Abstract
In MDR-TB, mycobacterium is resistant to battlefront drugs like rifampicin and isoniazid. Now it’s an urgent global challenge for treatment & diagnosis because more than 50% of drugs are resistant. Till today's information, 5 reasons are liable for MDR: (1) Errors of physicians/patients in therapy management, (2) Complexity and poor vascularization of granulomatous lesions, which obstruct drug distribution to some sites, leading to resistance development, (3) Intrinsic drug resistance of tubercle bacilli, (4) Formation of non-replicating, drug-tolerant bacilli inside the granulomas, (5) Development of mutations in Mtb genes, which are the foremost important molecular mechanisms of resistance. the most contribution of this work is a brief & clear explanation of things chargeable for resistant development, and recent diagnostic & treatment methods for MDR-TB. This study shall help researchers & scientists to develop replacement rapid diagnostic tools, drugs, and treatment protocols.
Introduction
What is tuberculosis?
Tuberculosis is one of the oldest diseases caused by a bacterial species known as “Mycobacterium tuberculosis” which severely affects the lungs. It is the most common organ to grow Tuberculosis, about 85% of patient with TB complains of pulmonary issues. However, in the case of tuberculosis, the infectious agent has a tendency to infect any body part likely the brain, kidney, and spine. 1 If someone is infected with TB bacteria, is not always become sick. Based on these characteristics, TB infection could be categorized into 2 forms: (i) tuberculosis (TB) disease and (ii) LTBI (latent tuberculosis infection). WHO estimated almost 2 billion people have latent Tuberculosis in the world. India comes in the top country having the greatest number of multi-Drug resistance patients. So, drug resistance in Tuberculosis becoming often common. Some other strains of tuberculosis are also present, So the problem of Drug resistance increasing every day. Because Mycobacterium strains have become resistant to drugs used as first-line treatment like rifampin and isoniazid. So, resistance development guidelines need to be updated.
What is the meaning of MDR or resistance in tuberculosis?
With an increasing number of MDR-TB, it is challenging the globe's urgent bases to control it before its spread to another level of drugs used in TB. If the patient is infected with TB strains and was resistant to medicine (antibiotics) used as first-line treatment, called multidrug-resistant (MDR) TB. These first-line treatments and the most effective antibiotics are rifampicin and isoniazid. More than half of drug resistance in tuberculosis comes from India (24%), China (13%), and Russia (10%). These are the top 3 countries. Wrong medication and incomplete course for TB lead to MDR-TB, in India and it is very common. In the year Dec 2014 Buczynski et al 2 , and Feb 2016 Jen et al 3 , had reported that 58% and (44/72, 61%) of patients respectively were having at least one type of error. The most common type of error was associated with doses of first-line drugs. Even, they found that during the hospitalization of patients, 85% of errors remained incorrect. In 2016, the WHO recommended intense chemotherapy for MDR-TB with some TB drugs. Association between mutations affecting the function and expression of chromosome-encoded targets and resistance to anti-tuberculosis drugs, methods, and molecular techniques have emerged ask comment.4,5 We revised the latest available information on the diagnosis, treatment, and prevention of MDR-TB.
Objective
To analyze recent developments in multi-drug resistance tuberculosis research.
To review and characterize the mechanism of drug resistance. and characterization of the mechanism of drug resistance.
Nowadays the MDR-TB may be a global challenge and therefore the world is accepting this fact. There are a few technologies and strategies which improve fast and accurate diagnosis moreover as in the treatment of MDR-TB. This review is going to help to grasp recent technology and strategies associated with MDR-TB. It will help to develop a brand-new methodology for diagnosis and treatment to cure global MDR-TB.
Type of Drug-Resistant Mechanism in TB
Bacteria have a remarkable genetic plasticity that permits them to fight a wide range of environmental threats, along with the residence of antibiotic molecules which can endanger their existence. As mentioned in reports, microorganisms sharing an identical ecological area of interest with antimicrobial-generating organisms have grown. Historically these mechanisms are developed in the bacteria to resist the impact of the dangerous antibiotic molecule and the environment. 6
Primary Resistance Pathway—when someone is infected with a strain that is resistant to Tuberculosis drugs. For instance, if an individual is infected with a mycobacterium resistant to the first-line tuberculosis drugs through coughing, sneezing, speaking, or singing. In this case, treatment of these drugs is not going to work on that individual. There is a need to treat them with new drugs or combinations of the drugs.
Acquired Resistance Pathway—when someone is infected with a strain that is susceptible to Tuberculosis drugs and gets an inadequate treatment that leads to resistance development with drugs vis mutation in strain. These types of resistance are developed by a mutation in the mechanism of (i) antimicrobial targets (decrease the affinity of drugs for the targets), (ii) drug uptake (iii) efflux mechanism (iv) Metabolic pathways of Mycobacterium . 7 Once the resistant strain of mycobacterium emerges, the antimicrobial drug kills only the susceptible strain of bacteria for antibiotics, but the resistant strain predominates. In many cases, these mutant strain leads to damage to the homeostasis of the cell (ie, decrease fitness).
These reasons encompass all aspects of mycobacterial treatment, including microbiological, clinical, and biological, responsible for the resistance generation.
(1) Lack of adherence to therapy by the patient and/or errors on the part of the physician in administering the therapy
(2) Poor granulomatous lesions vascularization and Complexity, lead to resistance development8,9
(3) Intrinsic drug resistance of tubercle bacilli 10
(4) Formation of non-replicating, drug-tolerant bacilli inside the granulomas 10
(5) The emergence of mutations in the Mtb gene is the crucial biological mechanism of resistance
This chapter is going to deliver more on Mycobacterium resistance with proper explanation and examples (see below; chapters 3.1-3.5).
Management errors in the treatment of Mtb
It is the result of human behavior and the carelessness of humans in treatment. There are several things responsible for poor outcomes in treatment which also include acquired drug-resistant tuberculosis. These factors are -
(1)
(2)
(3)
Complexity of TB granulomas
Tuberculosis disease takes months to a year for its treatment, resulting in its attributes in complex pathology of Tuberculosis. In Both types of TB (active and latent), an oversized range of heterogeneous granulomatous lesions from cellular granules that are well vascularized to caseous granules that are avascular, co-exists. Vascularized granules contain neutrophils and macrophages that are surrounded by the rim lymphocytes, while avascular caseous granules contain a necrotic center that is developed by the host cell lysis and bacteria. In this comportment, the tubercle Bacilli range from actively replicating (AR) stages, especially in vascularized granules to dormant slowly replicating or NR stages, especially in avascular caseous granules. In Mtb-infected animal experiments (on Rabbits), reported that some unbound Anti-tuberculosis drugs penetrate through the caseum by passive diffusion. Currently, 4 drugs that are effective against the intracellular bacilli of AR stages are PZA-RIF-INH-EMB. But it is not effective as the same accuracy for the extracellular bacilli of NR stages. Temporal and spatial differences in the distribution and accumulation kinetics of medicine in lesion-specific comportment may create a window for the development of drug resistance. 11
When caseous granulomas enlarge, the necrotic centers join also with bronchial airway structures to create pulmonary cavities, that either contains both intracellular and extracellular bacilli deduced from the solubilization of phagosomes of the cavities as well as from liquefied caseum. These bacilli multiply quickly when exposed to ambient oxygen in the cavity's lumen. Thus, in pulmonary cavities, a high bacterial load is found. There is an opportunity that a few bacteria undergo the chromosomal changes and pass this mutation into the next generation and thus develop resistance to front-line medicine used for the treatment of Mtb.
Intrinsic Mtb drug-resistance
Evolution is responsible for the development of many good characters. Mycobacteria additionally follow this character and Efflux channels, Cell envelope, and other mechanisms were used by Mtb to build intrinsic antibiotic resistance mechanisms (drug degradation, target modification and general modification mechanism). This mechanism is allowing the bacteria to succeed in high drug resistance levels.
Cell envelope
Mycobacterium cell envelopes are made up of the long-chain mycolic acids (MA), the periplasmic space (PS), the arabinogalactan (AG), a network of peptidoglycan (PG), the cytoplasmic membrane, and a loose matrix with the help of both secreted proteins glycan have formed the capsule. Our first-line TB drug inhibits MA synthesis by INH drugs, while inhibition of AG Synthesis is achieved by the EMB drugs and it is also made Mtb to susceptible other drugs. 12
It is also believed that the deepest hydrophilic layer of AG and PG prevents hydrophobic molecules from penetrating them. Instead, the AG and PG layers are connected to the layer of the hydrophobic MA at the exterior of the envelope, which is made of long-chain fatty acids and prevents the entrance of hydrophilic medicines. 13
On other hand, these drugs penetrate either by passive transport into or through the cell membrane which is rich in lipid components. Mutation into the cell membrane components increases the intrinsic type of resistance to the drugs. for example, mutated Mycobacterium smegmatis by the mycolate defective exhibited enhanced vulnerability to first-line drug RIF, novobiocin, chloramphenicol (CF), and erythromycin. 14
Some small hydrophilic drugs pass through semipermeable membranes without using energy through the water-filled porins. A minimum of 2 porins was synthesized by the Mycobacterium tuberculosis like rv0899 and rv1698 made 1 porin—OmpA. 15 But the penetration of hydrophilic types of antibiotics category β-lactam via the cell wall of mycobacterial was about a 100 times lower than penetration of it within the E. coli cell membrane. Thus, it is assumed that Mycobacteria cytomembrane components like β-lactam help in resistance to first-line antibiotic use in the treatment of TB.16,17
Drug efflux
Cells have many transmembrane protein transmembrane proteins that allow the expelling of medication from the cell interior to the cell exterior, these 5 transmembrane proteins are called drug efflux. Based on energetic and structural properties, these are organized into 5 classes of ATP-binding cassette (ABC) superfamily 18
(1) Major facilitator superfamily (MFS) 19
(2) Multidrug and toxic compound extrusion (MATE) family 20
(3) Small multidrug resistance (SMR) family 21
(4) Resistance nodulation division (RND) superfamily 22
On one side where the ABC members which are energized by ATP, are known as primary transporters. On the opposite side, except for ABC other transport that gets energy by sodium gradient or proton gradient, are known as secondary transporters for instance (MATE) and (MFS, RND, and SMR) respectively. Most efflux pumps of Mycobacterium belong near 2.5% of the complete genome of the ABC family), SMR family, RND and MFS superfamilies.
When a medication is interacting at the sub-inhibitory concentration for a prolonged time with Mycobacterium tuberculosis, it promotes to development of low-level resistance by overexpressing efflux pump genes. When a patient gets inappropriate treatment for TB, it converts into a high level of resistance. Several studies are suggesting this, for example, Mycobacterium tuberculosis exposure to first-line drugs like INH promotes the overexpression of mmR EP and MmpL7 genes. Furthermore, the number of efflux pumps is linked with resistance development for many drugs. 23
Other modifications
There are mainly 2 reasons liable for MDR-TB developments, the first is cell envelope and the second is efflux pumps. Another reason is related to the modification of the targeted receptors, inactivation or modification of the drug's antibodies, neutralization of the toxic substances, etc.
For instance—The drug-inactivating enzyme, Mtb β-lactamases liable for slow penetration through the semipermeable membrane and it has a low affinity for the protein that binds to the penicillin protein of Mtb. It is ok to come up with Mycobacterium intrinsically immune to most of the β-lactams proteins. 13
Mtb is of course immune to macrolides due to an rRNA methyltransferase and inducible erm (37), that affect ribosomes by methyltransferases 23 srRNA. clarithromycin and azithromycin are samples of macrolides.
Phenotypic drug-resistance
There are many studies suggesting that the population of the Mycobacterium which is phenotypically drug-resistant but genetically susceptible, is usually stated as persisters. This strain is found in cavities of the lung and caseous granulomas of tuberculosis patients. Persisters have characteristics of drug tolerance that are not heritable and are pursuable of their growth because the concentration of the drug is removed. Persisters also can survive because the drug stands there.
On the premise of their availability, it is often characterized into 2 types:
(1) Class I (Rare)—It is mainly found in replicate populations. They are films typically resistant to different drugs by a different mechanisms. Their overall population of Mtb may be killed by using drug combinations.
(2) Class II (Abundant)—It found almost all the populations of the cell. for instance, within the stationery, phase hypoxic condition, nutrition starvation. It is resistant to a protracted range of medicine; therefore, it is necessary to develop a brand-new antibiotic to beat these situations.
They get phenotypically resistant meanly via dormancy, but dormancy is not sufficient to develop the gap. There are other additional characteristics important to develop resistance that is found in many other in vitro stress Model studies.
There are a few models which are used to test the level of resistance in vitro, their results vary with the selection such as stress models, nutrient starvation, antibiotic-starved strains, stationary phase, hypoxia (Wayne dormancy model), acids/nitric oxide gas. 10
For example, In the Wayne model, through gradual adaptation of anaerobiosis, dormant bacilli are obtained. By an oxygen gradient that achieves by self-generated and along with this NRP (non-replicating persistence) stages 1 and 2 have been noticed. A thickened outer layer was developed by NRP-2 cells that aided in restricting first-line drug entry like RIF entry.
Acquired drug resistance
Group of a distinct drugs is employed to treat tuberculosis. Each and every molecule of drugs interacts with at least 1 or 2 or more targets to perform its functions means inhibiting Mycobacterium growth. As TB treatment is a concern for a very long time (months to a year), pushing the development of mutation into targeted sites of clinical strains. 13
On the premise of the main incidence, the review reports a specific mechanism that involved the genetic of Mtb induced this resistance to these drugs like CP, RIF, KM, INH, and others. In the following table of conferring resistance of the (WHO groups A, B, and C), drugs, targeted genes just in case of mutation, and gene products are given here (Table 1).
Drugs of TB and affected gene product.
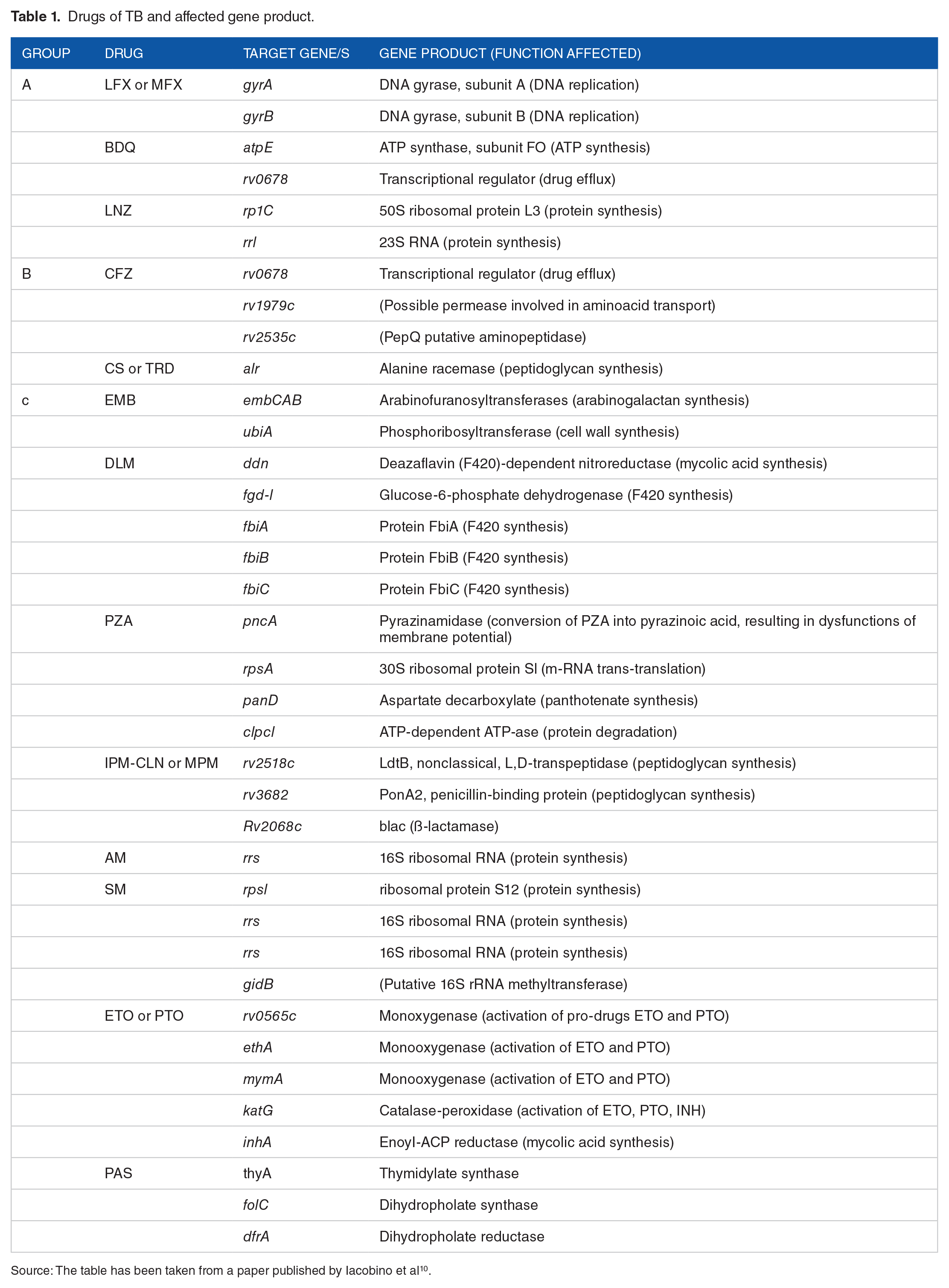
Source: The table has been taken from a paper published by Iacobino et al 10 .
Diagnosis of MDR TB
The following scenario was used to diagnose Mycobacterium tuberculosis:
(1) Drug susceptibility testing (DST)- is the oldest one and phenotypic testing continues to be considered the gold standard and accurate for, Mtb But this system takes a minimum period for results.
(2) However, some new techniques are developed which are rapid and also accurate for Mtb diagnosis. These techniques rely on the identification of the chromosomal mutation, including target gene sequencing, line probe assays, whole-genome sequencing, RIF/Xpert MTB system (USA, Cepheid, CA, Sunnyvale), DNA/RNA macromolecule amplification devices. 10
According to the 2022 report of TAG, 24 WHO recommended some new diagnostic tests for non-invasive samples by Cepheid's Xpert MTB/RIF Ultra in the year 2020. The other diagnostic technique also released in 2020, known as Xpert XDR can detect resistance to OFL, KM, INH, AK, and MFX. In the year 2021 for molecular testing, several protocols are standardized for the preparation of stool samples including simple one-step techniques and optimized source flotation.25,26,27 Stool samples (Non-invasive) increase the collection and diagnosis of samples in children; however, it is less accurate. Because its sensitivity is 56.1% and the specificity is 98.0%. On the other hand, samples that are more invasive like gastric aspirate show more accuracy with their high sensitivity (70.4%) and specificity (94.1). 28 WHO recommended, the use of artificial intelligence (AI), Computer-aided detection has been permitted for adult diagnosis based on X-ray databases but not children in 2021. A number of other non-sputum diagnostics are also promising for improved pediatric Mtb diagnosis; these are the TAM-TB blood test of Beckman Coulter and fingerstick blood test of “Cepheid's Xpert MTB-HR” designed for detecting of progression of LTBI to active Mtb.29,30
Commercial reporter gene assays recommended by the TAG as centralized DST “Nipro NTM+MDRTB detection kit2” and “GenoType MTBDRplus Version 2.0 (Hain Lifescience, Nehren” have been licensed by the WHO. From 2015 to 2019 many other systems were marketed, and the way of new centralized determination evolutionary techniques of molecular resistance have been approved by the WHO. these are supposed to use in RIF and INH, and these are a few examples—(i) Cobas MTB-RIF/INH that is developed by Roche, Basel, Switzerland, (ii) MTBDR version 2.0 based on Fluoro type for first-line drugs by Hain Life science. 31
Solutions and Methodology for Treatment for MDR-TB
In recent past years, Multidrug-Resistant tuberculosis (MDT-TB), which is a growing incidence of various parts, is not restricted only to developing nations, but even it is also spread to many industrialized and developed nations. Being a new challenging situation of the TB resurgence, especially with a strong impact worldwide and rapid emergence, it is important to develop new protocols and new categories (development of a vaccine against Mtb or monoclonal antibody 32 ) or combinations (combine the use of bedaquiline and pretomanid regimens33,34 of medicine in replacement of anti-tuberculous first-line drugs for effective clinical control and treatment of TB patients.
Complexity of TB granulomas resistance
The problem related to the Complexity of TB Granulomas mycobacterium resistance (discussed under Section 3.2) is the formation of a drug gradient into the caseous granulomas which promotes resistance to Mtb. The categorization of these granules is very difficult special in the brain cells and to target each type of granules during Mtb treatment, the characterization of granules could play key roles. To quantify the molecular weight of these granules, a metabolomic can be used. 35 Even, the use of the proteomic tool can explore in analyzing the proteins of various complex cellular processes which help in drug discovery.36,37 This problem is often addressed by making the combination of new drugs or regimes such as PZA-RIF-INH-EMB drugs effective against the AR stages of bacilli in granulomas. Oxazolidinones and Ethylenediamine are the new lead compound used for protein synthesis and multiple pathways respectively. 38 A few new regimes that are under development are depicted below (Figure 1).
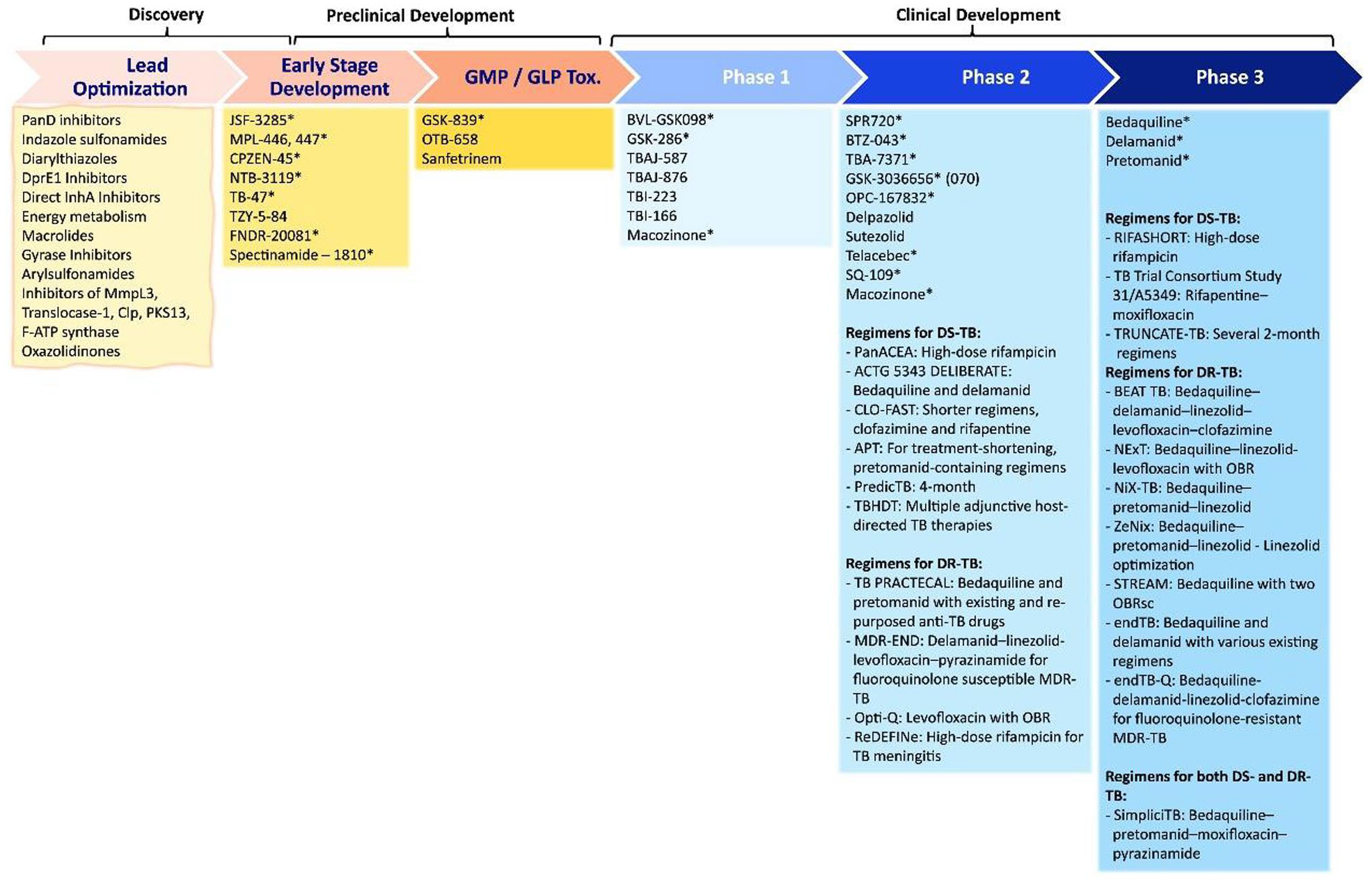
New regimes that are under development.
For rapid diagnostic tools and treatment methods, the use of proteomic and metabolomic should be more common.
Cell envelope resistance
The problem related to Cell Envelope mycobacterium resistance (discussed under Section 3.3.1) is the inhibitory response of the cell membrane to hydrophobic drugs and mutation into cytomembrane proteins (ie, porin proteins) which leads to resistance for little hydrophilic drugs. It is often overcome using the more lipophilic drug which may penetrate through a waxy bacterial plasma membrane. However, this issue is maybe more complicated, because some research advance report found that lipophilicity plays a vital role, but it is not an exclusive factor that play role in compound permeability. 39
Phenotypic drug-resistance of Mtb
The problem of drug resistance related to the phenotype of Mtb (under Section 3.4) is that persisters behave as a sort of reservoir for evolutionary/mutation to resist the primary line drugs. Thus, scientists and researchers should aim to develop a drug against these persisters (dormant Mtb). Then, it will reduce the time of treatment of tuberculosis and help in reducing MDR-TB. According to Lanni et al 11 and Iacobino et al, 40 the combination of Rifapentine and Rifampin at a neutral pH of 7.3 has shown significant results in the killing of the Mtb persisters. Not only one, but even, the combination of other drugs such as Nitazoxanide and Rifampin are equally effective against the dormant Mtb. 41 Our research area should also cover a higher understanding of the relationship between resistance and persistence, which will help in developing new, unique and novel drugs and drug combinations to combat and eliminate both types of bacilli, NR and AR.
Diagnosis improvement
Researchers are working day-night to develop a rapid and early diagnostic kit for the Mtb. A few of them are in the under-development stage and are mentioned below.
Research Gaps, Status, and Feature Trends
Concerning the event of the latest antituberculosis drugs, the subsequent points are important:
(1) Development of long-lasting antibacterial drugs and their activity should be tested in in-vivo. These types of drugs facilitate administration at long intervals, patients’ compliance and consequently directly observed therapy.
(2) There is an urgent must to develop a unique compound for MDR-TB.
(3) The development of a drug for the NR stage of Mtb or slow metabolites Mtb or if possible, for dormant populations of MTB organisms is a game-changer in the treatment of MDR-TB.
(4) To beat efflux pumps drugs resistance, scientists should be considered study on oligonucleotide mimics and PNAs (peptide nucleic acids). Their high specificity of supermolecule binding has the aptitude to beat efflux pumps’ drug resistance. We would like to explore more antibodies as drugs for Mtb treatment.
(5) By using advanced and recent bioinformatics/proteomics/genomics tools, 3D protein/drugs for Mtb can rapidly develop.
(6) Require a sustainable production of medication that may be little commercially beneficial for producing company.
Unfortunately, there are no new drugs are released 50 years after rifampicin in all told countries except the U.S. (rifabutin and rifapentine).
There is a variety of things that have discouragement companies to invest in and investigate new antituberculosis drugs. The research and development are very costly, and it is slow as well as difficult to develop new ant-TB drugs. The bacteria tubercle bacillus requires sophisticated, specialized lab facilities for working and handling it. But there is no. of model animals which mimic human tuberculosis and make it a little easy to work on it. That is why developing any anti-TB drug will take a while and is therefore very difficult.
The best prevention for MDR-TB is merely to forestall normal TB to converting into MDR-TB. Early diagnosis and treatment of MDR TB are not enough for a cure, effective and novel drugs also are required.
Because use of multi-drugs at the time for treatment of Mtb, Now, more than 50% have tolerance for MDR-TB. the globe has to be alert for this upcoming Mtb resistance problem with front drugs, otherwise, something is going to have happened like SARS-CoV2.
Conclusion
The successful control of MDR-TB from tuberculosis could be a significant challenge and combat worldwide. The overall summary is this, the comprehensive microbiological, biological, and clinical issues supporting resistance development in Mycobacterium have been provided during this review of the literature. This review paper also addresses all possible available solutions to combat tuberculosis. A few of them are used in the world as well as in India while a few of them are still in the under-development stages like vaccine development, monoclonal antibodies as drugs, and FISH, RDT-based techniques (nucleic acid amplification, microarray) and MALDI-TOF for the diagnosis purpose. In our opinion, even, scientists and researchers should be focused on WGS diagnostic method. Because the curve of HRM and WGS method which is used to scan for mutation of Mycobacterium is a convenient, rapid, highly accurate and sensitive technique. Thus, it will help in reducing the cocktail of medication for treatment, and long exposure to a sub-inhibitory concentration of medication. This effort will reduce MDR-TB development. Apart from the challenges and solutions of MDR tuberculosis, even this paper briefly comments on gaps between the research and what action can be taken to reduce it, what is the future trend of the researcher on MDR-TB such use of proteomics techniques on diagnosis, antibody and vaccine for treatment and cures. Finally, this critique supported the recent updates on mechanisms of drug resistance reported in the past few years within the different—different literature on various sources. This review paper also quotes recent guidelines from WHO on the behalf of international recommendations to facilitate the management of MDR and XDR tuberculosis by microbiologically and clinical facilities at the global level.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
PY significantly contributed to the compilation and analysis of data, manuscript drafting, and overseeing various stages of manuscript preparation, including reviewing, revising formatting, proofreading, and approving the final manuscript.
