Abstract
Background:
Bilateral internal mammary arteries (BIMAs) remain underused in coronary artery bypass grafting (CABG), especially in elderly, diabetic, and obese patients. This study investigated incidence of sternal wound infection (SWI), sternal instability (SI), and reintervention for bleeding (RIB) in this high-risk population.
Methods:
A single-center retrospective observational study was performed in “Grand Hôpital de Charleroi, Gilly, Belgium.” A total of 319 patients undergoing CABG from December 2011 to December 2015 were included. Three main outcome measures (SWI, SI, and RIB) were investigated in obese vs nonobese, diabetic vs nondiabetic, and elderly vs younger patients.
Results:
In all, 14 SWI, 11 SI, and 6 RIB were discounted. Death rate was as follows: SWI: 2/14 vs 17/305 (P = .178), SI: 2/11 vs 17/308 (P = .081), and RIB: 2/6 vs 17/313 (P = .004). In obese (n = 113) vs nonobese (n = 206) patients, there was no difference for SWI (P = .263), SI (P = .565), and RIB (P = .332). In diabetic (n = 118) vs nondiabetic (n = 201) patients, there was no difference for SWI (P = .642), SI (P = .497), and RIB (P = .298). In elderly (n = 62) vs younger (n = 257) patients, there was no difference for SWI (P = .619), SI (P = .915), and RIB (P = .385).
Conclusions:
Obesity, age, and diabetes treated by insulin (or not) do not seem to be risk factors for developing SWI, SI, or RIB in patients receiving a CABG using BIMA. Nevertheless, mortality was higher in RIB group.
Keywords
Introduction
Coronary artery bypass grafting (CABG) is one of the most common cardiac surgical procedures over half a century.1,2 The left internal mammary artery (LIMA) graft is the gold standard of CABG. 2 The use of a saphenous vein in CABG was very successful in the 1970s and 1980s due to numerous advantages: easier harvesting and handling, high procedure reproducibility, and good outcomes. 3 Suzuki et al 4 published the first report about bilateral internal mammary artery (BIMA) to revascularize coronary arteries in Circulation in 1973. The common use of LIMA as a conduit to left anterior descending artery appears after the Landmark Paper from the Cleveland Clinic group, reporting good surgical outcomes at 10 years. 5 Progressively, despite superior results of BIMA grafting,6,7 this technique remains generally underused: 20% in Europe, 8 ≤4.5% in the United States,8,9 12.6% in Australia, and approximately 30% in Japan. 9 The main common reasons discouraging surgeons in using BIMA grafting are technical challenges, longer operating time, and higher incidence of SWI.8,10 Even in studies promoting the use of BIMA, there are often restrictions concerning diabetic patients (DM), 11 elderly patients (EP) (and their propensity to co-morbidities), 12 and obese patients. 13 The risk of SWI and sternal complications due to the higher sternal devascularisation in these high-risk categories tends to avoid them for BIMA grafting procedures.11–14 This study aims to convince surgeons about the safe use of BIMA even in these categories.
Patients and Methods
Patients
A single-center retrospective observational study on 319 patients undergoing CABG made in our center (Grand Hôpital de Charleroi, Gilly, Belgium) from December 23, 2011, until December 27, 2015, was included. Coronary artery bypass grafting using BIMA and one or more additional grafts were only included. Surgical procedures using a single internal mammary artery (SIMA) were excluded from the study. The presence of an SWI was defined by the criteria of the Centers for Disease Control and Prevention 15 : (1) an organism isolated from culture of mediastinal tissue or fluid, (2) evidence of mediastinis seen during operation, or (3) presence of chest pain, SI, or fever (>38°C), and purulent drainage from the mediastinum, isolation of an organism present in a blood culture, or culture of the mediastinal area. Distinction was made with isolated SI defined by separation of the sternum at the midline due to bony fracture or disruption of the wires. 16 Patients ≥75 years were considered EP. Diabetic patients were separated into those who required or not insulin therapy. Obesity was defined by body mass index (BMI) ≥30 kg/m2. Risk factors as arterial hypertension (HTA), defined as grade I or higher hypertension (systolic 140-159 mm Hg and diastolic 90-99 mm Hg), 17 chronic kidney disease (serum creatinine >2 mg/d), and cerebrovascular disease (CVD) were mentioned. Status of chronic obstructive pulmonary disease (COPD) of the patients was also taken into account. Inclusion criteria include every patient submitted to a CABG using both mammary arteries (with or without some additional grafts) whatever the angiographic findings or the presence of the risk factors above mentioned. Procedures using only saphenous graft, radial graft, or only one mammary artery for coronary revascularization were excluded from the study. This study required no ethical approval after revision by our hospital ethics board.
Surgical procedure
Every patient was submitted to the same surgical BIMA harvesting and sternal closure by the same operator. All patients were disinfected with dermic isobetadine (iso-Betadine Dermique, 10% solution, polyvidone iode) on their whole body. A lateral drape with plastic protector was used. All procedures were performed via median sternotomy. No bone wax was used. Mammary arteries were harvested in a nonskeletonized fashion using an electrosurgical scalpel. The BIMAs were prepared with physiologic saline (0.9% NaCl, sodium chloride physiological solution; BioUltra, tablet, 100 cm3) mixed with papaverine (1.5 cm3). Combinations and numbers of arterial bypasses were selected according to the angiographic findings. All the patients operated during that period and who needed 2 grafts received LIMA and right internal mammary artery (RIMA), independently of age, diabetic status, or obesity. A radial or saphenous graft was used as a third graft if necessary. Radial grafts were harvested by endoscopy. The RIMA was used as free graft on LIMA in 228 patients (71%) and as in situ graft in 91 patients (29%). Some interventions included concomitant cardiac or aortic surgical procedures as valve replacement (21 aortic valve replacement, one mitral valve replacement), 5 carotid endarterectomies, 2 closures of oval foramina, or 2 Maze interventions. To make the sternotomy closure, the same procedure was always used, using double and single sternal wires. The wires were passed through the sternum approximately 1 to 1.5 cm lateral to the midline through intercostal spaces. A rotary movement of the wrist along with a vertical pull on the wires was used to twist the wires tightly until the 2 bone edges were close to one another. Three double sternal (DoubleWire; A&E Medical Corp, Farmingdale, NJ, USA) and 3 single sternal wires were used (SingleWire; A&E Medical Corp). The double sternal wire was placed with the double wire twister. Subcutaneous tissue was closed with polysorb 0 and the intradermic plan was made with rapid vicryl.
Statistical analysis
The continuous variables were tested for normality using the Shapiro-Wilk test. The continuous variable being non-Gaussian, the nonparametric Wilcoxon-Mann-Whitney test was used to compare EuroSCORE II, age, and BMI. The discrete variables were tested using the χ2 test. A P value of <.05 was considered significant.
Results
We included 319 patients, 258 men (81%) and 61 women (19%). The median age was 65 years (range from 39 to 86 years). There were 234 patients with HTA (73%), 118 patients were DM (37%), of whom 28 were treated by insulin (9%). There were 32 patients COPD (10%) and 29 patients with renal failure (9%). The median BMI was 29 kg/m2 (range from 17 to 45 kg/m2). Extracorporeal circulation (ECC) was used in 228 patients (71%) and 91 CABGs were done off-pump (29%). In all, 26 patients had CVD (8%) and 19 patients died (6%). A total of 1161 distal arterial anastomoses were made: 228 proximal arterial anastomoses and 47 distal venous anastomoses. The mean EuroSCORE was 4.9.
Three main outcomes were evaluated: SWI (group 1), SI (group 2), and RIB (group 3), using the above defined criteria.
In group 1, 14 patients on 319 patients were recorded (4%). The mean age was 67 years (range from 49 to 86 years). Only 2 patients were considered as EP (14%). The mean BMI was 28 kg/m2. Mean EuroSCORE was 5.8. Six patients had 3 distal arterial anastomoses and 13 patients had 1 proximal arterial anastomosis. Only 1 patient had 2 distal venous anastomoses. One radial graft was harvested in this group. Teen CABGs were made under ECC. Seven patients had an SI associated (50%). When comparing with patients without SWI, all comparisons in subgroups were nonsignificant for SWI. In this study, SWI was not a risk factor in these categories. Data are recorded in Figure 1.
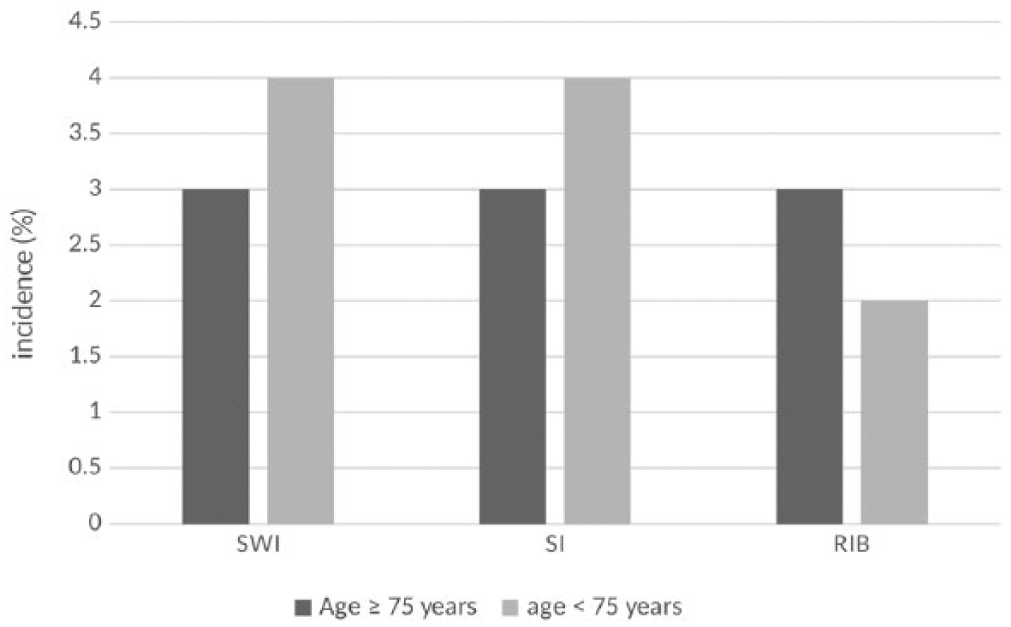
Outcomes in elderly persons. In this group, there was no difference for SWI (P = .619), SI (P = .915), and RIB (P = .385). Incidences of SWI, SI, and RIB were equal: 3% (2/62). In the younger population, incidence of SWI was 5% (12/257), SI 4% (9/257), and RIB 2% (4/257). RIB indicates reintervention for bleeding; SI, sternal instability; SWI, sternal wound infection.
In group 2 (Figure 2), 11 patients (3%) were recorded. The mean age was 67 years (range from 51 to 76 years). Two patients were EP (18%). The mean BMI was 29 kg/m2. Every patient had 1 proximal arterial anastomosis. One distal venous anastomosis was made on 3 patients. The biggest number of distal arterial anastomosis was 6 on 2 patients. One radial artery was harvested in 1 patient. Dead patients were not the oldest ones. The mean EuroSCORE was 4.4. Four patients had an SWI associated (36%).
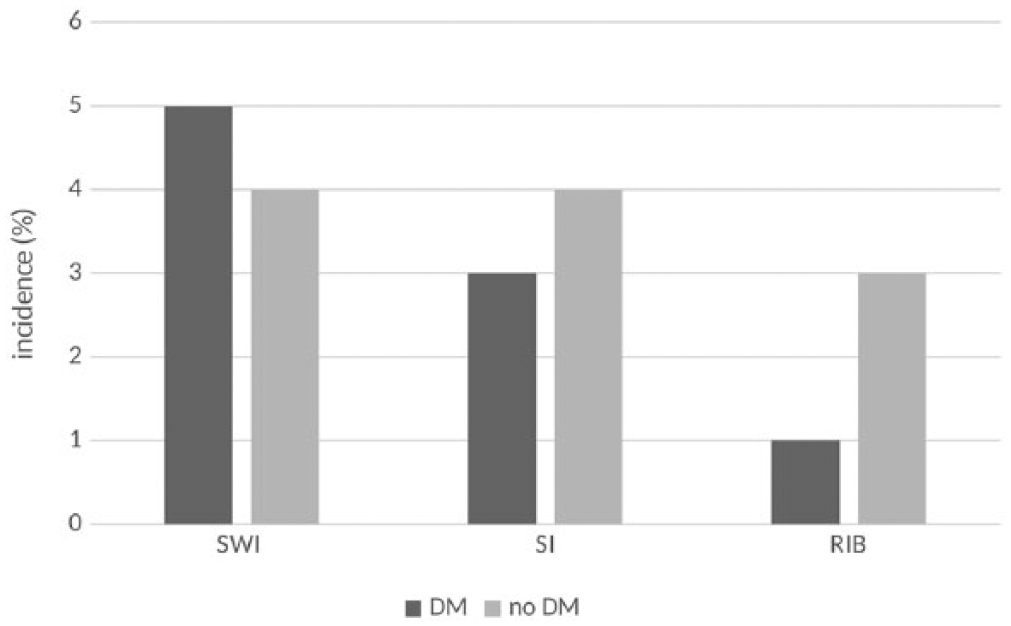
Outcomes in patients with DM. No differences were noted between SWI, SI, and RIB. In DM, incidence of SWI was 5%, SI 3%, and RIB 1%. In no DM, incidences of SWI and SI were 4% (8/201) and RIB 3% (5/201). DM indicates diabetes mellitus; RIB, reintervention for bleeding; SI, sternal instability; SWI, sternal wound infection.
Six patients were counted (2%) in group 3 (Figure 3). Every procedure was made in early postoperative period (48 hours postsurgery). The mean age was 66 years (range from 56 to 78 years), with 2 EP (33%). The mean BMI was 28 kg/m2. Twenty-five distal arterial anastomoses and 6 proximal arterial anastomoses were made. No distal venous anastomosis was made. One patient had an SI associated (17%) and no SWI was recorded in this group. Mean EuroSCORE was 12.8. Incidence of death was more than 6 times higher in patients with RIB (P = .004).
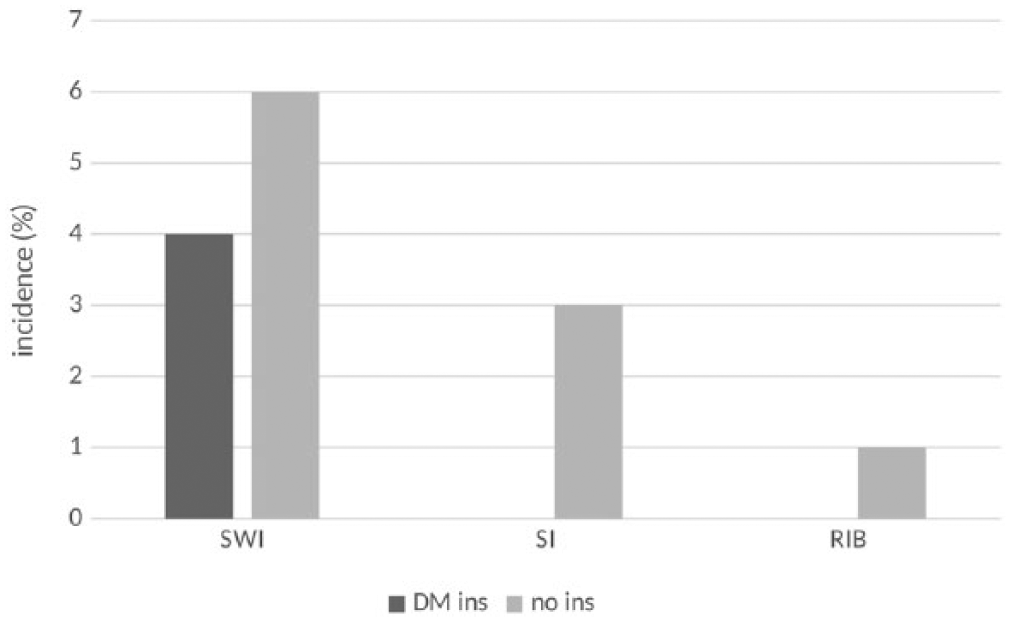
Outcomes in patients with DM with or without insulin. In this subgroup, treatment by insulin or not is also nonsignificant: SWI (P = .677), SI (P = .328), and RIB (P = .575). In insulin-treated DM, incidence of SWI was 4%, without SI or RIB. Without insulin treatment, incidence of SWI was 6% (5/90), SI 3% (3/90), and RIB 1% (1/90). DM indicates diabetes mellitus; RIB, reintervention for bleeding; SI, sternal instability; SWI, sternal wound infection.
Outcome analyses by categories obese vs nonobese patients, DM vs no DM, and EP vs younger patients are resumed in Figures 1 to 4. Characteristics of each subgroup are resumed in Tables 1 to 3.
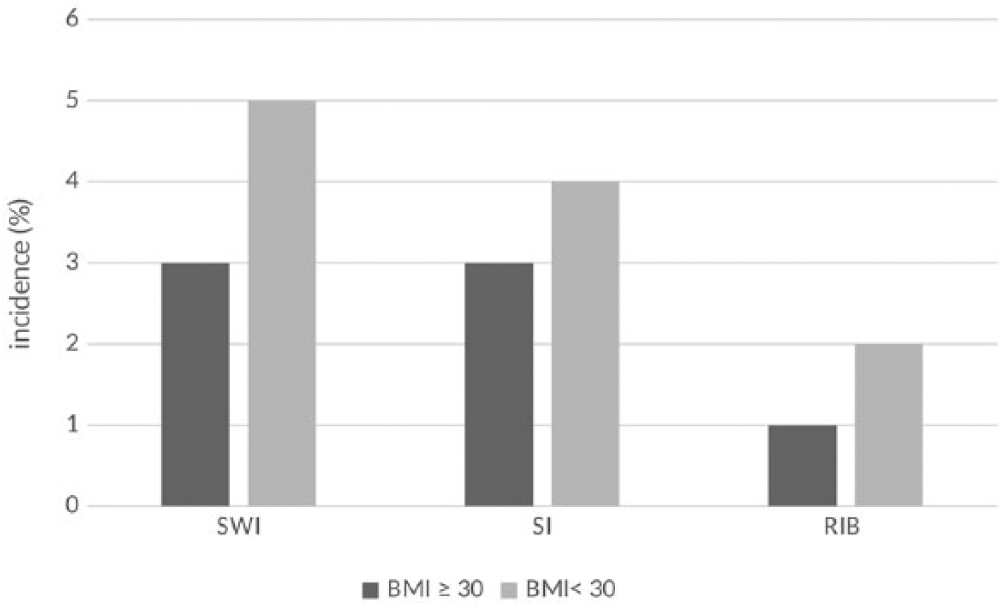
Outcomes in obese patients. In obese (n = 113) vs nonobese (n = 206) patients, there was no difference for SWI (P = .263), SI (P = .565), and RIB (P = .332). In obese patients, incidences of SWI and SI were 3% (3/113) and RIB 1% (1/113). In nonobese patients, incidence of SWI was 5% (11/206), SI 4% (8/206), and RIB 2% (5/206). RIB indicates reintervention for bleeding; SI, sternal instability; SWI, sternal wound infection.
Characteristics of group 1.
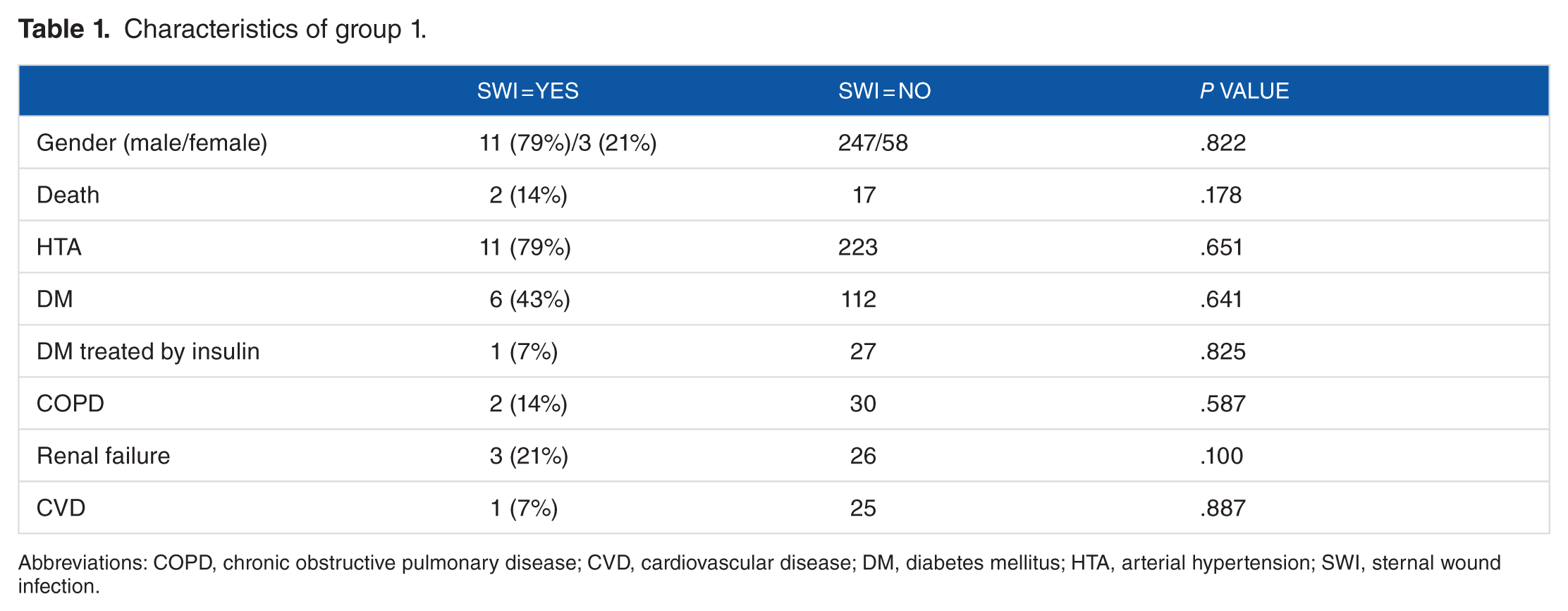
Abbreviations: COPD, chronic obstructive pulmonary disease; CVD, cardiovascular disease; DM, diabetes mellitus; HTA, arterial hypertension; SWI, sternal wound infection.
Characteristics of group 2.
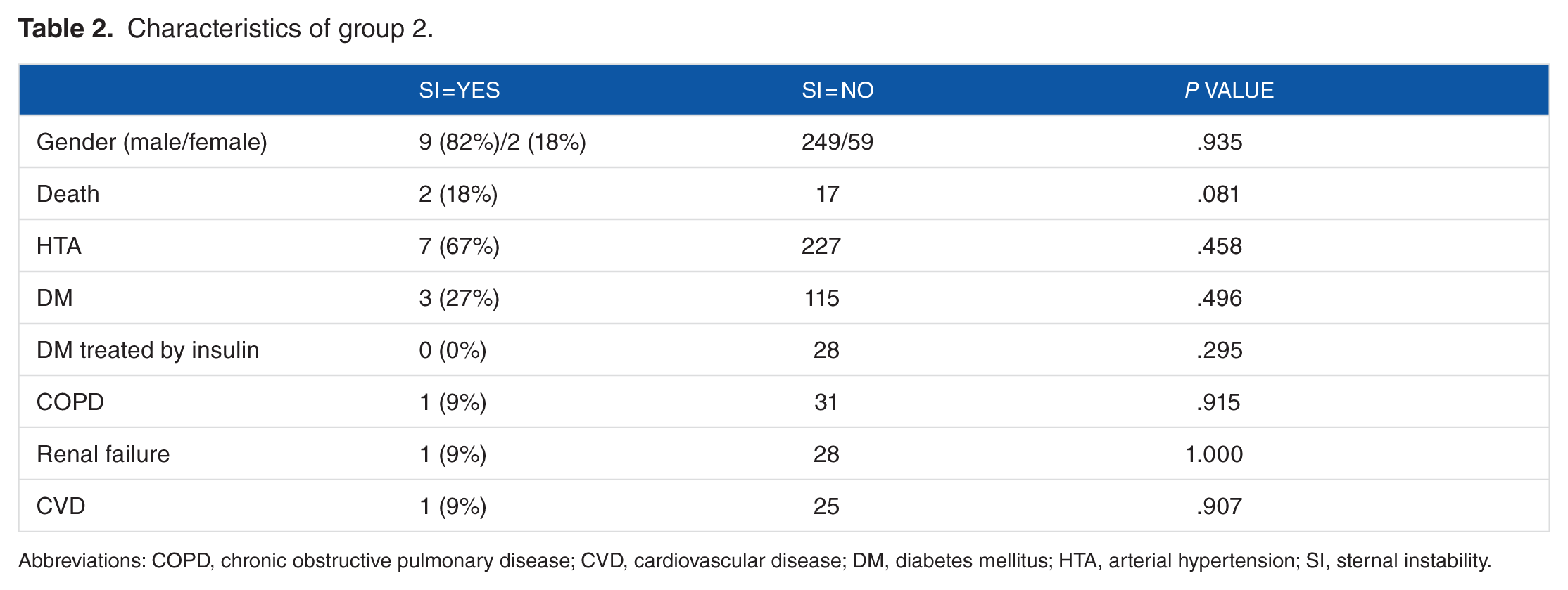
Abbreviations: COPD, chronic obstructive pulmonary disease; CVD, cardiovascular disease; DM, diabetes mellitus; HTA, arterial hypertension; SI, sternal instability.
Characteristics of group 3.
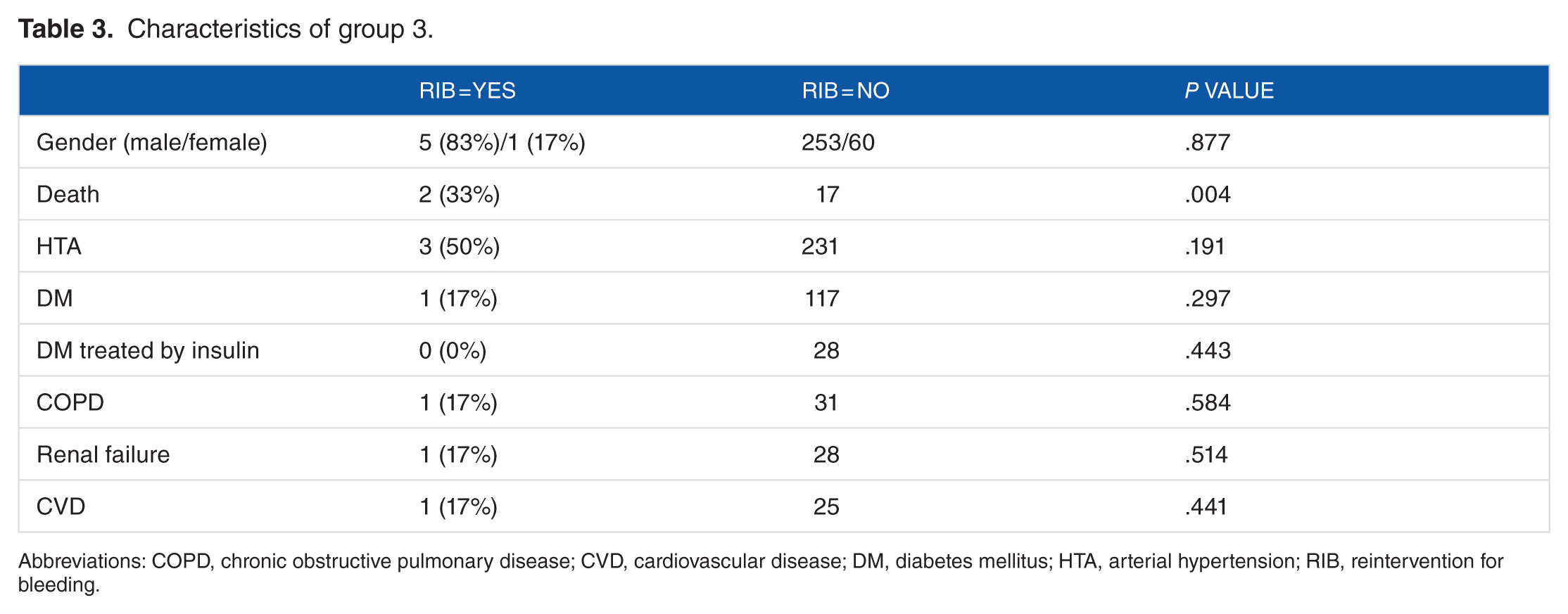
Abbreviations: COPD, chronic obstructive pulmonary disease; CVD, cardiovascular disease; DM, diabetes mellitus; HTA, arterial hypertension; RIB, reintervention for bleeding.
Discussion
We found a global incidence of SWI of 4% for BIMA patients. In this study, high-risk populations did not represent factors likely to cause sterna pathologies. Mortality was statistically increased in the group of reintervention for bleeding, whatever the target population is. The role of the skeletonizing technique is not highlighted here but did not seem to play some important roles. Distinguishing SWI from SI can help to clarify incidence of SWI in CABG including BIMA.
The incidence of SWI in the literature is variable. Itagaki et al 18 reported an incidence of SWI of 1.4%, without differentiating BIMA patients. However, this study compared BIMA with SIMA. All patients in our series had BIMA grafting, explaining the higher rate for SWI. Nevertheless, other studies reported higher incidence of SWI: Gatti et al 19 reported an incidence of 11.7% of SWI in their population of insulin-dependent DM (in our subgroup; incidence is 4%). Hirotani et al 11 earlier, published an incidence of chest wound infection of 5.7% in no DM (in our subgroup, incidence is 4%) and 10.0% in DM (in our subgroup, incidence is 4%). These studies aimed to compare incidence of SWI into 2 different groups of patients. At our knowledge, there is no work nowadays with the same design: we indifferently performed BIMA grafting in all our CABG despite patient’s comorbidities (eg, concurrent valve procedure included) and that is why our incidence of SWI is not comparable with other studies. The skeletonizing technique is often discussed for minimizing chest wall trauma 2 and reducing risk of SWI 20 by preserving intercostal collateral vessels and blood supply. However, Dai et al 12 also concluded that skeletonized BIMA should be the recommended procedure. In this study, we avoid the skeletonizing technique. Anyway, good results were obtained. Some works on canine models demonstrated that chest wall vascularization was significantly decreased after internal mammary artery mobilization regardless the technique used. 9 Even if the mainstream is to skeletonize the mammary artery, we think that this technique takes much more time in comparison with a nonskeletonized approach. Peterson et al 20 reported a difference of intraoperative time: 199 ± 75 minutes for a skeletonized approach and 184 ± 69 minutes for the conventional approach. Intraoperative time was not recorded in this study but this longer intraoperative time is certainly a factor that discourages surgeons to use BIMA. We agree with the fact that whatever the technique of harvesting used, the most important consideration is to preserve carefully the continuity between sternal and perforating vessels of mammary artery and sternal or intercostal branches. 21 Performing this study, we want to tackle the topic of sternal closure and SI. Creating 3 groups according to the type and the extent of sternal disturbances allowed to distinct the different clinical entities. Even if subgroups of the different sternal complications contain few patients, distinction between SWI and SI was crucial. In our study, every patient with SWI had a bacteriological documentation. The criteria defining SWI include SI, which can be a major risk factor in the development of SWI. 22 Sternal instability creates increased bones movements and local tissue necrosis that can promote a supportive environment for bacterial growth. 9 Nevertheless, SI per se is defined by separation of the sternum at the midline due to bony fracture or disruption of the wires. 16 However, this definition may be overly restrictive. Currently, there is no universally accepted definition of SI and accordingly no defined universally sternal precautions. 23 Some ascertainment can be made: paramedian sternotomy leads much more often to SI, whatever the sternal closure technique used. 9 There are several techniques of sternal closure that include stainless steel plates, stainless steel cables, and sternal screws with central lumen. 9 In this study, the same material to make sternal closure was always used, namely, 3 double sternal wires and 3 single sternal wires. This material is quickly and easily installed and can be used in every patient, regardless the risk categories. However, independently of the technique used to make sternal closure, we must have standard protocols: most possible atraumatic sternotomy, adherence to aseptic technique, avoidance of dead spaces, careful hemostasis, and prophylactic use of intranasal antibiotics to prevent methicillin-resistant Staphylococcus aureus colonization. 24 As a reminder, criteria defined by the Centers for Disease Control and Prevention were used to make the diagnosis of SWI and to distinguish it with SI. The distinction between these 2 entities can also explain the low incidence of SWI in our little sample. Indeed, distinction of different sternal complications may have an impact on the high-risk groups created, showing that with better definitions of sternal pathologies; high-risk groups may tend to become patients groups without restriction of use for coronary revascularization. Some other classifications to define SWI exist, such as Pairolero classification of infected median sternotomies that divides chest wounds into 3 categories based on duration and clinical findings. 25 We agree with Bryan and Yarbrough 26 that every case of SWI has to be reviewed and the main cause has to be analyzed.
This study has some weaknesses and limitations. We made a single-center retrospective observational study including only 319 patients. This little sample size and its retrospective observational aspect make it undoubtedly a weak power study, comparing with other studies of higher amplitude. Moreover, this kind of approach does not make possible avoiding confounding factors. There is no “lost to follow-up” patients registered but it would have been better to perform a prospective, randomized controlled trial with BIMA vs SIMA. However, this study also reflects significant methodological weaknesses in collection’s data in peripheral institutions, explaining lack of more preoperative variable in the results. Retrospective design is always subjected to inherent selection bias too (no data on SIMA grafting). The database only reflects the work of 1 surgeon and these results cannot be extended to all the team. Outcomes after 2015 were not analyzed. However, we think that peripheral surgical method and analyses deserve credit for raising concerns about a part of the surgical current reality even if results cannot be compared with powerful study resulting from tertiary institution.
Finally, nowadays, potential advantages of BIMA grafting are recognized overall in terms of long-term survival 1 and by not increasing operative morbidity. 27 One of the major restrictions for extending the use of BIMA grafting is the current impossibility of generalizing the procedure to higher risk patients. 28 This results tend to confirm recent results that promote the use of BIMA grafting in every kind of patients8,29 and consequently to confirm the generalization of the procedure, without being afraid of sternal complications.
The survival advantage of this procedure has to be better taken into account regardless the risk of SWI that seems to be more controlled nowadays and that needs to be clarified by definitions that are more precise. Some international consensus should be reached to give a single definition of this concept and to promote the best therapeutic attitude. Promoting a periodical review by a multidisciplinary medical audit of best practice for defining the best attitude in this field should be done. Future research works should be concentrated more on the way of using BIMA grafting without increasing preoperative risks than on the risk factors which tend to avoid their bilateral harvesting in CABG. One technique of surgical sternal closure is here pointed out but some research areas of research have to be investigated.
Conclusions
Obesity, age, and presence of insulin-dependent diabetes do not influence incidence of SWI on patients benefiting from CABG using BIMA. We emphasize that BIMA grafting is a good surgical procedure, even in EP, obese, and DM, without affecting significantly incidence of sternal wound complications. This study tends to convince surgeons about the advantages of BIMA grafting even in higher risk patients.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
JMR and PS conceived the presented ideas. CM analysed all the datas and performed the statistical analysis. TG and all authors discussed the results and commented on the manuscript. JMR wrote the paper with input from all authors.
Ethical Approval
Ethical approval was not required in our institution for this study.
Meeting Presentation
J Ravaux MD, T Guennaoui MD, C Mélot MD PhD, P Schraverus MD. Bilateral internal mammary artery bypass grafting and sternal wound infection in high risk population. Presentation at the abstract session of coronary surgery on May 12, 2017, at 66th international congress of the European Society for Cardiovascular and Endovascular Surgery, Thessaloniki, Greece.
J Ravaux MD, T Guennaoui MD, C Mélot MD PhD, P Schraverus MD. Infections sternales après pontages aorto-coronariens bimammaires dans les populations à hauts risques. Presentation at commented cardiac poster session (2) on June 9, 2017, at the 70th congress of the French Society of Thoracic and Cardiovascular Surgery, Marseille, France.
J Ravaux MD, T Guennaoui MD, C Mélot MD PhD, P Schraverus MD. Bilateral internal mammary artery bypass grafting: extent of use and focus on sternal wound infection. Oral podium presentation on the coronary heart disease session, on September 3, 2017, at the 27th congress of the World Society of Cardiovascular and Thoracic Surgeons, Astana, Kazakhstan.
J Ravaux MD, T Guennaoui MD, C Mélot MD PhD, P Schraverus MD. Bilateral internal mammary artery bypass grafting and sternal wound infection in high risk population (Abstract Book). The Journal of Cardiovascular Surgery June 2017; 58: 59.
