Abstract
Glaucoma is a leading cause of irreversible blindness worldwide. There is no current cure for glaucoma, and it is managed by lowering intraocular pressure, a major modifiable risk factor. Nutraceuticals have long been studied to protect retinal ganglion cells and the optic nerve from degeneration by targeting the metabolic and neurodegenerative aspects of glaucoma, and even contributing to pressure lowering. A range of vitamins, minerals and nutraceuticals have been and are undergoing investigation for glaucoma. Compounds such as NAD-boosting supplements, antioxidants, and combination therapies can potentially support retinal ganglion cell metabolism and reduce oxidative stress, leading to healthier neurons to preserve vision for longer. However, varying levels of evidence exist to support the use of nutraceuticals in glaucoma. Herein lies a comprehensive review on the latest research evidence for 35 different vitamins, minerals, and nutraceuticals, their proposed mechanism of action, and reported effects on retinal ganglion cell health and in people with glaucoma.
Keywords
Introduction
Glaucoma is a common neurodegenerative disease characterized by the degeneration of retinal ganglion cells and their axons, leading to characteristic structural changes at the optic nerve head and corresponding visual field loss. Despite being a multifactorial disease with a complex etiology, the unifying feature of glaucoma is retinal ganglion cell degeneration, which often results in irreversible blindness if left untreated. Importantly, while elevated intraocular pressure (IOP) is a well-established risk factor and the only available treatment target, it is neither necessary nor sufficient for the development of glaucoma, as evidenced by the existence of normal-tension glaucoma and the observation that many patients continue to progress despite achieving target IOP levels.1,2
The prevalence of glaucoma increases with age, making it a significant global health burden as populations age. It is estimated that the number of individuals affected by glaucoma will continue to rise, with substantial socioeconomic impact due to vision loss and associated disability.1,3 Age is the most prominent risk factor, but genetic predisposition, vascular dysregulation, and systemic metabolic dysfunction have also been implicated in disease susceptibility and progression. Recent genomic and metabolomic studies have revealed that mitochondrial dysfunction and impaired energy metabolism are central to the vulnerability of RGCs in glaucoma, highlighting the importance of bioenergetic support as a therapeutic target.4–6
Current clinical management of glaucoma is centered on lowering IOP through topical medications, laser therapy, or surgical interventions. While these approaches are effective in slowing disease progression in many patients, up to 40% still develop significant vision loss or blindness in at least one eye over their lifetime, underscoring the need for additional therapeutic strategies. 2 Notably, IOP-lowering therapies do not directly address the underlying neurodegeneration of retinal ganglion cells, and there are currently no clinically approved neuroprotective treatments that target the retina or optic nerve directly.
Diagnosis of glaucoma relies on a combination of structural and functional assessments, including optical coherence tomography (OCT) to measure retinal nerve fiber layer thickness, and standard automated perimetry to detect visual field defects. However, these modalities typically detect damage only after substantial RGC loss has already occurred. Studies suggest that up to 28% of retinal ganglion cells may be lost before early visual field defects become apparent. 7 Advances in imaging, home-based visual field monitoring, and artificial intelligence-assisted analysis are being developed to improve early detection and risk stratification, but challenges remain in predicting individual disease trajectories. Although glaucoma is highly hereditary, monogenic glaucoma is rare, with polygenic risk more at play. Polygenic risk scores are being developed which may help categorize patients into high and low risk bins. Whilst promising, research on polygenic risk scores remains in the experimental stage and requires validation across ancestrally diverse populations and longitudinal cohorts to determine whether their predictive utility can effectively inform early intervention and management of high-risk individuals.
Given the limitations of current therapies and diagnostic tools, there is a growing focus on developing new treatments that target the metabolic and neurodegenerative aspects of glaucoma. Research has identified that retinal ganglion cells exist in a state of metabolic vulnerability, particularly with advancing age and/or in the presence of elevated IOP.4,8 Strategies aimed at supporting mitochondrial function and cellular metabolism including supplementation with nicotinamide (the amide form of vitamin B3) have demonstrated robust neuroprotective effects in preclinical models and early-phase clinical trials, improving retinal ganglion cell function and visual outcomes.9,10 Other neuroprotective candidates, including citicoline, coenzyme Q10, and dietary interventions like the ketogenic diet, are also under investigation, though large-scale clinical evidence remains limited.4,5,11 In addition to targeting cellular metabolism and reducing oxidative stress, some nutraceuticals also have an IOP lowering effect, which may provide further neuroprotective effects in glaucoma.
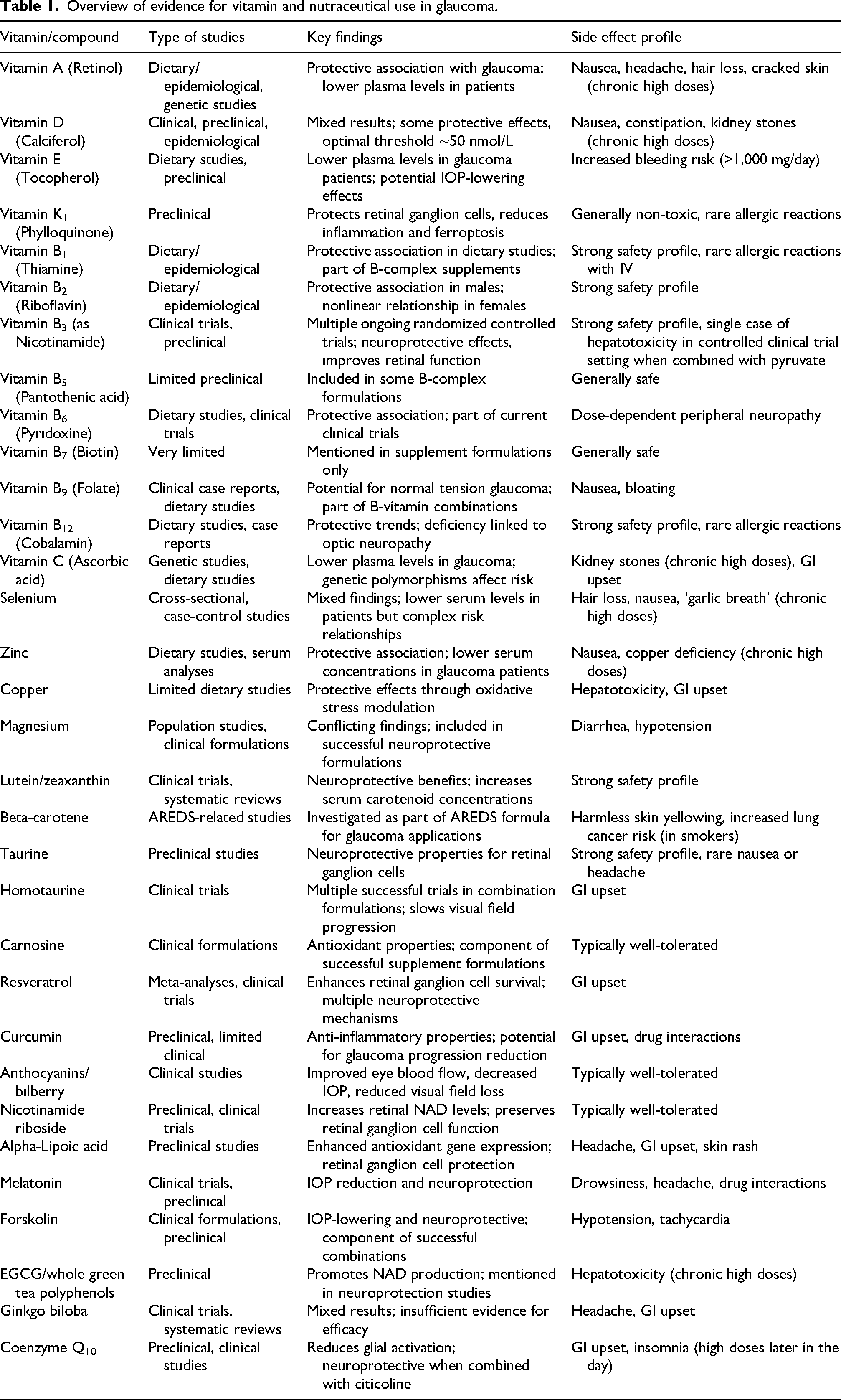
This comprehensive review covers 35 different vitamins, minerals, and nutraceuticals that have been investigated for glaucoma prevention or treatment. The evidence varies from robust clinical trial data to preliminary metabolomic findings, reflecting the diverse approaches being pursued in nutritional glaucoma research (these are overviewed in Tables 1 and 2). Many successful supplement formulations combine multiple compounds, suggesting synergistic effects may be more important than individual nutrient supplementation.
Overview of evidence for vitamin and nutraceutical use in glaucoma.
Overview of ongoing clinical studies for vitamins and nutraceuticals in glaucoma.
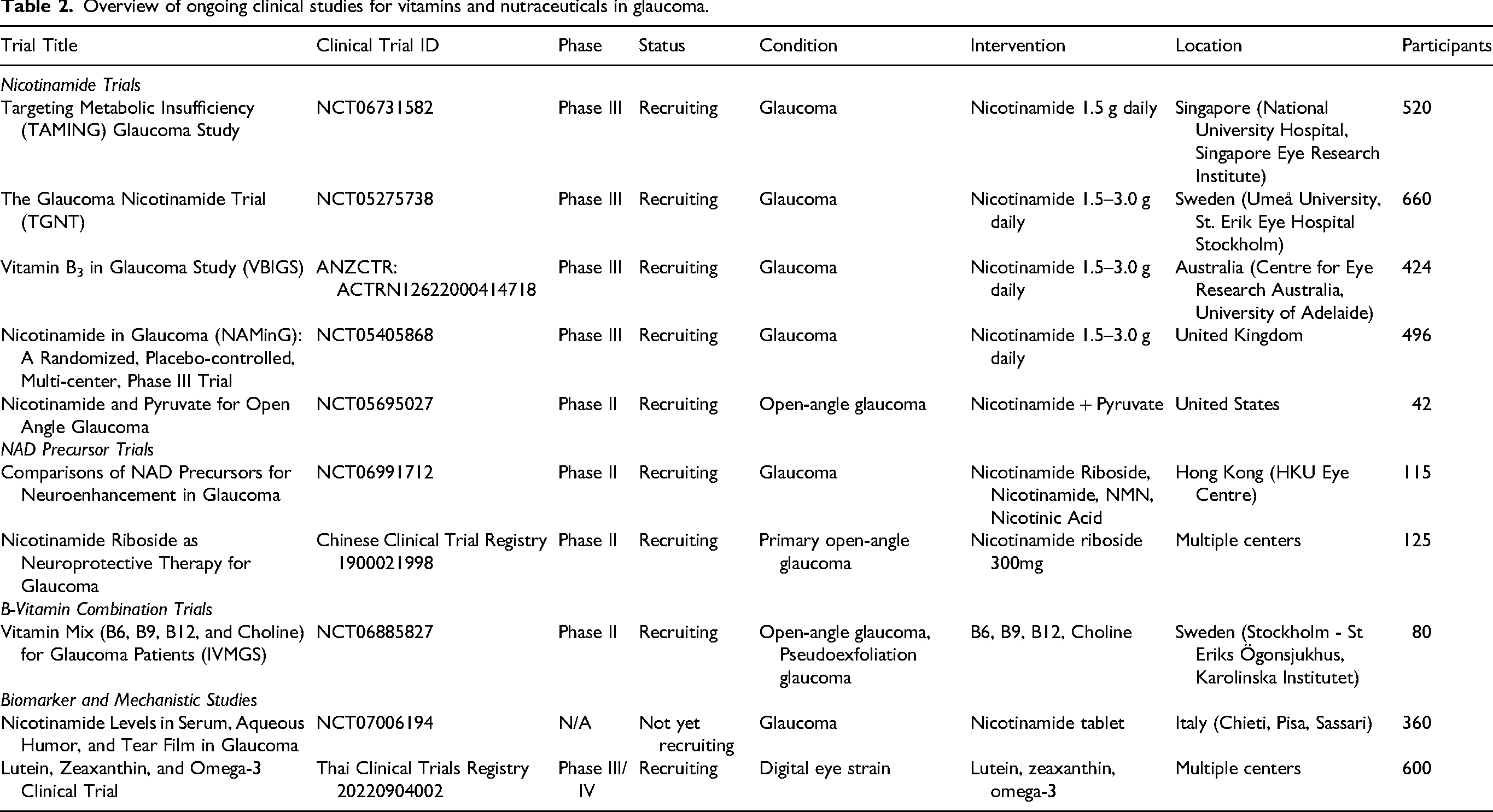

Fat-soluble vitamins
Vitamin A (retinol)
Vitamin A represents one of the most critical nutrients for eye health, functioning as both a structural component of visual pigments and a protective antioxidant. Vitamin A exists in two primary forms: retinol from animal sources and provitamin A carotenoids from plant sources, with beta-carotene being the most prevalent and effective provitamin A carotenoid. 12 Vitamin A plays a fundamental role in maintaining corneal health, helping to protect the surface of the eye. Dietary studies consistently show protective associations with glaucoma, with a systematic review and meta-analysis demonstrating that dietary vitamin A intake had an odds ratio of 0.45 for open-angle glaucoma after addressing heterogeneity.13,14
Vitamin D (calciferol)
Vitamin D has emerged as an important nutrient for eye health, with research suggesting it may help prevent or delay various ocular conditions through its antioxidant and anti-inflammatory properties. Its protective mechanisms appear to involve offsetting oxidative stress that contributes to the development of chronic eye diseases, including age-related macular degeneration (AMD), cataracts, and diabetic retinopathy.15,16 A large-scale UK Biobank study of over 322,000 participants identified 50 nmol/L as the optimal serum 25(OH)D threshold for reducing risks of cataract, AMD, and diabetic retinopathy, though no significant association with primary open-angle glaucoma was observed. 17 However, preclinical studies demonstrate that vitamin D3 supplementation can reduce inflammatory markers in the trabecular meshwork and provide neuroprotective effects. The levels of vitamin D in aqueous humor were notably lower in patients with both cataracts and glaucoma compared to those with cataracts alone. Mendelian randomization analyses found no statistical evidence that vitamin D levels or deficiency causally affect the risk of developing primary open-angle glaucoma. 18 These results indicate that vitamin D may not be a significant factor in modifying primary open-angle glaucoma risk and challenges the above data that vitamin D supplementation could be effective in reducing the risk of glaucoma.
Vitamin E (tocopherol)
Vitamin E shows potential in glaucoma management through its antioxidant and neuroprotective properties. 19 Studies have demonstrated that glaucoma patients have statistically significant lower plasma vitamin E concentrations compared to controls. 20 Recent investigations into mixed tocopherol and tocotrienol combinations show effectiveness in reducing IOP in animal models within 2 days of treatment. The neuroprotective and antioxidative properties of vitamin E derivatives make them promising candidates for glaucoma management. Clinical trials have evaluated vitamin E in combination with other compounds for glaucoma treatment. A fixed combination of citicoline 500 mg, homotaurine 50 mg, and vitamin E 12 mg demonstrated beneficial effects on contrast sensitivity and visual-related quality of life in patients with primary open-angle glaucoma. 21
Vitamin K (phylloquinone K1)
Vitamin K1 plays a protective role in ocular health through its antioxidant and anti-inflammatory properties, including the regulation of microglial ferroptosis and the upregulation of matrix Gla protein, which is essential for IOP regulation and trabecular meshwork integrity. Higher dietary intake of vitamin K1 has been associated with a reduced risk of cataract surgery and may offer broader neuroprotective benefits within the visual system. 22 Vitamin K1 represents an emerging area of glaucoma research with particularly promising preclinical results. Recent studies demonstrate that vitamin K1 can alleviate retinal inflammation following acute ocular hypertension by modulating microglial iron overload and ferroptosis. 23 High-dose vitamin K1 intake inhibits retinal ganglion cell loss during glaucomatous injury, potentially through two mechanisms: lowering IOP and directly counteracting glaucoma-induced cellular damage through neuroprotective effects. This vitamin shows capability to regulate ferroptosis pathways, which are increasingly recognized as important in glaucoma pathogenesis. 22
Water-soluble B-complex vitamins
Vitamin B1 (thiamine)
Vitamin B1 plays a crucial role in ocular health by supporting corneal nerve integrity and function, with supplementation shown to improve corneal nerve parameters and alleviate symptoms in dry eye disease. 24 Higher dietary intake of vitamin B1 is associated with a reduced risk of AMD and may also help protect against cataracts and uveitis. 25 Thiamine has shown protective associations in dietary epidemiological studies of glaucoma.13,26,27 Metabolomic profiling of aqueous humor from glaucoma patients revealed significantly decreased thiamine levels compared to controls. 28 Experimental studies demonstrate that thiamine treatment (alone or as part of a vitamin combo) significantly reduced inflammatory response and protected retinal ganglion cell function against neuroinflammatory damage in mouse models.28,29 Both agmatine and thiamine treatment significantly attenuated Toll-like receptor agonist-induced proinflammatory cytokine responses and rescued pattern electroretinogram amplitudes in treated groups.
Vitamin B2 (riboflavin)
Riboflavin plays a critical role in eye health, with deficiency leading to structural and functional damage to the retina and ocular surface, including retinal degeneration and corneal abnormalities. Supplementation with riboflavin has shown benefit in eye disease, such as improving retinal function in riboflavin transporter deficiency and is being used in corneal cross-linking procedures for conditions like keratoconus.30–32 Riboflavin is included in various B-complex supplement formulations that have demonstrated efficacy in preclinical glaucoma models. 33 Its role in cellular energy metabolism and antioxidant function provides biological plausibility for its protective effects.
Vitamin B3 (niacin, nicotinamide, nicotinamide riboside)
Nicotinamide adenine dinucleotide (NAD) is an essential metabolite and neuroprotective molecule, often referred to as the “longevity molecule”. NAD supports cellular metabolism by acting as a cofactor for hundreds of enzymatic reactions and serving as a key regulator of neurodegeneration.
34
NAD is produced in the body through three primary routes:
The capacity to maintain NAD levels in the retina and optic nerve declines with age, which increases the vulnerability of retinal ganglion cells to pressure-related stress, leading to dysfunction and degeneration.10,35 Preventing age-related NAD depletion, via administration of nicotinamide10,36 (the amide form of vitamin B3 and a precursor to NAD) or via gene therapy10,37 (targeting enzymes involved in NAD production), has demonstrated robust protection against metabolic decline and neurodegeneration in animal models of glaucoma. At the highest doses tested, nicotinamide also lowered IOP by 1 mmHg in control (but not ocular hypertensive) eyes. In patients with glaucoma, systemic nicotinamide is low, 38 NAD levels are significantly reduced in peripheral blood mononuclear cells and in the serum, 39 and key enzymes for producing NAD are low in post mortem retinas. 40 Population studies have also pointed to low niacin in glaucoma populations. 41 Supplementation with nicotinamide improves visual function in existing glaucoma patients 9 supporting the hypothesis that glaucoma has a strong metabolic component and that correcting these bioenergetic insufficiencies can provide neuroprotection in animal models and improve vision in at least some patients with glaucoma.
Nicotinamide riboside is another precursor to NAD with early evidence of protection in glaucoma. Rodent models of retinal ganglion cell injury demonstrated that high dose oral supplementation of nicotinamide riboside could prevent axonal degeneration, 42 and enhance cell survival. Preservation of retinal function was also observed in the acute optic nerve crush model. 43 There is currently one randomized controlled trial investigating the utility of low-dose nicotinamide riboside in glaucoma to prevent retinal nerve fiber layer loss. 44
Vitamin B6 (pyridoxine)
Metabolomic studies have identified vitamin B6 among compounds altered in glaucoma patients’ aqueous humor. 45 Vitamin B6 deficiency can cause optic neuropathy that is reversible if identified and treated promptly, emphasizing its importance for optic nerve health. 46 Current clinical trials are investigating combinations of vitamins B6, B9, and B12, and choline for neuroprotective effects in glaucoma.
Vitamin B9 (folate)
Folate is essential for DNA synthesis, cell division, and the formation of healthy red blood cells. Adequate folate levels are important for the health of the retina and optic nerve, and deficiency can lead to optic neuropathy and increase the risk of retinal vascular diseases and AMD.47–49 Research supports that folate supplementation may help protect against certain eye diseases, particularly those associated with elevated homocysteine levels or vascular dysfunction in the retina. Folate research in glaucoma is emerging as particularly relevant for normal tension glaucoma. Recent clinical approaches propose using L-methylfolate and methylcobalamin supplementation to address elevated retinal venous pressure, which impedes retinal perfusion and contributes to oxidative stress in normal tension glaucoma. 50 Folate was identified through an RNA-sequencing screen of retinal ganglion cell injury models and demonstrated to provide neuroprotection in a retina axotomy model. 51 Current clinical trials are investigating the combination of vitamins B6, B9, and B12 with choline, showing promising results in animal models. 45
Vitamin B12 (cobalamin)
Vitamin B12 is essential for DNA synthesis, red blood cell formation, and the maintenance of neuronal function. 52 It plays a critical role in eye health by supporting the optic nerve and protecting against neurodegeneration.53,54 Deficiency leads to optic neuropathy, which may cause progressive and potentially irreversible vision loss if not promptly treated. 54 Adequate vitamin B12 levels may help reduce the risk of AMD and other ocular diseases by lowering homocysteine and supporting retina and optic nerve health. 55 Vitamin B12 deficiency has been linked to optic neuropathy, with cases demonstrating that untreated deficiency can lead to irreversible optic nerve damage. 56 Vitamin B12 is included in current clinical trials investigating B-vitamin combinations for glaucoma neuroprotection. 45
Vitamin C (ascorbic acid)
Vitamin C has been studied extensively in glaucoma through both genetic and dietary approaches. A Mediterranean population study found that glaucoma patients had significantly lower plasma vitamin C concentrations compared to controls, and genetic polymorphisms in vitamin C transporter genes were associated with glaucoma risk.20,57,58 The corneal epithelium and lens have particularly high levels of vitamin C, and deficiency can impair corneal wound healing.59,60 Recent dietary studies show that higher quartiles of vitamin C intake were associated with lower odds of cataracts and glaucoma compared to the lowest quartile.61–63 Vitamin C has also been demonstrated to be neuroprotective and anti-neuroinflammatory in mouse models of ocular hypertension, with one report suggesting that these effects are exerted through SPP1.64,65
Minerals and trace elements
Copper
Copper has an essential role in retinal physiology, supporting antioxidant enzyme function and retinal cell survival. Copper deficiency is linked to optic neuropathy and AMD, with studies showing reduced copper levels in the retinal pigment epithelium and choroid complex of AMD patients. Supplementation with copper, often alongside zinc, has been associated with a reduced risk of AMD progression.66–69 In glaucoma, several studies have found that copper levels are elevated in the aqueous humor of glaucoma patients compared to controls, and this increase is often accompanied by a lower zinc level. 70 Other groups have observed a negative correlation between serum zinc and copper levels in glaucoma patients, suggesting that an increased copper-to-zinc ratio may be relevant in glaucoma pathophysiology. 71 Further research is required to determine whether copper is a causative factor or a biomarker of disease progression.
Magnesium
Magnesium is an essential mineral present in high concentrations in ocular tissues such as the cornea, lens, and retina, where it supports cellular metabolism, antioxidant defense, and ionic balance. Adequate magnesium levels are crucial for maintaining the structural and functional integrity of the eye, with deficiency linked to cataract, diabetic retinopathy, and glaucoma. Magnesium also exhibits neuroprotective effects by reducing oxidative stress and regulating calcium influx, which helps protect retinal ganglion cells. 72 In primary open-angle glaucoma, magnesium levels in ocular tissues and serum are significantly lower compared to healthy controls. 73 Magnesium supplementation may improve visual fields, enhance ocular blood flow, and reduce IOP in glaucoma patients, likely due to its vasodilatory, antioxidant, and neuroprotective properties.72,73 Supporting a role for magnesium in glaucoma, in a small clinical trial, oral magnesium therapy improved visual field parameters in glaucoma patients with vasospasm. 74
Selenium
Selenium is an essential trace mineral that functions as a key component of antioxidant enzymes (selenoproteins) which protect from oxidative damage. In the eye, selenium's antioxidant and anti-inflammatory properties may help prevent or delay cataract, AMD, and thyroid eye disease by counteracting oxidative stress and supporting ocular tissue health. Clinical studies suggest that selenium supplementation can reduce the severity and progression of mild thyroid eye disease, especially in populations with low selenium status.75,76 Current evidence suggests a potential association between higher selenium levels and an increased risk of glaucoma, though causality has not been established. A large cross-sectional study using NHANES data from US adults aged 40 and older found that higher dietary selenium intake was associated with an increased risk of glaucoma (odds ratio 1.39; 95% CI, 1.07–1.81), with a linear relationship observed across subgroups. 77 A case-control study measuring selenium in plasma and aqueous humor of patients with primary open-angle glaucoma and controls reported that individuals in the highest tertile of plasma selenium had a significantly higher odds of glaucoma (OR = 11.3), while those in the middle tertile of aqueous humor selenium had a significantly lower odds (OR = 0.06). 78
Zinc
Zinc is highly concentrated in the retina, where it plays a critical role in supporting retinal health and enabling vitamin A to produce melanin. Adequate zinc intake is associated with a reduced risk of AMD and may help slow its progression, while zinc deficiency can impair night vision and contribute to optic neuropathy.63,66,67,79,80 In glaucoma, the Composite Dietary Antioxidant Index study demonstrated that higher quartiles of zinc intake were associated with significantly lower odds of glaucoma (OR: 0.73). 63 Serum zinc concentrations are notably lower in glaucoma patients compared to healthy controls. 81
Other commonly explored nutritional supplements / nutraceuticals
Alpha-lipoic acid
Alpha lipoic acid is a potent antioxidant that protects ocular tissues by neutralizing free radicals and regenerating other antioxidants, contributing to the maintenance of retinal and vascular health in the eye. There is evidence for alpha-lipoic acid in diabetic retinopathy and dry eye disease by reducing oxidative stress and inflammation, and supporting nerve function and blood flow in ocular tissues. 82
Supporting this in glaucoma, in mouse animal models of glaucoma, dietary alpha-lipoic acid reduces oxidative stress, upregulates antioxidant enzymes, and provides retinal ganglion cell neuroprotection. 83 Novel liposomal formulations have been developed to improve alpha-lipoic acid bioavailability for glaucoma treatment. 84
Coenzyme Q10
Coenzyme Q10 is a vital mitochondrial antioxidant present in high concentrations in the retina, where it protects from oxidative stress and supports cellular energy production. Coenzyme Q10 levels decline with age, and this may contribute to AMD and optic neuropathies. Supplementation with coenzyme Q10 has demonstrated promise in experimental models for reducing retinal cell apoptosis and supporting overall retinal health.85,86 Coenzyme Q10 has demonstrated neuroprotective effects in both animal models and human studies of glaucoma, primarily by reducing oxidative stress and inhibiting retinal ganglion cell apoptosis. Both topical or dietary coenzyme Q10 can promote retinal ganglion cell survival, preserve optic nerve axons, and reduce markers of oxidative stress and apoptosis in glaucomatous eyes.86–92 Early clinical studies indicate that coenzyme Q10, especially when combined with vitamin E, may improve retinal function and visual cortical responses in glaucoma patients.93–95
Curcumin
Curcumin is the primary active compound derived from the rhizome of
Epigallocatechin gallate (EGCG)
EGCG is a major component of the green tea polyphenols. It is a powerful antioxidant with anti-inflammatory, neuroprotective, and anti-angiogenic properties, making it a promising therapeutic candidate. 101 Preclinical studies have demonstrated strong neuroprotective effects of EGCG in glaucoma models37,101,102 via oral or intraperitoneal routes. A recent study demonstrated EGCG as neuroprotective in ocular hypertensive rats, and was able to isolate a primary effect NAD production (although other mechanisms may remain and be viable to provide neuroprotection including via NF-κB).37,103,104 Subsequent work developed EGCG analogues also demonstrated strong neuroprotective potential. 37 Clinical evidence is limited but promising, with a randomized placebo-controlled trial showing that EGCG supplementation (200 mg/day) for 3 months improved pattern-evoked electroretinogram amplitudes in patients with primary open-angle glaucoma, particularly those with early to moderately advanced disease. 105 Additionally, a recent study demonstrated that both green tea extract and EGCG (400 mg capsules) significantly reduced intraocular pressure in healthy volunteers. 106 EGCG has demonstrated strong neuroprotection in animal models, however its poor viability may explain its lack of success in clinical trials.
Forskolin
Forskolin is a natural diterpene compound derived from the roots of
Ginkgo biloba
Glucose, lactate, and pyruvate
Retinal energy demands are met by glycolysis (2 ATP per glucose) and oxidative phosphorylation (≈32 ATP), with pyruvate and lactate serving as critical substrates.
Lutein and zeaxanthin
These macular carotenoids have substantial research in glaucoma, despite being more commonly associated with AMD. Following 18-month supplementation of open-angle glaucoma patients with macular pigment carotenoids (lutein, zeaxanthin and meso-zeaxanthin) in the European Nutrition in Glaucoma Management trial, Raman spectroscopic analysis confirmed increased serum carotenoid concentrations.124,125 Macular pigment optical density's implications in diabetic retinopathy and glaucoma, have been explored, underscoring the need for clinical measurement. 126 A randomized controlled trial demonstrated that pistachio consumption (a rich source of xanthophyll lutein; 57 g/day for 12 weeks) significantly increased macular pigment optical density in healthy adults selected for habitually low lutein and zeaxanthin intake. 127
Melatonin
Melatonin has substantial research in glaucoma covering both intraocular pressure regulation and neuroprotection. 128 Recent advances include the development of near-infrared activated liposomes for controlled melatonin delivery to the retina. 129 This remotely triggered delivery system can decrease intraocular pressure elevation by 24%, enhance retinal ganglion cell survival by 77%, and decrease glial fibrillary acidic protein activation by 75% in experimental glaucoma models. Ketorolac, melatonin and latanoprost tri-loaded PLGA microspheres have been developed for sustained drug release over 70 days, showing promise for treating glaucoma through combined hypotensive, antioxidant and anti-inflammatory activity. 130 Melatonin demonstrates integrative mechanisms of intraocular pressure control and neuroprotection, making it a multi-target candidate for glaucoma treatment.
Resveratrol
Resveratrol is a natural polyphenolic stilbene predominantly known for its high concentrations in grape skins. It exhibits potent antioxidant, anti-inflammatory, anti-angiogenic, and neuroprotective effects.131–135 Preclinical studies demonstrate that resveratrol protects retinal ganglion cells and lowers IOP through multiple mechanisms. Topical trans-resveratrol (0.2%) reduced IOP by up to 25% in steroid-induced ocular hypertension via agonism at adenosine A₁ receptors. In rodent models of acute IOP elevation and optic nerve crush, systemic or intravitreal resveratrol treatment (10–250 mg/kg or 30 µM) provided neuroprotection, preserved retinal thickness, upregulated SIRT1 expression, and inhibited pro-inflammatory and apoptotic markers. A systematic meta-analysis of 30 preclinical glaucoma studies found that resveratrol increased retinal ganglion cell survival and slowed retinal thinning.136–138 Although human clinical trials are limited, these data provide a robust foundation for advancing resveratrol research in glaucoma.
Taurine and homotaurine
Taurine is a conditionally essential amino acid highly concentrated in the retina, where it plays a crucial role in maintaining retinal structure, protecting photoreceptors, and supporting antioxidant defenses. Deficiency in taurine leads to retinal degeneration, oxidative stress, and loss of retinal ganglion cells, while supplementation has been shown to protect against light-induced and age-related retinal damage. Taurine's neuroprotective, anti-inflammatory, and anti-apoptotic properties make it important for ocular health.139–141 Metabolomic studies demonstrate reduced taurine concentrations in the eyes of glaucoma patients, supporting the hypothesis that taurine depletion may contribute to disease progression.
142
Further supporting this,
Clinical trial developments, future directions, and conclusions
Varying levels of clinical evidence exist for a range of vitamins, minerals and nutraceuticals. The current research landscape indicates that B vitamins, particularly vitamin B3 (nicotinamide), represent the most advanced area of vitamin research in glaucoma, with multiple Phase II and III clinical trials ongoing worldwide. Vitamin combinations targeting metabolic dysfunction in retinal ganglion cells appear more promising than single-vitamin approaches, however few have been performed with proper single-compound-only controls which makes scientific interpretation of the studies more difficult.
The most compelling evidence exists for nicotinamide, homotaurine, resveratrol, and melatonin, whilst emerging compounds like vitamin K1, nicotinamide riboside, and novel compounds based on EGCG show promise for future therapeutic development (see
Evidence level classifications for vitamins and nutraceuticals in glaucoma
Homotaurine, melatonin, nicotinamide
Coenzyme Q10, pyruvate, resveratrol, vitamin K1,
alpha-lipoic acid, curcumin, forskolin, lutein/zeaxanthin, nicotinamide riboside, selenium, vitamin A, vitamin B6, vitamin C, vitamin D, zinc
EGCG/whole green tea polyphenols, taurine, vitamin B9 (folate)
Copper, vitamin B1, vitamin B2, vitamin E
Ginkgo biloba, magnesium
Vitamin B5, vitamin B7
Given that glaucoma is a polygenic, multifactorial disease, there is unlikely to be a one-size-fits-all solution, and there is a potential that combination therapy, targeted to the right patients (
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: FH is supported by Glaucoma Australia Quinlivan Grant. Centre for Eye Research Australia receives operational support from the Victorian State Government. PAW is supported by Vetenskapsrådet 2022-00799 and The Ulla and Ingemar Dahlberg Foundation.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability and materials
No data was generated to create this article.
Data sharing statement
No data was generated in this study.
LLM statement
Perplexity AI was used to organize and to collate notes. LLMs had no role in the writing or analysis of the manuscript.
