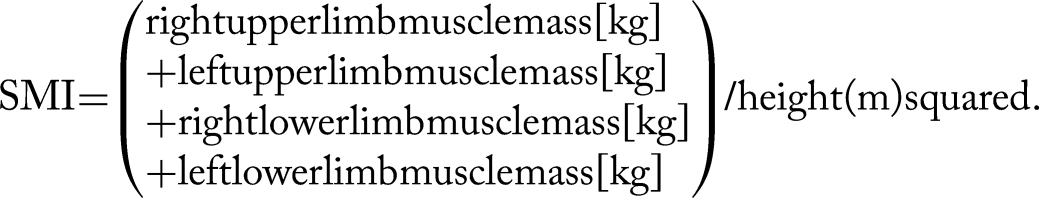Abstract
BACKGROUND
Chronic obstructive pulmonary disease (COPD) is accompanied by dyspnea on exertion due to airflow limitation caused by bronchial stenosis, with afflicted patients being less physically active. Therefore, physical activity is important for disease management.
OBJECTIVES
This study aimed to examine the relationships of walking and non-walking physical activities with cognitive function or physical characteristics of patients with mild COPD in a community without respiratory rehabilitation.
DESIGN
Cross-sectional study.
DATA SOURCES AND METHODS
We included 40 male patients (mean age, 75.7 ± 6.7 years) with stable mild COPD. A three-axis accelerometer was used to evaluate walking and non-walking physical activities in daily life. Cognition, respiratory function, skeletal muscle mass, limb muscle strength, exercise capacity, and health-related quality of life were assessed.
RESULTS
Regarding daily exercise amount (metabolic equivalents × hours; Ex), 87.5% of the participants had walking activities of 0–2 Ex, while 67.5% had non-walking activities of 1–3 Ex. Walking activity was significantly correlated with cognitive function (P < .05), walking distance (P < .01), and health-related quality of life (P < .05), but not with muscle mass. However, non-walking activity was significantly correlated with the body mass index (P < .05), muscle mass (P < .05), and walking distance (P < .01), but not with cognitive function. Moreover, the relationship between non-walking activity and health-related quality of life was weaker than the corresponding relationship with walking activity.
CONCLUSION
In patients with mild COPD, walking and non-walking physical activities showed different relationships with cognitive function and physical characteristics. The findings suggest that self-management of such patients requires maintenance of both walking and non-walking activities in a balanced manner.
Keywords
Introduction
Chronic obstructive pulmonary disease (COPD) is characterized by dyspnea on exertion due to airflow limitation caused by bronchial stenosis, 1 and patients with COPD are less physically active than healthy individuals. 2 Notably, physical activity in such patients is the greatest predictor of prognosis, 3 and participation in regular physical activity reportedly reduces the risk of all-cause mortality, respiratory mortality, and COPD exacerbations. 4 Therefore, physical activity is important for disease management.
The amount of physical activity is defined by energy requirement in metabolic equivalents (METs) and time. Throughout a day, people perform various activities, such as leisure, occupational, transport, self-care, or household chores. Some of these activities are aerobic physical activities, such as walking, while others are non-aerobic physical activities other than walking. Lewthwaite et al 5 conducted a systematic review of recommended physical activity in clinical practice guidelines for the management of COPD; they found that the most frequently-recommended type of physical activity was walking, but there were also several other types of aerobic and anaerobic physical activities, such as cycling, strength training, and nonspecific aerobic exercise. Thus, many types of physical activity are recommended, but there is no clear basis concerning which type of physical activity should be adopted.
As endurance training, mainly aerobic exercise, is recommended for patients with COPD with dyspnea to reduce shortness of breath, 6 it is desirable to increase the amount of physical activity through aerobic exercises, such as walking. However, the recommended level of daily pulmonary rehabilitation for patients with COPD with mild dyspnea symptoms (modified Medical Research Council dyspnea scale [mMRC]≤1) is still low, 7 and its effectiveness has not been fully established. Therefore, whether recommending walking or non-walking physical activity as a management of patients with COPD with mild symptoms remains debated. As the physiological mechanisms of exercise differ between walking activity, which is primarily aerobic, and physical activity other than walking, which is primarily non-aerobic, it is expected that the association with physical characteristics may also differ between these two types of exercise. In addition, there is no clear relationship between aerobic exercise and cognitive function. 8 It would be meaningful to examine this relationship in COPD cases, which are complicated by cognitive decline. 9
This study aimed to examine the relationship between different types of physical activity (walking and non-walking) and cognitive function or physical characteristics in patients with mild COPD in a community without pulmonary rehabilitation. Our findings would provide a reference for the type of exercise that should be recommended to patients.
Methods
Design
The study had a cross-sectional design.
Participants
From August 2018 to January 2020, out of 63 patients with stable COPD who visited three clinics and one hospital for a routine checkup, three female patients, 10 patients with mMRC≥2, one patient who could not perform activity measurement for >7 days, and nine patients with missing values were excluded from this study. Moreover, patients with obvious dementia, severe orthopedic or cerebrovascular diseases that would interfere with walking, or unstable heart diseases were also excluded. Finally, 40 male patients with mild COPD (mean age, 75.7 ± 6.7 years; mean forced expiratory volume in 1 s [FEV1]/forced vital capacity [FVC], 60.7 ± 8.8%) were included in the analysis.
Procedures
In this study, physical activity was assessed as the primary endpoint, while respiratory function, cognitive function, body composition, limb muscle strength, and exercise capacity were assessed as secondary endpoints.
A triaxial accelerometer (Active style PRO HJA-750C; OMRON, Kyoto, Japan) was used for the evaluation of physical activity. The triaxial accelerometer is a device that can evaluate the physical activity of walking (walking activity) and the physical activity of daily life other than walking (non-walking activity) separately. 10 The triaxial accelerometer was attached vertically to the waist of the pants, and participants were instructed to wear it except at bedtime and during bathing. The duration of wearing the accelerometer was 1 month. At the time of analysis, a minimum of 3 days (2 weekdays and 1 holiday) was required to evaluate the amount of physical activity. 11 As the physical activity of the elderly decreases after evening, 2 we excluded those who wore the activity meter for <3 days and those who did not wear it for >6 h per day. The measurement items were the average number of steps per day, average walking time per day, and Ex amount (METs × hours).
Following the recommendations of the American Thoracic Society Guidelines, pulmonary function was evaluated using a spirometer (AS-507; Minato Medical Science Co. Ltd, Osaka, Japan). 12 The predictive values of FVC and FEV1 were calculated using the formulas proposed by the Japanese Respiratory Society, 13 and %FEV1 was further classified by the Global Initiative for Chronic Obstructive Lung Disease (GOLD) grading scale. 6
Cognitive function was assessed using the Mini-Mental State Examination (MMSE) score 14 and the Japanese version of the Montreal Cognitive Assessment (MoCA-J). 15 The MMSE is widely used as a simple test of cognitive function, consisting of 11 questions. The total score of all items (maximum 30 points) was evaluated. The MoCA-J, like the MMSE, is a 30-point assessment of multidomain cognitive functions (ie, visuospatial, executive, attention, memory, language, and disorientation) and has been used as an assessment scale for mild cognitive impairment. 15 The total score of all items was evaluated.
Body composition was assessed via the bioelectrical impedance method using a body composition meter (Inbody 270; Inbody, Tokyo, Japan). The participants were asked to stand barefoot on the measurement table, place both feet on the electrodes, and hold the electrodes with both hands until the end of the measurement. The muscle mass, skeletal muscle mass index (SMI), and body fat percentage were measured. The SMI was calculated by dividing the muscle mass of the extremities (kg) by the height (m) squared as follows:
The QS was measured using a manual muscle strength measuring device (μ-TasF1; Anima Co., Ltd, Tokyo, Japan). In the sitting lower leg drooping position, the sensor pad was fixed to the anterior surface of the distal lower leg with a belt, and participants performed an isometric knee extension exercise with maximal effort for approximately 3 s, as described by Kato et al 17 The QS was measured twice on each side, and the normalized value (%) obtained by dividing the maximum value of either side by the BW was used as the representative value (QS/BW).
Exercise capacity was assessed by the Incremental Shuttle Walking Test (ISWT), as described by Singh et al 18 Walking distance was measured, and transcutaneous oxygen saturation and the pulse rate were assessed using a pulse oximeter (Radical RDS-1; Masimo, Tokyo, Japan) at rest before and immediately after the test. In addition, breathlessness and fatigue in the lower limbs were measured using a modified Borg scale. 19 As reproducibility can be confirmed even with only one measurement, 20 only one measurement was performed.
Furthermore, basic information of the participants was evaluated, including age, height, weight, body mass index (BMI), dyspnea (mMRC), 6 health-related quality of life (St. George's Respiratory Questionnaire [SGRQ]), 21 bronchodilator use, number of exacerbations, and hospitalization for exacerbations.
Statistical Analyses
The power analysis software G-power ver. 3.1.9.2 (University of Dusseldorf, Dusseldorf, Germany) was used to determine the sample size, and a minimum of 26 participants were required for correlation analysis, with 0.5 for the effect size, 0.05 for the alpha error, and 0.8 for the power of the test. Next, the relationships between physical activity and each evaluation index (the correlation between the mean value of walking activity and each evaluation index as well as the correlation between the mean value of non-walking activity and each evaluation index) were analyzed. After confirming normality by the Shapiro–Wilk test, analysis was performed with Spearman's correlation coefficient. 22 The statistical analysis was performed using SPSS ver. 28 (IBM, Armonk, NY), and the statistical significance level was set at 5%.
Results
The characteristics of the participants are presented in Table 1, and the data are shown as means ± standard deviations. Regarding respiratory function, most participants had mild-to-moderate airflow limitation in GOLD I or GOLD II (92.5%). Concerning the GOLD group classification, most participants were assigned to Group A (97.5%). Table 2 shows the amount of physical activity. Concerning the average number of steps taken per day, there was a large variation, and the largest percentage (25.0%) of participants made 2000–3000 steps. Regarding daily Ex, 87.5% of the participants had a walking activity of 0–2 Ex, while 67.5% had a non-walking activity of 1–3 Ex (Figure 1).

Distributions of participants based on average walking or non-walking daily physical activity.
Characteristics of the participants.

GOLD grade, mMRC, GOLD stage, bronchodilator use, and exacerbations are indicated by the number of participants; others are indicated by means ± standard deviations.
Exacerbation: number of exacerbations in the last year; bAdmission to hospital: number of admission to hospital in the last year; cPercentage of predicted value.
BMI: body mass index; mMRC: modified medical research council dyspnea scale; MMSE: mini-mental state examination; MOCA-J: Japanese version of Montreal Cognitive Assessment; SMI: skeletal muscle mass index; GS/BW: percentage of grip strength/body weight; QS/BW: percentage of quadriceps strength/body weight; ISWT: incremental shuttle walking test; LAMA: long-acting muscarinic antagonist; ICS: inhaled corticosteroid; LABA: long-acting β-agonists; SGRQ: St. George's Respiratory Questionnaire.
Physical activity of the participants (n = 40).

Values are indicated as means ± standard deviations. aEx: METs × h.
Correlation analyses of physical activity with cognitive function and physical characteristics are presented in Table 3 and Figure 2. There were significant correlations between walking activity and the MOCA-J score (ρ = 0.383, P < .05), walking distance assessed by the ISWT (ρ = 0.779, P < .001), and health-related quality of life assessed using the SGRQ (Total: ρ = -0.337, P < .05; activity: ρ = -0.405, P < .01). However, there was no correlation between walking activity and the BMI (P = .473) and muscle mass (skeletal muscle mass: P = .478; SMI: P = .330; right upper limb: P = .318; left upper limb: P = .421; trunk: P = .343; right lower limb: P = .597; left lower limb: P = .776). In addition, there were significant correlations between non-walking activity and BMI (ρ = 0.326, P < .05), muscle mass (SMI: ρ = 0.337, P < .05; right upper limb: ρ = 0.355, P < .05; left upper limb: ρ = 0.348, P < .05; trunk: ρ = 0.336, P < .05), walking distance assessed by the ISWT (ρ = 0.529, P < .01), and activity as assessed using the SGRQ (ρ = -0.337, P < .05). However, there were no correlations between non-walking activity and the MOCA-J score (P = .245), and the total SGRQ score (P = .161).

Relationship between physical activity and cognitive function and physical characteristics.
Correlations with the amount of physical activity (n = 40).

Notation is presented as Spearman's rank correlation coefficient, ρ. aEx: METs × h; BMI: body mass index; MMSE: mini-mental state examination; MOCA-J: Japanese version of Montreal Cognitive Assessment; SMI: skeletal muscle mass index; GS/BW: percentage of grip strength/body weight; QS/BW: percentage of quadriceps strength/body weight; ISWT: incremental shuttle walking test; SGRQ: St. George's Respiratory Questionnaire. *P < .05, **P < .01.
Discussion
This study examined the relationship between different types of physical activity and cognitive function or physical characteristics in community-dwelling patients with mild COPD who were not receiving pulmonary rehabilitation. The results revealed a significant correlation between walking activity and the MOCA-J score, the walking distance assessed by the ISWT, and health-related quality of life evaluated based on the SGRQ. Additionally, there was a significant correlation between non-walking activity and muscle mass or walking distance. The MOCA-J and the total SGRQ score were significantly correlated only with walking activity, while the BMI and the muscle mass were significantly correlated only with non-walking activity.
Previous studies on the relationship between physical activity and cognitive function in patients with COPD have demonstrated that cognitive impairment reduces physical activity because it is difficult for these patients to initiate activities or recognize the importance of exercise. 23 Moreover, physical activity has been reported to have a positive effect on cognitive function in patients with COPD by influencing mediating factors, such as anxiety, depression, nutrition, and sleep quality. 24 Thus, there may be a bidirectional relationship between physical activity and cognitive function in patients with COPD. As this was a cross-sectional study, a causal relationship between physical activity and cognitive function could not be determined; however, a significant correlation was found between walking activity and the MOCA-J score, further supporting the relationship between physical activity and cognitive function demonstrated in previous studies.15, 23, 24 The results of this study are particularly noteworthy as only the walking activity showed a significant relationship with cognitive function as assessed by the MOCA-J score, and there was no correlation between non-walking activity and cognitive function. The MOCA-J is considered an indicator of early cognitive decline. 15 Therefore, walking activity may be related to early cognitive decline, and it is necessary to consider the role of walking activity in the prevention of cognitive decline.
Among physical activities, only walking activity was significantly correlated with the total SGRQ score, a health-related quality of life index, and high walking activity was significantly correlated with high health-related quality of life. Esteban et al 25 determined the predictors of health-related quality of life in patients with COPD who were followed up for 5 years and found that the factor with the greatest impact on health-related quality of life was physical activity. Further, another study 26 similarly demonstrated the influence of physical activity on health-related quality of life. In contrast, physical activity is reportedly associated with the quality of life of patients with asthma, 27 a relationship that is common among patients with respiratory diseases. Based on our findings and those of previous studies, it is reasonable to assume that physical activity is important in maintaining health-related quality of life in patients with COPD. However, previous studies25, 26 did not compare the effects of various types of physical activity. Our study revealed that among different types of physical activity, walking activity might be necessary to maintain quality of life in patients with COPD.
Nevertheless, the BMI and muscle mass were significantly correlated only with non-walking activity. Physical inactivity in patients with COPD leads to skeletal muscle dysfunction and sarcopenia, a decrease in skeletal muscle mass. 28 Therefore, the BMI also decreases. Therefore, maintaining physical activity is necessary. Consistently, the results of this study showed that among physical activities, non-walking activity was related to skeletal muscle mass, and the amount of non-walking activity in daily activities was higher than that in walking activity (Figure 1). These results suggest that exercise in non-walking activity is related to the maintenance of skeletal muscle mass, especially in the upper limb and trunk muscles.
Furthermore, there was a significant correlation between walking activity or non-walking activity and walking distance assessed by the ISWT. Previous studies have shown a correlation between physical activity and exercise capacity, although the relationship was not strong. 4 However, this study found a moderate correlation between waking activity and exercise capacity. The findings suggest that the maintenance of physical activity is important for the maintenance of exercise capacity in patients with mild COPD.
A limitation of this study is that it was cross-sectional. Thus, the causal relationship between physical activity and cognitive function or physical characteristics could not be determined. Therefore, a longitudinal study is needed to confirm the present findings in the future.
In conclusion, walking and non-walking daily physical activities showed different relationships with cognitive function and physical characteristics in patients with mild COPD. Therefore, self-management may be necessary to ensure a good balance of both walking and non-walking-related physical activities in patients with COPD.
Footnotes
Acknowledgements
We would like to express our sincere gratitude to Mr Shota Kotani for his co-operation in collecting the research data.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author contribution(s)
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by JSPS KAKENHI [Grant Number JP21K10782].
Ethics Approval and Consent to Participate
The participants were fully informed about the contents of this study, and their written consent was obtained. This study was conducted in accordance with the Declaration of Helsinki and was approved by the Research Ethics Review Committee of Kyoto Tachibana University (Approval No. 17-07).