Abstract
Idiopathic granulomatous vulvitis is an uncommon anogenital area disease described in the last few decades. It causes an inflammatory reaction that culminates in swelling and possibly distortion of the female anogenital area. Many reported cases consider this non-infectious entity the genital counterpart to granulomatous cheilitis. We here present a 64 years old female patient with idiopathic granulomatous vulvitis co-existing with lipodermatosclerosis, with the excellent response of the former condition to hydroxychloroquine and potent topical steroids.
Introduction
Granulomatous vulvitis is a chronic and painless relapsing granulomatous disease affecting the anogenital area of females, mainly in their third decade. It was first described by Westermark and Henriksson in 1979. 1 It is deemed idiopathic post-exclusion of infectious etiologies alongside sarcoidosis, Crohn’s disease, and others, as the cause of inflammation is unknown. It is characterized clinically by swelling of the external genitalia and epithelioid non-caseating granulomas histologically. 2
Few cases of idiopathic granulomatous vulvitis (IGV) are reported worldwide, and even fewer in the Middle East, 2 thus making its treatment challenging over the long term with no current cure.
Case Report
We report a 64 years old single female patient who presented for evaluation of painful non-itchy vulvar swelling of several years duration that became more pronounced 1 year ago. She had no preceding fever, cough, shortness of breath, or weight loss. She also denied any change in bowel movement, oral ulcerations, or joint pain. The patient had a hysterectomy 10 years prior for menorrhagia attributed to uterine fibroids, complicated postoperatively by deep vein thrombosis of the lower leg. In addition, she underwent a colonoscopy 10 years earlier, which was normal.
Evaluation of the genitalia revealed indurated verrucous, skin-colored plaques on both sides of the labia majora with overlying intact vesicles. The skin of the mons pubis was erythematous and indurated. (Figure 1A). A thorough general inspection of the patient showed bilaterally brown-colored, non-scaly indurated plaques over both legs. These changes were consistent with lipodermatosclerosis (Figure 1B). The patient had noticed these changes years ago but wasn’t bothered by them and reported the onset after undergoing a hysterectomy.

(A) Verrucous plaques over both sides of the labia majora, with overlying vesicles. (B) Brownish-red pigmentation and induration above the ankles. Notice the overlying dilated veins.
The proposed differential diagnosis at this stage included cutaneous Crohn’s disease, tuberculosis, or acquired lymphangioma circumscriptum.
Multiple skin biopsies were taken: Punch biopsy taken from vesicles over labia demonstrated dilated lymphatic channels (Figure 2), while ellipse biopsy taken from indurated skin overlying mons pubis showed non-caseating epithelioid granulomas (Figure 3). Ziehl-Nelson, Periodic Acid-Schiff, and Grocott’s Methenamine Silver stains were performed and were negative for mycobacterial and fungal elements.

Dilated lymphatic channels within the papillary dermis. H&E stain 20X.

Non-caseating epithelioid granulomas within the reticular dermis. H&E stain 20X.
Detailed work-up ensued, including laboratory evaluation that showed normal blood cell count, kidney, and liver function tests. Antineutrophil cytoplasmic antibodies and quantiferon test for tuberculosis were negative.
Imaging included a Computerized Tomography scan of the chest, abdomen, and pelvis demonstrated normal lung parenchyma, skin thickening with extensive fat stranding of the abdominal wall and normal bowels, and an absent prehepatic inferior vena cava (IVC), which is a congenital anatomical variant of IVC-Azygos system. After excluding Sarcoidosis and Chron’s disease, the patient was diagnosed with idiopathic granulomatous vulvitis.
Regarding lipodermatosclerosis, the diagnosis in our patient was made clinically, and no skin biopsy was taken. Doppler US of the lower legs’ superficial and deep venous system showed bilaterally incompetent femoral and superficial popliteal veins. Thrombophilia work-up revealed heterozygous mutations in methyltetrahydrofolate reductase and factor V Leiden.
The vascular surgeon recommended the patient use compression stockings.
Treatment for idiopathic granulomatous vulvitis was started using hydroxychloroquine 200 mg twice daily and topical Clobetasol propionate for 6 months. The patient was evaluated monthly, and by the end of the 6 months, she reported a significant improvement in pain and appearance (Figure 4).
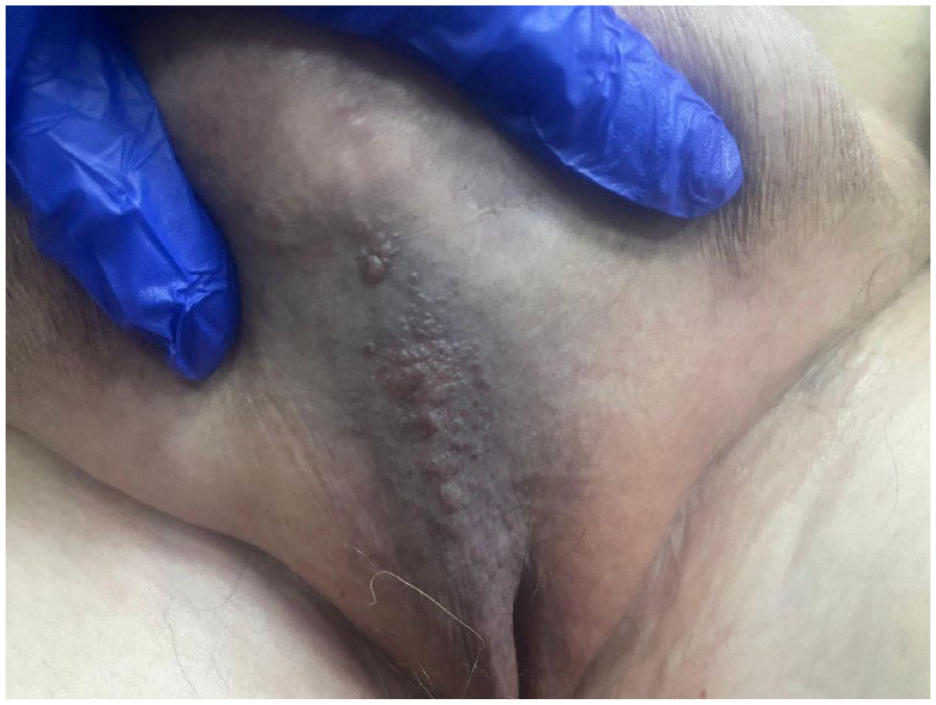
Clinical response after 6months of antimalarial therapy and topical steroids.
Discussion
Granulomatous vulvitis is a painless, chronic, relapsing granulomatous disease in 1979. The Ages of affected women vary from 20 to 77 years, with the majority being in their third decade. The etiology of the idiopathic genital granulomatous inflammation is unknown. 1
The condition begins with signs and symptoms of acute inflammation that follow a chronic relapsing course. It clinically presents with erythema, edema, and induration of the external genitalia. The latter changes with lymphedema, which results in genital distortion and or disfiguration.
The histologic finding of non-caseating epithelioid granuloma is characteristic.
Accordingly, based on the clinicopathologic picture, 2 main differentials must be excluded; Sarcoidosis and Crohn’s disease.1,2
Sarcoidosis is a systemic granulomatous disease of unknown origin, mainly affecting the lungs, with one-third of the patients having cutaneous manifestations. Histologically, it is characterized by non-caseating epithelioid granulomas with sparse or absent surrounding lymphocytic infiltrate. 3 In this case, the absence of respiratory symptoms and the demonstration of normal lung parenchyma and lymph nodes on imaging excluded the diagnosis of sarcoidosis.
Crohn’s disease is an inflammatory bowel disease, with mucocutaneous findings in 20% to 45% of patients. Cutaneous Crohn’s disease, genital or extragenital, occurs in association or precedes intestinal Crohn’s disease. Genital involvement is reported in two-thirds of children and one-half of adults, presenting as labial, penile or scrotal erythema or lymphedema. It is characterized histologically by non-caseating epithelioid granulomas. 4 In this case, the patient had no change in her bowel habits, weight loss, oral ulcerations, joint pain, or eye symptoms. In addition, abdomen imaging showed bowel loops within normal, making the Crohn’s disease diagnosis less likely.
While the clinical findings of translucent vesicles resembled lymphangioma cicrucmscriptum, which can be rarely acquired, 5 the histological findings of non-caseating epithelioid granuloma excluded this diagnosis.
Accordingly, due to its rarity, treatment of idiopathic granulomatous vulvitis is not unified. The reportedly used medications in literature are systemic corticosteroids, antimalarials, tranilast, metronidazole, clofazimine, and lymecycline.6-9 In our case report, the patient was treated with the antimalarial hydroxychloroquine 200 mg twice daily and topical Clobetasol propionate (superpotent corticosteroid) for 6 months. There was a marked reduction in the erythema and disappearance of the pain by the end of the 3 months.
Lastly, some patients with idiopathic granulomatous vulvitis have a history of hysterectomy, 6 but to the best of our knowledge, none reported venous insufficiency of the lower limbs. Both granulomatous vulvitis and lipodermatosclerosis developed progressively in our patient following a hysterectomy complicated by massive deep vein thrombosis. A degree of lymphatic dysfunction may occur post-thrombosis 10 ; lymphatic malfunctioning is well-recognized in patients who develop lipodermatosclerosis due to chronic venous insufficiency.11,12 Further, lymphatic dilation is a consistent feature of granulomatous vulvitis. We suggest that venous and lymphatic dysfunction resulting from deep vein thrombosis in this patient has possibly contributed to the formation of both lipodermatosclerosis and granulomatous vulvitis. While this association may be a coincidence, a causal relationship between these factors and granulomatous vulvitis remains to be further investigated.
Conclusion
To summarize, idiopathic granulomatous vulvitis is a chronic inflammatory disease diagnosed by excluding infectious and non-infectious causes, alongside characteristic histopathological findings of lymphatic vessel dilatation and non-caseating epitheloid granuloma. From our case report, we propose a potential relationship between lipodermatosclerosis and granulomatous vulvitis, and acknowledge the effectiveness of hydroxychloroquine and topical sterids in its treatment.
Footnotes
Author Contributions
JM: Main author, conceptualization of idea, writing the draft. EA: Data collection and draft writing. AQ: Literature review and draft writing. FA and DA: Draft writing and revision.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All relevant data are available within the manuscript.
Ethics Statement
The patient in this manuscript has given written informed consent to publish the case details and usage of the pictures. The Declaration of Helsinki was adequately addressed. The study was approved by the institutional review board of Jordan University of Science and Technology.
