Abstract
Introduction
Schizophrenia spectrum disorders are characterised by notable deficits in executive function, working memory, attention and social cognition. Previous studies in cognitive remediation therapies, of various dose and duration, have shown behavioural and neurobiological improvements. The current pilot study will be the first to test the Cogmed Working Memory Training (CWMT) program in schizophrenia spectrum disorder.
Methods
This pilot study was conducted using purposive sampling of consumers with schizophrenia spectrum disorders from a forensic mental health inpatient unit in Australia was used. Eleven participants completed 30 sessions of CWMT over a 2-month period. One participant completed 28 sessions. The primary outcome measure was the CogState Schizophrenia Battery (CSB). Secondary measures included the Brock Adaptive Functioning Questionnaire (BAFQ) and the Allen Cognitive Level Screen (ACLS). Measures were taken before and after the intervention, and at 6-months follow-up to detect maintenance of improvements.
Results
Significant improvements were seen in social cognition and emotionality. Trends toward improvement in executive function and working memory were observed in younger participants, but were not significant.
Conclusion
Findings indicate that the CWMT may be a beneficial tool for improving social cognition in patients with schizophrenia. CWMT interventions of longer than 2 months may be required to see measurable improvements in other cognitive functions. Age-related cognitive impairment should be controlled for in future studies. Larger studies should be conducted to confirm these findings.
Introduction
Schizophrenia is a chronic and debilitating psychiatric disorder, characterised by a range of specific impairments to thought, perception, mood, and cognition. 1 Affecting approximately 1 in 300 people, it is among the top 25 leading causes of disability globally.1,2 Impairments in cognition are key features of schizophrenia, particularly in executive functioning (EF), working memory (WM), attention, and social cognition.3–5
EF generally comprises a family of core cognitive processes that drive goal-oriented behaviour and complex procedures such as decision-making, problem-solving, self-regulation, planning, and cognitive flexibility.6–8 WM, sometimes defined as a core EF but often conceptualised as an independent cognitive system, involves the short term storage and manipulation of information for the execution of higher-order cognitive tasks. 9 Tests of WM are strongly correlated to general cognitive ability and are often used as predictors of cognitive function, leading some to consider WM a crucial component of intelligence. 10 Attention is a core EF that allows us to focus on pertinent stimuli while ignoring interference and irrelevant stimulus. 11 It is sometimes considered a gatekeeper for WM, as it drives processing toward relevant, goal directed information. 12 Social cognition concerns all the mental processes involved in the detection, processing, interpretation, and implementation of social and emotional communication and interaction, such as face perception, social cue perception, emotion recognition, empathy, and emotional regulation. 13
Cognitive impairment in schizophrenia can be used as a prognostic indicator, due to its close association with rehabilitation success, functional outcomes, problem-solving abilities, independent living, and social skills.14,15 These impairments are seen regardless of illness stage, and persist into the life of the patient. Meta-analyses have consistently demonstrated deficits in premorbid IQ across multiple domains, with risk of schizophrenia increasing with lower premorbid IQ.16,17 Having a higher IQ score (115 and over) was seen to be a protective factor, potentially providing a buffer with increased cognitive reserve. 16 Deficits in social cognition can interfere with social connectedness and lead to the withdrawal, isolation, and impaired daily functioning observed in schizophrenia. 13 Improvements in EF and WM could greatly improve patient health outcomes and quality of life, and reduce healthcare visits and financial expenditure in psychiatric treatment.
Forensic consumers with schizophrenia may experience even more pronounced deficits than those in residential care or in the general community. These consumers are detained under the Mental Health Act 18 as they require mental health care and treatment in a secure setting, and are frequently excluded from research. 19 Results of a multi-site European sample of consumers from forensic and general psychiatric settings found impairments in processing speed and emotion recognition to be more pronounced in the forensic sample. 20
Prior research has highlighted variations in the frontal cortex and subcortical structures in psychiatric disorders, associating these with the cognitive deficits observed. 21 The theory of cognitive control deficit in schizophrenia posits that cognitive defects are caused by the inadequate recruitment and coordination of brain regions implicated in EF, WM and social-emotional function. 22 This has been supported both by neuroimaging investigations and neuropsychiatric testing indicating reduced connectivity and the utilisation of different neurological pathways in task performance in schizophrenic individuals. 23 Imaging studies show atypical activity in the prefrontal cortex (PFC), the temporal, parietal and occipital regions, the thalamus and hippocampus. 24 General reductions in grey matter volume and cortical thickness are a common feature, particularly evident in the frontal, temporal, and parietal cortices. 25
Cognitive deficits in schizophrenia persist after pharmaceutical treatment, leaving clinicians to search for alternative interventions, such as cognitive remediation therapy (CRT). CRT is an umbrella term for cognitive training programs aimed at improving cognition, and are characterised by repeated, focused, and intensive training. 26 There is evidence to indicate that CRT can improve core domains of EF, social function and everyday functional performance.27,28 The underlying theory behind cognitive training is the principle of neuroplasticity; the process by which repeated cognitive engagement leads to changes in cortical density and organisation. 29 Brain imaging studies support the theory that improvements are due to neuroplastic alterations in brain networks. 30 Imaging studies show evidence of neural changes associated with CRT, including increased activity in areas known to be atypical in schizophrenia (numerous regions within the PFC, the insula, the anterior cingulate cortex, and praecuneus). 27 CRT has also been associated with the protection of grey matter and even enlargement of volume, indicating a potential for this treatment in the prevention or symptom reduction of schizophrenia. 31
Forms of CRT have been extensively implemented and studied in schizophrenia. Over 25 systematic reviews have so far been conducted, overwhelmingly supporting the use of CRT in this population.32–34 Studies of CRT in schizophrenia have shown long lasting improvements in WM, cognitive flexibility, and self-esteem. 35 Significant improvements were seen in WM, verbal memory, and EF for adolescents with early onset schizophrenia after 3 months of CRT, regardless of medication type. 36 Recent guidelines published by the European Psychiatric Association have even included cognitive remediation alongside pharmaceutical and physical exercise management as a recommended treatment intervention for the treatment of cognitive impairment in schizophrenia. 34 CRT studies have previously been conducted in forensic consumers with schizophrenia, finding improvements in memory, attention, negative symptoms, emotion regulation, and aggression from this form of treatment.19,37 A 3-month intervention by Pillet 38 found that CRT was the most beneficial for patients with the lowest initial performance. The elevated cognitive impairments observed in forensic consumers requires further investigation, but suggests a significant benefit of CRT for this population. The institutionalised setting in which these consumers reside provides little opportunity to practice real-world skills, making access to computer-assisted training programs essential for this cohort.
Prior evaluations and comparisons of CRT programs have been difficult due to inconsistencies in training methods, frequency, duration, and variations in targeted domains. Further research using a consistent and validated protocol is required. The Cogmed Working Memory Training (CWMT) program is an online, commercially accessible, and validated tool that includes optional interfaces (adult and adolescent) and protocols designed to be user-friendly and engaging for specific audiences. The CWMT has shown promising results in a number of prior studies involving mental health39,40 and substance use 41 but has not been used previously in people with schizophrenia or forensic inpatients with schizophrenic spectrum disorders. A prospective, self-controlled pilot study was therefore undertaken to test the feasibility of the CWMT program in forensic mental health inpatient services with schizophrenia spectrum disorders.
Aims and hypothesis
The current pilot study aimed to evaluate the feasibility and efficacy of using the CWMT program in people with schizophrenia in a forensic mental health inpatient setting. The study allows us to investigate the impact of this CRT program on individual cognitive domains and function. The following hypotheses were proposed: 1. Engagement in the CWMT program would lead to measurable improvements in cognitive functioning in one or more domains. 2. Improvements would be sustained for a period of at least 6 months after training.
Method
Study design, participants, and setting
This single-site, longitudinal, self-controlled pilot study was conducted in a large, public, forensic mental health hospital located in an Australian capital city. Eligible consumers from the hospital’s Secure Mental Health Rehabilitation Unit (34 beds) and High Security Inpatient Service (70 beds) were referred by clinical staff to researchers for recruitment and consent. Patients at these units may be treated under the Mental Health Act 2016. 18 Patients at these units were diagnosed using the International Diagnostic Classification of Diseases Criteria (ICD-10) by their treating psychiatrists and confirmed by the multidisciplinary team. This diagnostic process would include multiple psychiatric reviews and clinical observations by the multidisciplinary team over a period of several months. Consumers predominantly experience Schizophrenia, but may also have one or more comorbidities or complex medical history. Contraindications for participating included severe anxiety or depression, severe psychosis and photosensitive epilepsy.
This forensic inpatient service is managed under the public health service, and not under correctional services. The service has the physical infrastructure, policies and procedures and the specialist workforce required to accommodate patients from across the state who are involved with the judicial and corrective systems and require care in a secure setting due to significant risks and complexities. The majority admitted have either been diagnosed with, or are suspected of having, a serious mental illness and are convicted of, or are on remand and alleged to have committed a serious indictable offence. There are provisions under the Act for searches on entry, admission and where there is concern regarding risk. Due to privacy, confidentiality and risk concerns, consumers have restrictive access to mobile phones, the Internet, nail clippers, scissors, razors, all glass, and metal items (including soft drink cans). Some personal clothing items are restricted due to self-harm risks – hence shoelaces and draw strings from shorts and jackets are removed. There are provisions under the Act for patients to be placed in overnight confinement for security purposes. The service has regimented wake up times, mealtimes, meeting times, phone call times and light out times. There are procedures and policies for visitors to be approved, and scanning of visitors and their property.
Measures
CogState schizophrenia battery
The CSB was developed to provide a brief, standardized, and valid measurement of cognitive function and impairment in schizophrenia.42,43 The online test battery includes eight individual tasks that measure distinct cognitive domains. The test takes approximately 40 minutes to administer, and was overseen by occupational therapists within the clinical team.
Brock adaptive functioning questionnaire
This questionnaire was developed to measure functional impairment subsequent to head injury. 44 The BAFQ is a 68-item tool, scored on a Likert scale of zero to 4, consisting of 12 subscales: planning, initiation, flexibility, excess caution, attention, memory, arousal level, emotionality, impulsivity, aggressiveness, social monitoring, and empathy. Higher scores indicate poorer functioning. This tool was completed by the care coordinators of each patient.
Allen cognitive level screen
The ACLS is a brief, clinician administered screening tool that measures an individual’s functionality using a series of lace-stitching tasks, increasing in complexity. 45 In order to complete tasks, the participant must comprehend instructions and manipulate the material object utilising motor skills and sensory feedback. Allen’s Cognitive Levels include: Level zero (.8, coma); Level 1 (1.0 to 1.8, profoundly impaired and requiring 24-hour care); Level 2 (2.0 to 2.8, able to move around on their own, but need full-time help with activities of daily living); Level 3 (3.0 to 3.8, severely impaired cognition with an awareness of objects but not of cause and effect. Moderate supervision required); Level 4 (4.0 to 4.8, can perform goal-directed activities but fail to solve new problems. May live alone but require assistance); Level 5 (5.0 to 5.8, mild cognitive impairment with trial-and-error problem solving. May live alone with some assistance); Level 6 (6, no cognitive impairment, able to plan new activity and problem solve). 46 The ACLS gives people a score between 3.0 and 5.8, as those below 3 are unable to participate, and future planning is required for a score of 6 which the ACLS does not measure.
Intervention
The CWMT 47 is a computerised training program that targets the attention and WM of the participant. 48 The program relies on repetitive practice with a difficulty level that is customised to the abilities of the user. In the training protocol chosen, participants complete five tasks within the CWMT at each session, completing 3 sessions per week over a 10-week training period. Sessions last approximately 35 minutes, and include visuo-spatial or verbal memory tasks, such as recalling patterns or numbers, or tracking an object on screen. Each of these sessions was overseen by a trained coach or therapy aide, who provided support and positive feedback. The CWMT sessions were delivered individually or in a small group.
Procedure
All measures were delivered at baseline by trained clinicians. The CSB and the BAFQ were readministered at the completion of the intervention (10 weeks), and at 6 months follow-up (approximately eight to 9 months after baseline). The ACLS was conducted again at eight months. Participants were asked at the end of the 10-week intervention to provide feedback on the CWMT in a brief interview conducted by clinicians.
Statistical analysis
Statistical analysis was conducted using Statistical Package for Social Science (SPSS) version 28. Descriptive analysis was undertaken using means and standard deviation. Repeated measures ANOVA was used to determine changes over time. Subgroup analyses based on age were conducted where appropriate. Where the assumption of sphericity was breached, a Greenhouse-Geisser correction was used. Post-hoc analyses were conducted using Fisher’s Least Significant Difference. Outcomes were considered significant if P < .05.
Ethical considerations
The study obtained ethical approval from the participating hospital Human Research Ethics Committees (HREC/13/QWMS/47). Participants provided written informed consent to participate in the intervention, and for the use of their information. Participants deemed too cognitively impaired to consent by their clinical treating team were not recruited into the study.
Results
Participant demographics.
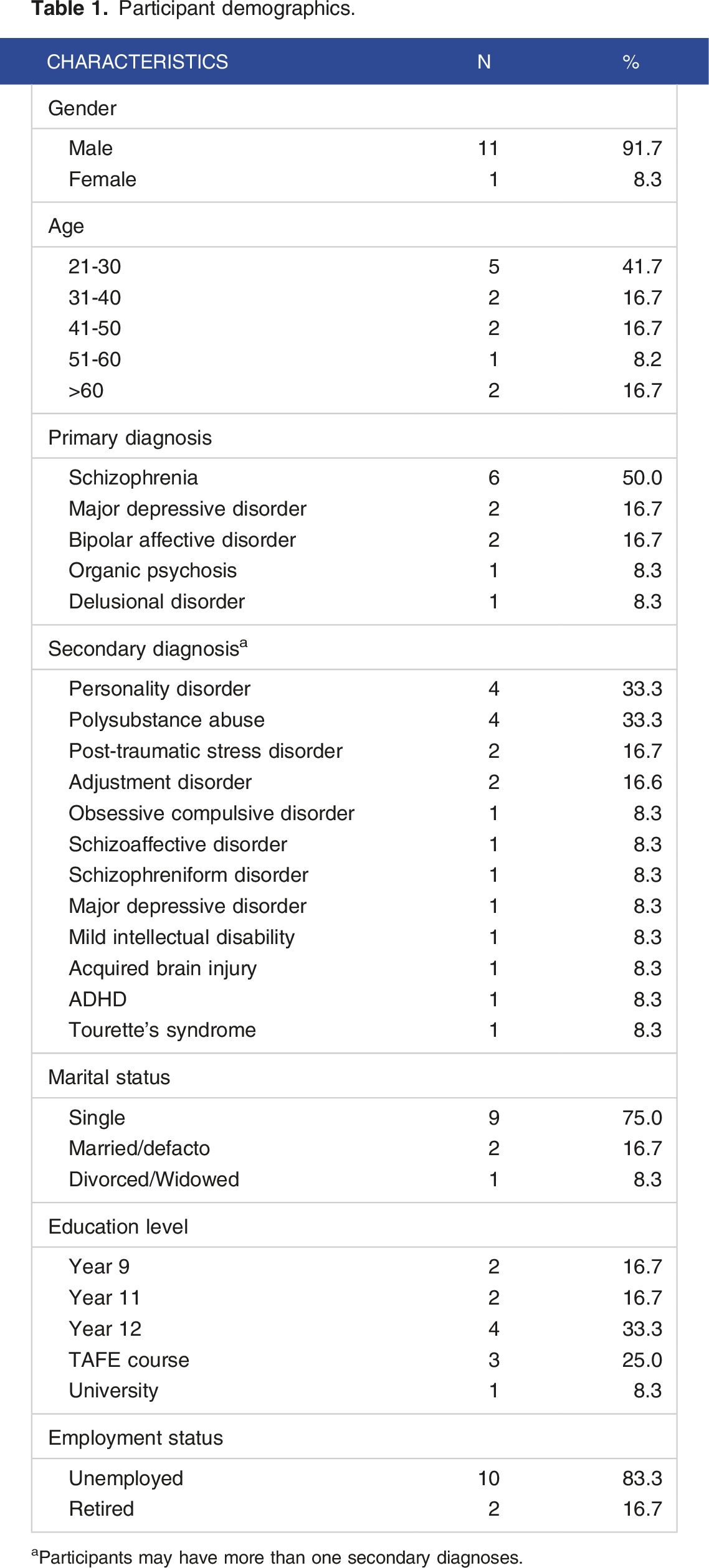
aParticipants may have more than one secondary diagnoses.
CogState schizophrenia battery
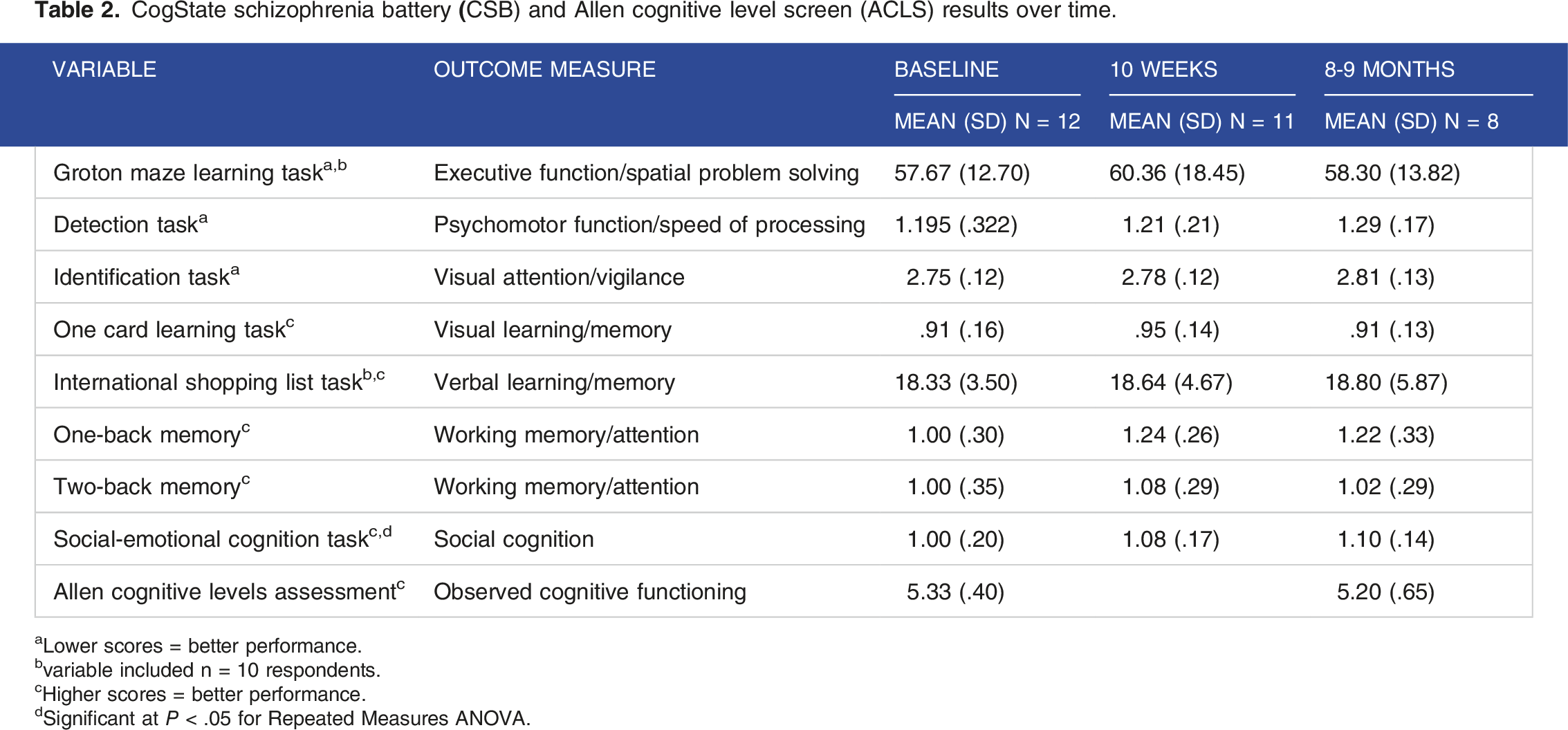
aLower scores = better performance.
bvariable included n = 10 respondents.
cHigher scores = better performance.
dSignificant at P < .05 for Repeated Measures ANOVA.
Brock adaptive function questionnaire (BAFQ).
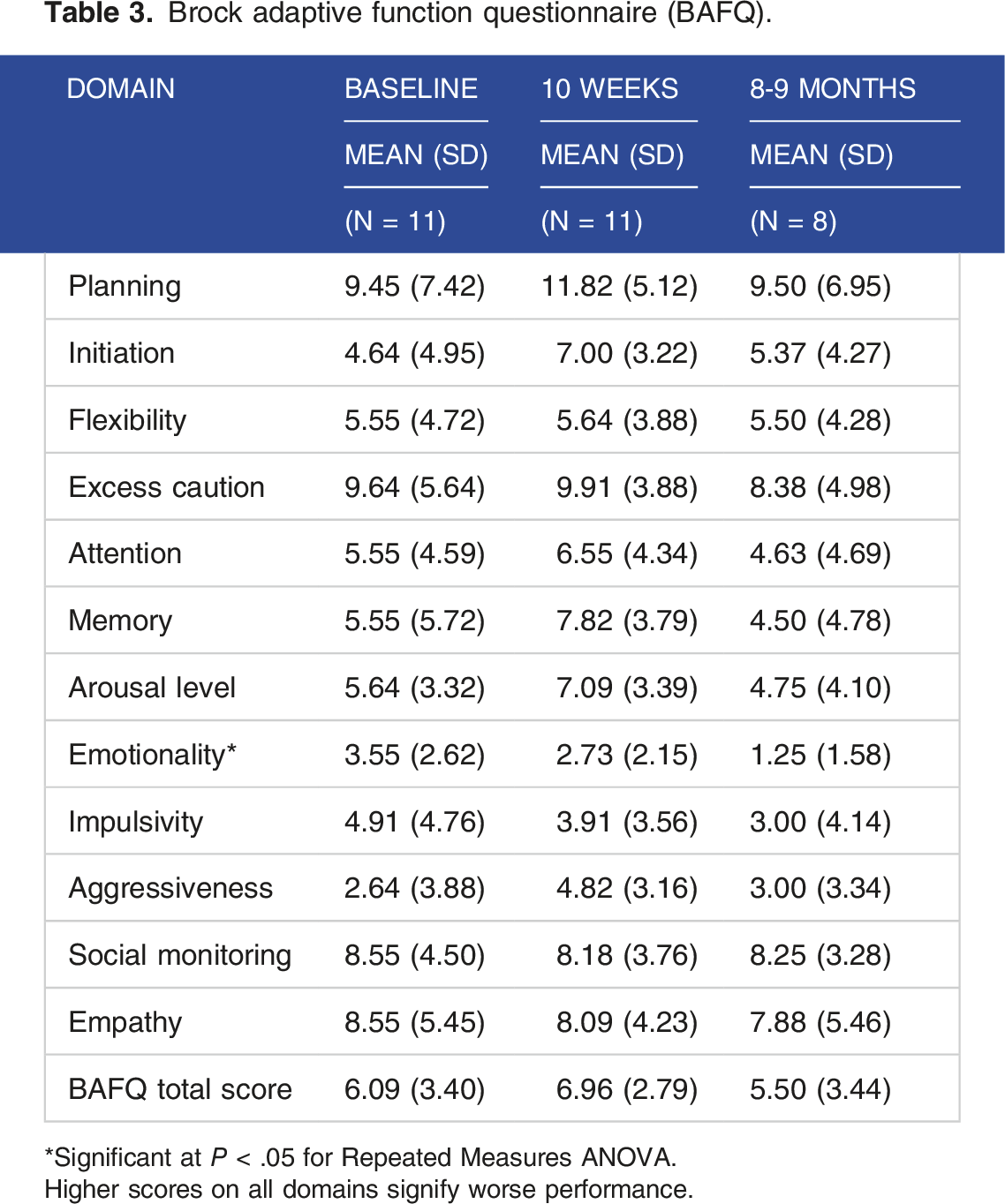
*Significant at P < .05 for Repeated Measures ANOVA.
Higher scores on all domains signify worse performance.
Eleven of the 12 participants provided brief feedback on their perspective of the benefits of the CWMT program during a post-intervention interview. Responses for the 11 participants were: 1) Staying focused for longer periods of time; 2) Being able to listen to and follow conversations. Feeling like they were able to express himself more clearly in conversations; 3) Feeling brighter; 4) Having better recall, better memory; 5) Remembering what they had read, e.g., found they could follow “Lord of the Rings” more easily; 6) Attention level improved; 7) Being able to focus earlier and not missing information. Being able to organise their planning better; 8) Feeling that they can read for longer periods of time. Being able to follow and remember the plot and storylines for multiple novel characters better; 9) Helped them to focus and to organise their thoughts to solve the problem; 10) Comprehending information easier, e.g., when reading the newspaper; 11) Ability to do mental arithmetic had improved.
Discussion
To our knowledge, this is the first study to examine the feasibility and efficacy of the CWMT program in people with schizophrenia in a forensic mental health inpatient setting. We examined the feasibility of an intensive, 10-week program of 30 sessions and weekly coaching. Our findings indicate that a cognitive training program, focussed on improving WM and attention, may be beneficial for patients with schizophrenia spectrum disorders by improving emotionality and social-emotional cognition. Social and emotional cognition have been identified as important targets in schizophrenia treatment, improving interpersonal relationships, and enabling independent living. Aspects of social cognition have shown strong relationships with functional outcomes, social problem solving and community functioning. 50 Improvements in cognitive domains could therefore reduce anxiety and social isolation, enhancing real-world functioning, social skills, support networks, and attainment of independent living. 51
In a forensic population with increased levels of aggression, social impairment and cognitive impairment, enhancements in these skills could provide significant benefit, and aid in reintegration into society. The importance of pairing computerised training programs with cognitive skills in real-world contexts, such as a vocational program, further study, or a rehab program, is to assist in generalising skills to everyday function. In an institutionalised setting, there is little opportunity to practise these new skills on the ward, except for socialising, which could explain the reason social-emotional cognition showed more improvement, and that the improvement was sustained 6 months after the program.
Participants scored an average of ‘level 5’ for the ACLS both at baseline and 6 months post-intervention, indicating an ability to learn by imitation and to apply learned skills, but with limited ability to organise, anticipate and plan.45,46 Participants were predominantly young, under-educated, unemployed, and single. These demographics are not unusual for a schizophrenia inpatient cohort; however, age of onset, employment, education, and cohabitation are all important determinants for future mental health status. Early intervention is crucial to improve long-term functional outcomes including employment, education, and health status. Our findings are similar to a large, Danish cohort study (n = 2 390 127) that found a strong positive correlation between early schizophrenia diagnosis (before 25 years) and being unemployed, having no higher education, and living alone. 52 This study also found that a less chronic course (defined as no further hospitalisation after 25 years of age) improved lifetime salary earnings from less than 14% of that earned by someone without a schizophrenia diagnosis to 39%, and increased the number of people cohabiting from 17% to 36%. These figures highlight the benefits of early treatment interventions.
Although our sample was mostly younger in age, around 40% were aged over 40 years. This may have impacted findings, as age and cognitive reserve were found to be associated with training outcomes in previous studies. Kontis et al 5 53 found that participants under 40 years of age saw greater improvements in WM than did those aged 40 and older. These differences may be due to increased brain plasticity at a younger age. Younger participants would therefore experience faster and more significant improvements than older patients or patients with lower initial cognitive reserve. When examining the results of only those participants under 40 years, changes in performance were more apparent, but still not significant. Time from symptom onset may also be a confounding factor in cognitive training. Past studies found that duration of untreated psychosis (DUP), number of previous episodes, and symptom severity were all negatively correlated with CRT outcomes. 53
Previous studies in CRT found that improvements in WM were related to improvements in social and emotional cognition. 54 While the current study found no significant improvements in WM, our significant findings regarding social-emotional cognition may indicate a number of possible explanations: that social-emotional cognition is independent of other cognitive improvements; that changes in social cognition appear before other improvements are observable on current neuropsychiatric testing instruments; or that improvements in WM and other cognitive domains were dampened by the characteristics of the setting or of participants due to the small sample size of our feasibility study. CRT is often paired with real world activities to assist participants to transfer the skills to their everyday life. This was difficult in a restrictive institutional setting, as participants were unable to appropriately practice or role-play real-world skills. This may have led to specific skills being untrained and unlearned, or may have impaired transfer of skills to other domains.
The study was able to obtain feedback from the participants regarding their own personal experience of the Cogmed training. Each participant reported an improvement in attention, planning, memory, arithmetic, or generally felt ‘brighter’. Both subjective and objective improvements identified in this study indicate that a computer-based cognitive training system may be beneficial for forensic consumers with schizophrenia. This cohort is frequently excluded from research despite the fact that their significant care and treatment requirements suggest a heightened need for treatment exploration and development. Participants’ outcomes, positive response, and feedback to the Cogmed training program demonstrate that it could provide a valuable and cost-effective tool for the treatment of forensic consumers with schizophrenia. Additional measures of psycho-social and real-world functioning should be included in future studies to assess the significance clinical implications of these findings. Given the positive feedback by participants, measures of subjective cognitive function may also be a useful tool. To further investigate the accuracy of any of these possibilities, additional research in a larger cohort must be conducted.
Strengths and limitations
A major limitation of the study was the small sample size. The study was able to engage twelve inpatients diagnosed with schizophrenia for a period of over eight months. People with schizophrenia are particularly challenging to recruit and maintain in a research study, due in great part to the paranoia and social withdrawal inherent in the illness. 55 While the small sample size mean the results should be interpreted with caution, the study was able to identify trend data that demonstrate the benefit of future, large-scale replication studies in an inpatient schizophrenia population. The lack of a control group meant we were unable to definitively determine whether improvements were due to the CWMT program, or a consequence on inpatient treatment. However, self-report outcomes by inpatients indicated that, subjectively, they believed the program had aided in their improvements. Randomised control trials should be conducted to determine the specific benefits of the training the transferability of the training, and the dose required to obtain these benefits.
Another limitation of the study was the focus on cognitive outcomes. Findings of improved social cognition suggest that CWMT may be a beneficial tool for improving real-world social and functional outcomes. For this reason, future studies should include additional measures of psychosocial functioning, real-world behavioural adaption and real-world functional outcomes. Participant feedback indicated improvements in memory and attention that were not picked up in test batteries. Measures of subjective cognitive function and self-efficacy should be included to examine improvements that testing measures were not sensitive enough to pick up, or that were outside the scope of the questionnaires used.
A strength of the study was the longitudinal nature of the project. Forensic consumers with schizophrenia are a particularly challenging cohort to recruit and maintain in research. Researchers were able conduct 10 weeks of regular treatment in all twelve participants, and followed up the majority of these participants for a further 6 months to determine the sustainability of improvements. While it is promising that a 10-week intervention yielded a gain with social-emotional and emotionality domains, it is plausible that a longer intervention period may have led to more improved cognitive outcomes, with further research required for comparison of intervention period lengths. Age, symptom severity, and other factors may have impacted results. Additional participant characteristics are required for future research to adequately control for confounding factors.
People living with schizophrenia are commonly reliant on a combination of pharmaceuticals such as antipsychotics, antidepressants, anxiolytics, and antimanic medications. 56 A number of these medications, such as clozapine and olanzapine, cause significant metabolic dysfunction, thought to impair cognitive function. 57 The impact of other medications used in schizophrenia on cognition is unclear. The medications used in the current study were not reported, but were considered by researchers and clinicians at the time. It was noted that one participant experienced a change in medication which may have impacted results. The impacts of medications will always pose a significant risk to validity and reliability in any study of mental illness.
Conclusions
Our findings indicate that online working memory training has the ability to improve social cognition, and maintain these improvements for at least 6 months in Forensic consumers with schizophrenia. Replication studies of CWMT in schizophrenic populations using controlled trials would provide a valuable addition to the current body of knowledge regarding cognitive training in schizophrenia.
Footnotes
Acknowledgements
We would like to thank and acknowledge the consumers and staff who participated in this study, Tom Meehan and Yolanda Mansfield from the Service Evaluation and Research Unit at The Park – Centre for Mental Health, Amanda Brown and Dianne Glasson from The Park Library, and Mimma Mason, Yvonne Peros and Amy Schulenburg from Pearson Clinical Assessment Australia.
Author contributions
Suzie Keller and Quang Hii contributed to study conceptualisation, design, and data collection. Kerri Gillespie conducted the formal analysis. Kerri Gillespie and Grace Branjerdporn prepared the original manuscript. All authors reviewed, edited, and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
