Abstract
Background:
The use of ChatGPT and artificial intelligence (AI) in the management of metabolic and endocrine disorders presents both significant opportunities and notable risks.
Objectives:
To investigate the benefits and risks associated with the application of ChatGPT in managing diabetes and metabolic illnesses by exploring the perspectives of endocrinologists and diabetologists.
Methods and materials:
The study employed a qualitative research approach. A semi-structured in-depth interview guide was developed. A convenience sample of 25 endocrinologists and diabetologists was enrolled and interviewed. All interviews were audiotaped and verbatim transcribed; then, thematic analysis was used to determine the themes in the data.
Results:
The findings of the thematic analysis resulted in 19 codes and 9 major themes regarding the benefits of implementing AI and ChatGPT in managing diabetes and metabolic illnesses. Moreover, the extracted risks of implementing AI and ChatGPT in managing diabetes and metabolic illnesses were categorized into 7 themes and 14 codes. The benefits of heightened diagnostic precision, tailored treatment, and efficient resource utilization have potential to improve patient results. Concurrently, the identification of potential challenges, such as data security concerns and the need for AI that can be explained, enables stakeholders to proactively tackle these issues.
Conclusions:
Regulatory frameworks must evolve to keep pace with the rapid adoption of AI in healthcare. Sustained attention to ethical considerations, including obtaining patient consent, safeguarding data privacy, ensuring accountability, and promoting fairness, remains critical. Despite its potential impact on the human aspect of healthcare, AI will remain an integral component of patient-centered care. Striking a balance between AI-assisted decision-making and human expertise is essential to uphold trust and provide comprehensive patient care.
Plain Language Summary
Regulatory frameworks must evolve to keep pace with the rapid adoption of AI in healthcare. Sustained attention to ethical considerations, including obtaining patient consent, safeguarding data privacy, ensuring accountability, and promoting fairness, remains critical. Despite its potential impact on the human aspect of healthcare, AI will remain an integral component of patient-centered care. The use of ChatGPT in the management of metabolic and endocrine disorders presents both significant opportunities and notable risks. The benefits of heightened diagnostic precision, tailored treatment, and efficient resource utilization have potential to improve patient results. Concurrently, the identification of potential challenges, such as data security concerns and the need for AI that can be explained, enables stakeholders to proactively tackle these issues. Regulatory frameworks must evolve to keep pace with the rapid adoption of AI in healthcare. Sustained attention to ethical considerations, including obtaining patient consent, safeguarding data privacy, ensuring accountability, and promoting fairness, remains critical. Despite its potential impact on the human aspect of healthcare, AI will remain an integral component of patient-centered care. Striking a balance between AI-assisted decision-making and human expertise is essential to uphold trust and provide comprehensive patient care.
Introduction
Diabetes and metabolic illnesses constitute a global health challenge of unprecedented magnitude, affecting millions of individuals worldwide and placing a significant burden on healthcare systems.1 -5 These conditions, characterized by disrupted glucose metabolism and impaired metabolic processes, encompass a spectrum of disorders including type 1 and type 2 diabetes and metabolic syndrome.6,7 The prevalence of diabetic conditions has reached epidemic levels, driven by factors such as sedentary lifestyles, unhealthy diets, and genetic predisposition.8 -10 As a result, the management of diabetes and metabolic illnesses has become increasingly complex, demanding innovative approaches, ongoing patient education, and rigorous monitoring to mitigate the risk of complications.11 -13
The landscape of healthcare is rapidly evolving, driven by the transformative potential of artificial intelligence (AI).14,15 AI, with its ability to process vast amounts of data, recognize patterns, and generate insights, has paved the way for more efficient and precise healthcare delivery.8,9,16 Among the emerging applications of AI, ChatGPT stands out as a promising tool in healthcare communication. ChatGPT, a sophisticated conversational agent, employs natural language processing (NLP) to engage in meaningful conversations with users, simulating human interaction. 17
The journey toward the creation of ChatGPT began with the debut of OpenAI’s GPT-1 in 2018, a groundbreaking moment that demonstrated the potential of training large-scale language models and laid the groundwork for future developments. Although GPT-2, released in 2019, performed better than GPT-1, it arrived with restricted access due to its improved capabilities and the ethical considerations it raised. A landmark moment came in 2020 with the release of GPT-3, a colossal model boasting 175 billion parameters, which marked an unprecedented leap forward. This release opened the way for a vast array of natural language tasks to be carried out and set new standards in the field.
Following this, OpenAI introduced ChatGPT, a model specifically tailored for conversational interfaces that continuously evolves through iterative updates based on user feedback. This progression not only underscores the rapid advancements that have been made in language comprehension and generation capabilities, but also brings to the fore the ethical implications of the development of such sophisticated AI models. This ongoing development journey reflects the dynamic and evolving nature of AI and its increasing impact on various facets of technology and society.
Technology has demonstrated remarkable capabilities to address information gaps, enhancing patient–provider communication and providing valuable insights into complex conditions. It thus has promise for supporting diabetes diagnosis and care.
Patient engagement and education are essential for the successful management of chronic diseases, such as diabetes and metabolic illnesses. 18 The multifaceted nature of these conditions requires a comprehensive approach that augments traditional medical intervention with deep data analysis and an understanding of individual patient needs. 17 Effective self-management, lifestyle modifications, medication adherence, and regular monitoring are crucial components of managing diabetes and metabolic illnesses; however, medical professionals have found that achieving patient engagement is challenging because patients struggle to maintain the constant attention needed to manage their conditions. 19
ChatGPT has shown promise in closing this gap by harnessing the power of AI. 20 Technology offers a novel approach to patient engagement and education, and ChatGPT is particularly promising due to the interactive and conversational nature of the technology. 1 It provides a unique opportunity to deliver tailored, on-demand education and support directly to patients in ways they can understand and identify with. 2 Individuals with diabetes and metabolic illnesses are therefore empowered to make informed decisions, adopt healthier lifestyles, and adhere to prescribed treatments.
Implementing ChatGPT in the management of diabetes and metabolic illnesses can provide personalized education that adapts to each patient’s learning style, pace, and level of understanding .21 -23 Through ongoing conversations, AI agents identify gaps in patient knowledge, dispel myths, and reinforce key disease management concepts, enhancing patients’ health literacy and empowering them to actively participate in their care.24,25 Moreover, the continuous availability of ChatGPT facilitates real-time support, allowing patients to receive immediate responses to queries, concerns, and doubts. 19 This support is effective in minimizing the anxiety and uncertainty that can be associated with managing chronic conditions. Real-time interaction with ChatGPT also has the potential to improve medication adherence, as the program can send reminders and address medication-related questions. 24
As ChatGPT can serve as a virtual companion to patients on their journey toward improved health, this study seeks to investigate the benefits and risks associated with using it in managing diabetes and metabolic illnesses, where its use presents both significant opportunities and notable risks. Specifically, we examine the perspectives of endocrinologists and diabetologists in primary and secondary healthcare systems on applying ChatGPT in their practice, including potential concerns and limitations related to its use. An examination of these benefits and challenges reveals a multifaceted scenario that warrants careful consideration, thoughtful planning, and responsible execution.
Methods and Materials
Study design
The study was carried out between February 6th and August 28th 2023 and employed a qualitative research approach. 26 This design was chosen as its adaptability and capacity for in-depth analysis contributes to a deeper understanding of participants’ experiences and opinions.27,28 Additionally, the method helps to generate diverse perspectives on how people view the issue at hand, and qualitative techniques aid in identifying gaps that might be overlooked in survey-based research.28,29 Figure 1 presents the flow chart of the study methodology.

Flow chart of study methodology.
Study setting
The study considered endocrinologists and diabetologists working as government or privately employed consultants and specialists in the primary and secondary healthcare systems of the United Arab Emirates.
Participant inclusion and exclusion criteria
The study population comprised all endocrinologists and diabetologists with at least 3 months of experience registered with the Ministry of Health and Prevention (MOHAP), Health Authority Abu Dhabi (HAAD), or Dubai Health Authority (DHA). Individuals who were not willing to participate in the study, had recently joined these organizations, or were in the probationary period were excluded.
Development of a research tool and interview guide
The study employed a dual-component research tool. The first section comprised 4 demographic questions about the participants’ gender, years of experience, and areas of specialization and the nature of their employing organization. The second section was a semi-structured interview guide based on a comprehensive literature analysis.9,14,16,17 This guide encompassed five critical questions aimed at exploring the benefits and risks of utilizing AI, particularly ChatGPT, in the management and treatment of diabetes and other metabolic disorders. Details of these questions are available in the Supplemental Materials section for reference. To assess the content validity of the guide, we engaged a panel of experts comprising two experienced endocrinologists, two diabetologists, and three academics at Ajman University. Their expertise was instrumental in ensuring that the questions were comprehensive, relevant, and aligned with the study’s objectives. Additionally, we conducted a pilot study with a subset of the target demographic to evaluate the clarity, comprehensibility, and effectiveness of the interview guide in eliciting meaningful responses. Feedback from this pilot phase led to refinements, enhancing the guide’s overall robustness and reliability. This thorough validation process significantly improved the quality and validity of our qualitative research methodology and was crucial in capturing the complex perspectives of healthcare professionals in the field, thereby enriching the depth and authenticity of our findings.
Sampling techniques and participant recruitment
Endocrinologists and diabetologists were purposefully selected using the convenience sample technique. 30 We targeted diabetologists and endocrinologists from diverse practice environments and levels of expertise. Direct outreach was conducted through medical associations, professional circles, and healthcare institutions. Prospective participants were presented with a detailed overview of the study’s objectives, the voluntary nature of their involvement, and assurances of confidentiality. Subsequently, potential participants were screened for suitability based on their professional background and relevant expertise. Interested individuals were provided with an extensive information document outlining the study’s purpose, the interview process, and their rights as participants. Informed written consent was obtained from each participant prior to commencing the interviews. This recruitment approach aimed to ensure a broad representation from the endocrinology and diabetology community, thereby enriching the qualitative data with a wide array of insights and perspectives.
Interviewer characteristics
To maintain consistency and mitigate potential biases due to varying interviewer characteristics, all interviews were conducted by a single experienced researcher. This interviewer, a male specialist in a specific area (ie, endocrinology), has a background in conducting qualitative interviews. The decision to use a single interviewer was strategic, aiming to standardize the data collection process. It is important to acknowledge that the interviewer’s gender might influence participant responses, and we used a uniform interview approach to minimize any gender-related biases in our study. Specifically, the interviewer rigorously followed a predefined interview protocol, ensuring that each participant was asked identical questions in a consistent manner. Limiting the potential effects of interviewer-specific factors on participant responses in this manner enhanced the overall reliability of the collected data.
Interview transcription and data collection and processing
Recruitment commenced at various private and governmental hospitals in different regions to ensure a diverse sample with varied practice characteristics and personal traits. The lead researcher, who has experience conducting in-depth interviews, conducted the interviews primarily at the participants’ places of employment and at a time and location convenient for them. An iterative interviewing method was used to explore new questions and responses that emerged from earlier interviews. Sampling continued until data saturation, when no fresh questions or subjects were found in 2 consecutive interviews.
The interviews were conducted in English, the national language of instruction, to facilitate communication with graduates of endocrinology and diabetes medicine. Each interview lasted between 30 and 40 minutes, and when necessary, respondents were questioned appropriately to elicit essential information, with additional field notes taken. The first and corresponding author, AAJ, transcribed the interviews, ensuring strict adherence to the ethical standards set by the Ajman University Ethical Committee, particularly concerning the privacy and security of the data. To enhance the credibility and accuracy of the qualitative data, participants were offered the opportunity to review and validate their interview transcripts. Each participant received a consent form clearly detailing the review’s purpose accompanied by a copy of their respective transcribed interview. Participants were encouraged to scrutinize the transcripts for precision and suggest any necessary clarifications or amendments. Confidentiality was stringently upheld, participation in the review process was completely optional, and not all participants chose to engage in it. This step was crucial for upholding the integrity of the data collection process and addressing potential discrepancies or misunderstandings. The research team remained dedicated to transparency and active participant engagement throughout the study.
Data saturation was reached after the twentieth interview, but an additional 5 interviews were conducted to check for the emergence of any new themes. The decision to conduct additional interviews was driven by the objective of ensuring comprehensive coverage of subjects and viewpoints. Initially, the plan was to conclude the interviews once a specific threshold had been met. However, the research team recognized that to capture a diverse array of insights, a more thorough exploration was essential. By extending the interview process, we aimed to enhance the transparency and depth of our research methodology, providing a richer and more detailed understanding of the diverse perspectives and topics within our study. This approach underscores our commitment to a thorough and inclusive research process, aimed at capturing the full spectrum of relevant insights. Data analysis involved line-by-line transcripts focusing on pertinent topics and content. Two researchers (AAJ and SSA) independently coded the transcripts, with the study’s co-authors comparing the coding and coming to an agreement.
Theoretical framework and data analysis
The interpretivist paradigm, which is based on social constructivism and phenomenology, is the basis for this qualitative investigation. This phenomenology provides a philosophical framework for examining people’s subjective experiences. Using this methodology, the study explores endocrinologists’ and diabetologists’ opinions, attitudes, and thoughts about ChatGPT to extract the essence of their interactions with the platform.
Moreover, in order to understand the social context in which endocrinologists and diabetologists engage with ChatGPT, social constructivism is used. This framework emphasizes the significance of social context in forming people’s understanding and experiences by acknowledging that knowledge and meaning are co-constructed through social interactions.
Braun and Clarke’s (2006) 31 6-phase thematic analysis framework guided the methodological approach for data analysis in this study (Figure 2). This renowned procedure facilitates the identification, examination, and reporting of patterns, or themes, within qualitative data. The framework aligns with the exploratory nature of the study and the iterative process of theme analysis, allowing for patterns to naturally emerge from the data and ensuring that the analysis remains open and free from preconceived notions. By adopting this approach, the research benefits from a structured yet flexible method that respects the data’s complexity and nuances.

Braun and Clarke’ 6-phase thematic analysis framework.
Robustness and reliability of the study
Our research adopted a comprehensive, multifaceted approach to enhance its reliability. Emphasizing methodological transparency, we have detailed our study design, data-gathering methods, and analysis techniques to promote both transparency and reproducibility. The research team engaged in continuous reflexivity throughout the study to identify and mitigate any potential biases. We employed purposeful sampling to ensure a diverse range of perspectives among participants, thereby giving the qualitative data with greater richness and depth. Moreover, we gave participants the opportunity to review and confirm their interview transcripts, further enhancing the validity of our results. Uniformity in data collection was achieved by entrusting all interviews to a single, experienced researcher, thereby minimizing possible biases. Rigorous adherence to informed consent protocols was maintained, and professional transcription standards were utilized to ensure both the accuracy and confidentiality of the data. Thematic analysis was systematically applied to identify and interpret patterns within the data. Collectively, these robust measures contribute significantly to the reliability, credibility, and trustworthiness of our research findings.
Results
Demographics of the study subjects (n = 25)
Table 1 presents the demographic information of the participants. A total of 25 endocrinologists and diabetologists were interviewed in this study. The average age of participants was 38 ± 2 SD, and 60% (n = 15) were male and 40% (n = 10) were female. Endocrinologists constituted 64% of the sample, and 36% were diabetologists. Participants’ years of experience were as follows: 5 (20%) less than 1 year, 8 (32%) 1 to 5 years, 7 (28%) 6 to 10 years, and 5 (20%) more than 10 years. Of the total, 52% were from public and 48% from private hospitals (Table 1).
Demographics of the participants (n = 25).

Thematic analysis
Benefits of implementing ChatGPT in diabetes and metabolic illnesses
The findings of the thematic analysis resulted in 19 codes and 9 major themes regarding the benefits of implementing ChatGPT in managing diabetes and metabolic illnesses (Table 2).
Major themes and codes of benefits of Implementing AI Chat-GPT in diabetes and metabolic illnesses.

Improved diagnostic precision
The majority of endocrinologists and diabetologists emphasized the importance of implementing ChatGPT in managing diabetes and metabolic illnesses in terms of detection at an early stage, bespoke treatment, and efficient detection of anomalies.
Individualized treatment programs
All the endocrinologists and diabetologists focused on the issue that applying ChatGPT in managing diabetes and metabolic illnesses could help in forming individualized treatment programs. Patient-specific interventions and tailored therapeutic recommendations were the most commonly identified approaches for individualized treatment programs.
Effective triage and screening
Another significant application of ChatGPT in managing diabetes and metabolic illnesses is effective triage and screening. Most of the participating endocrinologists and some of the diabetologists reported that triage efficiency and optimized workflows were key elements of effective triage and screening.
Decisions based on objective data
The majority of endocrinologists and diabetologists indicated the importance of implementing ChatGPT in decisions based on objective data in managing diabetes and metabolic illnesses. Data-driven treatment and adherence to standards were the most important reported measures for ChatGPT implementation in this area.
Prognostications
Disease development mapping and analysis of treatment response were the most common applications reported by participants that aid in prognostications of diabetes and metabolic illnesses.
Workflow improvement
The automation of key tasks and system integration were the factors most identified as assisting in workflow improvement in managing diabetes and metabolic illnesses.
Development and research
Many of the endocrinologists and diabetologists reported that ChatGPT could be applied in development and research on diabetes and metabolic illnesses. This theme included medical literature analysis and medication development.
Patient support and education
A further benefit of implementing ChatGPT in managing diabetes and metabolic illnesses is that it aids patient support and education, in particular, through the AI-driven Chatbot, as well as adherence to medical protocols.
Cost efficiency
The majority of participants reported cost savings as an important application of ChatGPT in managing diabetes and metabolic illnesses. Cost savings approaches consist of optimization of resources and resource allocation.
Risks of implementing ChatGPT in managing diabetes and metabolic illnesses
The extracted risks of implementing ChatGPT in managing diabetes and metabolic illnesses were categorized into 7 themes and 14 codes (Table 3).
Major themes and codes of risks of implementing AI Chat-GPT in diabetes and metabolic illnesses.
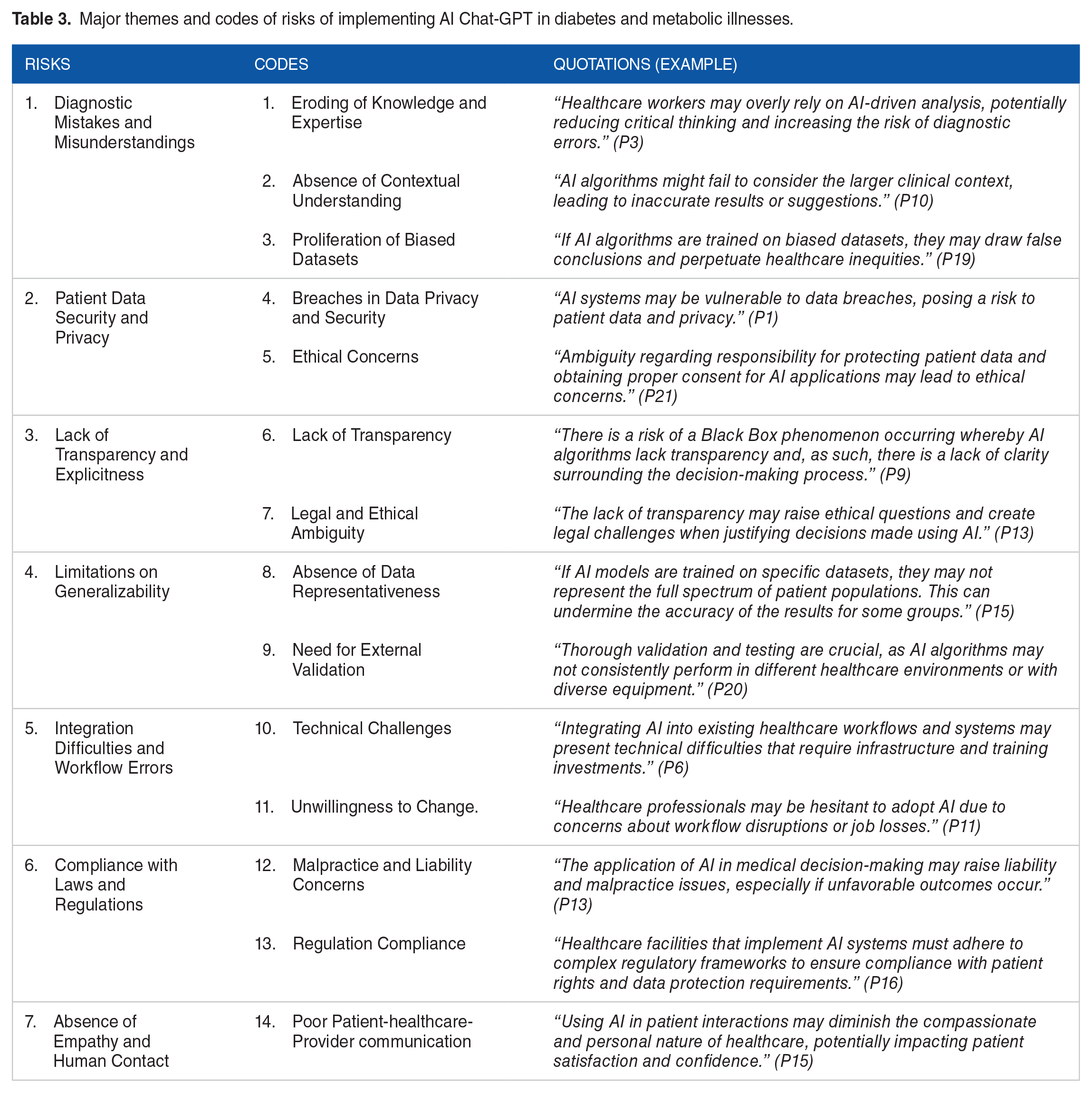
Diagnostic mistakes and misunderstandings
Endocrinologists and diabetologists believed that diagnostic mistakes and misunderstandings are among the important risks of using ChatGPT in managing diabetes and metabolic illnesses. This risk was defined in 3 ways: eroding of knowledge and expertise, absence of contextual understanding, and proliferation of biased datasets.
Patient data security and privacy
All groups of endocrinologists and diabetologists reported that breaches to patient data security and privacy are a major risk of using ChatGPT in managing diabetes and metabolic illnesses. Breaches in data privacy and security and ethical concerns were the most important reported factors in this theme.
Lack of transparency and explicitness
Lack of transparency and explicitness is another risk of ChatGPT application in managing diabetes and metabolic illnesses. This theme included lack of transparency and legal and ethical ambiguity.
Limitations on generalizability
All the participants agreed that lack of generalizability is another disadvantage of using ChatGPT in managing diabetes and metabolic illnesses. This theme was explained by the absence of data representativeness and the need for external validation.
Integration difficulties and workflow errors
Integration difficulties and workflow errors are further disadvantages reported by endocrinologists and diabetologists. The majority of the participants believed that technical challenges and unwillingness to change were important factors hindering the integration of ChatGPT application in the management of diabetes and metabolic illnesses.
Compliance with laws and regulations
All the participants reported that potential failure to comply with laws and regulations is a major risk factor for ChatGPT application in managing diabetes and metabolic illnesses. This theme is explained by 2 factors: malpractice and liability concerns and regulation compliance.
Absence of empathy and human contact
All the endocrinologists and diabetologists reported that poor patient–healthcare-provider communication is a considerable challenge for them in using ChatGPT in managing diabetes and metabolic illnesses.
Discussion
Our investigation of the use of ChatGPT in diabetes and metabolic illness management has revealed a landscape of both promising prospects and substantial impediments. The findings of this study clearly demonstrate that AI can offer tailored advice and improve patient involvement and adherence to therapeutic regimens. The recent algorithmic progress shown by Andellini et al’s empirical validation 32 demonstrated noteworthy potential in discerning glycemic episodes among pediatric Type 1 diabetes patients. The ability to offer tailored care enables healthcare personnel to undertake the necessary interventions in timely fashion, thus reducing the likelihood of complications. Moreover, Nashwan demonstrated that AI can considerably change the management of cardiometabolic pathologies, including diabetes. 33 Incorporating AI into the management of illnesses increases the precision of diagnoses and patient prognoses and fine-tunes treatments. Nonetheless, the study also reveals possible risks, including fears about data confidentiality, undue reliance on technology, and the possibility that an application will incorrectly recommend treatments. Similar concerns highlighted by Robinson et al 34 show the importance of scrutinizing AI-driven healthcare interventions and underscore that human vigilance remains indispensable.
Comparing the findings of the present study with extant research reveals some incongruities. The study accentuated ChatGPT’s potential to enhance patient engagement; however, some studies have found that certain applications do not have this outcome. For instance, Andellini et al’s study 32 centered on non-invasive glycemic event detection, a specialized domain in which patient involvement may be limited. This disparity in findings underscores the assorted uses of AI within diabetes management according to algorithmic variances, patient demographics, and the specific nature of interventions. It is crucial to grasp these divergences if we are to understand the complexity of AI’s influence on diabetes management and guide future research. To mitigate these disparities, future studies should seek to normalize AI algorithms, ensure data privacy, and integrate human oversight to mitigate errors. Cooperative research involving healthcare providers, technologists, and policymakers can lead to a more resilient and ethical AI implementation in managing diabetes and metabolic illnesses. Such an implementation can leverage the insights gleaned from Robinson et al’s observations 34 on decoding patients’ information needs and ensuring transparent communication.
The findings of this study have important implications for shaping the trajectory of diabetes and metabolic illness management. By spotlighting AI’s potential for tailored care, patient engagement, and precision therapies, the study reveals novel pathways for healthcare providers to improve treatment outcomes, fostering innovation in clinical practice and driving further exploration and assimilation of AI-led interventions. At the same time, identified risks, such as concerns about data privacy and the need for human supervision, underline the need for responsible practice. These insights steer standardized practices, ethical directives, and collaborative efforts involving technologists, healthcare providers, and policymakers. 35 The study shows how AI can be integrated into healthcare, advocating a balanced strategy that accounts for both the considerable potential benefits as well as the undeniable risks. By giving a detailed account of AI’s applications and constraints in diabetes management, it offers invaluable insights to steer future research, mold policy, and guide technological advances in medicine. As a foundational reference, it guides researchers, practitioners, and policymakers, thus paving the way for a more effective, ethical, and patient-centric deployment of AI in healthcare.
The current study revealed that across various medical domains, AI has substantial potential for positive impact: its capacity to enhance diagnostic accuracy, tailor treatment strategies, streamline workflows, and facilitate evidence-based decision-making could usher in a transformative era of patient care. By enabling early detection, personalized interventions, and predictions of disease progression, AI empowers healthcare professionals to make well-informed choices, resulting in swifter treatments and improved patient outcomes. Moreover, AI’s effectiveness in screening and prioritization could alleviate the workload of radiologists while enhancing patient care quality.
AI can also expedite drug discovery, identify emerging therapies, and aid medical literature analysis in research and development, fostering innovation and broadening medical knowledge. Moreover, cost savings could be made due to its potential to enhance patient care and healthcare system efficiency by supporting patient education, offering assistance, and optimizing resource allocation.
However, the integration of AI comes with considerable risks. Diagnostic errors arising from excessive reliance on AI, inadequate contextual understanding, and biased data can impede accurate diagnoses and patient safety. Concerns related to patient privacy and data security emerged due to potential data breaches and uncertainties surrounding data ownership and consent.
The opacity and lack of transparency in certain AI algorithms raise ethical and legal questions that might undermine trust in AI-driven decisions and contravene established medical norms. Furthermore, the inadequate representation of diverse patient populations or inconsistent behavior in various contexts could lead to healthcare disparities through limited AI applications.
Integrating AI could cause obstacles and potential disruptions in workflows. Thus, achieving a smooth and successful AI implementation requires effective communication, education, and collaboration, particularly given healthcare professionals’ apprehensions about change and job displacement. The insights drawn from this thematic analysis have profound implications for the future of healthcare. The ongoing advancement of AI technology is likely to continue influencing medical practices, diagnostic approaches, and patient management. Current limitations, such as lack of transparency and constrained applicability, will be addressed through enhancements in AI algorithms, techniques for clarity, and strategies for data representation.
Regulatory frameworks must evolve to keep pace with the rapid adoption of AI in healthcare. Sustained attention to ethical considerations, including obtaining patient consent, safeguarding data privacy, ensuring accountability, and promoting fairness, remains critical. Despite its potential impact on the human aspect of healthcare, AI will remain an integral component of patient-centered care. Striking a balance between AI-assisted decision-making and human expertise is essential to uphold trust and provide comprehensive patient care.
While our study provides valuable insights into the perspectives of endocrinologists and diabetologists on the potential use of ChatGPT in managing diabetes and metabolic illnesses, it is important to acknowledge certain limitations. Firstly, although our participant selection aimed for diversity, it may not fully represent the broader spectrum of opinions within the wider medical community. Additionally, the reliance on self-reported data introduces the possibility of recall bias. The use of a single interviewer, while ensuring consistency, could also introduce an element of interviewer bias. Moreover, perceptions of AI applications are subject to rapid change due to the evolving nature of technology and healthcare practices. Lastly, the qualitative nature of our study limits the generalizability of our findings beyond the specific context we explored. Despite these challenges, our research provides critical insights into the ongoing advancement of AI in healthcare and establishes a foundation for future investigations in this field.
Conclusion
In conclusion, this thematic analysis, derived from qualitative research, investigates the advantages and drawbacks of applying AI, specifically, ChatGPT, and sheds light on both its transformative promise and the risks it presents in the management of metabolic disorders. This investigation is fundamental in comprehending the intricate interplay between technological advancement and patient well-being. With the healthcare landscape in constant flux, the insights gleaned from this study can guide the responsible integration of AI.
The benefits of heightened diagnostic precision, tailored treatment, and efficient resource utilization hold the potential for improved patient results. At the same time, the identification of potential challenges, such as data security worries and the need for AI that can be explained, enables stakeholders to proactively tackle these issues.
The possibility of future repercussions underlines the need for collaboration among healthcare practitioners, AI experts, regulatory bodies, and patients. By embracing innovation while upholding ethical standards, safeguarding patient confidentiality, and staying true to the fundamental principles of empathetic care, the healthcare sector can leverage the potential of AI to redefine medical practices while retaining its dedication to patient welfare.
Supplemental Material
sj-docx-1-end-10.1177_11795514241235514 – Supplemental material for Benefit–Risk Assessment of ChatGPT Applications in the Field of Diabetes and Metabolic Illnesses: A Qualitative Study
Supplemental material, sj-docx-1-end-10.1177_11795514241235514 for Benefit–Risk Assessment of ChatGPT Applications in the Field of Diabetes and Metabolic Illnesses: A Qualitative Study by Ammar Abdulrahman Jairoun, Sabaa Saleh Al-Hemyari, Moyad Shahwan, Tariq Al-Qirim and Monzer Shahwan in Clinical Medicine Insights: Endocrinology and Diabetes
Footnotes
Acknowledgements
We would like to thank our colleagues for their participation in this study and their support of our work in this way; they helped us obtain results of better quality.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
