Abstract
In this article, we explore the perspectives of Māori with mate wareware (dementia) and their carers with respect to the use of their health records, particularly for the purposes of health research. Grounded in Kaupapa Māori research principles, we held two wānanga with members of a kaupapa Māori, mate wareware support group to explore their perspectives on uses of their health data. Themes developed that were relational with respect to agreed uses of data (whakaaetanga); reciprocal with respect to benefits to the community and future generations (manaakitanga); included expectations around degrees of control over data use (mana); included Māori cultural understandings of the relevance of spirituality and related tikanga to wellbeing (wairuatanga) and observed appropriate restrictions on sensitive material (tapu). Varied attitudes towards the use of health data in research strongly suggest that changes in health system data infrastructure are required to support Māori conceptions of appropriate data use.
Background
Recently, the views of the public have been canvassed regarding the use of their routinely collected health records not only for their health care but also for purposes including health resource planning and health research. There have been increasing research efforts to explore the potential use of artificial intelligence in health research. These initiatives require data to train AI models. Hence, it is important to understand what concerns might be raised by patients for the use of health records for research purposes like these.
Internationally, workshops between leaders of Alaska Native tribes and genomics researchers have highlighted a range of concerns regarding existing research practices and Indigenous communities, particularly due to a lack of meaningful involvement resulting in a lack of reciprocal benefits (Hiratsuka et al., 2020). In addition, tensions have also been noted between recent open health data trends and Indigenous data sovereignty interests (Cordes et al., 2024). However, even when researchers claimed to apply Indigenous data governance approaches to routinely collected health data, a review of relevant research found inconsistent reporting (Engstrom et al., 2024).
Previous studies on attitudes to health data use in Aotearoa have utilised surveys. Rosie Dobson et al. (2021) conducted an anonymous online survey in the Waitematā District Health Board. Cristian Gonzalez-Prieto et al. (2023) employed a similar anonymous online survey method as a basis for exploring attitudes to health data use specifically by those affected by mate wareware (dementia).
Gonzalez-Preito’s survey elicited some comments that raised some cultural considerations. Comments from two Māori respondents indicated that they did not agree with their data being used after they had passed away (Gonzalez-Prieto et al., 2023, p. 72). Other comments by Māori respondents indicated that they wanted to be phoned before their data was used and another wanted feedback about how their information has been used to help others. Māori respondents were a small portion of the survey population—of 202 respondents, 12% were Māori and 65% European—but their feedback suggested that it would be worthwhile to consider Māori perspectives more closely.
The format of the online survey meant that—while there was quantitative data from Likert-type scales used to measure comfort with different scenarios—there was very little qualitative information about the values and rationales that may inform these comfort levels. A follow-up qualitative study using one-on-one interviews with a sub-sample of online survey respondents was conducted by Groenewald et al. (2025) but only one of the 28 participants identified as Māori. Consequently, it was important to follow-up on Māori attitudes towards health data use, particularly by those with dementia and their carers. For our research, a wānanga format (group discussion and knowledge sharing) was more desirable than the one-on-one interview format.
Typically, clinical researchers—influenced by a biomedical model of health—focus primarily on characteristics of those who are directly affected by a condition. And clinical research has identified differences between Māori with mate wareware and other ethnicities, for example in patterns of mortality Cullum et al., 2020b; age of presentation of mate wareware in Cullum et al., 2018). However, recent research into Māori perspectives on mate wareware generated more holistic models, for example, the He Tūhononga Whaiaro model, which models the wellness of the brain in relation not just to aspects of the affected individual, but also in relation to the strength of connections to wāhi (place), tūpuna (ancestors), whānau (family group) and further social connections (for example, Menzies et al., 2022). Whānau activities are specifically centred in Dudley et al.’s (2019) research into Te Oranga Wairua (spiritual wellbeing) of the whānau in the context of Māori understandings of mate wareware. A similar culturally appropriate framework has also structured a Mate Wareware mobile app for whānau (Dudley et al., 2023). Māori affected with mate wareware are 3 times less likely than European New Zealanders to go into aged residential care (Ma’u et al., 2021, p. 52, 2022). So consideration of the effect of mate wareware on whānau is important. Similar concerns have led to calls for and research into a Māori prevalence study (Cullum et al., 2020a; Martinez-Ruiz et al., 2021, 2022, 2024), which is currently underway (Health Research Council, 2022).
To explore these culturally grounded concerns more deeply, the qualitative research in this study was informed by a Kaupapa Māori approach, emphasising Māori values, active involvement with the community and collective wellbeing. Māori researchers and Māori memory team staff agreed initial plans with the organisers of Mānawatia Pakeketanga, a community support organisation for whānau with mate wareware that is run based on Māori cultural activities (Reeve, 2024; Te Ahunganui: Te Apounga Trust, 2025). The timing and processes of the research wānanga were agreed with the members of that rōpū (group) across multiple visits. The reflexive thematic analysis was also conducted by Māori members of the research team.
It is also worth noting that there is no intention to develop the Māori perspective, as if there is a homogeneous view; there were a range of differences in views. Rather the themes identify areas that seemed to be important areas of discussion for our rōpū and that might warrant further consideration with respect to health information systems and health data use.
Methods
Participants
Given that a Māori cultural understanding of mate wareware centres the whānau, we aimed to include carers and whānau in our wānanga. The organisers of Mānawatia Pakeketanga in Manurewa floated the invitation to be involved with this study with the rōpū, who then invited two of the researchers to attend and discuss in greater detail, at which point the research pānui (notice) was discussed. There are typically three support staff, including two from the Counties Manukau memory team, who assist with the group activities. Through multiple sessions, researchers and the rōpū came to a collective understanding and agreement about proceeding with two wānanga (group sessions) with participants of Mānawatia Pakeketanga. For this research, two approximately 30- to 40-min wānanga were held with members: the first with the kaiāwhina (carer) rōpū and then the second a week later with the pakeke who have lived experience of mate wareware. On the scheduled day of each wānanga, participants self-selected as to whether they would like to participate or not.
The kaiāwhina rōpū contained six active participants, four of whom were Māori, one Cook Island Māori and one NZ European. There were eight participants in the pakeke rōpū, of whom six are Māori and two NZ European.
Contributing participants in the kaiāwhina rōpū ranged from 54 to 76 years of age and were all women. All of the pakeke with mate wareware were men aged from 75 to 79. Two support staff, who were also Māori, participated in the pakeke rōpū aged from early 50s to early 60s.
Participants in either wānanga received a $50 voucher as a small token of appreciation for their contribution.
Procedure
One of the organisers of the research wānanga, DW, is Māori—and does research in Māori data sovereignty. He has experience with research involving wānanga, but not within a clinical setting, which brought additional new considerations. The other main wānanga organiser, SY, is a Pākehā clinical psychologist from the Memory Team—who has a wealth of clinical expertise, understanding of how the health system operates, as well as research expertise.
It became clear that this research is itself an example of academic research that we were investigating Māori attitudes towards. It is worth commenting on the procedure for the wānanga as it surfaced some lessons about how the aims of the wānanga approach sometimes conflicted with the formalities of some clinical research ethics processes. For example, there was a tension between the collective verbal agreement about how to proceed as a rōpū that occurred during planning discussions with the group when contrasted with the rather legalistic-style individual consent forms. In some cases, participants rejected the consent forms and refrained from participation in the research wānanga until they were comfortable enough to actively contribute their view, after which they chose to sign the forms. However, the forms themselves acted to undermine the relational aspect of the wānanga. And it would be fruitful to employ the themes that arose in this research wānanga to reflect on how this study developed.
In July 2023, the research team met with members of the Counties Manukau Memory Team who provide health and social work support to Mānawatia Pakeketanga. The aim of this hui was to explain what the research was about and—as they were familiar with the rōpū—to work out ideas that would be safe and appealing to rōpū members. We agreed on a theme of “Let the Māori voice be heard” and that this is an opportunity to get thoughts in the open. It was also agreed that the rōpū itself will best decide if and how to approach this research. One of the memory team volunteered to raise this with the rōpū to see if they were interested in exploring the idea more.
Mānawatia Pakeketanga has an established order of activities each session that are familiar to members. It was important for the research, and researchers, to be as respectful, inclusive and non-intrusive as possible.
The research team were invited to join one of the weekly Mānawatia Pakeketanga sessions for introductions kanohi ki te kanohi (face to face). There we could meet the members, explain what we were researching and agree on an appropriate way to conduct the research. This occurred early August 2023. Once Mānawatia Pakeketanga indicated interest in supporting the research, a pānui was written and distributed by the Memory Team to Mānawatia Pakeketanga members along with a participant information sheet, consent form and socio-demographic information form.
The participant information sheet was distributed to attendees at Mānawatia Pakeketanga at the end of August. On the September 28 visit by DW and SY, it was agreed as a rōpū that we would hold the Kaiāwhina wānanga that day. The group would regularly divide into kaiāwhina and pakeke groups in the second hour for separate activities, and we decided as a group to hold the wānanga in that time-slot. The Pakeke wānanga was held on October 12.
The sessions were run in a wānanga style. There were various topics that the researchers aimed to better understand the participants’ views on but there was not a rigid question and answer style. Occasionally were some ideas or topics that were volunteered in answers to questions that we could explore a bit more deeply in the discussion. These unintended directions are a feature of the kōrerorero (discussions) rather than a diversion from the intended line of questioning.
The format involved some initial background about how health information is currently used. Throughout the wānanga, questions would be raised to hear thoughts about the following kinds of scenarios:
Patient health information that is used by a General Practitioner or other health professional for that patient’s treatment.
De-identified health information that may be used by GP surgeries and hospitals to better understand the community they are serving.
De-identified information sent to Te Whatu Ora—The Ministry of Health for health planning on a national scale.
De-identified health information used for research, for example, by universities.
De-identified health information shared overseas.
Analysis
Two wānanga were held on two separate meetings by two of the authors, DW and SY: the first with the kaiāwhina rōpū and the second with the pakeke rōpū. Audio recordings of the two wānanga were manually transcribed by two of the authors, DW and EM.
The two wānanga were semi-structured and resulted in approximately 70 min of audio and transcripts. Reflexive thematic analysis was employed to analyse the interview data. V. Braun and Clarke (2006) describe explicit decisions that need to be made in approaching thematic analysis (pp. 81–86). It is worthwhile making two of these decisions explicit.
First, the initial coding was based on a rich description of the dataset rather than detailing parts of the discussion that the researchers may have explicitly asked questions about. One feature of the wānanga was that discussions may go in multiple unexpected directions, so the flow of the discussion and volunteered comments may give rise to important information that is indicative of relevant experiences and concerns even if they were not explicitly requested. Consequently, there may be relevant connections that could be drawn from taking a holistic, exploratory approach to the kōrerorero rather than a potentially restrictive “interested” approach to coding.
Second, themes were primarily constructed from the transcripts of the wānanga (inductive) rather than based on theoretical interest. In one of the early planning meetings, we decided that the theme would be: “Let the Māori voice be heard!”, which was a prominent message of the pānui. So, the themes are intended to be identified and developed from the wānanga discussion in context. Having said this, there were some existing theoretical frameworks that were tested against provisional themes that were found to be ill-fitting. And while we will see in the discussion section that the top-level themes do fit a pre-existing framework, this was discovered after coding rather than something presupposed at the outset.
Quotes from the Kaiāwhina wānanga and the Pakeke wānanga are listed as such below.
Results
Five themes were grouped from codes identified from the transcripts. These are manaakitanga (reciprocity and support), whakaaetanga (agreement, consent), tapu (restrictions), mana (power and authority) and wairuatanga (spiritual practices) (Figure 1).
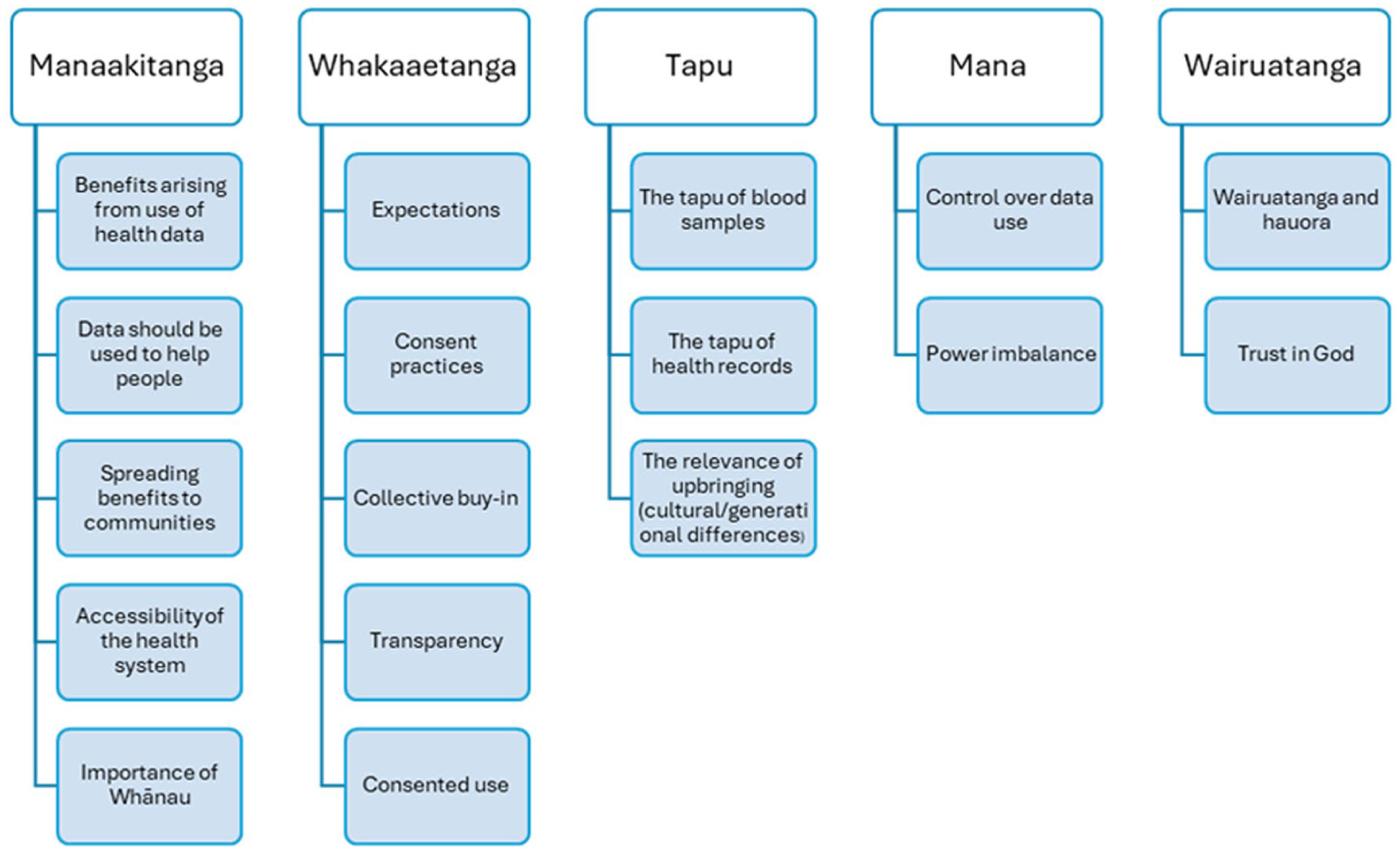
Five themes developed from codes identified from the transcripts.
Manaakitanga
The theme of manaakitanga relates to reciprocity and inclusion. This contains five sub-themes: the importance of health data use in research for helping others; a willingness to contribute; ensuring that benefits are shared and concerns that some are unable to be supported by the health system due to inaccessibility.
Benefits arising from use of health data: the first sub-theme included claims about the benefits that arise from the use of health data. It was noted that health data was important for diagnosis and treatment as well as for health service planning and funding. We all share in benefits like these and they provide a compelling reason to participate in health research:
[. . .] I think, certainly in New Zealand, we’re just trusting that um, data is collected for the betterment of an ongoing society really. And it needs to be done because then it shows some patterns of behaviour and patterns of illness and patterns of, you know all sorts of patterning. I think research is important. I’m happy to be a part of it really. And if you think about the amount of contribution that each of us make within a whole pool of research, it’s quite minimalist but, but it’s important. I believe in research. [Pakeke rōpū] And this kind of data helps with cures as well, doesn’t it? You know, all the data we receive about different things. [Pakeke rōpū] Because [. . .] until you get that data, the government, the government of whatever country doesn’t know how to prioritise this funding. [Pakeke rōpū] Research is necessary, research is great. I’m happy to be part of it. [. . .] That’s where I come from. Because it makes for a better world. [Pakeke rōpū] We all benefited from some sort of research. [Pakeke rōpū]
Data should be used to help people: some members expressed a strong belief that if their data is being used, it ought to be used to help people. Some added that they were happy for their data to be used after they had passed away—but compare with mana and tapu below:
If [there’s] any way that we can help anybody else, that’s what I want to do. And [name of partner] is of the same mind. [Kaiāwhina rōpū] I think that, if the information is private to the study that you’re doing, and [. . .] it has some long term effect, where you know you’re looking towards the future, then why not continue it? The fact that you’ve passed away, to my mind, doesn’t necessarily mean that that information should be taken off you, and stored for what? You know, that’s how I feel. [Pakeke rōpū]
Spreading benefits to communities: there were various comments about who should benefit from different uses of health information. When it came to health research, there was agreement that helping people in Aotearoa was a good thing, particularly future generations. And for those who were supportive of multinationals and researchers using some health data for research, there was an argument that this may be justifiable so long as this resulted in benefits that were accessible to communities. These benefits were not only in terms of accessible new treatments but also in terms of reporting back findings to the communities whose data contributed to the results:
I guess if you allow it to happen here, to help people, why not the reason be the same as if you sent it somewhere else? [. . .] Because after all your reasoning is to help, regardless of what country you’re in. [Pakeke rōpū] I just believe that research has long-term benefits for the next generations, as far as I can see. I mean I know that, I know that health companies made a lot of money out of it, and that’s not to say, that’s not a bad thing. For, if it makes it better for my mokos, then, or whomever might be forthcoming. [Pakeke rōpū] It’s a privilege for people to use it in the way that we want it to be used, not just so that they have a gain and then there’s still no benefit here. We’re here not for ourselves or our husbands but for the future of dementia. [Kaiāwhina rōpū]
Accessibility of the health system: difficulties in accessing the health system and finding relevant information were raised:
[On agreeing to let medical professionals learn from you:] hopefully someone, somewhere has a better idea of what is happening because, um, I don’t think people realise what’s going on. [. . .] I look at Mum and like I’m always like thinking: “is there somewhere we can get some information?” “Why don’t they tell us the stages?”. [Kaiāwhina rōpū] So lots of elderly people got lost in the system, lots of people with dementia got lost in our system. [. . .] we had 5 people—carers—that came and said: “We got lost in the system. Now my partner‘s or husband’s since gone into care or passed away.” [Pakeke rōpū]
Importance of Whānau: whānau arose in discussions in two main ways: first, to note that despite their important roles, carers are generally omitted from consideration by data and support systems related to mate wareware. Second, whānau were noted numerous times as providing a motivation for engaging in health research:
I just worry when she [mum] gets sick, you know, because of the emotional stress—I would hope that this information would help all the women here—or men—in looking after their partners. You know, because they are just kind of left to it. [Kaiāwhina rōpū] You do it for your whānau, don’t you? For others coming behind. [Kaiāwhina rōpū]
Whakaaetanga
The theme of whakaaetanga represents comments about coming to an agreement about the use of health information and biological samples. Several sub-themes are identified. The first regards general expectations about use. The next three sub-themes are characteristics of the consenting process: collective consent, transparency and informed consent. A further sub-theme is about conditions for future use.
Expectations: participants expressed some general If you want my data on a government level then I want transparency. You know, not. OK, it’s: A, B, C, D this is what we are doing with the data for this specific thing. Sweet. You can have it. [Kaiāwhina rōpū] [. . .] while we like to think that this benefits the next generation, whatever, as long as there is a targeted task, here, I’m happy with it. If it’s a thing where there is a whole lot of question marks, I wouldn’t be happy with it. If there is specifically what it is going to be used for, you know, for the likelihood of the next generation that are going to be dealing with mate wareware, then I’m in. If it’s going to be used for a whole lot of stuff, I’m out. [Kaiāwhina rōpū] we’re talking about you know sort of, we’re talking to the people that are here about something that’s um, they’re carrying with them day in, day out you know, the dementia thing, [. . .] not everybody wants the world to know about that sort of thing and so, you know we’re talking about trust and responsibilities. [Pakeke rōpū] I think with all the research, like even, this one, like you know, and it would be great to come back and tell them you know, what the outcome was [. . .] [Pakeke rōpū]
Consent practices: the nature of consent practices was also discussed. Many participants were not fully aware of the current uses of health records. They wanted greater transparency about what they are consenting to, including any risks. They also want consent processes that were understandable by participants and provided them with useful, effective control over data use that could change as health technologies and practices changed:
[Regarding consent:] We just agree, agree, agree to everything, but we just don’t really read them or understand, or not everyone is explaining, is what I think. [Pakeke rōpū] [I’d just like to be fully informed before I say “yes” or “no” to anything.”] [Kaiāwhina rōpū] And I think a lot of people think: oh yeah, it’s a good thing, we’ll just sign it. But then further down the track they start to doubt what they’ve actually signed. You know? [Kaiāwhina rōpū] Is there like thirty years ago or something when we signed up and we don’t know but times change—you know—so could the consent and that be changing also? Because medically everything changes and advances and all that kind of stuff. So should the form somewhere itself be upgraded every so many years. [Kaiāwhina rōpū] I would think, for me, we’re currently involved with the whole dementia area. So any research to do with dementia, I think that that’s a no-brainer. Yes, I’m happy for that. But. Yeah, you can do it that way, can’t you? You can choose to “Yes, it’s my information, that’s fine for any research that is around dementia and, yeah, all that involves.” Which involves a lot, a lot of areas because it involves wellbeing and music and all those things but that’s what I’d prefer to sign then I know that it’s all going to be helping that field. [Kaiāwhina rōpū] Being a power of attorney is really, really hard. So I was a power of attorney for my brother because his family were in Australia, and it’s not easy, it’s not an easy thing. You know. It’s really hard. You’ve got to make a decision and stick by it. All those sorts of things. It can affect other members of the family. [Kaiāwhina rōpū]
Collective buy-in: related to consent are considerations of collective buy-in. An initial comment is that, for Māori, collective buy-in is essential. This buy-in requires everyone to be on the same page about what is being agreed to and why:
When we’re talking about Māori, we have to come from that worldview [i.e., from a tikanga perspective], that this is what it is, and how do we, collectively, have buy-in to that? [Kaiāwhina rōpū] I mean in order for someone to have a buy-in, they have to be fully-informed about what they’re getting bought in to. Not just say: this is a piece of paper, read it and sign it. That’s why I won’t sign it. Because I haven’t had the buy-in as to what I’m signing. [Kaiāwhina rōpū]
Transparency: desires were expressed for greater transparency regarding health information and sample use and storage. When participants shared information and samples for one particular purpose, they were concerned that it might subsequently be used in ways that they had not been told:
We actually want to know that the information that we are going to be sharing or giving, it’s privileged so it should remain privileged. [Kaiāwhina rōpū] How do I know—and you just said that some information the government have—they already know something that I didn’t even know that they did have. [Pakeke rōpū] To be, even just to be aware—you know—that my information is being used for. . . because, you know, being quite naïve, just like, those records are mine and mine alone, you know, without them going in without, you know, taking all this information, even though everything has been taken out that you can’t identify, but it’s still. . . my information. [Kaiāwhina rōpū] They were doing a research study—don’t know what it was—[and requested to] have a sample of some of [my daughter’s] blood [. . .] And I thought ‘Well what are you gonna do with her blood afterwards?’. You know? And they couldn’t answer me. [Pakeke rōpū]
Consented use: the final sub-theme includes some stipulations surrounding consented uses. Generally, samples or health information should only be used for what has been consented to:
It’s not just: oh, we want to use [my health information] here or there. Like a specific task that needs to be done here. And my information will be specifically used for that task, not to be shared out all over the country because they want to gain—I don’t know—stats. That’s just me. [Kaiāwhina rōpū] [Regarding the possibility of health information going to multinational companies:] I’d be pissed off. I really would be pissed off, yeah. Without consent. [. . .] from my perspective, it would be a breach of privacy if they shared that information outside of New Zealand. [Pakeke rōpū] [Regarding blood samples for research:] I wouldn’t want them to bank it. You know? I don’t know how long blood samples last for, but I wouldn’t want them to keep it for like, 20 years and just use it for this and that and everything else. You know? Just that purpose only. [Pakeke rōpū]
Tapu
The importance of cultural considerations regarding tapu was raised. These comments were in relation to blood samples being tapu and medical records being tapu.
The tapu of blood samples: while the questions were about health information, one participant raised concerns regarding expectations and tikanga (custom and correct procedure) related to the tapu of blood samples used for research. These comments had some members of the pakeke rōpū agreeing with them, while another expressed that they were not concerned about these issues:
even though they think “oh, it’s just a blood sample” well it’s not actually just a blood sample, it’s a sample of my blood. [Pakeke rōpū] After you die, anybody’s samples, you know, you should be able to sign a form or something, saying, any body samples of mine should be offered back to the family, so that they can go and put them with you in your grave if they want to. . . I’d love that. [Pakeke rōpū] So that’s why we are particular about our blood samples; who’s taking them, where they’re going to, what are they doing afterwards, are they going to a foreign country—cause that’s our whakapapa. [Pakeke rōpū]
The tapu of health records: there were also comments that health records were tapu:
[Tapu is] a lot of things that Māori people don’t wanna share, cause it’s personal. And it goes right back to where, like, like myself. The reason why I didn’t join this? This is my reason: Is that first of all my doctor said to me, “anything to do with your health; nobody else should know about it.” [Pakeke rōpū] Some people can feel quite uh, not-tapu, about their own information being shared with others. [Pakeke rōpū]
The relevance of upbringing: cultural and generational differences: there was also agreement regarding a comment that there were generational and cultural differences regarding considerations of tapu balanced against engagement with medical research and the sharing of medical information:
And it would be a generational thing too, like, I’m sure. As our kids have gotten more educated, they’ve seen that, but I mean, think of some of our parents [laughs]. They wouldn’t even go to a doctor and medication, until they’re really crook. [Pakeke rōpū] Especially when people have been like that aye. That’s hard to break. That’s hard to pull apart when, when you’ve been like that aye, you know? Like iwis and hapūs, you know. And even you know, your families. Your families have are like that as well, you know? It’s hard to pull apart, you know?. [Pakeke rōpū] So you’re raising the issue of cultural context [. . .] Which is a pretty big issue. In terms of how I see things and how you see things. [Pakeke rōpū]
Mana
The next theme is mana. There were two sides: one sub-theme of having the power to control how one’s health information and biological samples are used and a second sub-theme about potential disempowerment related to opting out of sharing information.
Control over data use: there were differing degrees of comfort regarding potential uses of samples and data by different entities: general practitioner or health professional; regional hospitals and health providers; national-level health research; government and overseas multinational organisations, and there were correspondingly various statements about what kind of control participants preferred. There were multiple calls to have control over how samples and data were used and a variety of criteria were suggested. Regarding specific restrictions, some of which were noted earlier, there were comments that multinational use of data must gain consent; that public good rather than profit should result from health information use; that samples and information should not be sent overseas and that samples not be used after the person has passed away:
See, me, I like that thing where you said: the doctor, and then the community, and then, like, the hapū, iwi. I would stop at, like, government, for me, I would stop at that level, unless there’s transparency as to specific, you know, thing, that they want to use the data for. I want to give consent for that. [Kaiāwhina rōpū] I want to say that. It is a right of a person, an individual, to participate. It is also their right if they want to withdraw from participation too. It’s a right. It’s not a given. It’s a right. [Kaiāwhina rōpū] In terms of being culturally appropriate, or culturally sensitive, while we’re giving an informed decision maybe to go with the data, we still want to have the say here in terms of how that data is used. Is it used according to our tikanga. [Kaiāwhina rōpū] I would hate for them to take the information and use it in a negative way because there is always someone that’s—you know—wants to make money. So I’d hate for them to say: “Oh, we’ve found something!” . . .and it actually can, like, stop this from happening. . .—and then the but is it’s going to cost you $800,000, or something crazy. [Kaiāwhina rōpū]
Power imbalance: the flip side of control is a sense of power imbalance with respect to the current system. Concern was expressed multiple times about the undesired use of health information by the government. Others were concerned that the current system provided no way to opt out of health information sharing without opting out of mainstream health services:
Now how did the [Government] get [my health data]? So if I’m saying that well now I don’t wanna give this, because of that reason, well am I. . . missing something or. . . [Pakeke rōpū] Is there something that could start working towards the consent of—you know—it can be changed or—you know—without any repercussions of: no you can’t come and see me at the doctors. You know what I mean? [Kaiāwhina rōpū]
Wairuatanga
Comments about the importance of spiritual beliefs arose in the contexts of, first, wairuatanga as an integral part of rongoā Māori and, second, for one participant, faith in God with respect to important decisions.
Wairuatanga and hauora (wellbeing): one participant discussed some of the spiritual aspects of rongoā Māori, including practices related to tupuna (ancestors), wai tapu (sacred waters) and the use of karakia (incantations). They were raised with these practices and still practice related tikanga today:
[. . .] there were places that we were sent to down the coast that were wai tapu. You know places that you go and you, if you had something wrong with you, you’d go there and you’d sprinkle yourself with the water. And, and it worked for a lot of our, our whānau aye, you know? It worked. [Pakeke rōpū]
Trust in God: a second participant stated that they had trust in God to guide their decisions and anything that occurs after that decision is outside of their personal control:
Well my personal view on it is that if I trust God in things that I do; whether you send it overseas or not, I leave it in His hands. [Pakeke rōpū]
Discussion
In this section, we are going to delve more deeply into some of the results and place them in the context of related research, particularly research about relevant concepts when construed from a te ao Māori perspective (Māori world view).
The importance and nature of trust and trustworthiness
The issue of trust was identified by members of both the kaiāwhina rōpū and the pakeke rōpū as being important. But different degrees of cautiousness were expressed. For example,
We would like to trust people when we give information. That’s the word here, “trust”. That’s a big word for us, the trust that what we’re giving out is going to be put where we want it to be put, not all over the place. [Kaiāwhina rōpū]
And this contrasted with a more generous attitude:
Well, generally I think we, we’re trusting. And um, Māori have a really strong view about their own data and their own mana based around that but I think, certainly in New Zealand, we’re just trusting that um, data’s collected for the betterment of an ongoing society really. [Pakeke rōpū]
The word “trust” appears in the wānanga transcripts 26 times though researchers only mention “trust” two of those times. And for both wānanga, the term was first introduced by participants. One definition from philosophers Christoph Kelp and Mona Simion (2023) is that trust is “a disposition to fulfil one’s obligations”. From a Western perspective, the notion of trust is often a claim about whether the trusted individual has the capability to be trustworthy; however, Oster and Lightning (2022) note that, for Indigenous communities, trust in relationships is fundamental. Given this relational understanding of trust, it has been noted that there is no term in te reo Māori that is an exact translation of the English word “trust” (West et al., 2020, p. 33), even though there are numerous related cultural value concepts that imply reciprocal obligations. This means that it is worth considering what kinds of obligations may be expected from a Māori perspective when the word “trust” is used. This is because it may be the case that there are different understandings of what is required for trust for mainstream health researchers compared with Māori communities. And failure to understand these differences may result in actions (or inaction) that undermine relationships.
During refinement of the theme categories, it was noticed that our themes fit well with key characteristics of a Māori conception of trust identified in a Haemata report for the Office of the Auditor General from wānanga with Māori (Murphy et al., 2022, p. 10). Here are the four main dimensions of trust identified in that report:
Trust is Relational.
Trust is Reciprocal.
Tikanga Builds Trust and Confidence.
Power imbalance thwarts trust.
We found that the five themes from our research easily mapped to these characteristics from the Haemata account of trust from a Māori perspective (Figure 2). Consider the following:
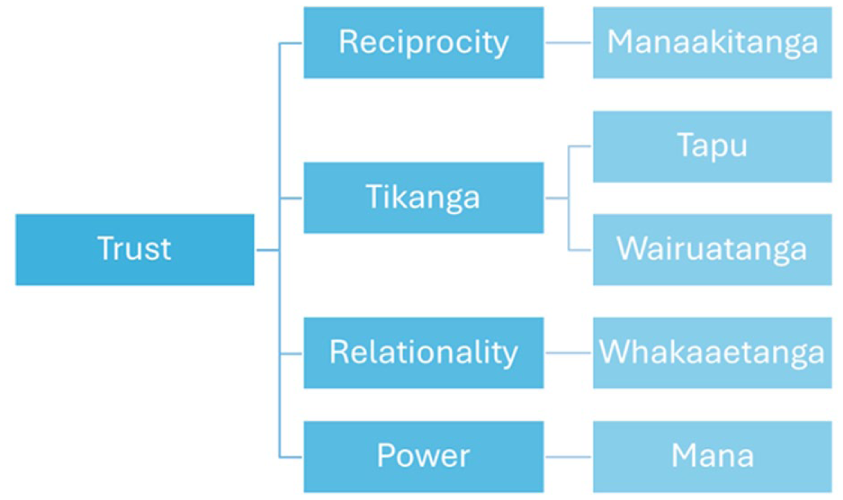
Framework for dimensions of trust from a Māori perspective.
So, our results may add empirical weight to this characterisation of trust. What this amounts to is less of an individualistic and transactional view of the obligations required for trust—for example, consent forms for participants to approve activities by experts who then have no further interactions with them—and more of a relational view, where the benefits of research are shared with the communities who are involved in that research.
The importance of this is that if there are different understandings from those in the health system and Māori communities about what obligations ought to be upheld to count as trustworthy, then this disconnect could cause mistrust.
Awareness of health information use and health research
There were comments from both rōpū that spoke to a lack of awareness of how their health data were currently being used. Support was expressed for health data used to better inform their health care. Support was similarly echoed for health data use in hospital resource planning and targeted research. But there was some concern expressed at the realisation that people’s health data may be used by Government agencies. But generally—across these examples—people had not been informed about how their health data might be used and were unaware that datasets may be created derived from their clinical information and that people outside of their immediate care may have access to that data.
While a couple of participants were aware of the importance of clinical data for health research, there was generally low awareness about the health research that is currently conducted.
There were varying degrees of support for the use of health data for research purposes. At least one participant was strongly supportive of health research, but others placed a number of conditions on the use of health data for research, for example, for it to be used for specific kinds of research; for research where there are concrete benefits to communities and for the benefit of future generations. Some comments regarding experiences with researchers indicated that some researchers had not done enough to engender trust, for example, no reporting back, and a lack of clarity about how samples would be used. These remarks imply a need for more transparent and more culturally appropriate data governance.
There was mention of the importance of data for purposes like funding support initiatives. However, the clinical data collected about those with mate wareware is unlikely to address some of the important resourcing and planning gaps identified by participants when it came to kaiāwhina. The day-to-day support and even the reliance of pakeke on their kaiāwhina for accessing the health system are unrecorded and unrecognised. Also, carers are given very little support from the health system for themselves. There does not seem to be information gathered by the health system to understand, recognise and adequately support their important role. Kaiāwhina are also not provided with sufficiently clear information for them to understand what to expect on their caring journey with mate wareware.
Implications of findings for future research and service delivery
The themes identified from our wānanga reflect not only cultural values but also more specific expectations about data governance. Whakaaetanga involves an obligation to meaningfully engage communities. For example, greater transparency is required around health data collection, sharing and use as there is currently low awareness of these practices. Manaakitanga requires that there are mechanisms for reciprocal benefit from health data use. To uphold mana, health data systems should be designed to give people greater control over how their health data is used, for example, the power to nominate what research areas they consent to their data being used; allowing for an ongoing consent process, rather than a one-time process. Our findings strongly suggest that changes are needed in relation to health research and service delivery in ways that are more likely to increase Māori participation and serve Māori aspirations.
Current consent practices for data use are often not informed—there is little information and minimal or no discussion about how or what data is shared and used—and consent for data sharing is also presented as a condition of receiving care from a health service, so to the extent that receipt of health care currently demands data sharing, it is not freely given. So, consent practices need to be re-designed with Māori to ensure appropriateness.
Conclusion
In this article, we held wānanga with kaiāwhina and pakeke living with mate wareware to discuss the use of health data for purposes including medical treatment, health care resource planning, medical research and statistics at local, regional, national and international scales. Many participants were supportive of their health data being used for the benefit of future generations of their whānau and for the betterment of society but the privilege of institutions using health data was often accompanied by a range of expectations regarding appropriate use.
Many of the themes identified and refined from these wānanga can be related to a Māori understanding of trustworthiness and considerations that may enhance or decrease trust in this sense. A perspective developed that was relational with respect to agreed activities (whakaaetanga); reciprocal with respect to benefits to the community and future generations (manaakitanga); including expectations around degrees of control over data use (mana) and including Māori cultural understandings of the relevance of spirituality and related tikanga to wellbeing (wairuatanga) and appropriate restrictions on sensitive material (tapu). The importance of these considerations with respect to data use varied among participants, with some taking a fairly open approach to their data being used in ways that are expected to help others, while other participants were more hesitant in the absence of evidence of the above considerations being addressed.
For both groups there was generally low awareness of how their health data is currently being used. This suggests that there is more work to do on raising awareness regarding health data usage.
Supplemental Material
sj-docx-1-aln-10.1177_11771801251404817 – Supplemental material for Māori perspectives on health data use for predicting mate wareware (dementia)
Supplemental material, sj-docx-1-aln-10.1177_11771801251404817 for Māori perspectives on health data use for predicting mate wareware (dementia) by Daniel Wilson (Ngāpuhi, Ngāti Pikiao), Susan Yates, Elisa Moller (Ngāti Maniapoto), Gillian Dobbie and Sarah Cullum in AlterNative: An International Journal of Indigenous Peoples
Supplemental Material
sj-docx-2-aln-10.1177_11771801251404817 – Supplemental material for Māori perspectives on health data use for predicting mate wareware (dementia)
Supplemental material, sj-docx-2-aln-10.1177_11771801251404817 for Māori perspectives on health data use for predicting mate wareware (dementia) by Daniel Wilson (Ngāpuhi, Ngāti Pikiao), Susan Yates, Elisa Moller (Ngāti Maniapoto), Gillian Dobbie and Sarah Cullum in AlterNative: An International Journal of Indigenous Peoples
Footnotes
Authors’ note
Funding
The authors disclosed receipt of the following financial support for the research, authorship and publication of this article: This research was funded by a Health Research Council grant. HRC reference: 20/1182. This research project was approved by the Auckland Health Research Ethics Committee on 18/10/2021 for 3 years. Reference number [AH22266].
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and publication of this article.
Supplemental material
Supplemental material for this article is available online.
Glossary
Aotearoa New Zealand
hapū subtribe
hauora wellbeing
iwi tribes
kaiāwhina carer
kanohi ki te kanohi meeting face to face
karakia incantation
kōrerorero discussion
mana power and authority
manaakitanga reciprocity and support
Māori the Indigenous people of Aotearoa New Zealand
mate wareware dementia
mokopuna grandchildren
pakeke mature adult
pānui notice
rōpū group
tapu restricted
te ao Māori Māori world view
tikanga custom, correct procedure
tūpuna ancestors
wāhi place
wairuatanga spirituality
wai tapu sacred waters
wānanga group discussion and knowledge sharing
whakaaetanga agreement, consent
whānau family group
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
