Abstract
Introduction:
Failed internal fixation of proximal femoral fractures is associated with significant morbidity, mortality, and financial burden. Conversion total hip arthroplasty (THA) is a technically demanding salvage procedure associated with high risks of periprosthetic joint infection and instability.
Methods:
Independent searches of MEDLINE, EMBASE, and the Cochrane library were performed for studies published from 1990 onwards regarding conversion THA in adults following failed proximal femur fixation. Following screening, 34 studies were included in this review.
Results:
Predictors of failure include female sex, smoking, and tip-apex distance >25 mm. Preoperative screening for occult, extra-articular infection is vital, as pathogens often reside near hardware rather than within the joint. CT, ultrasound, and SPECT-CT are essential for assessing bone stock and identifying fluid collections. Dual-mobility cups effectively reduce dislocation rates to 0–3%. Functional scores improve significantly, though 10-year survivorship is approximately 86%.
Discussion:
Conversion THA provides substantial functional recovery but carries a 7-fold higher infection risk than primary THA. Success requires meticulous screening tailored to previous hardware sites and selecting femoral fixation based on bone quality and cortical defects. Specialised implants are essential for optimising long-term outcomes in this high-risk population.
Keywords
Introduction
With increased life expectancy and greater functional demands in the elderly, the incidence of fragility fractures rises annually. 1 Failed internal fixation of proximal femoral fractures is associated with significantly increased risks of morbidity and mortality, and poses a significant financial burden on the healthcare institution.2–5 The overall risk of failed internal femoral fixation ranges from 5% for pertrochanteric fractures to 41% for displaced femoral neck fractures. 5 Some of these patients may require conversion to total hip arthroplasty (THA) to improve their function, mobility and quality of life. This article describes the existing evidence on the preoperative workup and surgical management of patients undergoing conversion THA following failed proximal fracture fixation, and reports on the functional outcomes, implant survivorship and complications associated with the surgical management of this complex patient population.
Material and methods
2 authors [AM, EO] with expertise in searching medical literature ran independent searches across 3 databases [MEDLINE, EMBASE, Cochrane] for relevant studies published in English from 1990 onwards that addressed THA in adult patients who previously underwent proximal femur fracture fixation. Appendix A documents the MeSH terms and search strategy utilised. Following duplicate removal, 2 independent reviewers [AM, EO] assessed the titles, abstracts, and full texts of the identified studies. Any differences and discrepancies that existed between the 2 reviewers were resolved by a 3rd reviewer [BK] prior to data extraction. The screening process is summarised in the flowchart (Figure 1). Exclusion criteria were applied, with small case series of fewer than 10 patients excluded, as well as grey literature and papers published. The abstracts and bibliographies of included studies were reviewed for background material and to identify key clinical themes. Proposed key themes were then discussed and agreed by the authorship group. Relevant to each theme, one author then extracted data and entered this into a standardised data collection form, with another author subsequently reviewing for accuracy. The highest available level of evidence for each theme was the primary guide of theme narration.
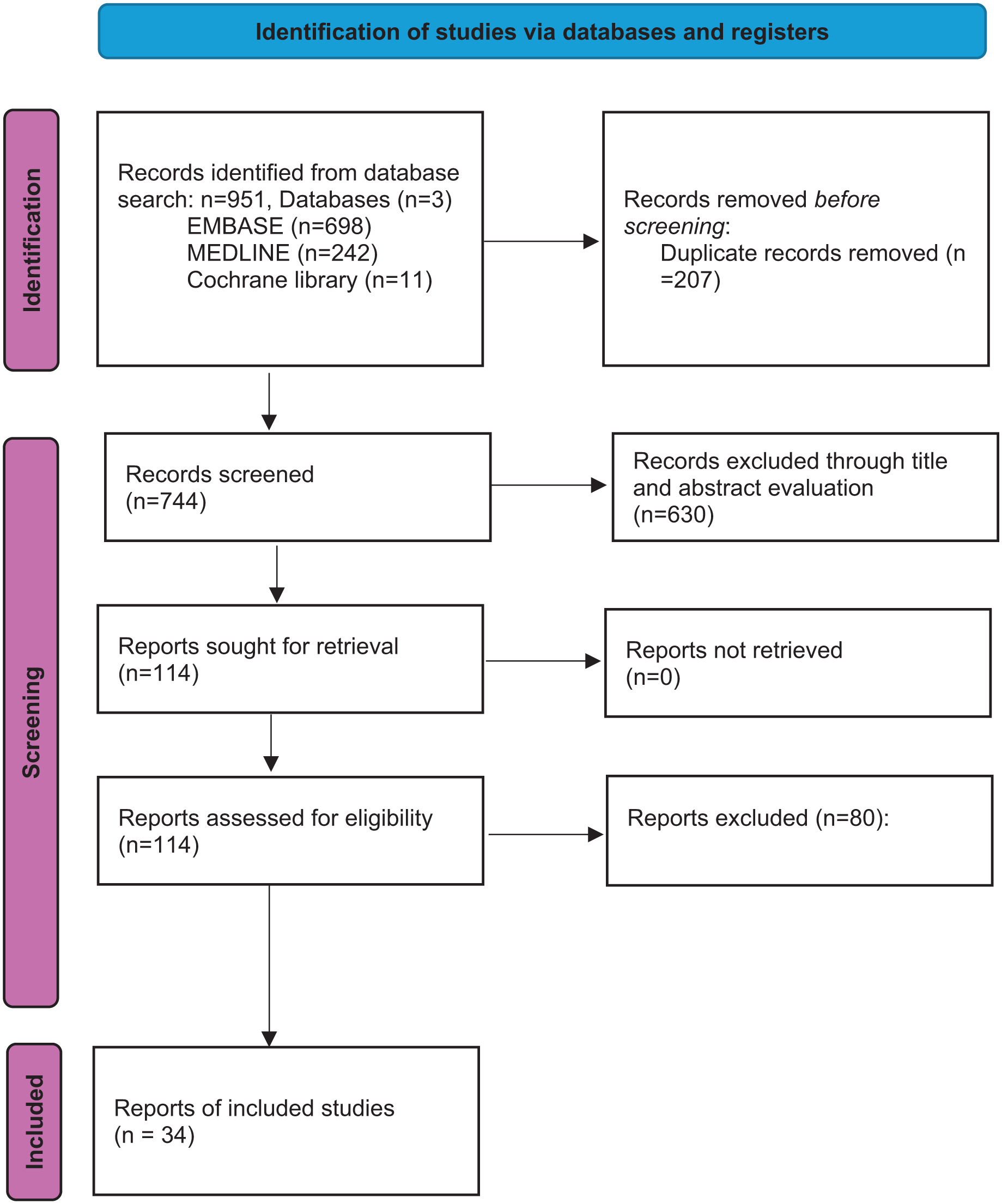
Flowchart illustrating the search strategy, number of records screened and included.
Results
Risk factors for fixation failure
It is well-established that the quality of the initial femoral fracture reduction and fixation is an important prognostic indicator that influences the long-term component survivorship and need for further revision surgery.5–7 Studies have reported several other risk factors femoral fixation failure. Kalsbeek et al. 6 performed a systematic review of patients with displaced femoral neck fractures, and reported that female sex (odds ratio [OR] 1.78; 95% confidence interval [CI], 1.26–2.52), smoking (OR 3.64; 95% CI, 1.68–7.91), age >50 years (OR 3.64; 95% CI, 1.68–7.91), inadequate fracture reduction (OR 2.28; 95% CI, 1.62–3.22) and fixation with cannulated screws or pins compared to fixed angle devices (OR 2.16; 95% CI, 1.03–4.54) were predictors of fixation failure. Garabano et al. 7 retrospectively analysed 251 consecutive patients with fixation failure after cephalomedullary nail fixation for intertrochanteric proximal femur fractures. The study found that female sex (p = 0.018), femoral neck angle (FNA) <125° (p = 0.003), a difference in FNA of 7.5° as compared to the contralateral hip on the lateral radiograph (p ⩽ 0.0001), superior (p = 0.0141) and anterior position (p ⩽ 0.0001) of the lag screw, and tip-apex distance (TAD) >25 mm (p = 0.016) were independent predictors of fixation failure.
Highest Level of Evidence: I
Early versus late failure
A bimodal incidence of femoral fixation failure is commonly described, with early failure defined as occurring within six months and late failure defined as occurring later than six months after surgery. Ballal et al. 8 analysed the outcomes of 216 patients who underwent proximal femoral nail fixation and reported that the quality of the initial fracture reduction was correlated to the risk of early failure. Suboptimal placement of the lag screw in the femoral head was another important prognostic factor for failure, with poor screw placement leading to an increased risk of screw cut-out or device breakage. The most common causes of late failures were fracture non-union or deep infections. Estrada et al. 9 noted that only Level III evidence exists in this area reviewed literature, reporting that early fixation failure was primarily caused by inadequate fracture reduction, whereas the leading cause of late failure was avascular necrosis of the femoral head. The risk of avascular necrosis was 58% with inadequately reduced fractures compared with 29% in fractures that were well-reduced. Accurate reduction and stable fixation are important surgeon-controlled risk factors that may help to increase survivorship and reduce the burden of conversion THA in patients with femoral fractures.
Highest Level of Evidence: III
Financial impact of failed femoral fixation
Failed femoral fixation places a significant burden on healthcare systems. Broderick et al. 5 reported that failure of fixation typically resulted in a two-fold increase in the length of hospital stay (LOS) at 67.1 days compared to 30 days for uncomplicated cases. Additional costs associated with revision surgeries can lead to an overall doubling of expenditure. The net costs for revision surgery average £20,095 compared to £8976 for uncomplicated cases, with additional costs for prolonged hospital stays and extra rehabilitation services. Patients who experience fixation failure often face extended periods of reduced function and loss of social independence, particularly in elderly patients, and referrals for enhanced social support are common. 5 The overall quality of life is also frequently diminished. At four months, the mean EQ-5D index score is lower at 0.49, compared to 0.66 in those with successful fracture healing. Failure of internal fixation necessitates conversion to THA when severe functional disability and persistent pain are present and the patient can safely undergo further surgery, otherwise, a poor prognosis can be expected. 10
Highest Level of Evidence: I
Preoperative workup
Exclusion of implant-related infection is critical before proceeding with conversion THA. Unlike revision of a primary arthroplasty, infections following failed internal fixation often reside in the soft tissues surrounding the hardware (extra-articular) rather than within the joint itself. This is particularly true for per- and subtrochanteric fractures, where the initial surgery is performed outside the hip capsule.
Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) remain standard screening tools, though their reliability varies for low-grade occult infections. Gittings et al. 11 reviewed 33 patients undergoing conversion THA and identified an 18% incidence of infection. They found that ESR > 30 mm/hour (OR 28.8) and CRP > 1 mg/dL (OR 11.5) were strong indicators of infection, with ROC curves showing a good fit (AUC 0.89).
While joint aspiration should be performed in suspected cases before commencing antibiotics, it may yield false-negative results in extra-articular failures where the infection localises around the hardware rather than the joint. Hemmann et al. 12 reported a 10% rate of positive intraoperative cultures in patients who had no clinical signs of infection preoperatively, highlighting the high rate of occult infections in patients undergoing conversion THA for failed osteosynthesis. In these cases, clinicians should consider ultrasound or MRI to identify periprosthetic fluid collections, such as haematomas or seromas, which may be more appropriate targets for aspiration than the hip joint.
Highest Level of Evidence: III
Preoperative imaging
Preoperative imaging following failed femoral fixation is essential for evaluating fracture reduction accuracy, secondary displacement, implant failure, and complications such as non-union or avascular necrosis. 13 While plain radiographs accurately reveal overt signs of failure like screw cut-out, metalware breakage, or fracture displacement, 13 advanced imaging is often required to assess more complex clinical questions.
Computerised tomography (CT) scans are particularly useful for assessing femoral and acetabular bone stock, the integrity of the greater trochanter, and the presence of non-union. 14 CT can also identify acetabular destruction caused by screw cut-out, which is a critical factor in deciding between standard or specialised acetabular components.
Given the high risk of occult infection in this population, MRI and ultrasound play a vital role in identifying fluid collections, such as haematomas or seromas, which may be missed on standard radiographs. 15 Ultrasound avoids the metal artifacts common in CT or MRI and is a valuable tool for guiding the aspiration of extra-articular liquid collections around nails or screws. 16 In equivocal cases, functional imaging such as SPECT-CT or anti-granulocyte scintigraphy may be considered to further differentiate between aseptic loosening and infection, though clinical evidence specific to conversion THA remains limited.
While three-dimensional (3D) CT-based imaging can assist in planning implant size and version in cases of distorted anatomy, the primary focus of preoperative imaging should be the evaluation of bone loss, non-union, and the exclusion of infection to ensure the stability of the subsequent reconstruction.
Highest Level of Evidence: II
Hardware removal
Removing hardware from the index femoral fixation may be surgically challenging and is associated with increased operative times, intraoperative blood loss, and iatrogenic fractures. Intraoperative fluoroscopy may be used to guide the removal of existing metalwork, intramedullary reaming and component fixation. 17
Highest Level of Evidence: III
Approach
Satisfactory outcomes have been reported for conversion THA using the anterolateral, direct anterior and posterolateral approaches.18–20 Crockatt et al. 21 demonstrated that an anterior approach is a safe and effective technique for simple THA conversion, such as in patients who had prior percutaneous screw fixation, but commonly requires a separate incision to facilitate implant removal. Alternatively, the posterior approach can incorporate previous incisions for removal of larger implants in complex conversion cases.
Single versus 2-stage conversion THA
Single-stage conversion THA is often preferred for cases of failed internal fixation in the absence of infection. The main advantages of a single-stage procedure are reduced anaesthetic risks and decreased postoperative morbidity compared with 2 separate surgical procedures. Earlier mobilisation after surgery may help to reduce the risks associated with prolonged immobility, and single-stage conversion THA is associated with reduced cost to healthcare systems compared with 2-stage conversion THA.
Despite this, it is important to consider the risk of positive intraoperative cultures despite a negative preoperative workup for infection. Hemmann et al. 12 retrospectively reviewed a series of 58 patients with failed fixation who underwent single-stage conversion THA. Patients had no clinical signs of infection and the mean time between internal fixation and conversion to THA was 3.8 ± 7.5 years. Intraoperative microbiological analysis was positive in 10% of cases and these patients all required six weeks course of antibiotics. There is very limited evidence as to the role of single-stage conversion THA in the presence of confirmed deep infection. Klatte et al. 22 evaluated single-stage conversion THA for failed fixation with concurrent deep infection. Surgery included an extensive debridement and chemical lavage. In their short series, 16 patients were followed up with an average follow-up period was 12 years (range 2–18 years). Although no subsequent PJI was noted, 4 patients experienced dislocations, with three patients needing further surgery.
2-stage revision THA is a well-recognised procedure. Articulating spacers may be used after the first-stage to enable movement around the hip joint, maintain muscle function and allow immediate mobilisation. 23 Furthermore, insertion of an antibiotic loaded spacer during a 2-stage revision for PJI may reliably eradicate infection and improve clinical function, including the spacer phase. 24
Van Den Kieboom et al. 25 reviewed outcomes in 40 patients undergoing two-stage conversion THA for failed fixation around hip and knee versus 80 2-stage revision THA and TKA for non-traumatic periprosthetic joint infections. The overall failure rate for conversion THA following fracture fixation was 42.5%, compared with 21.3% for non-traumatic periprosthetic joint infections (p = 0.03). Reinfection was the most common indication for failure, occurring in eight out of 27 patents in the failed fixation group (29.6%) versus 9.1% in the non-traumatic periprosthetic joint infection group.
Highest Level of Evidence: IV
Implant choice and cementation
Performing conversion THA after fixation failure is associated with higher rates of implant dislocation owing to distorted bony anatomy and muscle compromise. Dual-mobility (DM) implants may reduce this risk and increase the overall stability of the hip articulation. Boulat et al. 26 conducted a single-centre, retrospective study of all patients who underwent THA with a DM cup following failed internal fixation of proximal femur fractures. The study included 33 patients (4 men and 29 women) with a mean age of 74 years. The mean Postel-Merle d’Aubigné (PMA) score improved from 6.3 ± 2.8 to 14.8 ± 2.6 (p < 0.001) and the Harris Hip Score (HHS) increased from 30.27 ± 15.7 to 80 ± 13.8 (p < 0.001) at 44 ± 24 months after surgery. However, the overall complication rate was 21%, which included intraoperative femoral fractures and postoperative dislocations and infection. Of note, the overall dislocation rate in THA with DM cups following failed femoral fixation was only 3%.
Favreau et al. 27 conducted a single-centre retrospective review of 40 patients with a mean age of 77 years undergoing THA with DM cups after femoral fixation failure. Visual Analog Scale (VAS) improved from 7.9 ± 1.6 to 1.35 ± 1.5 (p < 0.0001), Harris Hip Score improved from 20 ± 11.8 to 78 ± 12.3 (p < 0.0001) and PMA score improved from 4.7 ± 2.9 to 14.6 ± 2.1 (p < 0.0001). The overall complication rate was 22%, but none of the study patients had dislocations. Another retrospective study by Assi et al. 28 included 31 patients with a mean age of 71 years undergoing THA using DM cups for failed femoral fixation. The mean modified Harris Hip Score (mHHS) at was 92.9 ± 9.1 and there were no cases of dislocation or aseptic loosening at most recent follow-up. 1 patient developed septic loosening of the implant, which was managed with a 2-stage revision THA. In total, 71% of the patients described their operated hip as a "forgotten hip", indicating a high level of satisfaction and functional recovery.
The use of DM cups should be taken into consideration in case of THA after femoral fixation failure.
Both cemented and cementless implants are used for conversion THA. Moon et al. 29 carried out a retrospective cohort analysis of 96 patients undergoing cementless THA after failed femoral fixation. All femoral stems demonstrated good integration, with 78 cases showing bony ingrowth and 18 cases with stable fibrous ingrowth at a mean of 6.3 years (range 3–13 years) follow-up. Shi et al. 30 retrospectively analysed 31 patients who underwent conversion THA following failed internal fixation of intertrochanteric fractures. The authors reported the mean Harris Hip Score increased from 28.4 points to 85.6 following surgery, and all stems showed radiographic evidence of osteointegration.
Morsi et al. 31 conducted a retrospective chart review of 107 patients undergoing conversion THA with cemented femoral prostheses. Screw holes from the metalwork removal were blocked with bone cement to achieve proper cementation. The mean preoperative Harris Hip Score was 28 and improved to 89.3 postoperatively. Overall, 102 of the 107 patients had good radiographic cement fixation, and none of the study patients had periprosthetic fractures, component loosening or revision surgery at latest follow-up.
The choice between cemented and cementless femoral fixation depends on the quality of the femoral bone stock and the presence of diaphyseal deformities.
Cementless fixation enables long-term biological stability through osseointegration. However, surgeons must be cautious as existing screw holes from previous hardware may act as stress risers, increasing the risk of intraoperative fractures during stem insertion.
Cemented fixation provides immediate mechanical stability, particularly in elderly patients with osteoporotic bone or wide canals where biological ingrowth potential is limited. 32 This method is highly effective for managing cortical defects, as surgeons can block existing screw holes with bone cement to ensure a uniform mantle and prevent cement egress. Cemented stems offer a reliable and cost-effective treatment option in cases where pre-existing pathology or significant bone voids compromise the femoral host environment.
Highest Level of Evidence: III
Functional outcomes
The functional outcomes of conversion THA following failed internal fixation are highly variable owing to heterogeneity between studies in fracture types, the patient profiles, pre-existing comorbidities, quality of fracture reduction and fixation, and surgical techniques for conversion THA. Mahmoud et al. 33 compared THA as a salvage procedure after osteosynthesis versus primary THA for a fractured neck of the femur in a review and meta-analysis that included seven case-controlled studies and four case series. In total, 558 patients (568 THAs) were reviewed with an age range of 30 to 96 years and follow-up period from 6 to 78 months. The study reported comparable EuroQoL (EQ-5D) scores and HHS between the 2 treatment groups. 1 of the included studies used the Merle d’Aubigne hip score and demonstrated better scores for primary THA compared with conversion THA following failed internal fixation. Morice et al. 34 examined the outcomes of 59 conversion THAs performed after failed femoral fixations and reported that conversion THA after intracapsular fractures had better HHS (78.7 vs. 65.6 respectively, p < 0.05) as compared to extracapsular fractures. With an endpoint of revision with implant change, the overall 40-month survival was 97% (95% CI, 0.62–0.85) for the intracapsular fractures and 84% (95% CI, 0.39–0.75) for the extracapsular fractures (p < 0.05).
Highest Level of Evidence: I
Implant survivorship
Implant survivorship is a key outcome in conversion THA following failed femoral fixation and has already been mentioned in some of the studies discussed above. Yu et al. 35 conducted a retrospective review of 120 conversion THAs following failed primary fixation of proximal femoral fractures at a mean follow-up period of 10.2 years (range, 8 to 12 years). Kaplan-Meier survival analysis showed implant survival rate was 95% (95% CI: 93–97%) at 5 years, 89% (95% CI, 86–92%) at 8 years, and 86% (95% CI, 83–89%) at 10 years. In addition, the HHS improved postoperatively, peaking in the first year after conversion THA revision and gradually decreasing thereafter. Similarly, Lu et al. 36 reviewed outcomes in 370 THAs for failed internal fixation of femoral neck fractures with a mean follow-up of 6 years. Kaplan-Meier survival analysis showed the survival rate was over 93% all study patients. Schmitz et al. 37 carried out a retrospective analysis on 4310 salvage-THAs, comparing these with primary THA. Kaplan-Meier survival analysis showed no statistically significant difference in revision rates for salvage-THAs and THAs for fractures (hazard ratio [HR] 1.0; 95% CI, 0.7–1.3), though both procedures had higher revision rates compared with THAs for osteoarthritis (HR 1.3; 95% CI, 1.0–1.5 for conversion THAs and HR 1.3, 95% CI, 1.1–1.7 for THAs for fractures). Furthermore, the 5-year revision rates were highest for salvage-THAs 5.0 (95% CI, 4.4–5.8), compared with 4.5% (95% CI, 4.1–5.0) for THA fractures and 3.1% (95% CI, 3.0–3.2) for THAs for osteoarthritis.
Highest Level of Evidence: III
Discussion
Complications
In a systematic review and meta-analysis, Mahmoud et al. 33 found an increased overall risk of complications (risk ratio 3.15; 95% CI, 1.39–7.11; p = 0.006) in conversion THA compared with primary THA for intracapsular femoral neck fractures. Conversion THA after failed femoral fixation was associated with an increased risk of infection (risk ratio 7.05; 95% CI, 2.08–23.86; p = 0.002), early dislocation (risk ratio 1.46; 95% CI, 1.46–10.25; p = 0.006) and peri-prosthetic fracture (risk ratio 5.55; 95% CI, 1.53–20.23; p = 0.009) compared with primary THA for intracapsular fractures of the femoral neck. Archibek et al. 38 conducted a retrospective review of 102 patients undergoing THA for failed internal fixation and found an overall complication rate of 11.8% (4.9% dislocations, 3.9% periprosthetic fractures, 2% haematomas, and 1% infection rates), and 7 patients required revisions or reoperations at mean 3.2 years follow-up. Hung et al. 39 reviewed outcomes in 315 patients undergoing conversion THA for failed internal fixation versus THA for hip osteoarthritis, and reported conversion THA for failed internal fixation was associated with an increased risk of early dislocations (9.5% vs. 1.9%, p = 0.002), reoperation (10.5% vs. 3.8%, p = 0.019) and increased need for revision surgery (5.7% vs. 0.5%, p = 0.003) compared with THA for hip osteoarthritis.
Conversion THA after fixation failure is associated with an increased risk of complications, and patients should be counselled accordingly before surgery.
Highest Level of Evidence: I
Limitations
The literature included in this review ranges from Level I (systematic review and meta-analysis) to Level IV (large case series). Levels of evidence are highlighted throughout and heterogeneity inevitably exists within and between subject headings. Lower levels of evidence are vulnerable to bias and carry the inherent limitations of retrospectivity. This review highlights gaps of knowledge in that topic, thus strong recommendations for treatment strategies can hardly be given.
Conclusion
Early failure following proximal femoral fixation is commonly associated with degree of dislocation or complexity of the fracture, suboptimal reduction and operating technique and infection, while late failure is usually secondary to intolerable loss of function, posttraumatic arthritis, avascular necrosis, fracture non-union or infection. Preoperative workup should include careful clinical examination, blood tests and in some cases hip aspiration to rule out possible infection. While 3D imaging assists in planning, surgical success depends on addressing bone stock and choosing fixation (cemented or cementless) based on femoral quality and cortical integrity. Single-stage revision conversion THA is preferred for cases with no evidence of infection and when hardware removal is not too complex, eg in THA after failed fixation of femoral neck fractures.
The use of dual-mobility implants should be considered to reduce the risk of dislocation. There is no clear recommendation for the use of cemented or cementless stems. Conversion THA following failed femoral fixation is associated with improvements in functional outcomes, though overall survivorship is reduced, and the risk of complications is increased compared with primary THA for osteoarthritis. Further research is needed for better understanding of the risk factors for failure, and to provide more robust evidence for the surgical management of this complex patient population.
Footnotes
Appendix A
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
