Abstract
Background:
Soil-transmitted helminths (STH) are still major health problems in resource-poor countries. Despite several epidemiological studies were available in Ethiopia, summarized data on the prevalence of STH among school-aged children (SAC) is lacking in the country.
Objective:
This study was aimed to summarize the existing published studies of STH among SAC children in Ethiopia.
Methods:
The search was carried out in open access databases such as Science Direct, Scopus, and PubMed Central which reported STH in Ethiopia. Open access articles published between 2000 and 2019 were included in this meta-analysis. The pooled prevalence was determined using a random-effect model while heterogeneities between studies were evaluated by I2 test.
Results:
A total of 46 338 children (Male = 23 374 and Female = 22 964) were included in the 70 eligible studies for this meta-analysis. The pooled prevalence of STH among SAC was 33.4%; 95% CI, 29.3% to 37.7% in Ethiopia. Ascaris lumbricoides (19.9%; 95% CI, 17.2%-22.6%) was the most prevalent STH followed by Trichuris trichiura (12.4%; 95% CI, 10.6%-14.1%), and hookworm (7.9%; 95% CI, 6.9%-8.9%) infection in the country. High prevalence of STH was observed in Oromia (42.5%; 95% CI, 31.6%-53.4%) followed by SNNPR (38.3%; 95% CI, 27.7%-48.8%) and Amhara (32.9%; 95% CI, 27.0%-38.8%) regional states. High heterogeneity on the prevalence of STH was observed across studies within and among regions (I2 > 96% and P < .001).
Conclusion:
This review showed that more than one-third of the Ethiopian SAC were infected with STH. The high prevalence of STH observed in this review highlight the needs of improved control and prevention strategies in Ethiopia.
Introduction
Soil-transmitted helminths (STH) are a group of Neglected Tropical Diseases (NTD), which is widely distributed in tropical and subtropical regions. STH affect more than 1.5 billion people in tropical regions in Africa, Asia and Latin America. 1 Ascaris lumbricoides is the most prevalent STH infecting about 1.2 billion people followed by Trichuris trichiura (infecting about 795 million people) and hookworm (Ancylostoma duodenale and Necator americanus), which infects nearly 740 million people worldwide.2,3 The high prevalence of STH in tropical regions is associated with low socioeconomic development and suitable environmental conditions that favor the transmission of these helminths. 4
According to World Health Organization (WHO), 568 million school-age children (SAC) live in areas where STH is intensively transmitted. 1 This indicates that SAC are at higher risk of being infected with STH. These could be associated with the fact that children are more exposed to contaminated soil when they play, walking barefoot, eat soil, and do not have good personal hygiene. It has been reported that the level of sanitation is very poor in developing countries; only 53% of peoples have access to improved sanitation facilities. 5 STH are responsible for chronic infections, which may lead to school absenteeism, delayed physical growth and impaired cognitive development, particularly learning, memory intelligence, and reaction time in SAC. 6
Soil-transmitted helminths is one of the major public health problems in Ethiopia that affect more than 79 million people, of which about 25 million are SAC. 7 The number of published studies on STH in Ethiopia has been increased in recent years. These epidemiological studies address not only the prevalence of STH but also the potential risk factors. There is a need to summarize the available epidemiological studies systematically to estimate the overall prevalence of STH at the national level and to identify high-risk regions requiring interventions. The WHO aims to control STH infections by 2020 by treating at least 75% of infected children in endemic countries. 1 In line with this, the Ethiopian government launched national mass drug administration (MDA) in November 2015 to reduce STH related morbidity. Such intervention needs a systematical summary of existing published studies to identify target groups and target regions.
Therefore, this review aimed to generate a quality estimate of the pooled prevalence of STH and their regional variations among school-aged children in Ethiopia.
Methods
Search strategies
The search strategies were taking into account the PICO elements (Population, Exposure, Comparison, and Outcome). In this review we focused on population and outcome due to all eligible articles were observational studies. We reported the pooled prevalence of STH among SAC in Ethiopia. In line with this, relevant literatures were systematically searched from 3 online databases (PubMed Central, Scopus, and Science Direct) using the following key-words: “A. lumbricoides” OR “T. trichiura” OR “hookworm” OR “nematodes” OR “whipworm” OR “roundworm” OR “helminth” OR “soil-transmitted helminths” OR “geohelminths” OR “nemathelminths” AND “Ethiopia.” The systematic review and selection of relevant literature were conducted according to PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-analysis) guidelines 8 (Supplemental Table S1).
Selection, inclusion, and exclusion criteria
Literatures published in English language from January 2000 to December 2019 were extracted from online public databases. We include original articles reporting the prevalence of STH (A. lumbricoides, T. trichiura, and hookworm) from SAC in Ethiopia. Original articles published in English, sample size at least 200 students and number of positive cases clearly stated in the paper were included in this review. Studies that report the prevalence of STH from patients (human immunodeficiency virus, tuberculosis, malaria, and other health complications), pre-school-aged children, and student under-treatment were excluded from the analysis.
Definition of soil-transmitted helminth infection and diagnostic methods
Soil-transmitted helminth infection is a type of helminths infection caused by roundworms (A. lumbricoides, T. trichiura, and hookworm), which are transmitted by soil contaminated with fecal matter. Several diagnostic methods are available for the detection of STH from patients as well as from the healthy community. However, we selected studies that used better diagnostic approaches namely Kato-Katz thick fecal smear, Mini Parasep concentrator, formal ether concentration, McMaster and Flotach techniques for this systematic review. Kato-Katz thick fecal smear is the WHO recommended technique for the detection of STH infection. 9
Methods of data extraction and quality assessment
The data extraction protocol was prepared and evaluated by all authors. From each published article we extracted the following information: study region, sample size, age range, population type (community or patient-based or school-based), study design, diagnostic methods, the prevalence of total STH, and individual species of STH.
Risk of bias assessment of individual articles included
The quality of studies included in the meta-analysis was assessed by using quality assessment tools developed previously for prevalence studies. 10 Studies were assigned either 0 (low risk) or 1 (high risk) for 10 parameters (Supplemental Table S2). The overall quality was determined by adding the assigned number for each parameter and classified as low risk (⩽2), moderate risk (3-4) or high risk (⩾5) of bias.
Risk of publication bias across studies included in this meta-analysis
The risks of publication bias across studies were assessed using funnel plot symmetry and Egger’s test. The Egger’s test P-value <.05 was used to determine the presence of publication bias across studies.
Statistical analysis
The prevalence of each STH was calculated by dividing the number of STH positive subjects to the total study participants. The heterogeneity among studies used for this meta-analysis was evaluated using inverse variance index (I2) test. 11 I2-value lower than 25%, between 25% and 50% and above 50% were regarded as low, moderate, and high heterogeneity, respectively. 12 Because there was an obvious heterogeneity observed among the studies included in the meta-analysis, we used a random-effect model at 95% confidence interval (CI) for estimating the overall effect. To sort out the cause of heterogeneity, we used a subgroup, sensitivity and meta-regression analysis. The meta-analysis was conducted using Stata software (version 14, STATA Corp College Station, TX), where P < .05 was considered as statistically significant.
Results
Literature search and selection
A total of 1338 studies that report STH infection in children in Ethiopia were available in an online database. Out of these studies, 875 articles were removed due to duplications while 291 articles were excluded based on title and abstract screening. The remaining 172 full-text articles were assessed for eligibility. Of these, a total of 102 articles were excluded from the analysis based on specific exclusion criteria and 70 articles were selected for this meta-analysis (Figure 1).

PRISMA flow diagram of publications considered for the review on STH in Ethiopia.
Characteristics of the eligible studies
The detailed characteristics of the 70 eligible articles included in the meta-analysis were presented in Table 1. The studies included in this meta-analysis were obtained from 5 regional states; 35.7% from Amhara,13-37 24.3% from SNNPR,38-54 22.9% from Oromia,55-70 15.7% from Tigray,71-81 and 1.4% Benshangul Gumuz 82 regional states. Unfortunately, there were no studies for other regions and city administrations of Ethiopia that fulfill the inclusion criteria used for this study. All studies included in this review were conducted on SAC (with a minimum age of 5 years) in Ethiopia. The upper age limits of children were not described in some studies.
Characteristics of the 70 eligible articles included in this review.
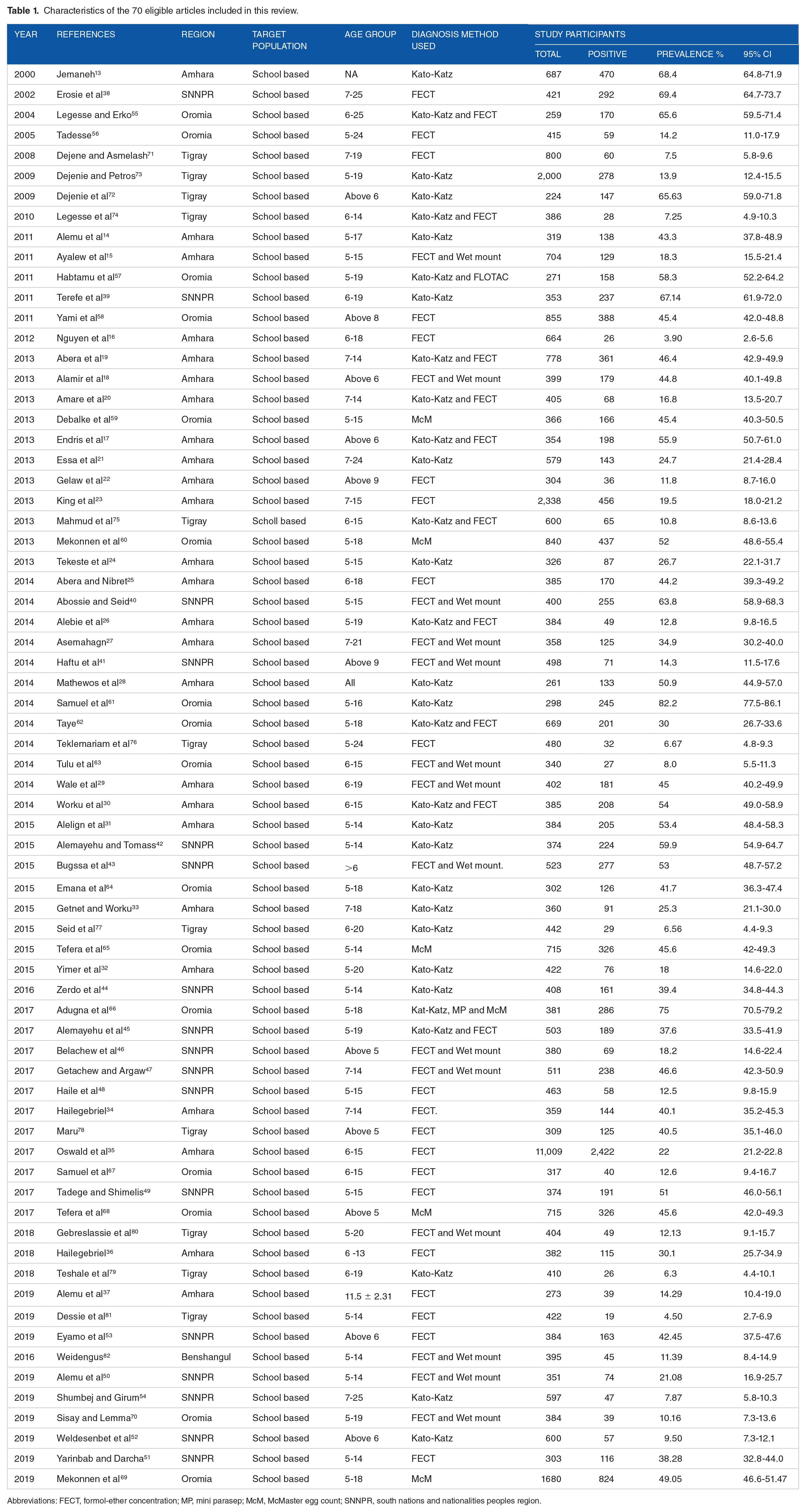
Abbreviations: FECT, formol-ether concentration; MP, mini parasep; McM, McMaster egg count; SNNPR, south nations and nationalities peoples region.
Risk of bias within individual studies
Among the 70 studies included for this meta-analysis, low risk of bias, moderate risk of bias and high risk of bias were observed on 46 studies (65.7%), 21 studies (30%) and 3 studies (4.3%), respectively (Supplemental Table S2). The overall summary of the risk assessment of all studies included in this meta-analysis showed lower-risk of publication bias across studies.
Prevalence and burden of STH among school-aged children in Ethiopia
A total of 46 338 children (Male = 23 374 and Female = 22 964) were included in the eligible studies. The prevalence of STH was ranged from 3.9% to 82.2% among SAC in Ethiopia. Out of the total 46 338 SAC, 15 477 (33.4%) of them were infected by STH in Ethiopia. The pooled prevalence of STH among SAC was 33.4% (95% CI, 29.3%-37.7%) with substantial heterogeneity (I2 = 99.3%, P < .001) in Ethiopia (Figure 2). Ascaris lumbricoides was the most prevalent STH 9221 (19.9%; 95% CI, 17.2%-22.6%) followed by T. trichiura 5746 (12.4%; 95% CI, 10.6%-14.1%) and hookworm 3661 (7.9%; 95% CI, 6.9%-8.9%) as shown in Supplemental Figures S1-S3, respectively. In addition, the burden of A. lumbricoides, T. trichiura and hookworm was 9221 (19.9%), 5746 (12.4%), and 3661 (7.9%), respectively in Ethiopia. High heterogeneities on the prevalence of STH were detected between studies included in the meta-analysis (I2 > 97% and P < .001). To sort out the causes of high heterogeneity, we did subgroup analysis and meta-regression.
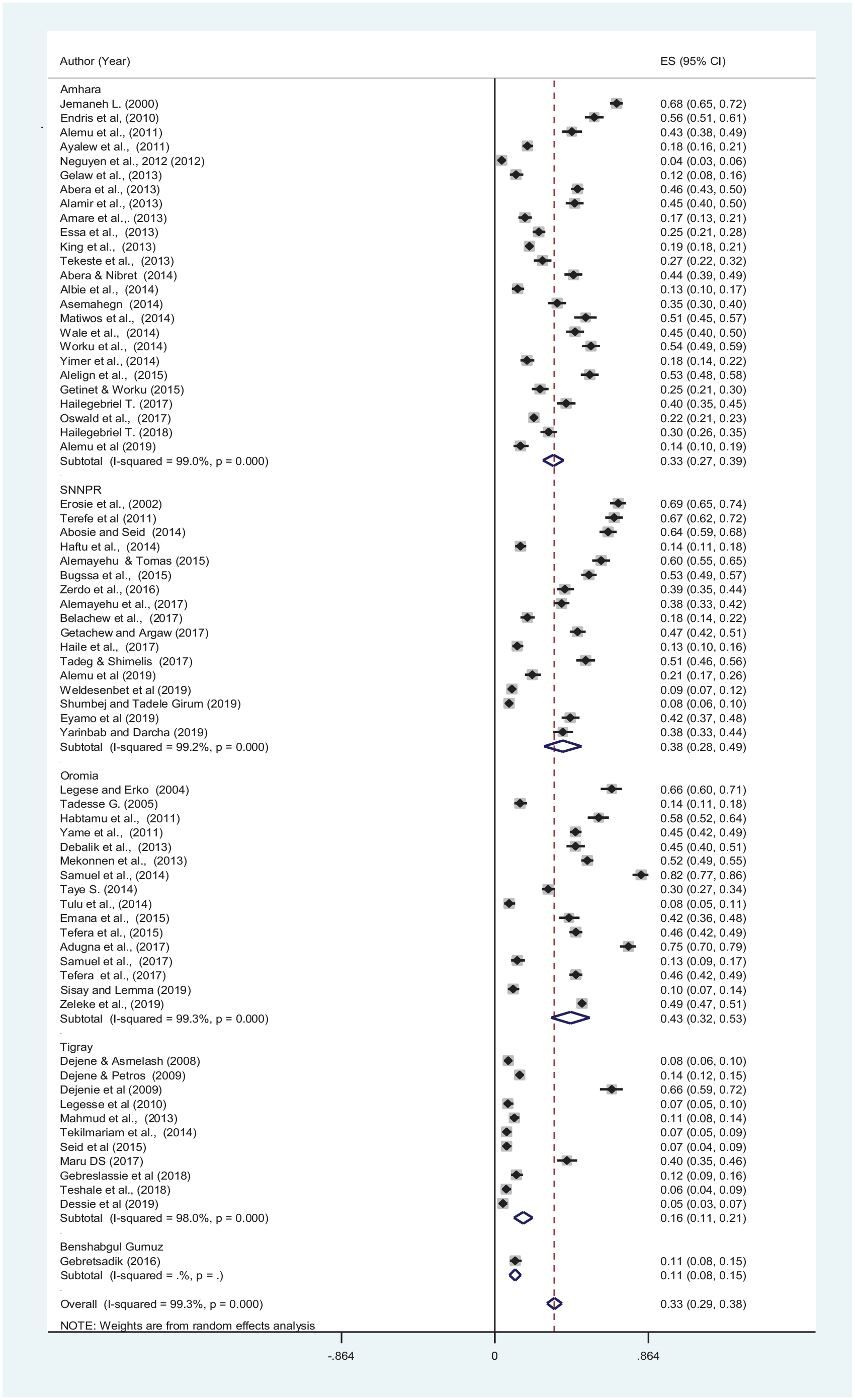
Forest plot for prevalence of STH among schoolchildren in Ethiopia. Each square represent effect size (ES) of individual studies and the horizontal line represent the 95% CI. The diamond indicates the pooled effect and the vertical dash lines indicate the overall estimate.
Sub-group analysis
The sub-group analysis indicates that STH was more prevalent in Oromia (42.5%; 95% CI, 31.6%-53.4%) followed by SNNPR (38.3%; 95% CI, 27.7%-48.8%) and Amhara region (32.9%; 95% CI, 27.0%-38.8%) while low prevalence in Tigray (15.9%; 95% CI, 10.6%-21.1%) and Benshangul Gumuz regional states (Figures 2 and 3). Ascaris lumbricoides were more prevalent in SNNPR (26.4%; 95% CI, 18.4%-33.9%), Oromia (23.0%; 95% CI, 16.9%-29.2%), Amhara (18.6%; 95% CI, 14.5%-22.9%) and Tigray (9.6%; 95% CI, 6.3%-12.9%) regions (Supplemental Figure S1). T. trichiura infection was more prevalent in Oromia (21.6%; 95% CI, 14.8%-28.4%), Amhara (11.9%; 95% CI, 8.7%-15.1%) and SNNPR (10.1%; 95% CI, 7.3%-12.9%) regional states (Supplemental Figure S2). Similarly, hookworm infection was more common in Oromia (14%; 95% CI, 9.8%-18.2%), SNNPR (9.3%; 95% CI, 6.8%-11.9%) and Amhara (6.1%; 95% CI, 4.8%-7.3%) regional states (Supplemental Figure S3). The prevalence of T. trichiura and hookworm were below 3% in Tigray region.
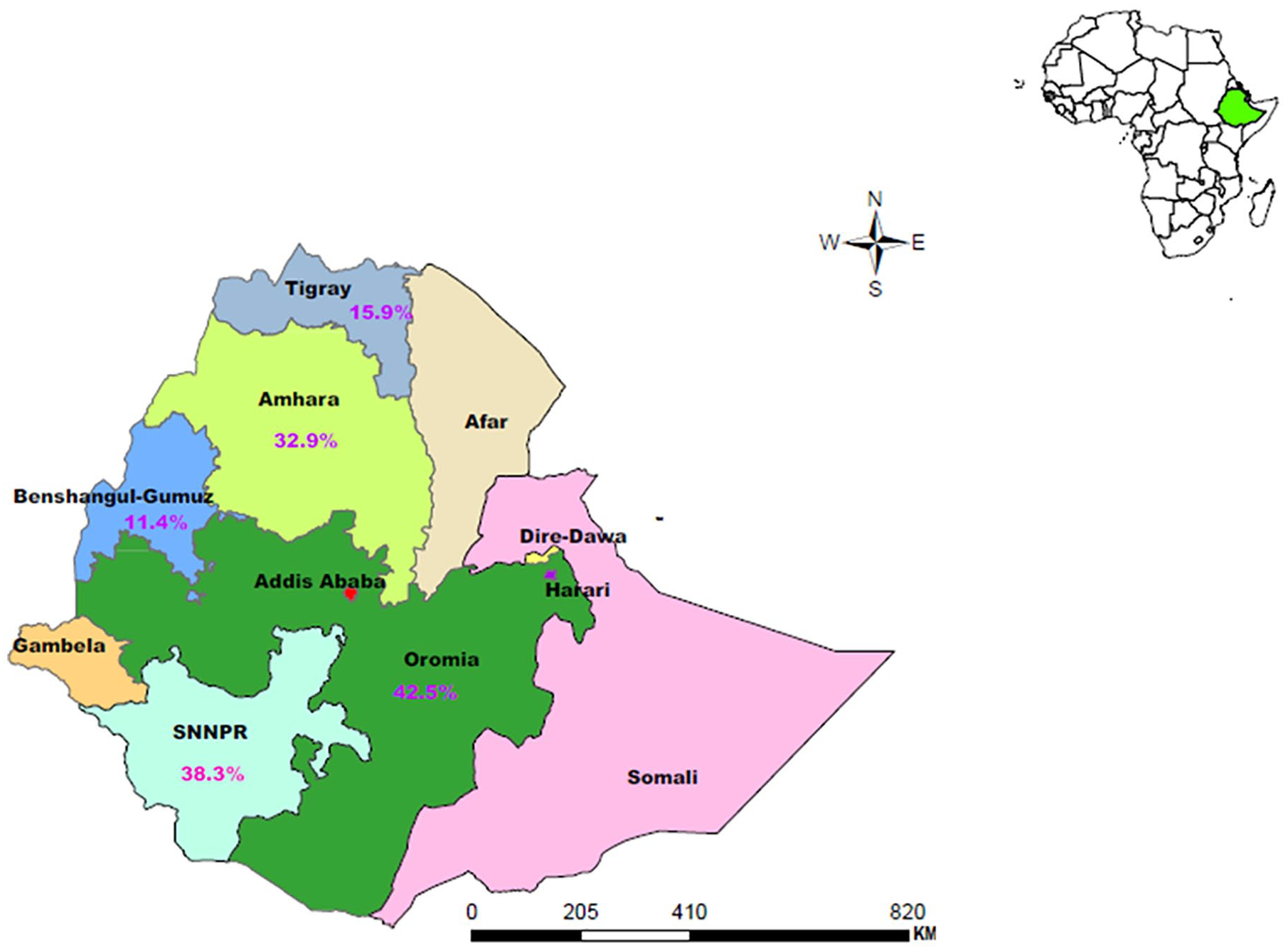
Regional distribution of STH among schoolchildren in Ethiopia.
The pooled prevalence of STH among SAC in years 2000 to 2010, 2011 to 2014, and 2015 to 2019 were 40.76% (95% CI 24.5%-57.1%), 34.4% (95% CI 27.2%-41.6%), and 30.6% (95% CI 25.0%-36.3%), respectively (Supplemental Figure S4). This finding has suggested the declining trends in the prevalence of STH in Ethiopia. In addition, Ethiopia launched national MDA program to reduce STH related morbidity in 2015. In order to see the contribution of MDA, we compare the pooled prevalence of STH before and after the launching of the intervention program. The result indicated that the pooled prevalence of STH declined from 35.9% to 30.6% after the launching national MDA programs in Ethiopia (Figure 4). This intervention program contributes for the reduction in the prevalence of STH in all regional states of Ethiopia. The pooled prevalence of STH was declined from 53.6% to 33.6%, 44.5% to 40%, 33.6% to 30.7%, and 17.9% to 13.6% in SNNPR, Oromia, Amhara, and Tigray regions, respectively. The highest reduction was observed from SNNPR as compared with other regional states in Ethiopia. The launching of MDA program showed encouraging results in the reduction of STH at least among schoolchildren in Ethiopia.
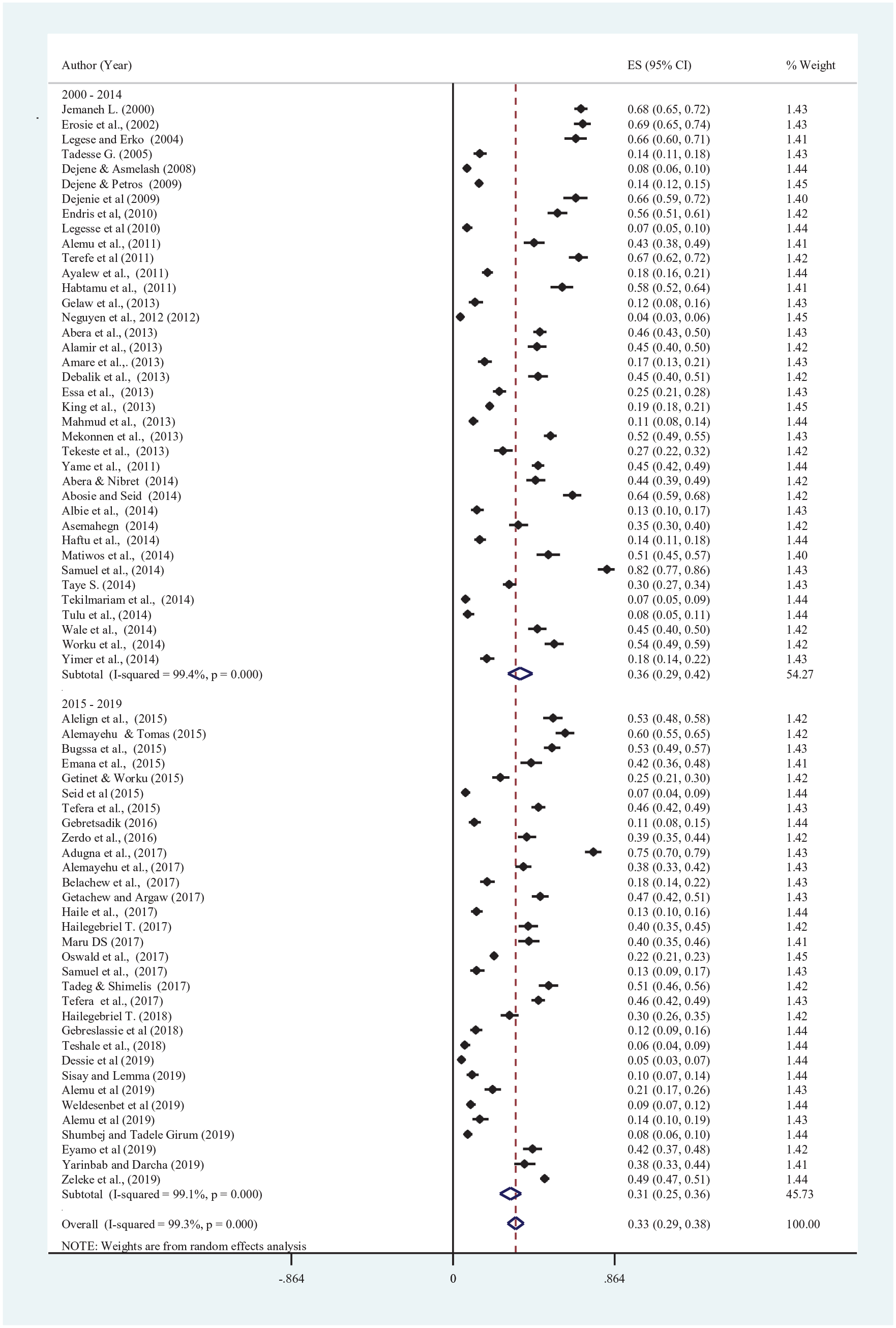
Forest plot showing the pooled prevalence of STH among schoolchildren in Ethiopia before and after the launching of MDA in Ethiopia.
Six parasitological methods individually or in combination were used in the eligible articles included in this meta-analysis. The pooled prevalence of STH were 47.8% (95% CI, 45.3%-50.37%), 37.3% (95% CI, 27.1%-47.6%), 33.6% (95% CI, 21.6%-45.7%), 28.6% (95% CI, 19.6%-37.6%), 26.4% (95% CI, 20.4%-32.3%) using McMasters, Kato-Katz, Kato-Katz and FECT, FECT and wet mount, and FECT, respectively (Supplemental Figure S6). The prevalence of STH were 75.1% (95% CI, 70.6%-79.5%) and 58.3% (95% CI, 52.3%-64.3%) using a combinations of Kato-Katz, McMaster and Mini Parasep, and Kato-Katz and FLOTAC, respectively (Supplemental Figure S6). The combinations of these techniques were used only in 2 separate studies.
Risk of publication bias across studies included in the meta-analysis
The funnel plot symmetry demonstrates the presence of publication bias among studies included in this meta-analysis (Figure 5). Similarly, the Egger’s test results (P < .05) indicate publication bias among studies.
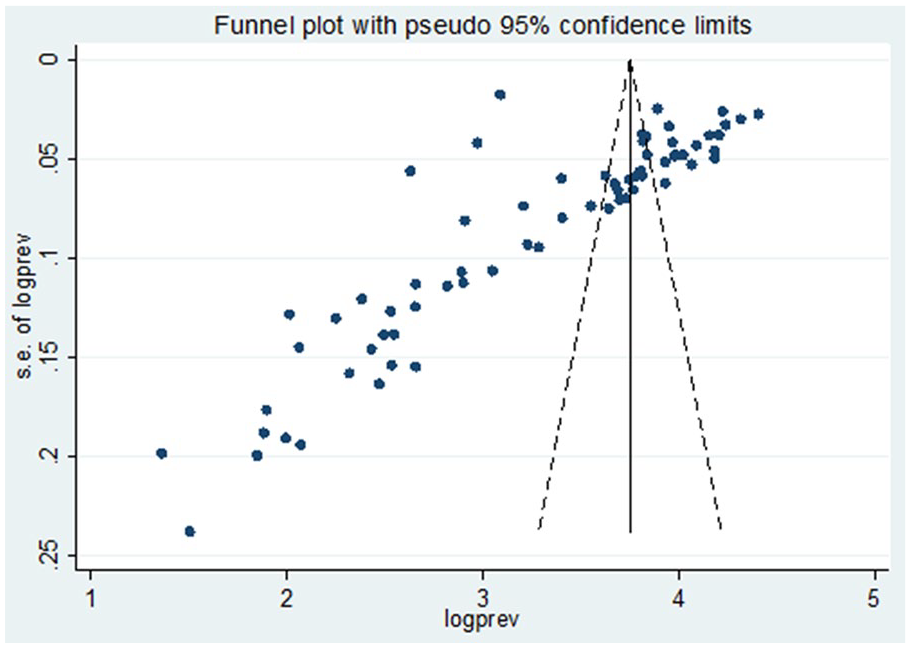
Funnel plot indicates publication bias across studies used in this meta-analysis.
Meta-regression and sensitivity analysis
We performed meta-repression analysis to identify the sources of heterogeneity across studies. The meta-regression analysis showed that region of study (regression coefficient: 0.809, 95% CI, 0.689-0.950, P = .011) might be the source of heterogeneity (Figure 6a). Years of publication (regression coefficient: 0.908, 95% CI, 0.689-1.195, P = 0.487, Figure 6b) and parasitological methods used (regression coefficient: 1.094, 95% CI, 0.969-1.235, P = 0.142, Figure 6c) did not contribute for the heterogeneity. In addition, sensitivity analysis was performed by recalculating the pooled prevalence of STH by sequentially removing one-by-one to assess the contribution of individual study the overall effect. The pooled prevalence remained stable and the result was not driven by individual studies included in the meta-analysis.
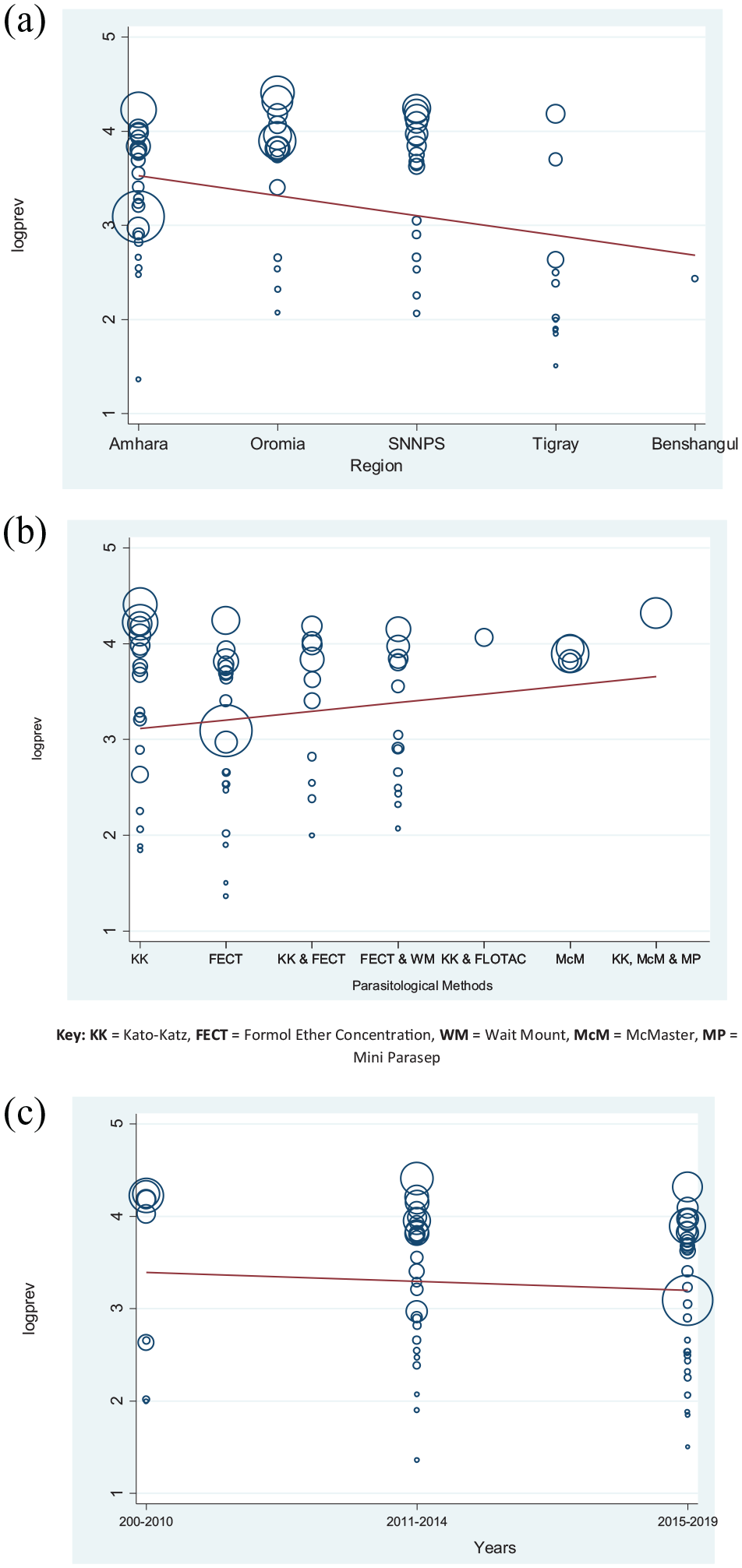
Meta-regression analysis of (a) Region of study. (b) Parasitological methods used. (c) Year of publication of STH among schoolchildren in Ethiopia.
Discussion
Soil-transmitted helminths are a group of NTDs that affects nearly a quarter of the world population. 1 To our knowledge, this is the first systematic review and meta-analysis on the prevalence of STH among SAC in Ethiopia. This review analyzed epidemiological studies on STH to estimate the pooled prevalence and to identify high-risk regions for interventions. In turn, we hope that our results will help policy-makers and other stakeholders to design appropriate control strategies for STH in Ethiopia.
The overall pooled prevalence estimates (33.4%) obtained in this review is similar to Turkey, 83 Kenya, 84 Nigeria, 85 and Rwanda. 86 The finding of this review is higher reports from sub-Saharan Africa87,88 and lower than STH reported from Afghanistan, 89 Kenya, 90 Nepal, 91 and Nigeria. 92 These differences might be associated with the presence of poor environmental sanitation and suitable climatic conditions in Ethiopia. Both the toilet coverage and level of sanitation in Ethiopia are one of the lowest in sub-Saharan Africa; about 52% of the Ethiopian population are still using unimproved sanitation facilities and 35% of them practice open defecation. 93 The pooled prevalence estimate of STH in this meta-analysis was even higher than that reported in a community-based study in Ethiopia. 87 Community-based studies are usually targeting both children and adult population. The exposure of adults for STH is lower than that of SAC due to better shoe wearing habits, avoidance of fecal contaminated soils and reduced soil contact. This indicates that a higher prevalence of STH is expected among SAC than in the general population. A similar observation was reported in a meta-analysis from South Asia and Southeast Asia. 94 All these data showed that SAC are vulnerable to STH than the general population in the country.
The study revealed that A. lumbricoides was the most prevalent STH followed by T. trichiura and hookworm which is in line with the global trend as well as meta-analysis reported from Nigeria, 92 South America, 95 and Southeast Asia. 94 The higher prevalence of A. lumbricoides is usually associated with the suitability of the environmental condition along with the high fecundity of Ascaris and the durability of their eggs in contaminated soil. It is known that adult A. lumbricoides produce up to 200 000 eggs per day. 96 The pooled prevalence estimate of hookworm in the present study is lower than reports from elsewhere.87,92,95,97 These variations might be explained by geographical difference, socio-economic characteristics of the study populations, level of environmental sanitation, shoe wearing habits, diagnostic methods used in the different studies. The study populations included in this review were school children, which might have better shoe wearing habit that reduce the level of hookworm infections.
There are clear differences in the pooled prevalence of STH among regions in Ethiopia. The highest pooled prevalence of STH was observed from Oromia region while low pooled prevalence was observed from Tigray region. This might be associated with environmental and climatic factors (temperature, rainfall, and humidity) that contribute to the high prevalence of STH in SNNP and Oromia regions. The south and southwestern part of Ethiopia, where SNNP and the Oromia regions are located, received high rainfall and forested nature 98 as compared with the northern part of Ethiopia, which consists of Tigray and Amhara regions.
The pooled prevalence of A. lumbricoides, T. trichiura and hookworm were varied from region to region in Ethiopia. The highest pooled prevalence of A. lumbricoides was observed from SNNPR regional state while T. trichiura and hookworm were more prevalent in Oromia region. The pooled prevalence of A. lumbricoides, T. trichiura and hookworm were very low as compared with other regional states. Climatic factors of Oromia and SNNPR may create favorable conditions for the high prevalence of STH in these regions.
Several parasitological methods were used among studies used in this review. McMaster egg counting technique showed the highest pooled prevalence of STH followed by Kato-Katz fecal smear and combination of Kato-Katz and FECT. Kato-Katz thick fecal smear is the recommended parasitological methods for the detection of STH.9,99 Several study showed that Kato-Katz is more superior to McMaster for the detection of STH.100,101 However, this review indicated that McMaster was superior to Kato-Katz. These might be associated with high infection intensity of STH in the areas; all studies reporting STH using McMaster egg count was from Jimma Zone and relatively higher infection of hookworm infection in the area. Combinations of Kato-Katz, McMaster and Mini Parasep or Kato-Katz and FLOTAC resulted in higher prevalence of STH than all other methods. However, only 2 separate studies used these methods for the detection of STH in the country. A single FLOTAC is more sensitive than double or triple Kato-Katz for the diagnosis of STH.102,103 Combinations of the 2 or more methods generally give higher sensitivity than a single method. 100
This meta-analysis showed that there is a slight reduction in the prevalence of STH among SAC in recent years in the country. The highest pooled prevalence was observed before 2010 while lower prevalence was observed from 2015 onwards. The meta-regression analysis showed no significant difference in the pooled prevalence of STH in the specified years. The pooled prevalence of STH was slightly reduced from 35.9% to 30.6% after the launching of national MDA program. This result showed that MDA bring a reduction on the prevalence of STH in the country. This suggests that MDA should be implemented in all school-aged children in all parts of Ethiopia. Moreover, additional measures such as proper environmental sanitation, increased community awareness and provisions of pure drinking water should be properly integrated into the ongoing MDA program. The pooled prevalence of STH before the launching of MDA program obtained in this review will be serves as baseline information for evaluating the outcome of MDA and other epidemiological studies in Ethiopia.
This systematic review and meta-analysis revealed that STH infections are still highly prevalent among SAC in Ethiopia. More-than one-third of SAC in Ethiopia are still positive for STH. We hope that the results of this meta-analysis will serve as an important input for policy-makers and regional administration on the control and prevention of STH in the country. This result highlights the importance of strong commitments and integrated work among stakeholders to improve environmental sanitation, increased public awareness and expand ongoing mass drug administration in Ethiopia. Combinations of these strategies might be effective in reducing the burden of STH infections from SAC in Ethiopia.
Although this systematic review generated valuable data on the prevalence of STH in Ethiopia, it has several limitations. First, the data used in this review were not derived from all regions in the country; the articles included in this meta-analysis were obtained from 5 regions (accounts for about 86% of the total population of the country) out of the 9 regional states of Ethiopia. The pooled prevalence of STH in this study may not fully represent the prevalence of STH in Ethiopia. Second, the publications on STH were not evenly distributed even in the 5 regions included in this review. Nearly 36% of the articles included in this study were reported from Amhara region while only 1.4% from Benshangul Gumuz region. Third, most of the eligible studies used single stool examination rather than multiple stool examination as recommended by WHO may results underestimation of the prevalence of STH in the country. In addition, only 44.3% of the studies included in this meta-analysis were used the recommended Kato-Katz that may leads to underestimate the true prevalence. Fourth, this review showed that there was high heterogeneity across studies included in this meta-analysis. These might be associated with study design, sources of the study population and regional variation on the prevalence of STH.
Conclusion
The present study revealed that more than one-third of SAC in Ethiopia are infected with STH. The prevalence of A. lumbricoides, T. trichiura, and hookworm among SAC follows the global trend where A. lumbricoides is the most prevalent followed by T. trichiura and hookworm. The prevalence of STH shows a slightly declined after the launching of MDA in the country. Regional variation is the major contributing factor to the heterogeneity across studies observed in the country. This review highlights the importance of an improved control and prevention strategies of STH in Ethiopia.
Supplemental Material
S1_Fig_xyz480369f1b0f5e – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S1_Fig_xyz480369f1b0f5e for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S1_Table_PRISMA_checklist_xyz48036d8019d19 – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S1_Table_PRISMA_checklist_xyz48036d8019d19 for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S2_Fig_xyz48036681e41be – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S2_Fig_xyz48036681e41be for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S2_Table_Assessement_of_quality_of_papers_-_Copy_xyz480362870cfc3 – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S2_Table_Assessement_of_quality_of_papers_-_Copy_xyz480362870cfc3 for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S3_Fig_xyz48036fd88fa9b – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S3_Fig_xyz48036fd88fa9b for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S4_Fig_xyz4803665f52a0b – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S4_Fig_xyz4803665f52a0b for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Supplemental Material
S5_Fig_Subgroup_analysis_by_parasitological_methods_used_xyz480369537874f – Supplemental material for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental material, S5_Fig_Subgroup_analysis_by_parasitological_methods_used_xyz480369537874f for Prevalence of Soil-Transmitted Helminth Infection Among School-Aged Children of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel, Endalkachew Nibret and Abaineh Munshea in Infectious Diseases: Research and Treatment
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of supporting data
All available data are attached with the manuscript.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
