Abstract
Background:
Healthcare-associated infection (HAI) is an important public health problem, particularly in intensive care units (ICUs). We aimed to examine the epidemiology and risk factors of HAIs in our ICUs and study their microbiological profile.
Methods:
We evaluated 100 consecutive patients in 3 medical and surgical ICUs of a tertiary care teaching hospital daily starting in January 2016 using the Centers for Disease Control and Prevention definitions and methods. We determined the incidence and sites of HAIs, identified the causative microorganism, and studied their antibiotic sensitivity profiles. We investigated risk factors for the development of an HAI using a multiple logistic regression model.
Results:
Of 300 patients, 129 patients (43%) developed HAIs (55.96 HAI events per 1000 ICU-days). Pneumonia was the most common type of HAI (57, 41%).
Conclusions:
We found a high incidence of HAIs in our ICUs and a high burden of multidrug-resistant microorganisms highlighting the importance of infection control and antibiotic stewardship.
Introduction
Healthcare-associated infection (HAI) remains an important global public health problem impacting patient morbidity and mortality as well as driving healthcare costs. Patients in intensive care units (ICUs), particularly in low and middle-income countries, are among the most at risk for HAIs. Studies estimate that 9.1% to 19.2% of ICU patients in high-income countries, and approximately 30% of the ICU patients in low and middle-income countries are affected by at least 1 episode of HAI.1-3 A significant proportion of these infections are device-associated infections (DAIs). 4 Furthermore, infections acquired in ICUs are frequently associated with drug-resistant organisms which further increase patient mortality, length of hospitalization, and costs.5,6
Evidence suggests that 35% to 55% of HAIs could be prevented regardless of the economic status of the country.
7
However, in Nepal, infection control and prevention efforts are often inadequate and surveillance data on HAIs as well as antimicrobial resistance are limited.8,9 Furthermore, only a few studies have described HAIs in Nepal using standardized definitions thus making comparison with the international and regional burden of the disease difficult. Available studies reveal a significant HAI burden in Nepal. In one such study, investigators conducted prospective surveillance of DAIs in a combined medical-surgical ICU of a teaching hospital in Nepal for 15 months and found 21.40 Ventilator-Associated Pneumonia (VAP), 8.64 Central Line-Associated Bloodstream Infections (CLABSI), and 5.11 Catheter-Associated Urinary Tract Infections (CAUTI) per 1000 device-days, respectively.
10
These rates are higher than those at the medical/surgical ICUs of 45 low and middle-income countries reported through the International Nosocomial Infection Control Consortium (INICC) (14.1 VAPs, 5.05 CLABSIs, and 5.1 CAUTIs per 1000 device-days).
11
These rates are also higher than those of the medical/surgical ICUs in the United States reported through the National Healthcare Safety Network (NHSN) (1.6 VAPs, 1.1 CLABSIs, and 2.7 CAUTIs, per 1000 device-days)12,13 as well as those of the medical/surgical ICUs of 20 different cities in India (10.4 VAPs, 4.82 CLABSIs, and 2.07 CAUTIs per 1000 device-days).
14
Furthermore, in the same study from Nepal,
The objectives of this study were to examine the epidemiology and the risk factors of HAIs in the ICUs and study their microbiological profile with the goal of helping to identify and prioritize problem areas for future action.
Materials and Methods
Study design and settings
We conducted a prospective cohort study in 2 medical and 1 surgical ICU of Tribhuvan University Teaching Hospital, a 700-bed tertiary acute care hospital in Kathmandu, Nepal. The surgical ICU and one of the medical ICUs have 5 beds each and the other medical ICU has 9 beds for a total collective capacity of 19 beds.
Participants
All patients admitted to the ICUs who were at least 18 years of age and admitted to the ICU for at least 2 calendar days were considered for inclusion starting in January 2016 until a consecutive cohort of 100 patients was reached from each of the 3 ICUs.
Variables and data collection
We reviewed the medical records of the enrolled patients daily while they were admitted to the ICUs and for 2 calendar days after being transferred out of the ICUs. We diagnosed HAIs based on criteria adapted from the 2008 US Centers for Disease Control and Prevention (CDC) definitions. 15 To diagnose Ventilator-Associated Events (VAEs), we used the criteria adapted from the 2015 CDC definitions. 16 HAI diagnoses were made using available clinical, radiographic, and microbiological data collected from the medical records and independent of diagnosis by the teams providing care to the patient. We categorized each patient as a trauma or non-trauma patient based on if the patient was admitted to the ICU after a traumatic event or due to its direct complication. A patient was considered immune-compromised if the patient had neutropenia (absolute neutrophil count <1500 cells/μL), was receiving steroid therapy (receiving more than an equivalent dose of 10 mg/day of systemic prednisone for ⩾ 4 weeks), on cytotoxic therapy, a previous or current diagnosis of Human Immunodeficiency Virus (HIV) infection, asplenia, and leukemia of any type. We considered patients with a history of any surgery within the preceding 30 days of hospital admission as surgical admissions. Invasive devices were defined as a Foley urinary catheter, central venous line (except hemodialysis lines), and endotracheal intubation. We focused on 5 HAIs—pneumonia (including VAEs), Urinary Tract infection (UTI), Surgical Site Infection (SSI), bloodstream infection, and gastroenteritis, and described their microbiological profile. We determined the antibiotic susceptibility of the bacteria isolated using the Kirby–Bauer disc diffusion method according to the Performance Standards for Antimicrobial Susceptibility Testing by the Clinical and Laboratory Standards Institute. 17 We defined multi-drug resistant bacteria according to the 2012 joint initiative by the European Centre for Disease Prevention and Control and the US Centers for Disease Control and Prevention. 18
Statistical analysis
We entered the data in Microsoft Excel (Office 365, Microsoft Corporation, Washington, United States) and analyzed in R.
19
We summarized demographic and clinical characteristics with a mean (± Standard Deviation [SD]) or median (Inter-Quartile Range [IQR]) and proportions. We calculated the incidence of HAIs as the number of HAI events per 1000 ICU-days. We calculated the Device Utilization Ratio (DUR) by dividing the total number of device days by the total number of hospital days and DAI rate as the ratio of number of DAIs for an infection site and the number of device-days multiplied by 1000. We performed a bivariate analysis to test for association of age, sex, ICU admission duration, smoking, presence of comorbidities, immunocompromised status, use of invasive devices, use of Proton Pump Inhibitors (PPI), and sedation with the development of HAIs using logistic regression analysis. We fitted a multiple logistic regression model with HAI as the binary outcome variable and the variables with
Ethics approval and consent to participate
Ethical approval was obtained from the Institutional Review Board, Institute of Medicine, Tribhuvan University (Reference number 315 [6-11-E] 72/73). Written informed consent to participate in the study was obtained from the patients or their surrogate decision-makers if they were unable to provide consent.
Results
Consent for participation in the study was obtained for all 300 patients approached. The median age was 52 (IQR 31-65) years. There were 157 (52.3%) male patients. The median duration of ICU stay was 6 (IQR 4-11) days for a total of 2502 ICU-days. Almost half of the patients (148, 49.3%) were smokers. Of all ICU admissions, 74 (24.7%) were surgical. One hundred ninety-three (64.3%) patients had at least 1 comorbid condition and 25 (8.3%) patients were immune compromised. Most patients (257, 85.7%) were on PPIs. There were 88 (29.3%) patients who had received sedation and 187 (62.3%) patients who had at least 1 invasive device placed during their ICU admission.
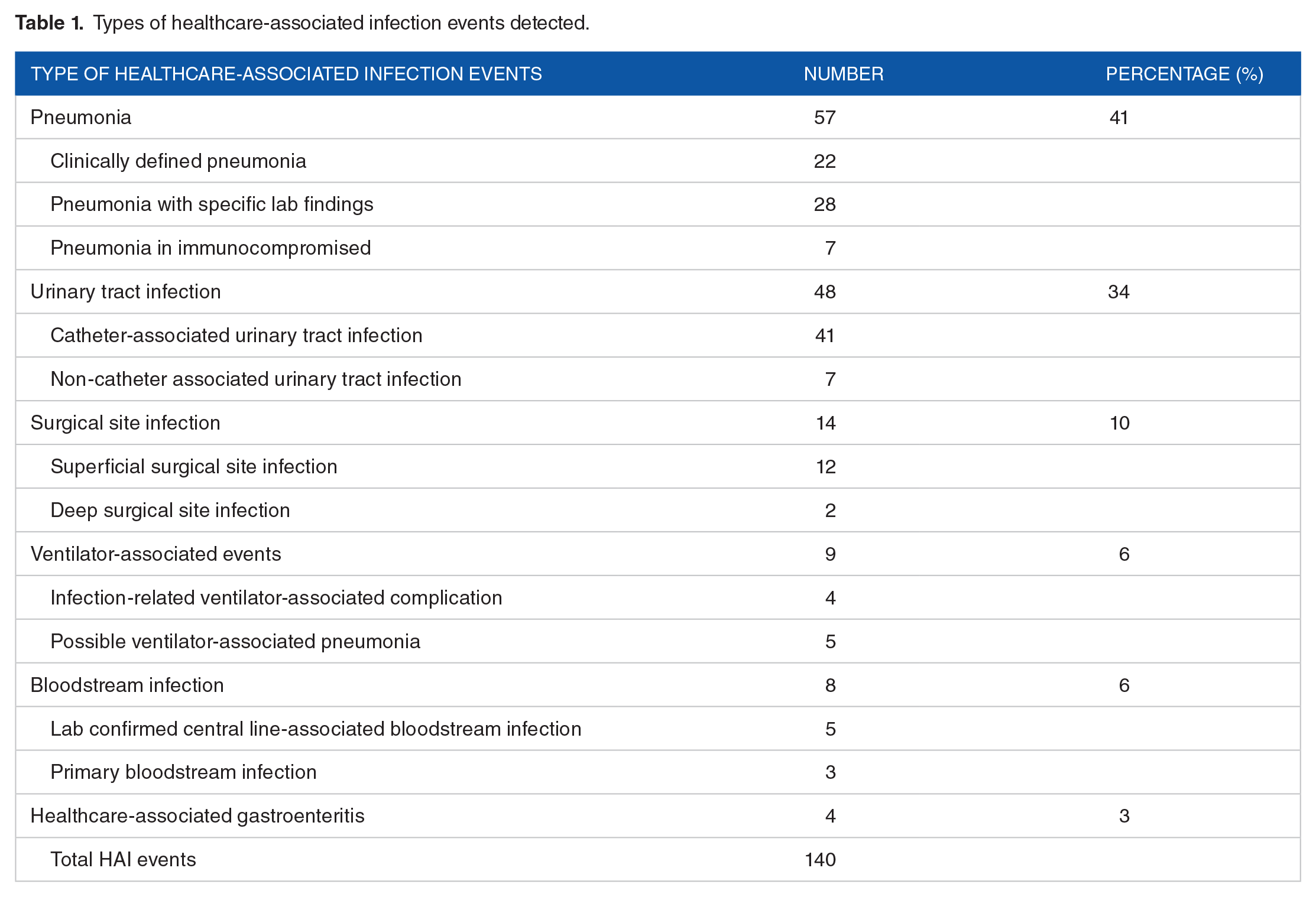
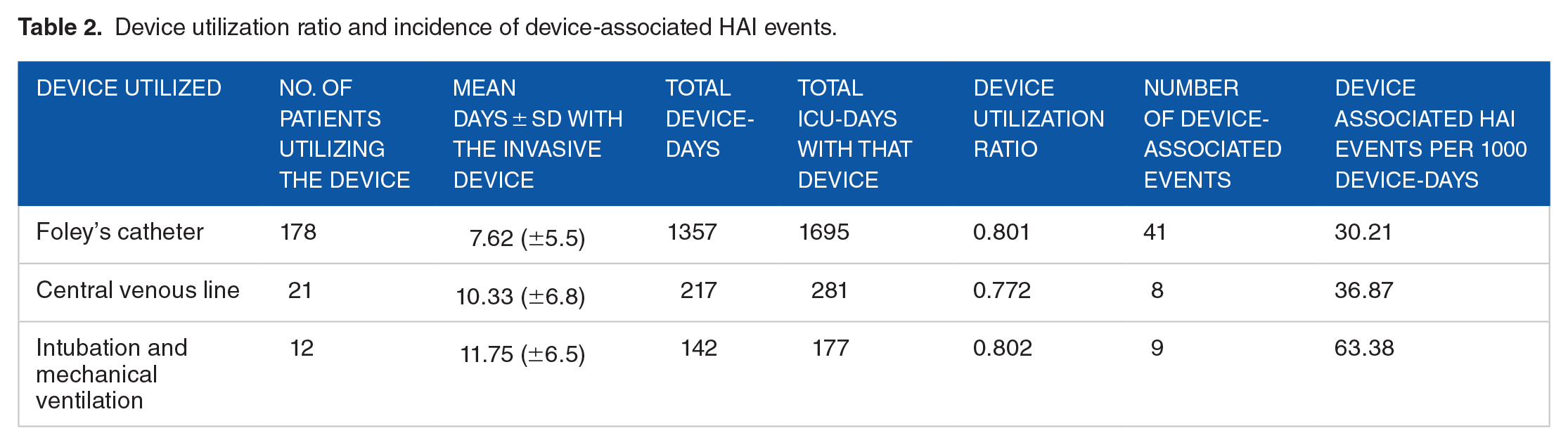
Of the 300 patients, 129 patients (43%) developed 140 HAI events and 11 (8.5%) patients among them developed 2 HAI events during their ICU stay. The incidence of HAI was 55.96 HAI events per 1000 ICU-days. Pneumonia was the most common type of HAI (Table 1) and endotracheal intubation and mechanical ventilation had the highest device utilization ratio (0.802) as well as the highest incidence of device-associated HAI events (63.38 Device associated HAI events per 1000 device-days) (Table 2).
Types of healthcare-associated infection events detected.
Device utilization ratio and incidence of device-associated HAI events.
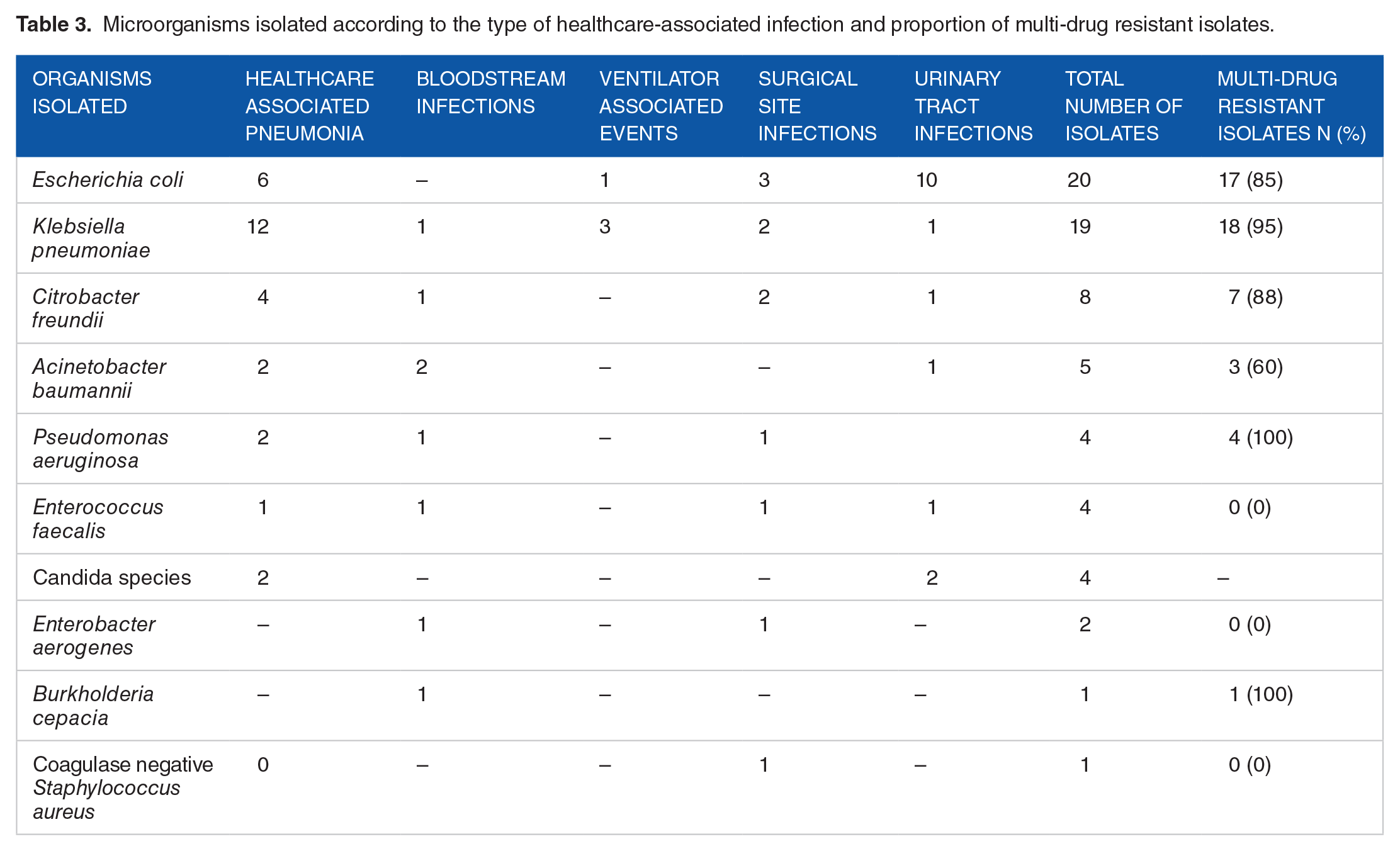
At least 1 pathogen was isolated from 61 of the 129 HAIs (47.3%). Of the 68 total pathogens, Gram-negative bacteria were the most common group of microorganisms isolated (n = 59, 87%),
Microorganisms isolated according to the type of healthcare-associated infection and proportion of multi-drug resistant isolates.
In the bivariate analyses to determine the association of age, sex, ICU stay duration, smoking, presence of comorbidities, immunocompromised status, use of invasive devices, PPI, and sedation with the development of HAIs, ICU stay duration, smoking, use of PPI, invasive device, and sedation had a
Bivariate analysis for the association of healthcare-associated infections with demographic and clinical characteristics.
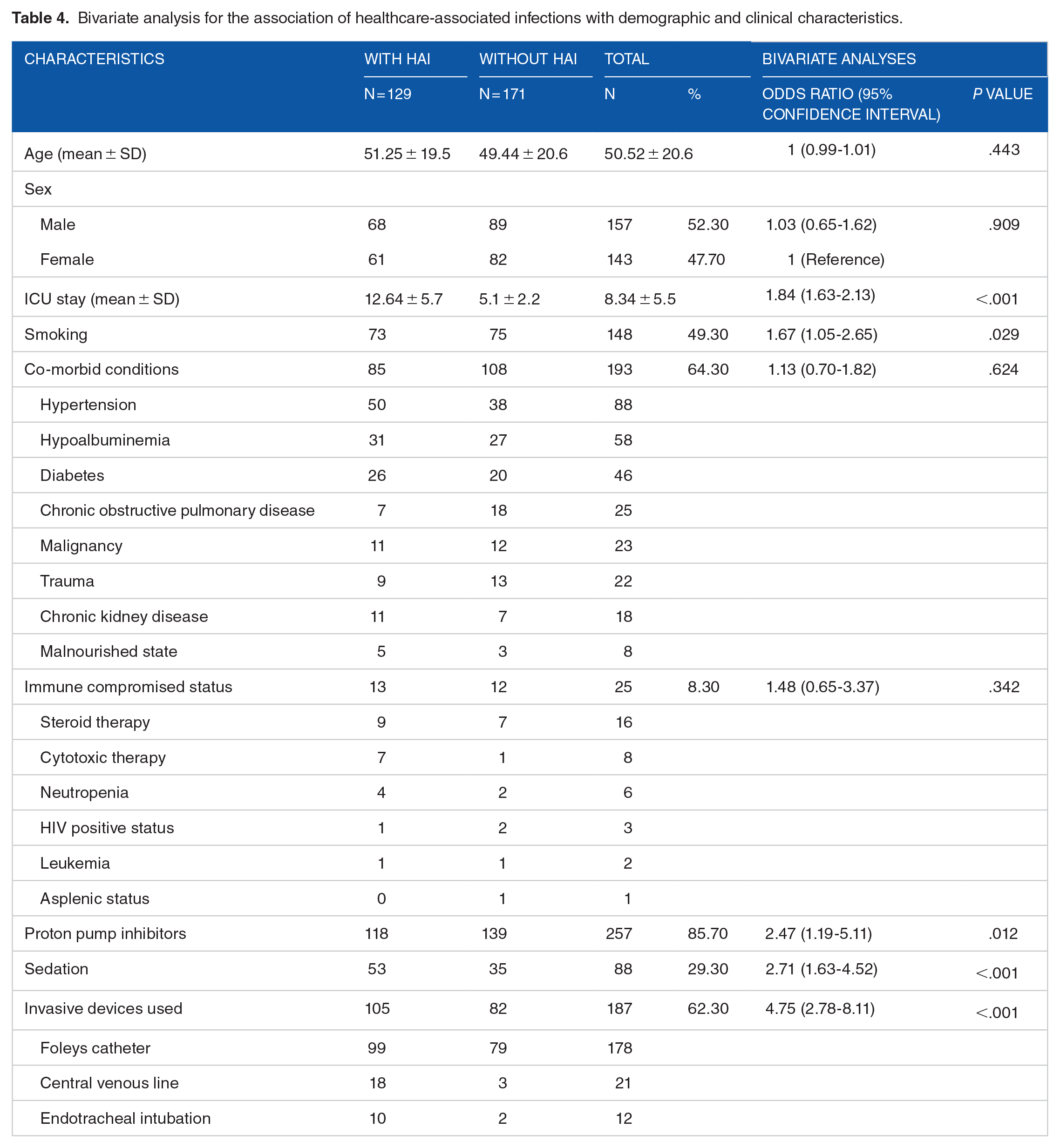
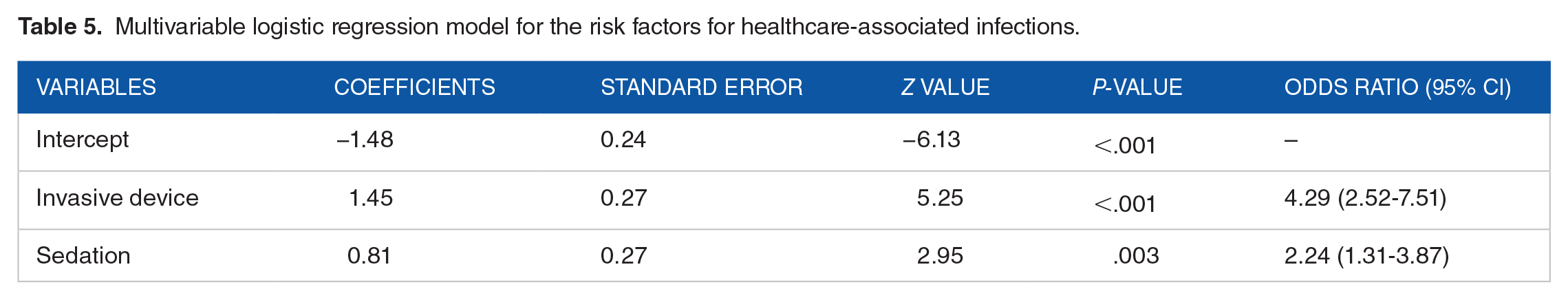
A multiple logistic regression model was constructed with ICU stay duration, smoking, use of PPI, invasive device, and sedation as the independent variables and HAI as the outcome variable. The model showed that ICU stay duration and PPI use were significant covariates for the development of HAI. Given the collinearity among ICU stay duration and PPI use, as indicated by VIF > 10 and because ICU stay duration could be potentially a cause as well as an effect of HAI, we reconstructed a multiple logistic regression model without ICU stay duration. In the final model thus obtained, the use of sedation and invasive devices were the covariates remaining in the model which contribute significantly to the model estimates. We did not find significant interactions between these variables and therefore did not include the interaction terms in the final model. We found the VIF for both the explanatory variables in the model as <10 and hence, concluded that there was no multicollinearity between the explanatory variables in the model. In the likelihood ratio test, the final model was a better fit to the data than the intercept-only model (χ2 = 45.55,
Multivariable logistic regression model for the risk factors for healthcare-associated infections.
Discussion
This study estimated the burden of HAIs, identified their risk factors, causative organisms, and antimicrobial resistance patterns in 3 tertiary hospital ICUs in Kathmandu, Nepal. The use of standardized definitions from the US CDC has allowed the comparison of our results to other hospitals and settings. We found a high incidence of HAIs, including DAIs. Gram-negative organisms were implicated in most of the HAIs and the burden of multi-drug resistant organisms was high. Furthermore, we identified the use of sedation and invasive devices as significant risk factors.
The burden of HAIs observed in this study (prevalence of 43%) was higher than that reported from the ICUs of high-income countries (prevalence of 9.1%-19.2%) but is comparable (pooled incidence density of 55.96 per 1000 patient-days) to that from other low and middle-income countries (pooled incidence density of 47.9 per 1000 patient-days [95% CI 36.7-59.1]).1-3 The DAI rates observed in our study (63.38 VAEs, 36.87 CLABSIs, and 30.21 CAUTIs per 1000 device-days) were also higher than those reported from the comparable ICUs of the INICC (14.1 VAPs, 5.05 CLABSIs, and 5.1 CAUTIs per 1000 device-days) 11 and much higher than those reported from the US NHSN (1.6 VAPs, 1.1 CLABSIs, and 2.7 CAUTIs per 1000 device-days).12,13 Several factors could have contributed to the higher HAI burden in our study. An important factor is the lack of an HAI surveillance system to identify and characterize the HAIs. This system would help identify and prioritize potential interventions as well as evaluations of these interventions. Also, this would raise awareness of the problem among healthcare workers which will further add to the HAI prevention efforts. Another factor is the poor implementation of the infection control and prevention programs including suboptimal hand hygiene compliance in our ICUs. Such gaps have been identified in many resource-limited countries and represent important areas that require action.8,21 In addition, the high device utilization ratios in our study ICUs, which assess the proportion of days in which patients were at risk for the DAI, have likely contributed to the high DAI rates observed. This calls for a focus on avoiding or minimizing the use of invasive devices and reducing the duration of use, in addition to the use of best practices during the insertion and maintenance of the devices. The higher DAI rates in our study compared to those reported in an earlier study from Nepal, despite similar device utilization ratios, likely reflect the differences in the patient population as our study was confined to the medical and general surgical patients whereas the other study included obstetric, gynecological and orthopedic patients as well. The higher DAI rates in our study could also be due to the level of sensitization of healthcare workers to infection control issues, staff to patient ratios, and ICU designs highlighting additional measures to be considered in our ICUs. 10
The most common HAI identified in this study was healthcare-associated pneumonia which occurred in 57 patients (41% of all HAIs). We report this non-ventilator-associated pneumonia separately from the ventilator-associated events. Healthcare-associated pneumonia has been reported as the most common HAI in the surveys from the US and the European Union and constitutes a significant proportion of the HAIs in the resource-limited countries as well.1-3 These infections are frequently underappreciated, but their impact on patient outcomes and healthcare costs is significant and according to an estimate from the US, may even surpass those due to VAP. 22 Though these estimates were lower than those for the patients with VAP, the overall number of deaths and costs attributed to non-ventilator-associated pneumonia were higher owing to its higher incidence compared to VAP. In addition, a recent prospective observational study at 23 medical and surgical ICUs in France showed that ICU acquired pneumonia in non-ventilated patients was associated with an increased risk of 30-day mortality (Hazard Ratio, 1.82 [95% CI, 1.35-2.45]), which was higher than that in the patients with VAP (Hazard Ratio, 1.38 [95% CI 1.24-1.52]). 23 These findings underscore the need for interventions that prioritize hospital-acquired pneumonia.
Less than half of the patients with HAIs (47.3%) have clinical cultures which detected a specific etiologic organism. This is lower than those reported from Europe (52.7%) 3 and the US (70.3%-73.8%).2,24 The underlying factors impacting the recovery of microorganisms from clinical samples are poorly explored in our and similar settings. However, the low yield in our study could be at least partially due to pre-analytical errors, particularly during specimen collection, specimen transport, or specimen receipt in the laboratory. Another important source of pre-analytical error is a prolonged interval between sample collection and processing and incubation in our microbiology lab. Our laboratory does not operate 24 hours a day or on holidays. This means that clinical specimens are stored in the wards for an extended time, often at suboptimal conditions. Such delays have been shown to result in a lower detection rate of pathogens. 25 To help mitigate these effects, communication and collaboration with the laboratory in identifying and minimizing these sources of errors are warranted.
In our study, Gram-negative bacteria were the predominant microorganisms isolated from the patients with HAIs (87% of all HAIs) and Escherichia coli was the most common microorganism. Similar findings were reported in the surveys from Europe and the US and in the meta-analysis of the studies from low and middle-income countries.1,3,24 Gram-negative microorganisms were predominant in another study from an ICU in Nepal which analyzed clinical samples from presumed cases of HAIs. 26 Perhaps, a more concerning finding in our study is that 74% of all the isolates were multi-drug resistant organisms. In an ICU of a tertiary care center in Nepal, investigators found that almost all (95.8%) of the Gram-negative bacteria, isolated from the patients with suspected HAIs, and more than 80% of the isolates obtained from the patients with DAIs, were multidrug-resistant.10,26 Overall, these rates are higher than those reported from the analysis of the US NHSN data on CLABSIs, CAUTIs, VAP, and SSI, 27 but the emerging problem of antimicrobial resistance has been recognized in several low and middle-income countries.28,29 One of the important contributors to this antimicrobial resistance problem, particularly in our ICUs, is the widespread empiric use of antibiotics and failure to narrow antibiotics to culture-directed therapy. Therefore, the optimal use of antibiotics through the implementation of antimicrobial stewardship programs should be prioritized. Such interventions are effective and constitute an important step toward preventing the emergence of antimicrobial resistance. 30
We found sedation use as one of the 2 statistically significant risk factors in our study which increased the odds of HAI by more than double (OR, 2.24; 95% CI, 1.31-3.87). Sedation and analgesia use is common among critically ill patients, particularly among agitated patients or patients under mechanical ventilation. Prior studies have also linked sedation with HAI, though most of the studies have been conducted on mechanically ventilated patients and the findings have been inconsistent.31,32 Possible mechanisms for these associations could be immunomodulatory properties of sedative agents altering the immunologic response to exogenous stimuli, prolongation of exposure to risk factors for infection, micro-aspiration, gastrointestinal motility disturbances, and microcirculatory effects. 32 Apart from minimizing sedation use, additional considerations like sedative choice, improvements in sedation practice, such as the introduction of guidelines and protocols, spontaneous awakening trials, and spontaneous breathing trials could also help mitigate the HAI risk among critically-ill patients.31-33
The other risk factor we identified in our study was the use of invasive devices which was associated with more than 4 times higher odds of HAI (OR, 4.29; 95% CI, 2.52-7.51). Invasive medical devices are used extensively in critically ill patients and several studies have established invasive devices use as an important risk factor. As an example, in the first European Prevalence of Infection in Intensive Care (EPIC) Study, among the 7 independent risk factors identified, 4 were associated with medical devices commonly used in intensive care: central venous catheter (OR 1.35; 95% CI, 1.60-1.57), pulmonary artery catheter (OR 1.20; 95% CI, 1.01-1.43), urinary catheter (OR 1.41; 95% CI, 1.19-1.69), and mechanical ventilation (OR 1.75; 95% CI, 1.51-2.03). 34 A range of factors related to causative bacteria, hosts, and invasive devices are involved in the pathogenesis of device-associated infections and have been reviewed elsewhere. 35 Optimal approaches to the placement, maintenance, and removal of these devices are therefore imperative to minimize the DAI rates.
This study has several limitations. We excluded pediatric patients and patients with cardiovascular and gynecological illnesses because these patients received care in the critical care units separate from our study ICUs. Furthermore, we did not include patients with hemodialysis lines. Therefore, our findings may not be generalizable to these patient populations. Since we did not measure the severity of illness, we could not include these variables in our regression modeling to determine risk factors for HAIs. This may have resulted in a less accurate assessment of risk factors in our study. As mentioned previously in the discussion section, pre-analytic errors may account for our relatively low positive culture rates in our clinical samples. We did not collect data regarding the indications for ICU admission or the antimicrobial agents used to treat patients which could be confounders.
Conclusions
In this prospective study of HAIs in 3 ICUs in a tertiary care center in Nepal, we found a high incidence of HAIs, including DAIs, a high burden of multi-drug resistant organisms, and identified the use of sedation and invasive devices as the significant risk factors. These findings call for increased emphasis on infection control and prevention as well as antibiotic stewardship in our ICUs.
Footnotes
Acknowledgements
We thank Bart K. M. Jacobs MSc, PhD, Biostatistician at the Institute of Tropical Medicine, Antwerp, Belgium for his important inputs in data analysis and interpretation.
Author Contributions
SKS, ABT, and PKS designed the study. SKS acquired, analyzed and interpreted the data and wrote the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of Data and Materials
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
