Abstract
Background:
Periacetabular osteotomy (PAO) has become a popular procedure for re-orientation of the acetabulum in patients with a developmental pathomorphology. Since its first description by Reinhold Ganz in 1988, many institutions worldwide have adopted the procedure for the treatment of developmental hip dysplasia (DDH) and have subsequently reported their results. The aim of this study was to provide a meta-analysis of the likelihood of long-term survival of a dysplastic hip after PAO.
Methods:
A systematic literature review was conducted using Medline, Cochrane and “Web of Science” databases to identify articles reporting survival estimates for PAO in patients with DDH. To be included in the analysis, studies had to include patient cohorts aged <40 years, with Osteoarthritis grade < Tönnis III and no form of neuromuscular dysplasia. Adjustment for cohort overlap was performed. Quality assessment included level of evidence (LOE) according to the oxford center for LOE criteria and the “Methodological index for non-randomized studies (MINORS)”. After data extraction, a random-effects meta-analytical model was applied to provide weighted mean estimates of survival at 5 years, 10 years, 15 years and 20 years.
Results:
Nine relevant articles included 2268 dysplastic hips that underwent PAO in 9 institutions. Of the included studies, 5 presented level III evidence and 4 presented level IV evidence. The MINORS score was 11 for 3 studies, 12 for 4 studies and 13 for 2 studies. The 5-year survival after PAO was 96.1% (95% CI, 94.9–97.3), the 10-year survival was 91.3% (95% CI, 87.7–94.8), 15-year survival 85.0% (95% CI, 78.9–91.1), 20-year survival 67.6% (95% CI, 53.9–81.3).
Conclusions:
The results provide a representative survival estimate of a dysplastic hip after PAO based on global evidence. This should provide clinicians and patients with an adequate reflection of prognostic expectations after this kind of surgery.
Keywords
Introduction
The pathomorphology of hip dysplasia and its prognostic impact on the hip has defined an entire field of reorientation osteotomies around the acetabulum throughout the last decades.1–3
In 1988, Reinhold Ganz reported a technique for acetabular reorientation, attempting to address issues facing prior osteotomies. 4 He referred to his procedure as periacetabular osteotomy (PAO). The technique was based on the concept of maintaining the integrity of the posterior column of the hemipelvis. The advantage was seen in simplicity of reorientation due to freedom of the mobile fragment from ligamentous restraints that remain attached to the intact posterior column, and the improved primary stability due to the increased contact with surrounding bone. 5
Since its first description, the procedure gained rapid recognition within the orthopaedic community. The number of articles dealing with PAO have increased exponentially throughout the years, with >100 articles published alone last year.
Several studies investigated the outcome after PAO upon which the success of the procedure is frequently defined.6–8 However, a pooled analysis of the long-term outcome of PAO regarding survivorship has not yet been performed.
Given the frequent encounter with the question of how long a dysplastic hip is likely to survive after PAO, the aim of the study was to: (1) systematically review the literature for articles reporting the survivorship of a dysplastic hips after PAO; and (2) provide pooled survival estimates based on weighted means.
Methods
Search strategy
A systematic literature review was conducted using the 3 databases Medline (PubMed), “web of Science” and Cochrane databases. No time or language restrictions were made. The search term used was “periacetabular osteotomy”. Two authors screened titles, abstracts and full-texts according to PRISMA guidelines. Duplicates were removed. The reference lists of included articles were screened to identify potentially relevant articles. All articles citing the very first description of the technique, 4 were screened to capture potentially missed articles.
Eligibility criteria
Articles were considered eligible if: (1) the PAO technique performed was based on bony cuts as described by Ganz; (2) The only indication was hip dysplasia with a lateral centre-edge angle (LCE) of <25°; (3) the mean age of included patients was <40 years; (4) studies reported a mean follow-up of ⩾5 years; and (5) articles included a survival analysis based on pre-defined endpoints with corresponding confidence intervals (CIs) or standard error (SE).
Excluded articles included reviews, case reports, studies with vague endpoint definitions and articles that did not provided a Kaplan-Meier survival estimate or an exact timepoint of failure for each of the hips. Cohort overlap was avoided by only considering 1 article for every institution per time point.
Data extraction
Extracted data included the number of included patients, the mean follow-up interval of the study, survival information with corresponding confidence intervals at 5 year, 10 years, 15 years, and 20 years.
Quality assessment
All studies were assessed independently for quality by 2 epidemiologically-trained authors. Disagreements were solved by consensus with the inclusion of a third author. Quality assessment included level of evidence (LOE) according to the Oxford center for LOE criteria and the “Methodological index for non-randomized studies (MINORS)”. 9 The MINORS score consists of 12 items that allows for characterisation of the methodological and scientific value of published articles. 9 The score showed a high overall reliability. 9
Synthesis of results and statistical analysis
Characteristics of included studies were tabulated. The endpoint of the study was defined as all-cause revision to hip arthroplasty. Standard error was calculated from confidence intervals of individual studies and was used to weigh the studies in a random-effects meta analytical model, assuming that survivorship approximated risk. STATA version 16.1 was utilised for analysis.
Results
From a total of 990 potentially relevant articles, 14 articles fulfilled eligibility criteria. After exclusion of overlapping cohorts, 9 relevant articles were included in the meta-analysis (Figure 1). The studies included 2268 dysplastic hips that underwent PAO in nine institutes. Of the included studies, 5 presented level III evidence and 4 presented level IV evidence. Given a maximum of 16 points, the MINORS score was 11 for 3 studies, 12 for 4 studies and 13 for 2 studies (Table 1).
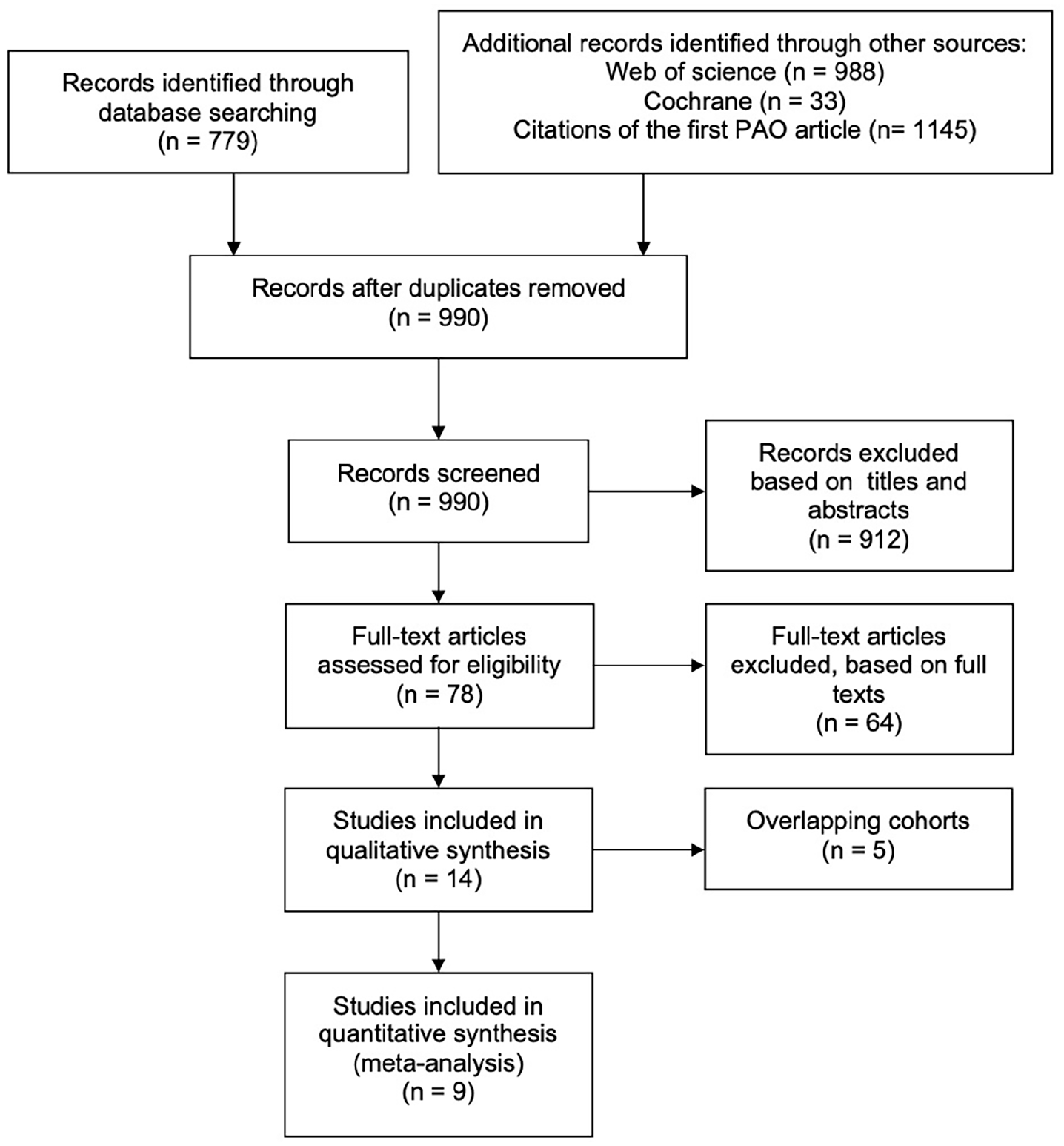
Flow chart representing the process of article selection.
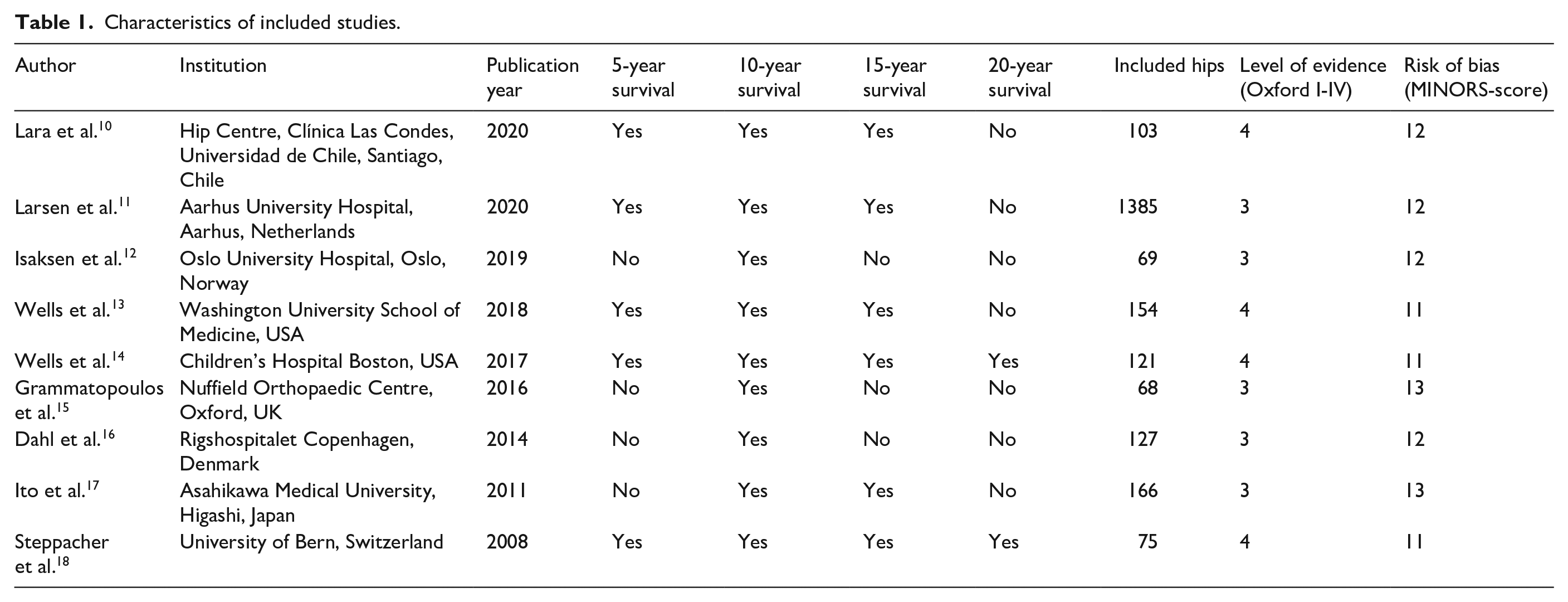
Characteristics of included studies.
5-year survival
There were 5 articles reporting the 5-year survival after PAO with low heterogeneity (τ2 0.0, I2 0.0%) as shown in Figure 2. The weighted 5-year survival estimate was shown to be 96.1% (95% CI, 94.9–97.3) (Figure 2).
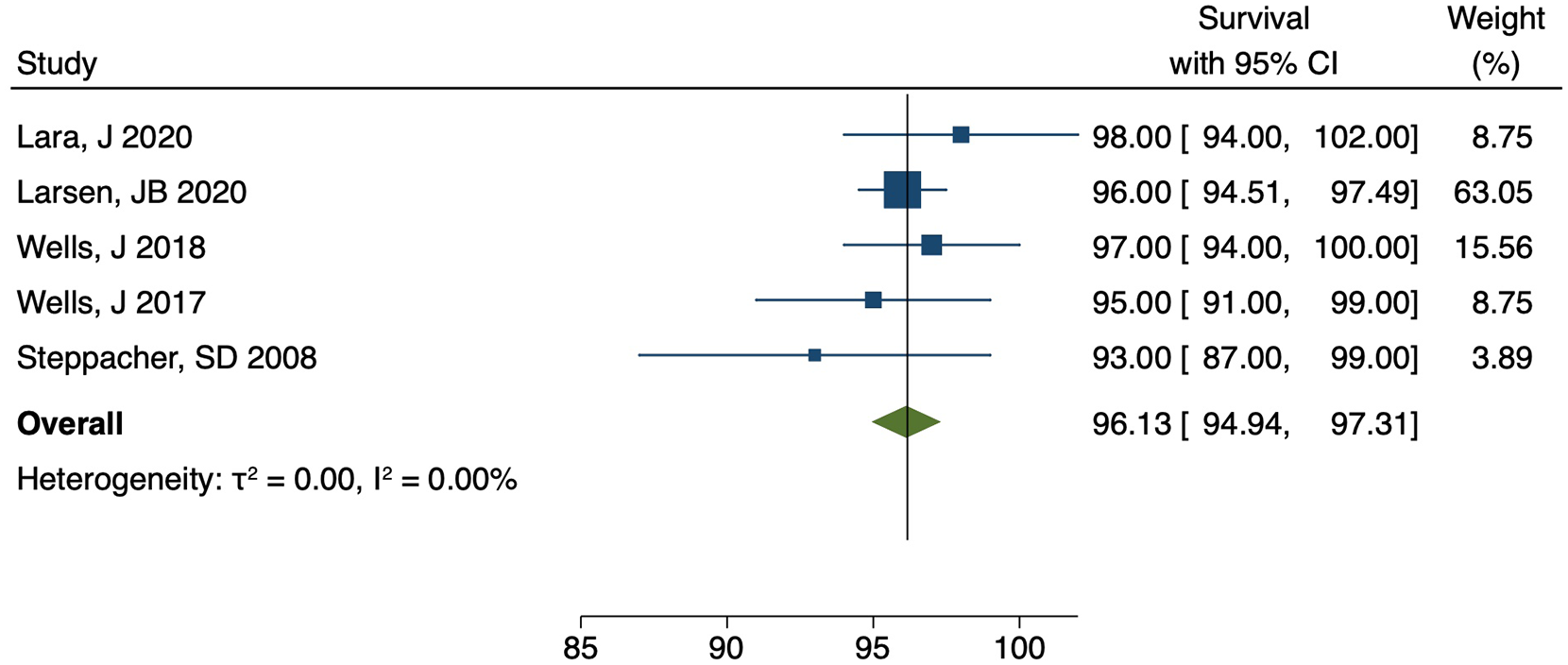
Meta-analysis of the 5 articles reporting the 5-year survival after PAO demonstrating a low heterogeneity (τ2 0.0, I2 0.0%). The weighted 5-year survival estimate is 96.1% (95% CI, 94.9–97.3).
10-year survival
There were 9 articles reporting 10-year survival with some degree of heterogeneity (τ2 17.9, I2 78.4%) as shown in Figure 3. The weighted 10-year survival estimate was shown to be 91.3% (95% CI, 87.7–94.8) (Figure 3).
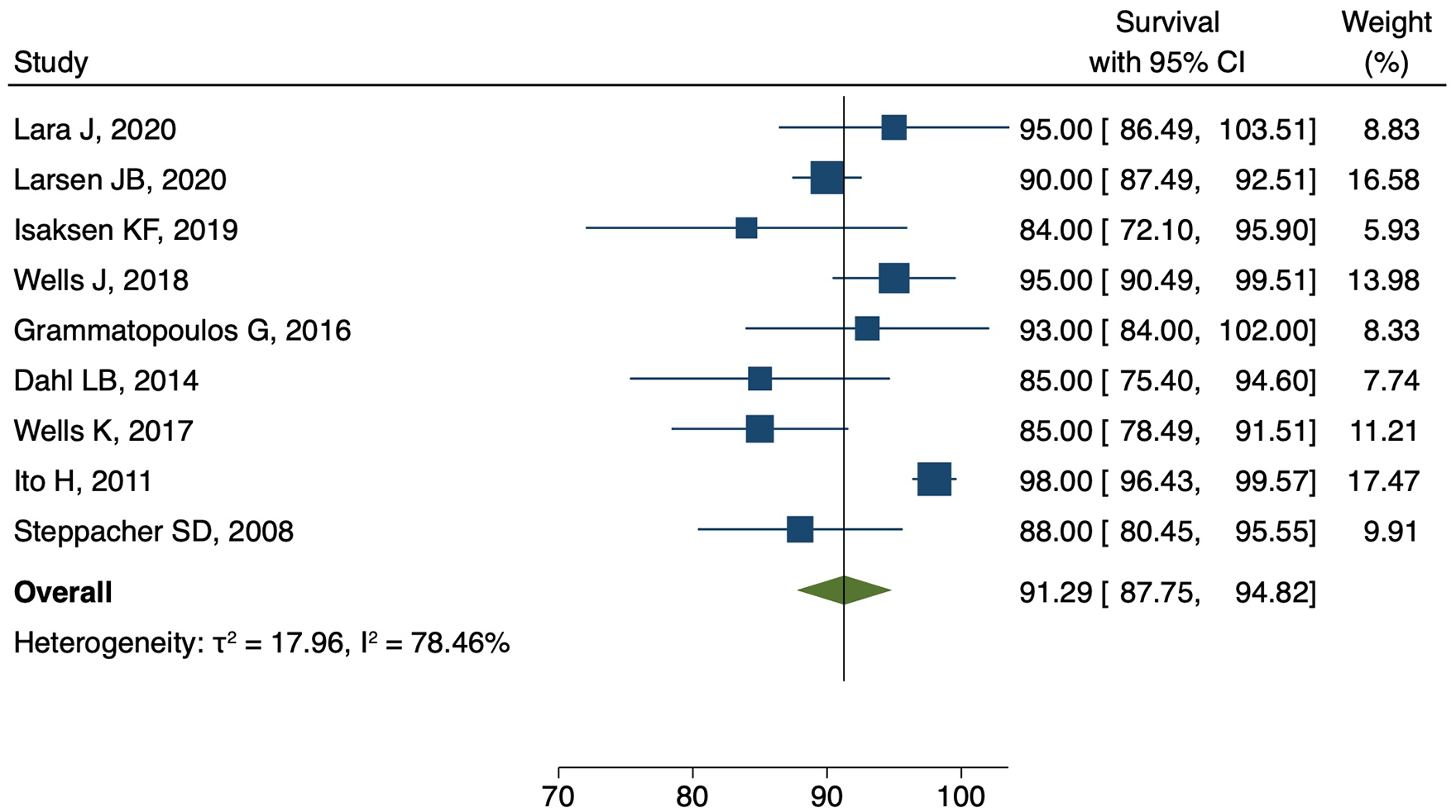
Meta-analysis of the nine articles reporting the 10-year survival after PAO demonstrating some degree heterogeneity (τ2 17.9, I2 78.4%) The weighted 10-year survival estimate is 91.3% (95% CI, 87.7–94.8).
15-year survival
There were 6 articles reporting 15-year survival with some degree of heterogeneity (τ2 39.0, I2 78.1%) as shown in Figure 4. The weighted 15-year survival estimate was shown to be 85.0% (95% CI, 78.9–91.1) (Figure 4).
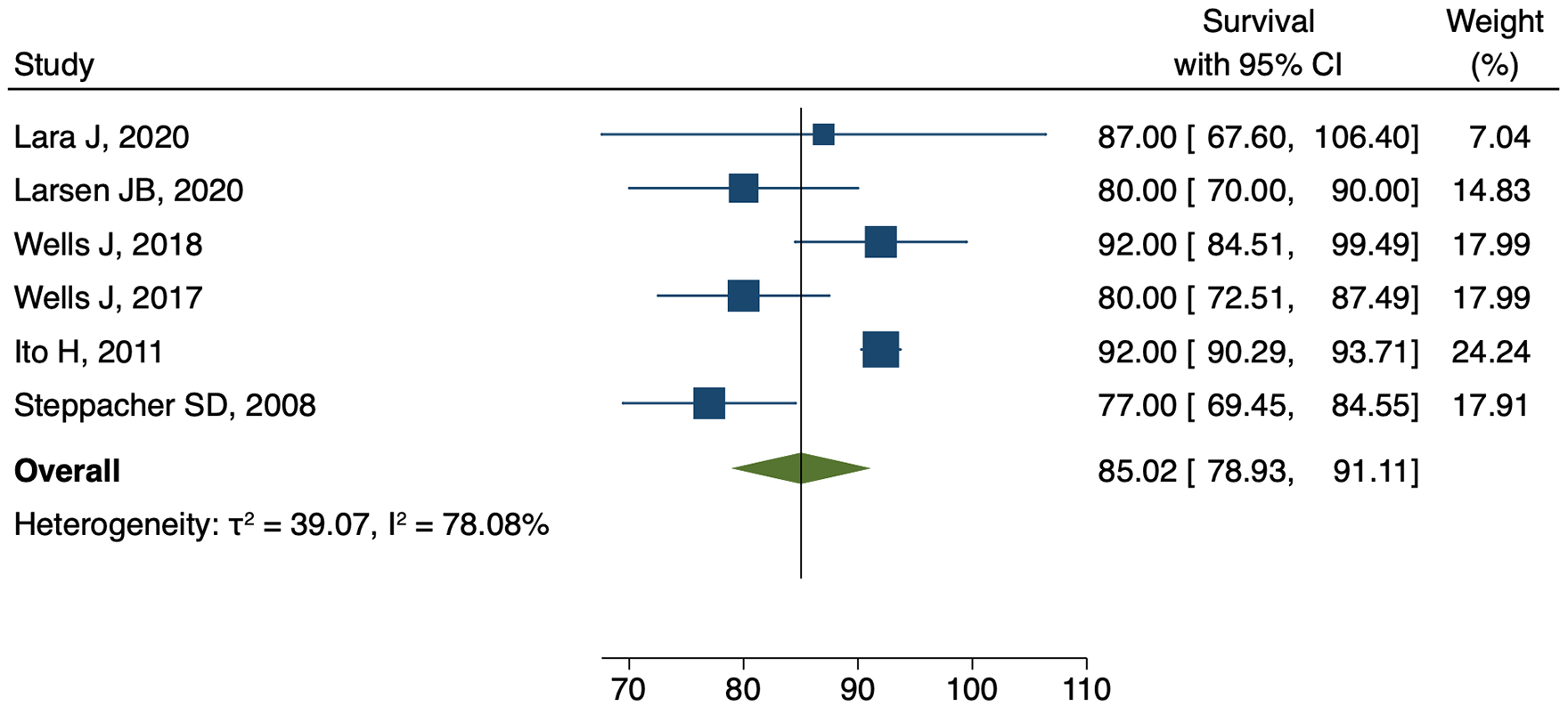
Meta-analysis of the 6 articles reporting the 15-year survival after PAO demonstrating some degree heterogeneity (τ2 39.0, I2 78.1%). The weighted 15-year survival estimate is 85.0% (95% CI, 78.9–91.1).
20-year survival
There were 2 articles reporting 20-year survival demonstrated in Figure 5. The weighted 20-year survival estimate was 67.6% (95% CI, 53.9–81.3).
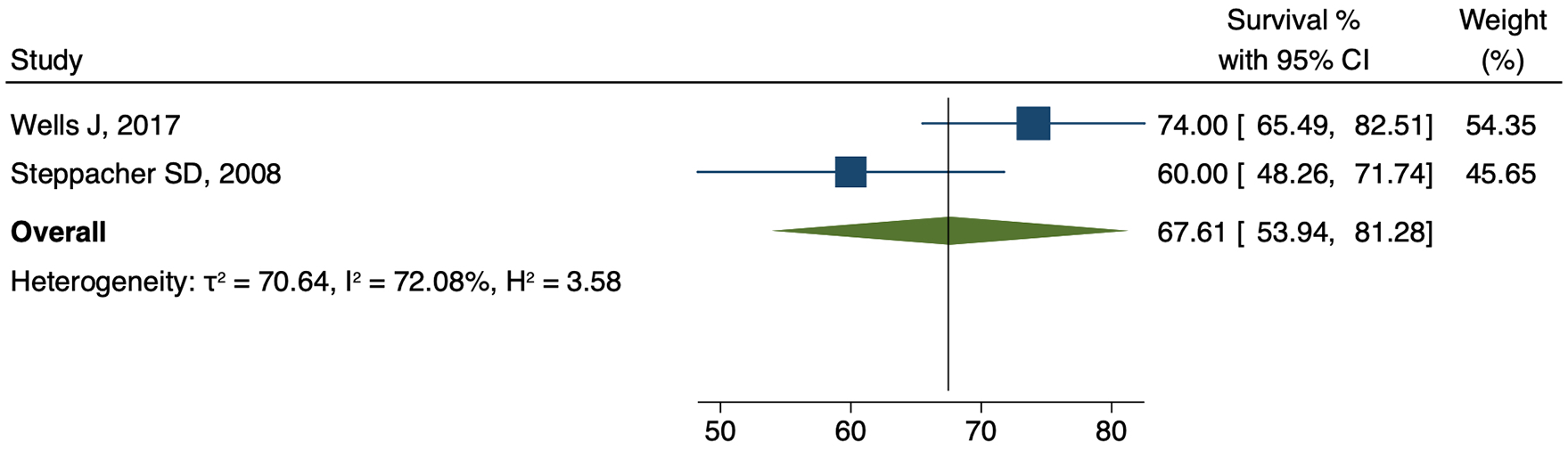
Weighted estimate of the 2 articles reporting 20-year survival. The 20-year survival estimate is 67.6% (95% CI, 53.9–81.3).
Figure 6 provides a graphical illustration of the weighted survival estimates and 188 confidence intervals per time interval.
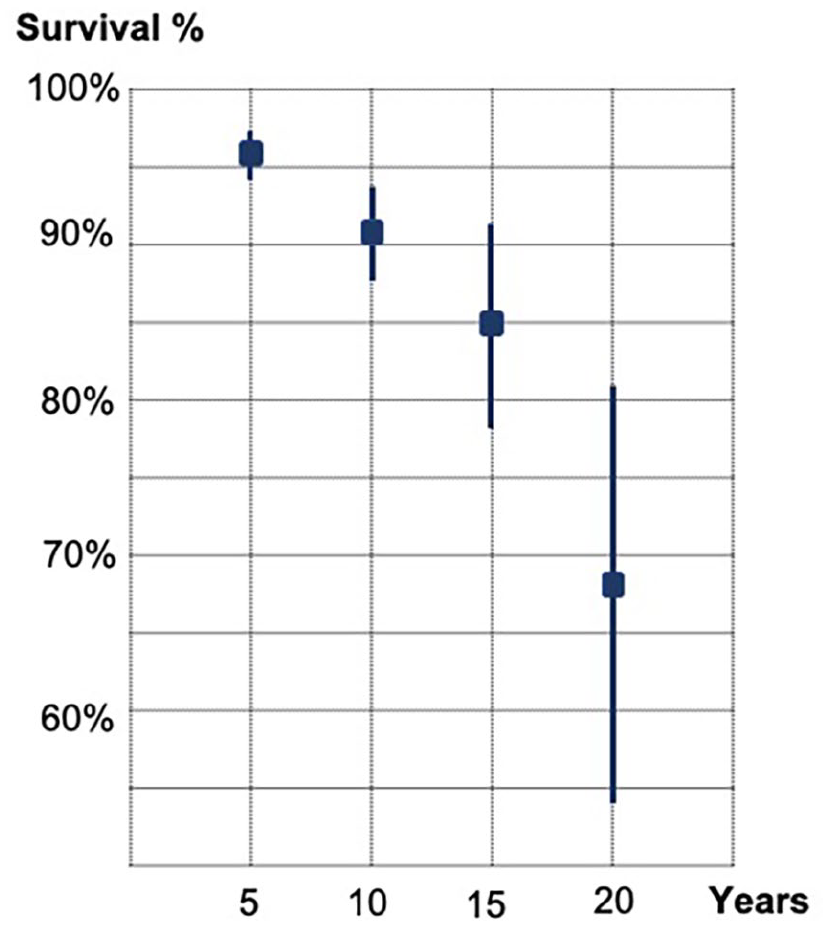
Graphical illustration of the weighted survival estimates and confidence intervals per time interval.
Predictors of outcome
Predictors of good outcome were shown to be preoperative osteoarthritis grade Tönnis <2, 16 postoperative centre-edge angle between 30° and 40°, 6 high postoperative joint congruence. 6
Predictors of bad outcome were shown to be preoperative arthritis grade Tönnis ⩾2, 16 preoperative joint incongruency, postoperative pincer impingement due to excessive postoperative femoral head coverage. 13
Discussion
The most important findings of this study are reflected in the pooled survival estimates of the dysplastic native hip after undergoing a PAO procedure for reorientation of the acetabulum. The overall likelihood of a hip surviving 5 years after PAO is 96%, 10 years 91%, 15 years 85%, and 20 years 68%.
During preoperative workup and preparation, it is of upmost importance to outline the expected prognosis of the hip after surgery to every patient. This highlights the clinical relevance of the findings of the current study. Citing an estimate of weighted means of a meta-analysis could provide a more accurate demonstration of expected results, compared to citing a single study. Furthermore, it was observed that age and degenerative changes present 2 repetitively reported factors influencing survival. This underlines the importance of narrowing indications for optimisation of results.
Historically, the assumption that hip dysplasia, if left untreated, would lead to osteoarthritis of the hip, was accepted due to the high abundance of hip dysplasia in arthritic hips. 19 It became a fundamental concept in hip surgery that osteoarthritis of the hip is rarely idiopathic and is most likely resultant to an underlying pathomorphological condition such as dysplasia.19–22 Therefore, the general therapeutic trend aimed towards correcting the deformity in the early times, leaving only a minority of studies that report the natural course of a dysplastic hip.22,23 It is therefore difficult to verify the power and prognostic effect of a PAO on the hip based on the current literature. Furthermore, due to the lack of long-term survival results of different types of acetabular osteotomies for the skeletally mature, it is difficult to compare PAO to different types of osteotomies such as the triple osteotomy.
It is important at this juncture to underline the fact that the studies in this analysis include early cohorts undergoing PAO before recognition of influential factors determining the success of the PAO procedure. Applying the current knowledge during patient selection may allow for even better results than the ones illustrated here. These include age at surgery, preoperative Merle d’Aubigné and Postel score, positive preoperative anterior impingement test, preoperative limp, osteoarthrosis grade, and the postoperative extrusion index.18,24 Further limitations include hip arthroplasty as an endpoint. Although this represents a statistically desirable binary measure, it does not reflect osteoarthritis or pain progression. However, considering pain or osteoarthritis progression would have further increased the heterogeneity of the study and weakened the outcome of this analysis. Furthermore, femoral pathology may have accounted to some degree of heterogeneity between studies. It should also be mentioned that each of the institutions treated different patient populations that surely showed some degree of demographic variation. Although the aim was improvement of femoral head coverage, a true definition of that aim was lacking. Hence, intraoperative assessment of coverage was not a defined constant amongst the studies.
There were only 2 studies reporting 20-year follow-up results of PAO. One reported 60% survival, the other 74% survival.18,14 The truth could lie somewhere in between. It is difficult to determine the exact reason for the discrepancy between both reports. Steppacher’s article reported the first ever treated population, the experience with the procedure was therefore the very first after its description, therefore, the prognosis of a patient treated with todays current knowledge is likely to be better.18,14
In conclusion, the results of this meta-analysis allow for a representative overall prognostic survival estimate of a dysplastic hip after PAO, based on available evidence. This should provide clinicians and patients with an adequate reflection of prognostic expectations.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
