Abstract
Objective
To compare the effects of Metformin with N-acetyl cysteine in polycystic ovarian syndrome (PCOS).
Methods
A prospective, randomised controlled study was conducted in the Department of Obstetrics and Gynaecology in a Medical College and General Hospital. Total 115 cases of polycystic ovarian syndrome presenting with different complaints were selected for the study. Fifty nine cases were treated with Metformin (Group-M) and other 56 with N-acetyl cysteine (Group-N). Primary outcome measures are improvement in clinical features and biochemical profile, where as secondary outcome measures are improvement in hormonal profile and ultrasonographic findings. Statistical analysis was done by Z test and Chi square test.
Results
From each group, 50 patients were ultimately evaluated. There was significant improvement in some of the clinical features like weight gain, acne and hirsutism in group-N (P < 0.05), but there was no significant change in other features like oligomenorrhea, amenorrhoea and infertility. The biochemical markers of insulin resistance like fasting insulin, fasting glucose/insulin ratio and HOMA-IR were significantly reduced in group-N. Hormone levels like serum LH, FSH, TT and LH/FSH ratio was significantly decreased in group-N, but FT, FT/TT ratio and SHBG were similar in both the groups. Ultrasonographic findings were similar in both the groups.
Conclusion
N-acetyl Cysteine had better improvement in clinical, biochemical and hormonal profile than Metformin in PCOS patients. It can be used as a substitute for insulin reducing medications in treatment of PCOS patients, considering its limited adverse effects.
Introduction
Poly cystic ovarian syndrome (PCOS) is defined as an ovarian dysfunction syndrome which manifests as a wide spectrum of disorder with the combination of heterogeneous symptoms and signs. It is considered to be the most prevalent endocrinopathy resulting from anovulation and affects 5%–10% of women. 1
Menstrual dysfunction typically occurs in PCOS, ranging from oligomenorrhoea to amenorrhoea. Other clinical features include obesity, infertility due to chronic anovulation, hirsutism and acne due to hyperandrogenism. Long term risks include endometrial hyperplasia, endometrial cancer, type II diabetes, hypertension and dyslipidimia.
According to Rotterdam criteria (2003), 2 PCOS is diagnosed, if there is presence of two out of the following three criteria:
Oligomenorrhoea and/or anovulation.
Hyperandrogenism (clinical and/or biochemical).
Polycystic ovaries, with the exclusion of other etiologies.
To a great extent, etiology of the syndrome has remained unknown although it has been revealed that, synthesis of high levels of androgen and insulin-resistance (IR) lies at the core of its pathophysiology. 3 It has been proven that, IR results in a disturbed response of glucose to insulin stimulation in skeletal muscles and increase of hepatic glucose production as well as lipolysis. 4 While post-receptor dysfunction in the pathway of insulin activity has been introduced as the reason for insulin resistance, the underlying reason for such a dysfunction still remains equivocal. 5
Metformin, an insulin sensitizer, is being used for long time in the treatment of PCOS. Problems associated with Metformin include gastrointestinal side effects, fear of hypoglycemia and increase serum homocystine levels in some patients. 6 Hyperhomo-cysteinemia is a risk factor for cardiovascular diseases, thrombophilia, pre-eclampsia and recurrent abortion. However recent reviews of randomized control trials of Metformin in PCOS have not shown the promise suggested by the early observational studies. 7
NAC (N-acetyl-cysteine) is a stable derivative of the amino acid cysteine, which has antioxidant properties and is required for the body's production of glutathione. Glutathione along with NAC are powerful antioxidants. Through acceleration of glutathione synthetase hormone (GSH) synthesis, 8 there occurs inhibition of oxidative stress and consequently the prevention of hyperinsulinemia induced insulin resistance and preservation of insulin receptors against oxidant agents. 9 NAC probably influences insulin receptor activity9,10 and results in an increase of glucose consumption, which is an indicator of the insulin sensitivity state.
NAC is not found in the diet, but is available as a nutritional supplement. It has proven activity on insulin secretion in pancreatic cells, acting as an insulin sensitizer. It also has antiapoptotic activity, protective action against focal ischemia at level of ovary. Apoptosis is responsible for follicular atresia. Studies have shown that, taking N-acetyl cysteine (NAC) reduces plasma homocystine (Hcy) levels. 11
In the present study, we have evaluated and compared the efficacy of Metformin and NAC on clinical, metabolic, hormonal, sonographic and fertility aspects among PCOS patients.
Materials and Methods
The study was prospective, randomised and comparative study. It was conducted in the Department of Obstetrics and Gynaecology, G.S.L Medical College and General Hospital, Rajahmundry, Andhra Pradesh, India. The study period was from 1st June 2006 to 31st December 2007. A total of 115 patients of PCOS diagnosed by Rotterdam criteria 2 (2003) were included in the study after obtaining written informed consent. It was approved by the Institutional Ethical committee.
Hypersensitivity to either Metformin or NAC, presence of infertility factors other than anovulation, pelvic organic pathologies, congenital adrenal hyperplasia, thyroid dysfunction, Cushing's syndrome, hyperprolactinemia, androgen secreting neoplasia, diabetes mellitus, consumption of medications affecting carbohydrate metabolism and taking hormonal analogues other than progesterone two months prior to enrollment, severe hepatic or kidney diseases and active peptic ulcer were considered as exclusion criteria.
After the diagnosis, cases were randomly assigned to either Group-M or Group-N.
In all the patients the main presenting complaint were noted and detail clinical examination was done. Patients' weight and height were measured, so that the body mass index (BMI) could be calculated. The waist/hip ratio (WHR) was calculated by means of dividing waist size by hip size. Clinical assessment of acne was done by Leeds acne grading technique and assessment of hirsutism was done by Ferriman-Gallwey score. All the patients underwent basic transvaginal pelvic ultrasonography for the diagnosis of poly cystic ovaries according to Rotterdam criteria (2003). 2 Baseline biochemical and hormonal tests were done on second day of cycle, after spontaneous menstruation or withdrawal bleeding with oral medroxy progesterone acetate. The samples were taken after over night fasting.
Follicle stimulating hormone (FSH) and luteinizing hormone (LH) (mIU/ml) were measured by immuno reactive multi analysis. Total testosterone levels (TT) (ng/ml), free testosterone (FT) (pg/ml) and sex hormone binding globulin (SHBG) (nmol/L) were measured by enzyme immunoassay (EIA). Fasting blood sugar (FBS) (mg/dl) and fasting insulin (mU/L) levels were measured by means of enzymatic colorimetry and EIMA, respectively. Homeostatic model of assessment of insulin resistance (HOMA-IR) index was calculated through the formula glucose x insulin/450.
Patients were divided into two groups considering the similarity of compound confounding variables and randomized in order to minimize the effects of confounding factors through a randomized method. One group (Group
Patients presented for infertility were treated with Clomiphene Citrate along with Metformin or NAC. Dose of Clomiphene was 50 mg/day from day 2 to 6 and gradual increment in next cycle by 50 mg/day with maximum up to 150 mg/day.
All patients were advised to avoid any change in their physical activity and nutrition and not to undergo any new pharmacotherapy during the study. Patients were asked to report any possible adverse effects. Each patient received the treatment for 3 months. At the end of treatment, they were evaluated for regression of main presenting complaints. Biochemical and hormonal tests were repeated again on 2nd day of menstruation. Transvaginal pelvic ultrasonography was repeated again.
Data analysis was carried out by SPSS version 16.00. Comparison of the effects of Metformin and NAC on patients with PCOS was performed by Z test. Comparison of the effect of Metformin and NAC before and after treatment was conducted by Z test. Comparison of qualitative parameters before and after treatment with Metformin and NAC was conducted by Chi square test with or without Yates correction. A 'P' value less than 0.05 was considered statistically significant.
Results
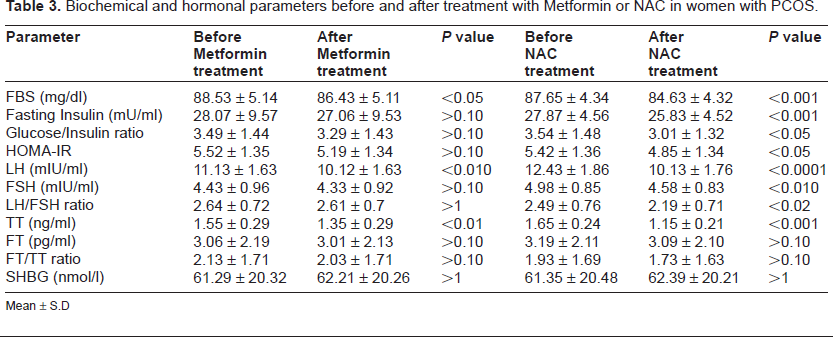
Total 15 number of patients (9 from Metformin group and 6 from NAC group) dropped out, due to intolerance of medication. Ultimately, evaluations were limited to 50 patients in each of the two groups. The Metformin and NAC groups were homogeneous, considering their demographic and clinical characteristics (Table 1), such as: age, socioeconomic status, body mass index (BMI) and waist to hip ratio (W/H ratio). Similarity was also observed when their main clinical feature was taken into consideration (Table 2): namely weight gain, oligomenorrhoea, amenorrhoea, hirsutism, acne and infertility. Both the groups were also similar in biochemical and hormonal profile (Table 3), like fasting blood glucose, fasting insulin, glucose/insulin ratio, HOMA-IR, LH, FSH, LH/FSH ratio, total testosterone (TT), free testosterone (FT), TT/FT ratio and SHBG level. All the patients in both groups had ultrasonographic features of poly cystic ovaries (PCO).
Clinical characteristics of the two groups of patients.
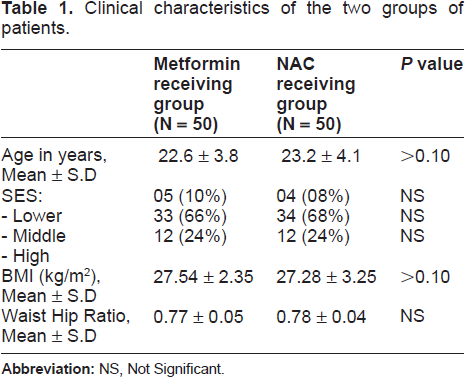
Clinical features before and after treatment with Metformin or NAC in PCOS patients.
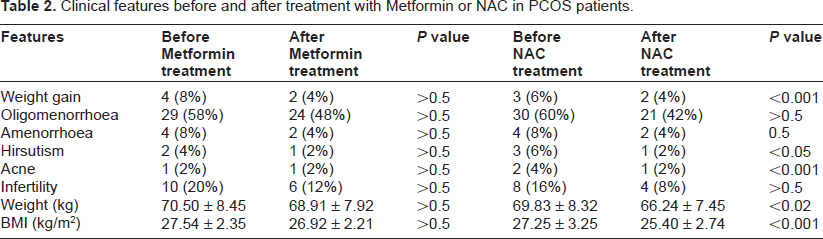
Biochemical and hormonal parameters before and after treatment with Metformin or NAC in women with PCOs.
Mean ± S.D
After completion of the treatment course, no significant change was observed in the results of sonographic examinations, but there was statistically significant improvement of weight gain, acne, and hirsutism in NAC group. No significant change in oligomenorrhoea, amenorrhoea and infertility was observed. Pregnancy rate following consumption of NAC was reported to be 50% as compared to 40% in the Metformin group (P = 0.50).
There was improvement in fasting blood sugar level after treatment in both the groups, but it was more significant in NAC group. Fasting Insulin level was not decreased in Metformin group, but there was significant decrease in NAC group (<0.001). Fasting glucose/fasting Insulin ratio and HOMA-IR was decreased significantly in the NAC group (Table 3).
Serum LH level was decreased in both the groups, but it was more significant in NAC group. Change in serum FSH level and LH/FSH ratio was not significant in Metformin group, where as it was significant in NAC group. TT was decreased in both the groups, but in NAC group it was more significant. Nevertheless, no significant change was observed in serum FT, TT/FT ratio and SHBG in both the groups (Table 3).
Overall, insulin resistance, which was determined by a combination of fasting insulin, fasting glucose/insulin ratio, FBS and HOMA-IR, had improved significantly after NAC treatment as compared to Metformin treatment.
Discussion
In PCOS; IR or compensatory hyperinsulinemia, hyperandrogenemia and disrupted folliculogenesis are distinct manifestations, which are somehow correlated to each other and increases the risk of long term complications.
This study has been conducted to evaluate the therapeutic effects of NAC and Metformin on clinical, biochemical, hormonal and fertility aspects of the disease, as well as a comparison of the therapeutic effects of the two drugs in women suffering from PCOS. The results illustrate the fact that, after 12 weeks of treatment with NAC, patients showed a significant decrease in weight gain, hirsutism and acne. Weight gain is an important predictor of insulin resistance. 12 In a study conducted by Saghar Salehpour et al, there was significant improvement in weight loss, BMI, waist size and WHR in NAC group as compared to placebo in six weeks of treatment. 13 In another study conducted by Fulghesu, 31 out of 37 women, who were enrolled, were obese. In this study, the administration of NAC did not result in any significant change in BMI. 9 In the study conducted by Elnashar on 64 women suffering from CC- resistant PCOS, patients were divided in to two groups, one receiving NAC and the second Metformin for a period of six weeks. Here again, no significant change was reported in either BMI or WHR. 14 Studies on other insulin sensitizing agents, such as Thiazolidinediones and Pioglitazone have reported weight gain in patients. 14 The significant weight loss in our study may be due to longer duration of treatment as compared to Elnashar et al.
In our study, there was insignificant decrease in other clinical features like oligomenorrhoea and amenorrhoea, these findings are similar to the findings of Salehpour et al 13 in a prospective experimental clinical trial of NAC with placebo in a group of 36 patients. Probably longer duration of treatment is required for improvement in menstrual problems.
There was improvement in infertility due to anovulation in both the groups, but it was not significant. In the study by Salehpour et al 13 ovulation rate following consumption of NAC was reported to be 55.60% (10/18) as compared to 16.7% (3/18) in the control group (P = 0.035). In our study, also the ovulation rate was 50% in NAC group. Through a five day treatment of obese CC- resistant PCOS patients with NAC, Rizk et al has reported a significant increase in ovulation rate (49.3%) and pregnancy rate (21.3%) as compared to the control group (1.3% and 0%; P < 0.0001, P = 0.00006). 15 Meanwhile, after a six week treatment course, Elnashar reported the ovulation rate to be 6.7% (2/30) in the group receiving NAC as compared to 51.68% (16/31) among patients treated by Metformin. 14 He concluded that, NAC per se can not be considered an effective medication in ovulation induction among women with CC- resistant PCOS.
Significant decrease in biochemical markers of insulin resistance like, fasting insulin, fasting blood sugar, fasting glucose/insulin ratio and HOMA-IR index was also found in other studies. In the study by Salehpour et al 13 there was significant drop in serum fasting plasma glucose (FPG), fasting insulin levels and HOMA-IR index, but the rise in glucose/ insulin ratio was not found to be statistically significant. Thus, it seems that, NAC consumption has been accompanied with an improvement in insulin sensitivity and glucose utilization.
Treating 20 PCOS women with NAC, Kilicdag 6 noticed that, despite the insignificant change in fasting plasma glucose (FPG) (P = 0.20), insulin levels dropped significantly (P = 0.001) and the decline in HOMA-IR index was also statistically significant (P = 0.001). In the study conducted by Fulghesu 9 through which insulin sensitivity was assessed using the colompe euglycemic hyperinsulinemic technique, patients with PCOS showed an increased sensitivity to insulin and a significant decline in insulin area under curve (AUC) after oral glucose tolerance test (OGTT), while FPG, fasting insulin and glucose AUC remained intact. While, Elnashar reported that, FPG and serum insulin levels dropped significantly among patients who received Metformin and such a change was not significant in the group of patients being treated with NAC. In his study, the glucose/insulin ratio did not show a significant change in the two groups. 14 But in our study, it was significant and better as compared to Metformin.
The significant decrease in serum LH, FSH and LH/FSH ratio in our study was not observed in the study by Salehpour et al. 13 They compared NAC with Placebo, but in our study the comparison was with Metformin. In Metformin group, there was decrease in serum LH, but there was insignificant decline in serum FSH and LH/FSH ratio.
The decline in TT in both the groups and more so in NAC group was also observed by different studies, e.g. Salehpour et al 13 Fulghesu et al 9 Elnashar et al 14 Kilic-Okman et al 16 and Peterson SW et al. 17 The insignificant change in FT, FT/TT ratio and SHBG before and after treatment in each group and in between the two groups was also reported by previous studies in this regard.9,13,14,16
Hyperandrogenism interferes with follicular maturity in women with PCOS and results in anovulation. 18 It seems that, for future ovulation induction, NAC preserves more follicles in the ovary through its anti-apoptotic mechanism. 19 But in our study, after completion of the treatment course, no significant change was observed in the results of sonographic examinations in both the groups and in between the two groups. It is similar to the findings by Salehpour et al. 13
Various studies have concluded that, Metformin does not result in an improvement of the hyperinsulinemic and excessive testosterone state. 20 Recently, one randomized clinical trial (RCT) has proven that, patients who take placebo in combination with CC have no significant difference in ovulation and pregnancy rates when compared with PCOS patients taking Metformin together with CC. 14 It seems that, the beneficial effects of Metformin are manifested in some special groups.
Overall, as compared to the long course of treatment (24–36 week) with other insulin reducing medications, the highly significant changes brought by a 12 week course of treatment with NAC suggest the hypothesis that, longer treatment with NAC may result in more desirable outcomes, such as more effective control of clinical hyperandrogenism, menstrual irregularities and sonographic findings. So far, no adverse effects have been reported for NAC as it is an amino acid. It was well tolerated by our sample population as compared to Metformin (10% vs. 15%) (P = 0.20).
An assessment of the therapeutic effects of the medication (NAC) when combined with behavioral modification can also be considered for future studies. It will be more helpful if future studies are conducted with more number of patients and for a longer period of treatment.
Conclusion
It can be concluded from the results of the present study that, NAC improves some of the clinical features, biochemical markers of insulin resistance, hormonal levels, anovulation, and consequently the long term health status of women with PCOS through inhibition of oxidative stress and improvement of peripheral insulin. Due to lack of adverse effects, NAC can be regarded as an appropriate substitute for insulin reducing medications in the treatment of PCOS patients.
Disclosures
This manuscript has been read and approved by all authors. This paper is unique and is not under consideration by any other publication and has not been published elsewhere. The authors and peer reviewers of this paper report no conflicts of interest. The authors confirm that they have permission to reproduce any copyrighted material.
