Abstract
Advances in mechanical circulatory support devices provided the technology to develop long-term, implantable left ventricular assist devices as bridge to transplant, destination therapy, and in a lesser group of patients, as bridge to recovery. Despite the benefits from this innovative therapy, with their increased use, many complications have been encountered, one of the most common being infections. With the driveline acting as a portal to the exterior environment, an infection involving this structure is the most frequent one. Because patients with destination therapy are expected to receive circulatory support for a longer period of time, we will focus this review on the risk factors, prevention, and treatment options for driveline infections.
Introduction
As the prevalence of heart failure continues to increase, it is estimated that 8 million Americans will suffer from this disease by 2030. 1 Despite improvement in guideline-directed medical and device therapy, the overall 1-year mortality rate remains as high as 30%, and it is further increased by the number of hospitalizations. 2 Heart transplantation remains the gold standard for treatment of advanced heart failure, but as the demand for heart transplantation exceeds the organ supply, and as certain comorbidities preclude heart failure patients to be candidates for heart transplant, mechanical circulatory support with left ventricular assist devices (LVADs) either as a bridge to transplant or as a destination therapy has gained popularity in the management of advanced heart failure.3,4 It has been demonstrated that mechanical support with pulsatile and nonpulsatile devices improves mortality and quality of life in a selected patient group.5,6 In April 2008, the Food and Drug Administration approved the use of HeartMate II (Thoratec, Pleasanton, CA, USA) for bridge to transplant 7 ; later on, in 2010, it was approved to be used as destination therapy, making this option available to a wider group of patients. 8 Since 2010, there has been a 10-fold increase in this practice in the United States and, according to the seventh INTERMACS annual report, from 2008 until 2014, a total of 4598 have been implanted, accounting for 38.2% of all LVAD implants; with another 4038 patients receiving it as bridge to candidacy (33.6%).9,10 In the recent ENDURANCE trial, the HeartMate II was compared with the HVAD (HeartWare ventricular assist device) system (HeartWare, Framingham, MA, USA) as destination therapy with equivalent results. 11
With increased duration of therapy, a new spectrum of long-term complications has arisen. Although disorders of coagulation (bleeding and thrombosis) remain as the most common complication, infection is becoming a major problem, being reported in 18% to 59% of the cases. Among those, the most prevalent is driveline infection (DLI), which will be the focus of our review.4,12
Definition and Dimension of the Problem
The International Society of Heart and Lung Transplant (ISHLT) defines the LVAD infections as all infections that occurred in the presence of an LVAD that may or may not have been directly attributed to its use but needs consideration due to the presence of the device. Left ventricular assist device infections may be local, with pocket infection and DLI or they may be systemic, with involvement of the blood stream and/or endocarditis. Furthermore, DLI is defined as an infection affecting the soft tissues around the driveline outlet, accompanied by redness, warmness, and purulent discharge. Despite DLI being a confined phenomenon, it can spread to other sites, worsening the severity of the disease and/or becoming systemic. 4 It is also known that the risk of infection increases with the duration of device implantation. 13
The prevalence of DLI varies from 14% to as high as 28% in the Randomized Evaluation of Mechanical Assistance for the Treatment of Congestive Heart Failure (REMATCH) trial, a landmark trial using a first-generation, pulsatile LVAD (HeartMate XVE, Thoratec, CA, USA). 13 These outcomes are very similar to those of a recent retrospective study involving 247 subjects, of which 32% developed LVAD infection, with DLI accounting for 47% of them. 14 Notwithstanding, a recent prospective study done by the Ventricular Assist Device Infection Study Group showed fewer incidences of infection (22%) among 150 patients scheduled for LVAD implantation (2006-2008) at 11 US centers. 3 Of these, DLI was the most prevalent type of infection (85%). The lower rate of infection found in this study might be due to the fact that 85 of the 150 patients received HeartMate II (continuous-flow device); of these only 18% developed LVAD infection, compared with 27% of the patients who received an older generation device. 3 It is suggested that the risk of infection is increased in pulsatile devices, as seen in the REMATCH trial; possibly driven by the larger size of the device and driveline itself, requiring more extensive planes of dissection and surgical time during implantation. 6 Furthermore, since the HVAD system rests within the pericardium and does not require creation of a preperitoneal pocket, it might reduce the likelihood of device infection, although this was not evident in the preliminary ENDURANCE trial report.11,15
Despite several published studies, the epidemiology of LVAD infections is still very limited due to several factors, including but not limited to the following: methodology, sample size, focus in outdated first-generation devices, and nonstandardized definition of device infection.3,14
Physiopathology and Microbiology
Modern LVADs still require a driveline, which permits communication between the pump and controller and delivers energy from an external source 13 ; therefore, the driveline acts as an entry point. 3 Microorganisms can colonize the driveline site during or after the device implantation. 13 Even though the infection is often associated with the preoperative period, only 15% of cases arise during the first 30 days after the surgery. 16 Because of this, the focus of study of the LVAD infections has been shifted to the late-onset infection. There are 4 main determinants for the infection defined by Pereda and Conte 13 and are summarized in Table 1:
Host determinants. Nutritional status, immunosuppression, oral hygiene, diabetes, renal failure, and obesity. 13 In patients with renal failure, for each gram of increased creatinine, the risk of infection increases by 70%; these patients are immunocompromised and sicker. 3 Long-term dialysis should be a relative contraindication for LVAD implant because infections in this group confer poor outcomes. Evidence regarding DLI and its association with obesity is conflicting; driveline exit site integrity can be challenging for the obese patients. 15 Depression is also associated with infections, with a 3-fold increase in LVAD infection, possibly related to ability or thoroughness with the driveline care and/or hygiene. 3
Implant and postoperative care determinants. Because the procedure is associated with accumulation of blood and fluid in pockets, this environment is ideal for the growing of microorganisms, also causing the necessity of a draining tube to stay in place longer, serving also as port of infection. 13
Characteristics of the device. In most of the LVAD models, the driveline is coated with highly textured polyester material, which protects the exit site improving the integration with the skin and soft tissue. The more rigid or thicker the driveline is, the higher is the risk of infection. In addition, the weight of the controller and battery increases tension and trauma to the exit site. 13 Given that trauma caused by the driveline mobility is one of the attributable factors for risk of infection due to exit site injury, Fudim and colleagues 17 considered the use of external anchoring suture to reduce trauma cause by this movement, but the results were discouraging because it failed to decrease the rate of infection.
Microbiological determinants. The microbiological determinants include the following:
Gram-positive cocci. The most common gram-positive bacteria isolated are staphylococci (41%) because they colonize the nose and the skin and adhere to the implanted prosthetic material forming a biofilm.3,12 The importance of the biofilm was demonstrated by comparing biofilm-deficient Staphylococcus with unaltered bacteria, the later found to be more aggressive and more rapid to migrate along the driveline. 18 According to a study done by Deng et al, 19 46% of all driveline or pocket infection cultures and 36% of blood cultures grew Staphylococcus, respectively. The most common being Staphylococcus epidermidis (38%), followed by Staphylococcus aureus (24%). 20 Among other gram-positive cocci isolated, the enterococcus species are not uncommon. 21
Gram-negative rods. Gram-negative rods are the second most common group of pathogens, representing 24.1% of all the infections, 14 with Pseudomonas species being the most common (they also have the capability to form biofilm).3,12,13 Klebsiella and Enterobacter species also play an important role; and along with Pseudomonas species are associated with poor outcome.4,14
Fungi. The rate of fungal infection was previously described to be around 15% by Gordon et al 22 in 2001 but was found to be only 6.6% in a recent cohort. 14 The most common fungal pathogen is Candida species. 4
Mycobacteria. Most of the cases have been reported in other devices, such as automated implantable cardiac defibrillators, 23 but a case of Mycobacterium avium complex has been described in a patient with LVAD. 24
Determinants of the infections related to left ventricular assist devices.

Multidrug-resistant organisms are another growing concern; in a recent single center study, 31.6% of the infections reported were found to be caused by drug-resistant organisms. These cases were associated with more frequent hospital admissions. 25
Prevention
Left ventricular assist device infections in the postoperative period are most likely due to intraoperative or perioperative contamination, the risk of which can be reduced with proper aseptic and antiseptic measurements. Another important part is avoidance of pocket hematoma. 26 Preoperative antibiotics for gram-positive and gram-negative coverage are recommended, and these should be given within 60 minutes of the first incision, with 1 dose prior to the procedure and not extended beyond 24 to 48 hours. 15 Proper care and early removal of central venous catheter should also be standard practice. 27
Nasal swab to screen for methicillin-resistant S aureus is also recommended, and if positive, the patient should receive topical treatment prior to the procedure. 15 Dental assessment and treatment, if possible, should be obtained prior to the surgery. 15
Because the driveline exit is the most common site of infection, care is imperative during and after the procedure. 26 The driveline should be stabilized immediately after the device is placed, and the dressing changes should start within 24 to 48 hours postoperatively and at least daily afterward. The dressing change should be done under sterile technique and the wound should be cleaned and rinsed with antiseptic solutions and dried before covering. 27 Another determinant is the tunneling technique to keep the driveline velour portion in the subcutaneous tissue. This has been studied by the Silicone Skin Interface Registry, showing a 50% reduction in infection compared with velour-to-skin method. 28 Because the abdominal wall muscle layer is a well-vascularized structure serving as source of nutrition substrates and antimicrobial elements, another new technique with promising results is the rectus-sparing technique, in which the driveline is located above the posterior fascia, thus leaving the preperitoneal fat layer intact. 29 A small study also showed that the use of a simple device to secure the driveline using a StatLock system and a silicone suture might prevent trauma and therefore DLI. 30 It is important to prevent such infections due to the increased risk of bacteremia and sepsis, which is associated with poor outcome. 4 Another important association described in patients with LVAD and blood stream infection is the increased risk of cerebrovascular accidents. 31
Diagnosis
According to the 2013 ISHLT guidelines, the following are class Ia recommendations for all patients with suspected device infection, which we have incorporated in an algorithm (Figure 1): complete blood count, chest radiography, and 3 sets of blood cultures in 24 hours must be obtained. For patients with suspected DLI, Gram stain, KOH, bacterial, and fungal culture from the site are suggested. Directed imaging studies based on clinical presentation and aspiration of potential sources are required if indicated. Consider erythrocyte sedimentation rate and C-reactive protein. 32 Imaging studies are limited in this setting: ultrasound can be useful in identifying fluid pockets, but it is not good for revealing whether the device is infected; computed tomography is also limited because of the artifact caused by the device itself. 12 A recent single center trial positron emission tomography/computed tomography was accurate in detecting both localization and even extension of the infection. 33
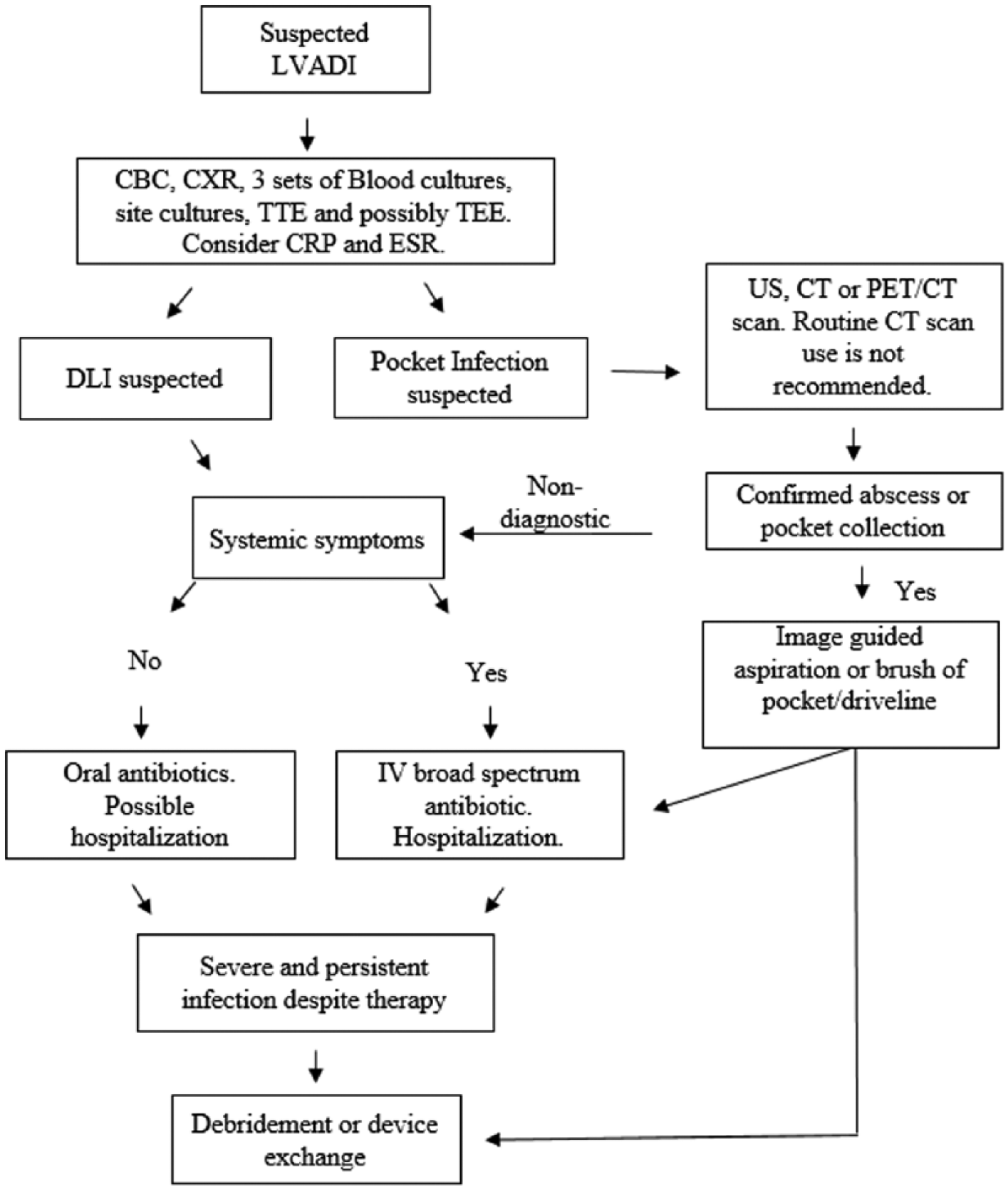
Management algorithm of suspected device infection. CBC, complete blood count; LVADI, left ventricle assist device infection; CRP, C-reactive protein; CT, computed tomography; CXR, chest x-ray; DLI, driveline infection; ESR, erythrocyte sedimentation rate; IV, intravenous; PET/CT scan, positron emission tomography-computed tomography scan; TEE, transesophageal echocardiogram; TTE, transthoracic echocardiogram; US, ultrasound.
Criteria proposed for diagnosis of pump or cannula infection are summarized in Table 2. The infection is proven when definitive microbiology is found, with histologic confirmation at explants, or when 2 major clinical criteria are met. Probable diagnosis defined by 1 major and 3 minor clinical criteria, or 4 minor criteria, whereas a possible diagnosis is determined by the presence of 1 major and 1 minor criteria or 3 minor criteria. An infection is unlikely if it resolves after 4 days of antibiotics, or in the presence of an alternate diagnosis, with no pathologic evidence at surgery with antibiotics for 4 or less days, or not meeting established definitions. 32 The major criteria include the following: (1) an indistinguishable organism recovered from 2 or more peripheral blood cultures taken more than 12 hours apart with no other source of infection is needed; all of 3 or most of ⩾4 separate positive blood cultures (with the first and last samples drawn at least 1 hour apart) with no other focus of infection. (2) Two or more positive blood cultures taken from the central venous catheter and peripherally at the same time. (3) Echocardiogram positive for ventricle-assisted device–related infective endocarditis. 34
Diagnosis of ventricular assist device–specific pump, cannula infection, and pocket infection.
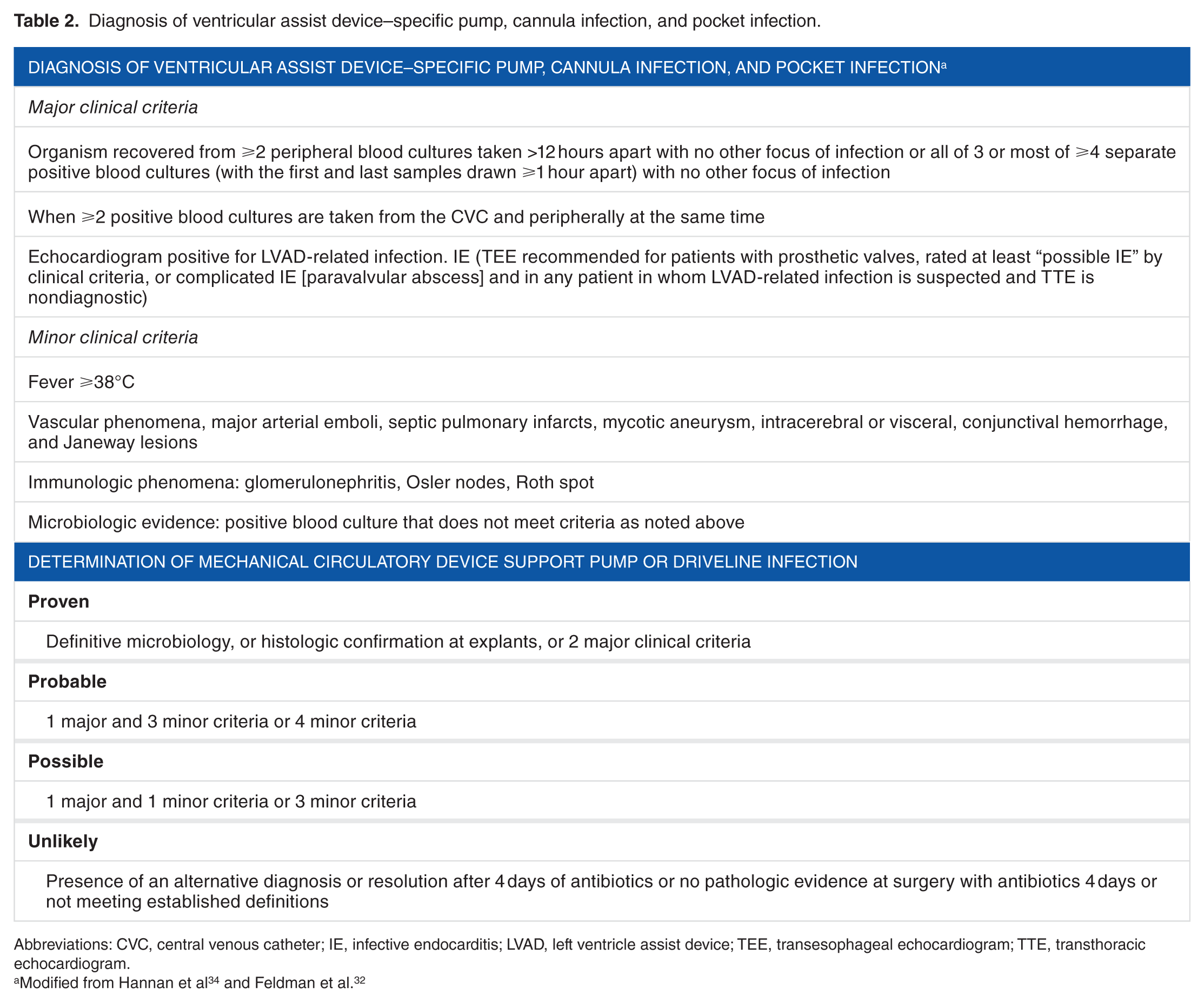
Abbreviations: CVC, central venous catheter; IE, infective endocarditis; LVAD, left ventricle assist device; TEE, transesophageal echocardiogram; TTE, transthoracic echocardiogram.
Treatment
Medical therapy
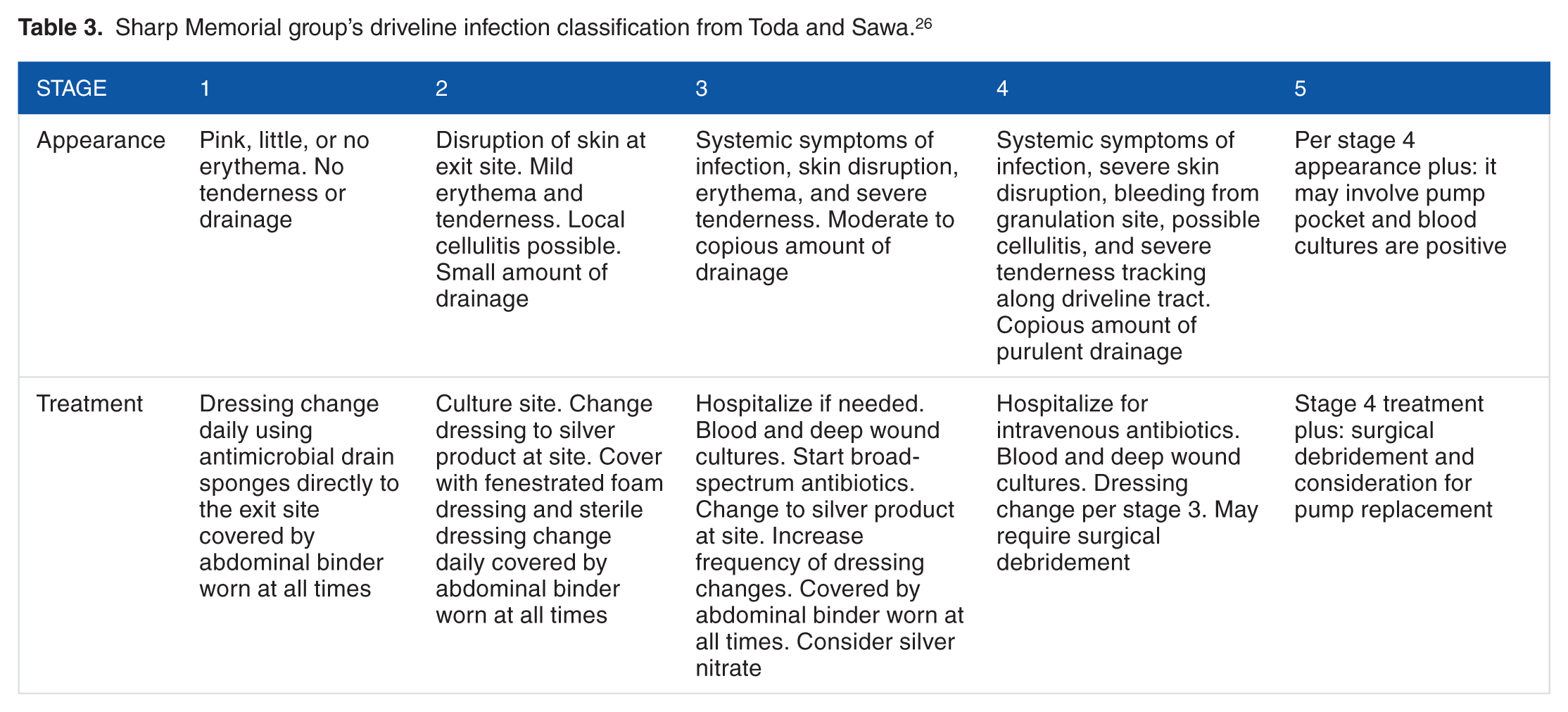
Due to the lack of data in this setting, most of the time, antimicrobials are chosen empirically. These are oriented to cover the most common organisms, such as gram-positive cocci and gram-negative rods. In cases with absence of systemic symptoms such as fever or chills, it is a common practice to start oral antibiotics such as doxycycline or ciprofloxacin, wound care, and immobilization of the driveline.12,27 Before starting empiric therapy, site and blood cultures are required. If the infection is more severe, hospitalization is necessary and intravenous broad-spectrum antibiotics are recommended (Figure 1). 12 The Sharp Memorial group classification is a useful tool for deciding treatment approach in patients with driveline infection (Table 3) (Figure 2). 26 Regarding suppressive therapy with long-term oral antibiotics, the evidence does not indicate that it helps to prevent recurrence,12,14 as it was studied in a retrospective cohort study, with more than a third of the patients having recurrence of the infection. The study had several limitations: it was retrospective, the information was limited to the medical records, definition of chronic suppression was not described in the literature, and different antibiotics were used. 35
Sharp Memorial group’s driveline infection classification from Toda and Sawa. 26
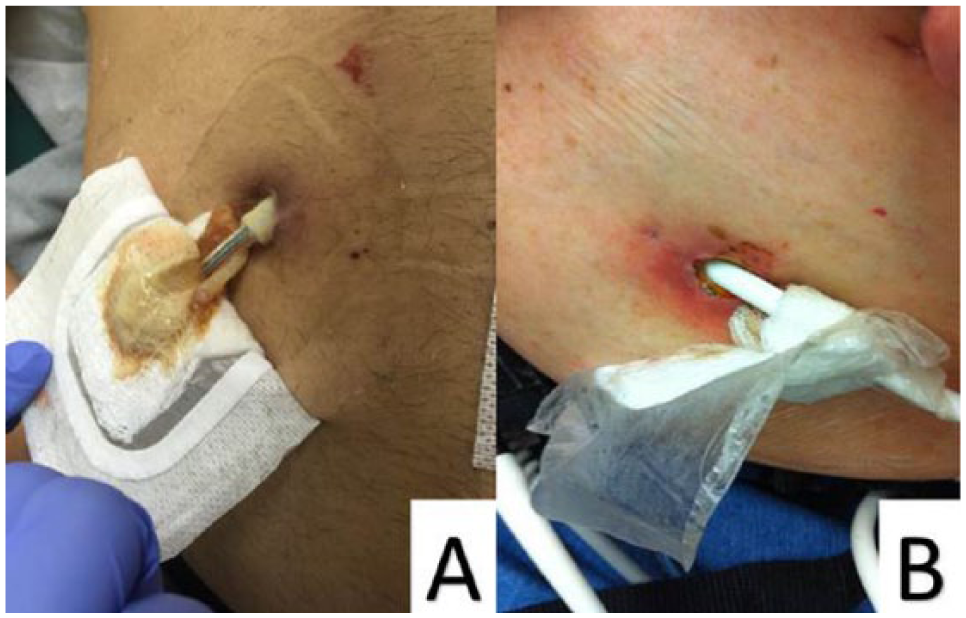
Example of 2 patients with driveline infection. (A) Driveline with purulent discharge and (B) surrounding erythema.
Surgical therapy
Device exchange is a last resource used in the setting of severe and persistent LVAD infection. In the REMATCH trial, 3 of the 29 devices that required exchange were due to infection, and it was associated with 100% mortality in 1 year compared with 53% in the group where the procedure was pursued for other reasons.36,37 Most of the information regarding LVAD exchange rely in small case series, making the data on the subject of this treatment very limited when it comes to management of such patients. 36 Furthermore, driveline unroofing and debridement should be considered in the setting of severe infection or refractory to initial antibiotic therapy.
Conclusions
Left ventricular assist device support in destination therapy population is rapidly growing, and complications related to its use are increasingly seen, with infection being one of the most common complications, and associated with poor outcome. The most predominant of all LVAD infections is DLI, sometimes localized, yet with the potential to become systemic with serious consequences. It is important to understand every aspect of this new condition, to prevent it, and to have effective treatments once it is diagnosed. It is paramount for this technology to evolve, to eliminate the actual driveline from the device, and therefore reduce this dreaded complication.
Footnotes
Peer review:
Four peer reviewers contributed to the peer review report. Reviewers’ reports totaled 593 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
All authors contributed equally.
