Abstract
Objectives:
The frequency of tinnitus in children and adults is practically the same. However, although adults reveal their symptoms and seek for medical aid, the suffering often remains unrecognized in the young. This is due to both the inability of children to properly describe their symptoms and the lack of recognition.
Materials and methods:
Among 5768 patients entering our department with complaints of tinnitus between 2010 and 2015, there were only 112 children. A full clinical history and medical status had been determined at the time of presentation and were analyzed retrospectively.
Results:
The average duration from first complain to clinical presentation was approximately 12 months. A normal hearing capability of less than 25 dB was measured in 80% of the cases. Only 23 patients presented with a hearing impairment. The causes ranged from hearing loss, previous orthodontic treatment, noise trauma, middle ear aeration, muscular neck tension, and skull base fracture. Typical co-morbidities such as sleeping disorders, concentration disorders, and hyperacusis were observed.
Conclusions:
This retrospective study shows that recognition of tinnitus in the childhood is generally delayed. A better characterization of complaints and triggers, however, is a prerequisite to sensitize medical personnel and caretakers for the suffering and to avoid developmental impairments.
Introduction
In the past few years, a discrepancy has become evident between the occurrence of tinnitus in pediatric patients and its clinical recognition. In general, it is assumed that the prevalence of tinnitus in children is equal to its prevalence in the adult population. 1 Also, the triggers for tinnitus initiation are known to be similar in both groups. Tinnitus can dramatically decrease the quality of life of the affected, resulting in social isolation and, in the worst case, giving rise to psychological disorders such as depression.2,3 Common accompanying morbidities such as sleeping and concentration disorders will affect learning abilities and school grades. It can also lead to symptoms such as headache, dizziness, and vertigo.2–5 Tinnitus often co-occurs with hyperacusis and has also been associated with otitis media.1,6
Of note, even exposure to leisure noise has been identified as a risk factor for childhood tinnitus in various studies. 7 In addition to the problems described, tinnitus in pediatric patients has another dimension because it contributes to impairments of language and communication skills during a critical period of life. The molecular disease mechanism is not clear; however, recent data revealed a cochleopathy as the molecular correlate of the inner ear. This coined the term hidden hearing loss. 8 It is now assumed that tinnitus reflects only the first symptomatic outbreak that, if neglected, may inevitably lead to hearing impairment. 9
Despite the obvious need, there are only few clinical and basic research efforts related to the incidence of tinnitus in the childhood. To date, only one study has thoroughly looked at treatment outcomes for children with tinnitus. 10 Moreover, a retrospective study of underage patients with a primary complaint of tinnitus from 2013 11 came to the conclusion that current epidemiologic data for the prevalence should be interpreted with extreme caution. Obviously, the examiner faces a number of methodological difficulties when studying tinnitus in children. For example, children report to the doctors at a great range of age with even more dramatic differences in development. Their linguistic inability to properly describe the symptoms and reliance on parental report make interpretation of data difficult. Thus, it is not surprising that the reported prevalence varies from 4.7% to 46% in children with normal hearing, 1 although it is more common in children with hearing loss as compared with those with normal hearing. 12
Given the lack of good clinical evidence, there is a need for further research in this field to help clinicians identifying the most effective diagnostic and treatment strategies for children in need. This study tries to overcome this limitation by compiling a reliable set of data characterizing the clinic and etiology of pediatric tinnitus. Briefly, clinical data of 112 children who were referred over a period of 5 years to our institution with complaints of tinnitus were retrospectively analyzed.
Materials and Methods
Data on 5768 patients entering the Department of Otorhinolaryngology—Head and Neck Surgery at the Helsinki University Hospital between 2010 and 2015 with tinnitus complaints were retrospectively analyzed. Among them there were 112 children under the age of 19 years. The cohort consists of 45 girls and 67 boys. All patients had troublesome tinnitus that had led to a referral and consequent visit to our institution.
No segregation of cases was made on the basis of audiometric results or socio-demographic variables. According to Finnish legislation, the study design required no Research Ethics Board approval because the data were collected retrospectively and the study had no impact on ongoing treatment decisions. Institutional research permission was granted. All patients were treated by a team of an ear-nose-throat (ENT) specialist and an audiological assistant and underwent standard audiological examination including tone audiometry for frequencies ranging from 125 to 8.0 kHz.
Results
The age of all children in this series with suspected tinnitus ranged from 6 to 18 (average ± SD: 14.4 ± 2.9) years (Figure 1). They were referred to our department by general practitioners (67%), school nurses and doctors (14%), private ENT doctors (11%), and pediatricians (8%). At our department, all children were interviewed by an experienced ENT specialist.
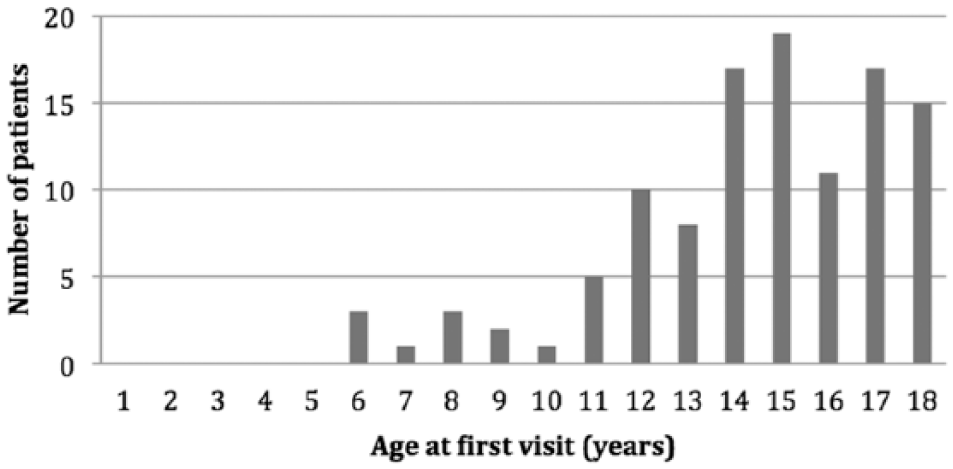
Age distribution of patients at their first presentation.
The tinnitus was classified idiopathic in the absence of a disease-related trigger in the patient’s medical history when presenting with first symptoms. However, 14% had experienced a noise trauma, 12% had a history of middle ear infection, 4% reported a preceding viral infection, 1 patient had an earlier basilar skull fraction, and 16% of the children had undergone orthodontic treatment, another 12% showed muscular neck tension, and 9% showed various psychological disorders (Table 1).
List of suspected main triggers and their distribution (number and percentage) as a causative factor for tinnitus in affected patients.
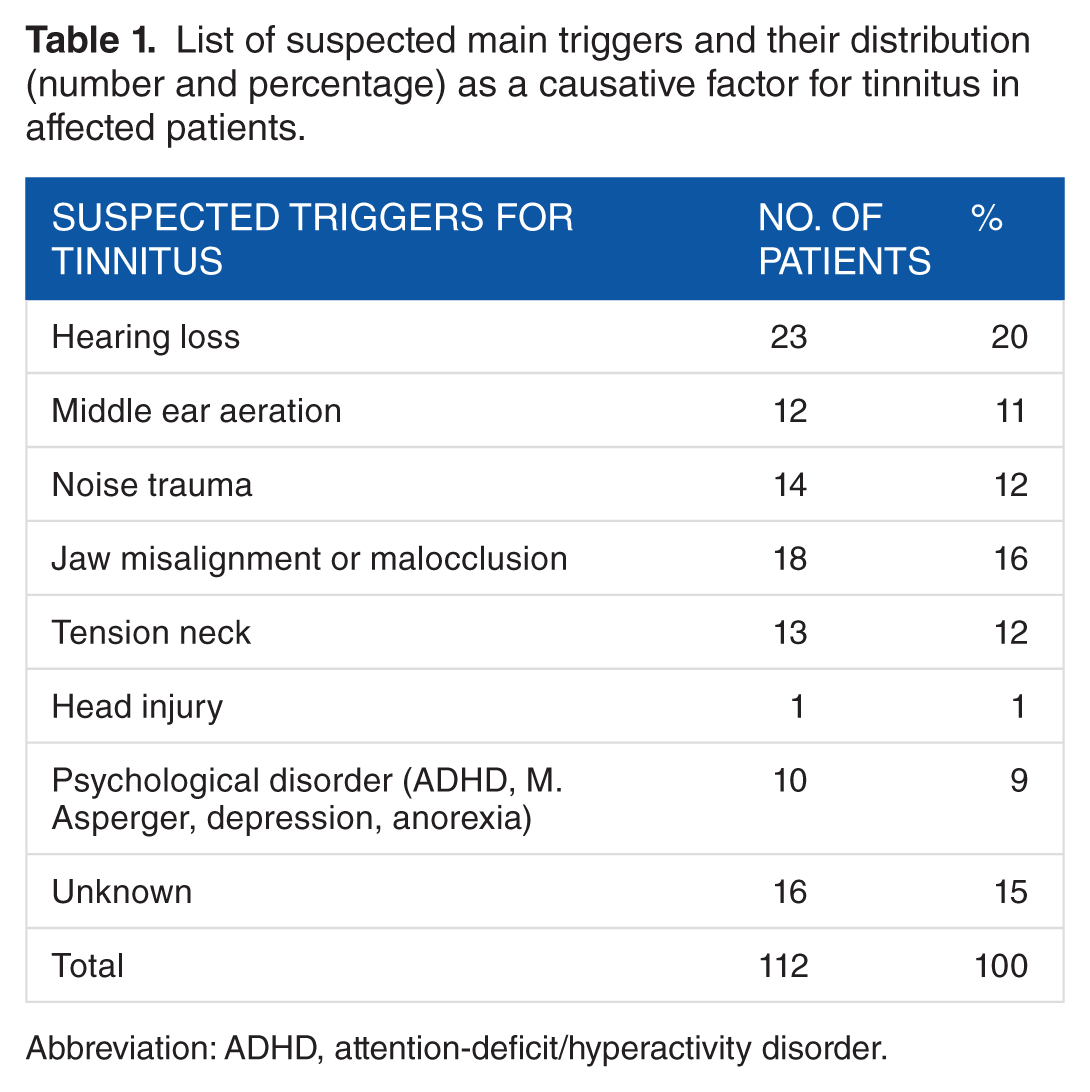
Abbreviation: ADHD, attention-deficit/hyperactivity disorder.
In 58% of the cases, the tinnitus was bilateral, whereas an isolated right-side or left-side involvement was seen in 24% and 18%, respectively. Tinnitus was almost exclusively described as continuous high-frequency tone (96%). Only 5 children reported of a pulsatile quality. A diagnostic magnetic resonance imaging of the brain in these patients revealed no pathologic abnormalities of the vascular pattern.
As part of the clinical evaluation, we measured the hearing capability of all patients by pure-tone audiogram. There are different approaches to define hearing loss. We classified hearing capability as normal if hearing loss was less than 25 dB at one or several frequencies or according to the pure-tone average (80% of all cases). Most importantly, our data show that of the 112 children, only 23 presented with clinically relevant hearing loss. In all, 21 had a sensorineural and 2 had a conductive impairment (Table 2) (20 patients showed unilateral and only 3 bilateral hearing loss).
Hearing capacity measured by pure-tone audiogram at first presentation.
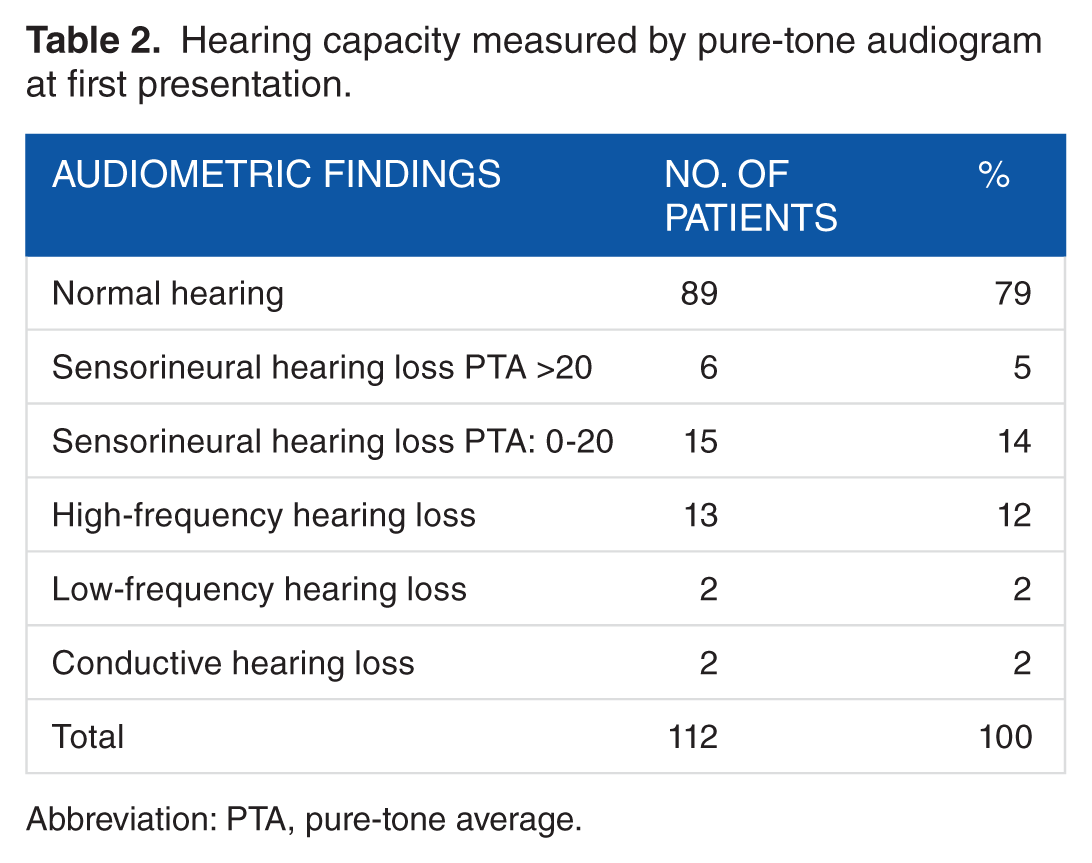
Abbreviation: PTA, pure-tone average.
Because tinnitus and hearing loss have a great impact on the child’s everyday life, we looked for typical co-morbidities (“soft signs”). We observed sleeping disorders in 38%, concentration disorders in 12%, and hyperacusis in 9% of all cases. Of note, children faced a delay of roughly 12 months from first symptoms to presentation in our department (Figure 2). Due to the retrospective analysis of data, the degree of developmental delay cannot be estimated in this study.
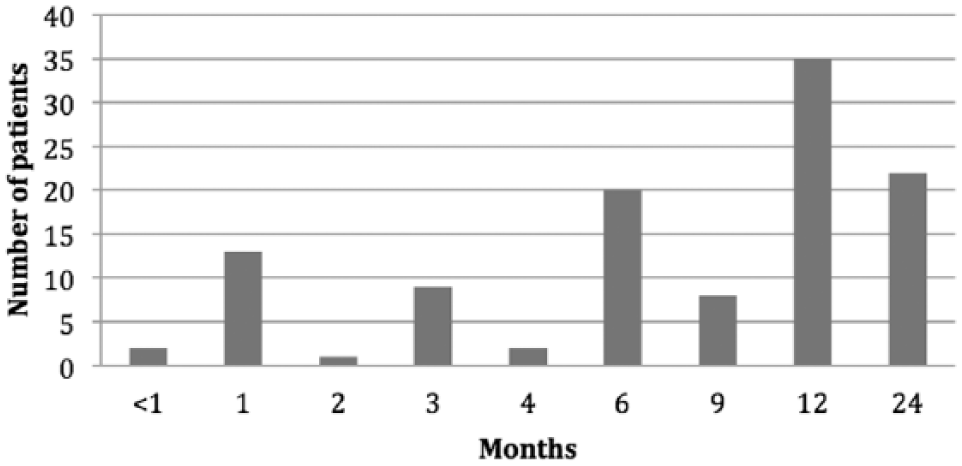
Duration of tinnitus at the time of first presentation.
Discussion
The aim of this study was to compile clinical data that characterize tinnitus in pediatric patients. The need for such data is tremendous because the diagnosis comes often too late with severe consequences far beyond reduction in quality of life. Most dramatic for the affected are developmental impairments and social exclusions. 13 The retrospective design of this study allowed a survey over a period of 5 years. At the same, this depicts its biggest limitation because it restricts all information to the medical records and does not allow follow-up examinations.
The most troublesome finding of this study is its confirmation of pediatric tinnitus as a largely ignored symptom. The time between the first appearance of symptoms and a presentation in our clinic was slightly above 12 months. It seems that children with the first symptoms of tinnitus are diagnosed and treated for too long in local services and referred to a special clinic as last resort. The reason for this unexpected pattern may be that children do not generally report tinnitus spontaneously and their complaints may not be taken seriously enough. 14 It has also been suggested that children consider the presence of the ear noises as normal. This is true especially if they have had it for a long time, or if they are distracted by their environment, for example, when playing with their favorite toys or enjoy other activities that make them forget it. 5
Our data reveal that tinnitus is not necessarily connected to hearing loss and cannot always be related to an initiating trigger. Most children in our study had normal hearing abilities, whereas inversely, the prevalence of tinnitus is up to 46% 15 in children with normal hearing threshold and 62% 12 in children with hearing impairment. Also, in our cohort, a history of middle ear pathology was reported in 12%, which seems not to be a significant factor in the genesis of tinnitus, specifically in children. Moreover, previous studies found no statistical differences between children with or without middle ear pathology.6,16 In contrast, we identified jaw misalignments and malocclusions as the most common trigger, which are treated by orthodontics. The relationship between the 2 is still only partially understood 17 ; however, the prevalence of tinnitus in patients with jaw misalignments and malocclusions ranges up to 76%, 18 which is a much higher rate than that of the general population.
All patients together with their parents were informed about the consequences and long-term prospects related to tinnitus. If possible, the trigger was eradicated or treated, for example, by dental or physiotherapy, or by prescription of a hearing aid device. Furthermore, regular follow-up visits were arranged depending on clinical manifestation. One underestimated trigger for the development of tinnitus is exposure to music specifically in the young population. The need to advise young people to be careful about excessive noise exposure is underlined by the finding that in 14% of the children, noise exposure initiated tinnitus. Leisure-time noise exposure earlier considered playing only a minor role as a health hazard is more and more recognized as a major risk factor. Adolescents and teenagers often expose themselves to loud music and excessive noise levels during social and music events: noise levels between 104 and 112 dB (A) can be measured in nightclubs and discos. 19 A recent study conducted on students at British universities showed that 88% of students experienced tinnitus after leaving a nightclub, and 66% had music-induced hearing disorder in the following morning. It was also reported that the use of hearing protection and knowledge about the risks of loud music were negligible. 20 There is now evidence from noise injury animal models showing that prior noise exposures can exacerbate and accelerate age-related hearing loss (presbycusis) 21 and can cause irreversible neural damages in the absence of elevated hearing thresholds. 22
To better understand similarities and differences between tinnitus in adults and children, it is important to better inform parents, teachers, and medical personnel and increase their awareness of tinnitus as an entity for differential diagnosis. Furthermore, more efforts are needed to encourage the scientific community to recognize this problem and follow it up systematically in tractable disease models. We need a better understanding of why this symptom occurs and how children communicate it. This is achieved by a combination of clinical skills as well as increasing awareness among medical personnel of typical complaints in this population. The young patients must be recognized as early as possible and should undergo a thorough and standardized evaluation. Basic research and clinical research needs to be directed in a coordinated manner to reveal mechanisms and to develop innovative treatment options. Our approach as a starting point for these efforts was to evaluate clinical data on patients with tinnitus to get a better profile of the disorder in this specific patient population.
Conclusions
Tinnitus in the childhood is underdiagnosed, and due to this negligence, proper therapies are unnecessarily delayed. In fact, the symptom can remain unrecognized for long in the young patient population with severe consequences for development of the individual. We propose that any type of pediatric tinnitus should be assessed by specialists to initiate proper diagnostics and treatments at the earliest possible time point and thus to avoid adverse long-term consequences for the young patient such as a delayed mental development. 23
Footnotes
Peer review:
Two peer reviewers contributed to the peer review report. Reviewers’ reports totaled 1171 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was supported by grants from a special governmental subsidy for health sciences research.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
AS, AM, and AA conceived and designed the experiments and jointly developed the structure and arguments for the paper. AS analyzed the data and wrote the first draft of the manuscript. AS, TJ, AM, and AA contributed to the writing of the manuscript; agree with manuscript results and conclusions and made critical revisions and approved final version. All authors reviewed and approved the final manuscript.
Disclosures and Ethics
As a requirement of publication, author(s) have provided to the publisher signed confirmation of compliance with legal and ethical obligations including but not limited to the following: authorship and contributorship, conflicts of interest, privacy and confidentiality, and (where applicable) protection of human and animal research subjects. The authors have read and confirmed their agreement with the ICMJE authorship and conflict of interest criteria. The authors have also confirmed that this article is unique and not under consideration or published in any other publication, and that they have permission from rights holders to reproduce any copyrighted material. Any disclosures are made in this section. The external blind peer reviewers report no conflicts of interest.
