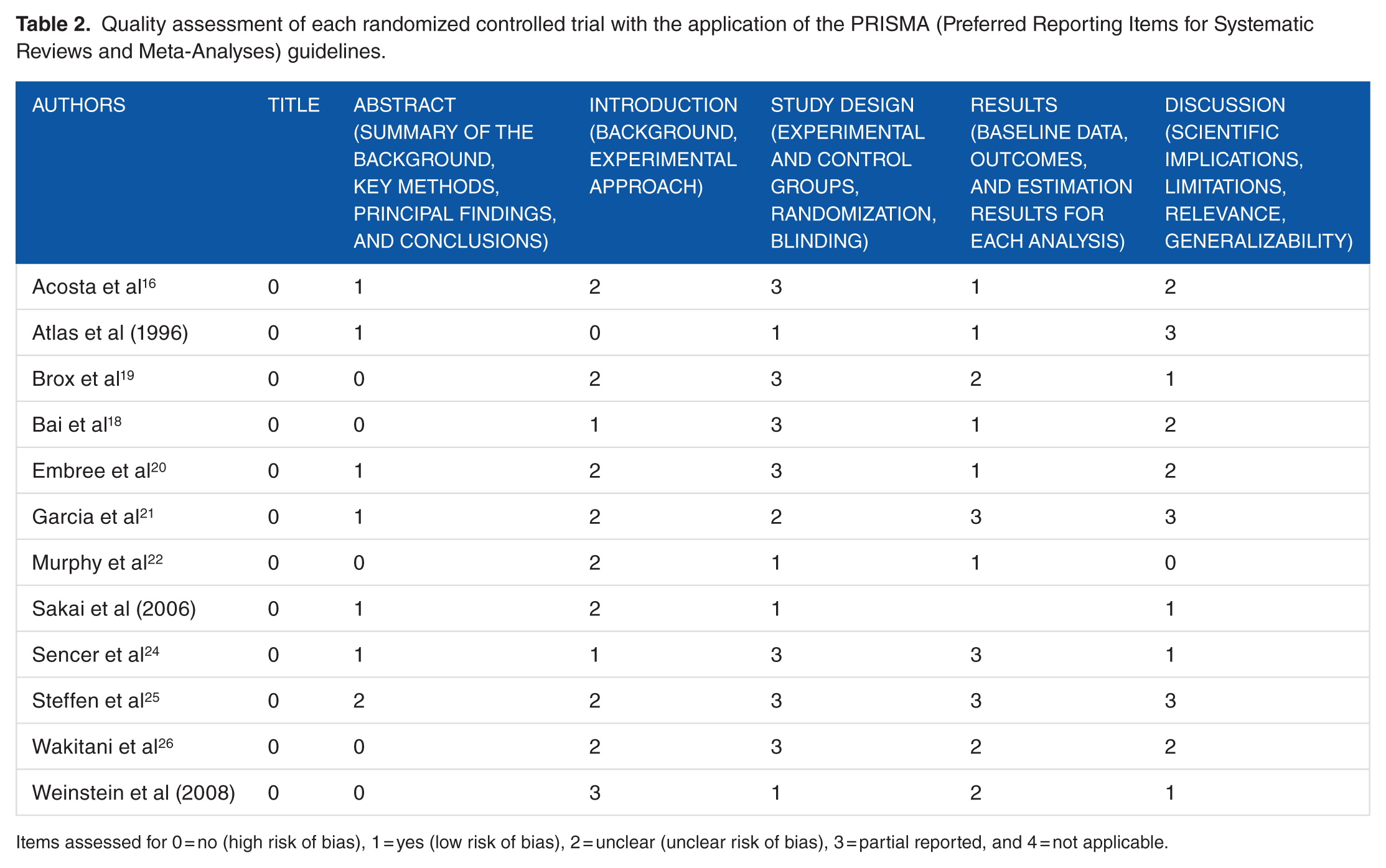
Items assessed for 0 = no (high risk of bias), 1 = yes (low risk of bias), 2 = unclear (unclear risk of bias), 3 = partial reported, and 4 = not applicable.
Results
Surgical
“The Gold Standard Technique” for lumbar spinal stenosis (LSS) treatment is microsurgery using microscope instruments to realize microsurgical decompression with segmental stabilization.8,28
Advantages
Surgical treatment allows decompression of the spinal canal and spinal nerves bilaterally through a unilateral approach. This surgical technique also decreases the trauma associated with the paravertebral muscles on the side of the patient in which the incision is made. This approach results in the preserved vascularization of the skin. 8
Complications
The long surgery time of this procedure is a major disadvantage to its usage and effectiveness. If inadequate decompression occurs, unfavorable clinical outcomes such as radiation exposure, dural tear, and a steep learning curve may arise.8,28
The New England Journal of Medicine published a large randomized and crossover study from Weinstein et al (2008) that reported the 2-year outcomes comparing surgical versus nonsurgical therapy for disk disease. The major outcomes that were assessed were measures of pain and physical functioning. These measures were reported on the Medical Outcomes Study 36-item Short-Form General Health Survey (SF-36) and on the Oswestry Disability Index (ODI). This study found that surgical treatment was more effective compared with nonsurgical treatment in relieving symptoms associated with IDD and in the improved physical functioning of patients at 12-week FU time. There was also notable evidence suggesting that physical functioning of patients in the nonsurgical group improved only slightly during the 2-year period. Patients with spinal stenosis who underwent surgery showed significantly greater improvements in pain, physical functioning, life-satisfaction, and self-rated progress than patients who were treated by a nonsurgical method.
The results of this study were supported from the implication of specific criteria used to include or exclude subjects, the large sample size, and adjustment for potentially confounding variables that were observed when monitoring patient’s baseline characteristics. However, the major limitation regarding this study was the amount of failure to randomize subjects. This limitation has the potential to reduce the power of the intention-to-treat analysis which was used to show the effects of each treatment. This study was also limited by the fact that in the nonsurgical treatments, there was a great degree of variability among the treatment protocols because a standardized protocol for nonsurgical treatment was not clinically feasible.
Endoscopic
The microendoscopic technique to ID treatment is used in spinal lumbar stenosis and is a less invasive form of surgery. However, there is no valid evidence from RCTs that examined the effectiveness of transforaminal endoscopic surgery, and the studies which have reviewed the effectiveness of the surgery were of poor methodological quality. 29
Advantages
The technique of using small incisions with less invasion of paraspinal muscle is an advantage toward the use of this procedure. Paraspinal muscle is not detached from the lamina of the vertebrae which results in less trauma to the surrounding tissue. Generally, the microendoscopic technique is a safe procedure that minimizes the resection and compression of tissue with minimal blood loss and is usually associated with earlier return to activities and work. 8
Complications
The field of view through the endoscope is limited which makes it difficult to evaluate the amount of bone that has been resected. Percutaneous transforaminal endoscopic discectomy is a widely accepted method used in the treatment of lumbar disk herniation. However, patients who have a high iliac crest, especially at the L5/S1 vertebral segments, have displayed difficulty in this procedure. The observed pain and difficulty in these patients is due to the nerve block that is applied to the iliac crest. 18
Bai et al investigated the efficacy of the bone puncture technique used through a transiliac approach to for the treatment of L5/S1 IVD herniation. This RCT found significant differences in postoperative pain and satisfaction scores between group undergoing intervertebral endoscopic discectomy versus patients in the conventionally treated group. The MacNab scale was used to evaluate patients who rated their postoperative functioning as excellent, good, or poor. The improvement seen in the endoscopically treated group compared with the conventional group indicates that the transiliac surgical approach is a safe, effective, minimally invasive method for treating IDD.
Sencer et al evaluated the long-term outcomes of patients who underwent endoscopic surgery for the treatment of IDD after a 1-year FU. Similar to most of the reviewed literature, the ODI was used to analyze treatment outcomes. During the FU period, 114 patients had no complaints, 30 patients had occasional pain, and 19 patients showed no signs of improvement or in the reduction in pain. As far as the complications associated with endoscopic surgery were concerned, 6 subjects experienced dural tears, whereas 5 patients experienced neurological deterioration.
It was unclear how the researchers classified the neurological deterioration of each patient, which was one of the limitations regarding this trial. After the data were analyzed, the researchers suggest that despite the difficulties of acquiring this new technique, good results can be achieved with sufficient experience. Fully endoscopic interlaminar or transforaminal surgeries may be a safe and effective treatment modality for lumbar disk herniations.
Conventional
Fusion
Procedures which involve fusion techniques, especially for those that require instrumentation, can be associated with high costs and contradictions. This type of treatment is best used for preoperation (preop), intraoperative instability or postoperatory listhesis. 8
Advantages
Laminectomy is a conventional treatment procedure that has been accepted as the ideal treatment method in spinal stenosis.8,22 This treatment is used for the adequate and safe decompression of LSS and is notable for its significant reduction in unfavorable symptoms and disabilities. There has also been a strong correlation between laminectomies and an improved health-related quality of life.
Complications
The most common complication that could arise due to conventional treatment is tears in the dura matter that may often lead to cerbrospinal fluid fistulas or possibly a pseudomeningocele. Patients may also be subject to nerve root lacerations, arachnoiditis, venous thrombosis, urinary tract infections, or superficial wound infections as a result of fusion treatment applications. 28
Prior to the study published from Brox et al, there has only been one randomized study which evaluated the effectiveness of lumbar fusion. The Swedish Lumbar Spine Study suggests that lumbar fusion was more effective than physiotherapy. 19 Brox et al compared the efficacy of lumbar fusion versus cognitive intervention and exercises in patients with disk degeneration in a single-blinded randomized study. After a 1-year FU visit, the ODI was used to determine group differences in pain, use of analgesics, depression, satisfaction with life, and the ability to return to work. The measures from the ODI showed equal improvement in patients with chronic low-back pain.
Nonsurgical treatment
A nonsurgical approach for treating IDD which is aimed toward targeting the etiology of diseased patients may be best in improving pain and function. This treatment protocol would attempt to mobilize the affected limbs, decompress the nerve roots that are involved, as well as focusing on breaking up adhesion, thus releasing nerve root entrapment. 22
Murphy et al attempted to assess the results of a nonsurgical intervention strategy for patients diagnosed with IDD that placed emphasis on distraction manipulation and mobilization of the affected nerve roots. Significant improvement in disability was observed in most of the sample population, and the improvement scores among each treatment group appeared to be consistent over an average of 16.5 months once the treatment had been removed. The consistent long-term improvement may be positively correlated with the emphasis placed on the management strategy in treatments which are designed to specifically address the pathophysiology of IDD and on exercises that were designed to accompany the distraction and neural mobilization techniques. During this study, there were only 2 patients in the sample who required surgery. This evidence suggests that the nonsurgical treatment approach may be an effective alternative to surgery for patients with IDD. From the findings implicated in this study, it may be reasonable to conclude that a nonsurgical treatment approach is a viable alternative to surgery for patients with IDD.
The major limitation of this study performed by Murphy et al was the inability to randomize the control group. Also, there was no confirmation of an appropriate diagnosis of IDD. These patients were included into the study based on the presence of low-back and/or leg pain. This study was also limited by its reported statistical findings which may have been statistically significant, but not clinically significant. Average change in pain intensity was reported to be 1.6 on the rating scale implicated in this study when a change in 2 points in considered to be clinically significant.
In the Maine Lumbar Spine Study, Atlas et al compared nonsurgical management with surgery in 141 patients who were diagnosed with IDD. The researchers found that after a 1-year FU, the surgically treated group showed a significant improvement in disability and functional status compared with the nonsurgically treated group. After a 4-year FU, results have shown that the nonsurgically treated group barely exhibited any signs of improvement in functional status compared with the surgical group. 30 This is juxtaposed to the improvement that was seen in the study performed by Murphy et al.
Stem cell therapy
Few studies have been published regarding the efficacy of stem cells as a regenerative therapy in patients subjected to disk degeneration. The researchers were also not able to locate RCTs that compare stem cell therapy with surgical treatment for IDD. However, the current researchers were able to review studies that analyzed the regeneration of the IVD in comparison with neutral controls.
The application of MSCs for IVD regeneration has been considered as a potentially viable approach. 25 Acosta et al injected damaged porcine IVDs with MSCs. Discs were then harvested at 3, 6, and 12 months. At each FU, there were no viable MSCs, along with any signs of proteoglycan synthesis. One possible reason for this includes the larger disk size and therefore the greater nutrient restriction present in the porcine model as compared with small animal models. This larger disk size more closely mimics the conditions in adult human IVDs, where nutrients must travel up to 8 mm from the terminal end of the blood vessel to cells in the center of the disk.
Sakai et al used bone marrow MSCs into a rabbit model of with a degenerated IVD to determine whether stem cells could repair the fibrocartilage in comparison with normal controls. Results suggested that after MSC transplantation, degenerated discs of MSC-transplanted group animals regained a disk height value of about 91%, magnetic resonance imaging signal intensity of about 81%, compared with noncontrol group discs. 31 To complement this study, researchers in the Wakitani et al study have used bone marrow MSC transplantation for tissue repair. The purpose of this study was to use these cell transplantations to repair defects in human articular cartilage in osteoarthritic knee joints. Once the transplantation methods were applied to the damaged cartilage, histologic changes in the cell-transplanted group versus the cell-free group were observed. The mean total grading scores were greater for the cell-transplanted group. In the cell-free group, the scores were significantly different from those of the cell-transplanted group (P = .0471, .0454). The findings of this study suggest that bone marrow MSC transplantation is easy to use clinically because cells are easily obtained. Mesenchymal stem cells can also replicate without losing their capacity of differentiation. 26 Mesenchymal stem cell transplantation procedures emphasize the availability and efficacy of this type of procedure for the repair of articular cartilage defects in humans. This procedure has the potential to induce similar morphological changes in IVDs and could be an effective therapeutic treatment for a patient with IDD.
Stem cell–based transplantation procedures encounter various obstacles that can negatively influence the treatment outcome. Embree et al suggested that the use of endogenous stem cells to regenerate injured tissue could bypass these obstacles. This study induced damage in the TMJ of a rat model for the purpose of using FCSCs to regenerate the damaged fibrocartilage. The results of this study have shown the efficacy of FCSC to repair fibrocartilage of an injured TMJ joint. The significance of these findings is the possibility of using FCSCs as a potential noninvasive stem cell–based strategy to treat fibrocartilage degeneration, especially in patients with IDD.
Although these findings may seem to have significant clinical applications, the conclusions made by the research are accompanied with a variety of limitations. Although fibrocartilage tissues consist of the TMJ, IVD, and knee meniscus, the development, function, biomechanical properties, and cellular and molecular properties are quite different among each type.32,33 Therefore, variations in FCSC applications would be needed, and the current findings of the study may not be generalizable to every type of fibrocartilage in the body. Under these circumstances, therapies may have to be adjusted for each fibrocartilage tissue type.
Discussion
Critique of current studies
In the current review, the available evidence regarding the treatment outcomes of surgical, nonsurgical, and stem cell therapy was systematically reviewed and summarized. The reviewed literature suggested that no clinical significance exists between surgical and nonsurgical treatment for IDD. Therefore, the researchers suggest that the decision to undergo surgical or conservative treatment should depend on the patient’s state of health at the time of surgery, as well as any other potentially alarming factors (altered mental status, level of consciousness, comorbidities, etc) that could be exacerbated with the proposed treatment. Both MSCs and FCSCs may be effective therapeutic options for the regeneration of a degenerated IVD. However, there have not been RCTs that studied the treatment outcomes with the use of stem cells against other treatment modalities (ie, surgery, conservative treatment). To move forward in the search of finding an effective treatment protocol for IDD, further research needs to be implemented that addresses the strength of association between each treatment while minimizing the limitations discussed in this review.
One of the limitations of this is the discrepancy among the methods and results of the studies that were reviewed. The limited number of the reviewed literature due to the specific inclusion criteria was a major limitation to this review. However, the 12 studies included in this article were consistent with the inclusion criteria and specifically focused on direct comparisons between each intervention that was studied. The greater specificity of the included literature enhanced the clinical significance of the current review. This study was also limited by the fact that the authors have failed to perform the homogeneity test, which could have affected the significance of the studies that were used in this review. Also, there was an inconsistent time frame used when selecting the literature among the different databases used. This was to accommodate a particular article that was not available to the authors in the other databases used.
In terms of outcomes, patient-reported clinical outcome measures were assessed. A limitation of the current review is that different scales were used within the literature that measured patient’s mean improvements in disability, pain, function, and muscle strength. The ODI seemed to be the most accepted scale to measure patient-reported clinical outcomes, whereas other assessments such as the Short-Form Health Survey and MacNab scores were also consistently seen. This variability in outcomes measures limits the review’s ability to accurately determine the exact significance of a difference between each experimental group, thus affecting the researcher’s assessment of a more superior form of treatment for patients with IDD.
Furthermore, the sample sizes of most studies were small, and different outcome measures were used. In addition to small sample sizes, most of the experimental designs of the literature reviewed (ie, Brox et al) consisted of short observation times.
The technological disadvantages of the procedures themselves may have also limited the studies reviewed. Contradictions ranging from difficulty to break the iliac region, iliac pain, vascular injury, uncontrolled bleeding, immune reactions, etc, could have all influenced the findings.
A significant criticism of current in vivo studies that have investigated the implantation of MSCs is that they inadequately replicate the environment of the human disk that would be seen in IDD. This is due to the fact that in in vivo studies, MSCs have been implanted either into healthy and young discs3,16,26,31 or into discs where degeneration was induced through injection into the NP.2,20,34,35 Although these techniques have been shown to induce degeneration of the NP and annulus fibrosis, there is no evidence that they lead to the damage typical seen in degenerated IVDs.
Future directions
This systematic review analyzed currently published literature to evaluate the treatment outcomes of surgical, nonsurgical, and stem cell therapy for patients with IDD. In the future, development of a standardized in vivo model that more accurately mimics disk degeneration in humans would allow for more meaningful study of all therapies targeting molecular and cellular components of degeneration. Further research should also investigate the direct comparison between stem cell transplantation (ie, FCSCs, bone mesenchymal transplantation) versus surgical treatment. The surgical comparison group against stem cell therapy could consist of microsurgery, conventional fusion procedures (ie, laminectomy), or endoscopic procedures, although it would be ideal to compare microsurgery with stem cell therapy due to its consideration for being the “gold standard” treatment procedure for IDD. Future research should also consider comparing the treatment outcomes of patient’s with IDD who were treated through nonsurgical approaches versus stem cell therapy. However, high costs of RCTs in this type of research may limit further investigation. Regarding stem cell therapy, one of the main obstacles is creating an animal model that can replicate the microenvironment seen in IDD. 36 Once an animal model has been established, more preclinical data will be available for collection in a directed way with favorable conditions.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Analyzed the data: DI, MS. Wrote the first draft of the manuscript: DI. Contributed to the writing of the manuscript: DI. Agree with manuscript results and conclusions: MS Jointly developed the structure and arguments for the paper: DI, MS. Made critical revisions and approved final version: DI, MS All authors reviewed and approved of the final manuscript.
