Abstract
Background:
Substance use disorders are more common among people with mental illness than in the general population. It makes recovery from mental illness more difficult, leads to frequent thoughts of suicide and re-hospitalization.
Objective:
Aimed to assess the prevalence of substance use disorders and associated factors among adult psychiatric patients in Jimma Town, Southwest, Ethiopia, 2017.
Methods:
A community-based cross-sectional study was conducted on a total of 300 patients with mental illness using the case tracing method. Participants were interviewed using the alcohol use disorder identification test questionnaire to assess Alcohol Use Disorder (AUD). Fagerstrom test tool for nicotine dependence and structured questionnaires were utilized to assess the socio-demographic characteristics of participants. Data were analyzed using SPSS version 20. The variable that showed association with AUD and nicotine dependence at P < .25 in the bivariate analysis was entered into multivariable logistic regressions to control confounders for both outcome variables independently. The significance of association was determined by P < .05 and strength was described using an adjusted odds ratio at a 95% confidence level.
Results:
The prevalence of alcohol use disorder and nicotine dependence was 14.3% and 23.3%, respectively. Female gender (AOR 0.15, 95% CI = 0.04-0.57), starting treatment within the first month of the onset of the illness (AOR 0.20, 95% CI = 0.05-0.82) and nicotine dependence(AOR 4.84, 95% CI = 1.85-12.67) associated with AUD. Additionally, being female (AOR 0.04, 95% CI = 0.01-0.25), joblessness (AOR 3.05, 95% CI = 1.30-7.16), absence of relapse of illness (AOR 0.18, 95% CI = 0.065-0.503), no improvement in illness (AOR 5.3, 95% CI = 1.70-16.50), and current khat use (AOR 3.09, 95% CI = 1.21-7.90) were associated with nicotine dependence.
Conclusion:
This study revealed a high prevalence of substance use disorders among psychiatric patients in the community. Being female, experiencing a shorter duration of illness before initiating treatment, and nicotine-dependence were significantly associated with AUD. On the other hand, female sex and absence of relapse of illness were negatively associated with nicotine dependence whereas, joblessness, less improvement of illness, and khat chewing were positively associated with it. Therefore, services on substance use disorders have to be extended to the community level with wide-scale training for the town’s health care providers, including health extension workers who have direct contact with these individuals. Accordingly, comprehensive and suitable interventions were advised to be provided on factors contributing to substance use disorders in general.
Introduction
Mental health is one of the vital elements of life and crucial for the wellbeing of individuals, societies, and countries. 1 Worldwide, about 450 million people suffer from mental or behavioral disorders. It accounted for 13% of the global burden of disease of which 4 of the 6 leading causes of years lived with disability are due to neuropsychiatric disorders such as depression, alcohol-use disorders, schizophrenia, and bipolar disorder.2,3 The most commonly diagnosed disorders were schizophrenia (64.3%), bipolar disorder (12.9%), and major depressive disorder (10%) among psychiatric patients in Ethiopia. 4
World Health Organization indicated that 8.9% of the total burden of disease comes from the use of psychoactive substances in which tobacco, alcohol, and other illicit drugs shared 4.1%, 4%, and 0.8% of the burden worldwide, respectively. 5 Substance use disorders are more common and challenging among people with mental illness than the general population.1,5-9
The overall prevalence of SUDs was higher among psychiatric services in hospital settings which been found to be 23% in Stanley, 10 36.3% in London, 11 and 37% in Denmark. 12 Alcohol use disorder was the most dominating SUD in psychiatric diagnosis with varying prevalence in different countries12-14 24.7% in Denmark, 12 31.6% in London, 11 and 51% in the USA. 15 Similarly there are varying figures in prevalence of AUD in Ethiopia accounting 2.7%, 16 24.5, 17 28.4%, 13 38.9%, 18 and 51.72% 19 in different settings. The prevalence of hazardous drinking was 5.7% whereas alcohol dependence was 2.5% in India. 20 In Ethiopia alcohol abuse, hazardous drinking, and alcohol dependence was 5.8%, 23.3%, and 9.8% among psychiatric patients respectively. On the other hand, 45.3% of males and only 21.4% of the females have AUDs. 18
Patients who diagnosed with severe forms of mental illness particularly schizophrenia 4 frequently manifest SUD compared to patients with other types of diagnosis. Some of the patients were Polly-substance users; alcohol with nicotine,13,18 khat with nicotine,21,22 and alcohol with nicotine and khat.21,23,24 Of these substances alcohol use disorder was strongly related to aggressive behavior in psychiatric patients. 4
On the other hand, nicotine is one of the several substances used in psychiatric patients. It is the most preventable cause of death worldwide and is accountable for the deaths of approximately half of its long-term users. In 2011, cigarette consumption killed more than 6 million people, nearly 80% in low and middle-income countries. It will kill 1 billion people in the 21st century if existing trends continue. On average, cigarette smokers lose about 15 years of their life.25,26 Approximately 47% of men and 12% of women smoke cigarettes worldwide and it is spreading rapidly in developing countries particularly among women. 27
The prevalence of nicotine dependence was high amongst persons with mental disorders. 21 It ranges from 16.6% to 88% in US23,28-31 and 13.1%, 13 20.5%, 21 40.1%, 19 to 47.6% 32 in Ethiopia among patients with mental illness.
The common reasons to use substances such as alcohol and nicotine in psychiatric patients were to cope and get relief from stress as self-medicating and to alleviate symptoms.8,13,14,24,33 However, far less attention has been paid to substance use disorders in psychiatric patients in which less than 25% of them get treatment for their substance use disorders. 13
Substance use disorders in these patients can lead to substantial negative consequences such as precipitating an earlier onset mental illness in certain individuals who are already vulnerable and makes recovery from mental illness more difficult.6,20,34-36 Additionally it can even worsen both the symptoms and the course of illness,7,37,38 increase vulnerability to relapses12,13,19 and re-hospitalization.7,13 Frequent thoughts and committing of suicide,8,21,39 homelessness 7 and risk of victimization 7 are very common among these patients. The other usual problems in psychiatric patients who have comorbid SUD are less employment level,15,38 frequent12,20/longer admissions,11,12,20 and committing violent acts. 40
Moreover, socio-demographic characteristics such as being male,13,21,23,38,41 single,11,20 younger age,13,14 fewer years of formal education, 17 and having parents who drink alcohol 4 were highly associated with experiencing SUD in psychiatric patients.
In Ethiopia, even though many people with mental illness were using substances, little is known about substance use disorders and associated factors particularly in psychiatric patients in the community. Therefore, this study was aimed to assess the prevalence of substance use disorders and associated factors among patients with mental illness who have been ever treated at Jimma university teaching hospital (JUSH), living in Jimma town.
Materials and Methods
Study design and setting
A community-based cross-sectional study was conducted in Jimma town, Southwest Ethiopia, from April 1 to May 30, 2017. The town is found in Oromia regional state and located 352 km southwest of Addis Ababa which is the capital city of Ethiopia. The town has 17 administrative units (kebeles). The total number of households reported within the town was about 32,191. The entire population of Jimma town from the 2007 central statistical agency (CSA) census is reported to be 120, 960 with a projection rate of 4.7. Accordingly, the total population had been estimated to be around 144,369 in 2011. The town has 2 hospitals; a general hospital and 1 specialized University hospital. Psychiatric outpatient and inpatient services are available only at the University hospital whereas, the general hospital focused on providing outpatient treatments.
Population
The Source populations were residents of Jimma town who have mental illness and age ⩾18 years. The study population was a sampled adult psychiatric patients who were residents of the town and have been treated for mental illness at the psychiatry clinic of JUSH. Patients with hearing impairment and cognitively impaired to consent were excluded from the study.
Sampling technique
There were more than 1200 individuals of all age groups who have ever followed-up treatment at psychiatry clinic with different diagnoses and duration of treatment. Out of these individuals, 698 adults (of age ⩾18 years) patients were identified from the medical registration office of the hospital.
First, addresses; phone numbers, and Kebeles (residential place) of all adult psychiatric patients (n = 698) who have been treated for mental illness at the psychiatry clinic of JUSH and residents of the town were listed out from the medical registration office. Additionally, important information like the type of diagnosis was extracted from their charts. Then the list of these patients was distributed to the health extension workers of every kebeles to trace their home using the registered address. To get study participants, tracing of individuals’ homes in the community was applied by health extension workers in each kebeles at Jimma town for all adult patients with mental illness who have been treated in JUSH psychiatric clinic. Based on this, 304 adult psychiatric patients were traced across the town whereas the rest of the patients couldn’t be traced because of many reasons (changing residency place, death, and others). Hence, these individuals became the final sample size of this study with the authors’ consensus.
Alcohol use disorder
Alcohol Use Disorder Identification Test (AUDIT) was utilized to assess alcohol use disorder. It was developed by WHO with sensitivity and specificity of 0.90 and 0.80 for Alcohol use disorder (AUDs) respectively. Utilizing AUDIT is an easy way of screening for problematic drinking. It assists to identify individuals with hazardous and harmful behavior of alcohol intake. It also used to suggest a guide for intervention that can help hazardous and harmful drinkers reduce or cease alcohol consumption. 32 Questions number 2 and 3 of AUDIT were modified according to the local context to calculate standard drink. There many types of local alcoholic drinks, few of them are “arake” (made distilled from fermented barley or maize combined with “gesho” [Rhamnusprinioides]), “tela” (fermented from barley and Rhamnusprinioides), and “teji” (honey wine) were first converted from local measurements (receptacles) to milliliters based on previous studies in Ethiopia that investigated the ethanol content of local beverages. 42 These receptacles are “malekia,” “tassa,” and “birille” for Arake, Tella, and Teji respectively. After converting the alcohols in these receptacles to milliliters, the mass and volume of the measured alcohols were calculated and converted to standard drinks. Local beer and wine were converted to standard drinks based on their alcohol content. South African standard drink containing 12 g of pure alcohol was used to determine standard alcohol drink in this study due to the absence of policy defining this issue in Ethiopia. 43 A total AUDIT score of 8 or more was used to define probable AUD. AUDIT score of 1 to 7 indicated social drinking, a score of 8 to 15 indicated “hazardous drinking”, a score of 16 to 19 was used for “harmful drinking” and a score of 20 or above indicated probable alcohol dependence. 32
Nicotine dependence
Fagerstrom Test, consisting of 6 items which were refined from the Fagerstrom Tolerance Questionnaire was used to assess nicotine dependence. The scores of items of the Fagerstrom test should be summed up to identify the of level nicotine dependence. Accordingly, the scores of 1 and more represented the presence of nicotine dependence. The categories of its severity were described with a Fagerstrom test score of 1 to 2 indicating low dependence with a recommendation of monitoring for withdrawal symptoms. The score of 3 to 4 represent low to moderate dependence, 5 to 7 moderate dependence, and score of 8+ indicating high dependence on nicotine. 44
Explanatory variables
World Health Organization Disability Assessment Schedule (WHODAS 2.0) which has been developed by the WHO to better understand the difficulties people may have due to their health conditions was used to assess functional disability. 45 In this study, the WHODAS 2.0 scales were dichotomized as the “Yes” (representing the presence of disability) or “No” (representing the absence of disability) category. The participants have a limitation in a specific domain of functioning when responding mild, moderate, severe, and extreme, in which these entire positive responses were merged into a “Yes” group. However, those who responded “none” were categorized as having “No” problem in their functioning.
Clinical Global Impression scale (CGI) was a 3-items observer-rated scale that measures illness severity, global improvement or change, and therapeutic response. It is designed to make use of all information available about the client. Thus, clinical interviews with the patient could be combined with the clinician’s observation for that time period.46,47
The second item of this tool was utilized separately more frequently in clinical and research areas to measure the level of clinical global improvement/change (CGIC). The CGIC is rated on a 7-point scale, for the total improvement using a range of responses from 1 (very much improved) through to 7 (very much worse). 48
Accordingly, in this study, an improvement from illness was decided by rating the second item (CGIC) independently by dichotomizing it into 2 categories as improved/not improved. While doing this, the prior worse stage of illness from history was compared with the condition since starting treatment for every client. Based on this information, the scores of “very much improved = 1” and “Much improved = 2” were categorized as “improved (treatment responders)” whereas, “minimally improved = 3,” “no change = 4 and minimally worse = 5,” “much worse = 6 and very much worse = 7” scores of the item 2 were considered “not improved (non-responders).”
Khat [Catha edulis] chewing was assessed by asking the history of khat chewing in the past 1 month. 49
Socio-demographic and economic factors such as age, sex, marital status, ethnicity, religion, educational status, occupation, and income were assessed.
Clinical related factors including the total duration of illness; prior to initiation of treatment and after initiation of treatment, number of admissions, frequency of relapse, functionality, symptoms improvement, suicidal attempt, and psychiatric diagnosis of the participants were also assessed.
Data collection procedures
Data was collected by interviewing traced individuals. About 2 psychiatric BSc. nurses and 4 postgraduate students in integrated clinical and community mental health had participated in data collection. Two days of training for data collectors were given on the objective of the study, data collection methods, tools, how to maintain confidentiality, consent form, and how to handle ethical issues. The questionnaires had been pretested at Agaro town on 5% of the total sample which is found 45 km away from Jimma town. Its results were not included in the final findings of the research. Data collection was supervised by 2 mental health professionals in addition to the principal investigator. Data quality and completeness of the questionnaires were checked by the supervisor monitored.
The questionnaires were prepared in English, translate into the local languages (Amharic and Afaan Oromo), and back-translated to English, so as to ensure its consistency. Finally, data collection was conducted using the Amharic and Afaan Oromo versions of the questionnaires.
Operational definition
Substance use disorders
Represented alcohol use disorder and nicotine dependence among adult psychiatric patients living in Jimma town in this study.
Alcohol use disorders
The overall AUDIT score of ⩾8 represented AUD. Additionally, the AUDIT score was categorized as 8 to 15, 16 to 19, and ⩾20 showing the severity of drinking that represented hazardous drinking, harmful drinking, and probable alcohol dependence, respectively.
Nicotine dependence
Fagerstrom test scores of ⩾1 were indicated the existence of nicotine dependence. The score of 1 to 2 indicated low dependence, 3 to 4 low to moderate dependence, 5 to 7 moderate dependence, and 8+ indicated high dependence on nicotine.
Current khat chewers
Adult psychiatric patients who chewed khat within 1 month prior to data collection time.
Data processing and analysis
Once all necessary data was obtained, each variable was coded, data was entered, and analyzed using Statistical Package for Social science version 20. The demographic characteristics of participants were computed by using simple descriptive statistics. Bivariate analysis was done to see the association of each independent variable with the outcome variables. All variables that have an association with AUD and nicotine dependence in the bivariate logistic regression with a P-value less than .25 were entered together into a multivariable logistic regression in order to control the potential confounders for both outcome variables independently. Finally, P-values of less than .05 was taken to declare that the association is statistically significant. The strength of the association of the variables was described using an adjusted odds ratio at a 95% confidence level.
Ethical consideration
Jimma University’s Institutional Review Board (IRB) was provided us the ethical clearance. Written informed consent was obtained from all participants of this study. The anonymity of data was kept at all stages of data processing. Patients who were severely ill including these having suicidal ideation were linked to JUSH for further evaluation and management.
Results
Socio-demographic characteristics of study participants
From a total of 304 traced psychiatric patients in Jimma town, 300 individuals participated in the study with a response rate of 98.7%. Four of the patients were missed do due to repeated closed homes during data collection. The majority, 185 (61.7%) of the participants were male. The mean age of participants was 34.99 (SD ± 11.5) years, ranging from 18 to 85 years. Of the total participants, 145 (48.3%) were Oromo in ethnicity and 129 (43%) were Muslims. Regarding marital status, 185 (60.7%) of the study participants were single. About 104 (34.7%) of the patients were attended primary education while n = 139 (46.3%) of them were jobless. Nearly two-third, 191 (63.7%) of the patients reported that they do not have a monthly income of pocket money (Table 1).
Socio-demographic characteristics of patients with mental illness who have been treated at JUTH, living in Jimma town, southwest Ethiopia, 2017 (n = 300).
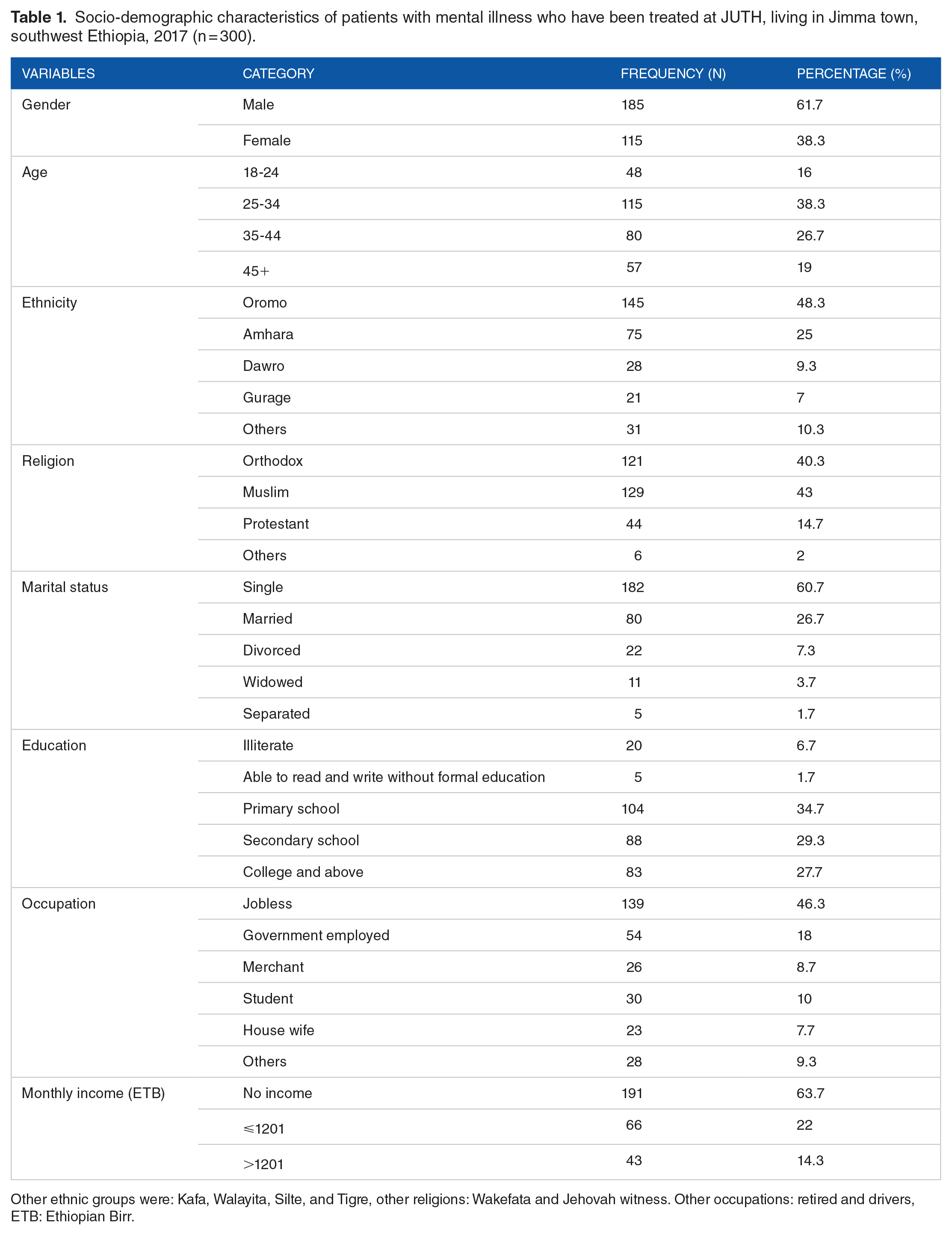
Other ethnic groups were: Kafa, Walayita, Silte, and Tigre, other religions: Wakefata and Jehovah witness. Other occupations: retired and drivers, ETB: Ethiopian Birr.
Clinical related factors of the study participants
The most common primary psychiatric diagnosis was schizophrenia 96 (32%) followed by major depressive disorder 73 (24.3%).
Among the study participants, 88 (29.3%) of them had a total duration of illness between 6 months to 4 years, while 72 (24%) of them had a longer total duration of illness from 11 to 28 years. Almost one-third, 97 (32.3%) of the patients stayed 6 months to 2 years before getting treatment for their illness. One-fourth 74 (24.7%) of them were treated for less than 1 year. About 203 (67.7%), 161 (53.7%), and 254 (84.7%) of them had experienced at least 1 relapse, have no history of admission, and improved from their illness respectively. A suicidal attempt was accounting for 92 (30.7%) of the participants. About 174 (58%) of the patients have disabilities in their functioning (Table 2).
Clinical related characteristics of patients with mental illness who have been treated at JUTH, living in Jimma town, southwest Ethiopia, 2017 (n = 300).
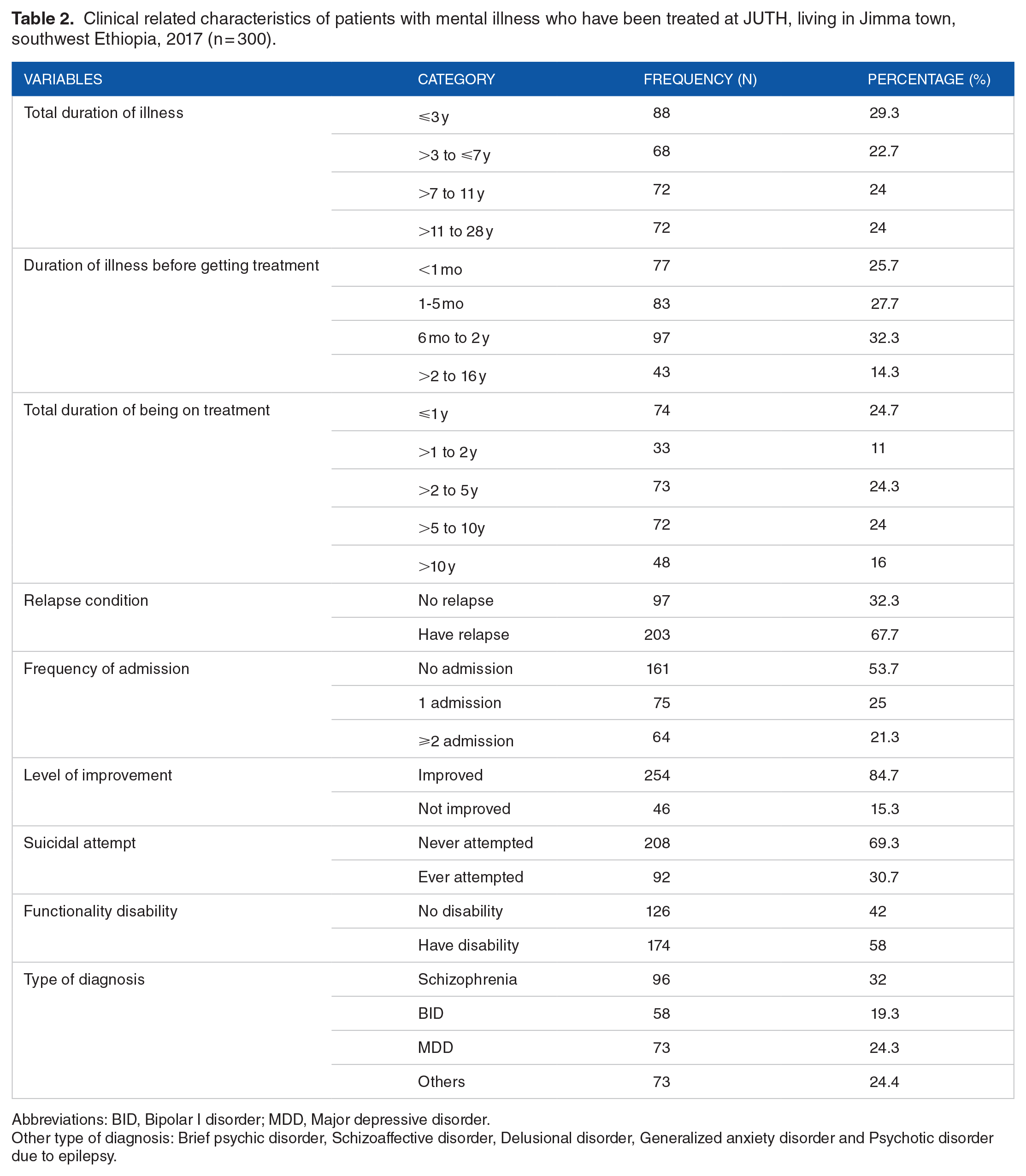
Abbreviations: BID, Bipolar I disorder; MDD, Major depressive disorder.
Other type of diagnosis: Brief psychic disorder, Schizoaffective disorder, Delusional disorder, Generalized anxiety disorder and Psychotic disorder due to epilepsy.
Prevalence of alcohol use disorders
Out of the total participants, 21.7% (n = 65) of them reported that they had drunk alcohol in the last 12 months. However, 7.3% (n = 22) were identified as social drinkers (AUDIT score 1-7). The overall prevalence of alcohol use disorder (defined as an AUDIT score ⩾8) was 14.3% (n = 43) with (95%, CI 10.3-18). Hazardous drinking, harmful drinking, and alcohol dependence were found in 8% (n = 24), 2.3% (n = 7), and 4% (n = 12) of the participants respectively.
Alcohol use disorder was present in 21.1% (n = 39) of males and 3.5% (n = 4) of females. Males were identified as more hazardous drinkers 10.8% (n = 20) compared to females 3.5% (n = 4). Similarly, only males were alcohol dependent in this study (6.5% (n = 12) males vs. none of the females). Amongst patients with AUD 72.1% (n = 31) of them chewed khat and 55.8% (n = 24) of them were nicotine dependent.
Prevalence of nicotine dependence
The prevalence of nicotine dependence was 23.3% (n = 70) with (95%, CI 18.5-27.3). Among patients with nicotine dependence 4% (n = 12), 8% (n = 24), 7.3% (n = 22), and 4% (n = 12) of them had low dependence, low to moderate dependence, moderate dependence and high nicotine dependence, respectively. Nicotine dependence was 36.8% (n = 68) in males and 1.7% (n = 2) in females.
Factors associated with alcohol use disorder and nicotine dependence
The bivariate logistic regression analysis showed that gender, ethnicity, religion, starting treatment within the first month of the onset of illness, staying for 1 to 6 months before initiating treatment, having no improvement of illness, suicidal attempt, absence of functional disability, having nicotine dependence and khat use had a significant association with prevalence of AUD (P < .05). Additionally in the bivariate analysis gender, marital status, educational level, occupation, longer duration of being on treatment (11 to 28 year), absence of relapse of the illness, having 2 or more admission, not having an improvement of the illness, bipolar I disorder, major depressive disorder, other psychotic disorders, AUD and khat use was associated with nicotine dependence (P < .05) (Table 3).
Socio-demographic and clinical related factors associated with AUD and nicotine dependence in the bivariate analyses among patients with mental illness who have been treated at JUTH, living in Jimma town, southwest Ethiopia, 2017 (n = 300).
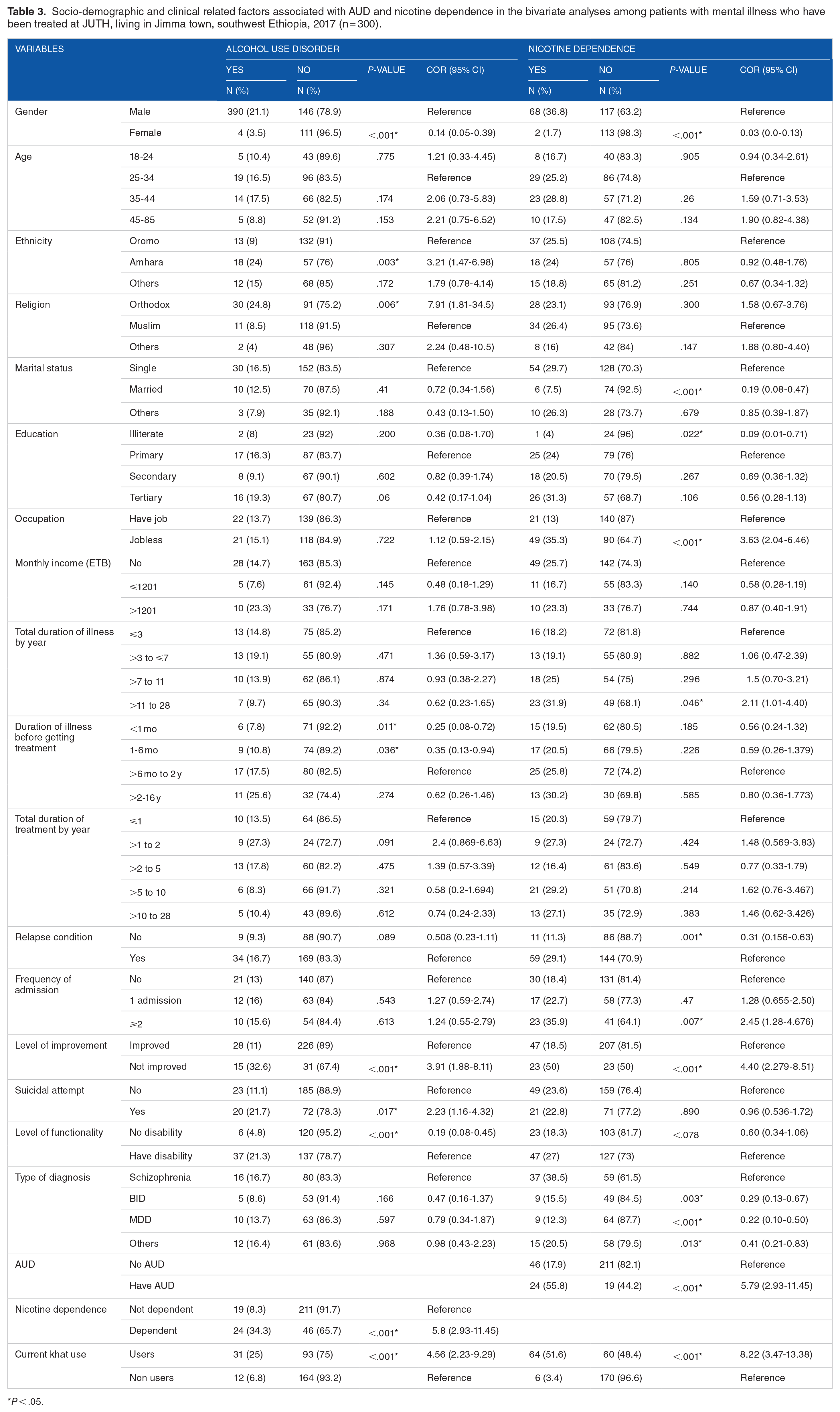
P < .05.
After adjusting for potential confounders by using multivariable logistic regression; female sex, duration of illness before initiating treatment, and nicotine dependence were significantly associated with AUD. Additionally, nicotine dependence was significantly associated with being female, joblessness, having a relapse, and the absence of improvement from mental illness.
The odds of having AUD among females was 85% times less likely compared to that of male participants (AOR 0.15, 95% CI = 0.04-0.57). The odds of patients who started their treatment within the first month of the onset of their illness to have AUD was 80% times less likely as compared to those who started the treatment within 6 months to 2 years (AOR 0.20, 95% CI = 0.05-0.82). Respondents with nicotine dependence had more than 4 times (AOR 4.84, 95% CI = 1.85-12.67) a higher prevalence of AUD than patients who were not nicotine dependent.
The odds of having nicotine dependence among females was 96% times (AOR 0.04, 95% CI = 0.01-0.25) less likely compared to their counterpart. Respondents who were jobless were 3 times (AOR 3.05, 95% CI = 1.30-7.16) higher affected by nicotine dependence than respondents who were on different works. Patients who have no relapse of illness had 82% times the lower prevalence of nicotine dependence than patients who have at least 1 relapse (AOR 0.18, 95% CI = 0.065-0.503). The odds of having nicotine dependence were more than 5 times (AOR 5.3, 95% CI = 1.70-16.50) higher among participants who were not improved from their illness than participants who have improved from their illness. The odds of nicotine dependence among patients who were khat chewers were 3 times (AOR 3.09, 95% CI = 1.206-7.896) higher when compared to non- chewers (Table 4).
Multivariable logistic regression of factors associated with AUDs and nicotine dependence among patients with mental illness who have been treated at JUTH, living in Jimma town, southwest Ethiopia, 2017 (n = 300).
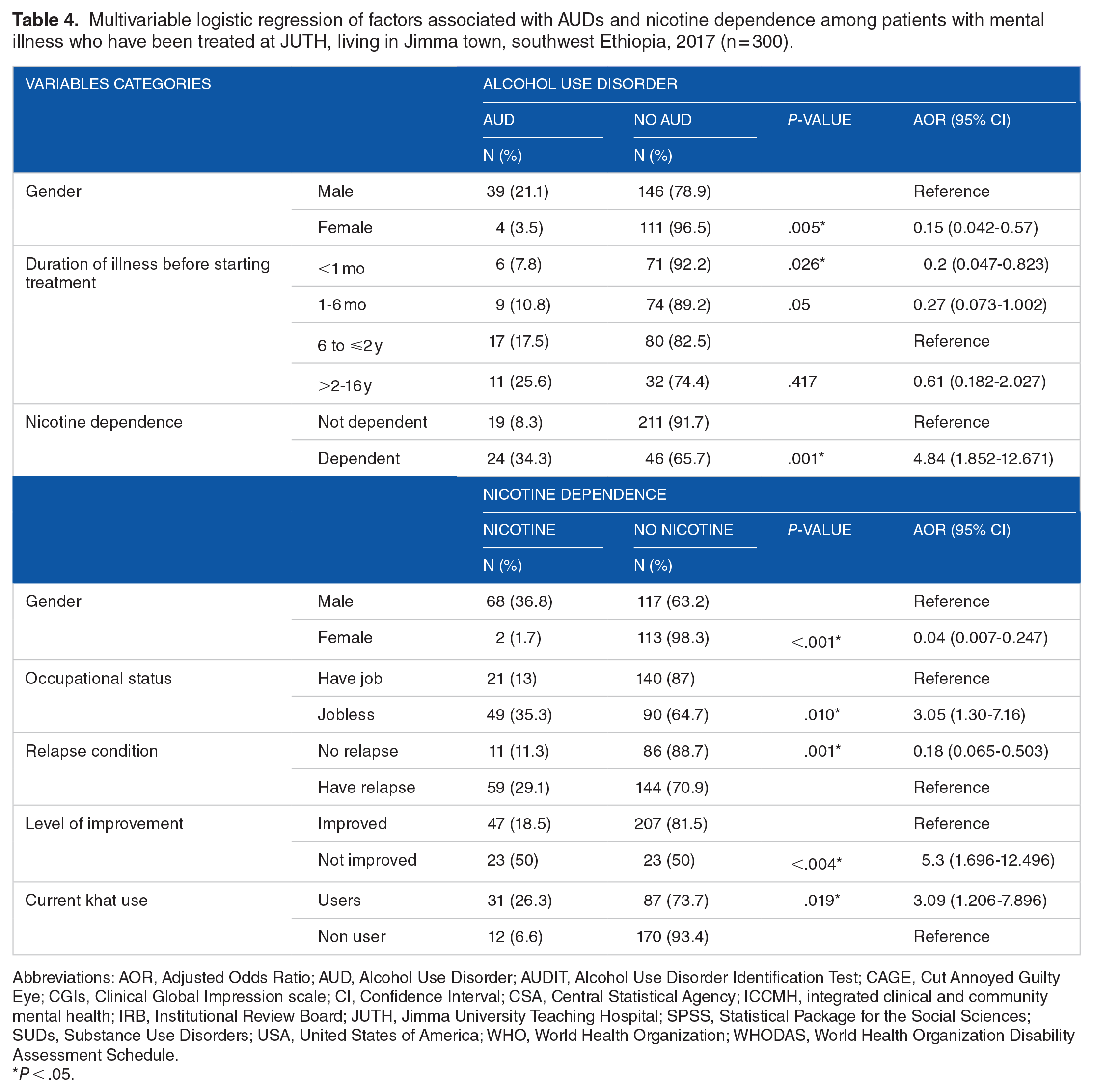
Abbreviations: AOR, Adjusted Odds Ratio; AUD, Alcohol Use Disorder; AUDIT, Alcohol Use Disorder Identification Test; CAGE, Cut Annoyed Guilty Eye; CGIs, Clinical Global Impression scale; CI, Confidence Interval; CSA, Central Statistical Agency; ICCMH, integrated clinical and community mental health; IRB, Institutional Review Board; JUTH, Jimma University Teaching Hospital; SPSS, Statistical Package for the Social Sciences; SUDs, Substance Use Disorders; USA, United States of America; WHO, World Health Organization; WHODAS, World Health Organization Disability Assessment Schedule.
P < .05.
Discussion
In this community-based cross-sectional study, the prevalence of AUD was 14.3%. which was lower than the finding of various studies conducted in psychiatric units in Ethiopia (28.4%, 38.9%, 51.72%),13,18,19 Denmark 24.7%, 12 London 31.6%, 11 and USA 51%. 15 This discrepancy could be because of the difference in study settings in which the previous studies conducted at hospital outpatient departments while the present study was carried out at the community level within which the prevalence of AUD might be lower. Additionally, it could be due to the difference between tools employed in this study (AUDIT) and the study was done in London 11 used (Alcohol Screening Questionnaire) that assesses a lifetime history of alcohol drinking. The prevalence of AUDs found in this study was in agreement with the finding of a study conducted in India among patients with a severe form of mental illness 16.8%. 20 However, it was higher than the result of the study conducted in Addis Ababa, Ethiopia (2.7%), 16 which might be due to this study used (AUDIT on small sample vs. the previous study used cut-annoyed-guilty-eye (CAGE) on the large sample), as well as CAGE is designed to detect more severe AUDs than AUDIT.
The prevalence of nicotine dependence was found to be 23.3% which is in line with the finding of the studies done in Ethiopia among psychiatric patients 20.5%.18,21 It was lower than that found in previous studies in different countries, 40.1% 19 in Ethiopia, and varies from 47.6% to 88% 32 in the USA. The reason could be due to the difference in study settings, the former studies were institutional-based whereas the current was carried out at the community level. This study demonstrated a higher prevalence of nicotine dependence than the other reports, 16.6% 28 in the USA, and 13.1% 13 in Ethiopia. This could be due to the latter study was involved only patients with a severe form of mental illness.
Being female was negatively associated with AUD which was in agreement with the study done in London among patients with severe mental illness, 12 in India, 20 and Ethiopia.4,13,18 This might be related to the fact that social desirability bias might be even stronger, particularly in women, as persons who use alcohol and other substances tend to under-report or deny their use. As part of this reason, cultural restrictions are high on females in the use of alcohol in which excessive alcohol drinking and being intoxicated is not acceptable especially, in females in Ethiopia. Also, women have a lower concentration of liver alcohol dehydrogenase than do men which is responsible for the metabolism of a substantial amount of alcohol before it enters systemic circulation. 41
Additionally, patients who started their treatment within the first month of the onset of their illness had decreased odds of having AUD as compared to those who started their treatment 6 months to 2 years later after the onset of their illness. This was in agreement with the study conducted in India. 20 This might be explained by the fact that psychiatric patients use different substances as self-medication for their illness which may extend the untreated duration of illness.
On the other hand, experiencing nicotine dependence among patients with mental illness was positively associated with AUD compared to patients without nicotine dependence. This finding was in agreement with the study conducted in Ethiopia on patients with mental illness in which cigarette smoking was significantly associated with AUD compared to non-smokers.18,21 This could be because once people start to use a given substance they might have a higher chance of adding another substance to get the desired effect.
Female sex was negatively associated with nicotine dependence compared to males, which was similar to a study done on a similar population in Scotland, 38 US, 23 and Ethiopia. 21 This might be due to cultural restrictions on females not to use many substances.
The study demonstrated that joblessness was positively associated with nicotine dependence. This is also consistent with the report of studies from Scotland 38 and the USA.15,28 The reason could be patients who have no job spent their time using substances as a coping mechanism for their worry about joblessness. Additionally, joblessness could be a reflection of the higher burden of symptoms of mental illness in patients who abuse nicotine 50 .
Having no relapse of mental illness by patients was negatively associated with nicotine dependence when compared with patients who have at least 1 relapse which was supported by the studies in Canada, 7 India,20,37 Scotland, 38 Denmark, 12 and Ethiopia.13,19 This may also be explained by the fact that nicotine dependence increases the metabolism of the medication that the patient was taking. This, in turn, leads to reduced drug plasma levels which increases the probability of having a relapse of mental illness. Also, relapse indicates a more severe illness with a higher symptom load leading the patients to use substances as a coping strategy.
Non-improvement of the illness was found to have a positive association with nicotine dependence. Studies carried out on patients with mental illness in countries such as India, 37 Scotland, 38 Norway, 34 and Ethiopia 4 supported our finding in which cigarette smoking delay the improvement of the illness or remission of symptoms. The possible reason could be smoking increases the metabolism of the drugs given for treating the illness. Additionally, this study revealed a higher relapse of illness in nicotine-dependent patients which could contribute to the non-improvement of the illness and vice versa.
Chewing khat was positively associated with nicotine dependence in patients with mental illness which was supported by studies conducted in Ethiopia.21,22 This could be because once the patients started using the substance, they continue to either increase the dose or add another substance to get the desired effect as they could develop dependence. 24
Limitations
The data was collected depending on patients’ self-report during the interview which might be subjected to recall bias. Additionally, the absence of a policy explaining the standard alcohol drink in Ethiopia and the use of cross-sectional design is another shortcoming of this study. The CGI does not provide a total score and has been criticized for its inconsistency, instructions, its unrepresentativeness for acute efficacy versus prophylactic utility, and time domains.
This study focused only on nicotine dependence which might underestimate the prevalence of smoked tobacco as a general. On top of this, the result of the study was discussed using the researches that were conducted in different hospital settings. It is due to the dearth of community-based information (data) regarding this title as per the effort of the authors to access the literature.
Conclusion
The most common substance use disorder among psychiatric patients who were residents of Jimma town was nicotine dependence followed by AUD. Being female and having a shorter duration of illness before initiating treatment was found to be negatively associated with AUD. However, nicotine-dependence was positively associated with AUD. On the other hand, female sex and absence of relapse of illness were negatively associated with nicotine dependence whereas, joblessness, less improvement of illness, and khat chewing were positively associated with it. Therefore, services on substance use disorders have to be extended to the community level with wide-scale training for the town’s health care providers, including health extension workers who have direct contact with these individuals. Accordingly, comprehensive and suitable interventions were advised to be provided on factors contributing to substance use disorders in general in this population.
Footnotes
Acknowledgements
We would like to thank our study participants for giving us their time to participate in this study. Finally, our gratitude is extended to Jimma University for supporting us financially.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The received financial support for the research from Jimma University.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
BD has contributed to the conception, design, conduct, analysis, and interpretation of the research and in the manuscript preparation. MS and EY contributed to the conception, design, and analyses of the research and in the review of the manuscript. DT, MA, AM, HH, HK, AN, BM, LA, and EA participated during the conception, designing of the study, and reviewing the manuscript. The authors were reviewed and agreed on the contents of the manuscript.
Data Availability
The data utilized for this study could be accessed from the corresponding author if demanded.
