Abstract
Introduction:
Systemic diseases can be found in neuromyelitis optica spectrum disorder (NMOSD) as a co-existing disease with paraneoplastic syndrome, sarcoidosis, or connective tissue disease. Cryptogenic organizing pneumonia (COP) in NMOSD with no evidence of these systemic disorders has rarely been reported.
Case presentation:
We present a 75-year-old patient who showed multifocal longitudinally extensive transverse myelitis and bilateral lung lesions that was seropositive for aquaporin-4 (AQP4) antibody. The patient initially presented with chronic cough, myalgia, and severe bilateral truncal neuropathic pain, and initial chest computed tomography demonstrated multifocal consolidations with reversed halo sign involving both lobes. Since this patient was over 50 years of age, our differential diagnoses included lung cancer and sarcoidosis. Through extensive studies including lung biopsy, an idiopathic type of diffuse interstitial lung disease—cryptogenic organizing pneumonia (COP)—was finally diagnosed. The patient was treated with high-dose methylprednisolone and it was tapered with oral steroids; mycophenolate mofetil was later added to the regimen. After treatment, the severe neuropathic pain and multifocal lung consolidation resolved.
Conclusion:
Herein, we presented a case of late-onset NMO with nonneoplastic, nonsarcoidosis, diffuse interstitial lung lesions, which is the finding of COP.
Introduction
Neuromyelitis optica spectrum disorders (NMOSD) are inflammatory demyelinating diseases of the central nervous system (CNS) usually presenting with optic neuropathy or longitudinally extensive transverse myelitis. 1 Anti-aquaporin-4 IgG antibody (AQP4-IgG) is considered a specific serum marker for NMOSD, and a few cases have shown multisystem involvement, including the lungs, breasts, and muscles.2-7 These reports have shown that NMOSD can coexist with paraneoplastic syndrome, sarcoidosis, and other connective tissue diseases.1-5,8 Herein, we describe the case of a 75-year-old woman who presented with severe truncal neuropathic pain and bilateral multifocal lung lesions and was eventually diagnosed with late-onset NMOSD associated with cryptogenic organizing pneumonia (COP), an idiopathic form of diffuse interstitial lung disease.
Case Presentation
A 75-year-old Korean woman presented to the emergency room with cough, myalgia, and severe neuropathic pain in the trunk, all of which began 1 month prior; dry cough and whole-body myalgia developed first and were followed by bilateral lancinating pain in the trunk with allodynia, 2 weeks later. Her pain visual analog scale (VAS) score was 9 to 10. Initial chest computed tomography demonstrated multifocal consolidations with reversed halo sign involving both lungs (Figure 1). Her vital signs were initially stable with no fever. With the suspicion of organizing pneumonia, percutaneous fine needle aspiration (PCNA) was attempted but failed because the patient could not tolerate the procedure due to severe neuropathic truncal pain. On the second day of admission, neurology consultation was requested for the severe neuropathic pain, and neurological examination revealed that the patient was alert with no cranial nerve deficit. Motor examination revealed normal strength in the both upper and lower extremities. Position and vibration sensations were normal. Pain and touch were hyperesthetic, and allodynia of touching the skin in the trunk between T4 and 10 was observed. Reflexes in the upper extremity were normal; however, hyperreflexia was noted in the lower extremities. Magnetic resonance imaging (MRI) of the spinal cord was performed to determine the cause of her severe neuropathic pain. T2 weighted imaging showed multiple short-segment hyperintensities in the spinal cord spreading from T3 to T8. Cord swelling was not observed (Figure 2). Brain MRI did not show any change in white matter. Although she denied any visual disturbance, her visual-evoked potential study showed a bilateral prolonged P100 wave. The patient showed unobtainable lumbar (N1) and cortical (P37) waves on somatosensory evoked potentials. Motor evoked potential study was normal. A cerebrospinal fluid (CSF) analysis was performed, and the results were as follows: white blood cell count, 20 (normal range: 0-5); total protein, 50.7 (normal range: 15-45) mg/dl; and glucose, 78 (normal range: 50-80) mg/dl. The serum AQP4-IgG was positive on cell-based indirect immunofluorescence assay. Tumor markers such as CEA (Carcino-embryonic antigen), CA19-9 (Carbohydrate Antigen), ANA (antinuclear antibody), ANCA (antineutrophil cytoplasmic antibodies), C3, and C4 and anti-dsDNA IgG antibodies were negative. Erythrocyte sedimentation rate and rheumatoid factor were elevated to 68 (0-20) mm/hour and 18.7 (0-14) IU/ml, respectively. Serological tests (for viruses and bacteria) to evaluate the infectious cause of pneumonia were all negative. The CSF study of viruses and bacteria to assess the infectious myelitis was also negative.
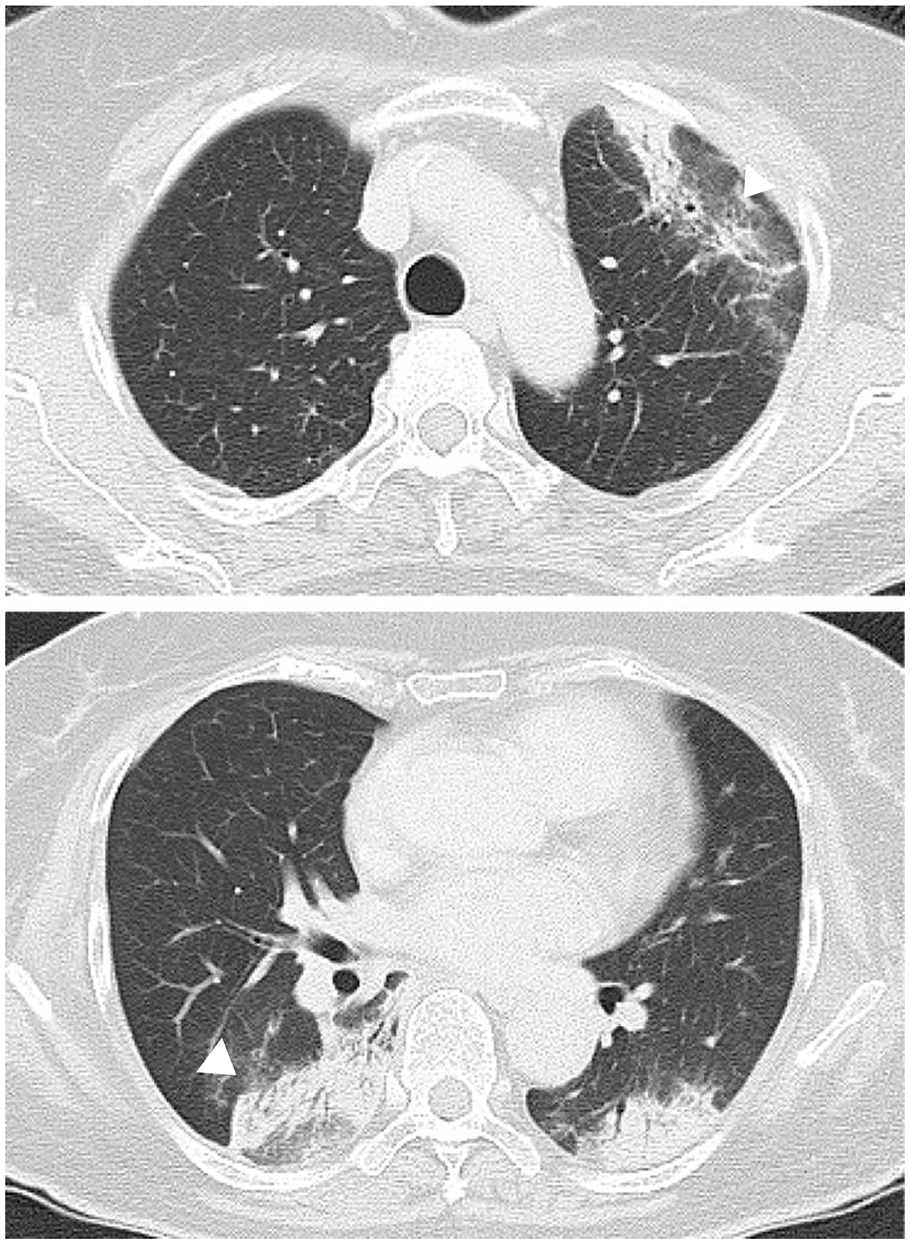
Initial chest CT showing multifocal consolidation with reversed halo sign (arrowheads) involving the right lower and left upper and lower lobes. These findings correspond to those of cryptogenic organizing pneumonia, a subtype of subacute interstitial pneumonia.

Magnetic resonance imaging of the spinal cord showing longitudinally extensive T2 hyperintensity at the thoracic level. (A) T2-weighted sagittal image showing multiple longitudinally extensive hyperintense lesions at the T3-8 levels. (B) Axial T2-weighted image showing a hyperintense lesion at central T5 spinal cord.
She was commenced on intravenous steroid pulse therapy (1 g) for 5 days. To rule out cancer, PCNA was performed in the right lower lobe and no tumor cells were present although interstitial fibrosis with mild inflammatory cell infiltration was observed. (Figure 3) Oral steroid (60 mg) was tapered and 2 g of mycophenolate mofetil was added. After 2 weeks of treatment, the neuropathic pain resolved considerably (she had a VAS score of 2-3) along with the multiple lung consolidations (Figure 4).

Fine needle biopsy of the consolidated lung lesion in the right lower lobe demonstrating interstitial fibrosis with mild inflammatory cell infiltration. (H&E stain × 200).

Chest radiograph showing interval changes. (A) Chest radiograph showing new multifocal consolidations (arrowhead) involving the right upper and lower lung zones. (B) Chest radiograph after steroid treatment showing resolution of consolidations.
Discussion
Longitudinally extensive transverse myelitis and optic neuritis are the core clinical presentations of NMOSD, and AQP4-IgG positivity is confirmatory after at least 1 classical episode based on international consensus diagnostic criteria. 1 AQPs are water channels that are expressed at the highest concentration in opticospinal tissues; complement activation by antibodies against AQP4 provokes the deposition of perivascular immune complex and astrocyte injury. 9 AQPs are also expressed outside the CNS in the various epithelia and endothelia involved in fluid transport, as well as other cell types such as the epidermis, adipocytes, and skeletal muscle. 9 Previous studies on NMOSD associated with lung cancer have found that some tumor cells express AQP4-IgG and that AQP4-IgG in the serum of NMOSD patients can react with antigens expressed by the tumor cells in the same patient. 10 This indicates that AQP4-IgG is involved in the pathogenesis of paraneoplastic NMOSD and therefore, may be a paraneoplastic antibody. Non-neoplastic lung involvement in NMOSD has been reported suggesting the coexistence of sarcoidosis and rheumatologic autoimmune diseases with transverse myelitis with the AQP4 antibody.5,8 There is the world’s first reported case of COP with NMOSD in elderly patients. 7 Similar to our case, lung lesion was manifested at initial phase of disease and COP was pathologically confirmed. COP, an idiopathic form of diffuse interstitial lung disease was diagnosed pathologically and there was no evidence of paraneoplastic, rheumatologic, or autoimmune disease.11,12 NMOSD occurring after the age of 50 years can be defined as late-onset NMOSD, and the possibility of a paraneoplastic syndrome seems particularly relevant in this age group. 13 The treatment of late-onset NMOSD can be complicated especially because an aggressive clinical course has been reported in this age group. 14 Also, the possibility of the coexistence of NMOSD with other systemic disorders should be considered to establish a proper treatment strategy. Biopsy was successful after steroid therapy; therefore, the pathological report might have been reflecting the anti-inflammatory effect of the steroid. However, we were able to exclude sarcoidosis and lung cancer.
Conclusion
This case highlights the rare association between COP and NMOSD. It is important to note that in the case of late-onset NMOSD associated with COP, both clinical symptoms and lung consolidations could improve with proper immune therapy.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Concept: S Kim, Design: S Kim, Materials: S Kim, SW Ra, HJ Cha, Writing manuscript: S Kim, Critical review: SW Ra, HJ Cha, S Lim.
Informed Consent
The authors obtained the approval of the institutional review board of the Ulsan university hospital for this case report and patient consent was secured to publish this study.
