Abstract
Thyroid storm is a rare, potentially lethal condition involving collapse of the hypothalamic-pituitary-thyroid feedback loop. Thyroid storm carries a significant mortality rate, thus requiring prompt identification and treatment. A 47-year-old woman presented to the emergency department complaining of palpitations, shortness of breath, and emesis for 24 hours after using methamphetamine. Past medical history was significant for untreated hyperthyroidism. Physical examination revealed a prominent, palpable thyroid. The Burch-Wartofsky-Score was 35. Management for thyroid storm included propylthiouracil (PTU), super saturated potassium iodide, intravenous hydrocortisone, and propranolol. However, a rare drug reaction to PTU on day 3 resulted in agranulocytosis. Propylthiouracil was withheld and a modified total thyroidectomy performed on day 8 without complications and the patient discharged on day 10 with levothyroxine. Undertreated hyperthyroidism may predispose patients to catecholamine-induced thyrotoxicosis due to catecholamine hypersensitivity. With known methamphetamine use, methamphetamine toxicity and a methamphetamine-exacerbated thyroid storm need to be included in the differential diagnosis in a patient presenting with signs of thyrotoxicosis. In addition, treating patients with agranulocytosis from PTU with a modified total thyroidectomy using ligation of the vascular supply as the initial surgical step limits release of thyroid hormone into the blood stream during thyroidectomy and decreases the possibility of intra operative thyroid storm.
Introduction
Thyroid storm, defined as temperature greater than 40°C, tachycardia, extreme hypertension, agitation, and diarrhea, is a rare, potentially lethal condition involving collapse of the negative feedback loop that regulates excessive thyroid hormone release. Hyperthyroid disorders are often not well defined by standard clinical signs and symptoms and are further complicated by overlapping presenting symptoms such as anxiety, sepsis, and high cardiac output states. 1 They often exist along a spectrum that includes the mildest form of hyperthyroidic, progressing to thyrotoxicosis, and then finally to the most severe form thyroid storm. Thyroid storm may develop in patients with long-standing untreated hyperthyroidism; however, it may also occur following an acute event such as surgery, trauma, myocardial infarction, pulmonary thromboembolism, and severe infection. 2
Patients typically present with an exaggeration of the usual symptoms of hyperthyroidism including tachycardia, hyperpyrexia, tremor, agitation, delirium, psychosis, stupor, coma, and diarrhea. 3 The Burch-Wartofsky-Score (Table 1) is used to assess the probability of thyrotoxicosis and it is solely based on clinical and physical criteria.
Burch-Wartofsky-Score.
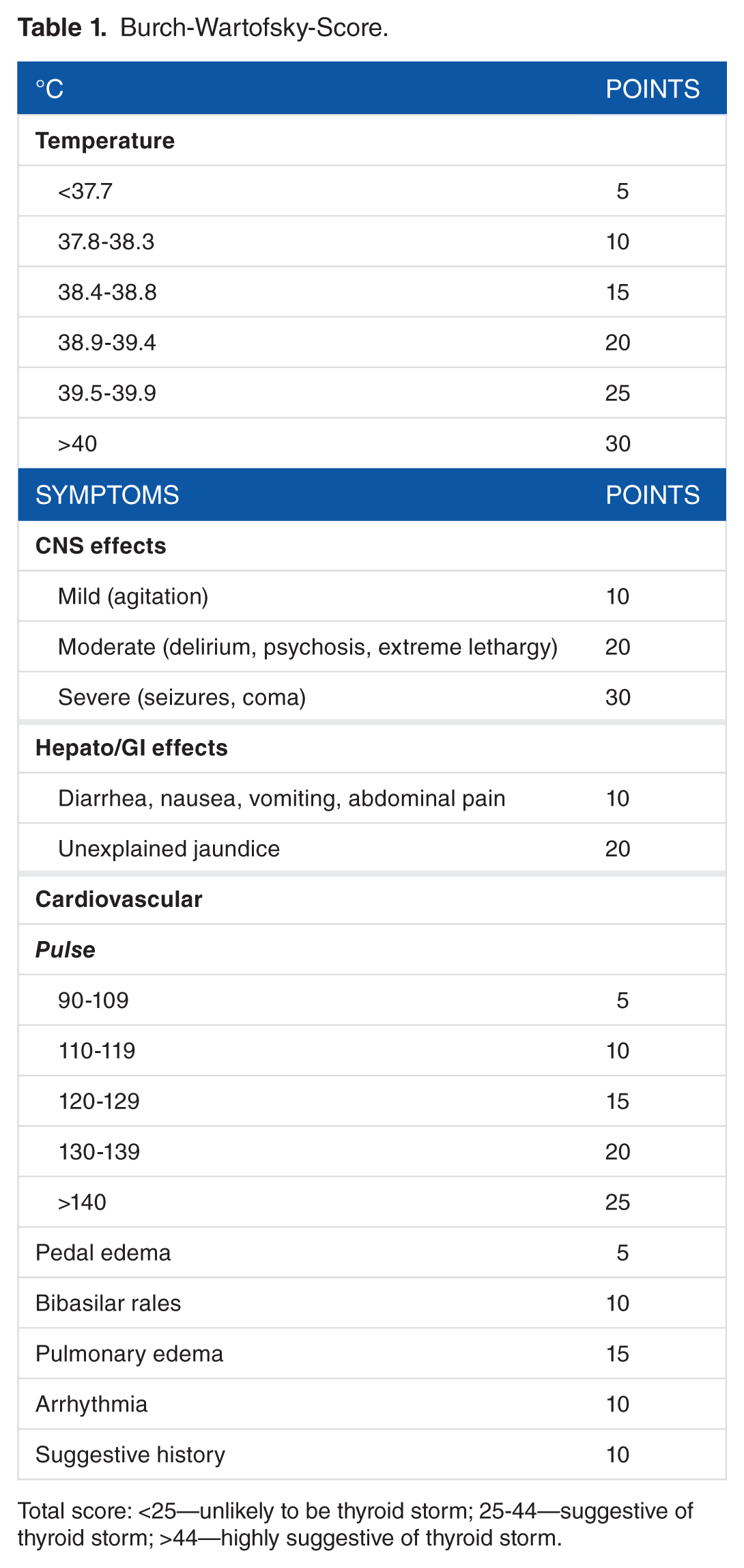
Total score: <25—unlikely to be thyroid storm; 25-44—suggestive of thyroid storm; >44—highly suggestive of thyroid storm.
This Burt-Wortofsky scoring is partially subjective and is to be used only as a guide. It is, however, helpful for initial assessment and treatment while awaiting thyroid function test results. 3 Thyroid function tests during thyroid storm may reveal suppressed thyroid-stimulating hormone (TSH) and elevated free T4 and T3 at levels comparable with those seen in uncomplicated overt hyperthyroidism. 4 Therefore, collectively, social history, focused physical exam, Burch-Wartofsky-Score, and thyroid function tests are crucial for thyroid storm diagnosis.
Case Description
A 47-year-old woman presented to the emergency department with tachycardia, shortness of breath, nausea and vomiting, and cardiac palpitations for 24 hours. Her past medical history was significant for untreated hyperthyroidism. The patient reported methamphetamine use for the first time the day before, which coincided with the onset of her symptoms. Her vital signs showed a heart rate of 123, blood pressure of 120/67, temperature of 36.4°C, and a respiratory rate of 20. On physical examination, the patient was actively emetic but compliant and nontremulous. There was a prominent, palpable thyroid (5.5 cm transversely) and distended neck veins with a carotid bruit.
At the time of admission, the abnormal lab results showed a TSH < 0.004 μU/mL (normal: 0.350-4.940), total T3 = 3.49 ng/dL (normal: 0.58-1.59), free T4 = 4.47 ng/dL (normal: 0.70-1.48), cortisol level = 24.7 μg/dL (normal: 3.0-23.0), K = 2.8, and a normal white blood cell (WBC) count of 7.4. Urinary drug screen was positive for methamphetamine. The Burch-Wartofsky-Score was 35. The patient was admitted and treated for suspected thyroid storm with propranolol 40 mg orally every 6 hours, propylthiouracil (PTU) 200 mg orally every 4 hours, super saturated potassium iodide (SSKI) 5 drops orally every 6 hours, and Solu-Cortef 100 mg intravenous every 8 hours.
On hospital day 3, she was noted to have a WBC count of 1.8. The agranulocytosis was thought to be caused by PTU which was immediately discontinued. The patient was placed on neutropenic precautions. A decision was made to surgically remove the thyroid to control her hyperthyroidism. The anesthesiologist was advised of the patients’ course and risk of anesthesia or surgery exacerbating her condition so appropriate precautions could be made. A modified thyroidectomy was performed on day 8 when the vital signs, electrolytes, and WBC had normalized. The surgical technique was modified in that the vascular pedicles of the thyroid gland were ligated before dissection and removal of the thyroid gland (Figure 1).There were no perioperative complications. The thyroid pathology revealed hyperplastic features with a small atypical follicular focus (negative for HBME-1 immunostain) and a benign parathyroid gland. The patient was subsequently discharged on levothyroxine on day 10 with a WBC count of 6.4 and in stable condition.
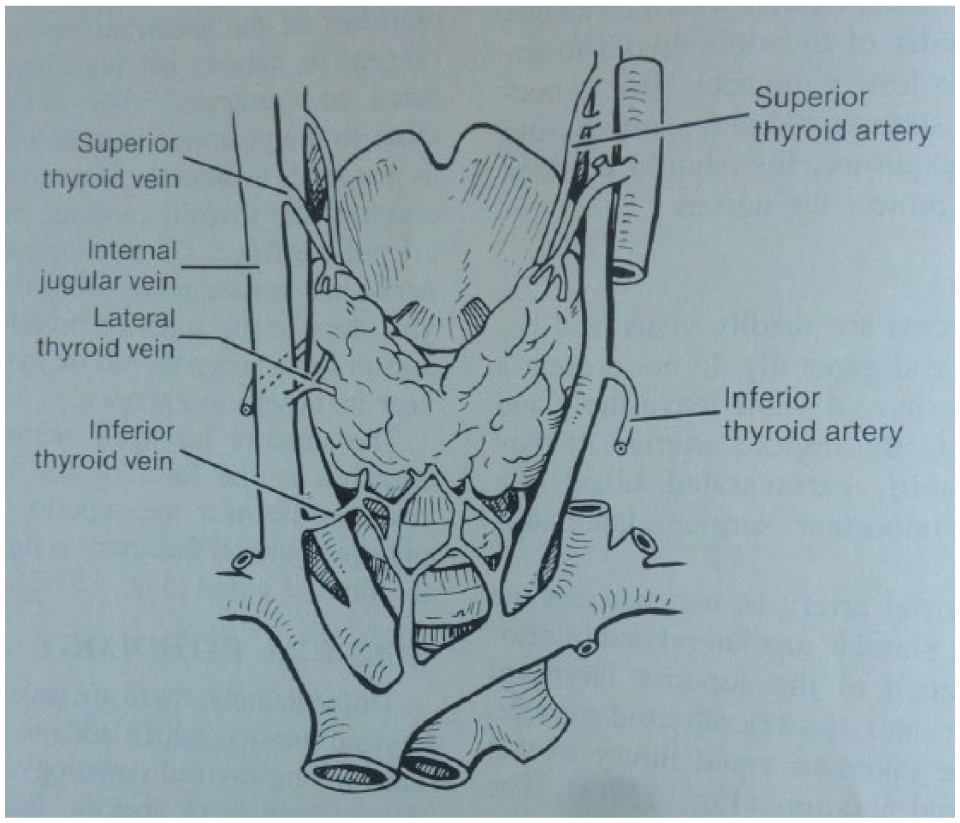
Venous drainage of thyroid.
Discussion
Thyroid storm is a well-described exacerbation of thyrotoxicosis and most patients are stabilized with medical management before considering surgical intervention. The use of methamphetamine in relation to the onset symptoms of thyroid storm is a unique aspect of this case and may identify methamphetamine as a culprit for triggering and/or exacerbating thyroid storm. This case also illustrates the importance of communication between the medical and surgical team in discussing the correct management, both medically and surgically, for complex thyroid storm.
Methamphetamine is a popular recreational drug that may be considered a potential “trigger” for thyroid storm. The prevalence of methamphetamine use is 5% in the US population, with an estimated incidence of 500 000 people using the drug in a given month. 5 This illicit drug belongs in the class of compounds known as phenethylamines, which act as sympathomimetic amines with a variety of stimulant, euphoric, and central nervous system effects that may mimic thyrotoxicosis.
When methamphetamine is ingested, the drug incorporates into cytoplasmic vesicles where it displaces catecholaminergic neurotransmitters such as epinephrine, norepinephrine, and dopamine into the cytosol. As cytosolic concentrations rise, the surplus of neurotransmitters becomes available for release. 6 Methamphetamine acts to indirectly induce the release of these catecholamines from presynaptic terminals into the synaptic cleft where they bind and activate postsynaptic receptors leading to adrenergic stimulation. Concomitantly, the drug acts to inactivate reuptake of these catecholamines, producing continuous activation of the adrenergic system. 6 This excessive adrenergic stimulation may potentiate a thyroid storm.
In addition to the catecholaminergic effects of methamphetamine, the use of methamphetamine has been shown to increase circulating free TSH as well as cause an exaggerated response to thyrotropin-releasing hormone in the presence of elevated free T4. 7 Methamphetamine use has also been shown to directly increase levels of T4. 8 Abstinence from methamphetamine use, conversely, leads to decreased T3 and TSH levels in those who have abused methamphetamine. 8 The patient in this case admitted to using methamphetamine for the first time before the onset of the symptoms; therefore, it is likely the catecholamine surge acted to acutely increase free T4 levels which aided the progression into thyroid storm. Methamphetamine-induced thyroid storm should also be included in the differential diagnosis for a patient presenting with typical symptoms of thyrotoxicosis.
Over time, an elevated level of free T4, as seen in hyperthyroidism, has been shown to increase the effects of catecholamines that manifest as exaggerated hyperadrenergic responses. 9 Therefore, it is possible in this case that the patient’s untreated hyperthyroidism lead to higher baseline levels of free T4 which contributed to the development of a hypersensitivity to catecholamines. This baseline hypersensitivity may have been further provoked by methamphetamine use, triggering succession into thyroid storm. Generally, a multimodal treatment approach is recommended in patients with thyroid storm, including β-blockade, antithyroid therapy, inorganic iodide, corticosteroid therapy, aggressive cooling with acetaminophen and cooling blankets, volume resuscitation, respiratory support, and intensive care unit monitoring according to the American Thyroid Association and the American Association of Clinical Endocrinologists Guidelines. 10
The classic antithyroid medications (ATMs) used are PTU and methimazole, and both are generally safe to use in the setting of thyrotoxicosis. The use of antithyroid drugs, although relatively safe, is not without potential side effects. The common adverse effects of PTU include pruritus, rash, urticaria, arthralgia, arthritis, fever, abnormal taste sensation, nausea, or vomiting, which are seen in up to 13% of patients. 11 A more rare but serious complication of thionamide therapy is agranulocytosis which has a prevalence of 0.1% to 0.5%, is dose-independent, and usually occurs between 2 weeks and first 2 months after beginning treatment. 12 Our patient experienced agranulocytosis to PTU after a short course of treatment (day 3). Patients who have experienced even minor side effects of an ATM experience an increased incidence of agranulocytosis when another ATM is restarted. 13 The exact cause of ATM-induced agranulocytosis is unclear but may involve an immune mediated mechanism directed against mature blood cells or their precursors. 14
Elective surgery should be postponed until the disease state has been stabilized. Serial monitoring of TSH, T3, and T4 along with the use of a β-blocker, PTU or methimazole, SSKI, and hydrocortisone help control the heart rate and limit conversion of T4 to T3. A thorough airway examination is performed to rule out a goiter which may cause airway difficulty. Hyperthyroid patients are usually volume depleted and vasodilated, so it is important to address the volume status during induction of general anesthesia. All medications, fluids, and equipment that may be needed during the case need to be present before induction as manipulations anytime during the induction or procedure may lead to a sympathetic reflex and/or initiation of thyroid storm. These problems may be prevented or minimized by administering an esmolol infusion along with chilled intravenous fluids.
Because thyroidectomy is itself a risk factor for inducing thyroid storm, preoperative management typically includes administration of PTU, SSKI, and β-blockers. 10 This regimen prevents the release of preformed thyroid hormone during manipulation of the thyroid and decreases the conversion of T4 to T3 in the periphery. An additional benefit of this combination treatment is the therapeutic decrease in blood flow to the thyroid. 15 Often, corticosteroids are co-administered when rapid preparation for emergent surgery is needed. 16 In this case, due to the patient’s agranulocytosis reaction to PTU, the drug could not be continued as preoperative management. Methimazole, also known to induce agranulocytosis, was not used as alternative management. The patient’s preoperative course included β-blocker, SSKI, and intravenous hydrocortisone only.
The thyroidectomy procedure was modified to minimize the continual release of thyroid hormone into the blood stream during dissection. The standard thyroidectomy procedure was revised in that the middle thyroid veins, as well as the superior and inferior thyroid vessels, were ligated initially. The recurrent laryngeal nerve was then identified and protected. The gland was dissected and removed, bluntly freeing the superior and inferior poles, respectively, after ligation. The surgery successfully removed the devascularized thyroid tissue without using PTU or exacerbating adrenergic symptoms during the operation.
Patients with undertreated hyperthyroidism may be at an increased risk for transitioning into thyroid storm with methamphetamine use due to catecholamine hypersensitivity and the release of thyroid hormone. Methamphetamine toxicity and a methamphetamine-exacerbated thyroid storm need to be included in the differential diagnosis in patients with hyperadrenergic symptoms; drug screening is warranted. Consider treating patients with significant reactions to antithyroid medications with a modified total thyroidectomy to prevent extrusion of thyroid hormone into the blood stream during the surgical procedure and allow safer thyroid hormone replacement therapy postoperatively. The medical team should be aware of the advantage of the modified surgical technique and its usefulness in certain situations when consulting a surgeon who is familiar with this particular technique. This may be particularly relevant in smaller hospitals where the thyroid storm is not commonly managed.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
OV, MD: Involved in initial literature search, writing of first draft, editing, revisions, and finalization of final draft.
DCM, MD: Involved in initial literature search, writing of first draft, editing, revisions.
DBH, MD: Involved in initial literature search, writing of first draft, editing, revisions, and finalization of final draft.
