Abstract
Background
Specific phobia (SP) is one of the most common mental disorders among general population. In this national survey in Iran, we aimed to identify the lifetime prevalence, predictors, and co-morbidities of SP among children and adolescents.
Methods
A face-to-face household interview was applied by 250 skilled clinical psychologists using the Persian version of the kiddie schedule for affective disorders and schizophrenia for school-age children/present and lifetime version (K-SADS-PL) to determine the prevalence of SP and its co-morbid conditions.
Results
About 30 000 individuals participated in this study. We identified 923 individuals (378 boys and 545 girls) with SP. The lifetime prevalence rate of SP was 4.8%. This condition was related to gender, age, and type of settlement. Female gender and living in urban areas were the main positive predictors of developing SP. We showed that parental educations and their history of psychiatric hospitalization were not predictors of SP occurrence. Anxiety and behavioral disorders were the most common reported co-morbidities in our included children and adolescents.
Conclusions
The findings of this study indicate that SP is a prevalent disorder among pediatric population with different co-morbidities and should not be underestimated.
Background
Anxiety disorders are among the most frequent psychiatric conditions. Subgroups included generalized anxiety disorder (GAD), agoraphobia, panic disorder, specific phobia, and social phobia. Marked persistent fear associated with a specific object or situation that results in avoidance and leads to functional impairment is now known as specific (simple) phobia (SP). 1 This condition is one of the most common mental disorders among general population but remained under-appreciated in the literature. Phobias of animals and heights are the most common forms of SP, but phobias of flying, closed spaces, water, storms, and blood have also been described. 2
The frequency of SP varies among populations with different age groups. The life-time prevalence of this event is about 2% to 14% among adults.3,4 Higher prevalence, however, was reported among children and adolescents.5,6 The incidence rate of SP was reported to be about .4 to 2.2 per 100 person-years,7,8 and the cumulative incidence of 27% was estimated in one study. 9 A prior study on adults with SP revealed that the incidence by age of first onset had the highest rate at or below 5 years of age.2,10 The frequency of SP was found to be higher in females than males. A recent cross-national survey in 22 countries with different levels of incomes showed that SP was more prevalent in high and upper-middle income countries, compared to nations with low and low-middle income levels. 11
People with SP are at increased risk of developing different co-morbidities. More than half of cases with SP developed at least one other mental conditions. 11 A national survey showed that anxiety disorders (eg, GAD, panic disorder, and social phobia) were the most common co-morbid conditions among individuals diagnosed with SP. 12 Mood disorders and substance use were other frequent co-morbidities found in this population.
Few studies reported the frequency and predictors of SP among pediatric populations. In this national survey in Iran, we aimed to identify 1) the prevalence of SP among children and adolescents; 2) the risk factors of SP by gender, age, and other demographic characteristics; and 3) the co-morbidity patterns in pediatric population diagnosed with SP. Due to the chronic nature of this condition and its high impact on the function of affected people, this information can be helpful for clinicians and health-care policy makers.
Methods
Study design
This was a population-based cross sectional study and was part of The Iranian children and adolescents psychiatry (IRCAP) which is a nationwide project extracting the characteristics of psychiatric disorders in Iran. The complete methodology was already published. 13
Participants and sampling
Iranian children and adolescents aged between 6 to 18 years old who fulfilled our inclusion criteria were included in our study. Inclusion criteria were 1) individuals who have resided in a province of Iran at least for 1 year and 2) cooperation for completing the questionnaires. Severe physical and mental disabilities which could interfere with proper responding were the exclusion criteria.
In order to determine the sample of study, we applied a multistage cluster sampling method. In the first step, we chose children and adolescents from every 31 province of Iran from both rural and urban areas randomly. In the next step, from each of the clusters, six individuals were selected with at least one participant of each gender and in different age groups (6 to 9, 10 to 14, and 15 to 18). Finally, hundred and seventy blocks were chosen using the postal codes.
Instruments
Socio-demographic form
Socio-demographic questionnaire including questions about type of settlement, age, gender, and education status of parents as well as their history of psychiatric hospitalization was designed and applied.
K-SADS-PL
Kiddie schedule for affective disorders and schizophrenia for school-age children/present and lifetime (K-SADS-PL) is a well-known semi-structure psychiatric interview based on diagnostic and statistical manual of mental disorders, fourth edition (DSM-IV), which takes 30 to 60 minutes to be completed. K-SADS-PL can be used for diagnosis of mood disorders, anxiety disorders, psychotic disorders, behavioral disorders, substance use, tic disorders, eating disorders, and elimination disorders. The Farsi version of this questionnaire was used for all the participants. The consensual validity of SP diagnosis by Farsi version of K-SADS-PL was reported to be high (kappa score: .91). 14 Test–retest and inter-rater reliability of this translated version were sufficient. Excellent sensitivity (100%), specificity (96.9%), negative (87%), and positive predictive values (100%) were also described for SP. 14
Procedure
The ethics committee of the National Institute for Medical Research Development approved the final protocol (Number: IR.NIMAD.REC.1395.001). Written informed consent forms were signed by both parents and all adolescents who were at least 15 years old. Moreover, assent was achieved from all children. The information about all participants was kept confidential.
The collection of data was carried out by trained clinical psychologists. For this purpose, two hundred and fifty clinical psychologists with Master of Science degrees were recruited by Medical Universities in each of the provinces and attended a 5-day workshop. During these sessions, they were taught how to efficiently apply a diagnostic interview as well as how to analyze the results and score them properly. These workshops used the following methods for teaching: presentations, role-playing, interviews with real cases, and discussions.
This was a face-to-face survey and the clinical psychologists referred to the houses of participants and interviewed the parents and their children to achieve the data. The aims of the study were first described for all participants and they were informed about their rights to refuse to participate. Children and their parents were interviewed separately using K-SADS-PL. Finally, interviewers scored the items based on their “best-estimate” clinical judgment for all disorders including SP. Children less than 11 years old were interviewed in the presence of one of their parents.
Statistical analysis
IBM SPSS Statistics version 20 was applied and P-values less than 0.05 were considered significant. Continuous variable (age) was reported as mean with standard deviation (SD) or with 95% confidence interval (95% CI). Ordinal variables (gender, age groups, place of residence, parental educations, and psychiatric hospitalization) and non-continuous quantitative variables (SP prevalence and co-morbidities) were reported by using percentage.
All of the reported data were adjusted according to the population of each province in 2017. We also determined the odds ratio (OR) and multiple logistic regression analyses results to assess which variables across diagnostic groups were statistically significant predictors of SP. Socio-demographic risk factors and comorbidities were assessed by applying logistic regression analysis in order to determine the correlated variables.
Results
The study started on October 14, 2016, and lasted until November 21, 2017. From 30,534 eligible children and adolescents aged 6 to 18 years old, 29,878 individuals participated in this study (response rate was estimated to be 92%). The mean age of participants was 11.8±3.8. (mean ± SD).
Rates of specific phobia based on socio-demographic characteristics.
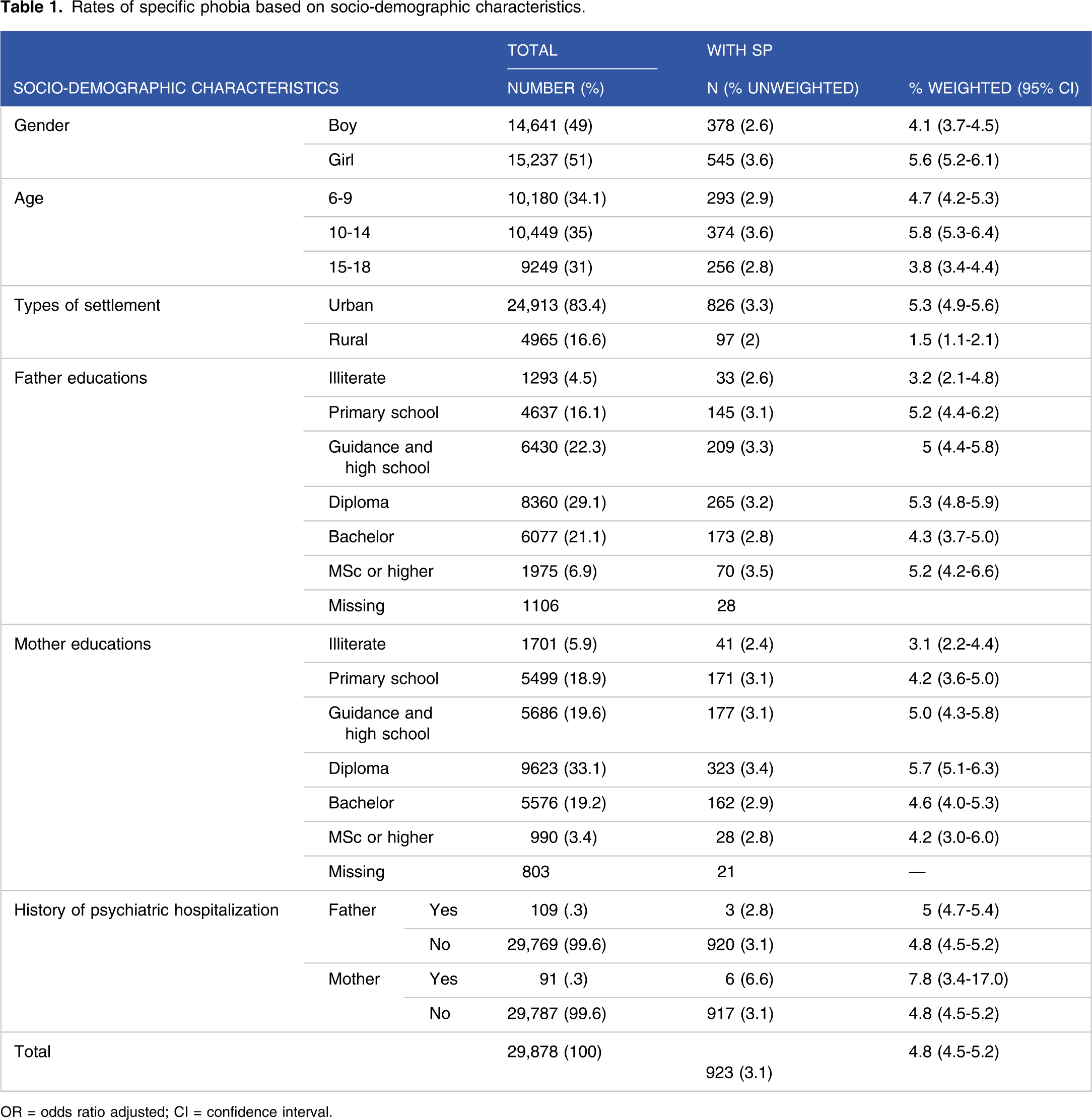
OR = odds ratio adjusted; CI = confidence interval.
Socio-demographic predictors for specific phobia based on univariate and multivariate analysis.
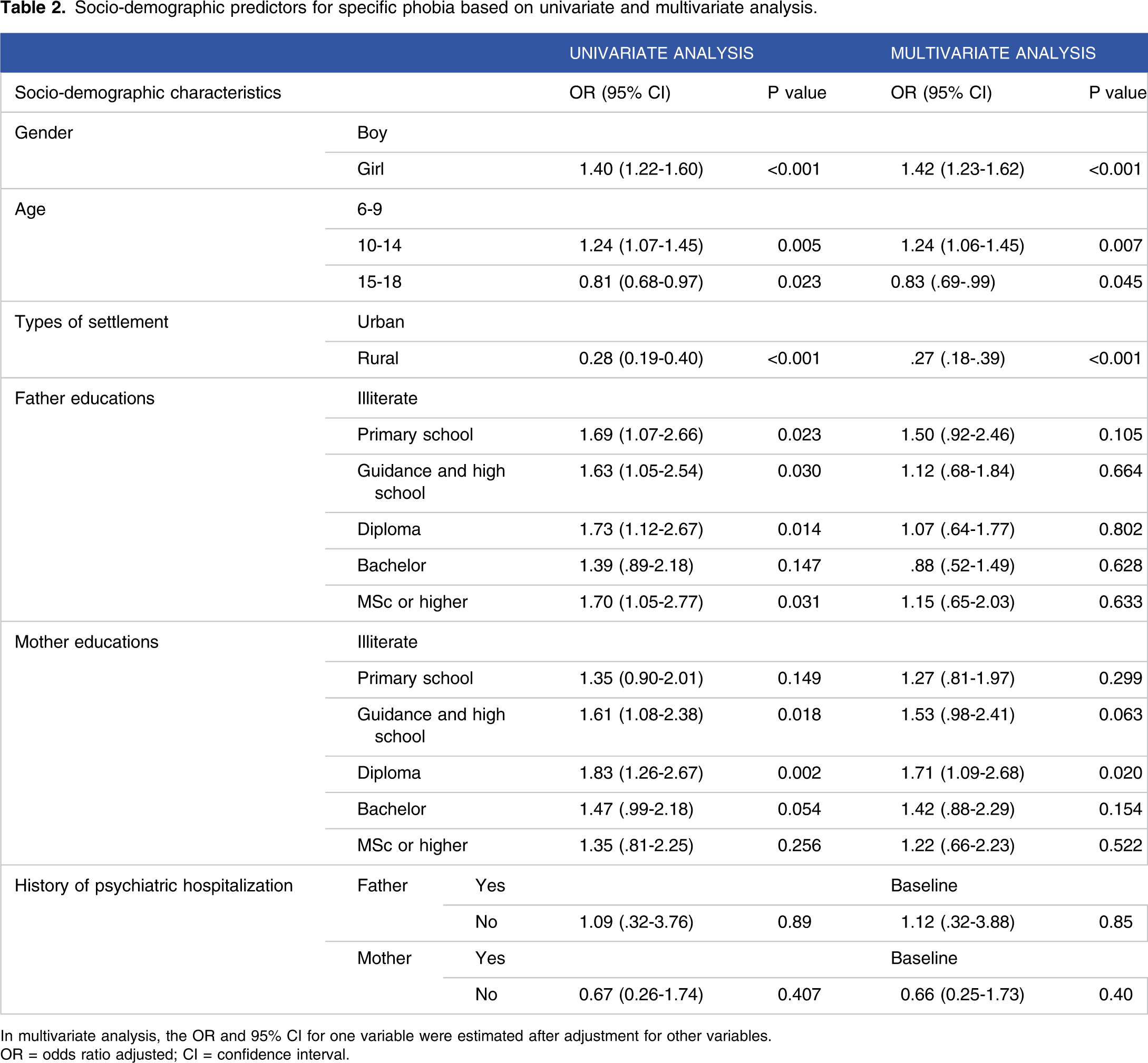
In multivariate analysis, the OR and 95% CI for one variable were estimated after adjustment for other variables.
OR = odds ratio adjusted; CI = confidence interval.
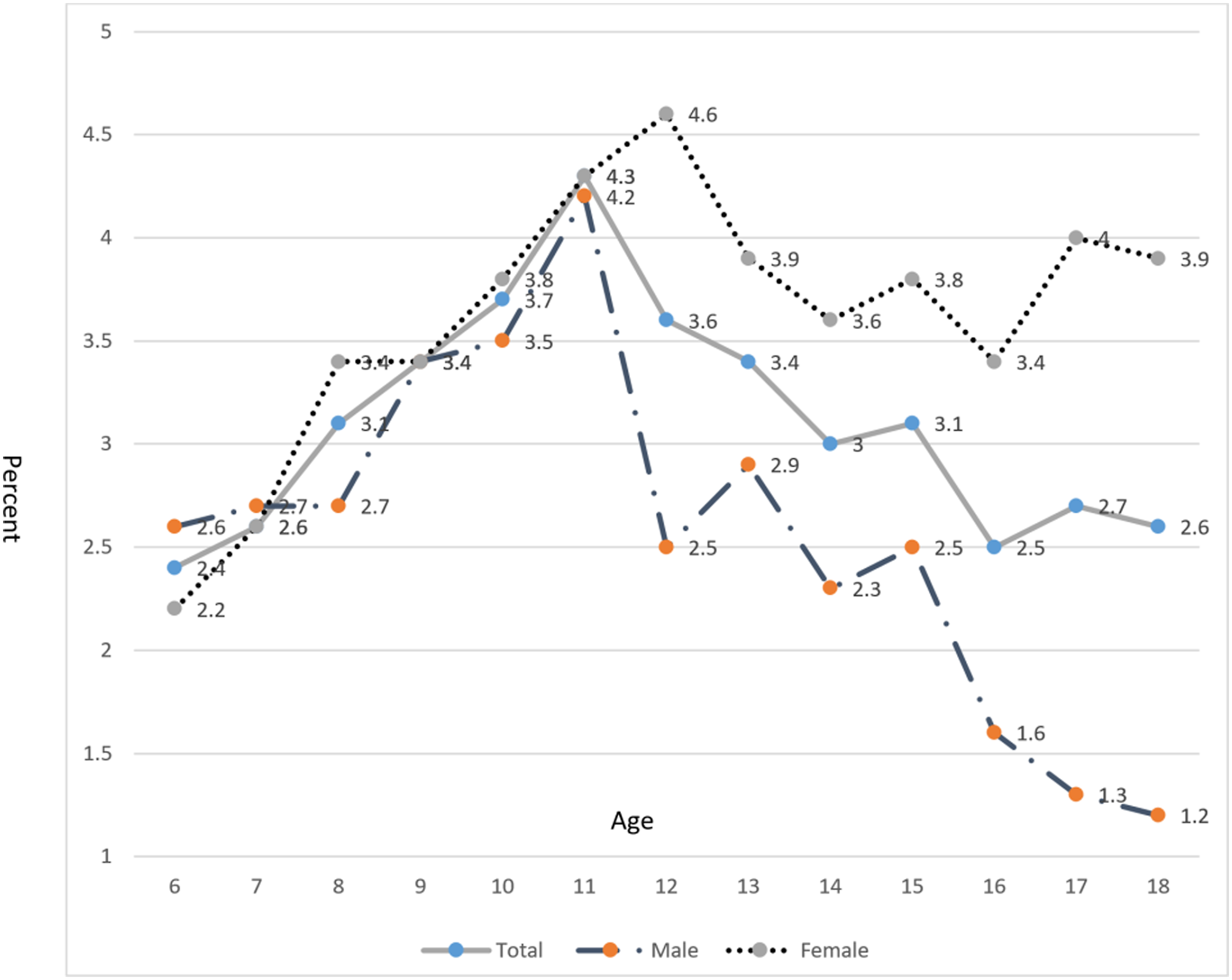
Rates of specific phobia by age trends and gender.
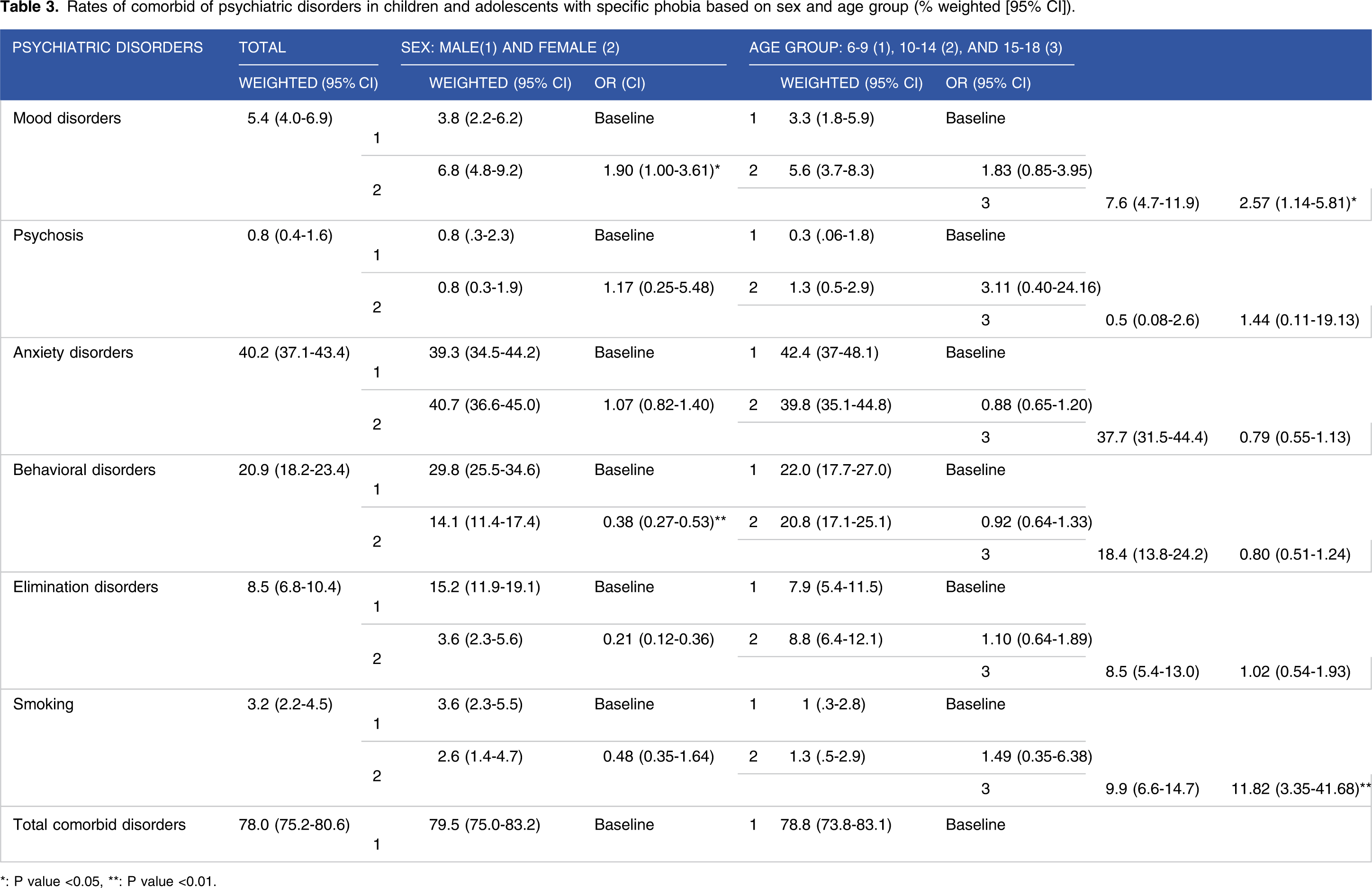
Over 80% of included children and adolescents (756 individuals) had at least one co-morbid condition accompanied with SP. From these individuals, 296 (32%) of cases had one co-morbidity and the rest (50%) had >1 co-morbidities. Separation anxiety disorder was the most common condition accompanied with SP (28.9%), followed by GAD (14.4%) and attention deficit hyperactive disorder (ADHD) (12.1%), respectively (Figure 2). Overall, anxiety conditions (40.2%), behavioral disorders (20.9%), and elimination disorders (8.5%) were the most frequent co-morbidities observed in our participants. The odds of mood disorders were significantly greater in females than males (OR: 1.90; 95% CI: 1.00-3.61), but behavioral conditions were statistically more common in males than females (OR: 2.63; 95% CI: 1.88-3.70). No significant differences in prevalence rates of co-morbid events among participants of different age groups were observed (Table 3). Prevalence of co-morbid disorders in specific phobia. Rates of comorbid of psychiatric disorders in children and adolescents with specific phobia based on sex and age group (% weighted [95% CI]). *: P value <0.05, **: P value <0.01.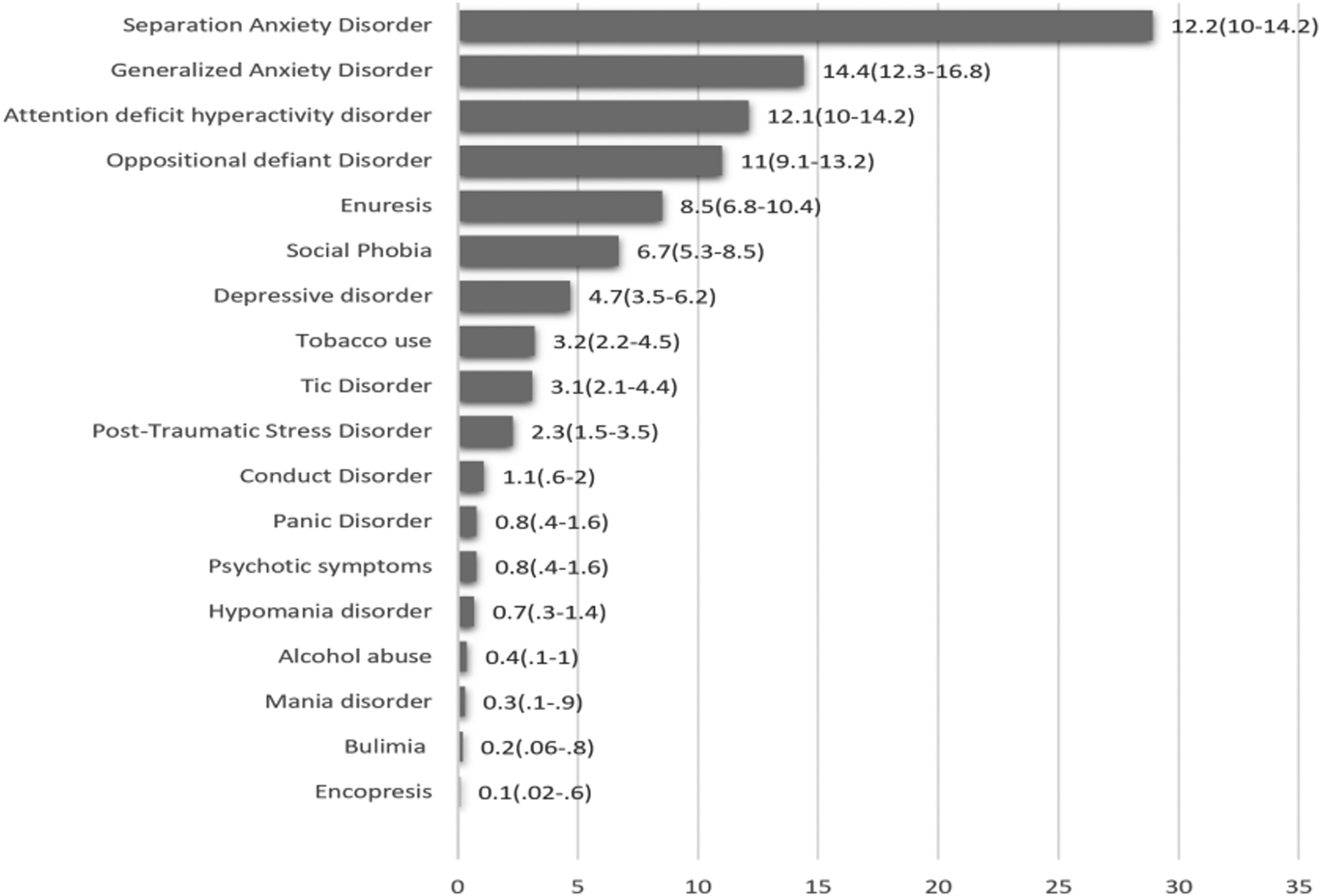
Discussion
Summary of results
To the best of our knowledge, this is the first nationwide study conducted on Iranian pediatric population, determining the prevalence, risk factors, and co-morbid conditions of SP. About 5% of children and adolescents were identified with SP using the K-SADS-PL assessment tool. This condition was related to sex, age, and type of settlement. Female gender and living in urban areas were the main positive predictors of developing SP. Anxiety and behavioral disorders were the most common reported co-morbidities in our included children and adolescents.
Previous studies
Prevalence of specific phobia
The data of one cross-national survey with over 124 000 participants aged 18 to 60 years old from 22 countries showed that the lifetime prevalence rate of SP was about 7.4% and was higher in females than males. 11 Our study indicated that Iran as an upper-middle income country had lower lifetime prevalence of SP than most of these countries and even nations with similar income levels (mean rate: 8%). Japan (3.8%) and Poland (3.8%) as high income countries, Romania (3.8%) as an upper-middle income country, and Iraq (4.2%) and Republic of China (2.8%) as low middle-income countries had lower prevalence rates of SP than the rate reported in this study. 11 Discrepancies in results can be due to the age range of participants, as well as geographical and cultural factors. Methodological differences can also affect the results. World Health Organization Composite International Diagnostic Interview (CIDI) (used in Ref. 11) and K-SADS-PL (used in our study) are two assessment tools in mental conditions. A prior study revealed that CIDI estimates were significantly higher than K-SADS-PL estimates for SP (51%). 15
The reported prevalence of SP in our study (4.8%) was lower than former studies performed on children and adolescents in South Korea (7.9%), 16 Turkey (11%), 5 the United States of America (15.1%), 17 Uganda (15.8%), 18 and Spain (16.2%). 6 However, one national cohort study with over 13,000 children and adolescents in Denmark showed that less than 1% of the individuals had SP. 19 Another study with about 1000 Nigerian adolescents aged 13 to 18 years old showed lower prevalence rate of SP (2.5%) than our estimated rate. 20 A study in Germany also indicated that the lifetime prevalence of SP was about 3.5% among 1 000 adolescents aged 12 to 17 years old. 21 We identified five previous studies with small sample sizes, performed on Iranian pediatric populations. The reported prevalence rates were 1.6% to 3% in three studies.22-24 One study, however, showed that over 20% of high school students had SP. 25 The prevalence of 18% for fear of physical injury was estimated in another study. 26 The discrepancies seem to be due to sample size and methodological differences rather than the cultural and geographical reasons.
Demographic associations
Data from current study showed higher prevalence of SP among females than males which was in line with multiple prior studies.5,16,18 One study on pediatric population, however, showed that the diagnosis of SP was unrelated to gender. 19 The etiology of this possible higher risk in females remained unclear, but the significant role of female reproductive hormone cycles on anxiety disorder onset and severity of condition have been described. 27 Some studies, on the other side, revealed the great influence of genetic, familial-environmental, and individual-specific-environmental factors on anxiety disorders in females. 28 Functional neuro-imaging showed that during an experimental condition of threat, anterior cingulate cortex, insula, and brain stem in females had higher activity than males. 29 Anterior cingulate cortex was shown to be critical in pathogenesis of psychiatric events including anxiety disorders. Further studies are needed to understand the exact pathomechanisms leading women more susceptible than males in developing SP.
Herein, we indicated that children and adolescents in urban areas were at higher risk of developing SP than pediatric population in rural regions. Similar result was achieved in two former studies in Norway3,30 and the United States of America.12,31 Cultural and geographical differences may explain increased risk of SP occurrence in urban areas.
Our findings revealed that parental education was not a predictor of SP development. A prior study on children and adolescents also showed that socio-economic status was not associated with developing SP. 16 We also identified that positive history of psychiatric hospitalization in parents did not significantly predispose their children to SP. The data on genetic contribution to SP is scarce and current studies involve overlapping samples. 32 A meta-analysis showed that according to these few existing studies, SP was moderately heritable with the highest mean heritability of 30% for blood, injection, and injury phobias. 32 Noted, twin studies suggest that common environmental factors lead to within-family resemblance in childhood, while genetic factors cause familial resemblance in adulthood. 2 Further studies should describe the inherited patterns in developing SP in both children and adults.
Co-morbid conditions
Anxiety disorders including separation anxiety disorder and GAD were the most frequent co-morbidities in our study and had the highest prevalence in prior studies too.16,21 Increased risk of developing ADHD and mood disorders in people with SP were also described. Many studies have shown the risk of developing other psychiatric comorbidities in individuals affected by a particular mental disorder.33,34 The underlying mechanisms are not clear but shared pathophysiological pathways including neuro-inflammation may somewhat explain this association. 35
Strengths
This study is the first nationwide epidemiological survey assessing psychiatric disorders among Iranian pediatric population. It was performed by the participation of a large number of children and adolescents from all provinces of Iran and results of this study can be generalized to the whole pediatric population in Iran. Using the worldwide accepted data gathering methods such as face-to-face household interview and semi-structured questionnaire (K-SADS) makes the results of this study more valuable and comparable.
Limitations
There are several limitations regarding interpretation of findings. The IRCAP study population did not include the children and adolescents in hospitals or prisons. The method of this study was cross-sectional which does not allow us to determine the casuality. Other major limitations of this study include lack of a control group and follow-up period. Because SP diagnosis is not a subjective assessment, the findings of our study were based on the participants’ reports which may lead to information bias.
Future directions
Nationwide prospective cohort studies can provide a great amount of information about this underestimated mental disorder in pediatric population. The exact pathophysiology of SP has remained unknown and there has not been a significant effective treatment for this condition. Determining the co-morbid mental disorders and socio-demographic characteristics of individuals with SP can have clinical implications.
Conclusions
The findings of our study reveal that SP is an important mental health issue among children and adolescents, which can be detectable early in life. Determining the co-morbid conditions and other demographic associations of SP can lead to a better understanding of the pathophysiology and underlying brain mechanisms of the development of SP.
Declarations
List of abbreviations
ADHD: attention deficit hyperactive disorder; CIDI: Composite International Diagnostic Interview; GAD: generalized anxiety disorder; IRCAP: Iranian children and adolescents psychiatry; K-SADS-PL: kiddie schedule for affective disorders and schizophrenia for school-age children/present and lifetime version; NIMAD: National Institute for Medical Research Development; OR: odds ratio; SD: standard deviation; SP: specific phobia.
Supplemental Material
sj-pdf-1-psy-10.1177_11795573211070537 – Supplemental Material for The Lifetime Prevalence, Risk Factors, and Co-Morbidities of Specific Phobia Among Pediatric Population: A Cross-Sectional National Survey
Supplemental Material, sj-pdf-1-psy-10.1177_11795573211070537 for The Lifetime Prevalence, Risk Factors, and Co-Morbidities of Specific Phobia Among Pediatric Population: A Cross-Sectional National Survey by Mona salehi, Man Amanat, Ali Khaleghi, Zahra Hooshyari, Seyed Ali Mostafavi, Nastaran Ahmadi, Seyed Kaveh Hojjat, Parvin Safavi and Mohammadreza Mohammadi in Clinical Medicine Insights: Psychiatry
Footnotes
Acknowledgments
We are very grateful to all parents and participants for partaking in this study.
Authors’ contributions
MRM: conception and design of the study and revising the manuscript critically for important intellectual content; MA: conception and design of study, drafting the manuscript, and revising the manuscript critically for important intellectual content; AK: acquisition of data and analysis and/or interpretation of data; ZH: acquisition of data and analysis and/or interpretation of data; SAM: analysis and/or interpretation of data; NA: acquisition of data; SKH: analysis and/or interpretation of data; and PS: acquisition of data. MS: conception and design of study and drafting the manuscript. All authors have read and approved the manuscript.
Declaration of conflicting interests
The authors declare that they have no competing interests.
Funding
This work was supported by the National Institute for Medical Research and Development (grant number 940906), who had no role in study design, data collection, analysis, or interpretation of data, in the writing of the report, or in the decision to submit the article for publication.
Ethics approval and consent to participate
The ethics committee of the National Institute for Medical Research Development approved the final protocol (Number: IR.NIMAD.REC.1395.001). The parents provided written informed consent before initiation of the study. The consent was also obtained from all adolescents aged above 15 years and the assent was achieved from all children who participated. The achieved data about children and their parents remained confidential.
Consent for publication
Consent for publication was obtained from all parents and children.
Availability of data and materials
All data generated or analyzed during this study are included in this published article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
