Abstract
Prodrug strategies use chemical modifications to improve the pharmacokinetic properties and therefore therapeutic effects of parent drugs. Traditional prodrug approaches use endogenous enzymes for activation. Bioorthogonal catalysis uses processes that endogenous enzymes cannot access, providing a complementary strategy for prodrug uncaging. Site-selective activation of prodrugs to drugs (uncaging) using synthetic catalysts is a promising strategy for localized drug activation. We discuss here recent studies that incorporate metal catalysts into polymers and nanoparticle scaffolds to provide biocompatible “enzyme-like” catalysts that can penetrate bacterial biofilms and activate prodrug antibiotics in situ, affording a new strategy to treat bacterial biofilm infections with the potential for reduced off-target effects.
Traditional prodrugs are inactive compounds that are enzymatically converted into active drugs inside the body, providing a means for regulating their pharmacological properties. Prodrug strategies have been applied to reduce toxicity and/or increase delivery of parent antibiotics. 1 As an example of the former, colistin, an antibiotic used to treat some cases of multidrug-resistant Gram-negative bacillary infections (eg, Enterobacterales, Pseudomonas aeruginosa), 2 is administered parenterally as colistin methanesulfonate, since it is less toxic than colistin. Caging of the amine functionality provides less toxic colistin methanesulfonate. As an example of the latter, the prodrug approach has been applied to improve the oral bioavailability of penicillin antibiotics (eg, pivampicillin). Ceftaroline fosamil is another example of a prodrug antibiotic, being a cephalosporin prodrug that upon activation yields the active metabolite ceftaroline, and metronidazole is a prodrug used to treat anaerobic bacterial, Helicobacter pylori and some protozoal infections.
Localized conversion of prodrugs provides a promising strategy to deliver antibacterial effects, while minimizing off-target effects of antibiotics, provided the prodrug itself has limited toxicity to the human. 3 For example, ester prodrugs have been used to target bacteria through activation by bacterial esterases. 4 When such prodrugs circulate to the site of infection, they are inactive until they are activated inside targeted bacteria, leading to high local concentrations of active drugs that selectively eliminate targeted bacteria while lowering off-target toxicity (eg, nephrotoxicity, hepatotoxicity), provided the prodrug has minimal adverse effects.
Biofilm-associated infections are particularly challenging to treat, often requiring high doses of antibiotics over extended periods of time, with the potential for significant off-target effects. And even with the availability of conventional antibiotics, many biofilm-associated infections remain untreatable with these drugs alone, requiring physical removal. Prodrug strategies may provide a potential strategy for reducing these concerns. 5 However, designing prodrugs that are not activated off-target by endogenous enzymes in the host has been challenging (Figure 1 Biogenic prodrug treatment). 6
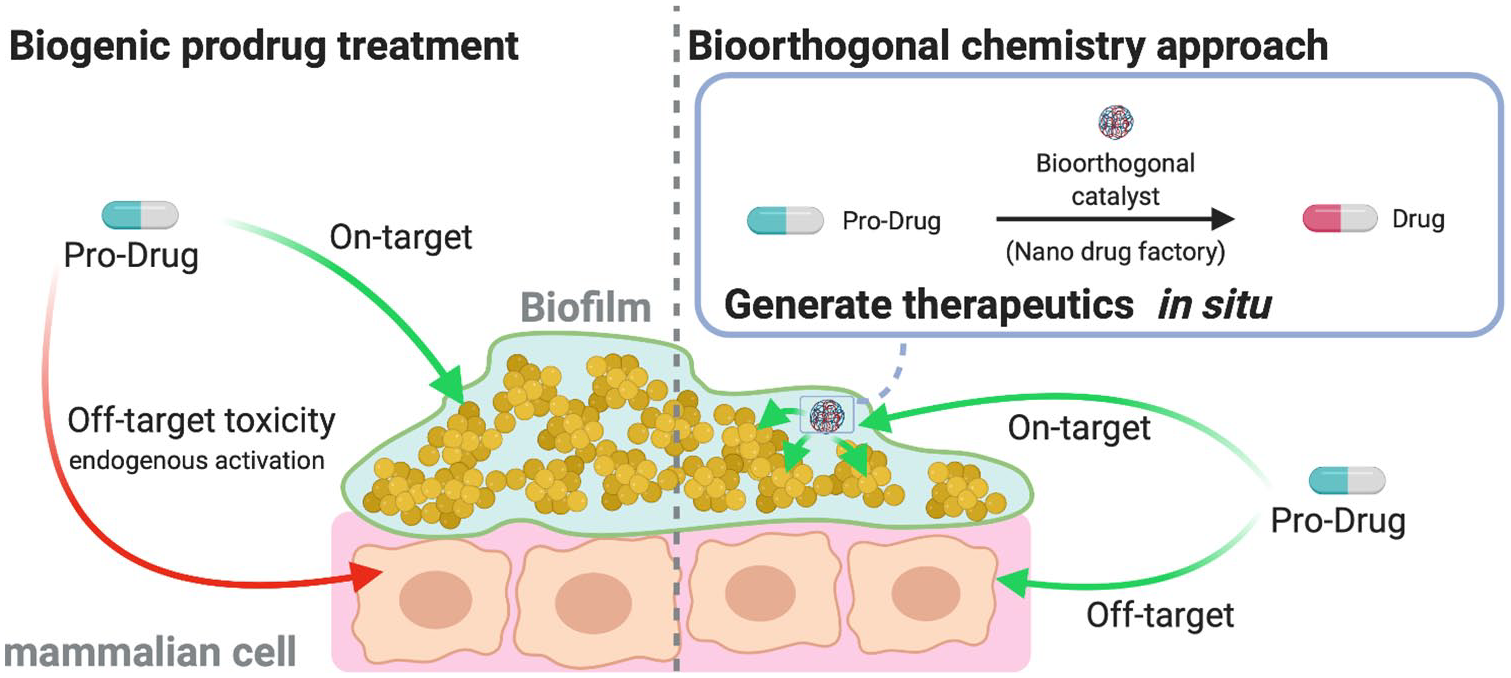
Biogenic prodrug treatment: Prodrugs are activated by endogenous bacterial enzymes. They may however be activated outside of the infection area, leading to off-target toxicity. Bioorthogonal chemistry approach: Prodrugs are activated by biocompatible exogeneous enzyme-like molecules. Once these catalysts penetrate biofilms, they act as “drug nanofactories,” converting prodrugs to antibiotics in situ. Meanwhile, prodrugs outside of biofilms are not activated, minimizing host toxicity from off-target activation of the non-toxic prodrugs.
Bioorthogonal chemistry uses processes that living systems cannot access, providing new strategies for prodrug activation. 7 Bioorthogonal catalysis uses prodrugs that can only be activated by synthetic catalysts, minimizing off-target activation by host enzymes (Figure 1 Bioorthogonal chemistry approach). 8 These synthetic catalysts can be localized at the disease site through topical administration or active targeting, serving as “artificial enzymes” for prodrug activation. Transition metal-based catalysts (TMCs) are promising tools for bioorthogonal approaches, catalyzing a wide range of reactions that cannot be driven by endogenous enzymes. 9 TMCs, however, generally have low aqueous solubility and stability in physiological conditions.
Natural enzymes use their peptide scaffold to stabilize and solubilize catalytic sites. 10 Artificial metalloenzyme-like materials (“polyzymes”) that use polymers in an analogous fashion to solubilize and protect TMCs have been recently developed. 11 In this system, a non-toxic polymer that assembled into ~50 nm diameter nanoparticles with a hydrophobic core and a positively-charged exterior (for penetration into biofilms 12 ) is used to encapsulate a hydrophobic non-toxic iron porphyrin catalyst. 13 In situ generation of antibiotics using this polyzyme was demonstrated using a bacterial biofilm model. Biofilms were first treated with polyzyme solution. Subsequently, either a ciprofloxacin or moxifloxacin prodrug modified with an azidobenzyl carbamate was administered. Upon diffusing into the biofilm, the prodrugs were converted to the antibiotic by the TMCs incorporated in the polyzyme, killing the embedded bacteria (Figure 2a Polyzyme). This approach in contingent on prodrugs being nontoxic to mammalian cells and not activated by cells. This polyzyme strategy uses biocompatible components to generate therapeutics on site, providing a safe, controllable, and sustainable way to manage biofilm infections.
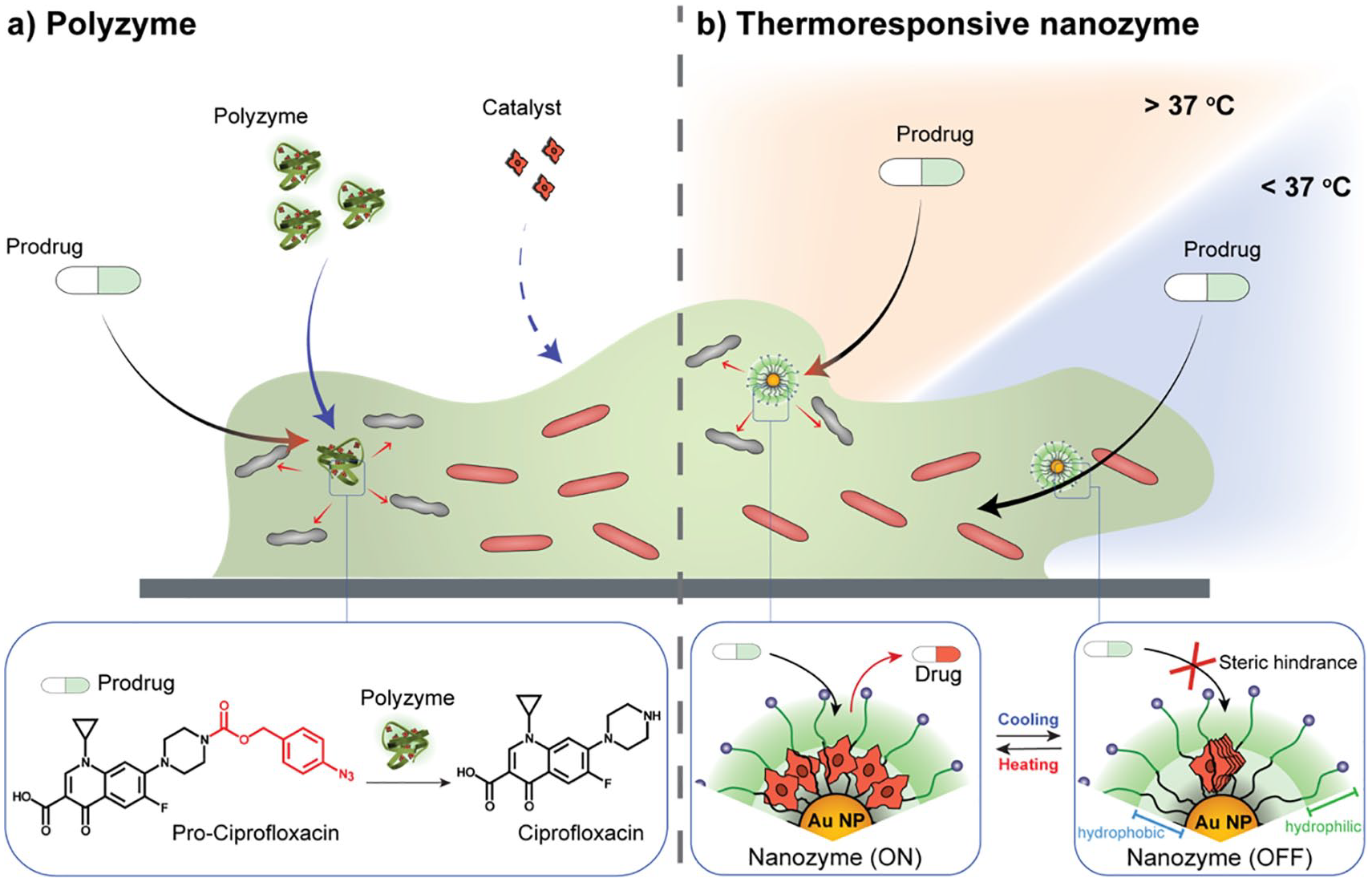
(a) Polyzymes penetrate biofilms and activate prodrugs in situ, while free catalysts are unable to penetrate biofilms. (b) Catalysts are stored in the hydrophobic pocket of the nanoparticle to form a thermo-responsive nanozyme. At temperatures <37°C, catalysts are aggregated, hence, prodrug cannot access catalyst. The stacked catalysts disassemble at 37°C and regain catalytic activity.
The polyzyme study demonstrated that TMCs can be used as bioorthogonal “nanofactories” to generate antibiotics in situ. In related research, 2 nm gold core nanoparticle-based bioorthogonal catalysts (nanozymes) were developed that can turn catalysis on and off using temperature control. 14 Similar to polyzymes, these nanozymes use hydrophobic interactions to encapsulate iron porphyrin, and positively-charged surfaces to penetrate biofilms (Figure 2b Thermoresponsive nanozyme). Encapsulated porphyrin catalysts are confined to the limited space provided by the hydrophobic region of small molecules, leading to aggregation of the porphyrin catalyst in the range of 25 to 37°C, with the deaggregation temperature controlled by catalyst loading. With these nanozymes, aggregation of porphyrins prevents prodrugs from approaching catalytic sites, “turning off” nanozyme activity. When the temperature is increased, however, aggregated porphyrins dissociate and are “turned on,” allowing prodrugs access to the catalytic sites and to be converted to the corresponding antibiotic in situ. This approach reduced Escherichia coli biofilm viability to ~10% at 37°C, whereas biofilms showed negligible differences in viability at 25°C. Notably, this temperature-controlled behavior is reversible, providing access to more precise temporal control for antimicrobial therapy.
Taken together, bioorthogonal activation of prodrugs using polyzymes and/or nanozymes provides a versatile tool for combatting chronic bacterial infections. The ability of these systems to generate antibiotics at infection sites has the potential to increase efficiency of bacterial killing while reducing off-target effects. Realizing these goals, however, will require efficient localization of polyzymes/nanozymes to infection sites, either through topical administration or via targeting strategies. 15 Finally, the promise shown by bioorthogonal antimicrobial strategies in vitro will need to be validated in vivo prior to clinical translation. 16
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by NIH grants EB022641 and AI134770.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
