Abstract
Background
Somatic complaints play a central role in the posttraumatic psychological symptom presentation among people within many cultural contexts. One theory about the function of somatic symptoms suggests that diffuse bodily complaints serve as idioms of distress. However, few studies have examined the effect of culturally adapted trauma interventions on reducing somatic symptoms specifically implemented in a low-income country.
Methods
We examined the effects of Islamic Trauma Healing – a brief, group- and mosque-based, lay-led intervention – on somatic symptom reduction in a pre-post feasibility study conducted in Somaliland. Inclusion criteria were DSM-5 trauma exposure and DSM-5 re-experiencing or avoidance. Participants (N = 26; 12 men, 14 women) reported large intervention effects for somatic symptoms (g = 2.74, SSS-8). Higher pre-intervention somatic symptoms showed moderate to large associations with higher overall PTSD symptoms (r = .43, P = .03). At post-intervention, somatic symptoms were only significantly associated with higher PTSD avoidance symptoms (r = .41, P = .04) and lower well-being (r = -.49, P = .01). No gender effects on total somatic symptom scores were observed.
Discussion
Results of this feasibility trial bring into focus overlap between mental health symptom reporting and somatic concerns as conceptualized within the context of cultural idioms of distress. Moreover, these findings suggest that diffuse transdiagnostic somatic symptoms could offer opportunity to learn about the intersections among culture, posttraumatic stress, and idioms of distress as mechanisms in global mental health intervention development.
Idioms of distress: Feasibility trial findings on reducing posttraumatic somatic symptoms through a community-based, culturally integrated intervention in Somaliland.
Somaliland, a self-declared but internationally unrecognized independent state located northwest of Somalia in the Horn of Africa, has experienced a protracted mental health crisis. 1 The broader region has experienced high levels of sociopolitical instability and civil violence beginning in 1980s, leading Somaliland to declare itself as an independent state in May of 1991. 2 In addition to civil war and armed conflict, the region has also been vulnerable to natural disaster, including drought or floods depending on the geographic area. 3 These factors have contributed to high rates of forced displacement from surrounding regions and neighboring areas of Somalia in recent decades. As of March 2023, the significance of the humanitarian crisis remained clearly reflected in data indicating approximately 3 million people internally displaced within Somalia’s broader borders (which includes the Somaliland region in reporting from the United Nations High Commissioner for Refugees). 4
Availability of data on mental health indicators in Somaliland and local regions remains limited due to human resources limitations and relatively low prioritization within the overall healthcare landscape. 1 Resource constraints interact with cultural factors to limit full integration of mental health care in local health systems. 5 Somali culture generally dichotomizes mental health into categories reflective of either being well or unwell, 6 with mental illness equated with psychotic symptoms and described as “waali” (“crazy”). 7 With mental illness traditionally viewed as severe and irreversible, stigmatization of chronic emotional distress complicates the detection and treatment of common mental symptoms including posttraumatic stress. 8
A dearth of culturally aligned mental health initiatives and shortage of trained mental health service providers in the region have combined to limit the development, dissemination, and uptake of trauma-focused interventions. A 2009 investigation by the World Health Organization identified two psychiatrists, one other medical doctor providing mental health services, one psychologist, and 20 other mental health workers to serve the entire Somaliland population. 9 More recent data suggests only three hospitals have a full-time psychiatrist. 1 Available mental healthcare providers often face low pay and adverse working conditions, leading to low availability of staff. Given expansive challenges to mental healthcare infrastructure, Somalis in need of mental healthcare turn to private and unregulated facilities that emphasize traditional and religious healing for mental illness. Some facilities are run by traditional faith-based healers who seek to provide for their community, other private inpatient facilities (known as an Ilaaj) involve forced detainment under what has been described as adverse and crowded conditions.1,10
The lack of trained mental health professionals has contributed to a paucity of in-country mental health data. Data collected from internationally displaced Somali refugees has been somewhat more available, lending indirect evidence of trauma burden extending from conditions in the region. These data indicate significant risk for pre-displacement traumatic exposure (e.g., in-country experiences) and a high burden of subsequent deleterious mental health effects.11-13 Yet, even when considered in connection to provision of post-displacement mental health services, discrepancies between cultural perspectives and biomedical conceptualizations have limited the ability to fully appreciate the mental health trauma burden of many Somalis or provide appropriate and culturally tailored interventions. Discrepancies in explanatory models of distress can contribute to inaccurate diagnostic appraisals, poorer treatment outcomes, and higher functional impairment in the absence of culturally adapted assessment and intervention approaches for people exposed to traumatic events and forced displacement. 14 In-country research on the trauma sequelae within low- and middle-income settings like Somaliland, on the role of cultural idioms of distress on symptom presentation, and on culturally aligned and theory-driven intervention approaches is needed.
Cultural idioms of distress
Cultural idioms of distress (CIDs) can provide insights into community health needs when implementing interventions in international and cross-cultural contexts.7,15 CIDs refer to common expressions viewed as acceptable ways to symbolize or otherwise communicate emotional distress in a specific culture. These idioms do not refer to specific symptoms or causes of distress, but instead communicate a range of struggles with hardship or discomfort. An understanding of CIDs is invaluable in creating an effective dialogue by providing a shared recognition of the pattern of distress the community and/or individual has experienced.
While conceptual overlap exists, there is a considerable degree of distinction between the phenomena described by Somali CIDs and Western psychiatric constructs. 15 Differences between Somali CIDs and Western psychiatric constructs cannot be reduced to linguistic differences. Indeed, attempts to map a single Western construct to a corresponding Somali CID may be counterproductive to treatment and risk misconstruing the phenomena described in each framework. Nonetheless, previous literature indicates potential benefits of developing a cross-cultural understanding of the relationships between non-Western CIDs and related, Western biomedical psychiatric constructs. 7 In other words, approaching global mental health with a “hybrid” understanding of the symptoms of emotional distress may prove the most useful in building a shared understanding of global mental health outcomes by increasing the accuracy of cross-cultural communication and underscoring the specific range of needs a community may experience.
In recent years, qualitative studies have identified several key idioms to used by Somalis to communicate distress. 7 These terms include: “buufis,” “buqanaan,” “welwel,” “murug,” “qaracan,” “jiini,” and “waali”. Buqsanaan, buufis, and welwel are primarily described as anxiety related. Buufis describes a type of obsession or paranoia, often after resettlement from harsh conditions; “to withhold breath”. Buqsanaan refers to a reaction to extreme stress or abuse and may be best described as an acute panic, including social isolation and externalization symptoms. Welwel refers to a more persistent form of anxiety, generally with somatic complaints, and is known to worsen over time. Murug, often referring to a form of dysphoric mood, is perhaps the strongest term to communicate a sense of deep loss or sorrow and may be predictive of further mental health deterioration. Qaracan may be the term most represented in Western psychiatry and can be compared to the Western understanding of PTSD. However, in some contexts qaracan may be described as the neglect of oneself and their religion. The term jinni or gini (i.e., possessed by an evil spirit or jinn) can refer to a variety of symptoms, from angry outbursts to poor hygiene, and is often used when symptoms are inexplicable and lead to a change in behavior or personality.7,16 Waali may be best described as “crazy” and may be similar to Western concepts of psychosis or dementia. 7
These Somali CIDs demonstrate conceptual interactions between religious beliefs, somatic experiences, and descriptors of psychological wellness. Somaliland has a devout Muslim culture that influences daily life above and approaches to help seeking, often resulting in Somalis seeking a treatment plan that better accommodates Islamic belief systems.16,17 When accessing healthcare, Somalis are likely to have already tried religious and traditional remedies and to report somatic symptoms rather than emotional indicators when experiencing psychological distress.18-20
Somatic concerns in the Somali context
Given the centrality of somatic experiences to several common Somali CIDs, these symptoms may rest at the core of understanding indicators of distress among Somalis participating in mental health interventions. Moreover, somatic complaints are highly common in survivors of trauma overall and have been found to positively associate with PTSD diagnosis.21,22 While unlikely to be representative of in-country samples, such correlations have been consistently found in samples of people forcibly displaced from low- to middle-income countries (LMICs).23,24 Some population-based investigations noted that survivors of trauma had higher odds of experiencing cardiovascular, endocrine, and pulmonary diseases when compared to individuals who didn’t report any trauma history. 25 A diverse literature has highlighted the multifactorial etiology of somatic symptoms in PTSD including biological (e.g., the hypothalamic – pituitary – adrenal [HPA] axis), genetic, and epigenetic components affecting the central nervous system and immune response. 21
Although few studies have examined mental health outcomes within Somaliland or Somalia, some insight on the interactions between CIDs, somatic concerns, and psychological distress may be gleaned from refugee samples including some who were displaced from the region. 26 While trauma-load and symptom presentation differed between groups, somatic and pain-fatigue symptoms of emotional distress were common. The focus and nature of somatic complaints tend to vary between different cultural groups.24,27 Gender may influence perception and attitudes toward mental and somatic distress,28,29 although further research examining potential gender differences in communicating distress across cultures is needed.
Members of social groups who are exposed to protracted sociopolitical conflict and potential psychosocial instability often report high rates of co-occurrence of PTSD and somatic symptoms. For example, somatic symptoms are a vital part of posttraumatic symptomology in refugees and torture survivors. 26 Nonetheless, there is scant literature investigating the effects of trauma-focused interventions on somatic symptoms among Somalis. Culturally aligned models of care and ‘emic’ perspectives are essential to consider when working with both resettled and non-displaced communities.30,31 There is a large potential for misunderstanding and miscommunication when describing psychological distress and related experiences as there may not be common words for common mental health concepts, such as PTSD, shared between academics and the community of interest. 17 Therefore, understanding cultural idioms and fostering a common vocabulary may be a vital step in securing participation and adherence from treatment-seeking Somalis. There is evidence in refugee research that trauma interventions are effective in reducing symptoms when the treatment is co-designed with the input of the target communities and integrates foundational cultural principles.
Intervention: Islamic trauma healing
Islamic Trauma Healing (ITH) 32 is a manualized, faith-based group intervention that integrates cognitive-behavioral principles of change with Islamic faith and culture. Details about the development of the Islamic Trauma Healing intervention 8 and the implementation of the program through this feasibility trial 33 have been published previously. The intervention was developed in collaboration with Imams, community members, and an Islamic scholar to integrate evidence-based principles of trauma recovery while focusing on central Islamic tenets. 8 ITH relies on existing infrastructure, is conducted within mosques, and is implemented by community lay leaders with no prior training in mental health, all of which encourage participation and sustainability. The lay-led and mosque-based nature of the intervention seeks to promote community building, healing within the context of local culture, and stigma reduction.
The ITH intervention consists of weekly two-hour sessions administered across 6 weeks. The intervention is designed for same-gender groups, with two lay leaders for each group. Sessions include psychoeducation, discussing prophet narratives related to trauma healing (cognitive restructuring), and privately turning to Allah in informal prayer, or du'a (imaginal exposure). Each session includes time for community building rituals (e.g., tea) and a brief supplication written by an Imam for spiritual preparation. Intervention components target trauma-related beliefs and aim to reduce trauma-related avoidance. The intervention manual contains clear instructions to assist group leaders in progressing through session-by-session content. Lay leaders guide group members in discussion of narratives of Islamic prophets who have experienced trauma in order to facilitate cognitive shifts congruent with Islamic principles. For example, discussions of the prophets Yusuf [Joseph] and Musa [Moses] include topics such as, “Where was Allah in the midst of Yusuf’s trials?” and “How does this relate to Musa overcoming his fears?” Additionally, graduated exposure to trauma memories is facilitated through du'a, or individual informal prayer, during which group members turn to Allah regarding their traumatic experiences privately. Across the sessions, group members are guided to gradually focus on approaching the most difficult or impactful aspects of the trauma memory during du'a and expressing gratitude to Allah for lessons learned from the traumatic experience.
In addition to the specific cognitive-behavioral mechanisms of the intervention (i.e., cognitive restructuring and imaginal exposure), there are foundational mechanics embedded within the intervention by local Somali culture. These contextual mechanics are foundational due to their role in ensuring the intervention is sustainable and scalable. This includes the removal of Western psychiatric terminology, such as “mental illness” and “therapy” to reduce stigma. As mentioned above, men’s and women’s groups are separated and led by a same-gender leader. To further reduce stigma and increase accessibility, community leaders are trained via a train-the-trainer model led by current group leaders to allow additional lay-leaders to receive the training necessary to implement like programs in their communities. Indeed, this type of deep, cultural integration of evidenced-based PTSD treatments and Islam is crucial for the success and continuation of the intervention. 8 Lacking data on program implementation within Somaliland specifically, previous research has supported the efficacy of community-based mental health programs in LMICs. 34 This includes studies finding significant reduction in symptoms following group interventions led by members of the community despite an otherwise lack of formal mental health training.
Current study
The present study investigated the effects of the Islamic Trauma Healing program on somatic symptom reduction in a pre-post feasibility study conducted in Somaliland. Considering CIDs, we hypothesized that participants would report a significant reduction in somatic symptoms post-intervention even as compared to other symptoms of distress targeted through the intervention (e.g., depression; posttraumatic stress). Item-level examination of individual somatic symptoms and their associations was planned to better understand how distress indicators responded to the intervention. Exploratory analyses also investigated potential gender effects in intervention responses on somatic symptoms, specifically.
Method
Approval from the Institutional Review Board at redacted for peer review was obtained prior to implementation of this feasibility trial. The Somaliland Ministry of National Planning and National Development and the Somaliland Ministry of Endowment and Religion Affairs also provided local permission for the study. Information about the intervention, implementation, and main outcomes of the trial have already been published. 33
Participants
Demographics and sample characteristics of somaliland sample (N = 26).
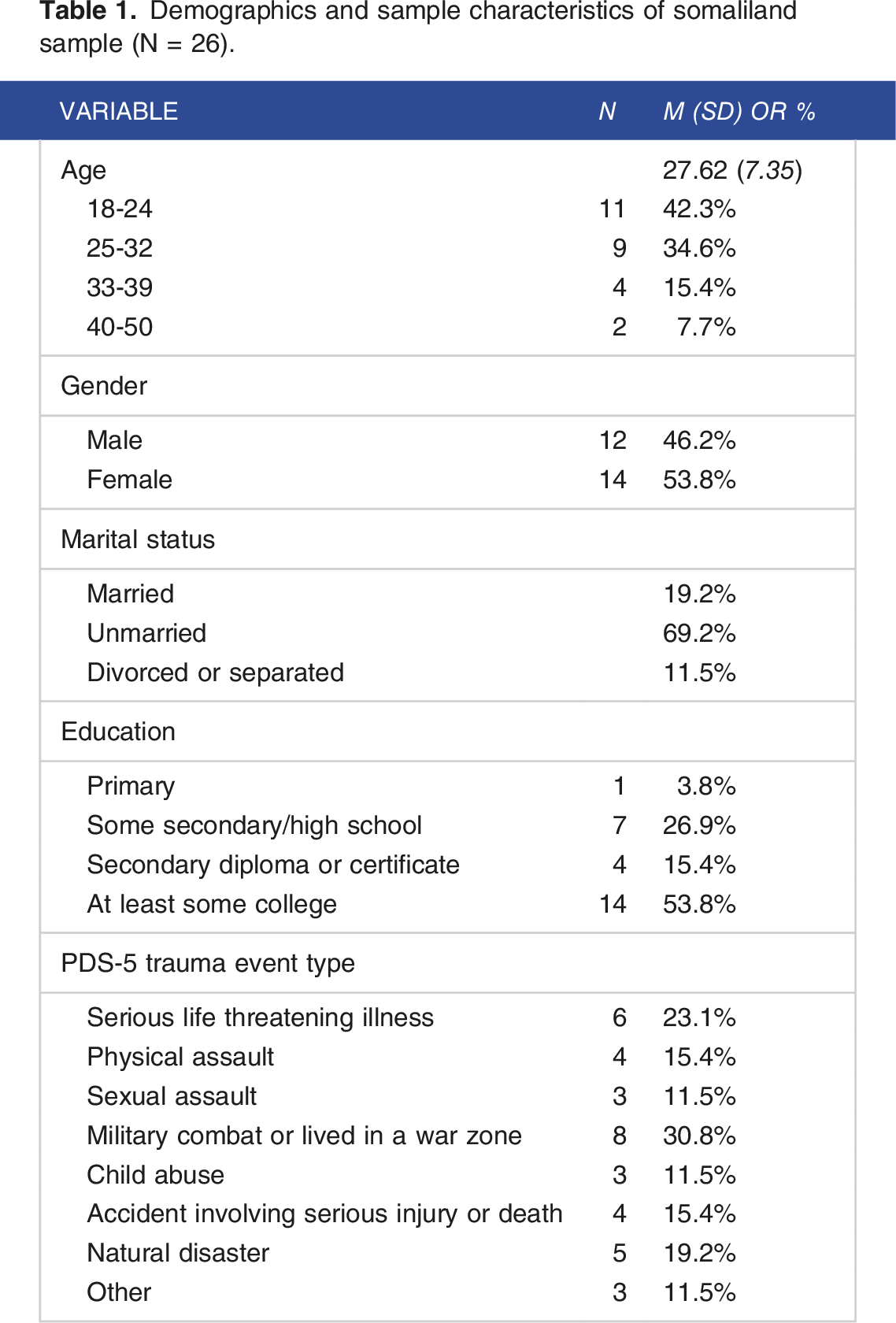
Measures
Participants completed questionnaires using mobile devices (e.g., tablet) and headphones with audio of Somali translations also provided. All questionnaires were forward- and back-translated from English to Somali, with assistance and clarification regarding survey questions provided by a Somaliland study team as needed. Questionnaires were completed at the beginning and end of the 6 group intervention sessions.
Posttraumatic stress disorder
PTSD symptom severity was measured using the PTSD Scale Self-Report for DSM-5 (PDS-5). 35 This self-report measure of PTSD symptom severity in the last month contains two screening questions for Criterion A trauma history that identify lifetime trauma exposure and an index trauma. Twenty DSM-5 PTSD symptom severity items are measured on a 5-point frequency and severity scale ranging from 0 (not at all) to 4 (6 or more times a week/severe). In this sample, PDS-5 symptom scale yielded a Cronbach’s alpha of .93, suggesting strong internal consistency.
Depressive symptoms
The Patient Health Questionnaire-9 (PHQ-9) 36 was used to measure symptoms of depression. The PHQ-9 is a nine-item scale asking participants to rate depression symptoms in the past two weeks on a 4-point severity scale ranging from 0 not at all to 3 nearly every day. Internal consistency of the PHQ-9 in the present sample was strong (.85).
Somatic symptoms
Somatic Symptom Scale-8 (SSS-8) 37 is an abbreviated 8-item version of the PHQ-15 questionnaire. Instructions and response options from the original PHQ-15 were used in the current study. Participants reported somatic symptoms (e.g., stomach pain, fatigue, headaches, dizziness) experienced within the past week (e.g., How much have you been bothered by the following symptoms?) on a 3-point severity scale scored from 0 (not bothered at all) to 2 (bothered a lot). Cronbach’s alpha was .72 in this sample.
Subjective well-being
The WHO-5 Well-being Index (WHO-5)38,39 was used to assess self-reported emotional wellbeing. This five-item measure assesses subjective wellbeing according to a 6-point Likert-type scale ranging from 0 (at no time) to 5 (all of the time), with higher scores reflecting higher well-being. Sample items include “I have felt calm and relaxed” and “I have felt active and vigorous.” The WHO-5 demonstrated strong internal consistency (.94) in the current study.
Procedures
Prior to implementation, a 2-day in-person training on the procedures of the intervention led by a U.S.-based team of clinical psychologists in Djibouti, Djibouti. Training consisted of 8 hours of didactic and practical instruction covering an overview of the program and manual, review and role play practice of group session elements, and proactive problem-solving of potential complications related to implementation. Lay leaders were provided with a session-by-session manual covering all elements of the program. The manual also contained ethical standards related to confidentiality, safety procedures, and informed consent. Supervision of Islamic Trauma Healing group sessions was provided weekly by a team of clinical psychologists and graduate students via a free cross-platform centralized messaging system (e.g., WhatsApp). 40 Key considerations for each group session were identified in advance of WhatsApp supervision meetings (e.g., “In this session, participants turned to Allah in du'a about the trauma for the first time. How did it go?”). This approach allowed for targeted feedback on core elements of the intervention and opened dialogue for feedback and problem solving. Supervision meetings were simultaneously translated for leaders with limited English language proficiency.
Statistical analyses
All analyses were conducted using IBM SPSS Statistics Version 28. For the analysis, we utilized descriptive statistics, Pearson’s correlations, and multiple regression with two-tailed significance levels was set to P = .05. There was no missing data for any variables of interest.
Results
Pre-intervention somatic symptoms and correlations with mental health
Pre-intervention correlations between somatic and mental health symptoms among somaliland participants (N = 26).
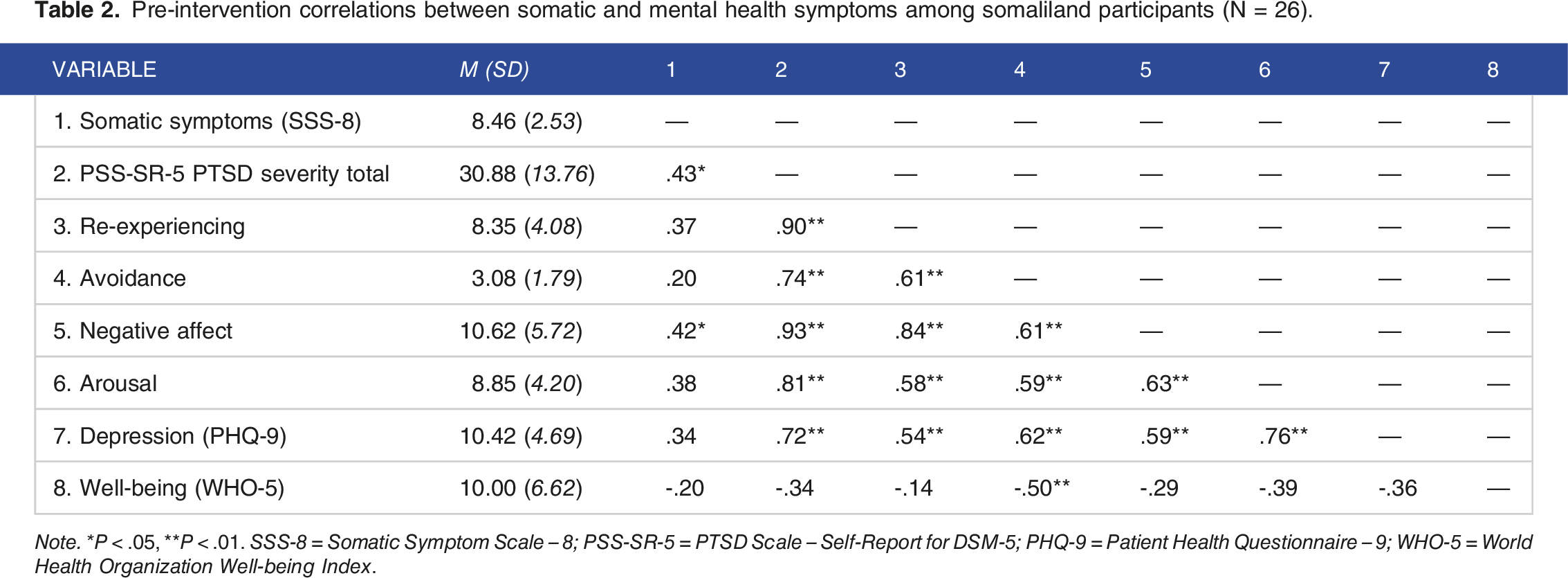

Note. * P < .05, **P < .01. SSS-8 = Somatic Symptom Scale – 8; PSS-SR-5 = PTSD Scale – Self-Report for DSM-5; PHQ-9 = Patient Health Questionnaire – 9; WHO-5 = World Health Organization Well-being Index.
Bivariate correlations analyzed item-level associations between somatic symptoms and other indicators of distress and well-being at baseline. Trouble sleeping had a strong positive association with higher overall PTSD severity (r = .56, P = .003), higher PTSD negative affect and cognitions symptoms (r = .56, P = .003), and higher PTSD arousal symptoms (r = .53, P = .005), as well as moderate positive associations with higher PTSD re-experiencing symptoms (r = .48, P = .01), presence of a PTSD diagnosis (r = .57, P = .03), and higher depression severity (r = .43, P = .03). Pain in the arms, legs, or joints was moderately associated with higher overall PTSD severity (r = .48, P = .01) and higher depression severity (r = .45, P = .02). None of the other individual somatic symptoms were strongly associated with PTSD, depression, or well-being total scores.
Gender differences
An independent samples t-test was performed to compare male and female participants on somatic symptom severity at baseline. Women and men did not differ significantly on overall baseline somatic symptom scores (t[24] = −1.35, P = .236). At the individual symptom level, women reported significantly more trouble sleeping (M = 1.57, SD = .65) as compared to men (M = .75, SD = .45; t[24] = -3.69, P < .001). There were no other statistically significant item-level differences in somatic symptoms based on gender at pre-intervention.
Post-intervention somatic symptom outcomes
Post-intervention correlations between somatic and mental health symptoms among somaliland participants (N = 26).
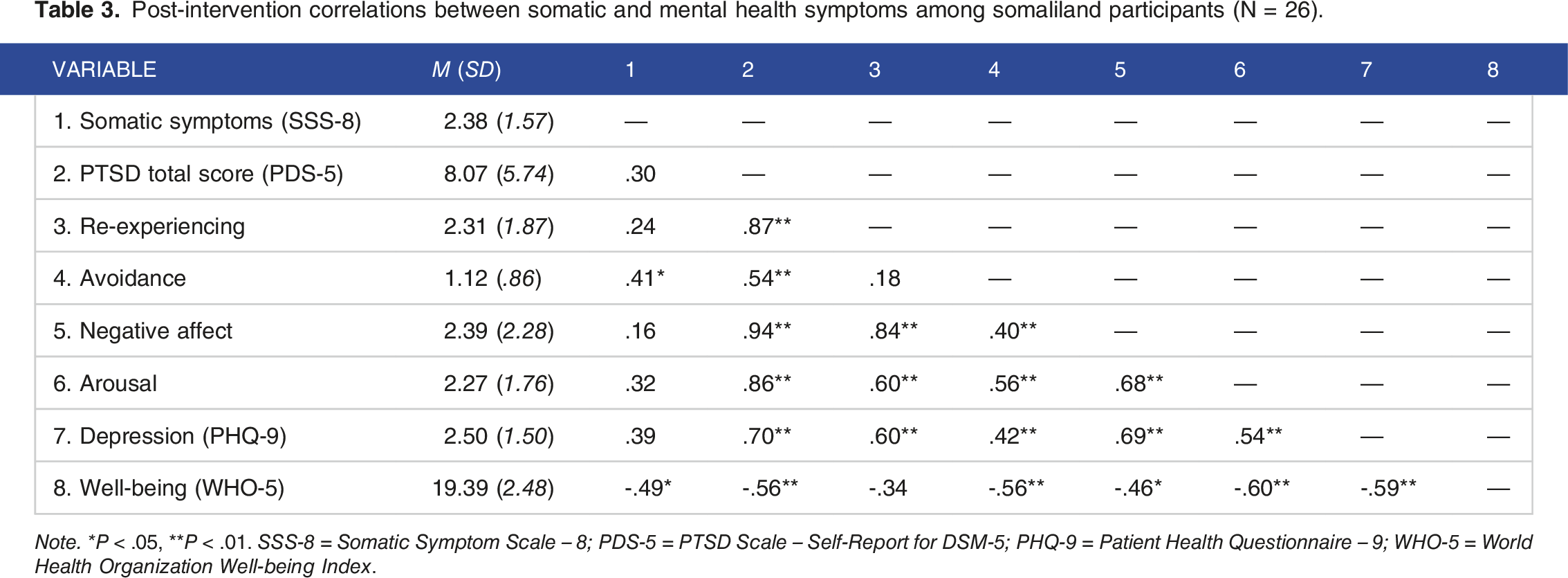

Note. * P < .05, **P < .01. SSS-8 = Somatic Symptom Scale – 8; PDS-5 = PTSD Scale – Self-Report for DSM-5; PHQ-9 = Patient Health Questionnaire – 9; WHO-5 = World Health Organization Well-being Index.
As previously reported in the main outcome paper, 33 there were large intervention effects for changes in PTSD and depression symptoms as well as overall well-being. However, the strongest effect was observed for pre- (M = 8.46, SD = 2.53) to post-intervention (M = 2.38, SD = 1.57) changes in somatic symptoms (t[25] = 12.10, P < .001, g = 2.74). Following the intervention, no somatic symptoms were endorsed at the highest severity level (e.g., “bothered a lot”). Participants most frequently reported being “bothered a little” by the following symptoms post-intervention: headaches (n = 13; M = .50, SD = .51), trouble sleeping (n = 10; M = .38, SD = .50), feeling tired or having low energy (n = 9; M = .35, SD = .49), back pain (n = 9; M = .35, SD = .49), and pain in the arms, legs, or joints (n = 14; M = .31, SD = .47). As shown in Table 3, higher post-intervention somatic symptoms were moderately to strongly associated with higher post-intervention PTSD avoidance symptoms and lower well-being scores.
Another set of bivariate correlations were conducted to analyze for potential item-level shifts in associations post-intervention. Following the intervention, pain in the arms, legs, or joints had a moderate to strong positive association with higher overall PTSD severity (r = .45, P = .02), higher PTSD re-experiencing symptoms (r = .43, P = .03), higher PTSD avoidance symptoms (r = .50, P = .01), the presence of a PTSD diagnosis (r = .41, P = .04), higher depression severity (r = .45, P = .02), and lower well-being (r = -.41, P = .04). Dizziness was moderately and positively associated with higher overall PTSD severity (r = .46, P = .02), more severe PTSD re-experiencing symptoms (r = .46, P = .02), and higher PTSD negative affect and cognition symptoms (r = .44, P = .03). Trouble sleeping was moderately associated with lower well-being (r = -.48, P = .01). No other individual somatic symptoms were significantly associated with PTSD, depression, or well-being at post-intervention.
Gender differences
There was no difference between men and women regarding total somatic symptom scores (SSS-8) at post-intervention. Women reported higher post-intervention higher dizziness (M = .43, SD = .51) as compared to men (M = .00, SD = .00; t[24] = -2.89, P = .008, g = 1.10). These scores reflect low severity on the symptom across genders and represent reductions from baseline levels for female and male participants alike. Pre-intervention gender differences in trouble sleeping were no longer present post-intervention.
Post hoc analysis: Baseline somatic symptoms predicting of change in PTSD symptoms
Finally, to understand the potential predictive ability of somatic symptoms, individual baseline somatic symptoms were examined as a predictor of change in PTSD severity from pre to post intervention, using a standard multiple regression. The overall model was significant, F(8, 25) = 2.77, P = .03, with the R 2 = .57 and 95% confidence limits from .40 to .73. An adjusted R 2 of .36 indicated that approximately a third of the change that was observed in PTSD symptoms was predicted by baseline somatic symptoms, with more trouble sleeping (b = .71, t = 3.89, P = .001, 95% CI: 5.92 - 19.95) and higher back pain symptoms (b = .67, t = 2.63, P = .018; 95% CI: 2.60 - 23.81) uniquely contributing to the prediction of larger PTSD symptom change.
Discussion
Few studies have examined the effectiveness of trauma-focused, evidence-based interventions on somatic symptoms amongst global mental health. To our knowledge, this is the first study investigating the implementation of one such intervention in Somalia or Somaliland. This feasibility study investigated the effects of Islamic Trauma Healing (ITH) on somatic symptoms associated in a sample of trauma-exposed individuals in Somaliland. There were large pre-to-post intervention reductions in somatic symptoms, and somatic symptoms showed the largest changes over the intervention compared to PTSD and depression symptoms and wellbeing. Higher somatic symptoms were moderately to strongly associated with higher PTSD total and negative cognition and mood symptoms at baseline, and moderately to strongly associated with higher PTSD avoidance symptoms and lower well-being at post-intervention. Notably, the somatic symptom of trouble sleeping at pre-intervention was strongly associated with PTSD, depression, and well-being, and post-hoc predicted larger changes in PTSD severity with the intervention. This may argue for the utility of self-reported sleep difficulties as an important behavioral marker or proxy for mental health, potentially reflecting an important idiom of distress in this sample. Taken together, in this feasibility study, large reductions in somatic symptoms were observed following participation in the Islamic Trauma Healing intervention thus highlighting the potential importance of assessing somatic symptoms in capturing distress and clinical change among trauma-exposed populations in LMIC settings.
Consistent with prior studies highlighting the centrality of somatic symptoms as indicators of or related to emotional distress,7,11,26 this study found that higher levels of somatic symptoms were moderately related to higher emotional distress, across PTSD, depression, and well-being. Headaches, dizziness, and trouble sleeping were the somatic symptoms most frequently endorsed at the highest severity, suggesting that these symptoms may be particularly common among Somalis experiencing trauma-related distress. Indeed, difficulty sleeping is included in the DSM-5 PTSD and major depression symptom criteria. More generally, arm, leg, and joint pain was also moderately associated with higher PTSD and depression severity, suggesting that capturing a wider range of somatic symptoms than is currently reflected in Western diagnostic criteria for PTSD and depression may provide a more complete picture of trauma-related distress among Somalis.7,11 Specifically, trouble sleeping emerged as a consistent and strong marker of distress, being associated with PTSD, depression, well-being, as well as predicting improvements in PTSD severity and gender differences in trouble sleeping disappearing with intervention.
Indeed, problems sleeping is emerging an important transdiagnostic marker across many mental disorders41-43 and improving sleep health is emerging as a means to foster mental health resilience. Given its concrete behavioral presentation and relative ease of cross-cultural conceptual translation, it may be a prime candidate for capturing mental health distress across samples and contexts. Notably, the ITH intervention produced the strongest reductions in somatic symptoms compared to PTSD, depression, and well-being, highlighting both the effectiveness of ITH for both emotional and somatic facets of distress as well as the importance of somatic symptoms to understanding clinical change processes and therapeutic outcome among Somalis. Considering that ITH is a trauma healing program at its core, such reduction in somatic complaints suggests functional overlap between trauma-related emotional distress and somatic complaints in this small sample feasibility study. These findings argue that clinical trials for psychological distress in Somali samples should include somatic complaints as primary or secondary outcome measures.
There was evidence that some associations between somatic symptoms and emotional distress changed from pre- to post- intervention. Specifically, although higher somatic complaints at baseline were significantly associated with greater overall PTSD severity and more negative alterations in cognition and mood, these associations were reduced to a statistically non-significant level following the intervention. Components of the manualized and culturally embedded intervention, particularly cognitive restructuring through prophet narratives and approaching trauma memories through du'a, as potentially helping to disentangle associations between upsetting thoughts and emotions with somaticized distress responses. A recent systematic review of diverse trauma intervention approaches found evidence for targeting improvement in maladaptive posttraumatic cognitions as a general mechanism of change across adult and pediatric study samples. 44 This appears to be in accord with mechanistic studies of trauma-focused psychotherapy demonstrating changes in posttraumatic cognitions as preceding other intervention effects.45-47 Additional research into changes in cognitive mechanisms potentially underlying somatic-posttraumatic stress symptom associations over the course of the culturally integrated interventions like ITH will be needed in order to better understand the clinical significance of these findings.
Interestingly, at post-intervention, higher somatic symptoms became significantly associated with higher levels of avoidance and lower subjective well-being. This pattern of shifting associations is consistent with the relationship between trauma exposure and somatic symptoms being partially mediated by active avoidance symptoms. 26 Consistent with cognitive and emotional processing theories,48,49 trauma exposure influences or biases a person’s appraisals of potentially threatening stimuli. Within specific cultural paradigms, congruent with medical anthropology perspectives,50,51 trauma exposure may also shift appraisals of physical and physiological experiences. Appraisals may in turn contribute to increased avoidance, catastrophic thinking about symptoms, and an exacerbation of the symptom experience. 52
Large intervention effects across PTSD symptom clusters were observed in this sample, including symptoms of trauma avoidance. The finding that the post-intervention association between somatic and posttraumatic avoidance remained statistically significant while other PTSD symptom clusters did not may gesture toward culturally nuanced idioms of distress not directly measured in the present study. Given multiple overlapping idioms present within a culture and variation in the degree to which those idioms are adopted by individuals in a cultural group,1,7,8 a specified a priori ‘emic’ approach will likely be needed in order to parse out these relationships for members of a particular cultural group.30,31,53 Previous research conducted in other LMIC settings has suggested that individuals with less identification with biomedical constructs of mental illness and/or high concerns about stigma to be more likely to report a higher balance of somatic symptoms. 54 These factors may be particularly relevant to settings like Somaliland, where stigma associated with mental illness is high and there is no terminology in the native language to describe DSM-5-based concepts of traumatic events or psychiatric reactions. Future mixed methods studies may also be most helpful in better understanding whether the associations we observed between somatic symptoms, PTSD clusters, and well-being reflect idioms of distress in specific cultures and in what ways these relationships are altered by virtue of targeted mental health interventions.
Limitations
There are several noteworthy limitations to consider when interpreting this work. Interpretation of these results must take into account limits to generalizability due to the small sample size. Although this study revealed large pre-post intervention effects on emotional distress and somatic symptoms, it utilized a small sample that may not be representative of the broader Somali population. This study also lacked a control condition and long-term follow up, which tempers any conclusions related to causal factors. Replication will be needed in a larger sample and a more specified randomized control trial design than the present study. In addition, while this study stands out for its explicit assessment of both emotional distress and somatic complaints, the somatic measure used was developed from a Western measure. 37 Measures that specifically assess Somali idioms of distress, 7 are sorely needed to best capture distress and clinical change in this population.
Conclusions
This feasibility study provides new insights into the in-country implementation of deep cultural adaptation of a traumatic stress intervention. These analyses highlight the potential of trauma-focused global mental health interventions to reduce somatic symptoms, potentially as partial indicators of emotional distress. Islamic Trauma Healing, a community-based and religiously aligned intervention, produced large reductions in emotional distress and even larger reductions in somatic symptoms in this Somaliland-based sample. This study highlights the centrality of somatic symptoms in understanding clinical change among trauma-exposed Somalis and reinforces the importance of moving beyond conventional, Westernized indicators of distress when caring for and attempting to conceptualize the experience of global populations exposed to trauma and related psychopathology.
Footnotes
Acknowledgments
This work would not have been possible without approvals provided by the Somaliland Ministry of National Planning and National Development and the Somaliland Ministry of Endowment and Religion Affairs. We also offer our appreciation to the Ma’alin Haruon Masjid in Hargeisa, Somaliland, and Abu-Bakar Al-Siddique Islamic Center in Borama, Somaliland for providing support and space for the Islamic Trauma Healing intervention. The efforts of group leaders in Hargeisa (Mohamed Ahmed Abdi, Zeinab Adam Abdillahi, Ayan Abdillahi Ali, and Khadar Hindi Boton) and Borama (Aden Mohamed Ali, Hibaq Isse Ibrahim, Salma Hassan Ibrahim, and Abdirahman Muse Tubeec) were critical to the successful implementation of this feasibility study in Somaliland.
Author contributions
The authors express gratitude to the Somaliland Ministry of National Planning and National Development and the Somaliland Ministry of Endowment and Religion Affairs for providing approval to carry out this work in Somaliland. Much gratitude to Ma’alin Haruon Masjid, Hargeisa, Somaliland, and Abu-Bakar Al-Siddique Islamic Center, Borama, Somaliland for supporting the Islamic Trauma Healing program and allocating physical space to conduct group sessions. Thank you to Mohamed Ahmed Abdi, Zeinab Adam Abdillahi, Ayan Abdillahi Ali, and Khadar Hindi Boton at Ma’alin Haruon Masjid, Hargeisa, Somaliland. Equally, many thanks to group leaders at Abu-Bakar Al-Siddique Islamic Center, Borama, Somaliland: Aden Mohamed Ali, Hibaq Isse Ibrahim, Salma Hassan Ibrahim, and Abdirahman Muse Tubeec. Michele Bedard-Gilligan, Shannon Dorsey, Debra Kaysen, and Hamza Zafer, served as consultants on this study and Co-Investigators on the UW Population Health Initiative pilot grant project.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study received funding from the University of Washington Population Health Initiative.
