Abstract
Background:
In Madagascar, human papillomavirus (HPV), human immunodeficiency virus (HIV), and hepatitis B virus (HBV) infection, as well as syphilis share common risk factors but seem to differ in their prevalence. We measured and compared their prevalence in the country.
Methods:
The data used in this study came from the Saint Damien Health Centre in Ambanja, Madagascar. The tests used for disease detection were the Alere Determine, Virucheck, rapid plasma reagin, and S-DRY self-HPV samples for HIV infection, HBV infection, syphilis, and HPV infection, respectively.
Results:
In men and women, respectively, the prevalence was 0.6% and 0.4% for HIV infection, 2.2% and 2.0% for HBV infection, and 0.6% and 0.3% for syphilis. The HPV infection prevalence was 39.3%.
Conclusions:
Despite common risk factors, the prevalence of HPV infection was high, in contrast to a much lower prevalence of other sexually transmitted infections (STIs) in the same geographical area. Further investigations are required to clarify the status of STIs in the Malagasy population.
Introduction
Few data on the epidemiology of sexually transmitted infections (STIs) in Madagascar are available. The prevalence of human immunodeficiency virus (HIV) infection seems to be low, although it is difficult to estimate precisely. In 2008, the HIV/AIDS World Bank Program reported a prevalence of 0.29% to 1.47%, depending on the geographic area within the country, with higher rates in coastal cities. 1 In contrast, the prevalence of syphilis in 2008 was 5.6% (15% in 1995), although in other sub-Saharan African states, such as Botswana, it was as low as 0.95%. 1
The prevalence of human papillomavirus (HPV) infection in Madagascar varies widely across the country, mainly depending on population factors, such as the region of residence and occupation.2,3 In a previous study, we reported a high prevalence (38%) of 14 high-risk HPV (hrHPV) types in Malagasy women aged 30 to 65 years. 4 Chronic infection with hrHPV is known to be the primary cause of cervical cancer (CC). 5 About 90% of HPV infections are cleared within 6 to 24 months, and several cofactors are considered to affect the chronicity of HPV infections, including the viral load, coinfection with several HPV types, environmental factors, such as smoking, and coinfections with other STIs. 6 Furthermore, multiple independent risk factors for the HPV infection’s acquisition in women are known, such as the younger age, the number of sexual partners, early age at first sexual intercourse, and use of oral contraceptives.7–9
Human immunodeficiency virus infection significantly increases a woman’s risk of developing CC by impairing her natural cell-mediated immune response, thereby altering her capacity to properly eliminate HPV. This causes HPV to persist in the cervix, with the subsequent premalignant and malignant transformation of the infected cervical cells.10–12 One goal of this study was to confirm this high prevalence of HPV infection in Madagascar in a larger series. Another was to compare it with the prevalence of HIV infection and other STIs in the same region to assess possible links between HPV infection and diseases that share several risk factors with it.
Materials and Methods
Study design and population
This study was conducted in collaboration with the Saint Damien Health Centre in Ambanja, Madagascar. This city has more than 33 000 inhabitants and is located at an important crossroads in northern Madagascar (Diego Suarez Province). It is surrounded by plantations and cattle-breeding areas. Since 2010, the Saint Damien Health Centre has been involved in various screening and prevention programs for CC and STIs.
This study is based on data from both the blood donor clinic at the Saint Damien Health Centre and a CC screening campaign conducted at the same facility. The first set of data was obtained from blood samples collected between 2010 and 2015, which were screened for HIV, hepatitis B virus (HBV), and syphilis. Women and men from Ambanja (n = 8432) and its surroundings, aged 16 to 75 years, contributed to this database, and all the participants from this region who volunteered to be screened were included.
The second database included data from 1020 women, aged 30 to 65 years, who performed HPV self-sampling from 2013 to 2015 as part of the CC prevention campaign undertaken by the Saint Damien Health Centre. 13 In developing countries, cytology as a screening method for CC seems to be difficult to conduct on a large scale. A previous study conducted in Cameroon showed that HPV-based screening is feasible and increases the effectiveness of CC screening in low-resource settings. 14 In addition, it has been shown that the acceptability of the self-HPV test is excellent for Malagasy women, whether they come from the city or the countryside. 15
This study includes people from 2 different populations but from the same geographical region. The screening programs, for blood donors and CC, are centralized and managed from the Saint Damien Health Centre. All the participants were volunteers. In this sense, it can be imagined that people who know that they are infected with an STI or who are ill are less willing to participate in screening programs, especially for donating blood. The socio-demographic data collections have not been specifically designed for this study.
The collaboration between the Geneva University Hospitals and the Saint Damien Health Centre was established in 2010 and has offered screening services for CC ever since. These services are provided at both the health facility and surrounding health dispensaries. The goals of this collaboration are to simultaneously train Malagasy health workers to prevent and manage CC while screening and treating the target population. Women residing in the Ambanja region are considered eligible to participate in this program, and the exclusion criteria include a previous history of CC or cervical therapy that would affect the visualization of the cervix and current pregnancy. The collection of data from this CC screening campaign was approved by the Cantonal Human Research Ethics Commission of Geneva (CCER; original project number CER: 14-071; amendment number: PB_2016-02338) and the Malgasch National Commission for the Ethics of Science and Technology.
Study protocol
All patients received general information about CC, its prevention, and the relevant screening and treatment services available. They were informed of their test results and an appropriate management strategy was proposed in cases of HPV infection. All the participants were also asked to complete a socio-demographic questionnaire reporting information such as their age, home location, and professional activities.
HIV, HBV, and syphilis detection
The participants received information about syphilis, HIV, and HBV infection from the health professionals. They were told that they would be tested for these STIs before they could donate blood.
The Alere Determine HIV-1/2 Ag/Ab Combo (Alere Medical Co., Ltd., Matsudo-shi, Chiba, Japan) was used to screen for HIV infection. This is a qualitative, rapid point-of-care immunoassay (results are available in 20 minutes) that detects both HIV-1/2 antibodies and HIV-1 antigen in several types of samples.
The Virucheck HBsAg assay (Orchid Biomedical Systems, Goa, India) was used to detect HBV infection. This is a rapid, qualitative, 2-site sandwich immunoassay that detects an HBV surface antigen in serum and plasma specimens.
The rapid plasma reagin (RPR) test was used to detect syphilis. This is a rapid, qualitative test based on an 18-mm circular nontreponemal flocculation card–containing antigen. The antigen suspension is carbon particle cardiolipin antigen 1, which detects reagin, an antibody-like substance in the serum or plasma of syphilitic individuals. Reagin binds to the test antigen (cardiolipin-lecithin-coated cholesterol particles), causing macroscopic flocculation.
HPV sample collection and analysis
Eligible women signed an informed consent form and then performed a self-HPV test using a dry swab. They were instructed to hold the brush with their fingertips and insert it into the vagina while carefully avoiding contact with the external genitalia. When patients felt resistance (at least 6-cm depth), they were instructed to turn the brush 3 times while maintaining the pressure with their fingers, remove it gently, and place it into the plastic tube.
Human papillomavirus genotyping was performed with the Anyplex II HPV28 Detection test (Seegene Inc., Seoul, South Korea), a semiquantitative, real-time multiplex polymerase chain reaction (PCR) assay used to screen and type 28 HPV genotypes. Using the Dual-Priming Oligonucleotide (DPO; Seegene Inc.) and Tagging Oligonucleotide Cleavage and Extension (TOCE; Seegene Inc.) technologies, this test can simultaneously detect 19 hrHPV types (16, 18, 26, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 68, 69, 73, and 82) and 9 low-risk HPV (lrHPV) types (6, 11, 40, 42, 43, 44, 54, 61, and 70). β-Globin is also detected as the internal control to confirm the assay validity. Knowing the step at which the melting curve becomes positive allows for semiquantification of the DNA load of the β-globin and HPV genomes, which can vary from low (+: positive after 40 PCR cycles, <102 copies/reaction), to intermediate (++: positive within 31-39 PCR cycles, ≥102 and <105 copies/reaction), to high (+++: positive before 31 PCR cycles, ≥105 copies/reaction). Whenever the quantity of HPV genome was insufficiently high enough to be detected by the Anyplex device by running up to 40 PCR cycles, the test result was considered as invalid. Analyses were run twice before officially declaring the test result as “invalid.”
Statistical analyses
Data were analyzed with the Stata Statistical Software: Release 13 (StataCorp LP, College Station, TX, USA). Socio-demographic data and infection status of the study participants in the blood donor database were first determined. The prevalence of each STI was calculated in terms of different independent variables that were common to the 2 databases used. The prevalence of each STI was also stratified by age group. All hypotheses were bilateral, and P values of <.05 were considered statistically significant.
Role of the funding source
This study, and more specifically the CC screening campaign, was supported by the Action Madagascar Foundation and the University Hospitals of Geneva, Switzerland. The funding bodies had no role in the study design, data collection or analysis, decision to publish, or preparation of the article. They mostly provided material assistance on the field.
Results
Socio-demographic characteristics
In total, 7632 men and 800 women were included in the blood donor group (Table 1). Of these, 6715 (79.9%) were aged 20 to 39 years, and the average age was 30.7 ± 7.9 years for male participants and 31.0 ± 8.3 years for female participants. Among the professional activity categories, farmers were most strongly represented (41.5%, 2380/5732). The male and female populations included the same proportions of farmers and students. However, women worked independently more often than men (43.6% [217/498] vs 27.5% [1439/5234], respectively; P < .001). In this population, women more often came from rural areas than men (52.0% [259/498] vs 38.4% (2008/5224], respectively; P < .001).
Socio-demographic data and infectious status of the study participants in the blood donor group (n = 8432).
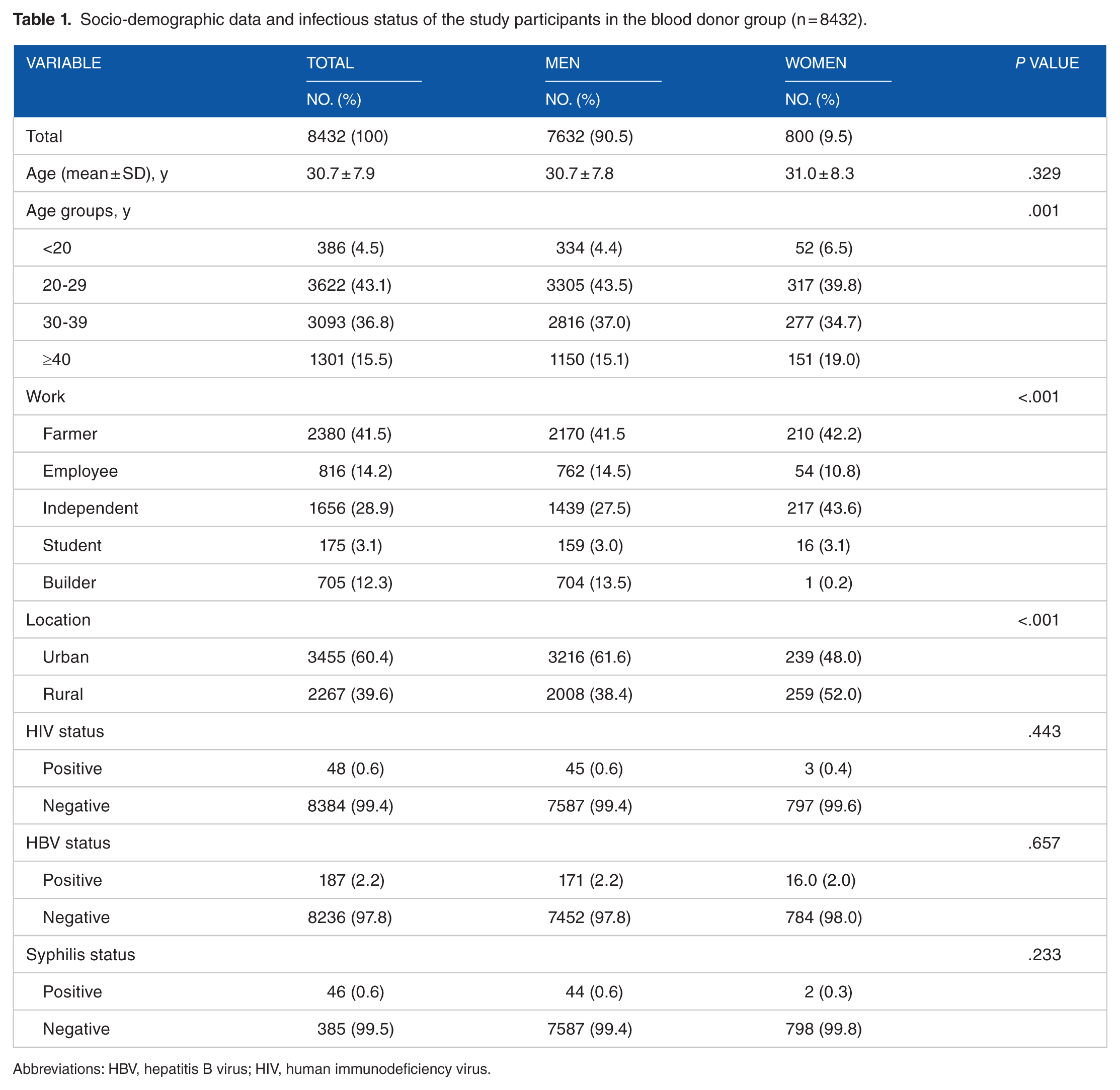
Abbreviations: HBV, hepatitis B virus; HIV, human immunodeficiency virus.
In the group of women screened for CC, the women were older than in the donor group, with a mean age of 43.4 ± 9.1 years. Similar to the donor population, 509 (55.4%) of these women lived in rural areas and 482 (58.1%) were farmers.
Prevalence of STIs
The prevalence of STIs according to socio-demographic factors is shown in Table 2. Of the 1020 women in the CC group, 401 (39.3%) were positive for hrHPV infection and 124 (12.6%) for lrHPV infection.
HIV, HBV, HPV, and syphilis infection status according to different variables.
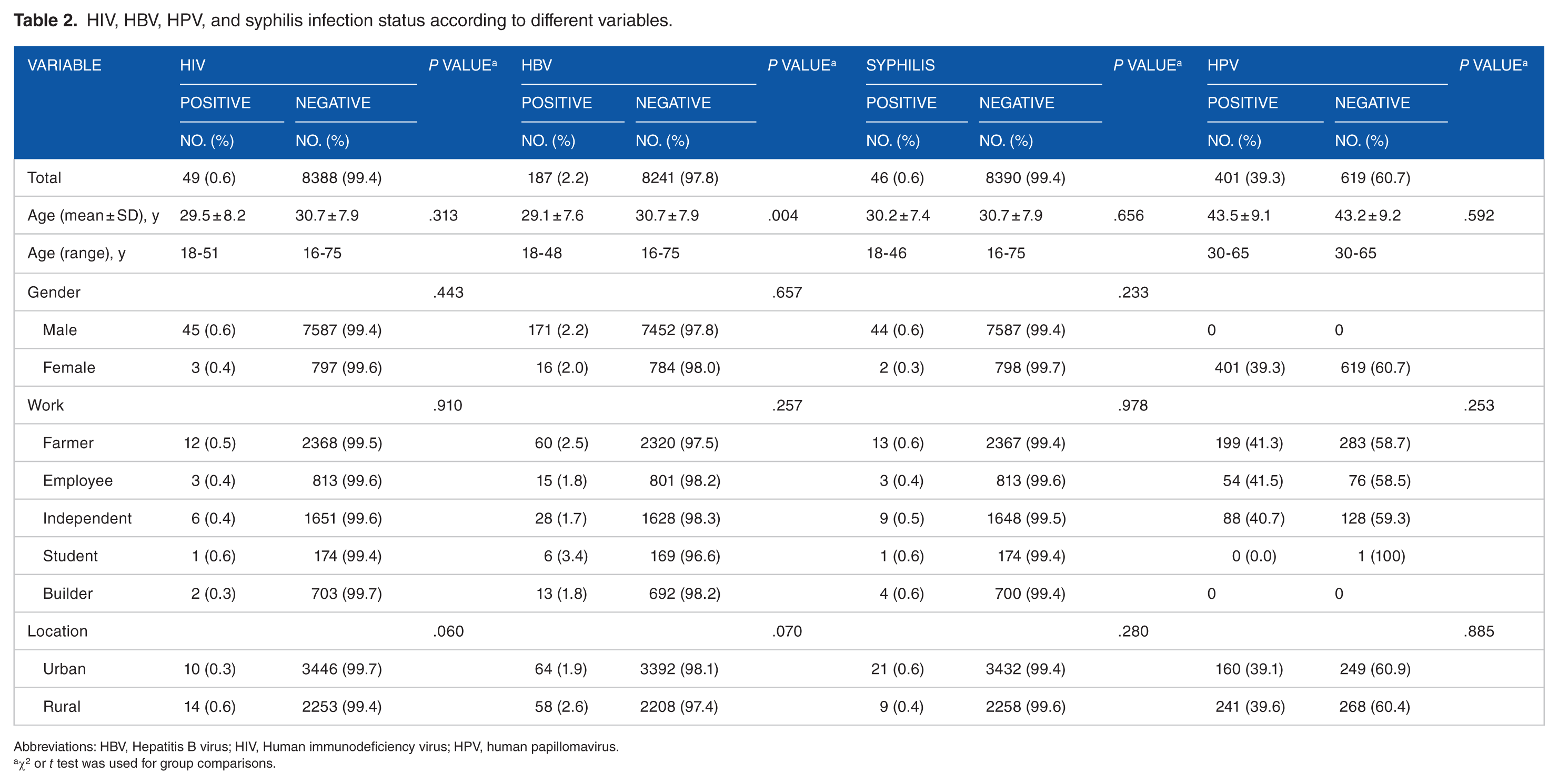
Abbreviations: HBV, Hepatitis B virus; HIV, Human immunodeficiency virus; HPV, human papillomavirus.
χ2 or t test was used for group comparisons.
The prevalence of HIV infection was 0.6% (45/7632) in men and 0.4% (3/797) in women. The mean age of the HIV-positive population was 29.5 ± 8.2 years (range: 18-51 years). Hepatitis B virus infection prevalence was 2.2% (171/7623) in men and 2.0% (16/800) in women. Hepatitis B virus–positive individuals were aged 18 to 48 years (mean age: 29.1 ± 7.6 years). Among men, 0.6% (44/7631) tested positive for syphilis, and 0.3% (2/800) of women tested positive. Syphilis-positive individuals were aged 18 to 46 years (mean age: 30.2 ± 7.4 years).
Figures 1 and 2 show the prevalence of STIs stratified by age for women and men, respectively. Hepatitis B virus infection was the most frequent STI in men, regardless of age, and tended to decrease with age. The prevalence of HPV infection was extremely high in women compared with the other STIs.
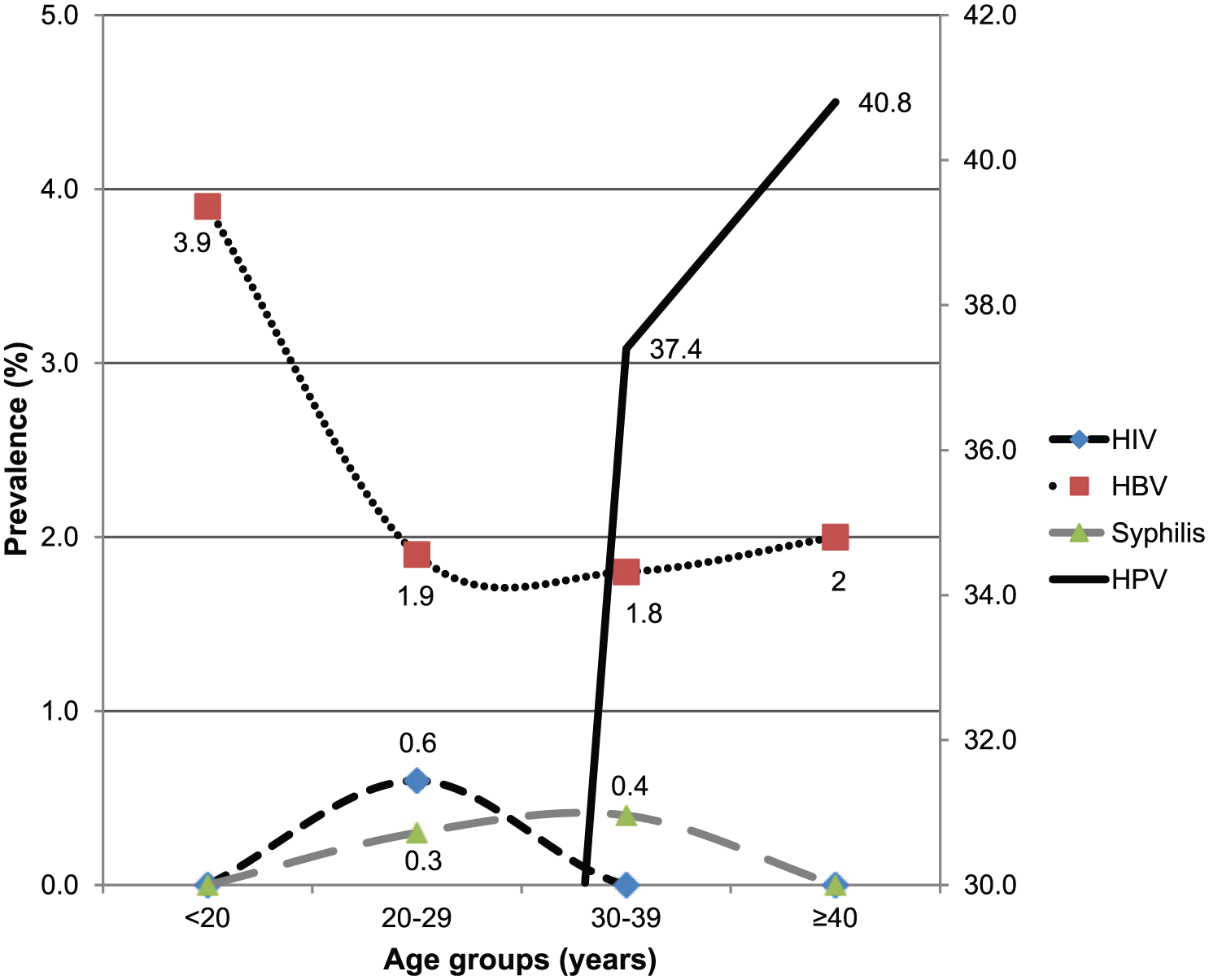
Prevalence of sexually transmitted infections among female participants stratified by age group. HBV indicates hepatitis B virus; HIV, human immunodeficiency virus; HPV, human papillomavirus.
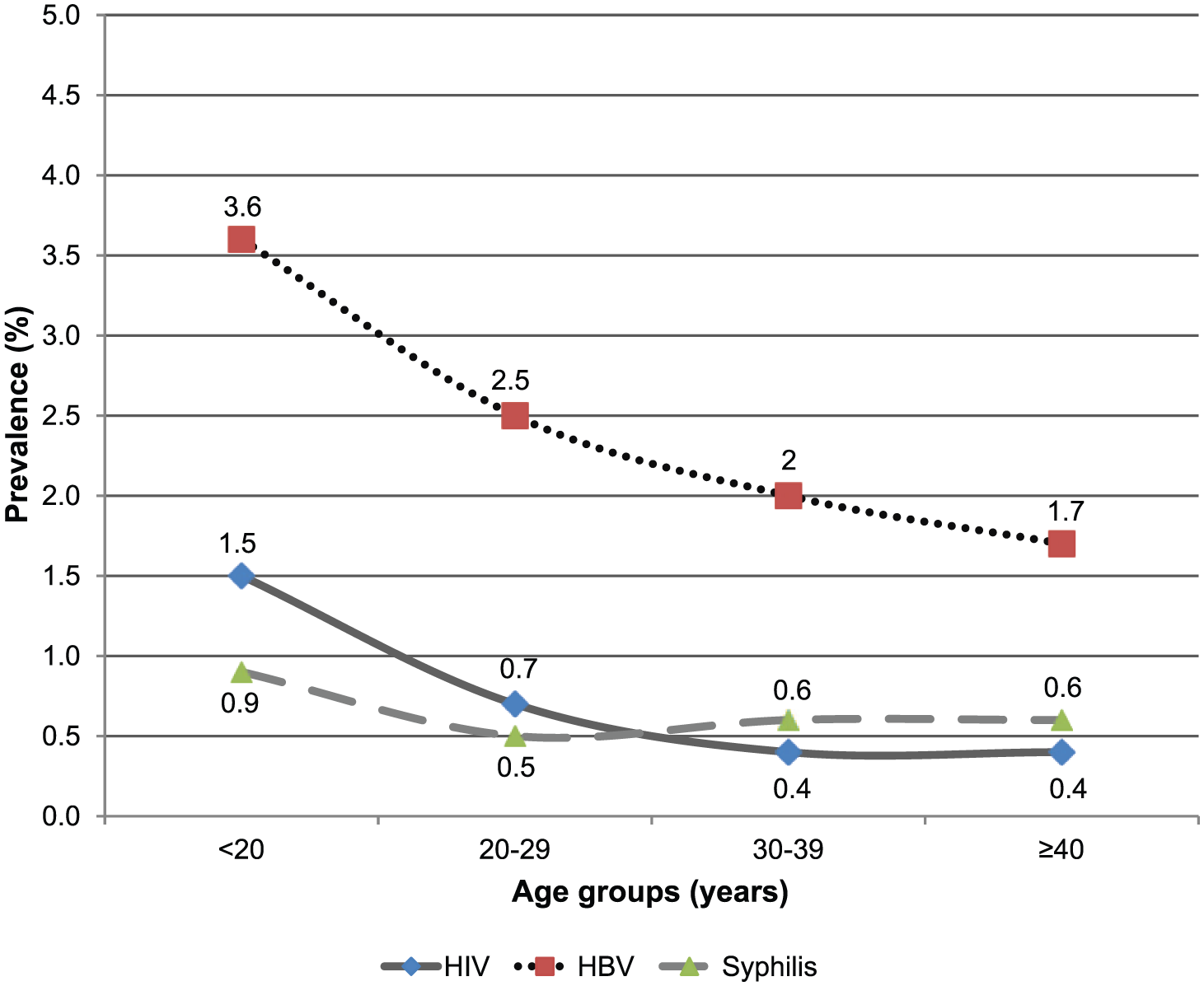
Prevalence of sexually transmitted infections among male participants stratified by age group. HBV indicates hepatitis B virus; HIV, human immunodeficiency virus.
Figure 3 reports the prevalence of hrHPV and lrHPV infections among the female participants stratified by age group. High-risk HPV types were generally more prevalent than lrHPV types in this population. There was also a direct link between increasing age and HPV prevalence for both hrHPV and lrHPV genotypes.
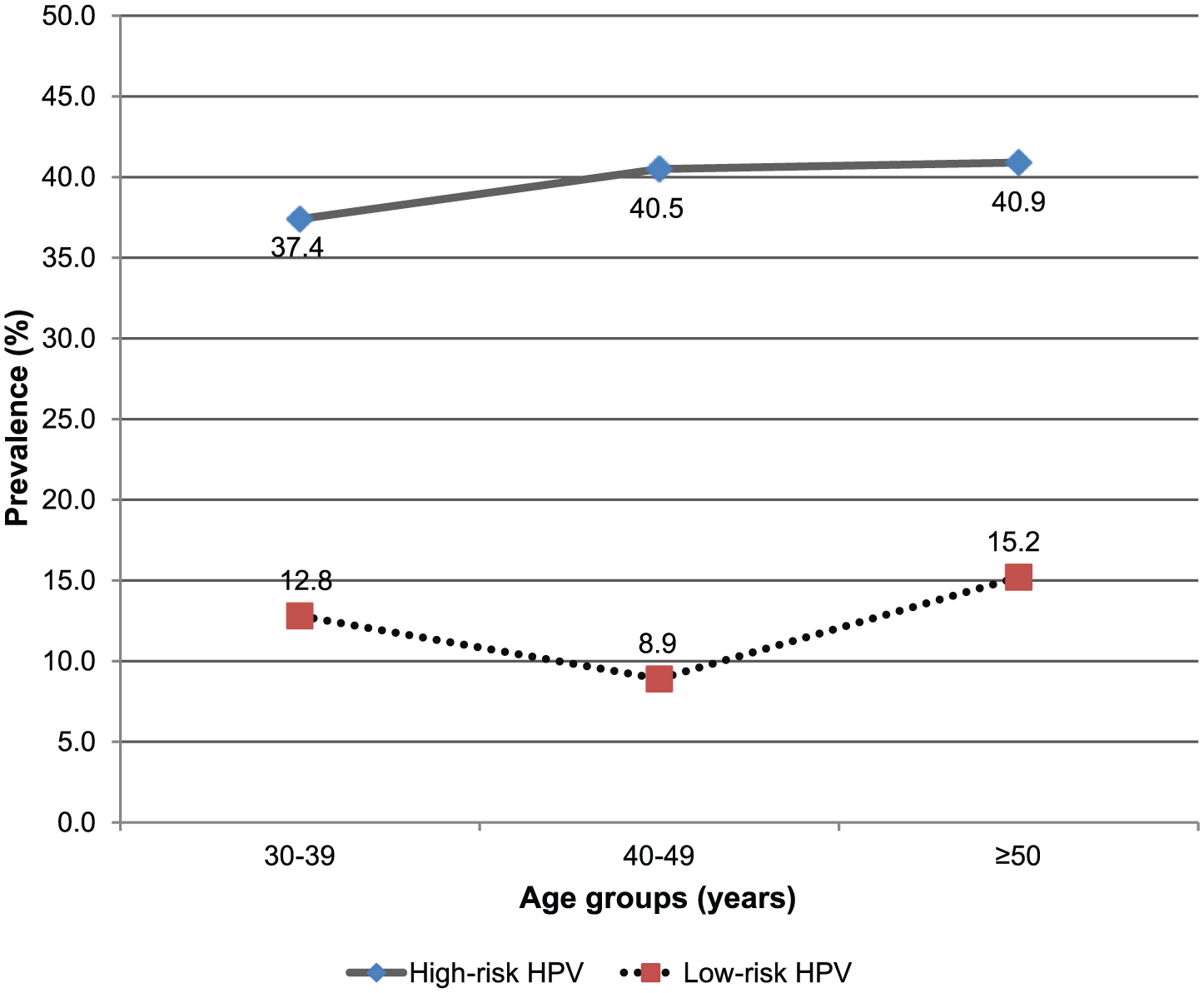
Prevalence of hrHPV and lrHPV infection among female participants stratified by age group. HPV indicates human papillomavirus; hrHPV, high-risk HPV; lrHPV, low-risk HPV.
Discussion
In contrast to the high prevalence of HPV infection (39.3%) detected, the prevalence of the other STIs was relatively low. The high rate of HPV infection among the Malagasy women screened is consistent with published meta-analyses and a systematic review of East Africa, which reported HPV rates of 33.6% and 42.2% in women with normal cytology.16,17
The prevalence of HPV infection in sub-Saharan African countries varies from 10.5% (Nigeria) to 47.9% (Guinea), with 39.0% in Cameroon. 18 Another study in Madagascar in 2010 reported an HPV rate of 36.7% in a population of female sex workers aged 18 to 58 years in Antananarivo. 2 Although that study population differed from ours, the estimated prevalence of HPV infection was similar to our finding but lower than that in other African countries (among female sex workers, the prevalence of HPV infection was 62.6% in South Africa and 43.0% in Senegal). 2 We also observed a higher prevalence of hrHPV than lrHPV types in our study population. This may be partly explained by the fact that the Anyplex II HPV28 test detects a greater number of hrHPV than lrHPV genotypes (19 and 9, respectively).
The prevalence of HIV infection in Madagascar seems to be lower than that observed in other East African countries. According to the Joint United Nations Programme on HIV/AIDS (UNAIDS) global report of 2010, the prevalence of HIV infection in this region ranged from 5.6% in the United Republic of Tanzania to 25.9% in Swaziland. 18 In Cameroon, where the prevalence of HPV infection is extremely close to that found in this study, the self-reported prevalence of HIV infection was 9.0% in a population of women aged 30 to 65 years screened for HPV infection and CC. 19 In 2014, the National AIDS Committee of Madagascar reported an HIV infection prevalence of 0.5% in the general population, 20 but a higher prevalence in high-risk populations, including sex workers (1.3%), intravenous drug users (7.1%), and men who have sex with men (14.7%), among whom 99.3% of new infections arose. Therefore, the AIDS epidemic currently seems to be concentrated in some subgroups of the Malagasy population. Wang et al 21 reported 2000 new cases of HIV infection in Madagascar in 2015, 42 510 people living with HIV, 4420 HIV/AIDS-related deaths, and antiretroviral therapy coverage of 1.35% in the infected population.
Despite the low prevalence of HIV infection, the risk factors for STIs, including poverty, sex work, and difficulty in accessing the health system, are still major issues in Madagascar. The prevalence of other STIs is also relatively high in the country. According to The New York Times, the prevalence of STIs among sex workers in Antananarivo (capital of Madagascar) was 77.5% in 2004. 22 In 2005, a study conducted in rural Madagascar showed that, in this setting, 37.5% of women and 26.8% of men were infected with a curable STI. 23 The prevalence of syphilis in Madagascar in 2008 was 5.6% (15% in 1995), whereas in other sub-Saharan African countries, such as Botswana, it was only 0.95%. 1
In 2001, Behets et al 24 examined the epidemiologic factors for STIs in Madagascar in women seeking primary care for vaginal discharge and reported a 4% prevalence of syphilis. The discrepancy with our finding (0.3% in women) is attributable to at least 2 factors: the women in the study by Behets et al came exclusively from an urban area (Antananarivo city), and the women in our study were not necessarily attending the clinic for genital discharge. The prevalence of syphilis was investigated in various African countries in 1990 with RPR testing and was 0.5% in Zimbabwe, 8.2% in Mozambique, 10.0% in Swaziland, and 17.6% in Malawi. 25 In contrast, the prevalence of syphilis in the Ambanja region remains low, which we assume to be the consequence of the effective prevention and screening programs implemented in the country.
In 1996, Boisier et al 26 used HBsAg testing to estimate an HBV infection prevalence of 20.5% in the general Malagasy population. Similar to our findings, this prevalence was independently higher in men and in the rural population. The mean HBV infection prevalence of 2.2% in our study population and the well-known routes of HBV transmission (vertical, early-life horizontal, and adult horizontal) 27 suggest that medico-surgical advances and prevention programs have reduced this disease in Madagascar in the past 20 years.
The presence of an STI is itself a risk factor for contracting another STI. This is probably attributable to both the impairment of the immune response by STIs, such as HIV infection, and the presence of risk factors that are common to many STIs. In Zimbabwe, Smith-McCune et al found that women with an HPV infection were at higher risk of HIV infection. Moreover, the HPV-induced inflammatory reaction in the cervix attracts HIV target cells, such as lymphocytes and macrophages, thus facilitating viral entry into the host. 28 According to Catarino et al, 19 the independent risk factors for HPV infection in Cameroon include being a housewife, young, single, using hormonal contraception, and HIV coinfection. Both HPV and HIV infections share the same transmission routes and behavioral risk factors. Therefore, our findings on the prevalence of HPV infection in Madagascar should imply a higher prevalence of HIV infection on the island.
Genital ulcer is another risk factor for contracting HIV infection. In Kenya, Greenblatt et al 29 observed a 16.5% rate of HIV infection in men presenting with genital ulcer. Galvin et al 30 also observed that contracting HIV after sexual intercourse with an HIV-positive person is rare unless a genital ulcer is present. Our findings suggest that if there is a correlation between the prevalence syphilis and HIV infection in Madagascar, the prevalence of syphilis is too small to be a significant risk factor for HIV infection. Nevertheless, given the evidence-based correlation between HPV infection and HIV acquisition, it is unusual that the HIV infection prevalence in Madagascar remains below 1% despite an HPV infection prevalence of 39.3%.
The insular position of Madagascar, its low level of migration and its efficient prevention programs seem to constitute protective factors against STIs. 20 Moreover, circumcision is widely practiced on the island and is known to protect men from syphilis.20,31 All these elements favor low rates of STIs, although there are many risk factors for STIs and at least some are present and increasing in Madagascar. These factors include sex work, migration from rural to urban centers, blood rituals involved in some local customs, and multiple sexual partners, which may increase the prevalence of some STIs more than others.20,32 A study conducted in Toamasina Province among 15- to 24-year olds reported that among sexually active individuals, only 4 in 10 men and 2 in 10 women had ever used a condom, and that less than 15% had used one during their last episode of sexual intercourse. 33
A particular strength of this study is that it provides recent information about 4 STIs in Madagascar based on a relatively large population sample. These data should be useful in improving the efficiency of programs that focus on the prevention, screening, and treatment of STIs in this country.
Our study had some limitations. Because it was a retrospective study, only a limited amount of socio-demographic data were available for the blood donor sample. Moreover, we analyzed data from 2 different populations, although we do not believe this affected our epidemiologic analysis. Although these 2 populations differed in their age and sex distributions, all the participants were from the Ambanja region and the aim of this study was to establish the prevalence of HPV infection and other STIs in this area. Thereafter, the most important bias of this study is certainly the fact that the recruited participants were volunteers in the 2 populations. In effect, people who know they are infected by an STI will probably not go to screening, especially for blood-giving. However, as shown above, our results are consistent with prevalence found in the literature. Moreover, in view of the difficulties in finding reliable data on developing countries, this alternative seemed to us a good idea to assess the situation in this setting. Other potential biases are the limited geographical area where the study was conducted and the limitation in the access of the health system in this setting due to the lack of socio-economic means.
In conclusion, the prevalence of STIs in the Malagasy population is paradoxical insofar as it is difficult to understand how such a high rate of HPV infection can coexist with a low and apparently stable rate of HIV infection. Our results suggest that the prevalence of STIs results not simply from a single cause-effect association but rather from a complex network of environmental, genetic, behavioral, physiopathological, and migratory factors. However, the HPV status in Madagascar is alarming, so efforts to establish solid CC screening programs in this context must continue. Currently, the screening and prevention programs for the STIs seen in this study are ongoing on the field. Next steps in the population-based assessment are to reinforce ongoing efforts, continue them, and involve new projects. Among these, it seem important to us to mention the screening of other areas and population in Madagascar (specifically, the cities and the population with several risk factors), vaccination campaign, routine serologic control of blood donations, reduction in the number of sexual partners, increase in the use of condoms, and education of the young Malagasy population about STIs.
Although HPV infection, syphilis, and HBV infection do not seem to influence the prevalence of HIV infection in Madagascar, we consider it important to note the potential involvement of these STIs, particularly HPV infection and syphilis, in a hypothetical future increase in the HIV infection epidemic on the island. Therefore, further investigations are required to clarify the situation, by studying a broad spectrum of sexually transmitted coinfections in HPV-positive and HPV-negative Malagasy women and their influence on the prevalence and persistence of HPV infection. Assessing the correlations between HPV infection and other STIs will provide new insight into the natural history of HPV infections and the development of CC. Although there are not yet any data on the burden of HIV infection and other STIs in Madagascar, information on their prevalence is important for a general evaluation of the reproductive health and health promotion among the population.
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Action Madagascar Foundation and the University Hospitals of Geneva, Switzerland. The funding bodies had no role in the study design, data collection or analysis, decision to publish, or preparation of the manuscript.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Disclosures and Ethics
This study was approved by the Cantonal Human Research Ethics Commission of Geneva (CCER, CER: 14-071) and the Malgasch National Commission for the Ethics of Science and Technology (no: 94 MSANP/SG/DGS/DLMNT/SLMV).
