Abstract
Introduction
Fifty percent of people living with schizophrenia do not receive proper treatments, and adherence level has been reported as low as 65%. Furthermore, the level of satisfaction has been reported to be very low in this population.
Objective
The purpose of this study was to evaluate treatment satisfaction, adherence, and the prevalence of drug therapy problems (DTPs).
Methods
A hospital-based cross-sectional study was carried out on 118 patients with schizophrenia. DTPs, adherence, and treatment satisfaction were determined using the Cipolle, Morisky, Green, and Levine, and Treatment Satisfaction with Medicines Questionnaire tools. The data were then entered using Epi-Info™ version 7.2.1 and SPSS version 22 was used for analysis. Descriptive statistics were used to summarize patients’ characteristics. Univariate and bivariate logistic regressions, with a significance threshold of P < .05, were used to analyze the associations.
Results
DTPs were found in 52.5% (P < .001) of the participants. The most often detected DTPs were ‘adverse drug reaction', (26.1%); ‘dose-too-low', (20.5%); and ‘ineffective-medicine therapy', (20.5%). Risperidone was the most prevalent medication (79, 47%) found in DTPs. DTPs were associated with age ≥ 65 years [AOR = .044, 95% CI (.003-.741); P < .030], drug-source [AOR = .774, 95% CI (.070-.826); P = .241], treatment duration [AOR = 5.820, 95% CI (1.451-23.342), P = .013], and the number of drugs taken [AOR = 5.936, 95% CI (1.623-21.71), P = .007]. Adherence status revealed that 69 (58.5%) of the participants were poorly adherent to their treatment. Overall, 68.8% of those who took part in the study were satisfied according to satisfaction ratings.
Conclusions
There is a high burden of DTPs in the study setting in the form of Adverse drug reactions, low dose schedules, and ineffective treatment associated with poor medication adherence; even though two-third of the participants were found to be satisfied with the clinical services given at the clinic.
Introduction
Schizophrenia is one of the major mental health problems causing severe disability and requiring rapid treatment with the earliest signs of psychotic episodes.1,2 Schizophrenia is associated with a chronic relapsing course and significantly affect treatment outcomes.3,4 In 2017, the World Health Organization (WHO) reported that schizophrenia affects 21 million people worldwide.4,5 The lifetime prevalence of schizophrenia is estimated to be very low (.5%), however, once it occurred the risk of premature death is expected to be as twice as the death from any other causes among the general population. 6 The use of drugs remains the cornerstone of therapy like other chronically debilitating diseases. 7 Proper utilization of medicines for the intended use largely depends on several related factors. 8
Drug therapy problems (DTPs) are any unintended incidents related to drug therapy that actually or potentially result in negative consequences to the goal of the treatment under the plan. 9 DTPs are categorized into seven major classes. These include; dosage too low, dosage too high, need additional drug therapy, unnecessary drug therapy, ineffective drug therapy, non-adherence, and Adverse Drug Reactions (ADRs). 10 DTPs are hence a major public health concern that could occur anywhere in the globe with no limit for a boundary. 11 Studies revealed that 5-10% of hospital admissions are associated with DTPs 12 and treatment adherence has also been used as one of the seven categories under DTPs that could affect patients proper drug therapy. 13
Treatment satisfaction is also a related factor that affects treatment outcomes and largely the preparedness of the psychosocial aspect of the patients to deal with their treatment. Satisfaction is an impression gained (positive or negative) by patients concerning the issued health services in general and has a real impact on the patient’s health-related decision-making.14,15 The negative impression of patients towards treatment strategies could have serious consequences on medication adherence and are of particular concern in patients with chronic diseases. 16 It has been estimated that up to 50% of patients with chronic illness discontinued their medication without seeking medical advice simply because of the issues related to satisfaction with treatment strategies. 14 Therefore, healthcare professionals should be equipped with proper knowledge, attitudes, and experiences to handle their patients’ level of satisfaction. 17 Accordingly, one in two people living with schizophrenia do not receive proper treatments,18-20 and adherence level in this population has been reported to be as low as 65%, 21 Furthermore, their level of treatment satisfaction was reported to be low compared to the general population. 5
The high risk of mortality associated with treatment failure, relapse, and refractoriness makes schizophrenia very challenging in clinical setups. 22 If DTPs and related issues are not resolved in a timely fashion, severe clinical consequences will result in the form of treatment failure, morbidity, mortality, decreased quality of life, increased health care costs, and other harms. 23 Addressing DTPs, treatment satisfaction, and adherence is, therefore, will bolster clinical services, alleviate the burden of disease, and dictate treatment outcomes properly. Every healthcare practitioner should be responsible for helping patients with such problems that require a certain level of professional activity to identify, prevent, and resolve problems. 24
In Ethiopia, studies regarding DTPs in patients with schizophrenia are generally insufficient. The current study aims to determine DTPs, identify medication adherence, and assess the level of treatment satisfaction among patients on follow-up care at the psychiatry clinic of Tikur Anbessa Specialized Hospital (TASH), Ethiopia.
Methods
Study design
The study design was a hospital-based cross-sectional study, carried out at the psychiatric clinic of TASH, Addis Ababa, Ethiopia. TASH is the oldest and the biggest governmental teaching referral hospital in the country, affiliated with Addis Ababa University (AAU). Approximately 230 patients with schizophrenia are visiting the clinic annually and the clinic is serving patients four mornings per week.
Study period
The study was carried out for one year between July 2017 and January 2018 as part of the Medication Therapy Management Project which ran between 2017 to 2021.
Source population
Sources population was all patients visiting the TASH psychiatry clinic for different problems and management.
Study population
The study population were all patients with schizophrenia visiting the hospital during the data collection period and fulfilling the inclusion criteria.
Inclusion and exclusion criteria
Study participants with ages greater than 18 years old, and who had been on follow-up care at the psychiatry clinic for a minimum of 6 months were included. Severely ill patients requiring such as severe somatic diseases, concomitant forms of dementia or mental retardation cases that requiring urgent medical therapy, unwilling individuals to participate in the study, as well as patients with incomplete medical records, were excluded.
Sample size determination
The sample size was calculated using a single proportion formula with the assumption of a 5% margin of error, 90% confidence interval, and 24.4% prevalence of drug-related problems (DRPs) in patients with schizophrenia from a prior study. 25 The sample size was determined using an estimated population size of 230 schizophrenia patients who visiting the hospital annually. Using a single proportion formula, the sample size was determined to be 112 patients. Considering a 10% contingency, the sample size reached to 123. All participants fulfilling the study criteria during the study period were included using a convenience sampling technique.
Data collection procedure
Socio-demographic and clinical characteristics were collected through chart review and patient interviews using standard checklists and questionnaires. The questionnaires were prepared in English and translated into Amharic and then back-translated to English to check for accuracy and consistency. Charts were reviewed for laboratory results, current medications, co-morbidities with their treatment, relevant previous medical and medication histories, and ADRs. Adherence was measured using the free online accessible Morisky, Green, and Levine (MGL) Adherence Scale (https://www.moriskyscale.com/mgl-morisky-green-levine-scale.html#/), which is in the public domain and does not require a license fee. Patient satisfaction was assessed using The Treatment Satisfaction with Medicines Questionnaire (SATMED-Q). It is a brief, feasible, and easy to self-administer multi-dimensional generic questionnaire comprising 17 Likert-type items.1,2 The SATMED-Q investigateses 6 dimensions (undesirable side effects, treatment effectiveness, convenience to use, impact on daily activity, medical care, and global satisfaction). Two trained psychiatry nurses (for the interview) as well as the research team along with a clinical pharmacist (for chart review) did the data collection. Collected data were checked daily for completeness and compliance. An immediate correction was made if any errors were identified during review of the data. A pre-test was performed for the data collection tools on 5% of the sample before the actual data collection and close supervision was performed daily.
Statistical analysis
The appropriateness of medical therapy was evaluated using various references and guidelines. The Micromedex® drug interaction checker was used to identify drug-drug interactions. Absolute contraindications and major drug interactions were considered as significant drug interactions, whereas moderate and minor interactions were omitted. Identified DTPs were categorized as per the classification of Cipolle (modified). 3 The existence of DTPs was assessed based on established standard guidelines like the American Psychiatric Association practice guidelines for the treatment of patients with schizophrenia, the Maudsley Prescribing Guidelines in Psychiatry, Texas Medical Algorithm Project Procedural Manual, and standard books such as Kaplan BJ., Kaplan and Sadock’s Synopsis of psychiatry. All the mentioned guidelines and reference books are essential evidence-based references on the safe and effective prescribing of psychotropic agents.26-28 The data were then entered using Epi-Info™ version 7.2.1 and the statistical package for social science (SPSS) version 22 was used for analysis. Descriptive statistics such as frequency, percentage, mean and standard deviation (SD) were used to summarize patients’ characteristics. Tables and charts were used to present the results. Univariate and bivariate logistic regression analysis was performed to relate each dependent variable to DTPs and adherence. Among the univariate analysis, those variables with P < .20 were selected for multivariate logistic regression analysis. P-value <.05 was considered statistically significant. Drug risk ratio (frequency of involvement in DTPs divided by the frequency of prescription) was used to identify drugs that were prone to create DTPs.
Ethical issues
The study protocol was approved by the IRB (002/17/Pharma) of the College of Health Sciences of Addis Ababa University. In addition, permission was sought from the Department of Psychiatry. Patients/their guardians (family members) aged 18 years and above were approached and informed consent was taken after discussing the objective, benefits, and risks of the study. They were also informed that declining to participate does not affect the service they get from the clinic and are free to withdraw from the study at any time. This was followed by securing written consent. Anonymity and confidentiality were assured by removing all identifiers and restricting data access.
Results
Socio-demographic and clinical characteristics
A total of 123 patients were enrolled during the study period and data for 118 subjects were used for analysis, providing a response rate of 96%.
Socio-demographic and clinical characteristics of patients with schizophrenia attending psychiatry clinic, Tikur Anbessa specialized hospital.
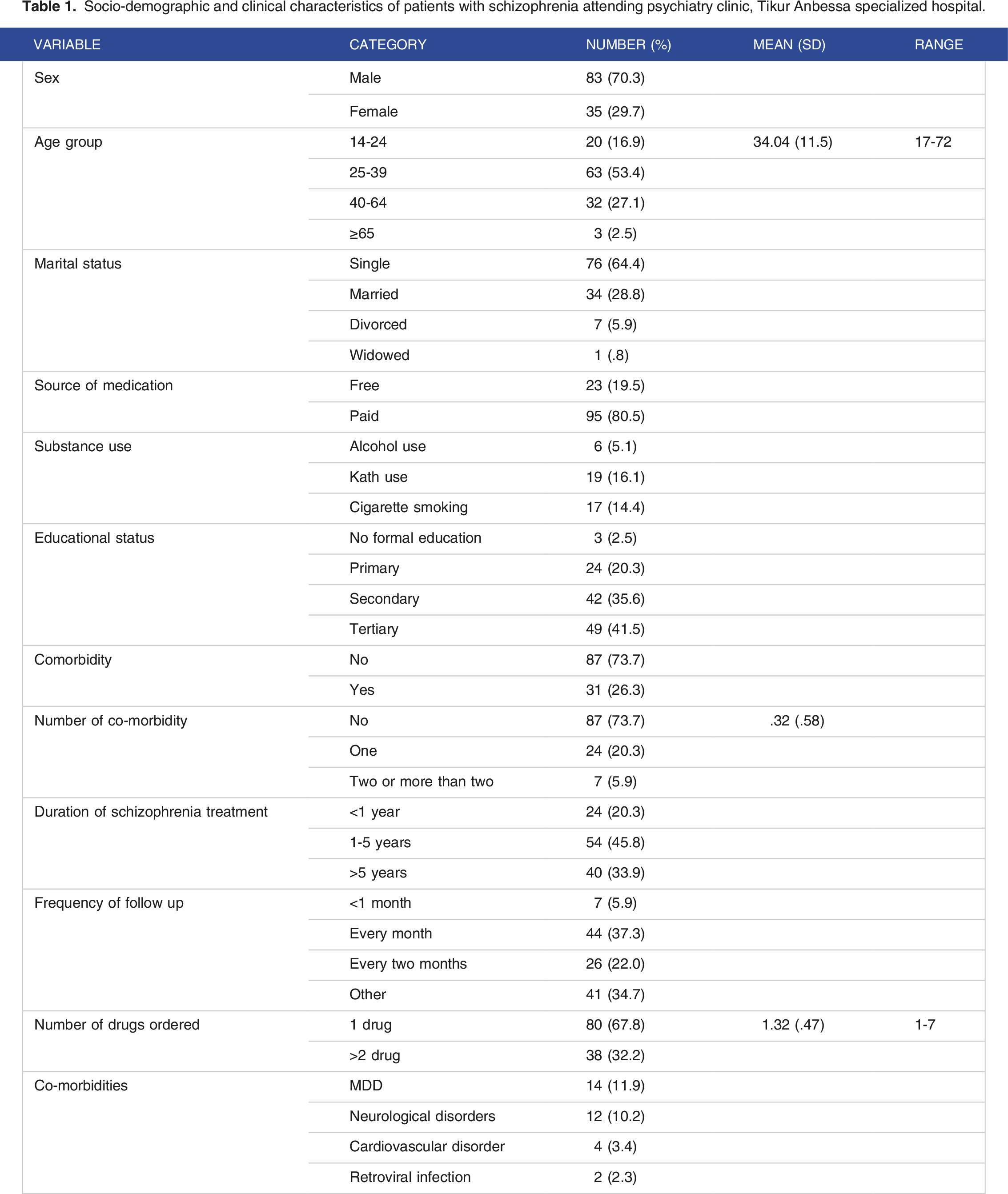
About a quarter of the partcipants (26.3%) had co-morbidities and the common co-morbidities were major depressive disorder (MDD) (11.9%), neurological problems (10.2%), cardiovascular diseases (CVDs) (3.4%, and retroviral infections (2.3%). Close to half (46%) of them were on follow-up care for the duration of 1 to 5 years. Around 37.3% of them had frequent follow-up visits (every month), (Table 1).
Medication patterns
About two-third (67.8%) of the study participants were on monotherapy and the rest received >2 medicines, with a mean and SD of 1.54 (.993) medications (Table 1). Risperidone was the single most frequently prescribed antipsychotic drug (79, 47%) followed by Fluphenazine depot (13, 7.7%), chlorpromazine (12, 7.1%), and haloperidol (11, 6.5%). Trihexyphenidyl & Fluoxetine were prescribed 9 times each, Olanzapine 5 times, Clonazepam 4 times, Carbamazepine 3 times; whereas, Thioridazine and Trifluoperazine were prescribed only once. The most frequently used route of administration was the oral route (91.5%).
Drug therapy problems
DTPs were found in 52.5% (P < .001, 95% CI = 46.2-72.7) of the study participants. A total of 88 DTPs were identified from 62 study participants. A single DTP was identified in 42 (35.6%), two DTPs in 14 (11.9%), and three DTPs in 6 (5.1%) partcipants. Of the total study participants, the average number of DTPs per patient was .75. The most commonly seen DTP categories were ADRs (26.1%), Dose too low (20.5%), and Ineffective drug therapy (20.5%) followed by drug interaction (18.2%), (Figure 1). The magnitude of specific DTPs among patients with schizophrenia attending the psychiatry clinic of Tikur Anbessa specialized hospital.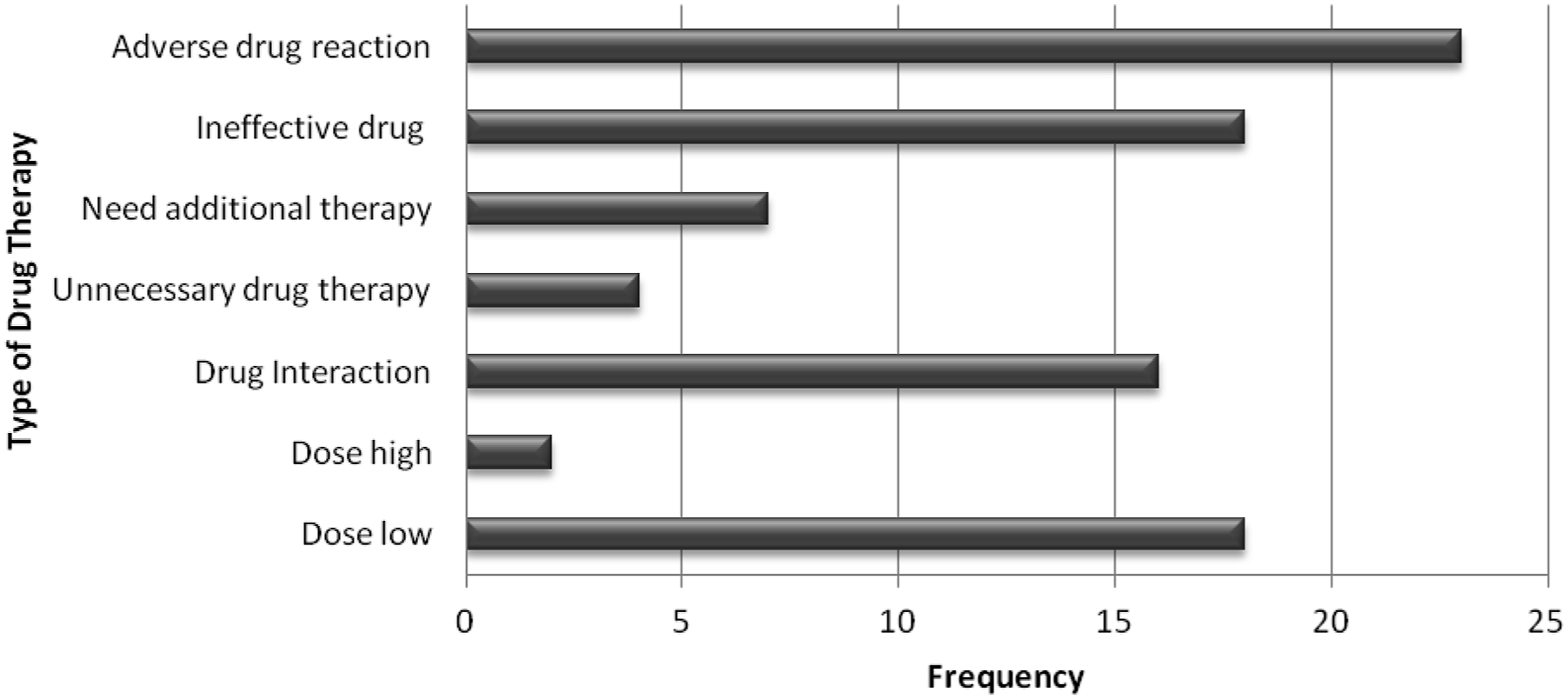
Antipsychotic medications with their specific DTPs among patients with schizophrenia attending the psychiatry clinic of TikurAnbessa specialized hospital.
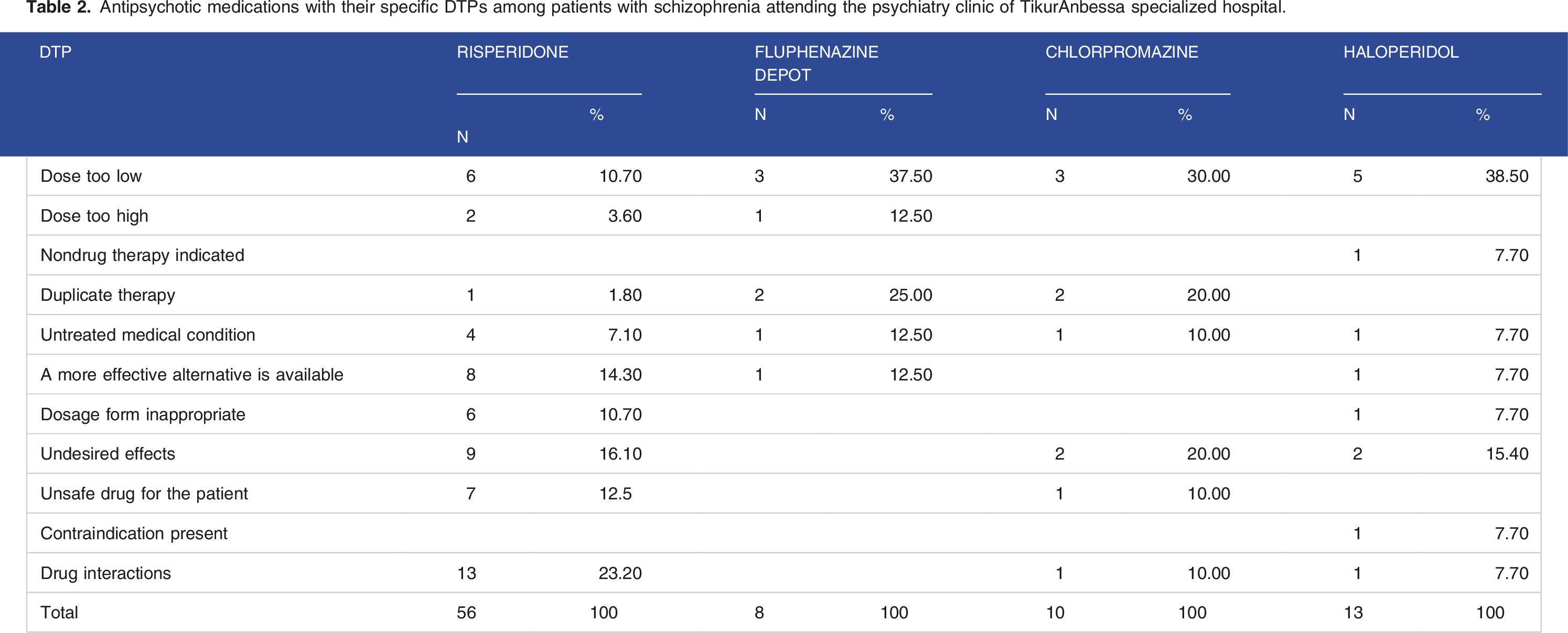
Haloperidol was found to be one of the drugs with the highest drug risk ratio (1.09) followed by chlorpromazine (.75) and fluphenazine depot (.54). All of these drugs had a risk ratio of above .5, indicating that DTP could occur in 50% of the cases, where these drugs were used. However, risperidone had a drug risk ratio of .11, which was considered as the lowest drug risk ratio.
Association studies
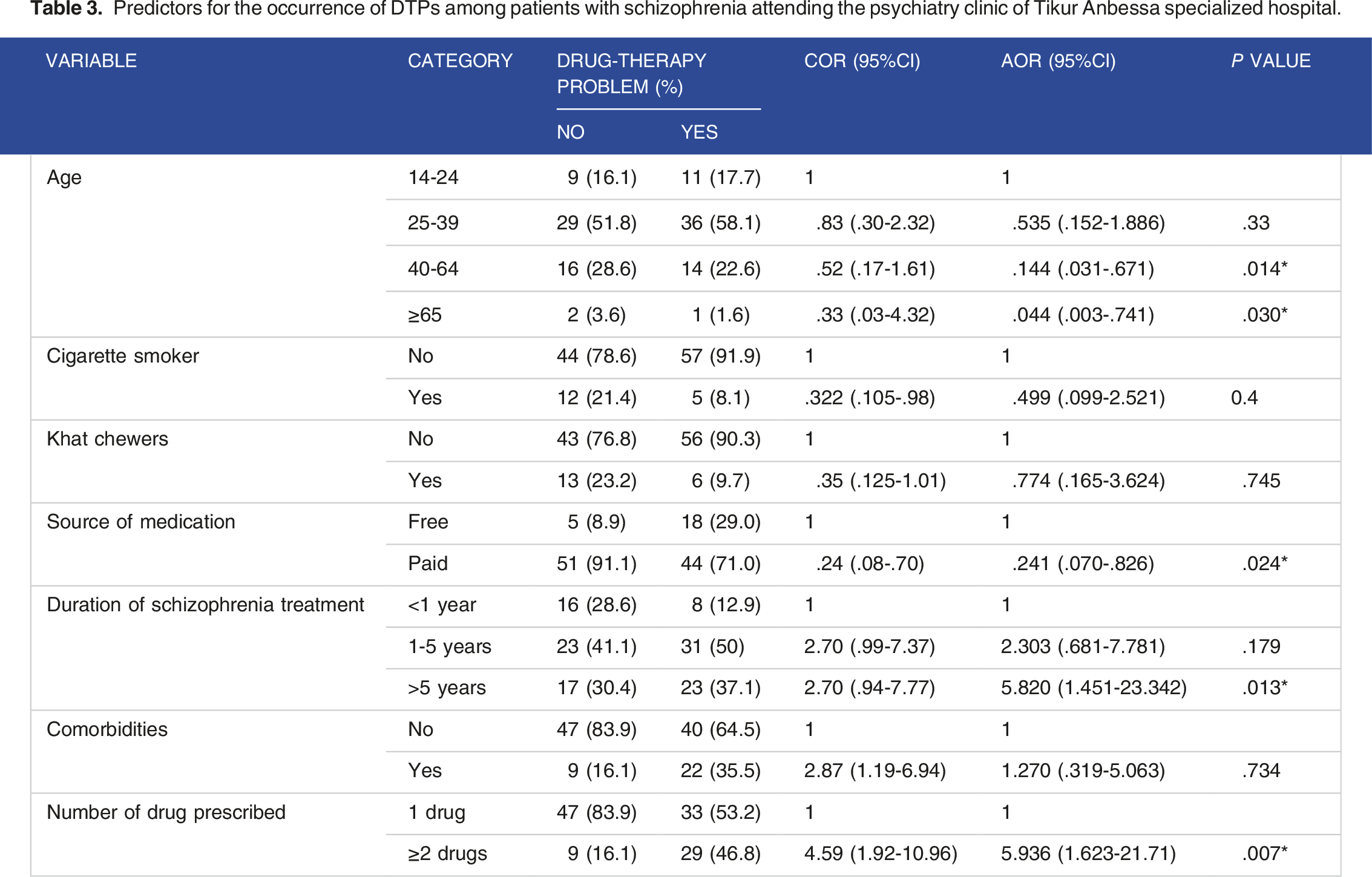
Predictors for the occurrence of DTPs among patients with schizophrenia attending the psychiatry clinic of Tikur Anbessa specialized hospital.
Adherence and reasons for non-adherence
Adherence status using the MGL scale revealed that 69 (58.5%) of the participants had poor adherence, while 35 (29.7%) and 14 (11.9%) of them had medium and good adherence. For this study, the original three categories of adherence were re-categorized into two, using two as a cutoff point. Patients with high and medium adherence were re-assigned as adherent (≤2) and low adherence was regarded as non-adherent (≥2). The reasons for poor adherence were lack of information (25%), drug products not available/affordable (17.2%), forgetfulness (15%), feeling better (13.2%), and feeling worse (12.4). Other variables were ‘Patients didn’t follow the appointments properly (Poor follow-up by Patients)’ (43, 11.5) and Unclear information about proper drug usage (Directions not understood) (20, 5.4%).
Predictors of adherence
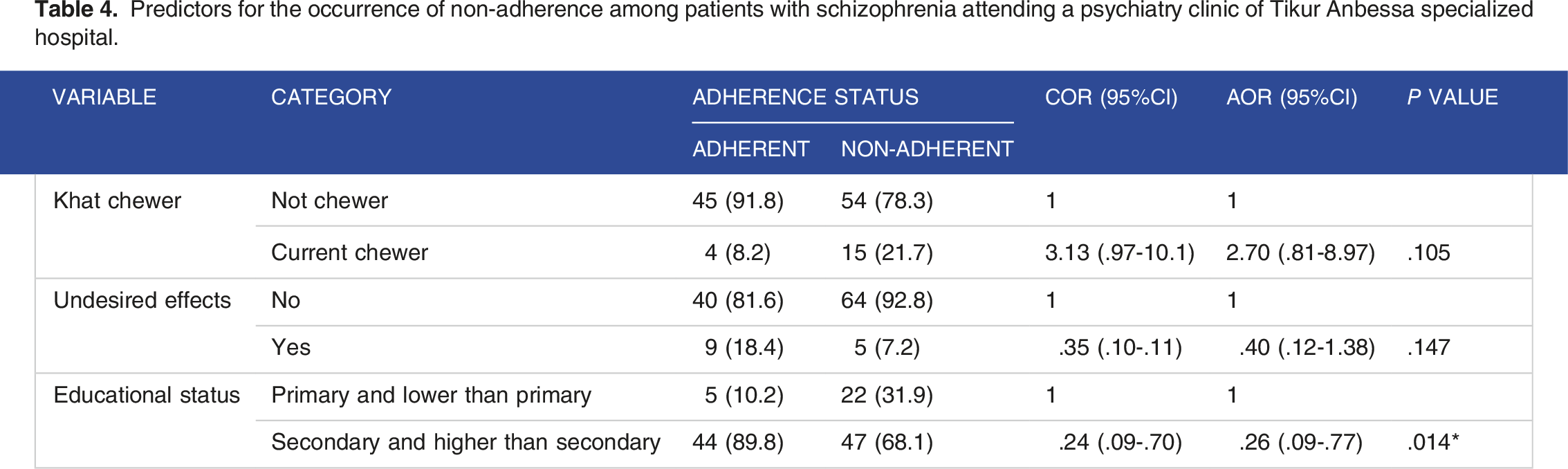
Predictors for the occurrence of non-adherence among patients with schizophrenia attending a psychiatry clinic of Tikur Anbessa specialized hospital.
Patients’ treatment satisfaction
Level of patient satisfaction among patients with schizophrenia attending a psychiatry clinic of Tikur Anbessa Specialized Hospital.

Discussion
This study aimed to assess DTPs, medication adherence, and treatment satisfaction among patients with schizophrenia. Risperidone was the single most frequently prescribed antipsychotic drug (47%) followed by Fluphenazine depot (7.7%), chlorpromazine (7.1%), and haloperidol (6.5%). A similar finding was found from a study done in Australia, which indicated that risperidone oral and long-acting injection was the most commonly prescribed agent (31%). 4 Similarly, a study done in India reported that risperidone was the most commonly prescribed antipsychotic (44.71%) followed by olanzapine (34.81%), and aripiprazole (7.12%). 29 Another study conducted in India also showed that the commonest antipsychotic drug prescribed was olanzapine (48.6%) followed by risperidone (45.8%). 5
The reason for the high prevalence of risperidone's use in our study could be the low cost and non-availability of alternative antipsychotic drugs, which, in turn, made it difficult for psychiatrists to switch to another antipsychotic. This was supported by the Indian study. 29
Similarly, a study done by Kogut et al. (2005) on atypical antipsychotic medications showed about one-third of patients were prescribed a dosage that was not within the recommended range. The degree of inappropriate dosing was about 27%, where patients received a medication below-range dosage, which was below the range recommended in the product labeling. Six percent of patients received medication at dosages that were higher than recommended in the product labeling. 6
In our study, the prevalence of DTP was 52.5% (P < .001). DTPs were common among patients with chronic illness,7,8 even if the complete DTPs in patients with schizophrenia were largely lacking.
The most commonly seen DTPs in our study were ADRs (26.1%), dose too low (20.5%), ineffective drug therapy (20.5%) followed by drug interaction (18.2%). These findings were in agreement with the study done in India, where 13.8% were receiving high doses, 24.13% were receiving low doses and 31% were on a combination of typical and atypical antipsychotics. 9
Switching drug therapy was found in 55.5% of participants identified as receiving ineffective treatment in our study and this finding was higher than the study done in India, where switching was observed only in 26% of patients. The reasons for the switch of drug therapy included lack of efficacy, ADRs, high cost, or non-availability of the drug. 29
In our study, only 2 individuals were found to take their medications without tapering them to the minimum effective dose in the maintenance phase of treatment. Although the finding that only two partcipants experienced such scenario appears to be good, there is a need to ensure that each individual on antipsychotic treatment should receive the desired drug therapy as recommended by Remington and colleagues in their randomized control trial. They recommended that patients who take their dose of antipsychotics every other day instead of daily, gradually reducing the dose to the minimal effective dose: a dose by which the patient does not suffer from side effects but also does not relapse should be considered. 10
In our study, an undesired effect occurred in 14 (15.9%) participants and this was higher than the study done in India and UAE, where 6.41% and 10.2% of the study participants, respectively, were reported to develop undesired effects.11,12 In contrast, our finding was lower than two studies done in India, where the undesired effect rate was reported to be 20.4% and 43.5%, respectively.13,14 The reason for the lower rate could be under documentation in medical records and/or the method of data collection as in the case of prospective and retrospective studies. Similar scenarios were shown by different researchers, and Cortese et al. (2004) explained that it might be due to physicians’ under-detecting and under-recording of undesired effects. Similarly, a study done in Ireland stated that documentation regarding undesired effects was found only in 14% of patient records. 15
The prevalence of major drug interactions in our study was 13.6%, where risperidone and fluoxetine had the highest frequency. This finding was lower than the study done in Pakistan, where 51.7% of patients had drug-drug interactions. The reason for this variation could be due to exclusion of severity level and inclusion of many psychotic ilnesses other than schizophrenia in the Pakistan study as well as usage of a small sample size in the present study. 16 In contrast, a higher report was seen in another study from Pakistan (64.8%), and a similar but opposite reasons can be applied to this. 17
Our study revealed that the likelihood of DTP occurrence decreases as age increases from 14-24 age group to the 40-64 and >65 age group. This could be due to the protective effect of age on the development of DTPs, which implies the higher the age of the patient the lesser the occurrence of DTPs. However, the genuine reason might be associated with the time of the disease presentation, and the peak of the disease presentation has been reported during young age between 12-24 years. 18 The other explanation for this might also be as age increases patients may become more cooperative with the treatment plan and thus help to improve therapeutic alliance with the psychiatrist. These explanations have been supported by a study conducted in South Africa, where the relapses of schizophrenia were more likely to occur in the younger patients, ie, the age group <50 years was more likely to relapse. 19
Duration of schizophrenia treatment had an association with DTPs. Patients with >5 years of treatment were 5.8 times more likely to develop DTPs compared with the duration of treatment of less than one year (P = .013, 95% CI = 1.451-23.342). A cross-sectional study conducted in Ethiopia showed that a longer duration of antipsychotic treatment was significantly associated with a risk of DTPs. 20 In addition, participants taking several medications or had a higher risk of experiencing DTPs (P = .007), as the number of the drug increases the probability of drug interaction increased and other drug-related factors may also increase. 21
The prevalence of antipsychotic drug nonadherence was found to be 58.5%, in which, 69 of the total study participants were nonadherent to their treatments. This finding was in line with the study conducted in Nigeria, in which the prevalence of treatment non-adherence was 51.7%. 22 The result was higher than a cross-sectional study done by Girma et al (2017) at Amanuel Mental Specialized Hospital, where the nonadherence rate was 48.4% and lower than the study done at Gondar University Hospital, Northwest Ethiopia, where the non-adherence rate among patients with schizophrenia was 75.7%. 23 The reason might be due to the use of different types of adherence assessment tools, patient density, and the variation in the study area.
In our study, educational status was significantly associated with nonadherence, where patients with the educational level of high school and greater were .26 (P = .014, 95% CI = .09-.77), 4 times less likely to be non-adherent than patients who only had primary and lower than primary school education. This was similar to the study done in northern Ethiopia where educational status was to some extent associated with adherence and illiterate patients were (AOR = .13) 7 times less likely to be adherent. 24 And it is backed by a systemic review that indicated educational status was considered as a factor for non-adherence in chronic illness treatment including psychiatry. 30
Patients’ satisfaction is a key factor in predicting patients’ treatment processes and outcomes and can influence disease control and treatment because more satisfied patients are more prone to follow the physicians’ instructions. In this study, the total satisfaction of the study participants was 68.8% and satisfaction regard to effectiveness, side effects, convenience, and global satisfaction were 63.0 ± 15.4, 72.7 ± 24.8, 69.4 ± 13.8, and 68.9 ± 14.6, respectively. The result of the study is comparable with a study done in Palestinian, where patients with schizophrenia satisfaction concerning antipsychotic effectiveness, side effects, convenience, and global satisfaction were 72.6 ± 20.5, 67.9 ± 31.47, 63.2 ± 14.3 and 63.1 ± 18.8, respectively. 31 A study conducted in Japan showed that patients taking second-generation antipsychotics have better subjective treatment satisfaction than those taking first-generation, especially in terms of side effects (87.7% vs 69%) and global satisfaction (64.3 vs 55.6.) For that reason, in addition to the regular clinical assessment, physicians should give importance to subjective treatment satisfaction. 32
Limitations of the study
A cross-sectional study variable may not be suitable to determine cause-effect relationships. Results are also not to be used as a representative of the whole population as the study was conducted in a single hospital for a limited period. The smaller sample size and the use of convenient sampling could lower the power of statistical determinations.
Conclusions
There is a high burden of DTPs in the study setting in the form of ADRs, low dose schedules, and ineffective treatment associated with poor medication adenerence; even though two-third of the participants were satisfied with the clinical services given at the clinic. The most frequent DTPs were ADRs, adose-too-low, ineffective treatment, and drug interactions. Advanced age, the source of pharmaceuticals (free or paid), the duration of therapy, and the number of medications prescribed at a time were all factors independently associated to the emergence of DTPs.
Footnotes
Acknowledgements
We would like to thank the Medication Therapy Management (MTM) thematic research project of AAU (AAU-MTM Project 2017-2022) for partly funding this research project and we would also like to thank the AAU research and technology transfer office for sponsoring this project.
Author contributions
Conceptualization: - MA, AB, ST, EE; Data curation: - GT, MA, AB, WS, ST, EE; Formal analysis: - GT, MA, WS, ST; Funding acquisition: - GT, MA, AB, ST, EE; Investigation: -MA, AB, WS, ST, EE; Methodology: - GT, MA, AB, WS, ST, EE; Software: -GT, MA, WS, ST; Supervision: -MA, WS, ST; Writing – original draft: - GTD, WS, MA; Writing – review & editing: - EE, MA, AB.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The original funding source for conducting the research was sponsored by AAU. Part of the research was also sponsored by the MTM project of AAU.
Authors’ information:
![]() ), Addis Ababa, Ethiopia;
), Addis Ababa, Ethiopia;
