Abstract
Hydatid disease, caused primarily by Echinococcus granulosus, is prevalent in regions where livestock farming is common. Although typically considered benign, ruptured hydatid cysts into the abdominal cavity present a rare but severe complication requiring urgent surgical intervention. We hydatid liver cyst, emphasizing the unprecedented nature of this occurrence, as it has never been reported in the literature before. The case underscores the role of computed tomography (CT) imaging in diagnosis and multidisciplinary management involving emergency physicians, radiologists, anesthetists, and surgeons. Key points highlighted include the rarity of postpartum hydatid cyst rupture, the diagnostic utility of CT scans, and the necessity of immediate surgical intervention. Surgical strategies include conservative techniques and intraoperative lavage with hypertonic saline solution to prevent recurrence. Postoperative albendazole therapy and regular follow-up aid in preventing recurrence and early detection of complications. This case underscores the importance of suspecting ruptured hydatid cysts in postpartum women with underlying hepatic hydatid cyst and features of peritonitis, necessitating prompt recognition and management of complications in hydatid disease
Introduction
Hydatidosis, a parasitic infection primarily caused by Echinococcus granulosus and less frequently by Echinococcus alveolaris, is prevalent in regions such as the Mediterranean, including Morocco, the Middle and Far East, Australia, New Zealand, and South America, where livestock farming is common. 1 Although hydatid disease typically affects the liver and lungs, it can also involve less common sites like the spleen and central nervous system. 1
While generally considered benign, hydatid disease can lead to severe complications such as cyst rupture and secondary bacterial infections, significantly worsening the patient’s condition and requiring urgent medical intervention. 2 Rupture into the abdominal cavity is particularly rare and severe, necessitating emergency surgical intervention. 3 Postpartum cases of cyst rupture are exceptionally rare, highlighting the need for prompt recognition and management. 3 Diagnostic methods typically include ultrasonography (US) and computed tomography (CT), often presenting with acute abdominal signs like guarding, rebound, and tenderness. 3 The rarity of this complication warrants its consideration in the differential diagnosis of acute abdomen, particularly in endemic regions. Despite this, specific management guidelines for peritoneal perforation remain lacking. Treatment approaches for uncomplicated cases apply similarly to complicated ones, emphasizing the necessity of emergency surgical intervention in cases of cyst rupture. 3
Herein, we present a case of a young woman who developed peritonitis secondary to a ruptured hydatid liver cyst 17 days after giving birth, with CT scan findings aiding in diagnosis and necessitating urgent and multidisciplinary management involving emergency physicians, radiologists, anesthetists, and surgeons.
Case Presentation
A 20-year-old woman, gravida 1, para 1, with presented to the emergency room with complaints of severe abdominal pain, distension, and fever. She had delivered a healthy baby boy vaginally 17 days prior. The patient reported the onset of abdominal discomfort 2 weeks of postpartum, which progressively worsened. The patient had no prior medical history or diagnosis of a hepatic hydatid cyst. She denied any history of trauma or recent travel.
On examination, the patient appeared acutely ill, with a temperature of 38.9°C, a blood pressure of 120/60 mmHg and tachycardia of 108 beats per minute. Abdominal examination revealed marked tenderness, guarding, and rebound tenderness throughout the abdomen. No allergy related symptoms were noted. Laboratory investigations showed leukocytosis (18,500/mm³) with neutrophil predominance, eosinophil count of 980/mm³ (5.3% of the total white blood cell count), elevated C-reactive protein (CRP) levels, and mild transaminitis. An abdominal ultrasound revealed free fluid in the peritoneal cavity with multiple septations and debris, suggestive of peritonitis.
A contrast-enhanced CT scan of the abdomen and pelvis was performed, revealing a peripheral superficial collapsed cystic lesion in the left lobe (II segment) of the liver that has lost its spherical shape, with thick enhancing walls and a parietal defect, consistent with a ruptured hydatid cyst. Evidence of spillage of cyst contents into the peritoneal cavity appearing as serpentine structures, were noted, along with diffuse thickened peritoneal enhancement and free peritoneal fluid (Figure 1).

CT scan axial images after intra-venous contrast injection (a) revealing the presence of an heterogenous collapsed cystic lesion in the left lobe of the liver (segment II; head white arrow) with a parietal defect (white arrow), (b) with spillage of its heterogenous content appearing as serpentine structures (orange arrow), free peritoneal fluid (orange asterisk), thickened peritoneum (yellow arrow).
Given the clinical suspicion of peritonitis and the CT scan findings, the patient was taken for an emergency laparotomy. Intraoperatively, a large ruptured cyst was found on the inferior side of the II segment of the liver, with spillage of hydatid cyst contents into the peritoneal cavity associated to a yellow serous fluid (Figure 2). The patient underwent a partial cystectomy, followed by an irrigation with hypertonic saline solution thorough the cyst pouch and the peritoneal cavity. Postoperatively, the patient was started on broad-spectrum antibiotics and anthelmintic therapy.
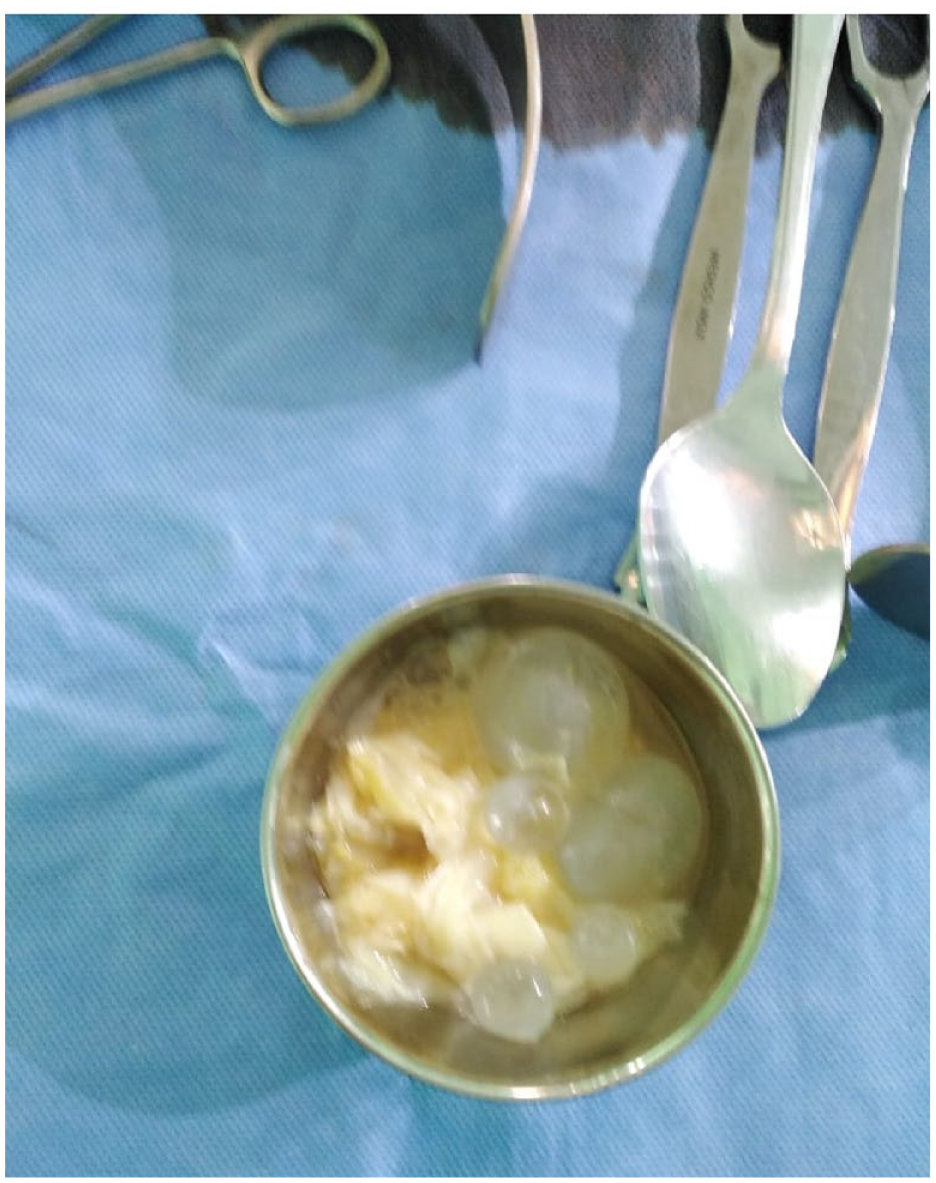
Macroscopic image of the ruptured hydatid cyst content and multiple cysts removed from peritoneal cavity.
The patient’s postoperative course was uneventful, with resolution of fever and leukocytosis within 48 hours. Serial abdominal ultrasounds showed resolution of the peritoneal fluid collection. Liver function tests remained within normal limits, and the patient was discharged home on postoperative a week after, with appropriate follow-up arrangements.
Discussion
Echinococcal infections are the leading cause of liver cysts worldwide. 1 These cysts, known as hydatid cysts, can rupture due to various factors, including both major and minor blunt abdominal trauma. A significant portion of affected individuals may not exhibit any noticeable symptoms, leading to undiagnosed cases. However, when symptoms do arise, they may present in atypical ways, particularly with severe trauma. 4
Research has highlighted the incidence of peritoneal perforation associated with hydatid cysts, with studies reporting rates of 7.8% in large case series. Trauma remains the primary precipitating factor for such perforations, but increased intracystic pressure can also contribute to cyst rupture.1,4,5
An intriguing aspect highlighted by recent investigation is the lack of documented cases of hydatid cyst rupture during the postpartum period. Despite thorough searches of medical databases like PubMed using specific terms such as “postpartum ruptured hydatid liver cyst,” no instances have been reported in the literature. This finding raises interesting questions regarding the potential influence of hormonal changes and physiological adaptations during the postpartum phase on the risk of hydatid cyst rupture, warranting further exploration in future research endeavors.
Given the patient’s 2-week history of pain, which coincides with the postpartum period, it is plausible that the rupture could have occurred intrapartum or even before delivery. The postpartum period, characterized by significant physiological changes, may increase the risk of cyst rupture. Hormonal changes and increased abdominal pressure during pregnancy and delivery could contribute to cyst rupture, as observed in this case. This hypothesis aligns with the understanding that increased intracystic pressure can lead to cyst rupture, especially in scenarios involving significant physiological stress, such as childbirth.
The most common initial indication of peritoneal perforation is abdominal pain, often accompanied by symptoms such as nausea and vomiting, attributable to irritation of the peritoneum. However, the potentially life-threatening consequence of intraperitoneal perforation lies in the manifestation of allergic reactions. Studies indicate that 16.7% to 25.0%, of individuals with burst hydatid cysts experience allergy-related symptoms. Furthermore, there have been documented cases of fatal anaphylactic reactions following cyst rupture.6,7 Researchers have reported varying rates of anaphylaxis among patients with ruptured hydatid cysts, ranging from 1% to 12.5%. 6 this suggests that while allergic responses are not very commun, the possibility of anaphylaxis should always be considered and appropriate measures initiated promptly. 1
The main ways used to diagnose ruptured hydatid cysts are ultrasonography and computed tomography (CT), with reported sensitivities of 85% and 100%, respectively. 6 While ultrasonography (US) is reliable for spotting echinococcal cysts in the liver, CT scans can provide the most detailed information about the location and severity of intraabdominal hydatid disease, including the presence of exogenous cysts. Evaluating with CT minimizes the risk of recurrence and enables more effective treatment. 1
Akcan et al, 1 discussed risk factors associated with liver hydatid cyst perforation. Three main risk factors were identified: young age, cyst diameter larger than 10 cm, and superficial location of the cyst. They suggested that younger individuals, who are more likely to be involved in accidents such as traffic collisions, may experience increased risk of perforation due to trauma. Additionally, it points out that the absence of healthy liver tissue surrounding large and superficial cysts may contribute to their vulnerability to rupture, as seen in this case. 1
Immediate action is crucial in the emergency room (ER), involving close monitoring, intensive care measures, administration of vasoactive drugs, antihistamines, and corticosteroids as first rescue measures. 8
Urgent surgery is the cornerstone of treatment, aiming to address the primary liver hydatid cyst and prevent local and peritoneal recurrences. the surgical approaches for primary liver cysts include conservative methods like the unroofing procedure or partial cystectomy, and radical methods like pericystectomy and hepatectomy. 9 In emergencies, conservative methods are preferred for their lower risk and shorter operative time. 10 Followed by an intraoperative Lavage using hypertonic saline solution of 3% to 30% to remove cyst contents and prevent allergic reactions. Scolicidal solutions are also used to eradicate protoscoleces and stop contact between the hydatid cyst content and the peritoneum. 11
Postoperative albendazole treatment of 15 mg/kg/day is initiated promptly to prevent recurrence, no clear consensus on the exact duration but some authors maintained it for at least 12 months.8,12
Patients undergo regular follow-up with hydatid serology and abdominal ultrasonography every 3 to 6 months to detect recurrence early. CT scans are reserved for doubtful cases to minimize radiation exposure. 12
Conclusion
In conclusion, we present a rare case of a young postpartum woman who developed peritonitis secondary to a ruptured hydatid liver cyst, an occurrence not previously reported in the literature. This case emphasizes the importance of considering uncommon etiologies in postpartum peritonitis and highlights the need for prompt recognition and management of complications in hydatid disease. The role of computed tomography (CT) imaging in diagnosis and guiding multidisciplinary management involving emergency physicians, radiologists, anesthetists, and surgeons is critical. Urgent surgical intervention remains the cornerstone of treatment, with conservative techniques favored in emergencies for their lower risk and shorter operative time. Intraoperative lavage with hypertonic saline solution and postoperative albendazole therapy are vital in preventing recurrence and facilitating early detection of complications. This case underscores the need for continued research to explore optimal strategies for preventing and managing such rare but serious conditions, particularly in unique clinical scenarios like the postpartum period.
Footnotes
Acknowledgements
The authors are grateful for the reviewer’s valuable comments that improved the manuscript.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contribution
All authors have accepted responsibility for the entire content of this manuscript and approved its submission.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
