Abstract
We present a case of a flush chronic total occlusion of the superficial femoral artery treated successfully with a combined antegrade approach using radial access and a retrograde approach using a pedal access. Patient has total occlusion of the contralateral left external iliac and common femoral artery. Our case illustrates the feasibility of the combined pedal-radial approach in treating flush occlusions of the superficial femoral artery.
Keywords
Introduction
Femoral access has been widely used to treat iliac and infrainguinal disease. Recently, pedal or radial access has gained more acceptance among endovascular specialists particularly in patients with critical limb ischemia. We report a case of combined pedal-radial access to treat a flush occlusion of the right superficial femoral artery in a patient with contralateral occlusion of the left femoral artery.
Case Report
The patient is a 52-year-old man with history of severe peripheral arterial disease status post amputation above the knee (AKA) on the left with a non-healing left stump wound and right lower extremity ulcerations. Patient has a long-standing history of type 2 diabetes mellitus and continues to smoke. He was referred for consideration of revascularization given his nonhealing wounds. Our institutional Review Board does not require informed consent or ethics approval for case reports.
Patient underwent a peripheral angiogram from a right common femoral artery (CFA) access site. He was found to have a long occlusion from his mid to distal left external iliac artery into his CFA and proximal left superficial femoral artery (SFA). His right SFA also had a flush total occlusion. The right SFA occlusion extended to the distal portion of this vessel with reconstitution of the popliteal from the profunda femoris (PF). The right tibioperoneal artery was severely diseased and the posterior tibialis artery was totally occluded above the ankle. The right anterior tibialis was patent to the foot and had no significant disease. The proximal left external iliac artery underwent stenting from the contralateral approach at a site of severe 90% lesion at its origin. This vessel was feeding collaterals to his left stump. Patient returns in a few days for staged treatment of his right flush occluded SFA at its origin. Access site from the contralateral occluded left CFA was not possible. A dual access from the right radial artery and right dorsalis pedis (DP) artery was planned. Our case illustrates the feasibility of the radial access approach for peripheral angioplasty using long wires and balloons and shows the feasibility of the pedal-radial access for the treatment of a flush occlusion of a chronically occluded SFA.
Procedure
The right DP was accessed using a micropuncture needle under ultrasound guidance. A 6F Glidesheath Slender (Terumo) was placed into the right DP. A total of 400 µg of intravascular nitroglycerin was administered via the pedal sheath. Also, a total of 4000 units of intravenous heparin was administered. The radial artery was then accessed with another 6F Glidesheath Slender and the long Wholey wire was advanced from the right radial sheath into the distal abdominal aorta over a 110 cm pigtail catheter. Abdominal aortogram was performed with iliac runoff noting flush occlusion of the right SFA at its origin and occlusion of the left external iliac and left CFA.
Using the Wholey wire, the short 6F Slender sheath was exchanged with a 118 cm long destination sheath (Terumo) placed in the distal aorta. The Wholey wire was then exchanged for a 400 cm 0.035″ stiff angled glidewire (Terumo) and introduced initially into the PF artery. A 150 cm glide catheter (Terumo) was then placed over the 400 cm wire and advanced to the right PF where an injection of contrast was performed to visualize the reconstitution of the right SFA and outflow vessels distally by collaterals (Figure 1). The catheter was then pulled out into the right CFA for dye injection. The angled 150 cm NaviCross catheter (Terumo) was advanced from the pedal sheath with a 260 cm Glidewire Advantage (GWA) (Terumo) to cross the distal cap of the right SFA occlusion (Figure 2A). The pedal catheter and wire were advanced to the proximal SFA and the wire was noted to be in the subintimal space and could not cross into the right CFA despite the use of multiple wires (including 0.018″ Astato (Asahi) and V-18 (Boston Scientific) wires). The 400 cm wire from the radial approach was then able to go beyond the proximal cap with the aid of the NaviCross catheter and advanced intraluminally to the right popliteal. The monorail 200 cm length, 5.0 mm × 100 mm MetacrossRX balloon (Terumo) was then used to dilate the totally occluded right SFA. The V-18 wire was then advanced retrogradely from the pedal sheath into the true right CFA lumen into the distal aorta. Two 6 mm × 100 mm Zilver PTX (Cook) drug eluting stents were placed from the origin of the SFA to the medial SFA followed by a Lutonix (Bard) drug-coated balloons to the distal SFA. There was less than 5% residual narrowing seen in the SFA post treatment. The right CFA was then dilated with 6.0 mm × 60 mm Lutonix balloon for 3 min at 8 atm. A type C dissection was seen in the right CFA and an 8.0 mm × 80 mm Lifestent (Bard) was placed in the proximal 1/3rd and mid 1/3rd of right CFA via the pedal approach yielding 0% residual narrowing. The distal 1/3rd of the right CFA was not stented. Stents were post dilated with a 6.0 mm balloon (Figure 2C). The radial sheath was then pulled and hemostasis achieved with a TR wrist band (Terumo). The pedal sheath was removed and hemostasis was carried on with manual compression. Excellent pulses were seen in the right radial and right pedal post treatment.
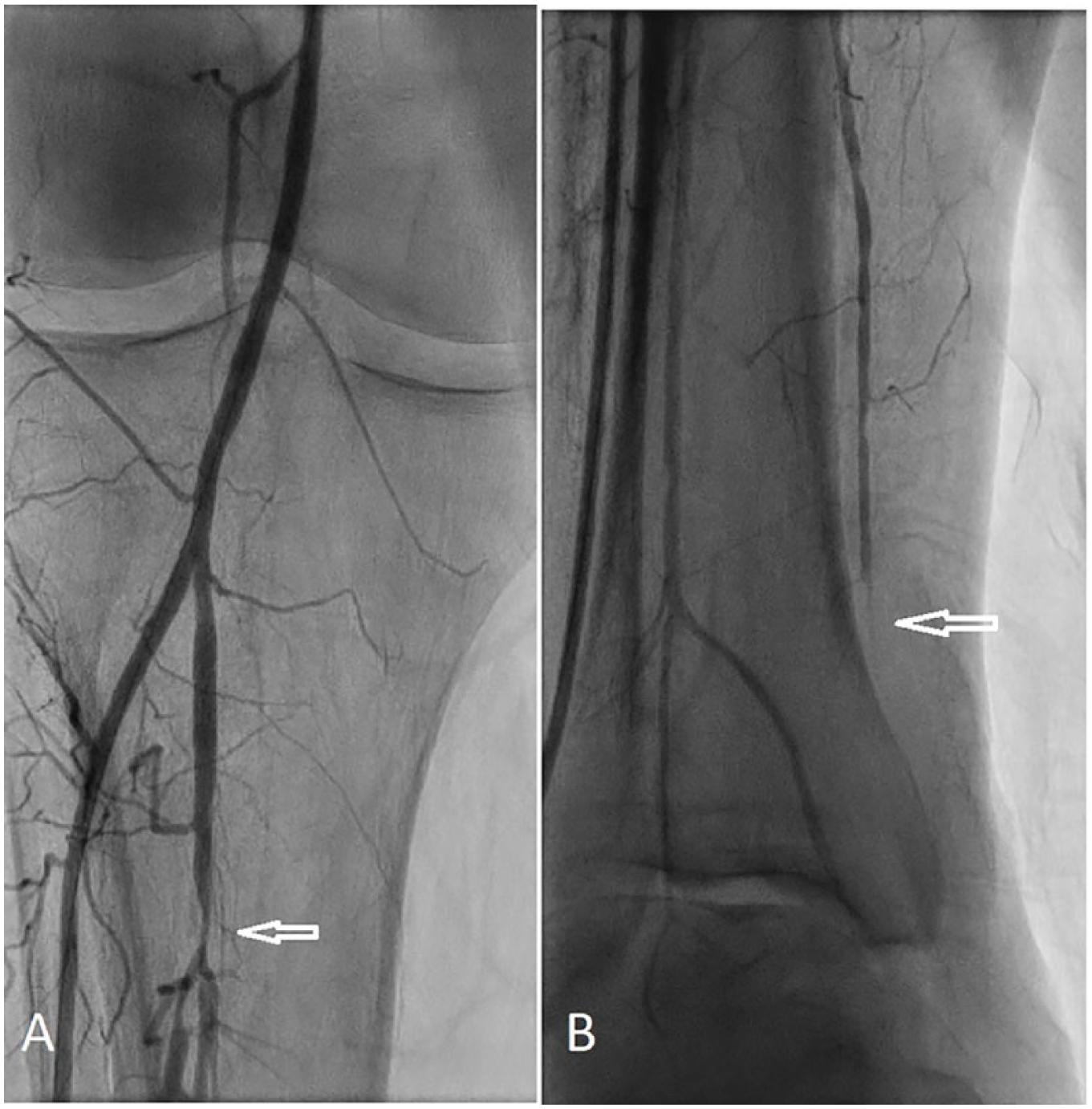
Pre-intervention baseline outflow anatomy visualized from above (A) and from a retrograde injection via pedal access (B). Arrow in (A) shows severe right tibioperoneal disease. Arrow in (B) shows occlusion of the right posterior tibialis above the ankle.
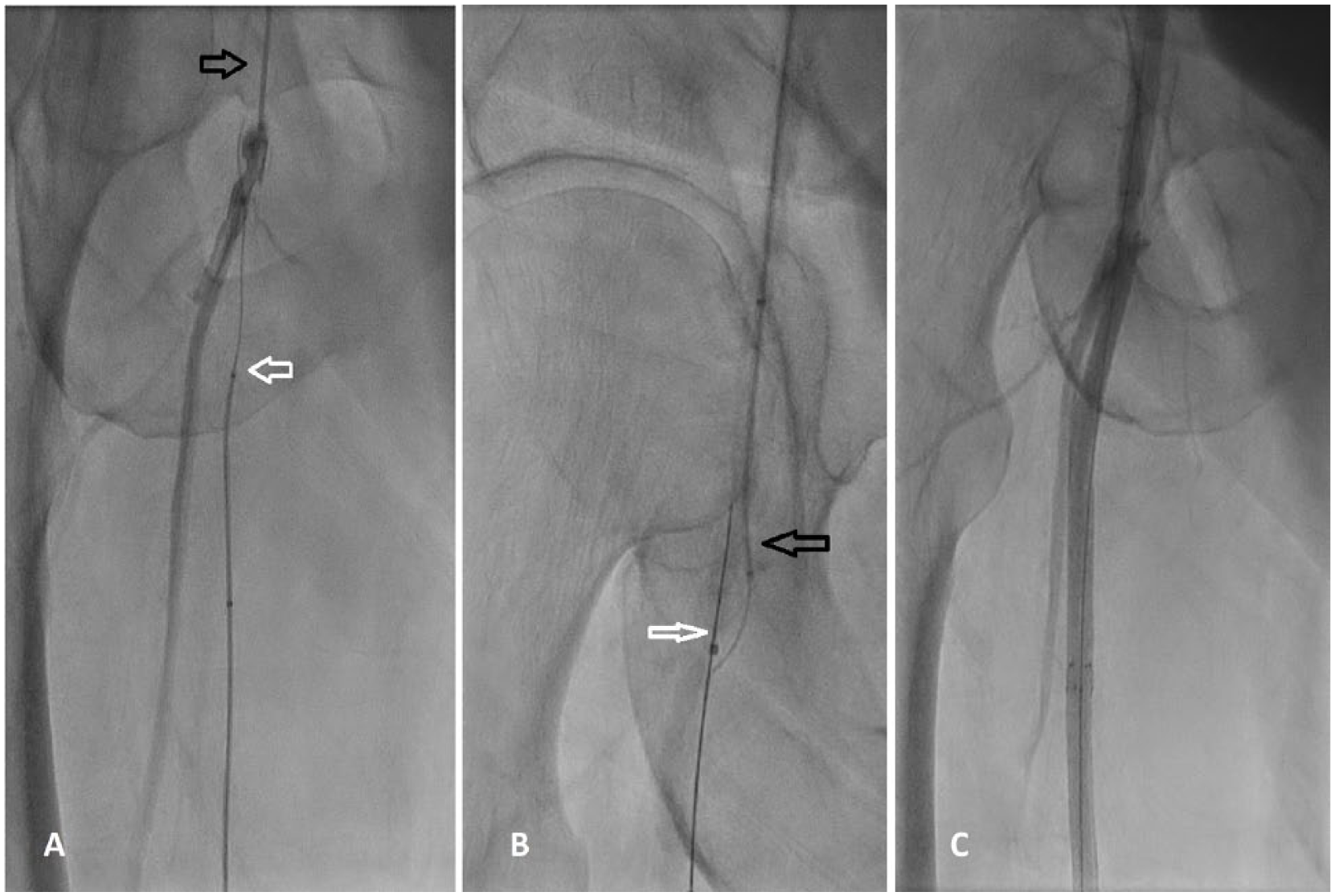
(A) Antegrade angiogram from catheter using a radial access (dark arrow) showing the occluded right superficial femoral artery at its origin and the patent profunda femoris artery. Catheter and wire from the retrograde pedal approach is also shown (white arrow) and wire is subintimal into the right femoral artery. (B) Wire and catheter crossing the proximal SFA antegradely (dark arrow). The position of the origin of the SFA has been facilitated by the presence of a catheter and wire close to the origin from the retrograde approach. (C) Final treatment of the SFA and CFA with excellent results.
Discussion
In patients with critical limb ischemia, revascularization is essential for limb salvage. Pedal access has been used successfully with excellent safety profile.1–3 However, visualization of the artery and crossing the lesion from a retrograde pedal approach remain challenging particularly when treating a flush occlusion of the SFA at its origin. Approaching and visualizing of the artery proximal to the lesion is important to (1) visualize the bifurcation of the right common femoral and the PF arteries; (2) provide access to cross the lesion from an antegrade or antegrade/retrograde dual approach; and (3) provide access to protect the right PF artery when crossing and treating the origin of the SFA.
Typically, a contralateral access from the CFA is performed to secure this antegrade approach. However, in our patient, this was not possible since the contralateral CFA was totally occluded. A brachial approach was feasible but this access is associated with a sizable risk of complications. A radial approach is ideal but until now long wires, sheaths, and balloons to reach the distal SFA from the wrist were not available in the United States. The recent release of the new long radial tools for peripheral angioplasty in the United States offers an opportunity to effectively start peripheral angioplasty using radial access. Currently, this approach is limited to the availability of long wires (400 cm), long crossing catheters (180 cm), and long balloons (200 cm). Long drug-coated balloons and stents are not yet available in the United States for distal infrainguinal endovascular treatment from a radial access but have been available outside the United States. In our case, a pedal access was needed for a retrograde attempt to cross the total occlusion and to allow drug eluting stents and drug-coated balloon delivery to the target lesion. Although crossing the total occlusion from a pedal access was not successful, this approach allowed the identification of the origin of the SFA occlusion facilitating the crossing from the radial access. It is possible that in certain cases, the use of Goose Neck snares (Medtronic) may be needed to capture the radial wire from the pedal access but this was not necessary in our case.
The transradial approach to lower extremity interventions has been reported initially in a few case reports and small series showing that it is safe and with high success rate.4–9 A transradial approach allowed the treatment of bilateral iliac or SFA arteries in the same setting and was thought to be feasible as a first line access in suprainguinal interventions. Recently, Lorenzoni et al 10 reported in a prospective study of 110 consecutive patients (170 lesions) the feasibility of using the transradial approach to treat both suprainguinal and infrainguinal lesions. Occlusions were present in 22% of patients with a technical success rate of 91% in all lesions and 63% success rate in total occlusions. Access artery occlusion occurred in 18 (16%) patients with no discomfort. Also, Roy et al 11 reported a retrospective single center experience with transradial access for peripheral arterial interventions. In 188 patients (210 lesions) who underwent aortoiliac (62.4%) or femoropopliteal (37.6%) interventions, the radial access was used in 65 procedures. There were no significant differences found between CFA access and radial access in procedure time and length of stay. Access site complications occurred in 6.0% of CFA vs 3.7% of radial access (P = .12). Recently, Patel et al 12 reported on 184 SFA chronic total occlusions (CTO) interventions in 161 patients treated with transradial or transpedal approach. Primary transradial approach was used in 46 patients (47 lesions). Primary crossing success rate was higher with transradial compared with transpedal (74% vs 54%, P = .01).
The addition of a pedal approach to radial approach was recently described in a series of 15 patients with long total occlusions and unfavorable anatomy, flush occlusions, or calcified distal reconstitution. 13 Of the 15 patients, 7 required pedal-radial rendezvous to facilitate retrograde crossing. Treatment was successful in all patients and no complications reported. Ruzsa et al 14 reported data on 145 consecutive patients with symptomatic SFA treated via primary radial access with secondary access achieved through the pedal or popliteal artery. Combined radial and pedal access was performed in 15.1% of patients. CTO was present in 63 patients. Success rate was 90.4%. Access site minor complications occurred in 4.8%. Finally, Patel et al 12 used a dual transradial-transpedal approach in 72 patients with uncrossed lesions with either approach alone, resulting in a crossing and procedural success of 99% and 96%, respectively. Our case adds to the body of evidence that a dual pedal/radial access is feasible to treat flush occluded long SFA lesions in patients with critical limb ischemia and no alternative access.
Limitations
The radial approach is not without limitations when it comes to peripheral interventions. Tortuosity of the innominate artery or the aorta, planned hemodialysis, and upper extremity occlusive disease can be a hindrance to treat the lower extremities from a radial access site. Also, longer fluoroscopy times have been reported with a radial approach when compared with a femoral approach. In addition, sheath size is a limitation to a radial access and potentially limits the use of certain devices. There are conflicting reports to potential complications using transradial access and ranging from none to about 18% and mostly related to radial artery occlusion and dissection. A radial access however resulted in shorter hospital stay. Furthermore, a radial access may not provide enough wire or balloon support unless the sheath reaches the iliac arteries. A 118 cm Destination sheath (Terumo) is now available in the United States. A long sheath extending from the wrist to the iliac arteries for a prolonged period of time may increase the risk of thrombosis of the right subclavian and its runoffs. Maintaining an activated clotting time between 250 and 300 s is particularly important with a radial access using long sheaths. Finally, a combined pedal-radial access increases the success rate to recanalize total occlusions. The use of pedal access however can be associated with access site complications and can have severe consequences in patients with single runoff to the foot. However, this can be justified when no other access is feasible in patients with critical limb ischemia and at high risk of amputation. Another advantage of having a pedal access is also to treat potential distal embolization that may occur during intervention from a radial access. Further studies are needed to determine the routine use of a radial-pedal access in patients with peripheral arterial disease. At this time, this approach may be limited to select cases of limb salvage.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
Dr Shammas receives research and educational grants from Boston Scientific, Intact Vascular, and Bard. Dr Radaideh has no conflict of interest.
Author Contributions
NWS is the operator in this procedure and wrote the case procedural details. QR is the cardiology research fellow who conducted an extensive review of the literature on the topic and wrote the preliminary early manuscript. Both reviewed and agreed to the final manuscript version.
