Abstract
Juvenile fibroadenoma typically is seen in the adolescent patient and has distinctive clinical and histopathological features that are related to the early onset of the benign tumor. Only rarely can juvenile fibroadenoma occur as a prepubertal lesion or may be detected earlier in childhood, raising questions about differential diagnosis and management of the lesion. We present a case of very early first manifestation of juvenile fibroadenoma in a 2-year-old patient. Under clinical observation and conservative management over a 7-year period, there was no progression. At the age of 9 years, rapid growth of the lesion occurred causing clinical symptoms. Complete surgical excision resulted in a good clinical outcome. Histologically, the diagnosis of juvenile fibroadenoma was made. In summary, juvenile fibroadenoma is the most common breast neoplasia in adolescents and may cause excessive unilateral growth resulting in gross asymmetry and pain. However, it can be detectable in early childhood and after a dormant period of several years, as in this case, lead to sudden massive growth at the onset of puberty. The clinical management should include an interdisciplinary treatment approach with gynecology, pediatrics, and pediatric surgery to balance the risks and benefits of conservative management. Surgical removal can be safely postponed until it becomes necessary due to clinical symptoms.
Keywords
Established Facts and Novel Insights


Introduction
Pediatric and adolescent breast masses are nearly always benign lesions but can pose problems in clinical management. This is because of the patients’ age, size of the lesion, asymmetry, or rapid growth.1,2 In a review of 15 publications, less than 1% were malignant. 3 Optimal management of breast masses in the juvenile patient includes accurate diagnosis, counseling of the patient, and appropriate surgical treatment, when indicated. The differential diagnosis in this setting not only includes a range of pathological lesions, 4 but also includes developmental abnormalities,5 -8 inflammatory processes, 9 premature breast development and juvenile hypertrophy,8,10,11 benign proliferative lesions or cysts, 12 or malignancy and other lesions.3,13 -17 Asymmetric development is within the spectrum of physiologic variability of breast growth and should not be interpreted as a neoplastic process. 18 Breast abscess was reported in neonates or associated with dermatologic conditions such as desquamative erythroderma, severe monilial rashes, or staphylococcal pyoderma infection.9,19 In these circumstances, biopsies are unnecessary and surgical excision is not indicated because surgical excision of developing breast tissue can result in a breast deformity. However, unifocal, neoplastic lesions can be of greater concern, because of the growth and the size of the lesions. Juvenile fibroadenoma and juvenile hypertrophy are the most common causes for unifocal breast enlargement.7,12 Clinically, juvenile fibroadenoma is characterized by the following features: (1) occurrence in adolescents (⩽18 years), less frequently in young adults; (2) hormonal sensitivity with rapid increase in size; (3) enlargement of the breast 2 to 4 times resulting in gross asymmetry; (4) protrusion of the skin; and (5) displacement of the nipple. 20 In a review of 153 patients with juvenile fibroadenoma, the mean age of the patients was 16.7 ± 4.1 years (range: 9-25 years). 21 In this highly sensitive phase of breast development, the treatment must be planned very carefully in a multidisciplinary setting.21 -25 As a rule, pediatric breast masses should be treated conservatively, in the first place.26,27
Case Report
Clinical history
The patient was first referred to our breast unit in 2015 at the age of 2 years with unclear retromammary palpation findings on the left side. According to the mother, the main finding had been present since birth. However, within the past 2 months, a second focus had developed medially and the primary tumor had enlarged. The little patient had no complaints. Clinically, there was a slight enlargement of the left breast (Figure 1A). Retromamillary on the left side, 2 adjacent findings measuring 1 to 2 cm were palpable, displaceable to the pectoral muscle and the nipple. Sonographically correlating with this was a 17-mm smooth-bordered main finding with directly medially adjacent secondary finding of 9 mm in diameter (Figure 2A). Both lesions were hypervascular and were classified as BIRADS4a. In the subsequent tumor board, in consultation with the pediatric surgical colleagues, the recommendation for excision after histological confirmation through core-cut biopsy was given. Still, the patient’s parents were informed that the risk of malignancy was low and that the development of the mammary gland could potentially be impaired as a postoperative complication. During a detailed discussion, the parents decided for conservative management under close clinical control.

(A) Clinical presentation of the then 2-year-old girl in 2015: The left breast was swollen, but did not cause any complaints. (B) Clinical presentation of the 9-year-old patient in 2023: In addition to the massive swelling, there is a marked redness of the left breast. (C) Clinical presentation 2 weeks after surgery.

(A) Sonographic image of the first diagnosis of the mass in 2015. The fibroadenoma in the retromamillary area of the left breast presents as an encapsulated, oval, homogeneous, isodense subcoutaneous tumor measuring 27 mm. (B) Follow-up after 2 years shows a slight regression of the mass. (C) On presentation for treatment in 2022, the tumor has grown to the size of 55 mm with irregular shape.
Over a period of 3 years, the patient was repeatedly examined at our breast unit, where the sonographic findings showed a slight regression (Figure 2B). We do not have clinical follow-ups between the age of 5 and 9 years. Yet, according to the patient and her parents, there was no noticeable growth during this period.
Preoperative course
In 2023, the 9-year-old patient presented again to our breast unit. According to the parents, the size of the left breast had more than doubled within 3 months. A retromamillary mass, measuring about 7 cm, was found slightly painful on palpation (Figure 1B). The contralateral breast showed age-appropriate development. Sonographically, a smooth-bordered, hypoechogenic, retromammary mass with an extension of 55 mm was seen, which had apparently arisen from the previously described, now confluent juvenile fibroadenomas (Figure 2C). The findings showed unsuspicious elastography (<3.5 m/s), and no hyperperfusion in duplex sonography. The finding was classified as BIRADS 4a. Lymph node status was unremarkable on both sides.
Due to the rapid growth and the pain symptoms, excision of the lesion after histological confirmation by core-cut biopsy was planned. The biopsy confirmed the clinical diagnosis of a juvenile fibroadenoma. Re-examination 1 week after the biopsy revealed significant redness and increased tenderness of the entire breast, and antibiotic treatment with clindamycin was started. The parents decided together with the young patient to have the recommended excision performed.
Surgical therapy
On admission for surgery 2 weeks later, the redness had slightly regressed. The lesion, which completely hollowed out the small breast, was completely removed via an areolar margin incision (Figure 3). The operation was without complications. Both breasts were now symmetrical again, and the redness of the left breast slowly regressed postoperatively.
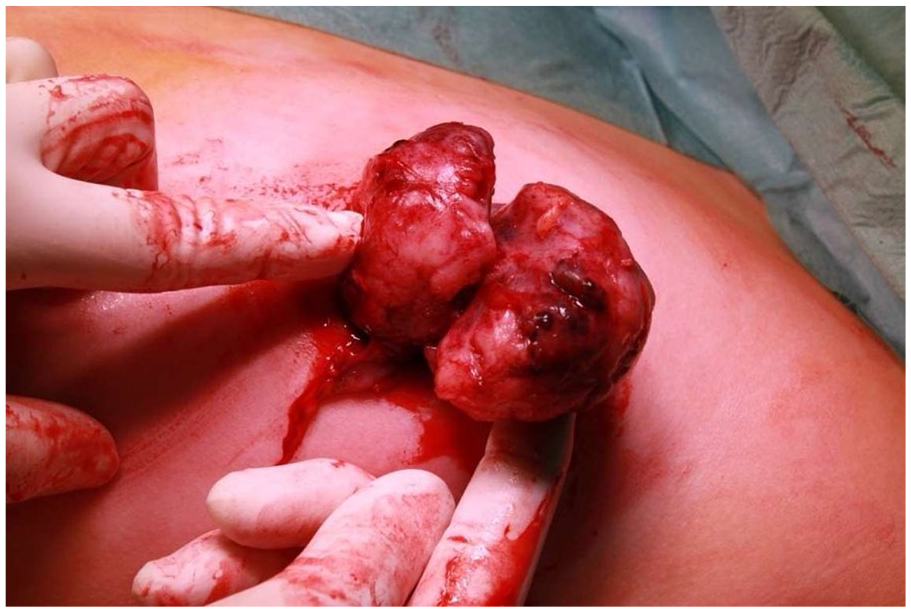
Intraoperative situs: The lobulated fibroadenoma is bluntly extirpated with intact capsule.
Histopathological findings
A binodular 89 g, 7 cm × 5.5 cm × 4.5 cm, encapsulated, yellow-brownish specimen was received with intact capsular margins (Figure 4). Histologically, a fibroepithelial lesion consisting of cellular, monomorphic stroma, and hyperplastic ductules was found, and a diagnosis of a juvenile fibroadenoma with gynecomastoid epithelial hyperplasia was made (Figure 5).

Macroscopic aspect of the surgical specimen: The capsule and the binodular structure are clearly visible.

HE-stained slide: Cell-rich, mitotically active stroma without atypia. The proliferative epithelial changes show the picture of gynecomastoid epithelial hyperplasia.
Epicrisis
Ordinary postoperative course and discharge on the third postoperative day. A wound control after 10 days showed a further regredient redness and normal scar conditions. The young patient was now symptom-free and expressed relief that the masses had been removed completely. The patient was followed up for 1 year after surgery without signs of recurrence (Figure 6).

Clinical presentation of the 9-year-old patient 6 weeks after surgical removal of the juvenile fibroadenoma from the left breast: The scar is unremarkable without any signs of inflammation. The slight residual swelling of the left breast decreased further in the following weeks.
The patient and her parents gave written informed consent for publication of the details of their medical case and any accompanying images.
Discussion
To the best of our knowledge, this is the first case described in the literature with rapid growth of a juvenile fibroadenoma at the onset of puberty. Our case demonstrates that juvenile fibroadenoma can be detected as a small lesion already at 2 years of age but beginning to grow rapidly at the onset of puberty. The occurrence of fibroadenoma very early in childhood is extremely rare. This must be differentiated from transient breast hypertrophy that occurs in up to 90% of neonates due to maternal hormonal influence. 24 To our knowledge, there are only 4 reports of juvenile fibroadenomas in children less than 2 years of age. In one case report, a 16-month-old girl with a 6-month history of unilateral breast enlargement caused by a 3-cm well-circumscribed, solid tissue mass is described. 28 The tumor was surgically removed and pathologically identified as juvenile fibroadenoma. Another 2 case reports describe similar fibroadenomas in small children aged 17 and 13 months.29,30 The earliest documented case concerns a 4-month-old male infant with fibroadenoma. 31 In addition, our case demonstrates that a watch-and-wait strategy is safe, and surgical removal can be postponed for years until the onset of puberty, when it becomes necessary to intervene surgically because of tumor growth and size.
Juvenile fibroadenomas typically are encountered between 9 and 17 years of age, but also adult-type fibroadenomas can occur in adolescence.2,23 In rare cases, juvenile fibroadenoma can occur bilaterally 32 -35 and may reach very large size36 -40 growing of up to 28 cm, 41 causing problems with surgical management.42 -45 Juvenile fibroadenomas differ from their adult counterparts in several aspects, namely a broad and more cellular fibrous stroma, pericanalicular or mixed peri- and intracanalicular growth pattern and epithelial hyperplasia. Often but not always a moderately or very cellular stroma is seen, but without heterogeneous stromal expansion or stromal overgrowth, which is a characteristic feature of phyllodes tumors (PT). Epithelial hyperplasia can be florid in appearance and can be very prominent in younger patients. 46 Often a gynecomastoid pattern is seen, 47 but ductal or lobular carcinoma in situ has not been described in association with a juvenile fibroadenoma. In the usual case of juvenile fibroadenoma, presenting early after onset of puberty, stromal mitoses are increased, and juvenile fibroadenoma may show areas with brisk mitotic activity, having up to 6 to 7 mitoses/10 HPF. 47 Neither this nor the appearance of leaf-like fronds should lead to the diagnosis of a benign PT in the absence of other histologic features of PT.23,46,48 It is important to avoid an overdiagnosis of benign PT, because this may lead to unnecessary surgery. Molecular analysis of juvenile fibroadenoma supports this, especially the lack of TERT promoter mutations which is characteristic for PT indicates the indolent nature of juvenile fibroadenoma.49,50
Conclusions
Regarding the clinical management in case of very early appearance, an interdisciplinary treatment approach with gynecology, pediatrics, and pediatric surgery should be followed, and a conservative approach is preferred. 51 In cases of moderate size without growth tendency and without symptoms, the indication for surgical therapy should be critically evaluated, also because surgical interventions can lead to an impairment of breast development. In case of rapid growth or clinical discomfort due to the finding, core-cut biopsy for histological confirmation should be performed, followed by surgical excision of the finding.18,52 Complete excision is important and should be performed to reduce the risk of recurrence. Breast conservation is possible even in cases of large juvenile fibroadenomas. 42 For reliable differentiation of juvenile fibroadenoma from PT, histopathologic diagnosis should be confirmed by a pathologist with profound experience in breast histology.
Footnotes
Acknowledgements
The authors would like to thank Prof Dr J Heil for providing the clinical information for the patient’s first visits in the breast unit.
