Abstract
Background:
Despite the association of insulin resistance (IR) in the pathophysiology of Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD), few studies have evaluated the utility of acanthosis nigricans (AN) as a clinical predictor for this condition. Thus, we aimed to determine the role of AN as a risk factor and clinical predictor of MASLD.
Methods:
This cross-sectional study conducted a comprehensive clinical history and physical examination. The presence of acanthosis nigricans was assessed in the neck, elbows, axillae, and knuckles. Liver biochemical parameters were measured, hepatic fat was analyzed using the controlled attenuation parameter (CAP), while hepatic stiffness was evaluated in kilopascals (kPA) with the FibrosScan 530 Compact and Smart Exam software. Multiple analyses were performed to determine the relationship between acanthosis nigricans and MASLD.
Results:
We recruited 251 adult participants. The mean BMI was 29.9 ± 7.3 kg/m2, including 40.2% of participants with obesity and 63.7% with AN. Transient elastography evaluation resulted in 65.7% and 6% participants with hepatic steatosis (S3, 48.6%) and fibrosis, respectively. A non-adjusted (OR 2.63, 95% CI 1.57-4.52) and adjusted model (OR 1.97, 95% CI 0.95-4.12) were determined for AN as a risk factor for liver steatosis. Furthermore, the presence of AN in knuckles resulted in an association to predict liver steatosis (OR 2.09, 95% CI 1.01-4.35), while a multivariate analysis indicated that AN predicts a higher steatosis grade (S2 OR = 6.58, CI 95% 1.18-36.53; S3 OR = 2.36, CI 95% 1.04-5.3).
Conclusions:
Acanthosis nigricans demonstrated to predict a higher steatosis grade in adults with overweight and obesity. Our study supports the clinical applicability of AN as a screening tool for MASLD to identify high-risk subjects in resource-limited settings. Additional studies are needed to define alternative diagnostic tools for the early identification of metabolic risk factors in populations with specific clinical or demographic characteristics.
Plain language summary
This study investigates the potential of acanthosis nigricans (AN) as a clinical predictor for Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD). Conducted with 251 adult participants, the study assessed the presence of AN and evaluated liver health through biochemical and physical measurements. Results indicated a significant association between AN and higher grades of liver steatosis, particularly in overweight and obese individuals. The study supports the use of AN as a cost-effective screening tool for MASLD in resource-limited settings, though further research is recommended to explore additional diagnostic methods. This research is significant because it evaluates the role of acanthosis nigricans (AN) as a clinical predictor for Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD), a prevalent condition linked to obesity and insulin resistance. Understanding the association between AN and MASLD can enhance early detection and intervention strategies, especially in resource-limited clinical settings where advanced diagnostic tools may not be available. The study’s findings highlight the potential of using AN as a simple, non-invasive screening tool to identify individuals at high risk for MASLD, which could lead to timely management and better health outcomes. The study emphasizes the need for further research to develop alternative diagnostic tools tailored to populations with specific clinical or demographic characteristics, such as the Latin American population, where the prevalence of overweight, and obesity is rising.
Introduction
Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) is the most common cause of chronic hepatic disease worldwide, characterized by the accumulation of fat in the liver that may progress to inflammation and, eventually, cirrhosis.1,2 MASLD has been associated with type 2 diabetes (T2D) and metabolic syndrome components, such as obesity, hypertension, and dyslipidemia. 3 MASLD prevalence is around 25% in the adult population, 2 while in Mexico, it has been estimated at 14.3% using different screening methods. 4 However, subjects with T2D and obesity exhibit a MASLD prevalence of up to 60% and 80%. 2
Insulin resistance (IR) has been previously associated with the development of MASLD, preceding the clinical expression of a broad spectrum of metabolic disturbances.3,5,6 Particularly, acanthosis nigricans (AN) is a well-known clinical sign of IR.7,8
Acanthosis nigricans (AN) is a useful clinical screening tool for early stages of IR in populations with and without normal body mass index.9,10 Previously, Uwaifo et al 11 reported a low prevalence of AN (14%) in 28 biopsy-proven nonalcoholic steatohepatitis patients. Also, participants with AN had worse insulin resistance than those without AN, as determined by HOMA-IR and QUICKI surrogates. Additional studies in several populations, using different imaging methods, and assessing AN in multiple sites have addressed the utility of AN as a potential MASLD/Metabolic dysfunction-associated steatohepatitis (MASH) clinical marker.12,13
Despite the association of IR in the pathophysiology of MASLD, few studies have evaluated the utility of AN as a clinical predictor of this condition. In this cross-sectional study, we aimed to assess the prevalence of MASLD in adults with and without AN. Additionally, we conducted an exploratory analysis to assess the potential role of AN as a risk factor and clinical predictor of liver steatosis, as determined by transient elastography.
Methods
Design, Setting, and Participants
Approval from our University Institutional Review Board and Ethics Committee was obtained before recruitment and data collection (EN23-00010, 10-Feb-2023). From February 2023 to February 2024, we enrolled adult outpatients attending the Endocrinology Division at “Dr. Jose E. Gonzalez” University Hospital in Monterrey, Nuevo Leon, Mexico. Eligible participants were individuals aged 18 years or older, with or without AN, and who consented to participate. Exclusion criteria included the intake of insulin sensitivity modifying drugs, personal history of hepatic disease, self-reported daily alcohol consumption exceeding >20 g for women, and >30 g for men 14 or refusal to participate.
Study Protocol and Measurements
After obtaining informed consent, a comprehensive clinical history and a complete physical examination were obtained as well as close-up photographs of the neck, elbows, axillae, and knuckles areas for AN assessment. Qualified physicians performed clinical AN evaluation. A Cohen’s kappa index greater than 0.7 was calculated to estimate the chance-adjusted level of agreement before the formal AN assessment. Height and weight were measured in meters and kilograms using a calibrated stadiometer (Seca 700). Body mass index (BMI) was calculated by dividing the weight by the squared height, and patients were classified as normal, overweight, and obese according to the WHO BMI categories. 15 Systolic (SBP) and diastolic (DBP) blood pressure measurements were taken twice using a digital sphygmomanometer (TRU, VSM MedTech Devices Inc., 30, Coquitlam, Canada) and the mean values were recorded. Participants were asked to arrive with at least an 8-hour overnight fast for blood testing. We performed biochemical analysis of alanine aminotransferase (ALT), aspartate aminotransferase (AST), and gamma-glutamyl transferase (GGT) through enzymatic kinetic methodology in the UniCel DxC 800 chemistry analyzer (Beckman Colter, USA). Finally, we evaluated the presence and severity of hepatic steatosis and fibrosis by transient elastography using the FibroScan 530 Compact (Echosens, France) and Smart Exam software (Echosens, France). The probe size (M or XL) was selected according to the software recommendations. The degree of hepatic steatosis was determined through the Controlled Attenuation Parameter (CAP) score and classified as S0 (no steatosis, ⩽248 dB/m), S1 (mild, 249-268 dB/m), S2 (moderate, 269-280 dB/m), and S3 (severe, ⩾280 dB/m), while liver stiffness measured was used for fibrosis staging as F0 (no fibrosis, 1.5-6.5 kPa), F1 (mild, 6.6-7.2 kPa), F2 (moderate, 7.2-9.6 kPa), F3 (severe, 9.7-14.5 kPa), and F4 (cirrhosis, >14.5 kPa).16,17
Statistical Analysis
The sample size for the primary outcome was estimated using a mean comparison formula (90% power, 95% confidence) based on the probable difference in transient elastography results (fatty liver, 2 dB/m; liver stiffness, 1 kPa) between groups with and without acanthosis, resulting in a minimum sample of 84 participants per group. In addition, a proportion method was used to calculate the sample size (power, 97.5%; confidence, 95%; prevalence, 0.3) for the prevalence secondary outcome, requiring 236 subjects. According to their distribution, numerical variables were expressed as means and standard deviations or median and interquartile range (IQR). Categorical variables were expressed as frequencies. Normality of distribution of continuous variables was tested using the Kolmogorov-Smirnov test. Normally distributed continuous variables were contrasted through Student’s t-test, whereas non-normally distributed ones were contrasted using Mann-Whitney’s U test. Unadjusted odds ratios (OR) with 95% confidence intervals were calculated to determine the strength of association of the variables with MASLD qualitatively and quantitatively. A logistic regression model was applied for multivariate analysis to determine the independent association of included covariates with MASLD. Covariates were selected based on their clinical relevance and statistical significance in the bivariate analysis. Assessment of the relationship of each covariate with the degree of hepatic steatosis was made through a multinomial regression model. Statistical analysis was performed using SPSS version 25.0 (IBM Corp. Armonk, NY). A P-value threshold <.05 was considered statistically significant.
Results
Demographic Characteristics
We recruited and evaluated 251 participants (females, 63.3%) aged 19 to 77 years (
General characteristics of the population.

Abbreviations: BMI, body mass index; CAP controlled attenuation parameter; IQR, interquartile range; kPa, kilopascal; SD, standard deviation.
The phototype was documented using the Fitzpatrick classification.
Characteristics of Participants With Acanthosis Nigricans
Participants with AN 160 (63.7%) had a mean age of 39.3 ± 13.3 versus 40.5 ± 16.2 years in those without AN (P = .53). Around 60% of the study population without AN was overweight or obese compared to 80% in the AN group. The AN group presented a higher CAP score at the Fibroscan test than the control group without AN (282.8 ± 58.1 vs 247.6 ± 58.6 dB/m, P < .001). Liver steatosis was more prevalent and significantly different (P < .001) in the AN group (n = 118, 73.8%) when compared to the group without AN (n = 47, 51.6%). Severe steatosis (S3 > 30% hepatocytes) was the most frequent (n = 122, 58%) steatosis grade in the AN group. Contrarily, we did not find a statistical difference between groups in liver stiffness related to fibrosis. Overall, the remaining characteristics are described in Table 2.
Comparison between acanthosis nigricans groups.

Abbreviations: BMI, body mass index; IQR, interquartile range; SD, standard deviation.
Patients were included in the acanthosis group independently from the site of presentation. Comparisons between continuous variables were performed with the Student’s t or Mann-Whitney’s U tests; categorical variables were compared with the X2 test.
Associated Characteristics With Fatty Liver
A logistic regression was performed to evaluate the association between AN and liver steatosis (Table 3). A non-adjusted model revealed that AN at any site was a risk factor for liver steatosis (OR 2.63, 95% CI 1.57-4.52). Nevertheless, when covariates were adjusted (body mass index, age, and waist), the significant association was not maintained (OR 1.97, (95% CI 0.95-4.12). The adjusted model resulted in an R2 Nagelkerke of .544. The subanalysis of an adjusted model focused on assessing the presence of AN in knuckles to predict liver steatosis resulted in a significant association (OR 2.09, 95% CI 1.01-4.35). The adjusted model resulted in an R2 of Nagelkerke of .546 (Table 4).
Association for acanthosis nigricans in any site and knuckles to address association with hepatic steatosis.

R2 Nagelkerke = .544.
R2=.546.
P = .033.
Association of AN with steatosis grades by multinomial regression.

R2 Nagelkerke = .522. The reference class is S0.
P < .027. **P = .025.
Additionally, we conducted a multinomial regression to assess the association of AN with specific steatosis grades using S0 as a reference (Table 4). Multivariate analysis indicated that AN predicts a higher steatosis grade (S2 OR = 6.58, CI 95% 1.18-36.53; S3 OR = 2.36, CI 95% 1.04-5.3).
Biochemical Analysis Between Groups of Hepatic Steatosis and AN
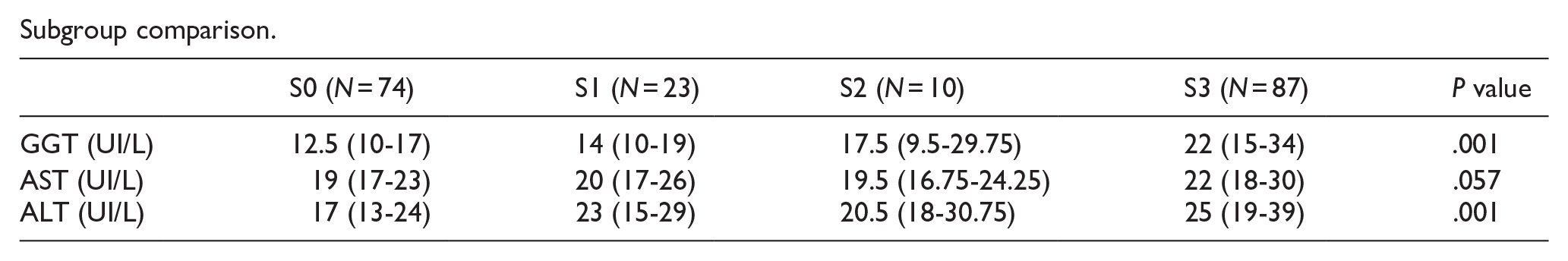
A Kruskal-Wallis H test was performed to determine statistical differences in the biochemical liver profile (AST, ALT, and GGT) between liver steatosis and groups with and without AN. We obtained biochemical results within normal parameter values. Liver S3 steatosis grade had higher values within normal ranges (P < .001). No differences were found between AN groups (Table 5).
Biochemical analysis between groups of hepatic steatosis and acanthosis nigricans.

Abbreviations: ALT, alanine transaminasel; AST, aspartate transaminase; GGT, gamma-glutamyltransferase;.
Values are expressed in median and interquartile range IQR.
P < .05.
Subgroup comparison.
Discussion
Main Findings
As a well-known and recognized dermatological sign linked to IR and obesity, AN may have potential utility as a screening clinical tool in MASLD.11,13 In this cross-sectional study, we found a general AN prevalence of 63%, derived from clinical evaluation of the neck, elbows, axillae, and knuckles. Severe liver steatosis (S3, 58%; CAP ⩾280 dB/m) was observed in 72% of the participants. Our main findings indicate that the presence of AN in knuckles predicts liver steatosis with a significant association (OR 2.09, 95% CI 1.01-4.35, R2 Nagelkerke .546, P < .05), while multivariate analysis (multinomial regression) indicated that AN predicts a higher steatosis grade S2 and S3. In agreement with previous evidence,7,8 AN in the knuckles was highly prevalent and seems to be a very early clinical sign of insulin resistance before occurrence in other classical sites, arising a caution of compensatory hyperinsulinemia. The observed size effect may have been influenced by our sample size, especially in subgroup analyses. The resulting confidence intervals might be used to suspect a possible overestimation effect based on the observational study design.
Interestingly, we found a higher prevalence of liver steatosis compared to that previously reported. 2 In turn, the high AN prevalence between 25% and 75% was in agreement with similar studies previously conducted in subjects with obesity; however, our population was mainly comprised of subjects who were overweight and obese. Notably, the prevalence of overweight and obesity in the Mexican population reported by the National Health and Nutrition Survey (ENSANUT 2018-19) was 75%, which mirrors what was observed in this study. 18 As an insulin resistance clinical feature, AN has been reported to have a wide range and variable prevalence depending on population characteristics, such as ethnicity, age, skin phototype, obesity, and diabetes. Therefore, the present findings may not be applicable to groups with different clinical or demographic characteristics.
Comparison With Previous Evidence
In 2006, Uwaifo et al 11 suggested a limited screening utility of AN in a small cohort of patients with NASH demonstrated by biopsy. They determined AN presence by physical examination of the nape od of the neck and axillae. Acanthosis nigricans was found in 4 out of 28 participants, having a sensitivity of 80% and a negative predictive value of 29% for NASH detection. Interestingly, when comparing AN cases versus controls without AN, authors identified a subpopulation of patients with NASH significantly more obese and hyperinsulinemic. Thus, AN presence would indicate a higher metabolic risk.
In counterpart, nonalcoholic fatty liver disease (NAFLD) was associated with AN on a bivariate (OR 11.7, 95% CI 9.19-14.9, P < .001) and multivariate (OR 6.12, 95% CI 4.7-7.98, P < .001) analysis performed in adults from an urban area in Sri Lanka. 19 Although the evaluated sample was large (n = 2985), NAFLD was diagnosed by ultrasound and no further details about AN assessment were provided. Nonalcoholic fatty liver disease was found in 31.6% of the men and 37.5% of the women who were investigated (general prevalence, 32.6%). In our study, AN at any site had an adjusted OR of 1.98 (95% CI 0.948-4.118); when confounders were adjusted, the significant association was not maintained. Therefore, further evaluation of specific subgroups of patients is needed to clarify AN use as a screening tool for MASLD.
A case-control study on type 2 diabetes patients proposed AN as a potential clinical marker for liver fat and stiffness. 13 Acanthosis nigricans and liver span (OR 1.8, 95% CI 0.9-3.5, P = .09), liver steatosis (CAP, OR 7.5, 95% CI 0.9-61.1, P = .05), and fibrosis (kPa, OR 2.5, 95% CI 1.5-4.06, P = .001) showed a significant association when using an adjusted multivariable logistic regression model. However, AN evaluation was restricted to the neck area, surrogate markers of IR were not assessed, and results yielded a limited diagnostic accuracy. Similarly, a cross-sectional study in Mexican adolescents with obesity claimed a correlation between AN and mild liver steatosis. 20 Around 65% of the participants exhibited AN, at least in 2 areas. Nevertheless, a small sample was evaluated (n = 61), liver steatosis was assessed by ultrasound, and knuckles and IR biochemical markers were not included. Thus, this independent association between the presence of AN and hepatic steatosis and fibrosis might remain debatable and could be specific to exclusive subgroups of patients with clinical or demographic characteristics partially defined.
The prevalence of AN is also affected by ethnicity, age, and skin phototype. The more common Fitzpatrick phototypes in our population were 3 and 4, raising the expected prevalence compared to other types. This suggests that an ethnic predisposition to AN development is more frequent in the Hispanic and African population. 8
Levels of the liver enzymes have been reported to be both non-significant and significantly different. ALT, AST, and GGT were similar between AN (+) and AN (−) subjects, according to Uwaifo et al. 11 Similarly, we did not observe differences in biochemical parameters between AN groups. However, participants with S3 and fibrosis had slightly higher values in AST, ALT, and GGT. Oppositely, high ALT was significant (OR 2.28, 95% CI 1.32-3.94, P = .003) in a logistic regression model of factors associated with NAFLD. Significant differences in liver function tests between patients with and without AN were also found by Dutta et al 13 in a more recent study.
Limitations and Strengths
We acknowledge the limitations of the present work. Our sample was mainly composed of overweight and obese adults; however, ENSANUT 2018-19 reported a prevalence of 75% in the Mexican population, which is represented correctly. Also, we did not measure surrogate markers of IR, such as HOMA-IR. Those surrogates were not considered since 2 previous studies in our group have demonstrated higher HOMA-IR and insulin levels in AN cases.7,10 However, insulin- and non-insulin-based surrogates of insulin resistance would highlight the mechanistic relation of AN in the context of MASLD. As a strength, we demonstrated the presence of steatosis and fibrosis by transient elastography, the current recommended non-invasive imaging procedure for liver evaluation.
Conclusion
Acanthosis nigricans was useful to predict liver steatosis, particularly higher and severe grades, in adults with overweight and obesity. Thus, our results support the clinical applicability of AN as a screening tool for MASLD in resource-limited settings. Additional studies are needed to define alternative diagnostic tools for the early identification of high-risk subjects with specific clinical or demographic characteristics, especially in the Latin American population, where overweight, and obesity are a rising challenge.
Footnotes
Acknowledgements
The authors wish to thank Susana Chávez Moreno, MD, for her support in the English edition of this manuscript.
Ethical Considerations
This study was approved by the Institutional Research Ethics Committee (Facultad de Medicina, Universidad Autonoma de Nuevo León-UANL) with the registration number EN23-00010.
Consent to Participate
Prior to enrollment, all participants provided written informed consent. The research was conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Consent for Publication
Not applicable.
Author Contributions
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated and analyzed during the current study are available from the corresponding author upon reasonable request.
