Abstract
Background:
Pathogenic viruses have been abundant and diverse in wastewater, reflecting the pattern of infection in humans. Human feces, urine, and perhaps other washouts that frequently circulate in sewage systems may contaminate wastewater with SARS-CoV-2. It’s crucial to effectively disinfect wastewater since poorly handled wastewater could put the population at risk of infection.
Aims:
To emphasize the presence and spread of SARS-CoV-2 in sewage (wastewater) through viral shedding from the patients to detect the virus in the population using wastewater-based epidemiology. Also, to effectively manage the transmission of SARS-CoV-2 and reduce the spread of the virus in the population using disinfectants is highlighted.
Methods:
We evaluated articles from December 2019 to August 2022 that addressed SARS-CoV-2 shedding in wastewater and surveillance through wastewater-based epidemiology. We included the papers on wastewater disinfection for the elimination of SARS-CoV-2. Google Scholar, PubMed, and Research4Life are the three electronic databases from which all of the papers were retrieved.
Results:
It is possible for viral shedding to get into the wastewater. The enumeration of viral RNA from it can be used to monitor virus circulation in the human community. SARS-CoV-2 can be removed from wastewater by using modern disinfection techniques such as sodium hypochlorite, liquid chlorine, chlorine dioxide, peracetic acid, and ultraviolet light.
Conclusion:
SARS-CoV-2 burden estimates at the population level can be obtained via longitudinal examination of wastewater, and SARS-CoV-2 can be removed from the wastewater through disinfection.
Background
A positive single-stranded RNA virus with an envelope, SARS-CoV-2 (severe acute respiratory syndrome-coronavirus-2) is a member of the ß-coronavirus genus. 1 The COVID-19 outbreak brought on by the SARS-CoV-2 virus, which is believed to have originated in Wuhan, China, had driven the entire world into anarchy. 2 SARS-CoV-2 is highly homologous to SARS-CoV and infects cells via ACE2 (Angiotensin-converting enzyme receptor-2). 3 SARS-CoV-2 is a highly contagious virus that spreads by respiratory droplets, direct contact with infected people, and contaminated surfaces. 2 Other potential exposure routes may include the fecal-oral route and transmission by aerosols. 4 It was shown that aerosols produced during hospital, industrial, recreational, and domestic activities assisted SARS-CoV-2 spread into environmental effluent, placing the nearby communities at risk for infection. 5
Household sewage, industrial sewage, and other pollutants are contaminating water supplies. Organic materials, bacteria, ammonia, pesticides, and many other toxins are present in contaminated water. 6 Consequently, individuals are more aware of health-related issues, which has led to key public health concerns in water disinfection. 7 By treating contaminated water supplies and safeguarding them, it is possible to reduce the spread of diseases like cholera and typhoid fever that are spread by water. In the United States, the adoption of water disinfection decreased the incidence of cholera by 90%, typhoid by 80%, and amoebic dysentery by 50%. This shows that water disinfection is one of the most significant public health advancements of the past century and may be effective in controlling the spread of SARS-CoV-2. 8 In the process of producing drinking water; organic matter, bromide, iodide, and anthropogenic contaminants react with disinfectants (chlorine, ozone, chloramines, and chlorine dioxide) to produce a class of chemicals known as disinfection by-products (DBPs). The type of disinfectant, water quality, and water treatment conditions influence DBPs’ composition and levels. 9
Human effluent in wastewater can be used as a tool for disease surveillance. 10 The emergence of the SARS-CoV-2 virus and its presence in water, soils, and other environmental compartments may pose a hazard to public health and the environment. 11 If aerosols are produced, the wastewater plumbing system’s ability to host dangerous bacteria increases the possibility of viruses like SARS-CoV-2 being transmitted by air. 12 To collect information on the prevalence and dynamics of infection for entire populations, raw sewage water from the entire community that contains solids extracted during the primary sedimentation phases is collected and monitored. Even with limited testing capabilities, the assessment of raw sewage and sludge-based surveillance remains crucial. 13
Additionally, self-isolation and quarantine sites for infected individuals both lead to significant viral shedding into the system. 14 The potential for prolonged viral shedding in feces for nearly 5 weeks after the respiratory samples of the patients had tested negative for SARS-CoV-2 RNA and even the likelihood that the organism can remain viable for days may help facilitate fecal-oral channel transmission.15,16 Various investigations have found SARS-CoV-2 in wastewater.17,18 A catchment was used to concentrate SARS-CoV-2 RNA from wastewater and reverse transcriptase quantitative polymerase chain reaction was used to count the number of viral copies. 18 Where in-person testing may not be possible, longitudinal examination of wastewater can offer population-level estimates of the burden of SARS-CoV-2. 19 When the SARS-CoV-2 virus is still contagious in wastewater, it could pose harm to human health by way of aerosol inhalation or ingestion. The report mentioned the potential to culture different coronavirus kinds from wastewater for a few days.20,21 For discussing the discovery of SARS-CoV-2 viral RNA in human excretions and their passage to the sewage system/wastewater, there is currently only a limited number of data accessible. The analysis of numerous peer-reviewed scientific publications and published articles clarified the essential understanding of water-based epidemiology for the coronavirus.
The world is currently grappling with the effects of the emergence of the novel coronavirus that causes COVID-19 and the severe acute respiratory syndrome SARS-CoV-2, and the difficulties in preventing their spread are growing as evidence of their presence in sewage and stool samples emerges. 22 The embedded virus particles in the stools that were obtained in wastewater pipelines from asymptomatic patients and/or inadequately or ineffectively treated wastewater may endure for a longer period and hence may serve as a secondary source of infection. 23
Certain situations and factors, such as wastewater quality, investment, operational expenses, and management level, influence the choice of specific types of disinfection technology. 24 The entire globe is/was focusing on the control of this pandemic in light of the alarming situation with COVID-19. Numerous clinical findings suggested that the virus may be present in the municipal wastewater of the impacted societies. 25 Utilizing wastewater-based epidemiology (WBE), which is useful for early warning of disease outbreaks and is faster, more widely applicable, and less expensive than clinical screening.26-29 In a few recent research, SARS-CoV-2 was found to be molecularly detected in wastewater samples.17,30 An advanced study is necessary to establish the methodology and consequences for determining the presence of SARS-CoV-2 in wastewater. It is suggested that water-based epidemiological research be accelerated to halt the pandemic from spreading further.
We incorporated information from limited studies that were published in English literature from the end of December 2019 to August 2022 and elucidated the excretion of SARS-CoV-2 RNA from patients and the presence of the viral RNA in wastewater from various geographical regions. Studies that did not follow the guidelines for water-based SARS-CoV-2 epidemiology and related viral shedding were disregarded. The review also included articles that discussed the disinfection of wastewater to remove coronaviruses. Data from PubMed, Research4Life, and Google Scholar served as the foundation for this review. We thoroughly searched reference lists from publications and reports by hand. The keywords utilized were “2019-nCoV,” ‘SARS-CoV-2”′ or “COVID-19” combined with “gastrointestinal,” “digestive,” “feces,” “wastewater” “sewage” and “disinfection of wastewater” accompanying “SARS-CoV-2.” We analyzed relevant research and gathered information on the identification of SARS-CoV-2 RNA in shedding, wastewater sewage harboring the viral RNA, and wastewater treatment. Due to the terms and ease of comprehending the presence of the virus in the wastewater and its removal, only 47 research were included in our investigations.
Spreading of Viruses Through Respiratory and Fecal Routes
The digestive tract appeared to be the site of viral shedding for a longer period than the respiratory tract. The virus has been suggested to present in feces for an average of 27.9 days (SD 10.7) following the beginning of the first symptom, which is 11.2 days (SD 9.2) longer than it was in respiratory samples. 18 Compared to respiratory samples, studies have shown that viral RNA is more persistent in feces samples.18,19 Despite the respiratory samples from the patients being negative for SARS-CoV-2 RNA, there is a chance that the virus may have been shed for a longer period of over 5 weeks in the feces. These studies exhibit the likelihood of the occurrence of fecal-oral transmission following viral clearance in the respiratory system, and they also elucidate active viral replication in the patient’s gastrointestinal tract. 18 The high rate of viral shedding into the system is a result of self-isolation as well as quarantine areas for sick individuals. 12 The absorptive enterocytes from the ileum and colon as well as the esophageal epithelial cells have significant levels of ACE2 expression, which raises the possibility of fecal transmission. 18 The COVID-19 virus has been associated with gastrointestinal symptoms such as vomiting and diarrhea. PCR testing for comparison between feces and respiratory materials for the period supported the idea that the virus particles were more resilient in the gastrointestinal system than in the respiratory tract. SARS-CoV-2 may spread easily through feces when the viral load in the stool is large or in an environment that is conducive to viruses. The SARS-CoV-2 virus is shed in feces in part as a result of infection. The piping system for wastewater has flaws that make it easier for polluted air to leak out and cause cross-contamination. 12 Some coronaviruses may be able to persist in the gastrointestinal system and transmit orally through the “fecal-oral” route or through the inhalation of wastewater droplets that are contaminated. 12
Wastewater Surveillance for Estimating SARS-CoV-2 Prevalence
SARS-CoV-2 wastewater surveillance was found to be useful for estimating prevalence and providing an early warning for inflated epidemics as elucidated by the tools for tracking clinical cases in a community.12,17,19,31 Quantification of SARS-CoV-2 conducted from samples incurred from wastewater in diverse settings suggested that viral RNA can be present in wastewater.19,29,32,33,34 For the epidemiological tracking of SARS-CoV-2 infection in large populations at relevant scales, wastewater monitoring could serve as a potentially useful technique. 35 Despite the uncertainty and heterogeneity in the input parameters, 19 the model calculated a median range of 171 to 1090 infected individuals in the catchment, which was a reasonable agreement with the clinical observation. Sewage from different inlets and outlets in China has been found to contain SARS-CoV-2 RNA. Three sewage samples from the inlets of preprocessing disinfection equipment were found to contain the viral RNA with cycle threshold values of 29.37, 30.58, and 32.42, respectively. Likewise, the sewage sample from the outlet of the preprocessing disinfection pool was weakly positive with a cycle threshold value of 33.55. The sewage sample taken from the final sewage disinfection pool outflow, however, came up negative. 35
The wastewater plumbing system and its specific design can harbor pathogenic microorganisms which enhance the potential for enabling airborne transmission of viruses such as SARS-CoV-2 whenever it is accompanied by the generation of aerosols. 14 We emphasize that it is conceivable for SARS-CoV-2 RNA to be present in wastewater and that WBE can serve as a sensitive as well as an early warning tool. A study demonstrated the presence of SARS-CoV-2 in sewage which can be focused on determining the circulation of the virus in the human population. The quantification of SARS-CoV-2 in wastewater affords the ability to monitor the prevalence of infections amongst the population through WBE. 28 Since wastewater contains viruses discharged from both symptomatic and asymptomatic persons in a catchment, WBE is a potential method for determining the prevalence of viruses in a specific wastewater treatment plant (WWTP) catchment population. 36 It is conceivable for SARS-CoV-2 to be transmitted enterically, and exposure to SARS-CoV-2 through sewage might be dangerous to one’s health. SARS-CoV-2 environmental surveillance may provide information about whereabouts the infection is spreading among the given population. 37 Longitudinal analysis of wastewater can provide population-level estimates of the burden of SARS-CoV-2 where in-person testing may not be available. 18
Through the quantification of viral genomes in the wastewaters of Paris, the effects of lockdown on SARS-CoV-2 dynamics were assessed. Viral genomes in the wastewater could be detected before the beginning of the exponential growth of the epidemic and subsequently marked decrease in the quantities of the genome units as observed concomitantly with the reduction in the number of new COVID-19 cases which was an expected consequence of lockdown. 14 Even though the prevalence of COVID-19 in sewage is low, the virus was found in sewage, indicating that sewage monitoring might be a sensitive technique to track the circulation of the virus. 17
Disinfection Technologies to Eliminate SARS-CoV-2
Typically, the process for disinfecting hospital wastewater includes the units in order of primary disinfection, sedimentation, dechlorination, moving bed biofilm reactor, repeated disinfection, and discharge (Figure 1). The most often employed disinfectants used for disinfection of hospital wastewater disinfection include sodium hypochlorite, liquid chlorine, chlorine dioxide, ultraviolet irradiation, and ozone. 24 Disinfection using chlorine dioxide, liquid chlorine, and sodium hypochlorite is preferable. 38 The presence of the RNA of the SARS-CoV-2 virus has been detected in untreated wastewater (influents) in WWTPs and secondary treated water samples. 30 The presence of SARS-CoV-2 viral RNA may be eliminated by using modern disinfection techniques, such as sodium hypochlorite, a combination of hypochlorite and ultraviolet, peracetic acid, and high-intensity UV lighting at the tertiary effluent sample of WWTPs.30,39
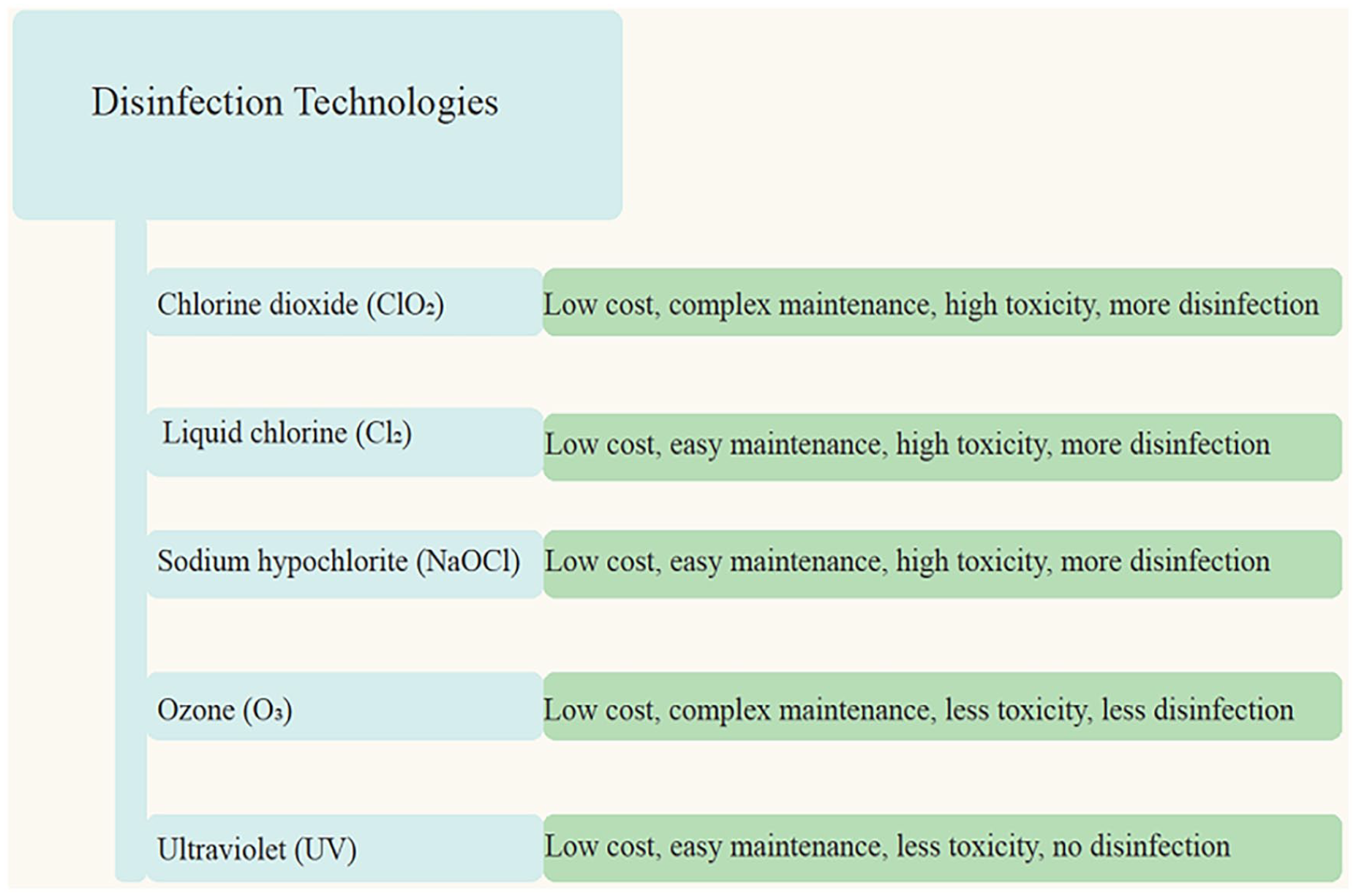
Comparison in the selection of various disinfection technologies for hospital wastewater based on different factors and conditions.
In general, all SARS viruses may be rendered inactive by using ordinary disinfectant technologies, however, chlorine and UV irradiation disinfection may be the most effective among others.38,40 Although several studies are being conducted on the best disinfection technique for wastewater treatment, they have not yet reported on the specifics of the disinfection procedure or its efficacy against the SARS-CoV-2 virus.
A recent study conducted by Zhang and his co-workers on medical wastewater for the determination of effective deactivation of SARS-CoV-2 utilizing sodium hypochlorite was done to revise the existing standard of disinfection for improving efficacy. Furthermore, the findings demonstrated that free chlorine concentrations of >0.5 mg/L (contact times of 1.5 hour) were insufficient to completely eradicate the SARS-CoV-2 virus in wastewater. Thus, 6700 g/m3 of sodium hypochlorite was employed to completely disinfect the SARS-CoV-2 virus in wastewater. However, the ecology and public health may be seriously threatened by the application of this high concentration of disinfectant and its disinfection by-product residuals. 23
Importance of SARS-CoV-2 Surveillance in Wastewater to Ensure Public Health
Public health and economic progress were impacted by the pandemic. 5 Since the discovery of the epidemiological surveillance of pathogens in wastewater systems in the 19th century, it has made a substantial contribution to the surveillance of highly transmissible infectious illnesses. 41 In theory, a sewage system stores the biological waste that it carries from the human population. Along with the biological components, pathogens enter the sewer system through excreta such as feces, urine, saliva, and other excretions. 42 Wastewater testing has previously been utilized to monitor for significant health hazards like antibiotic resistance, population-level illicit drug usage as well as the presence of viruses (e.g., Vibrio cholerae, poliovirus) in a community.43,44 Monitoring a community’s wastewater and sewage has proven to be an effective approach to predict both minor outbreaks and epidemics of enterovirus and adenovirus disease.45-47 Detection of harmful viruses in sewage systems has offered early warnings of viral epidemics such as Hepatitis A virus and Norovirus even before the causing infections were identified in healthcare as shown by previous studies.27,48 This information facilitates informed and timely public health responses from the concerned authority. 41 Wastewater surveillance is a useful addition to the surveillance pyramid because it offers mass monitoring using a low-cost, effective, and non-invasive method. Furthermore, it can uncover prevalence rates that are “hidden” by asymptomatic infections, poor health facilities, and situations with restricted diagnostic capability.49,50
Wastewater surveillance for the SARS-CoV-2 presents both opportunities and challenges. The propensity of this method to make quantitative projections from the viral RNA is often constrained by the complexity of wastewater matrices, the diluted nature of biomarkers in wastewater, the difficulty in identifying the ideal sample locations, and the need for efficient virus-concentrating methods.51,52 In addition, specialized tools and expertise are needed for the precise measurement of virus levels in wastewater mixes, and quality assurance methods different from clinical testing are needed for precise molecular quantification. 41 Therefore, some technical and practical challenges must be addressed before applying this surveillance method.
Challenges to Disinfecting Wastewater to Eliminate Viral Pathogens Like SARS-CoV-2
Many readily accessible disinfectants can effectively combat SARS-CoV infections on surfaces or in water. Many of these disinfectants are common chemicals like alcohols, chlorine, hypochlorite solutions, and ozone that are cheap, simple to apply, and exhibit quick and excellent biocidal activity. 30 Since free chlorine could effectively inactivate SARS-CoV-2 by damaging the proteins on its envelope, chlorine disinfectants are now the most popular. However, excessive use of disinfectants might result in their entry into nearby water sources or the sewer system of the city via wastewater or rains leading to the accumulation of disinfectants and its byproduct in surface waters. 53 These disinfection byproducts (DBPs) present risks to human health. 54 For example, the use of the most popular disinfectants like chlorine provides numerous benefits, but it has been found to produce harmful and carcinogenic halogenated by-products Likewise, the effluent was found to contain large amounts of DBPs due to the usage of very high doses of sodium hypochlorite. 53 Wavelengths of ultraviolet radiation between 200 and 300 nm are considered effective in degrading the genetic makeup of bacteria, viruses, and other microbes, inhibiting protein production. However, it is considered a relatively unsuitable method due to insufficient depth of penetration and also contains some health hazards. Similarly, viruses have a higher level of ozone tolerance than bacteria. 55 The genomic structure of the virus responsible for the production of different proteins (structural, non-structural, and accessory proteins) that make them contagious should be also noted. 56 Therefore, a suitable approach utilizing either a single effective method or combining different methods for the precise elimination of viruses is warranted.
During the low- and middle-risk COVID-19 periods, the SARS-CoV-2 RNA has been found in groundwater, surface water, wastewater, sludge, and other hospital-related water systems.5,57 However, there is no suitable standard procedure for RNA detection in wastewater. The method employed to determine the virus concentration is not very effective at recovering these viruses.58,59 Currently, the fastest approaches for promptly detecting viral infection at the source include nucleic acid-based detection methods such as real-time quantitative polymerase chain reaction, recombinase polymerase amplification, CRISPR-Cas based nucleic acid detection, loop-mediation isothermal amplification and immunoassay techniques such as enzyme-linked immunosorbent assay, blotting assays, and lateral-flow immunoassay. 60 The most beneficial method for detecting viral nucleic acids is still quantitative reverse transcriptase polymerase chain reaction (qRT-PCR), which has the advantages of specificity, speed, high throughput, and reliability. 61 RNA of SARS-CoV-2 has been using electronegative membrane-direct RNA extraction, ultrafiltration, ultracentrifugation, and PEG precipitation with the sequence confirmation through directing sequencing of qPCR products (Sanger sequencing) in different parts of the world. 62 Independently assessing new technologies can provide various diagnostic approaches that enable faster and more precise screening of those who have been reported to be contaminated. Implementing precise and timely testing procedures is crucial for effectively combating epidemics. The reliance on test applications for clinical diagnosis and disease detection, however, places restrictions on conventional epidemic testing. This can be avoided by routinely expanding the wastewater surveillance method’s community of people being tested until a critical level of positive case detection is attained. This will show how quickly an infection is spreading within a population. Therefore, to greatly increase the detection rate, more thorough and stringent testing is essential.
Conclusion and future prospective
This review concentrated on the occurrence and transmission of SARS CoV-2 in sewage and employed WBE to track the virus in the neighborhood. RNA of SARS-CoV-2 has been detected in feces,63,64 urine,65-68 blood, 69 respiratory secretions,70-72 oropharyngeal and tracheal secretions,65,73,74 ophthalmic and conjunctival secretions.75,76 SARS CoV-2 is acquired via wastewater together with human waste products including feces and urine and then circulates in the sewage system. According to the review, the presence, and dynamics of the virus in sewage can be used as a tool to track the infection or transmission within the community. However, further research is needed to determine how sewage virus aerosols (bioaerosols/aerosols) spread COVID-19 to people. Wastewater pipes should be appropriately treated with the right disinfectant technologies before discharge since the stool-embedded SARS-CoV-2 virus particle works as a secondary source of infection and also stays for a longer amount of time depending on various causes or situations. Monitoring the SARS-CoV-2 genome quantitatively in wastewater can help track the spread of the viruses in underdeveloped countries. Treatment for viral inactivation can lessen the virus’s load on the environment and secondary transmission. It is possible for the virus to spread to different organisms, experience mutation, and alter properties. For the foreseeable future, several situations should be taken into account. Future research must also be done on the possibility of viral transmission in aerosols released from wastewater or sewage systems. Additionally, the ecology and public health may be seriously threatened by the application of a high concentration of disinfectant along with its persistent disinfection by-products. As a result, other methods for disinfecting wastewater must be developed.
Footnotes
Acknowledgements
We appreciate the authors of the works cited in this article for their efforts in the struggle against COVID-19. We also want to express our gratitude to all the experts from the Nepal Academy of Science and Technology, Lalitpur, and the Central Department of Microbiology, Kathmandu for their constructive suggestions while writing.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Prashanna Koirala—literature search, methodology, illustrations, data interpretations, manuscript writing, revision, and edits. Sandesh Dhakal—literature search, manuscript writing. Bikram Malla—Edited the manuscript. Archana Ghimire—literature search, manuscript writing. Mohammad Ataullah Siddiqui—literature search, manuscript writing. Prabin Dawadi—conceived and contributed to study design, literature search, methodology, illustrations, data interpretations, manuscript writing, edits, and revision.
