Abstract
We describe a patient with a matured transposed brachiobasilic fistula that was difficult to cannulate due to “rolling” and the inability to fixate. After placing multiple parallel transcutaneous sutures close to the fistula, there were no difficulties with needling. Even after removing the sutures, cannulation went uneventful.
Introduction
Native arteriovenous fistulas remain the gold standard in most dialysis patients with a reasonable life expectancy. Adequate cannulation and dialysis of AVFs depends on characteristics like diameter, flow, and depth, among operator dependent factors such as experience and cannulation technique. Every now and then, however, the dialysis nurse and vascular access surgeon may encounter an AVF that fulfills all maturation criteria while being difficult to puncture even by the most experienced personnel. Often, these AVFs are characterized as “rolling” or “displacing” and this poses the surgeon to a difficult decision whether at all, and how to intervene. Usually, the first step is to advice decreasing mobility of the AVF by using tourniquet fixation or pressure on the AVF by a colleague. Besides, implantable devices are available to put around the outflow vein in order to keep it in place for cannulation. 1 However, these measures may not have the desired effect, putting the patient in discomfort and the nurse in despair, while sometimes performing an invasive procedure without a reasonable result. Therefore, additional treatment strategies for hypermobile outflow veins could be of help to all parties involved in AVF care.
Case presentation
The patient is a 65-year old non-diabetic pre-dialysis female with a transposed left brachiobasilic AVF that was created some weeks ago. Flow is over a liter per minute and diameters are at least 5.5 mm over a long trajectory. The depth of the transposed basilic vein is less than 5 mm. Following the initial AVF creation, the patient endured an unrelated prolonged admission due to a severe pretibial posttraumatic necrotizing infection of the lower leg that responded well to antibiotic treatment and superficial necrosectomy. During these weeks of admission and recovery, the patient lost 20 kg toward a BMI of 18. Thereafter, dialysis was initiated with the inability to dialyse through two needles due to a hypermobile AVF resulting in multiple mispunctures despite external compression and fixation. The patient was referred to the vascular surgeon with the question to somehow revise the AVF. Diameter, depth, and flow were confirmed to be adequate, and it was noted that the patient was cachectic. Shared decision making did not result in surgical revision due to the risk of complications and the uncertain outcome. However, the patient was in great discomfort during needling and it was postulated that fixation of the surrounding skin by plicating the skin parallel to the AVF would be a relatively non-invasive procedure with a reasonable chance of relief.
After tourniquet application, the AVF was marked over the course of the upper arm by ultrasound and the most superficial and wide parts that were considered easiest to cannulate were marked. These locations were locally anesthetised with lidocaine 1%, and transcutaneous, transfascial ethilon 3-0 sutures were placed and tied over a vascular clamp (to prevent too much tension on the skin) on both sides bilaterally, just next to the AVF in a parallel fashion. Ties were not too tight to prevent skin ischemia or compression on the fistula (Figure 1). Afterward, patency and adequate diameters were confirmed by ultrasound.
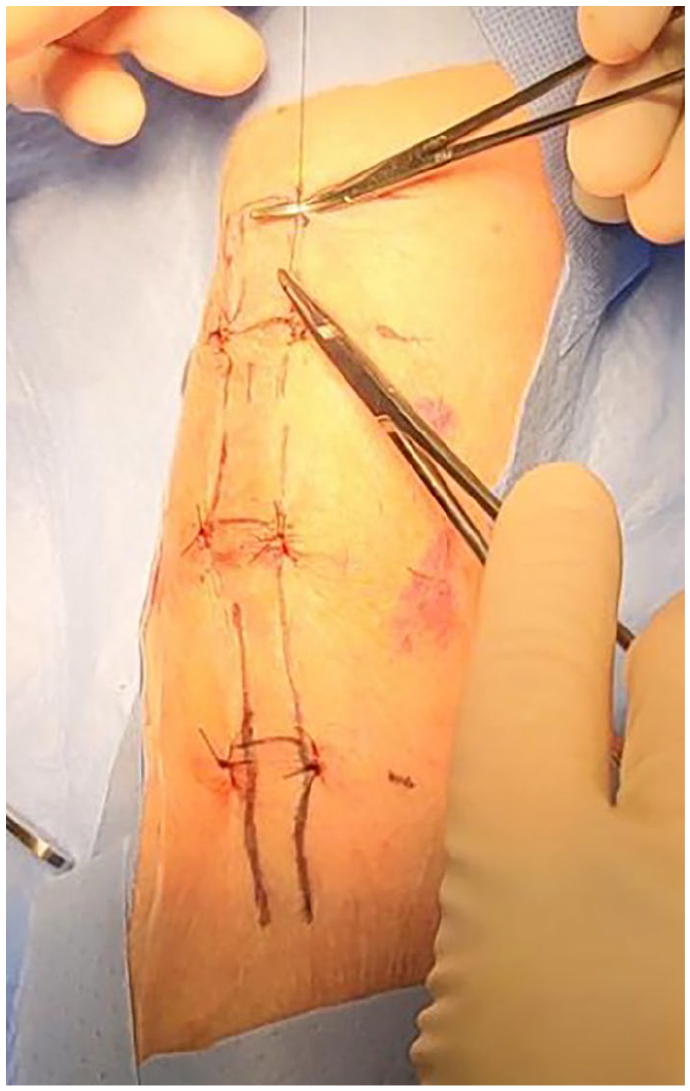
Parallel plication technique for temporary fixation of a “rolling” AVF. Ethilon sutures are placed bilaterally to the fistula and transcutaneously toward the fascia preventing the AVF to move left or right and enabling adequate needling. Placing the knot of the suture over a vascular clamp prevents too much tension to the skin and compression to the fistula.
Immediately, the AVF was easy to cannulate with two needles without any mispunctures during the first 3 weeks, after which the sutures were removed. Thereafter, cannulations and dialysis sessions went uneventful, to great satisfaction to the patient and nurses. Mild scar tissue formation at the site of the sutures as well as the puncture sites may have prevented further mobilization. Taken together, the parallel plication technique might be a minimally invasive addition to existing possibilities to increase cannulation success. The excessive weight loss in this case may have contributed to the hypermobility of this specific AVF.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The patient consented for the publication of the picture.
