Abstract
Background:
Breast cancer is the most common malignancy among Saudi women, and early detection remains a critical factor for improving survival outcomes. Despite ongoing awareness initiatives, screening uptake remains low, suggesting that perceptions and beliefs may influence women’s engagement in preventive behaviors.
Objectives:
To assess perceptions of breast cancer among women attending Johns Hopkins Aramco Healthcare (JHAH) facilities using the Breast Cancer Perception Scale (BPS) and to examine associations between perception domains and sociodemographic as well as screening-related factors.
Design:
A cross-sectional, questionnaire-based study was conducted between October 2024 and March 2025.
Methods:
Eligible female patients aged 20 years or older with active MyChart accounts were invited to participate electronically. Perception was measured using the validated 24-item BPS, which comprises 6 subscales. Due to non-normal data distribution, non-parametric tests (Kruskal-Wallis and Mann-Whitney U) were employed, with a Bonferroni correction for multiple comparisons.
Results:
Participants had a mean age of 37.5 ± 8.3 years, and 61.4% held a university degree. Postgraduate education was significantly associated with higher scores for Perceived Knowledge, Treatment Belief, Health Check, and Risk, as well as lower stigma (P < .001). Employed women demonstrated greater Perceived Knowledge (P < .001). Those with a family history of breast cancer reported higher Fear and Risk perceptions (P < .001). Prior screening experience (clinical breast examination or Mammography) correlated with higher Knowledge and Health Check perceptions and lower stigma (P < .001). Overall, 51.7% of participants reported adequate knowledge, while 64% to 70% expressed moderate to high levels of fear.
Conclusion:
Perceptions of breast cancer among Saudi women are shaped by educational level, employment status, family history, and screening experience. Targeted educational interventions that address knowledge gaps and cultural stigmas are essential for enhancing participation in screening and early detection practices.
Introduction
Breast cancer is the most common malignancy and remains the leading cause of cancer-related deaths among women worldwide. Its risk increases with advancing age, genetic susceptibility, radiation exposure, reproductive factors, and lifestyle behaviors such as physical inactivity and unhealthy diet.1 -3 In Saudi Arabia, breast cancer accounted for 29.7% of all cancer cases and 8.5% of cancer-related deaths among women in 2018, making it the most prevalent cancer in the country.4,5 A recent analysis of data from the Global Burden of Disease (GBD) database reported an age-standardized incidence rate of 46.0 per 100,000 (95% confidence interval [CI] = 34.5-61.5) in 2021, projected to increase to 49.6 per 100 000 (95% CI = 46.8-52.3) by 2026, indicating a rising national and global burden. 6
Early detection significantly improves prognosis, as delays in diagnosis and treatment are associated with more advanced disease and lower survival rates. 7 Despite national awareness campaigns and screening initiatives, participation in breast cancer screening remains low in Saudi Arabia, with only 8% of women undergoing screening in 2015. 8 This gap suggests that factors beyond knowledge may influence women’s engagement in preventive behaviors.
According to the Health Belief Model, beliefs, values, and attitudes can significantly influence people’s health-related behaviors. 9 The model suggests that some factors can influence whether or not a person makes behavioral changes when faced with a potential risk of developing a condition: their perception of the severity of the condition, their susceptibility to the condition, the benefits that a behavior change will have on prevention of the condition, and the perceived difficulties in implementing the recommended changes in behavior. 10
Recent evidence indicates that women’s perceptions of risk, benefits, and barriers significantly shape their willingness to participate in screening and prevention. Rainey et al 11 found that women’s adoption of risk-based breast cancer screening depends mainly on their perceived susceptibility, perceived severity, and perceived benefits vs barriers to action.
Accordingly, this study aims to assess the level of breast cancer perception among women attending Johns Hopkins Aramco Healthcare (JHAH) facilities in Saudi Arabia using the Breast Cancer Perception Scale (BPS) and to identify the demographic and clinical factors associated with these perceptions. Understanding these perceptions may inform targeted strategies to enhance screening participation, guide culturally sensitive health promotion initiatives, and support early detection programs.
Methods
Study design and setting
This cross-sectional study was conducted at 5 JHAH facilities between October 2024 and March 2025. The target population consisted of adult women residing primarily in the Eastern Province of Saudi Arabia, including Dhahran, Al-Hasa, Ras Tanura, Abqaiq, and Udhailiyah. The reporting of this study conforms to the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) statement 12 (Supplementary File 1).
Participants and recruitment
Eligible participants were female patients aged 20 years or older with active MyChart mobile application accounts. MyChart is a secure online portal and mobile application that enables patients to access their electronic health records, schedule appointments, and communicate directly with their healthcare providers. The study population primarily comprised Saudi nationals; however, a subset of participants represented other nationalities, reflecting the multinational composition of Saudi Aramco employees and their dependents served by JHAH. Women with a current or previous diagnosis of any cancer and those attending medically designated oncology or specialty facilities were excluded to minimize potential bias associated with personal cancer experience.
A convenience sampling approach was employed by electronically distributing the survey to all eligible women through MyChart using a coded algorithm developed by the Health Informatics team, based on the inclusion and exclusion criteria. A total of 2401 responses were received, representing 37.6% of the eligible population identified through the application.
Data collection tool
A self-administered electronic questionnaire was used, consisting of 2 sections. The questionnaire was available in both Arabic and English to accommodate the linguistic diversity of the JHAH population, which includes Arabic-speaking and non-Arab expatriate patients.
The first section collected demographic and clinical information, including age, nationality, residence, marital and occupational status, education level, family history of breast cancer, and screening practices (breast self-examination, clinical breast examination (CBE), and Mammography for women aged 40 years and above).
The second section employed the BPS, a validated instrument developed by Taylan et al 9 to assess perceptions related to breast cancer based on the Health Belief Model (Supplementary File 2). The original developers evaluated the BPS construct validity using exploratory and confirmatory factor analyses (EFA and CFA), with model fit indices meeting acceptable standards (χ2/df ⩽ 5.0, root mean square error of approximation [RMSEA] ⩽ 0.08, goodness-of-fit index [GFI] ⩾ 0.90, and comparative fit index [CFI] and incremental fit index [IFI] > 0.90). To ensure cultural and linguistic appropriateness, the Arabic version of the BPS was validated through a multi-step process. The questionnaire was first translated into Arabic and then reviewed by a panel of experts in public health to assess the accuracy and clarity of the translation. Based on their feedback, modifications were made, followed by back-translation into English to confirm consistency with the original instrument. A pilot study was then conducted among 20 participants; their data were excluded from the final analysis. In the present study, the internal consistency of the BPS was assessed using Cronbach’s alpha (α = 0.81).
The BPS comprises 24 items across 6 subscales, each rated on a 5-point Likert scale, ranging from “Strongly Disagree” (1) to “Strongly Agree” (5). Items 9–13 are reverse-coded. Higher subscale scores indicate greater perception within each domain. The subscales are: Perceived Knowledge (Items 1–4), Perceived Treatment Belief (5-8), Perceived Need for Health Check (9-13, reverse-coded), Perceived Stigma,13 -16 Perceived Fear,17 -20 and Perceived Risk.21 -23
Statistical analysis
Data were analyzed using R (version 4.4.1). The sample (n = 2401) included categorical predictors: education, occupation, family history of breast cancer, CBE, and Mammography. The outcome variables were the 6 breast cancer perception subscales: Perceived Knowledge, Perceived Treatment Belief, Perceived Need for Health Check, Perceived Stigma, Perceived Fear, and Perceived Risk.
Due to non-normality (Shapiro-Wilk test, P < .0001), non-parametric tests were used. Kruskal-Wallis tests assessed differences in subscale scores by education and occupation, while Mann-Whitney U tests evaluated differences by binary predictors (family history of breast cancer, CBE, and Mammography). Cohen’s d was calculated as the effect size. Bonferroni correction was applied for multiple comparisons. Multivariate effects were assessed using multivariate analysis of variance (MANOVA) with Wilks’ Lambda. A significance level of α = 0.05 was used for all analyses.
Results
Demographic characteristics
Of the 6383 eligible women invited via MyChart, 2401 completed the survey, yielding a 37.6% response rate (Figure 1). The sample (mean age 37.51 ± 8.34 years) was primarily university-educated (61.4%, n = 1474), employed (50.0%, n = 1201), and without a family history of breast cancer (74.1%, n = 1778). More than half had never undergone a CBE (53.8%, n = 1292) or Mammography (61.2%, n = 1470) (Table 1). Among participants with a family history of breast cancer, 54.0% had undergone CBE and 43.6% had undergone Mammography, compared with 45.7% and 36.5%, respectively, among those without a family history.

STROBE flowchart of participant recruitment and inclusion.
Sample characteristics (n = 2401).

Breast Cancer Perception Scale
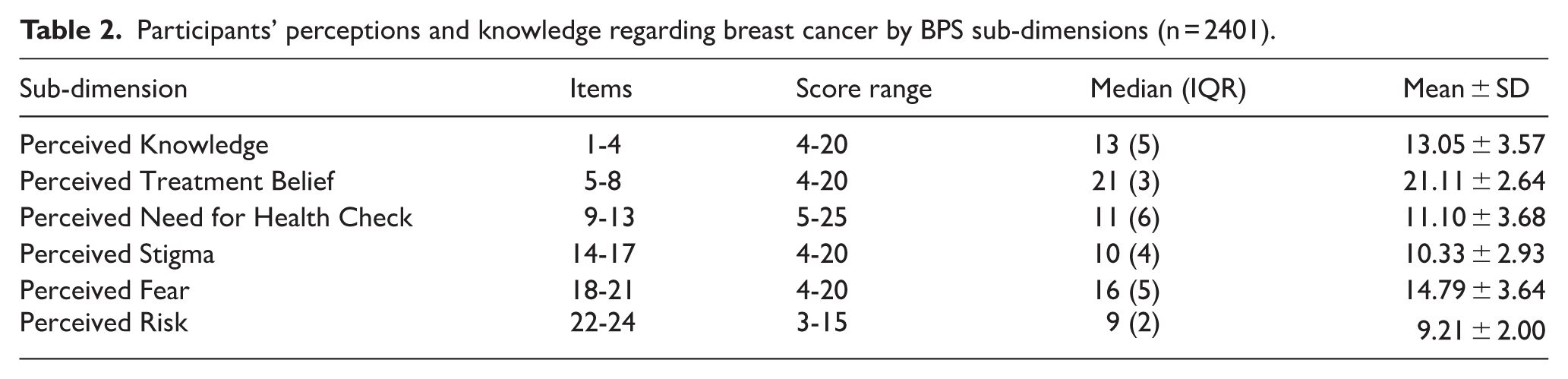
Participants’ perceptions of breast cancer showed moderate Perceived Knowledge (median 13 [interquartile range, IQR 5], mean 13.05 ± 3.57, range 4-20), with 51.73% agreeing their knowledge is adequate, indicating gaps in understanding, while a strong Perceived Treatment Belief (median 17 [IQR 3], mean 21.11 ± 2.64, range 4-20) reflected confidence, as 93.17% to 95.29% acknowledged early detection’s role in recovery and 52.94% believed breast cancer is treatable. In contrast, the Perceived Need for Health Checks was low (median 11 [IQR 6], mean 11.10 ± 3.68, range 5-25), with 32.90% not visiting doctors unless symptomatic, potentially hindering early detection, despite 91.09% recognizing the importance of breast self-examination. Emotional responses were significant, with high Perceived Fear (median 16 [IQR 5], mean 14.79 ± 3.64, range = 4-20), as 64% to 70% reported anxiety, and notable Perceived Stigma (median 10 [IQR 4], mean 10.33 ± 2.93, range = 4-20), as 62.26% were reluctant to see male doctors. Similarly, moderate Perceived Risk (median 9 [IQR 2], mean 9.21 ± 2.00, range = 3-15) was evident, with 52.56% noting family history’s role, alongside concerns about quality of life (59.48% for sexual health, 31.07% for caregiving, 45.02% for marital issues) and body image (32.86% believing treatment affects beauty), underscoring stigma’s impact (Table 2).
Participants’ perceptions and knowledge regarding breast cancer by BPS sub-dimensions (n = 2401).
Differences by education and occupation
Education showed differences in Perceived Knowledge, Treatment, Health Check, Stigma, and Risk (P < .001, ε2 = 0.005–0.017), but not in Fear (P = .381) (Table 3). Post hoc tests revealed higher knowledge and health checks for postgraduates compared with those with a bachelor’s degree or below (P ⩽ .022). Occupation differences were significant for Knowledge, Treatment, Health Check, Stigma, and Risk (P ⩽ .002, ε2 = 0.005–0.018), with Employed and Housewife scoring higher than Not Employed on Health Check (P ⩽ .008) and Employed lower than Housewife on Stigma (P = .001) (Table 3 and Figure 2).
Statistical results for education and occupation on breast cancer perception subscales.

Note: Adjusted P-values use Bonferroni correction.
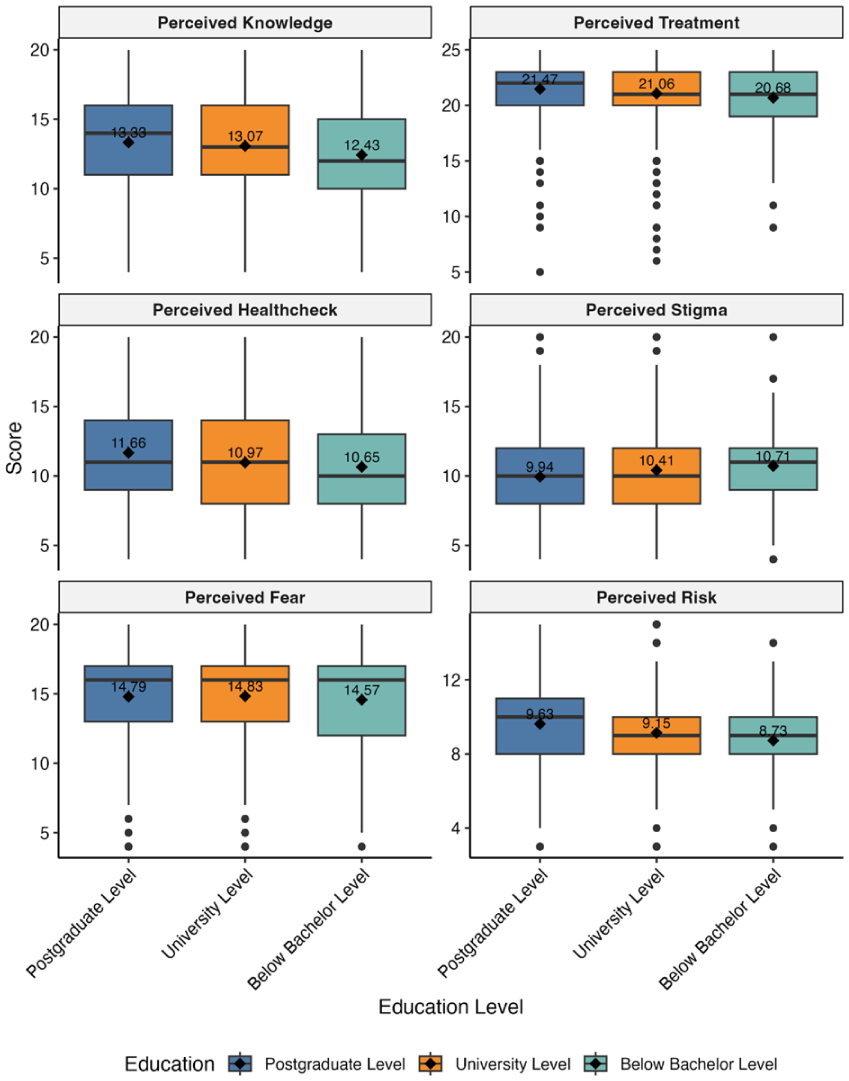
Distribution of breast cancer perception subscales by education level (n = 2401)
Binary predictors and multivariate effects
There were differences by Family History for Knowledge, Treatment, Health Check, Fear, and Risk (P ⩽ .047, d = 0.085-0.810), but not Stigma (P = .088). Clinical Breast Examination and Mammography showed differences for Knowledge, Treatment, Health Check, Stigma, and Risk (P ⩽ .004, d = 0.127-0.851), but not Fear (P ⩾ .136); MANOVA confirmed multivariate effects for all predictors (P < .001, Wilks’ Lambda = 0.836-0.970) (Table 4).
Statistical results for binary predictors and MANOVA on breast cancer perception subscales.

Note: Mann-Whitney U tests were used due to non-normality (Shapiro-Wilk, P < .0001). Adjusted P-values use Bonferroni correction. MANOVA results use Wilks’ Lambda.
Subscale correlations
Correlations between subscales showed moderate positive relationships between Perceived Knowledge and Health Check (r = .335, P < .001), and Perceived Stigma and Fear (r = .346, P < .001), indicating that higher knowledge is associated with better health check perceptions, and higher stigma is linked to greater fear. Moderate negative correlations were found between Perceived Health Check and stigma (r = −.310, P < .001), and Perceived Health Check and Fear (r = −.224, P < .001), suggesting that stigma and fear reduce health check engagement. Weak correlations included Perceived Knowledge and Fear (r = −.183, P < .001), Perceived Stigma and Treatment (r = −.203, P < .001), and Perceived Risk with other subscales (r ⩽ .|135,| ns for Knowledge, Treatment, Health Check), indicating limited relationships (Figure 3).

Correlation heatmap of breast cancer perception subscales (n = 2401).
Discussion
This study provides comprehensive insights into women’s perceptions of breast cancer across multiple psychosocial domains in Saudi Arabia. The findings reveal considerable variations in awareness, emotional response, and screening behavior that collectively influence early detection efforts. Despite widespread recognition of breast cancer’s severity and the importance of early diagnosis, notable perceptual and behavioral gaps persist.
In the present study, approximately half of the participants (48.3%) perceived their awareness of breast cancer as inadequate. This finding is comparable to results from different studies conducted across various regions of Saudi Arabia that assessed knowledge and awareness of breast cancer. For instance, 46.4% of female students at Hail University and 67% of school teachers in Makkah demonstrated poor knowledge of breast cancer.13,14 Similarly, among patients at Najran Hospital, only 54.4% exhibited adequate knowledge of the disease. 15 All these studies also reported low engagement in breast cancer screening practices. Collectively, these findings across different Saudi regions highlight a consistent pattern of limited knowledge and inadequate participation in breast cancer screening behaviors.
Although most respondents (over 93%) acknowledged the benefits of early detection, only 46.2% had ever undergone a CBE, and 38.8% had undergone Mammography. This discrepancy between knowledge and practice aligns with findings from a previous study, which identified psychosocial discomfort, stigma, and time constraints, rather than lack of awareness, as key barriers that hinder women’s participation in breast cancer screening in Saudi Arabia. 16 Participants with a prior screening history demonstrated greater perceived knowledge and health check and reported lower stigma toward breast cancer. This association may reflect a bidirectional relationship: exposure to screening could enhance knowledge and reduce stigma, while women with higher knowledge and less stigma may be more motivated to participate in screening.
Education and occupation also emerged as important determinants of perception. Women with postgraduate education exhibited higher levels of knowledge and treatment belief and lower stigma scores, contradicting previous claims of no association between education and knowledge. 17 Similarly, employed women showed greater perceived knowledge and lower stigma than housewives, likely reflecting higher health exposure and greater autonomy in seeking care, consistent with previous literature linking education and employment to health literacy and screening adherence.18,19
Family history of breast cancer was reported by 25.9% of participants, which is higher than the 18.4% observed in a Turkish study. 20 Having a family history was associated with heightened fear and perceived risk of developing breast cancer. Women with a family history were also more likely to participate in screening, with 54.0% having undergone CBE and 43.6% Mammography, compared with 45.7% and 36.5%, respectively, among those without a family history. These findings suggest that familial exposure may increase perceived susceptibility and promote screening behavior; however, the overall screening rate among high-risk women remains suboptimal, underscoring the need for targeted counseling and education to translate perceived risk into consistent preventive action.
Fear was widespread, with 64% to 70% reporting anxiety about breast cancer or treatment, and 62.26% were hesitant to see male doctors, a key cultural barrier in Saudi Arabia. Stigma, more pronounced among the less educated, delays help-seeking, with studies noting a 5.7-fold increase in delays.17,21,22 Some research has indicated that women exhibiting a greater degree of risk aversion tend to abstain from participating in breast cancer screening to evade the risk of receiving a diagnosis of breast cancer, which elicits anxiety or psychological distress.23 -25
Body image concerns were also noticeable, with participants believing that breast cancer treatment adversely affects a woman’s beauty. Moreover, participants expressed apprehensions regarding the effects of breast cancer on the quality of life, encompassing sexual health, caregiving, and marital matters. These findings align with the study conducted by Abdel-Aziz et al, 16 who recorded how stigma associated with breast cancer in Middle Eastern societies frequently pertains to apprehensions regarding marriageability and feminine identity. These worries highlight the significance of comprehensive psychosocial aid in breast cancer awareness and management programs. The reluctance to undergo examination by male physicians (62.26% agreed or strongly agreed) signifies a significant cultural obstacle unique to the Saudi context. Health care facilities may anticipate enhancing the accessibility of female practitioners to mitigate this obstacle.
This study has several limitations. The cross-sectional design restricts causal interpretation. The convenience sampling method and a response rate of 37.6% may have introduced selection bias favoring participants with higher health literacy and digital access, as recruitment relied on the MyChart platform. Consequently, this can reduce the generalizability of the findings. In addition, the use of self-reported data may be prone to recall bias. Future research employing probabilistic sampling and qualitative interviews could enrich understanding of the complex interplay between cultural norms, emotional responses, and screening behaviors.
Despite these limitations, the study possesses notable strengths. It includes a large, diverse sample (n = 2401) from multiple JHAH sites, employs a validated instrument adapted into Arabic through expert review and pilot testing, and comprehensively explores 6 distinct perception domains. By distinguishing between cultural and psychological influences and access-related factors, this study makes a significant contribution to the evidence base guiding the development of tailored interventions to promote early detection among Saudi women.
Conclusion
Postgraduate education and screening history were linked to higher Knowledge, Treatment, Health Check, and lower Stigma, while Family History increased Fear and Risk. High fear and cultural barriers (eg, male doctor reluctance) underscore the need for targeted education, stigma reduction, and access to female practitioners to improve screening uptake in Saudi Arabia.
Supplemental Material
sj-docx-1-bcb-10.1177_11782234251410402 – Supplemental material for Perceptions of Breast Cancer: A Cross-Sectional Study Using the Breast Cancer Perception Scale (BPS)
Supplemental material, sj-docx-1-bcb-10.1177_11782234251410402 for Perceptions of Breast Cancer: A Cross-Sectional Study Using the Breast Cancer Perception Scale (BPS) by Omer Kheir, Nada Baatiah, Anwar Alotaibi, Sheikha Dossary, Mohammad Dhalaan, Hayat AlMushcab, Mariam Al Romaihi, Maryam Al Darweesh, Rasiel Kabli and Mohammad Ghamdi in Breast Cancer: Basic and Clinical Research
Supplemental Material
sj-docx-2-bcb-10.1177_11782234251410402 – Supplemental material for Perceptions of Breast Cancer: A Cross-Sectional Study Using the Breast Cancer Perception Scale (BPS)
Supplemental material, sj-docx-2-bcb-10.1177_11782234251410402 for Perceptions of Breast Cancer: A Cross-Sectional Study Using the Breast Cancer Perception Scale (BPS) by Omer Kheir, Nada Baatiah, Anwar Alotaibi, Sheikha Dossary, Mohammad Dhalaan, Hayat AlMushcab, Mariam Al Romaihi, Maryam Al Darweesh, Rasiel Kabli and Mohammad Ghamdi in Breast Cancer: Basic and Clinical Research
Footnotes
Acknowledgements
The authors would like to express their gratitude to the JHAH staff, especially Dr Nafeesa Faris, Dr Mohammed Al Mohammed, Dr Ammar Sattar, and Dr Hanady Daher, for their assistance.
Ethical considerations
Ethical approval was obtained from the Institutional Review Board of JHAH (IRB #24-23) in accordance with the Declaration of Helsinki. No identifiable information was collected for the participants. Data were securely stored in a password-protected Excel file, accessible only to the study investigators.
Consent to participate
All participants received information about the study objectives and provided electronic informed consent through the MyChart application before participation.
Author contributions
O.K.: Conceptualization; Methodology; Project administration; Supervision; Writing—original draft.
N.B.: Formal analysis; Writing—original draft; Writing—review & editing.
A.A.: Formal analysis; Project administration; Visualization; Writing—original draft.
M.G.: Writing—original draft.
S.D.: Writing—review & editing.
M.D.: Writing—review & editing.
H.A.M.: Writing—review & editing.
M.A.R.: Data curation; Validation.
M.A.D.: Data curation; Validation.
R.K.: Data curation; Validation.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting this research’s findings can be obtained from JHAH. Restrictions exist concerning access to these data, which were utilized under license for this research. The data can be accessed from the corresponding author upon a reasonable request with JHAH’s authorization.
Use of artificial intelligence-assisted tools
The authors used ChatGPT (OpenAI, GPT-5 model) to assist in improving the language, grammar, and clarity of the manuscript. The tool was not used to generate, analyze, or modify any scientific data, and all interpretations, conclusions, and analyses are the authors’ own.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
