Abstract
Migration of foreign bodies into the heart, although unusual, has been reported since 1834 when Davis published the first bullet embolus. Our case was a 29-year-old woman who suffered from a grenade explosion wound with a residual burst fragment inside her arm soft tissue. Two months later, she was admitted with progressive fatigue, palpitation, shortness of breath, and swelling in legs and neck. She was taking hormonal therapy for infertility as medical history. Ascultation detected holosystolic respiratory variable murmur maximal over the left lower sternal border. Severe tricuspid regurgitation and an obliterating mass on tricuspid valve (TV) with characteristic of central linear echogenicity were detected by transthoracic echocardiography. The diagnosis of “the embolized missile into heart with superimposed thrombosis” was determined. The patient underwent open heart surgery and the thrombotic rod shape chip that was embedded in anterior tricuspid leaflet was removed and then TV was repaired.
Keywords
Introduction
Foreign bodies traveling through the major veins to the heart are rare according to what Davis published, “The first bullet embolus to heart in 1834. 1 Progressive proximal movement of foreign body (FB) should alert the clinicians to the possibility of its migration in the vein. 2 Due to the direction of blood flow, intravenously FBs can easily cause lethal pulmonary embolisms (PEs), while arterial FBs can cause limb necrosis.3,4
Clinical Summary
Our case is a 29-year-old nulliparous woman presented to the emergency department with a grenade explosion wound on her right arm. She had sustained an open wound and proximal humeral fracture. The patient ultimately underwent surgical plating. After suitable treatment, she was discharged. On the next week of follow-up, the X-ray showed a harm ended needle shape (3×12 mm) high-density shadow in the arm soft tissue as a residual fragment of burst. She was admitted in our service 2 months later, with progressive fatigue, palpitation, shortness of breath, and swelling in legs and neck. On further exploration of her medical history, she identified infertility as medical history, and to treat this condition she was taking clomiphene citrate and gonadotropin-releasing hormone (GnRH) for the past 5 months. Physical examination revealed jugular venous pulse elevation, hepatomegaly, and holosystolic respiratory variable murmur maximal over the left lower sternal border (Rivero-Carvallo’s sign). Transthoracic echocardiography disclosed mean pressure gradient across tricuspid valve (TV) about 10 mmHg, central jet area about 11 cm2 and systolic reversal flow in hepatic vein which conformed with severe tricuspid regurgitation. It also revealed a mass at TV level with characteristics of central linear echogenic entity (Figure 1). Fluoroscopic evaluation revealed the restricted motion with approximately semiopen position of the TV leaflets. It also showed paradoxical ventricular septal motion, shift of the atrial septum toward the left atrium, and a sessile Echogenic mass (thrombus) attached to the atrial side. A multidetector heart computed tomography uncovered abnormal high-density linear structure at the TV level. Doppler ultrasonography ruled out deep vein thrombosis (DVT) and perfusion pulmonary scan precluded PE. Presence of the projectile particle inside the arm tissues in previous X-ray and its absence in the recent images (Figure 2) raised the index of suspicious of “the embolized missile to heart that was complicated with thrombosis.” Most likely the grenade fragment entered blood stream via the right cephalic vein and then migrated proximally toward the heart. With the diagnosis of TV foreign body with superimposed thrombus, the patient was administered 250 000 IU streptokinase by intravenous route followed by 100 000 IU hourly. In spite of decreasing in thrombus size, after 2 days the investigations revealed no improvement in the leaflet’s motions. Therefore, decision was promptly made to remove the particle. After median sternotomy and vertical pericardiotomy, cardiopulmonary bypass using ascending aortic and bicaval cannula was established. Aorta was cross-clamped and antegrade cardioplegia was administered. The right atrium was opened and a clot covered cylindrical structure about 23×14 mm was found that had deeply embedded itself in the anterior TV leaflet (Figure 3). The operation also identified the finding which included a torn anterior common chordae and an incompetent semiopen and perforated anterior leaflet accompanied by mild dilated annulus. The common chordate was implanted to anterior papillary muscle and leaflet was repaired using pericardial patch. The De Vega technique was carried out using No: 2-0 polyester suture beginning from posteroseptal commissure in a counterclockwise direction to the anteroseptal commissure and was reversed in clockwise direction to the first point. We used a strip of autologous pericardium in the suturing process for additional stability. An acceptable coaptation of leaflets was achieved by regurgitation jet saline test. Intraoperative transesophageal echocardiography did not detect any paradoxical ventricular septal motion or shift of atrial septum. It also revealed maximum TV annulus circumference about 12 cm without any regurgitation through it. Aortic cross-clamp time was 56 minutes. During 6-month follow–up, the patient was complete symptom free, and function of TV was in satisfactory range without regurgitation.
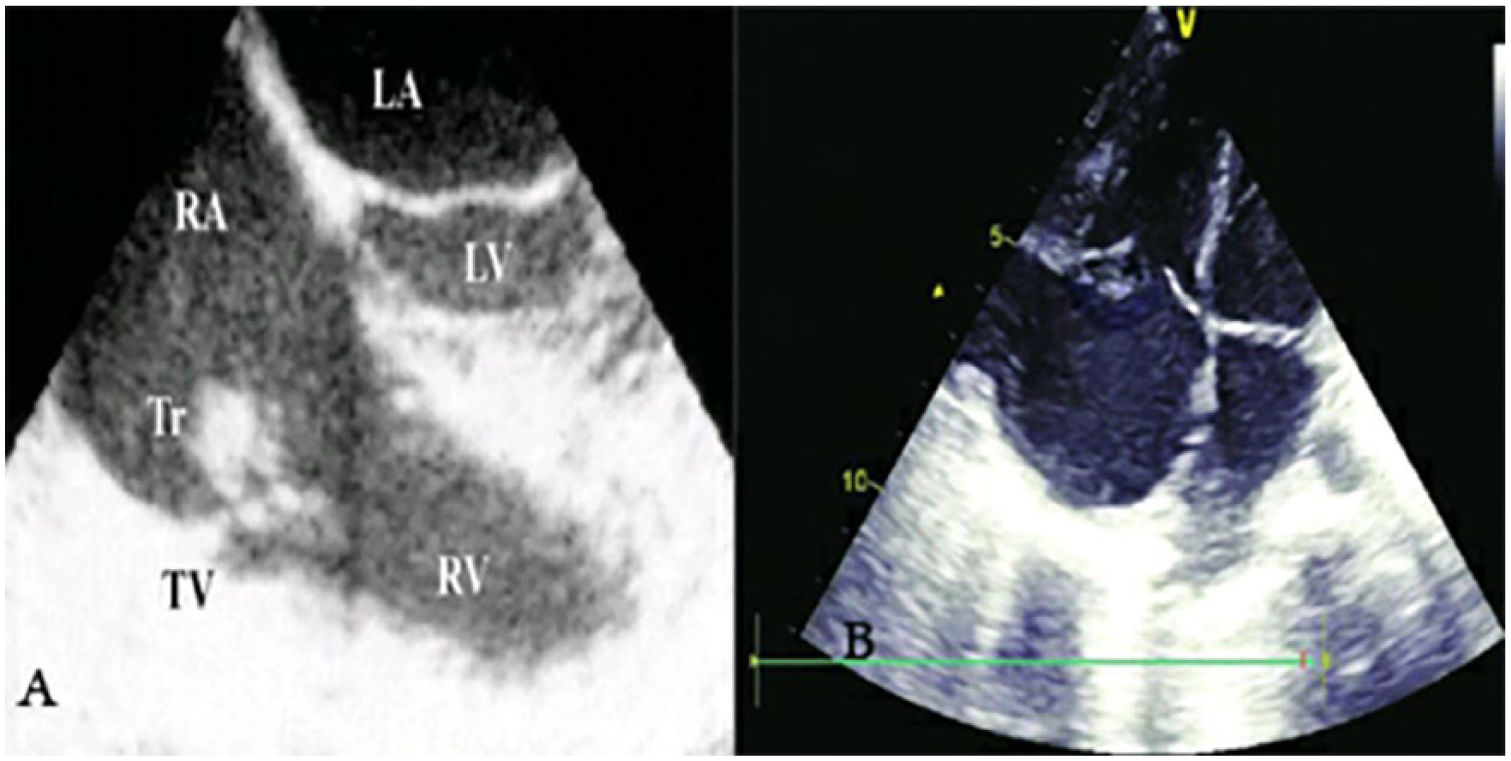
Transesophageal echocardiography showed sessile echogenic mass (thrombus) attached to the atrial side of the tricuspid valve: (A) Transthoracic echocardiography demonstrated a central linear echogenic mass at TV level and (B) Fluoroscopic evaluation revealed the restricted motion with approximately semiopen position of TV and a sessile echogenic mass on the atrial side. LA, Left Atrium; RA, Right Atrium; LV, Left Ventricle; RV, Right Ventricle; TV, Tricuspid Valve
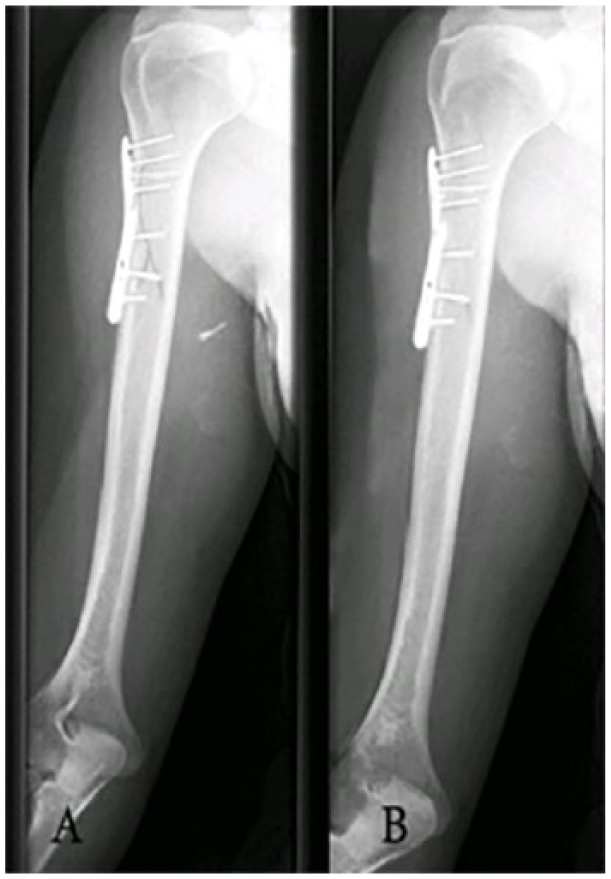
Present and disappearance of grenade burst fragment on right arm X-ray: (A) a week after explosion; (B) 2 months after explosion.
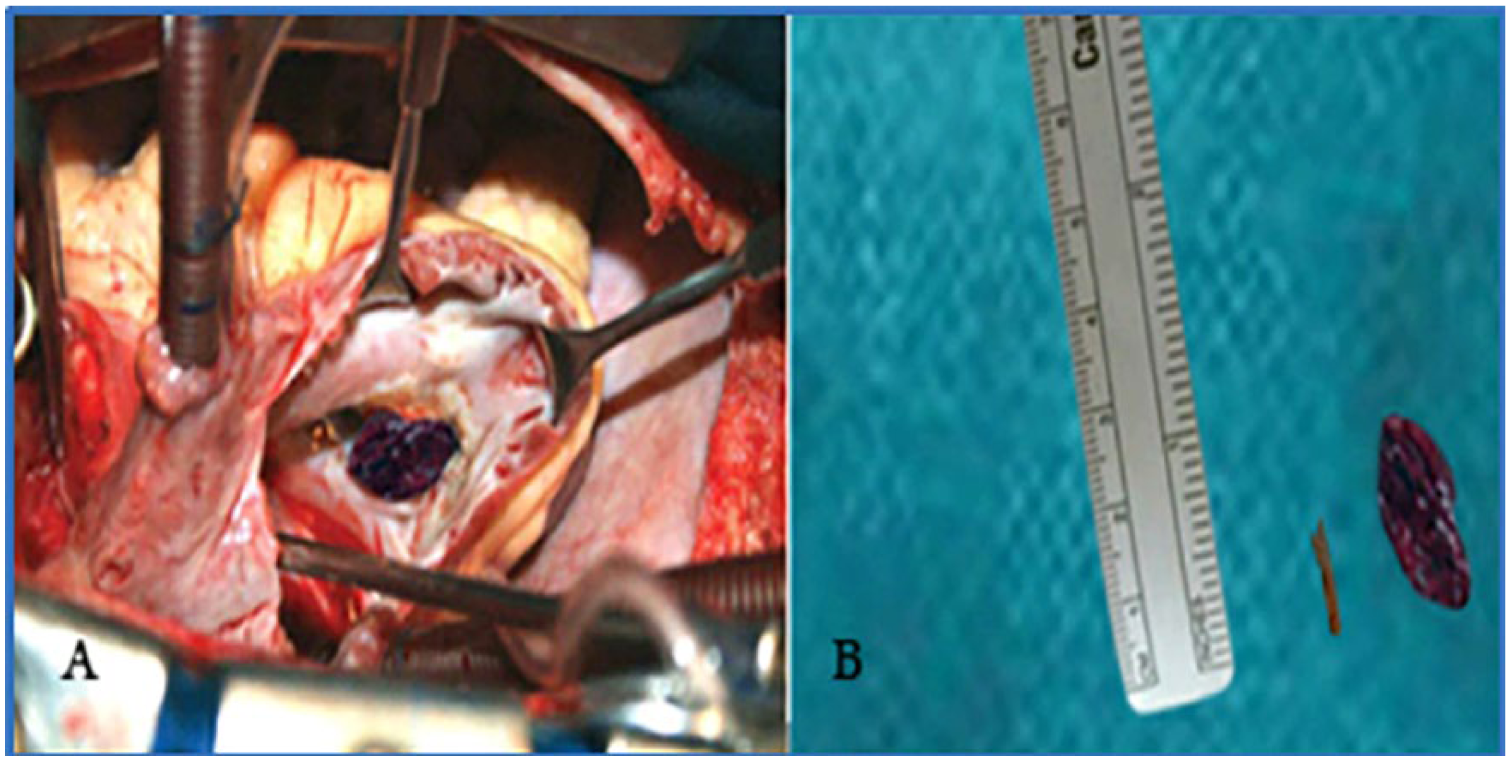
Twenty-nine-year-old woman with foreign body (FB) embolization to heart: (A) thrombotic FB anchored to anterior leaflet of tricuspid valve; (B) removed thrombus and its burst chip nidus.
Conclusion and Discussion
In this report, the grenade chip started its displacement in the subcutaneous tissue and eventually found its way through the cephalic vein toward heart. The particle anchored itself to the edge of anterior TV leaflet via its branched end followed by fixation and thrombus formation. All laboratory investigations for probable hypercoagulable diseases such as rheumatologic disorders were negative. The only precipitating iatrogenic state for thrombosis was GnRH therapy. However, regarding Rudolf Virchow criteria, the patient had already met the criteria to become more susceptible to TV thrombosis. These conditions were endocardial erosion due to deep penetration of foreign body in anterior leaflet, right cardiac side low blood flow velocity in the setting of hypercoagulability status owing to hormonal therapy besides the thrombogenic effect of retained grenade fragment as Alvarez and colleagues reported in 2018. As it is stated in the literature, the incidence of prosthetic valve thrombosis (PVT) is 0.5% to 6% in the aortic and mitral positions, whereas up to 20% in tricuspid position. 5 We encountered a case who instead of an artificial valve had retained a lead fragment into right side of the heart followed by an ongoing obliterating thrombotic process . The management of Intracardial foreign body has been controversial due to confined reports until now. It has been reported a bullet, a sewing needle, an acupuncture needle, as well as welded metal and orthopedic hardware migrating through the veins to heart.6–8 However, it came to our attention that our case is the first report in which an explosion fragment embedded adjacent to cephalic vein was later found attached to TV whereas perpetrated in creating a nidus for thrombus formation followed by TV incompetency.
Footnotes
Acknowledgements
The authors wish to thank Professor Zahra Sepehrmanesh, Dr Soroush Sarmast, and Dr Behina Sarmast for their assistance in this study and Dr Kevin Brady and Dr Fariba Brady from New Jersey for their editorial assistance.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: As we are from lower income country, the processing charge has been waived.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Both authors (Prof.Dr.Ahmad Takriti and Dr.Hossein Sarmast) performed the operation and collected the clinical data.Dr.H.Sarmast wrote the manuscript and Prof.Dr.A.Takriti revised and edited it.Both authors read and approved the final manuscript.
Availability of Supporting Data
The datasets during the current study available from the corresponding author on reasonable request and for this purpose, the author received written consent from patient.
Consent for Publication
Written consent for publication was obtained from patient.
Ethical Approval and Consent to Participate
In 2018, the ethics committee was held in the Cardiac Surgery Hospital of Damascus University and Department review board approval to publish a case report study entitled “Tricuspid valve incompetency due to the grenade chip embolization to the heart” was obtained. As well as written consent was received from patient.
