Abstract
Background
DiGeorge syndrome (DGS) is a rare genetic illness characterised by the abnormal development of the pharyngeal pouch system. It is known to have a high association with intellectual disability and psychiatric disorders.
Purpose
This case report details a unique 22-year journey of a 49-year-old female with an established diagnosis Intellectual disability, Schizophrenia and Borderline Personality Disorder associated with DGS. This report demonstrates the challenges faced for a patient with 22q11.2DS in the 3 intersecting domains of physical, psychiatric and psychological illness.
Results
The report draws attention to the limitations in follow up care, risk management and discharge settings in the face of the treatment refractory nature of her underlying health conditions.
Conclusions
The case highlights the lack of specific treatment guidelines and psychosocial supports for the neuropsychiatric phenotypes associated with 22q11.2DS. More research is needed to inform guidelines and considerations of care for the`-se patients.
Keywords
Background
22q11.2 deletion syndrome (22q11.2DS) is a constellation of signs and symptoms associated with a microdeletion in the long arm of chromosome 22. 1
Due to the variability of phenotypic presentation of the mutation, the genetic illness has also been known by various names such as DiGeorge or Velocardiofacial syndrome and is often still referred to as such. Di George Syndrome was initially historically first identified in infants with heart defects, hypocalcemia and immunological deficiencies, while Velocardiofacial was identified in children with hypernasal speech and distinct facial features. Further genetic research revealed that both these syndromes were related to the same genetic etiology. 2
Classically the features of 22q11.2DS include the triad of outflow tract cardiac anomalies, hypoplastic thymus and parathyroid hypoplasia. 3 Approximately 90% of patients with 22q11.2DS have de novo heterozygous deletions in chromosome 22q11.2.4,5 The inheritance of 22q11.2 is autosomal dominant 6 and population studies have reported the incidence of 22q11.2 to be around 1 in 4000 livebirths and 1 in 1000 fetuses.7,8
Partial 22Q11.2DS refers to syndrome with some degree of preserved thymic tissue while complete 22q11.2DS refers to syndrome without thymic tissue, which fatal without transplantation due to severe immune deficiencies. 9
The prognosis for partial 22q11.2DS patients and complete 22q11.2DS patients who survive thymic transplantation is largely dependent upon the severity of the cardiac defect, degree of hypoparathyroidism, and intellectual development. 10 The overall mortality was found to be 8% in a large survey of 558 22q11.2DS patients. 10 In most cases, death occurred in the first six months of life and was secondary to cardiac-related complications. 10 Most babies with 22q11.2DS have successful corrections of their heart disease and will live normal life spans. 11 Immune problems subside with time, and endocrine problems tend to be intermittent and treatable with appropriate medications. Speech problems respond well to speech therapy and surgery. 11
The cognitive phenotype is highly variable between individuals with 22q11.2DS. 12 While most patients with 22q11.2DS have IQ in the borderline range, this is IQ 70-84,13,14 approximately one third of patients have mild intellectual disability.12,14 Severe impairments are uncommon.12,14 Particularly, arithmetic skills are more severely impaired than reading skills 15 ). There are also relative impairments to domains of executive function, motor function, verbal learning, and social judgement 14
While being a rare congenital disorder and having specific studies lacking, 22q11.2DS has been found to be associated with various psychiatric disorders including psychosis. 16 The most extensive study found during review of the literature was the ‘International Consortium on Brain and Behaviour in 22q11.2 Deletion Syndrome’, a multinational large cross sectional study of 1402 participants. 16
For children specifically, ADHD was the most frequent disorder at 37%, however anxiety disorders were also very common at 35%. The study found that the prevalence of both decreased with respect to age. Anxiety disorders were mostly specific phobias, starting at 22% but decreasing eventually to around 2.3% once reaching mature adulthood. Generalised anxiety remained roughly the same around 10%. 16 Psychotic type disorders (including schizophrenia, schizophreniform, schizoaffective, and brief psychotic disorder) were most prevalent at 41% as patients reach young adulthood. 16 Mood disorders increased significantly with age starting at 2% in childhood up to 15.75% in mature adulthood. The study found low prevalence of bipolar disorder/hypomanic disorder reaching only 3.94% in mature adulthood and no incidence found in childhood. 16
Substance use does not appear to play a role in the increased predisposition towards mental health disorders in this subgroup of patients. In fact, patients with 22q11.2DS are 20 times less likely to use substances in general. 17 Further, weekly nicotine and alcohol use is significantly lower than in patients without 22q11.2DS. 17 The mechanisms behind this are yet to be researched, however.
Early studies suggest that there are no significant differences in the age of onset and nature of positive vs negative symptoms of schizophrenia in this subgroup of patients.18,19 Few studies have evaluated the effectiveness and safety profile of psychotropic medication in people with 22q11.2DS. 20 It has been suggested by authors in this field that newer agents such as risperidone, olanzapine and quetiapine are better tolerated by children with 22q11.2DS, however consideration should be given to the unique metabolic and congenital cardiac vulnerabilities that patients with DiGeorge are prone to.20,21
Specific psychiatric guidelines are lacking, however general recommendations are to manage similarly to standard practice guidelines for schizophrenia. 22 However, some authors have also advocated that antipsychotic use patients with 22q11.2DS should ‘start low and go slow’, to reduce extrapyramidal and metabolic side effects.20,23
Case Report
Ms. P is a 49 years old, single, unemployed female with an established history of suffering from Schizophrenia, Borderline Personality disorder, Intellectual impairment and underlying 22q11.2DS. She is currently admitted to a long stay, community based dual disability rehabilitation unit. She has spent most of her adult life in psychiatric inpatient care and in similar long-term community-based rehabilitation facilities since her first episode psychosis in 1997. Written consent was obtained for the purposes of this case report.
Since her first episode, Ms. P has struggled with treatment refractory symptoms of schizophrenia characterised by a range of persecutory delusional beliefs, auditory hallucinations and disorganised speech and behaviour. This is on the background of long-term difficulties with mood instability, low self-esteem, impulsivity and low frustration tolerance. She has periodically presented with episodes of self-harming behaviour, suicidal and homicidal thoughts, verbal and physical aggression. She also suffers from multiple chronic physical health illnesses further complicating her care.
Developmental history
Ms. P was born as the youngest in a siblingship of 3, with an older sister and brother. There was no identified history of mental or genetic illness in any close family members. The pregnancy was uneventful, and Ms. P reached term delivery. At birth Ms. P was found to have a cardiac murmur, facial and pharyngeal abnormalities including ‘bat ear appearance’ and pharyngeal incompetence. On genetic testing it was established that she had a microdeletion in the 22q11.2 region and was subsequently diagnosed with 22q11.2DS. Ms. P had a total of 14 childhood surgeries to help correct for the various anatomical abnormalities and complications associated with 22q11.2DS. She was diagnosed with a mild intellectual disability at school. She suffered from sensorineural deafness which further added to her challenges. She was reported to be a shy, insecure, and overly self-conscious child with limited friends and eventually left during year 11.
Ms. P had multiple attempts at simple part times jobs between the ages 17 to 24, however struggled with following instructions, impulsivity, and poor performance. She also began smoking, having around 30 cigarettes a day, but remained a social drinker. Ms. P only had one relationship, at the age of 23, which lasted a year. It was during this time she was introduced to cannabis by her partner, of which she smoked daily during the length of their relationship. It was in this context that she suffered from her first psychotic episode.
First contact with mental health services
Ms. P first presented to mental health services at the age of 24 following an 8-month gradual deterioration. She was reported becoming more agitated, irritable and had started to develop persecutory delusional beliefs. Her admission was precipitated by an argument with her parents where she slit her wrists and threatened to kill her mother.
During admission, the treating team noted difficulty with emotional regulation, maladaptive coping mechanisms and manipulative attitudes towards her parents. She was diagnosed with a psychotic illness and commenced on a Thioridazine 300 mg. As carer’s burnout was evident, a referral to Continuing Care Unit (CCU), a community residential rehabilitation service was made. The goals were to optimise and monitor her medication, provide support with forming greater independence and providing respite for her carers.
Initial approach to rehabilitation
At CCU, rehabilitation was interrupted by challenges in her mental state and escalating non-psychiatric medical concerns. She faced a myriad of physical health concerns, such as a needing chemotherapy for CNS lymphoma, developing chronic lymphedema with leg ulceration, chronic pain from fibromyalgia, pseudo seizures and recurrent ear infections. This frequently necessitated transfer to the general hospital, especially for the management of cellulitis from her chronic leg ulcer.
Acute exacerbations of her behavioural symptoms were often precipitated by stressors, such as parents leaving the country, change in setting of care, needing chemotherapy, or perceptions that her needs were not being met.
Examples of behaviours of concerns included: 1. demands to be admitted to an inpatient unit 2. physical and homicidal threats to staff 3. somatic complaints 4. assaulting a police officer 5. drug overdoses 6. self-cutting 7. an attempted hanging 8. flushing medications
After further review, a diagnosis of borderline personality disorder was confirmed. While continued attempts were made to discharge Ms. P to supported residential services (SRS), her fluctuating mental state and the rapidity at which her behaviours would escalate meant these attempts were unsuccessful. Her time in the CCU eventually ended after 8 years when her behaviour escalated to a serious physical assault against a staff member. As a result, she was referred to a restrictive care setting, called the Secure Extended Care Unit (SECU) to help manage her escalated behaviours.
Despite this, her behaviour profile remained mostly the same, and she continued to have poor engagement with the rehabilitation activities. Various psychotropic medications were trialled over the years, including higher than recommended doses such as aripiprazole 45 mg and olanzapine 40 mg. First generation antipsychotics of chlorpromazine up to 600 mg and Zuclopenthixol 20 mg were also tried to limited benefit. She was also initiated on clozapine, but this needed to be ceased due to developing neutropenia. Mood stabiliser augmentation was also pursued with sodium valproate doses up 2 g, however with minimal improvements.
Continued attempts to discharge to supported residential accommodation failed, due to fluctuating behaviours remained unsuccessful due to challenging behaviours. After another 12 year of living in SECU with minimal improvements, she was referred to TSU (Transitional Support Unit), her setting of care at the time of writing this report.
The re-evaluated TSU approach
TSU is a state level specialist community based dual disability rehabilitation unit. The service aims at catering towards patients with intellectual disabilities and comorbid mental health disorders in a lesser restrictive community environment. At TSU her treatment approach was reviewed with consideration given to a refreshed formulation of her dual disability. Treatment was rationalised to reduce her medication burden and the potential of antimuscarinic side effects, which may have been contributing to delirium and constipation. Aripiprazole dose was reduced to 30 mg, and olanzapine was weaned and ceased. Furthermore, treatment interventions were made with the view to optimise management of her physical comorbidities in effort to reduce distress and improve function.
An MDT led, Behavioural Support Plan (BSP) was successfully implemented, helping staff utilise strategies in addressing Ms. P’s learned behaviours with respect to her intellectual disability. Such interventions had early success with respect to improved engagement and decrease in challenging behaviours. Some difficulties, however, remained with regards to management of her physical health comorbidities. Compliance with recommended interventions, such as dressing changes remained poor and at times Ms. P appeared to self-report paranoia and accusations against certain wound care nurses. It is unclear if these self-reports were based in her own experience of paranoia or whether these were contrived.
Liaison and reviews with the TSU clinical psychologist and her behavioural support practitioner to address these challenges were ongoing. They hypothesised by making accusations towards certain wound dressing nurses, it was possible Ms. P was gaining comfort in being able to have some degree of control in the institutional setting as well as delaying the painful dressing changes. As such, her behaviours had become entrenched following the 20 years of institutionalisation. It was further likely that her intellectual disability impeded recognising the long-term consequences of such actions. It was envisaged that her ‘paranoia’ towards certain co-patients was a further attempt at control in trying to reduce the amount of exposure she had to those residents whom she did not enjoy the company of. The BSP thus was updated to reflect the dynamic nature of Ms. P’s behaviours of concern and the nature of her institutionalised behaviours.
Focussed approach and the behavioural support plan was effective in managing Ms. P’s risk profile. Staff management was overseen by a clinical psychologist and behavioural support practitioner through staff training and a behavioural support plan. The foundations of the plan were rooted in the early identification of warning signs and preventing unnecessary escalation. This was achieved by breaking suggested management into clear goal directed steps and responses to concerning behaviours. These interventions showed marked improvement in her mental state, and Ms. P was observed to be more interactive, pleasant, and even playing musical instruments. She began to take interest in her rehabilitation and the focus of her care progressed from managing her symptoms towards discharge planning.
Discussion
It is quite likely Ms. P’s genetic illness played a causative role in the development of her schizophrenia, given the high degree of association with 22q11.2DS. 18 Her use of THC for one year prior to her presentation may have indeed served as a precipitating factor. 24 The psychosis found in 22q11.2DS generally appears to be similar in terms of character and symptomatology compared with those without the mutation, 19 as appears to be reflective in the case of Ms. P.
Over the years various strategies and medication trials were used attempting to treat Ms. P’s symptoms. This included various combinations of first and second-generation antipsychotics, including clozapine. These were often used in combination or at higher than recommended doses, yet Ms. P’s symptoms remained treatment refractory.
In TSU, an approach of weaning and rationalisation was well-tolerated with improvement in her baseline mental state. This is consistent with previous studies indicating that there is no clinically significant improvement in efficacy with combination or high dose atypical antipsychotic treatments when compared to monotherapy. 25 It is worth noting that these studies in general did not account for heterogeneity of subjects, such as the presence of conditions such as 22q11.2 deletion syndrome.
Neuropsychiatric and behavioural approach based on biopsychosocial management principles
Clinical guidelines remain limited for genomic disorders in general, despite increased recognition with genomic testing. 26 An approach was taken in keeping with general principles of neuropsychiatry 26 for involving a broad systems-based approach, and by coordinating individualised multidisciplinary care. Such approaches, have been used in other neurocognitive syndromes such as Lesch-Nyhan syndrome. 26
The multisystem based approach could be broadly categorised using the biological and neurobehavioral framework as described below.
Biological approach
Summary of biological challenges and interventions.
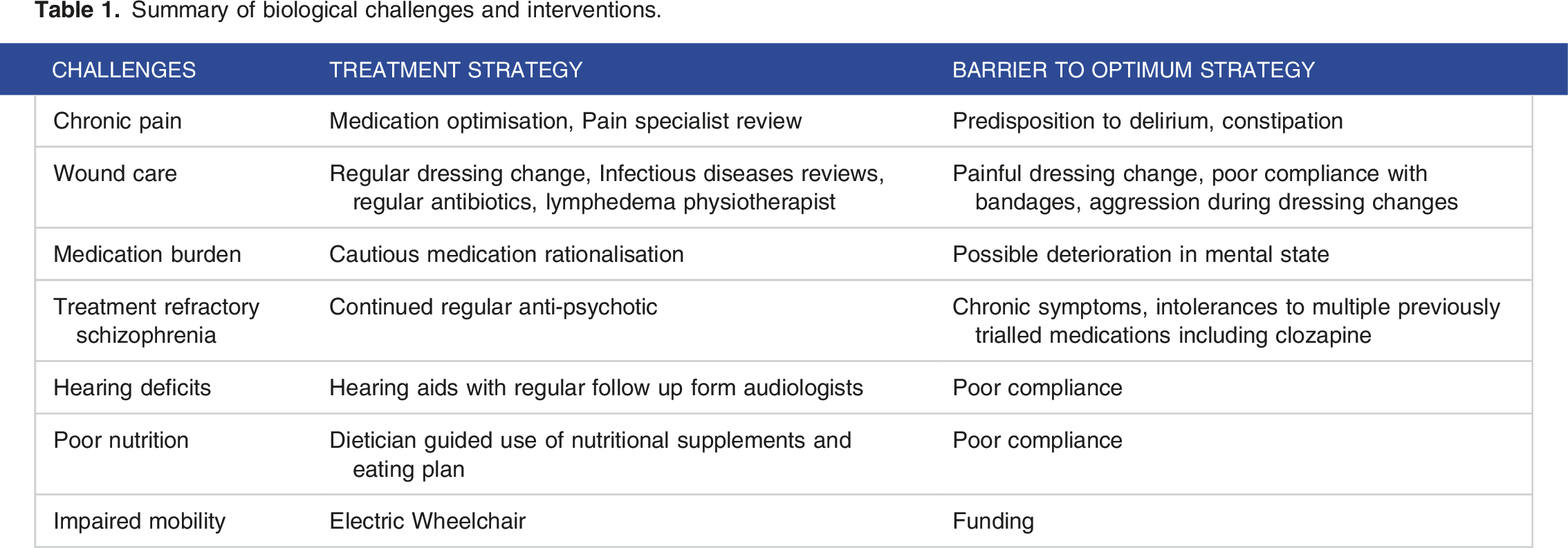
As highlighted, Ms. P’s symptoms remain treatment refractory despite multiple years of trials of various pharmacological therapy. Research into genetic studies may hold further avenues of treatment for those with genetic syndromes, such as in 22q11.2, which are known to carry specific mutational patterns. While currently the role of genomic testing is mostly restricted to diagnosis, recent interest in the broader psychiatric sphere has been generated in the prospect of genetically informed tailoring of pharmacological management. 27 Such advances could have future promising implications in the efficacy of pharmacological relief of symptoms for patients such as Ms. P. 27
Neurobehavioural approach
Research has shown that patients with 22q11.2DS associated schizophrenia score higher on excitability and impulsivity metrics compared to those without. 19 Impairments to social cognitions have also been highlighted by research, specifically in the domains of emotional processing. 28 It remains unclear from the research body why these impairments occur. This may go towards explaining in a biological basis towards the self-destructive behaviours and agitation towards staff which has complicated Ms. P’s management for so long. It is possible that this may have left her predisposed towards developing the emotional dysregulation that is common in personality disorder.
The Behavioural Support Plan (BSP) has been critical in the management of the maladaptive behaviours. It has been hypothesized that the long-institutionalised care has led to the formation of poor coping mechanisms as a method to regain a sense of control over Ms. P’s environment. This may have been formed due to professionals, parents and authority figures taking a more assertive approach to her health given her vulnerabilities, thus leaving her feeling powerless. It was evident that the 12 years of highly restrictive practice was not effective at reducing Ms. P’s symptoms. Additionally, positive behavioural support has shown effectiveness in both severe and high-rate behavioural problems. 29
This served as a rationale behind a more inclusive approach with Ms. P making her own weekly routines and reinforcing a sense of control. This intended to foster a more constructive attitude towards engaging in rehabilitation. As described, the revaluated approach in this case study showed substantial improvements in this regard with the case study of Ms P.
Notably, research into personality disorders with individuals afflicted with 22q11.2DS is conspicuously absent. It is worth noting that there is an inherent predisposition for patients with childhood difficulties towards personality disorders, particularly borderline personality disorder. 30 As such, the case article calls attention to the gap in this area of research.
Future approaches and discharge planning
At time of writing this report, discharge planning was still an ongoing process. Over the years, suitable discharge planning has been a multifactorial challenge with many past unsuccessful attempts at facilitating community level care. Change to routine has historically been a significant barrier, both for Ms. P but also for her carers. It is possible that those unfamiliar with the baseline learned institutional behaviours of Ms. P, may be quick to escalate her care due to appearing to have high risk. This may have led to her ending up in more restrictive environments or unsuccessful discharges. The tendency to use her mental illness as a justification for her behaviours and to refuse unpleasant but necessary aspects of her physical care further reinforce this difficulty.
The case of Ms. P highlights a need for such specialist community supports which are not readily available. This has raised great challenges in finding a suitable home away from the clinical environment. An awareness and understanding of the nature of Ms. P’s condition, associated behaviours, and structured bespoke support plans is likely to be critical.
To address this, the treating team included comprehensive handover and training future carers’ carer training in Ms. P’s behavioural support plan. This involved a staggered transitional discharge process in which the treating team. This goal was to allow carers to gain familiarity with Ms. P, and hopefully reduce the likelihood for excessively restrictive behavioural containment measures and allow for effective de-escalation measures. Additionally, the treating included the plan to provide ongoing liaison with family and carers, by offering participation in carer support group in addressing their anxieties.
As current medical power of attorney and having made many administrative decisions throughout Ms. P’s life, her parents have been supportive and involved throughout her care. However, this may not be a long-term option as they enter their later years. If Ms. P is to move towards community care, it is likely she would be subject to more administrative life decisions, when compared to living in a healthcare setting. Therefore, the current treating team has recommended an application for state guardianship to allow for these decisions to be made in a manner which serves the best interests of Ms. P.
A collaborative approach is recommended with the next of kin in determining the level of involvement and decision-making capacity for Ms. P in the future that all stakeholders are comfortable with. While parents have been supportive, an independent guardian would also serve as a further a protective factor in terms of advocacy for Ms. P’s vulnerability with her mental illness and intellectual disability. A capacity assessment by the clinical psychologist further supports the need for a decision maker.
As a rare illness, there is a distinctive lack of community residential or peer-support services for people with 22q11.2DS. There are also limited options for patients who have both psychiatric and physical healthcare needs, which poses a serious challenge to the needs of someone to the likes of Ms. P. Any potential long-term accommodation should have capacity to facilitate physical and mental healthcare. Operationally, this may include working with closely community mental health clinics or physical health outreach programs for timely review and management of acute deteriorations or crises. From a structural standpoint, such accommodation should be able to facilitate physical needs such as mobility requirements.
The complexity of lifetime care required by these patients may warrant the further establishment and availability of specialist clinics. These clinics may reduce burden on healthcare services by providing expert opinion and streamline supports by coordinating appropriate care. Indeed, already some countries and healthcare systems already have introduced multidisciplinary clinics to cater for such patients of rare illness with individualised multisystem needs 31 .
Conclusion
This case report showcases the complexity of treatment of comorbid multiple psychiatric and physical illness associated with 22q11.2 deletion syndrome, in the face of lack of specific guidelines. It shows that prolonged admission and purely pharmacological approach is not necessarily effective in psychotic and behavioural symptoms management. Indeed, such practices may contribute to the presentation itself. MDT approach based on neurobehavioral management principles in a lesser restrictive environment was shown to be effective in improving treatment outcomes after years of more restrictive practice for treatment refractory symptoms.
More research is called for to help clinicians grasp the optimal management approaches in providing the best clinical outcomes and in navigating the complex challenges posed by this cohort of patients. This would also help generate management guidelines in long term and rehabilitative care. Furthermore, this case report highlights the limited resources in terms of necessities for discharge accommodation and community supports currently available for people with 22q11.2 deletion syndrome and comorbid psychiatric illness.
Footnotes
Author contributions
Authors AK and RB have jointly contributed to the concept and design of this article. This includes acquisition and interpretation of the data as well as the editing of the manuscript. Author AK was the lead for the writing of the manuscript and the associated revisions. RB provided supervision for the production of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Approved by The Monash Health Research Office ERM Reference No. 80177 HREC Reference Number: QA/80177/MonH-2021-287069(v3).
