Abstract
Objective:
This systematic review and meta-analysis aimed to assess the pool estimates of extended-spectrum β-lactamases producing K. pneumoniae (ESBL-KP) and study their drug resistance profile by evaluating the studies from Nepal.
Methods:
A literature search was carried out in PubMed, Google Scholar, and NepJOL to screen all articles on ESBL-KP published between 2011 and 2021 from Nepal. This review was conducted following Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines. Relevant data were extracted, and R language 4.2.0 software was used for statistical analysis.
Results:
The pooled prevalence of K. pneumoniae was 5%, while the pooled prevalence of ESBL and multidrug resistance (MDR) in K. pneumoniae were 23% and 55%, respectively. Imipenem was the drug of choice (in vitro) against ESBL-KP infection.
Conclusion:
Our analyses showed a high prevalence of ESBL-KP and their high resistance toward commonly used drugs. This study highlights the need for the development of new antibiotics for the management of ESBL-KP infections.
Introduction
The increasing incidence of antibiotic-resistant bacteria is a concern both to clinicians and patients due to implications such as therapeutic failures, prolonged hospitalization, and nosocomial infections. Extended-spectrum β-lactamase (ESBL) producing bacteria have been reported to be a common cause of healthcare-associated infections, which can have serious clinical consequences and result in multiple drug resistance.1,2 ESBL enzymes hydrolyse penicillin, oxyimino-cephalosporins such as third-generation cephalosporins, and monocyclic amide antibiotics such as aztreonam but are inhibited by sulbactam, tazobactam and clavulanic acid.3-5
Enterobacteriaceae is the major family of bacteria associated with ESBL production. 6 ESBL-producing Enterobacterales were placed under WHO critical priority pathogen list for research, innovation and new drug development. 7 In Enterobacteriaceae family, K. pneumoniae is one of the common ESBL-producing members with the potential to cause infections in both hospital and community settings, resulting in increased morbidity and mortality as well as high medical expenses. 8
The initial occurrences of ESBL-KP were reported in Europe in 1983 9 and the USA in 1989 10 and since then, there has been a continuous increase of K. pneumoniae-mediated cephalosporin-resistance around the world.11-13 During the late 1980s, ESBL-KP outbreaks were mostly generated by TEM and SHV producers.5,14 Recently, the CTX-M enzymes-producers have increased throughout the world.15,16 These ESBL encoding genes are commonly found on mobile genetic components, such as plasmids, which frequently carry genes conferring resistance to other classes of antibiotics such as aminoglycosides, fluoroquinolones, chloramphenicol, and trimethoprim/sulfamethoxazole.17,18 As a result, many of these bacterial strains are multidrug-resistant (MDR) and infection by these drug-resistant isolates increases the likelihood of treatment failure and may lead to death.8,19,20
South Asia has been identified as a hotspot for antimicrobial-resistant bacteria.21,22 The problem has been frequently accounted in developing countries such as Nepal, where the prevalence of MDR and ESBL-producing bacteria has increased over the past years.23,24 There are some scattered studies that reported ESBL-KP in Nepal. However, these are not available in an organized form. To the best of our knowledge, this is the first systematic review and meta-analyses on the burden of ESBL-KP in Nepal. This study aimed to estimate the pooled prevalence of ESBL-KP and their antibiotic resistance profile and the relationship between ESBL production and multidrug resistance by analyzing available studies. This study could aid in designing and implementing hospital infection control strategies to minimize the occurrence and spread of ESBL-KP.
Methodology
Literature review and data sources
A comprehensive literature search was conducted to identify all articles published between January 2011 and December 2021 reporting the prevalence of ESBL-KP from human specimens in Nepal. It was carried out through the electronic databases PubMed, Google Scholar, and NepJOL using the following terms: ‘Klebsiella pneumoniae’, ‘extended-spectrum β-lactamases’, and ‘ESBL’ together with ‘Nepal’. Searches were limited to articles published in English language. Discussions and references of the selected studies were thoroughly scanned for locating additional relevant articles. This study followed the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines for reporting systematic reviews and meta-analyses (Figure 1).
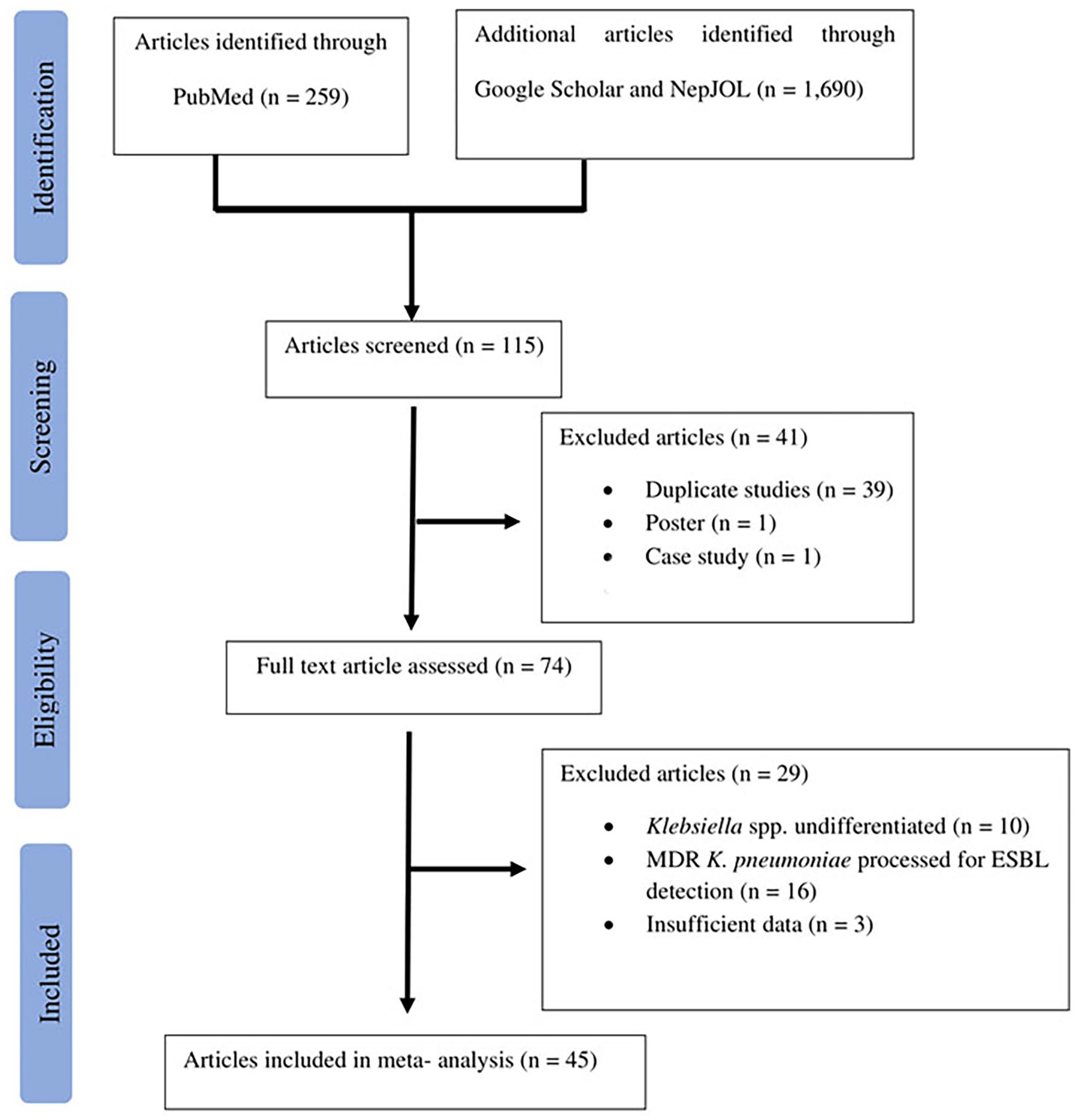
PRISMA flow diagram summarizing the process of literature search and selection.
Study selection procedures and eligibility criteria
Two reviewers (MS and CK) separately examined titles and abstracts of articles for possible inclusion in the review. Eligible studies were chosen in 3 steps: first, based upon the title; second, based on the abstract and third, based on the full-text articles. The selected articles were then reviewed and evaluated by other authors (PD and MRB). To be included in the meta-analysis, studies had to meet the following criteria: prevalence of ESBL-KP in Nepal published between 2011 and 2021, ESBL-KP isolated from human specimens and specify laboratory methods for ESBL detection. Studies were excluded for the following reasons: articles reporting ESBL-KP on non-human subjects, duplicate studies, undifferentiated Klebsiella spp., review articles, case reports, posters, retrospective studies, articles with incomplete information related to ESBL-KP detection method and not falling within the specified time. Studies reporting ESBL-KP only among MDR isolates, and studies from countries other than Nepal were also discarded.
Data extraction
Data were extracted independently by 2 reviewers (MS and CK) from all eligible studies and entered into MS Excel 2007. The extracted data included first author’s surname, year of publication, study area, study setting, sample size, total number of multidrug- resistant K. pneumoniae (MDR-KP), ESBL diagnostic method, the prevalence of ESBL-KP, antibiogram of ESBL-KP, sample-wise distribution of ESBL-KP and genes variant encoding ESBL. The data was retrieved and analyzed twice to eliminate any possible errors.
Outcome measurements
The main outcome of the study was evaluating the prevalence of ESBL-producers among K. pneumoniae isolates in Nepal. The distribution of ESBL-KP according to sample type and their antibiogram was also recorded. Furthermore, the prevalence of MDR-KP and its correlation with ESBL production were documented.
Quality assessment of studies
The quality of individual studies included in the meta-analysis was evaluated independently by 2 reviewers (MS and CK) using a checklist provided by the Newcastle–Ottawa Scale adapted for cross-sectional studies. 25 Any differences were checked and resolved through discussion with the third and the fourth authors (PD and MRB). The checklist consists of 10 questions that each reviewer answered separately for each study. Scores varied from 0 to 10, and studies with ⩾6 points were included in the systematic review and meta-analysis (Supplemental Table S1).
Statistical analysis
The statistical analysis was performed using the R programing language 4.2.0 (Meta package). Data were pooled using a random-effect model and the I 2 statistics (measure of inconsistency) was used to assess heterogeneity across studies with I 2 values of 25%, 50%, and 75% indicating low, moderate, and high heterogeneity, respectively. 26 In addition, contour-enhanced funnel plots and Egger’s test were utilized for detecting possible publication bias. 27
Results
Search results
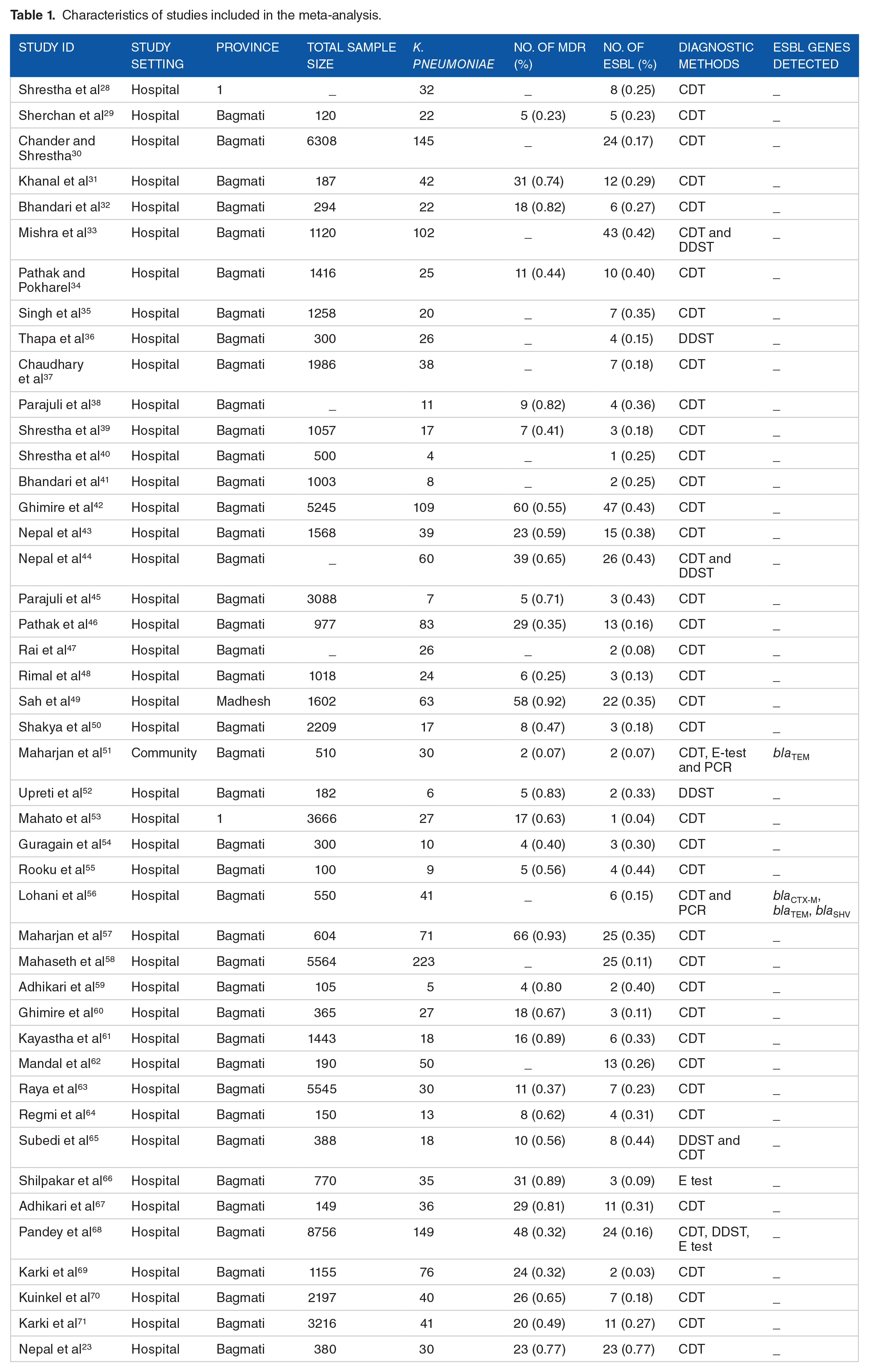
A total of 1949 potentially relevant articles were initially identified, of which 1834 articles were eliminated after screening the titles and abstracts. After excluding duplicate studies, posters, and case studies, 74 articles remained for further full-text assessment. Based on inclusion and exclusion criteria, 41 articles were further removed, and only 45 articles meeting the inclusion criteria were included in the final meta-analysis. In the total 45 included studies, a total of 1927 K. pneumoniae were isolated, of which 676 were MDR and 462 produced ESBL. Based on the study setting, the majority of the studies, 97.77% (44/45) were hospital-based, while only 2.22% (1/45) were community-based. The flowchart of article selection along with the reasons for exclusion are presented in Figure 1, and the main characteristics of the included studies are provided in Table 1.
Characteristics of studies included in the meta-analysis.
Laboratory methods used for ESBL detection
This meta-analysis revealed that the majority of the studies conducted in Nepal used only phenotypic tests for ESBL detection. Altogether, 3 different phenotypic tests were used for ESBL confirmation: combined disk test (CDT), double disk synergy test (DDST), and epsilometric test (E-test). Out of 45 studies included in this meta-analysis, 37 (82.22%) used CDT alone for ESBL-confirmation, 2 (4.44%) used DDST only and one (2.22%) study performed only E-test to estimate ESBL-proportions among K. pneumoniae. Similarly, 4 (8.88%) studies used both DDST and CDT, while 1 (2.22%) study performed CDT, DDST and E-test in combination for the confirmation of ESBL-phenotypes. Only 2 (4.44%) studies carried out molecular tests for the detection of ESBL-encoding genes (Table 1).
Province-wise distribution of articles on ESBL-KP in Nepal
The majority of the studies on ESBL-KP were reported from Bagmati Province (93.33%), while there were limited studies from Madhesh Province and Province No. 1 (2.22% in Madhesh Province and 4.44% in Province No. 1). No studies were identified on this subject from other provinces. The number of studies on ESBL-KP was few until 2014. The highest number of articles investigating this topic were published in the year 2017 (Figure 2).
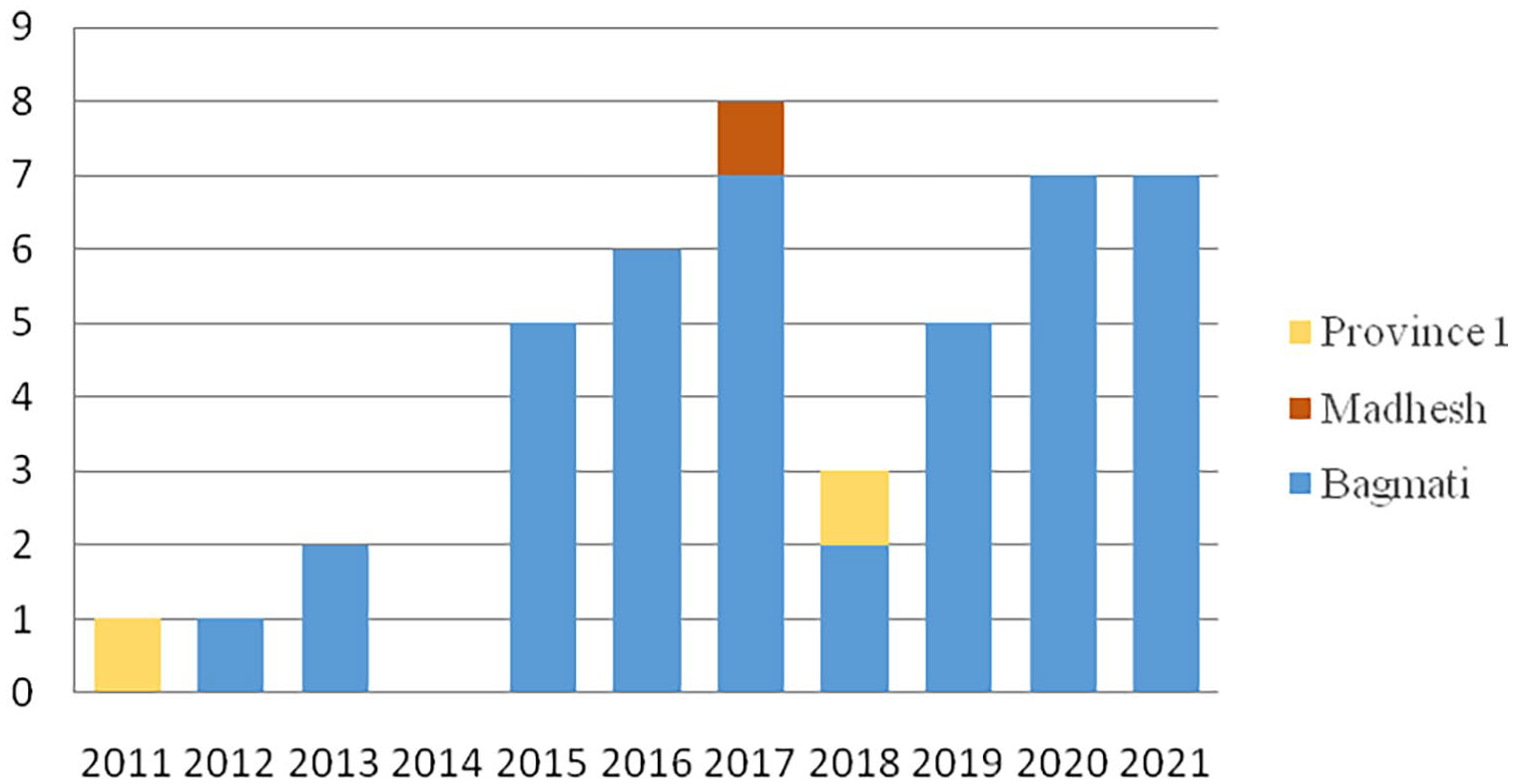
The annual publication of articles on ESBL-KP in different provinces of Nepal (2011-2021).
Meta-analysis on the prevalence of K. pneumoniae
Based on the analysis of the eligible studies, the pooled prevalence of K. pneumoniae was found 5% (95% confidence interval (CI), 0.03-0.07) among processed samples with significant heterogeneity (I 2 = 96%; P < .01) (Figure 3).
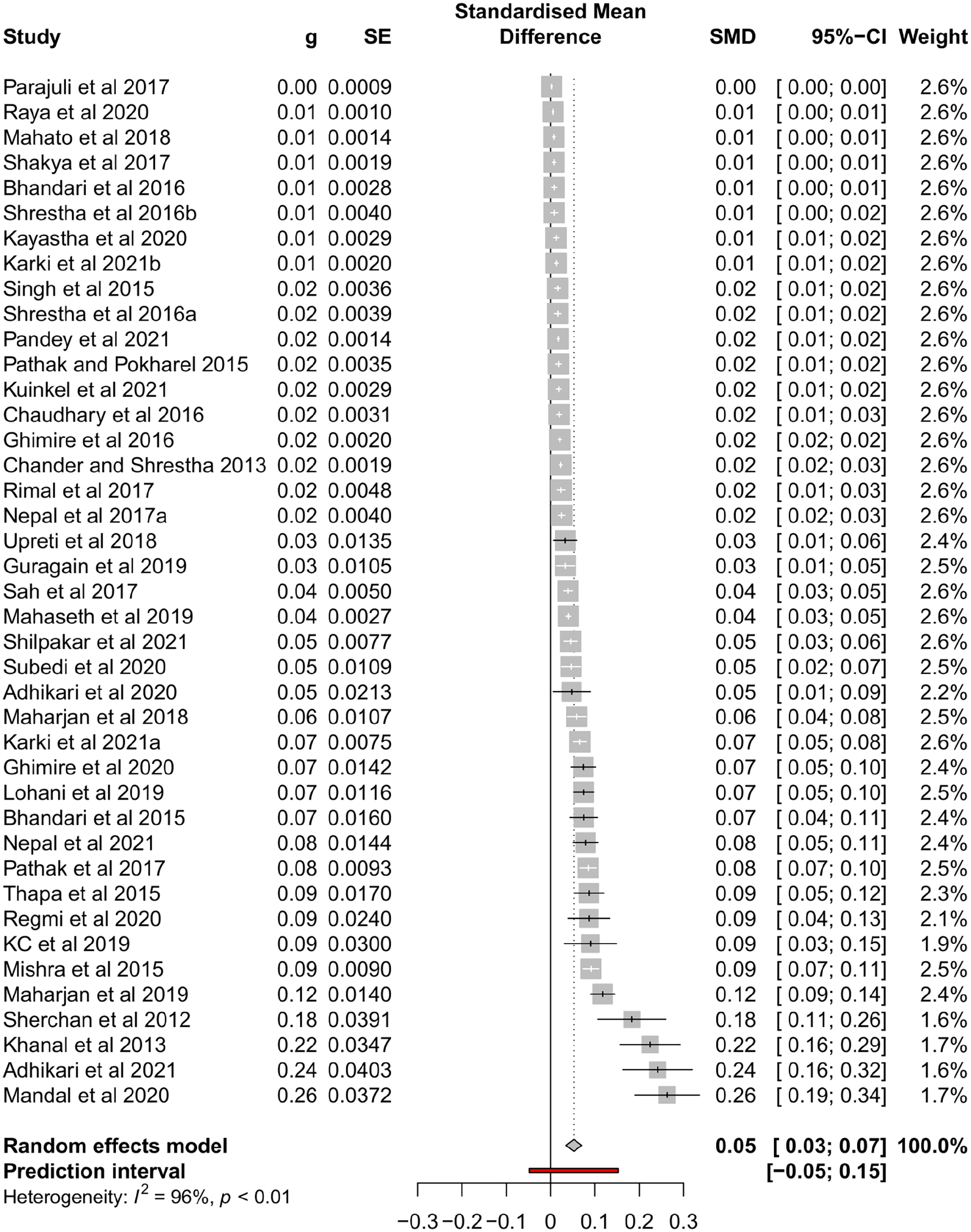
Forest plot depicting the pooled prevalence of K. pneumoniae in Nepal.
Meta-analysis on the prevalence of MDR among K. pneumoniae isolates
The overall pooled prevalence of MDR isolates among K. pneumoniae was 55% (95% CI, 0.47-0.64), with a high level of heterogeneity (I 2 = 81%, P < .01) among the studies (Figure 4).
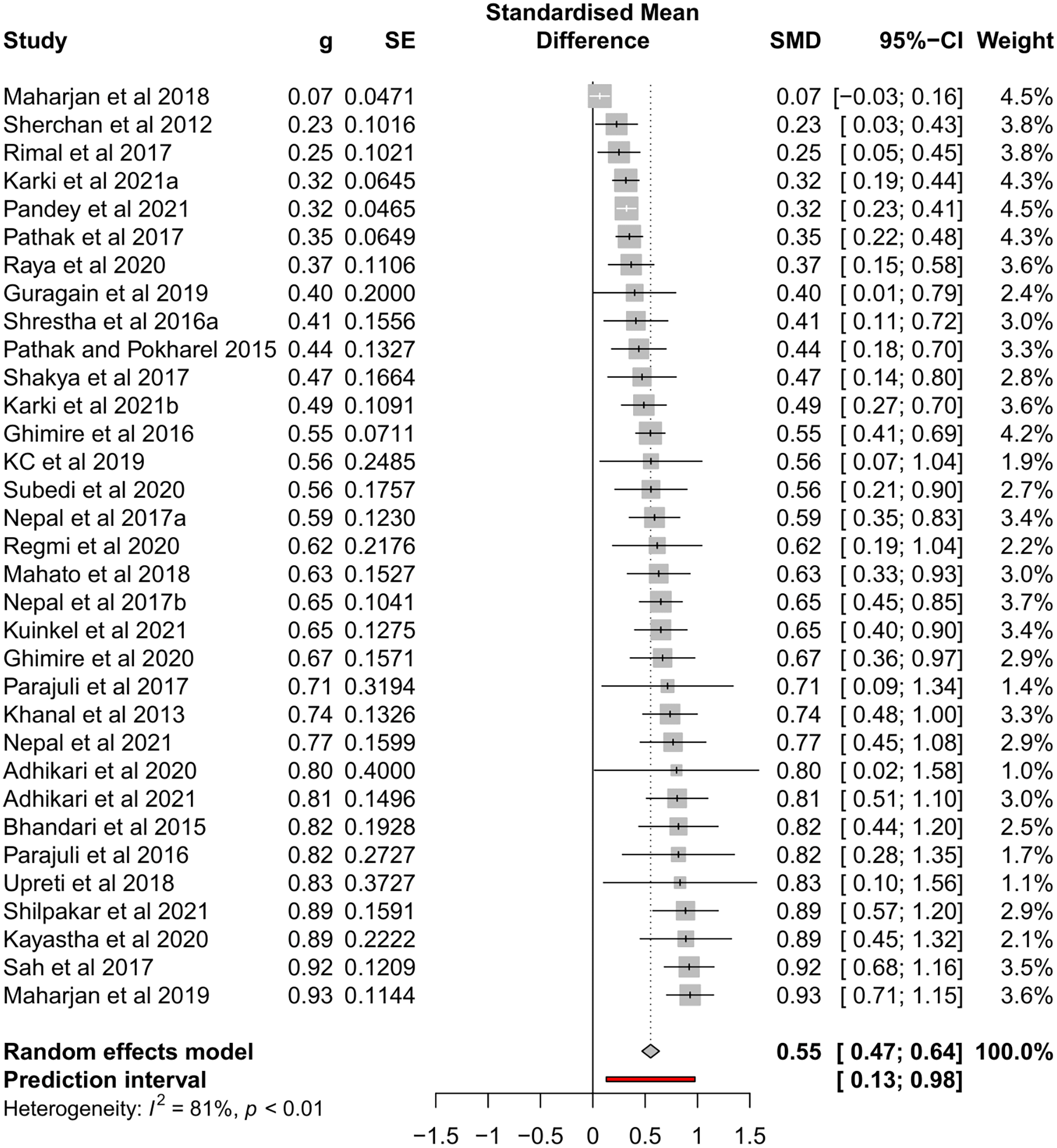
Forest plot of pooled prevalence of multidrug resistance among K. pneumoniae in Nepal.
Meta-analysis on the prevalence of ESBL-KP in Nepal
The pooled prevalence of ESBL-KP was 23% (95% CI, 0.19-0.27), with a high heterogeneity (I 2 = 76%, P < .01) among the studies analysed (Figure 5).
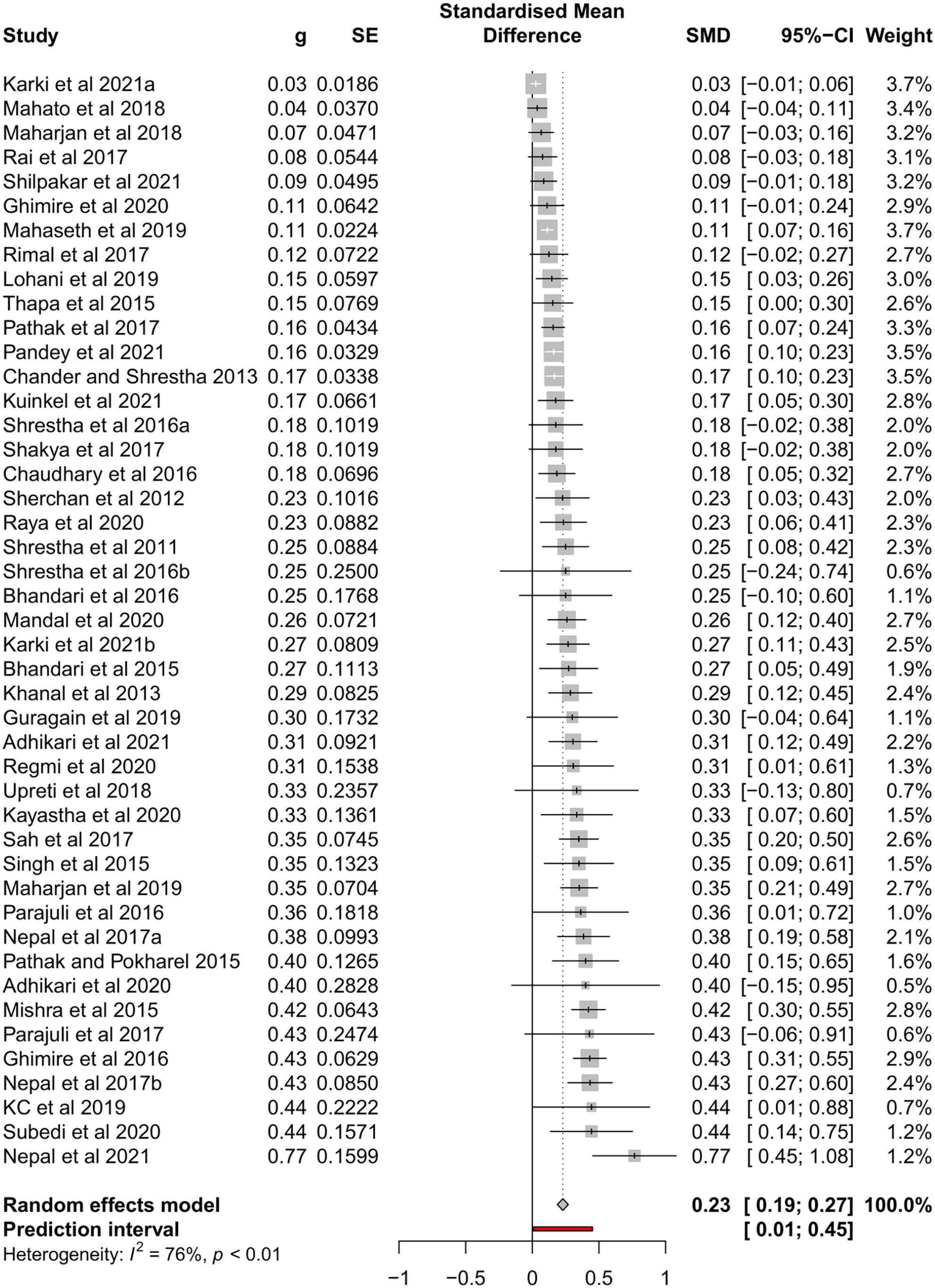
Forest plot showing the prevalence of ESBL-KP isolates among the Nepalese population.
Distribution of ESBL-KP according to the type of samples
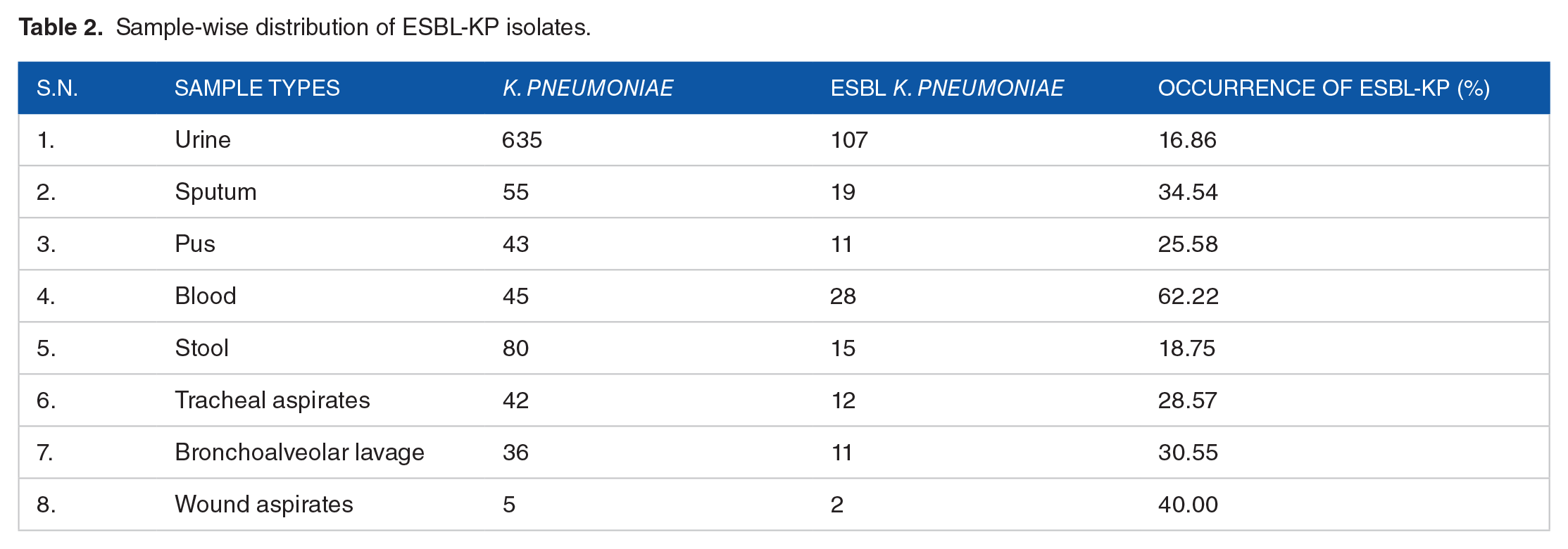
Sample-wise distribution study revealed blood as the most common sample from which ESBL-phenotypes were recovered. Blood samples accounted for 62.22% of the ESBL-KP isolates, followed by wound aspirates (40%), sputum (34.54%), bronchoalveolar lavage (30.55%), and tracheal aspirates (28.57%). One-fourth of the ESBL-positive isolates were obtained from pus samples. The rate of the isolation from urine and stool specimens were 16.86% and 18.75%, respectively (Table 2).
Sample-wise distribution of ESBL-KP isolates.
Correlation between MDR and ESBL production among K. pneumoniae isolates
A strong positive correlation (Pearson’s correlation coefficient of 0.82; 95% CI: .67-.91) was observed between ESBL production and multidrug resistance in K. pneumoniae strains (Figure 6 and Supplemental Table S5).
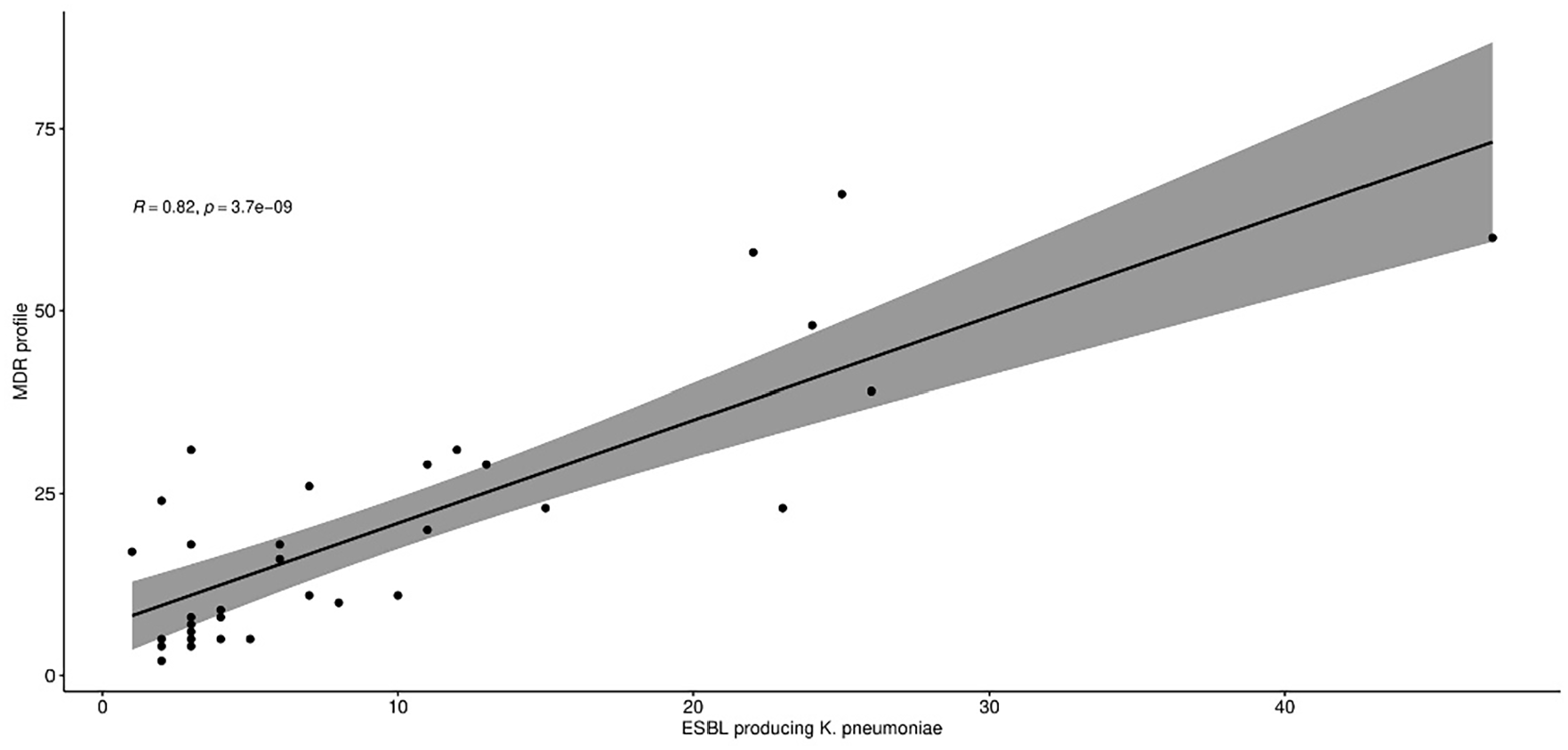
Relationship between multidrug resistance and ESBL production in K. pneumoniae isolates.
Antimicrobial resistance patterns in ESBL-KP
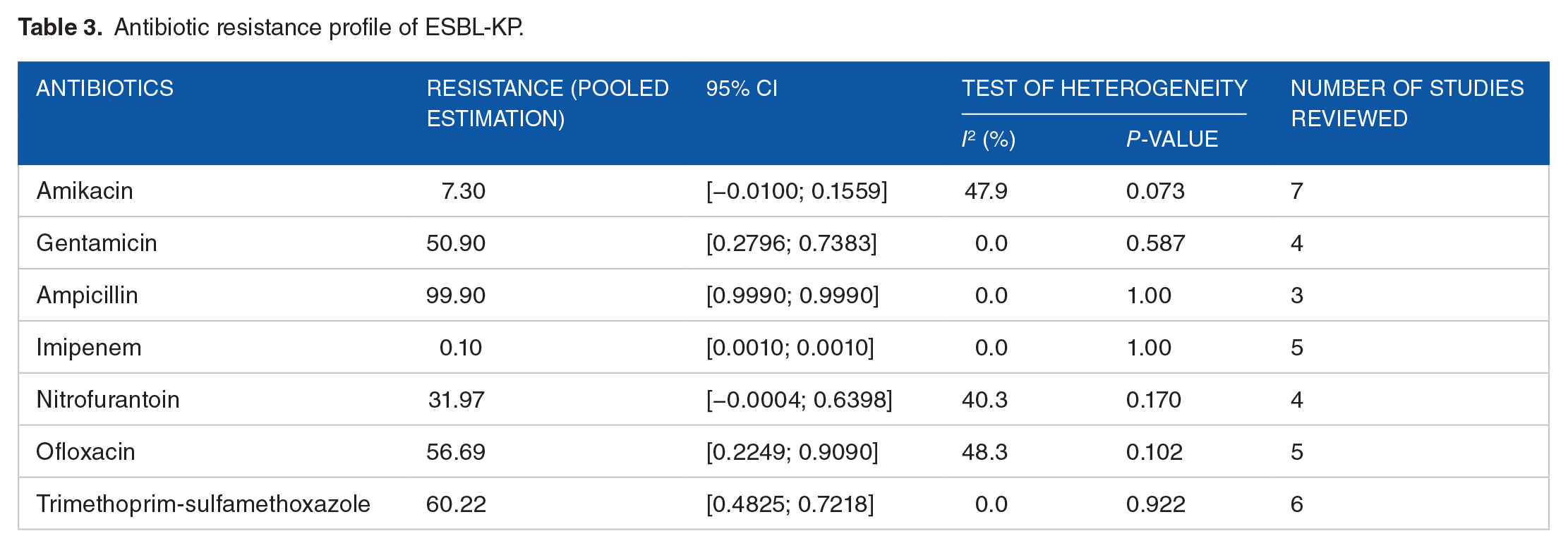
The antibiotic resistance pattern (in vitro) of ESBL-KP is shown in Table 3. Imipenem was found to be the most effective antibiotic (99.9% sensitive) against ESBL-producing strains of K. pneumoniae, followed by amikacin (92.7% sensitive) and nitrofurantoin (68.03% sensitive). The resistance toward ampicillin was very high (99.9%). Higher resistance was also observed against trimethoprim-sulfamethoxazole (60.22%), ofloxacin (56.69%), and gentamicin (50.9%).
Antibiotic resistance profile of ESBL-KP.
Publication Bias
Quality assessment of all the included studies performed using Newcastle-Ottawa Scale showed the total score ⩾6 indicating satisfactory and fair selection of articles. The funnel plots for accessing the bias for studies reporting K. pneumoniae, ESBL production and MDR profile in K. pneumoniae showed the majority of the studies are statistically significant for the inclusion. However, on performing Egger’s tests for these parameters, all plots were found asymmetrical (P < .001) indicating publication bias (Supplemental Table S2, S3 and S4). Based on the contour-enhanced funnel plots and quality assessments, the analyses were considered suitable for the publication (Supplemental Figure S1, S2 and S3).
Discussion
Drug-resistant strains of K. pneumoniae are becoming a serious concern worldwide. This meta-analysis shows the overall pooled prevalence of K. pneumoniae in various processed specimens as 5% in Nepal. However, Odari and Dawadi 72 reported the prevalence of K. pneumoniae in clinical specimens in the context of Nepal as 3%. The variation could be the result of difference in time of the study. Odari and Dawadi carried out the analyses of studies on K. pneumoniae from 2015 to 2021 72 while our studies included data between 2011 and 2021.
Management of antibiotic resistance in Gram-negative bacteria, mainly MDR-KP, currently represents a significant challenge in the field of infectious diseases. 73 In our study, the pooled prevalence of MDR isolates in K. pneumoniae was estimated to be 55%, which is in agreement with those of the studies conducted in Bangladesh (55%), 74 Indonesia (54.49%), 75 and Iran (58%). 76 On the contrary, our pooled prevalence is lower than those of the studies from Pakistan (63%), 77 Brazil (84%) 78 and India (75%) 79 but much higher than study from Ethiopia (20%). 80
Our study showed that the prevalence of MDR-KP was higher in Bagmati Province. The majority of megacities is located in the province and contains dense populations. The high resistance may be linked with antibiotic prescription patterns, environmental exposures, hygiene practices, study periods, poor health, and medical facilities.21,72,80
A strong positive correlation was observed between ESBL production and multidrug resistance. This might be due to the fact that ESBL genes in combination with other resistance genes confer such resistance.8,81
K. pneumoniae is a leading cause of opportunistic healthcare-associated infections, which are increasingly complicated by the production of ESBL-enzymes by these bacteria.12,82 In the present study, the pooled prevalence of ESBL-KP was 23%. Our result is in accordance with studies conducted in Bangladesh (25.335%) 83 and Sri Lanka (25%), 84 but higher in comparison to the study reported from Pakistan (15.25%). 85 There are many factors that contribute to a high frequency of ESBL-strains, including acquisition of novel resistance-genes, transfer of resistance contributing genes, lack of effective antibiotic surveillance systems, inadequate infection control strategies, easy availability and misuse of antibiotics, inappropriate dosing schedule, lack of new antibiotics and limited diagnostic facilities. 80 These factors could have contributed to the higher occurrence of ESBL-KP in Nepal.
The study on antibiogram of ESBL-KP revealed a very high level of resistance to ampicillin (99.90%) which is consistent with studies conducted in Bangladesh, 74 Saudi Arabia 86 and Indonesia. 87 The increase in resistance toward these antibiotics may be due to the inappropriate use of antibiotics without medical supervision and with improper administration, as well as insufficient therapy. 88 The majority of ESBL-KP were found sensitive to imipenem (99.90%) and amikacin (92.7%). These are in parallel with the findings of studies conducted in Pakistan (imipenem 100%, amikacin 95.2%), 89 Indonesia (imipenem 91.5%, amikacin 90.4%) 87 and France (imipenem 99.3%, amikacin 93.2%). 90 The higher susceptibility of ESBL-KP toward imipenem may be due to the finite use of this antibiotic in Nepal. Besides ESBL production, factors such as biofilm formation and production of other antibiotic hydrolysing enzymes were found to be responsible for emergence in the resistance in Enterobacteriaceae.91,92
In this study, ESBL-KP strains were predominantly recovered from blood (62.22%). Sarojamma and Ramakrishna also reported blood as a major source of ESBL-producers. 93 This could be due to the factors like inappropriate use of syringes, poor hand washing practices among healthcare professionals and improper disinfection of skin of prolonged hospital-stayed patients during transfusion.94,95 However, reports from other investigations show higher prevalence from other human samples.90,96
Strengths and limitations of our study
This is the first study to calculate the pooled prevalence of ESBL-KP in Nepal. Studies available from all geographical regions of the country, and studies on both hospital and community-based settings were included in the meta-analysis. Our exploration also revealed the pooled estimate of MDR-KP and their correlation with ESBL production, distribution of ESBL-KP in different specimens, and the resistance profile of ESBL-KP to commonly administered antibiotics. The findings from our study could be of use to clinicians and health policymakers. However, this review has some limitations. First, the study on potential risk factors associated with ESBL-infections such as socioeconomic status, prior antibiotic use, and past medical history of patients was not possible to accumulate due to limited prior research on these factors. Second, the prevalence of ESBL-KP in non-human subjects was not studied due to low number of articles addressing the topic. Third, most studies on ESBL-KP were from hospital-setting, and the precise ratio of nosocomial versus community-acquired bacteria was not determined. Fourth, it was also impossible to determine the mortality rate associated with infections caused by ESBL-KP as no studies were found reporting the consequence. Additionally, investigation on ESBL-genotypes is limited in Nepal. Thus, the pooled prevalence of infections is primarily based on studies on ESBL-phenotype.
The increase in the occurrence of MDR and ESBL-producing strains necessitates an improvement in laboratory facilities as well as laboratory experts’ diagnostic skills for assessing antibiotic resistance profiles. The scarcity of studies from provinces other than Bagmati indicates the need for research on this topic from all parts of the country. Our study revealed that the majority of studies on ESBL-KP were from hospital-settings, while studies from community-settings on ESBL-strains were rare. Thus, community-based studies on ESBL strains are recommended. Further research is also required to evaluate the risk factors that might affect the development and implementation of a rational and effective ESBL-KP control strategy. Routine screening of ESBL-strains, molecular approaches for the detection of ESBL-genotypes and proper antibiotic prescription policies are urgently required to combat the burden of ESBL-KP.
Conclusion
Overall, high ESBL production was seen in K. pneumoniae which could contribute to multidrug resistance. A decreased susceptibility of ESBL-KP toward the majority of commonly used antibiotics was seen, thereby highlighting the need for rationale use of appropriate antibiotics. The better options for the treatment of ESBL-KP could be imipenem and amikacin.
Supplemental Material
sj-docx-1-mbi-10.1177_11786361221145179 – Supplemental material for Systematic Review and Meta-analysis on Extended-Spectrum β-lactamases Producing Klebsiella pneumoniae in Nepal
Supplemental material, sj-docx-1-mbi-10.1177_11786361221145179 for Systematic Review and Meta-analysis on Extended-Spectrum β-lactamases Producing Klebsiella pneumoniae in Nepal by Manita Shyaula, Christina Khadka, Prabin Dawadi and Megha Raj Banjara in Microbiology Insights
Footnotes
Acknowledgements
The authors like to express their gratitude to all researchers of the studies included in this meta-analysis.
Funding:
The author(s) received no financial support for the research, authorship and publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Author’s Contributions
MS conceived the idea, and MS and CK designed the study. MS and CK reviewed the literature and extracted the data. PD and MRB rechecked the data. PD analysed the data. MS, CK and PD drafted the manuscript. MRB revised and reviewed the manuscript. MRB supervised the overall data analysis and writing. All authors read and approved the final manuscript.
Data Availability
All supplementary files, data generated and analysed will be made available by the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
