Abstract
Purpose
To study peripheral capillary non-perfusion (PCN-P) in branch retinal vein occlusion (BRVO) by means of ultra wide-field fluorescein angiography (UWFFA), and to correlate its extent and severity with optical coherence tomography (OCT) and OCT-angiography (OCTA) parameters and best corrected visual acuity (BCVA).
Methods
Prospective case series with 2 years of planned follow-up. We recruited patients from June 2019 to December 2019. Ophthalmologic examination included BCVA, UWFFA, OCT and OCTA. Partial (p) and complete (c) ischemic index (ISI) were evaluated on UWFFA images. Vessel density (VD) in both the macular region and the optic nerve head (ONH) was calculated.
Results
Twelve BRVO subjects and 12 healthy controls were recruited. Mean age was 63.8 ± 8.74 years. Mean BCVA improved from 0.43 ± 0.25 logMAR to 0.15 ± 0.18 after two years (p < 0.01), while mean central macular thickness (CMT) decreased from 463.83 ± 200.85 µm to 353.17 ± 108.85 µm (p > 0.05). Mean cISI, pISI and total ISI were 25.2 ± 13.0%, 6.3 ± 5.0% and 31.5 ± 12.0%
Conclusion
The amount of complete and partial ischemia may have different implications in BRVO, with the former being more associated with microvascular impairment and the latter with macular edema.
Keywords
Introduction
After diabetic retinopathy, retinal vein occlusion (RVO) is the second most common vascular cause of vision loss. 1 While the clinical diagnosis of RVO is often made through a fundus examination, fluorescein angiography (FA) is a useful exam to rule out potential differential diagnoses and to assess the presence of macular ischemia and large areas of non-perfusion. The introduction of ultra-widefield FA (UWFFA) has changed the way retinal non-perfusion is measured due to its 200° field of view, which allows the detection of areas of peripheral capillary non-perfusion (PCN-P).
Optical coherence tomography angiography (OCTA) is a recent non-invasive technique which currently represents an ideal tool to investigate macular microvascular abnormalities in RVO. 2 In the latest years, several studies gathered data of BRVO patients to investigate the relation between PCN-P, quantified by using UWFFA, and macular microvascular changes, identified by OCTA.3–6 More recently, non-perfusion areas have been subclassified in partial and complete ischemia, aiming to better understand the different clinical implication of the severity of peripheral ischemia. 7
In this investigation we aim to study PCN-P in BRVO eyes, by means of UWFFA, and to correlate its extent and severity with OCT and OCTA parameters, including microvascular changes, central macular thickness (CMT), and visual acuity.
Methods
Our study was designed as a prospective case series with 2 years of planned follow-up. We enrolled consecutive BRVO patients presenting at the Ophthalmology Department of the IRCCS San Raffaele Hospital between June 2019 and December 2019. We also enrolled an age- and sex- matched healthy group of control subjects. All patients provided signed informed consent. The entire study was carried out in accordance with the Helsinki Declaration and was approved by the Ethical Committee. The inclusion criterion was a clinical diagnosis of BRVO.
We considered as exclusion criteria: high media opacities, the presence of concomitant retinal or optic nerve diseases, any ophthalmic surgical procedure over the six months prior the OCTA acquisition, and any systemic disease that could potentially affect our results.
A complete ophthalmological examination including best corrected visual acuity (BCVA) measurement with the ETDRS charts and slit-lamp examination of the anterior and posterior segments was carried out for all patients. All patients underwent OCT, OCTA and UWFFA. All structural OCTs were acquired with the Spectralis HRA + OCT (Heidelberg Engineering, Heidelberg, Germany). The acquisition protocol included radial and dense scans (ART > 25), and raster scans with the enhanced depth imaging (EDI) mode to measure CMT over the follow-up.
Swept-source 4.5 × 4.5 mm OCTA images centered on the fovea and at the optic nerve head (ONH) were collected with the DRI OCT Triton (Topcon Corporation, Tokyo, Japan) at baseline, and those obtaining a Topcon's quality index > 80 were used for our analyses. The superficial and deep capillary plexa (SCP and DCP), and choriocapillaris (CC) were automatically segmented for both macular (m) and ONH (n) scans, while manual segmentation was employed in case of segmentation errors. For ONH reconstructions, the radial peripapillary capillary (RPC) plexus segmentation was also considered. All reconstructions were loaded into ImageJ software (https://imagej.net/Welcome) to calculate vessel density (VD). All images were binarized with a “mean threshold”, and the ratio between white and total pixels (i.e., the VD parameter) was calculated. For the SCP and DCP measurements, we manually segmented and excluded the foveal avascular zone (FAZ). OCTA quantitative findings were compared between BRVO and control group. Furthermore, the FAZ area in the inner retina slab was measured with the IMAGEnet 6 segmentation tool.
At baseline visit we performed UWFFA using the Optos 200Tx fundus camera. The regions of PCN-P visible in the UWFFA images were subclassified as done in a previous study. 7 In brief, a partial ischemic area was identified as the presence of a cluster of small, fragmented areas of hypofuorescence, together with dilated and irregular capillaries. Complete ischemia was defined as an area of contiguous hypofuorescence due to capillary loss and precapillary arterioles and postcapillary venules obstruction. Each image was independently evaluated by two masked retinal specialists (AA and AA), and the mean values obtained were used for the analyses. The graders manually outlined the border of non-perfusion areas (NPA) and the total visible retinal area (TRA) with the OptosAdvance software. The extent of complete (c) and partial (p) ischemic areas (see Figure 1), were calculated on the basis of the grading results (expressed by the software in mm2 or cm2), and total (t) ischemic area was obtained by the sum of both values. Finally, ischemic index (ISI) was calculated as described previously. 2 This method was used for each PCN-P area to calculate pISI, cISI and tISI.
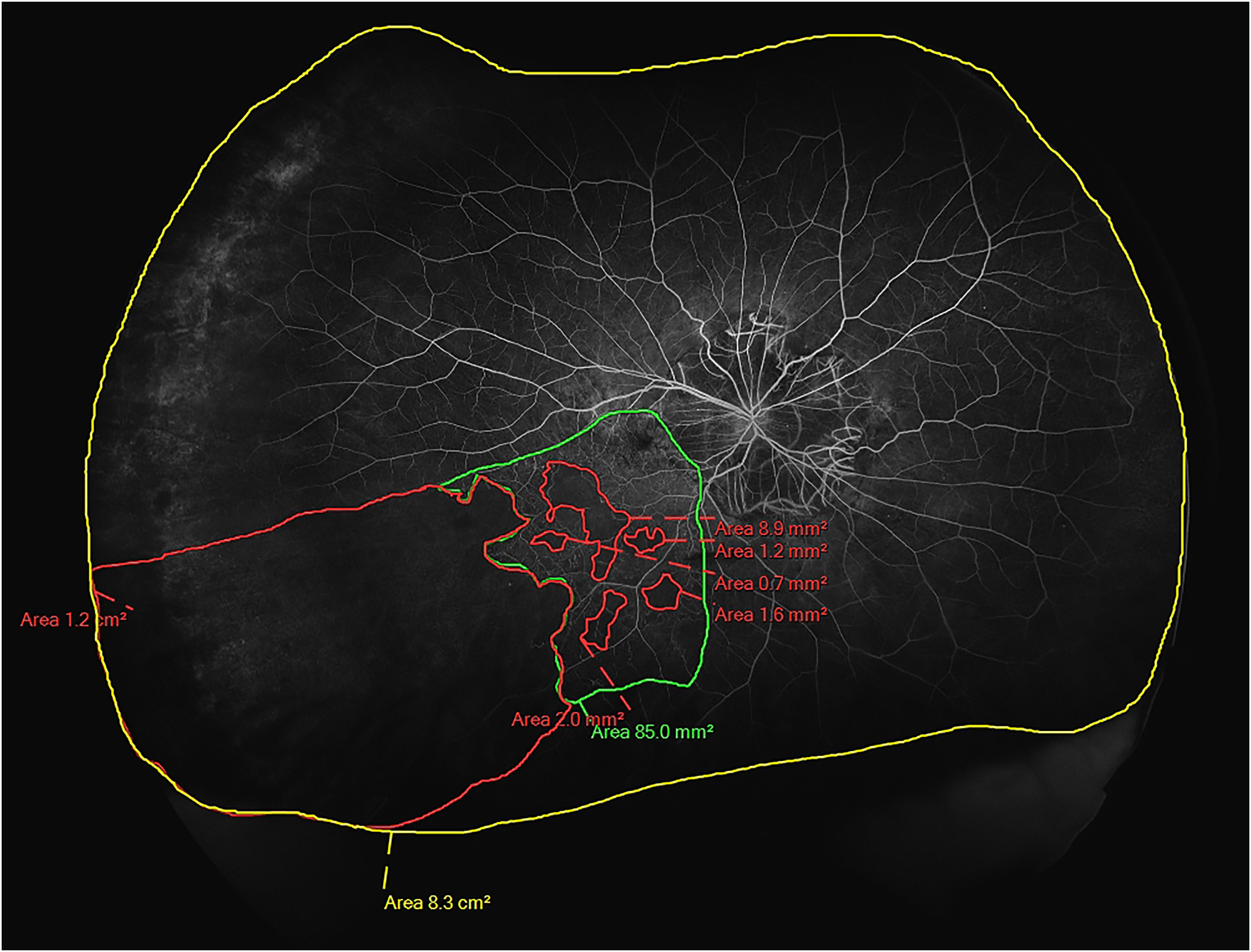
Ultra wide-field fluorescein angiography of a right eye with branch retinal vein occlusion. The outermost line delimitates the total retinal area; a large area of complete ischemia is visible in the temporal periphery, whereas other smaller, scattered zones of complete ischemia are sorrounded by a larger region of partial ischemia in the posterior pole and temporal mid-periphery.
In case of macular edema, each BRVO eye was treated with a loading phase of 3 monthly ranibizumab injections, followed by a pro-re-nata regimen with monthly examination. Further injections were administered if macular edema was detected on OCT images.
The primary goal was to better investigate the role of complete and partial P-CNP on mVD and nVD in BRVO-affected eyes. The secondary outcome was to analyze their relationship with BCVA and CMT outcomes.
All statistical analyses were performed by means of SPSS package software (SPSS, Chicago, Illinois, USA). Continuous variables between groups were compared by unpaired t-test or Mann Whitney's U test, as appropriate. Before and after comparisons were made with paired t-test. Statistical significance was set at p < 0.05. Correlations between quantitative data were assessed with Spearman's correlation coefficient in case of normal distribution, and with Kendall's Tau-b test in case of non-normal distribution.
Results
Twelve BRVO subjects and 12 healthy age- and sex-matched controls were included in the study. Five (41.7%) BRVO patients were male and 7 (58.3%) females, with a mean age of 63.8 ± 8.74 (range 48–77) years. Macular edema was present in all patients. Mean BCVA at baseline in the BRVO group was 0.43 ± 0.25 logMAR, improving to 0.15 ± 0.18 logMAR after two years follow-up (p < 0.01), while mean baseline CMT was 463.8 ± 200.9 µm, improving to 353.2 ± 108.9 µm at the end of the follow-up (p > 0.05), with a mean change in CMT of −110.67 ± 191,92 µm. In the control group, mean baseline BCVA and CMT were 0.0 ± 0.0 logMAR and 241.33 ± 10.53 µm, not changing over the course of the follow-up. All demographic and OCT features are reported in Table 1. In comparison to healthy individuals, the BRVO group displayed lower VDs for all except mSCP and mCC (all p < 0.01). See Table 2.
Demographic and OCT features.
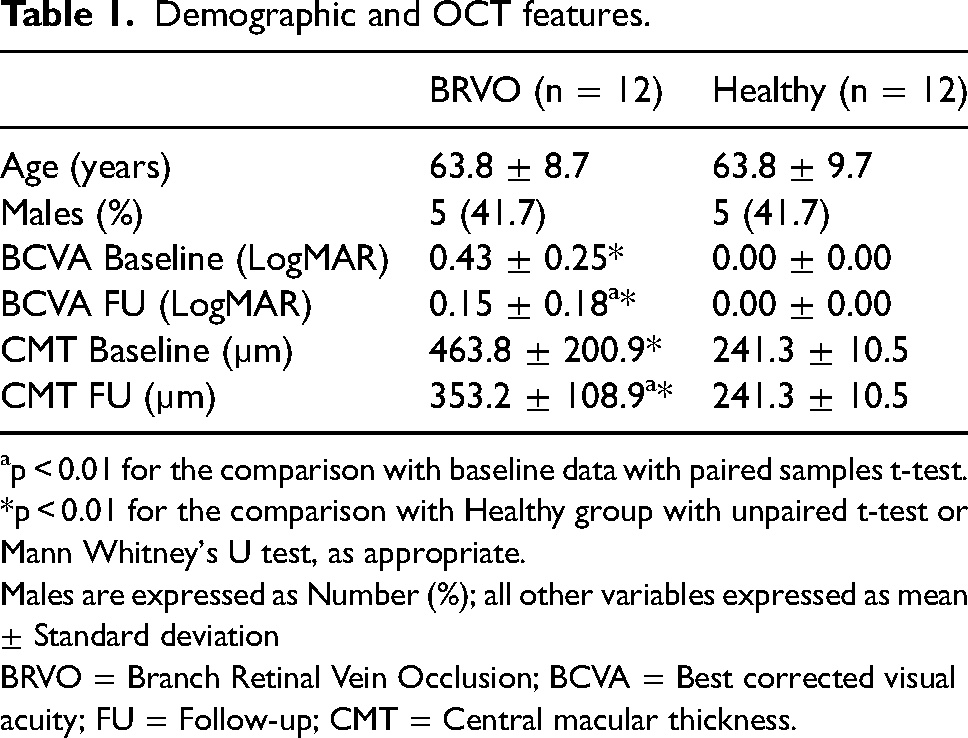
p < 0.01 for the comparison with baseline data with paired samples t-test. *p < 0.01 for the comparison with Healthy group with unpaired t-test or Mann Whitney's U test, as appropriate.
Males are expressed as Number (%); all other variables expressed as mean ± Standard deviation
BRVO = Branch Retinal Vein Occlusion; BCVA = Best corrected visual acuity; FU = Follow-up; CMT = Central macular thickness.
Vessel density data.
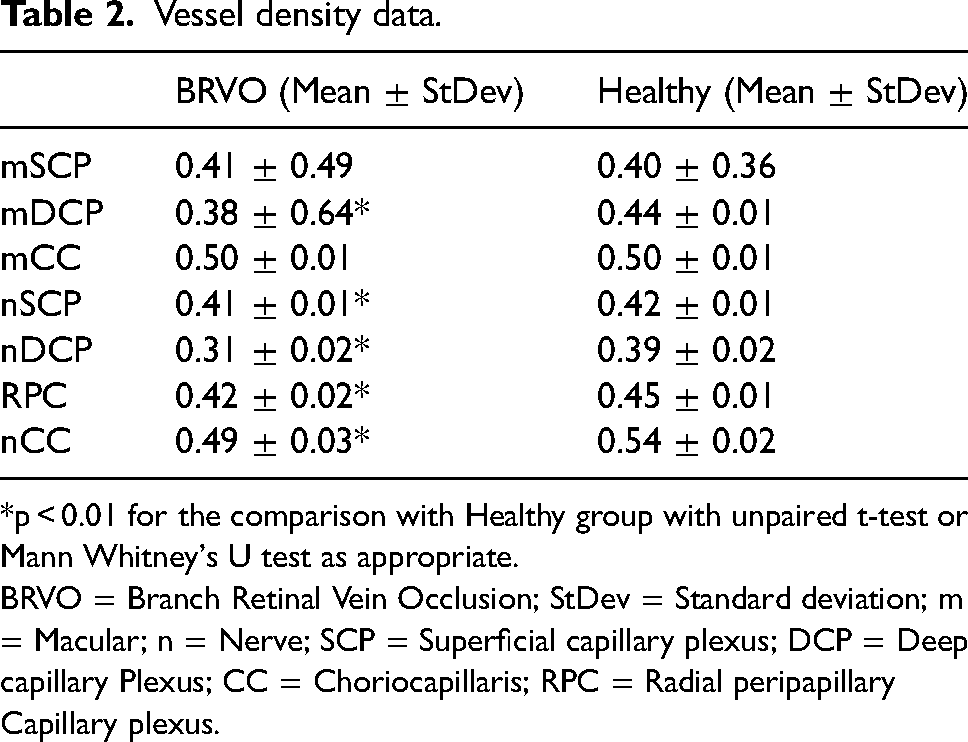
*p < 0.01 for the comparison with Healthy group with unpaired t-test or Mann Whitney's U test as appropriate.
BRVO = Branch Retinal Vein Occlusion; StDev = Standard deviation; m = Macular; n = Nerve; SCP = Superficial capillary plexus; DCP = Deep capillary Plexus; CC = Choriocapillaris; RPC = Radial peripapillary Capillary plexus.
BRVO patients had a mean FAZ area at baseline of 347.50 ± 158.27 µm2, while mean cISI, pISI and tISI were 25.2 ± 13.0 (%), 6.3 ± 5.0 (%) and 31.5 ± 12.0 (%), respectively (see Table 3).
OCTA and UWFFA data in BRVO patients.

All data expressed as mean ± Standard deviation.
BRVO = Branch Retinal Vein Occlusion; FAZ = Foveal avascular zone; c = complete; p = partial; t = total; ISI = Ischemic Index.
Correlations
Both cISI and tISI showed a statistically significant negative correlation with mDCP (p < 0.01; Figure 2), whereas only pISI correlated with baseline CMT (p < 0.05). Additionally, cISI also negatively correlated with RPC (p < 0.05). Interestingly, neither ISI nor CMT correlated with baseline or follow-up BCVA. Likewise, FAZ area did not correlate with ISI. Table 4 illustrates the correlations between UWFFA data and all the analyzed parameters.
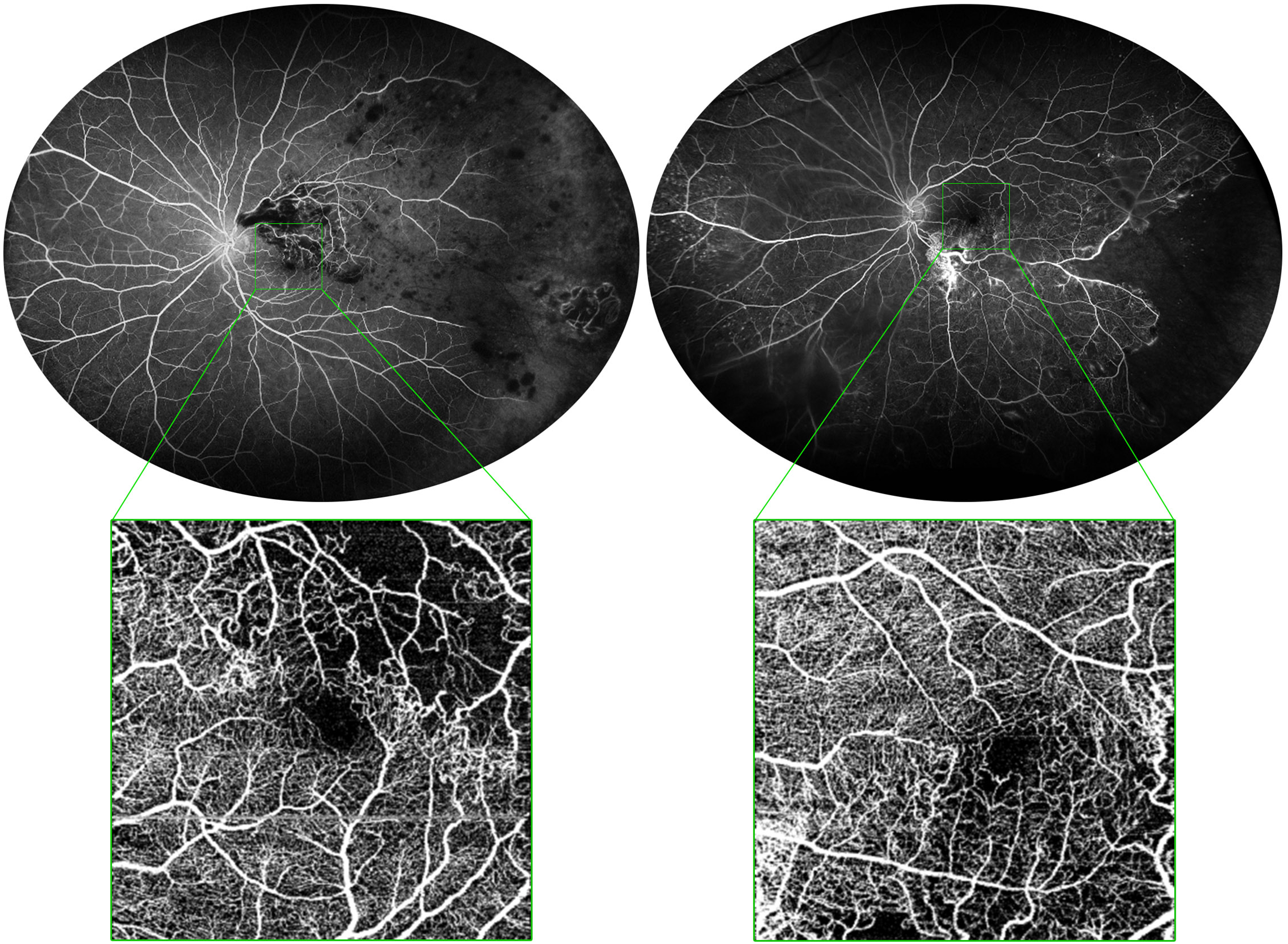
Ultra wide-field fluorescein angiography of two patients showing the correlation between ischemic index (ISI) and vessel density on optical coherence tomography angiography (OCTA). Left patient displays a more severe ISI than right patient, as well as a greater reduction in vessel density on OCTA.
Correlations between UWFFA and other parameters.
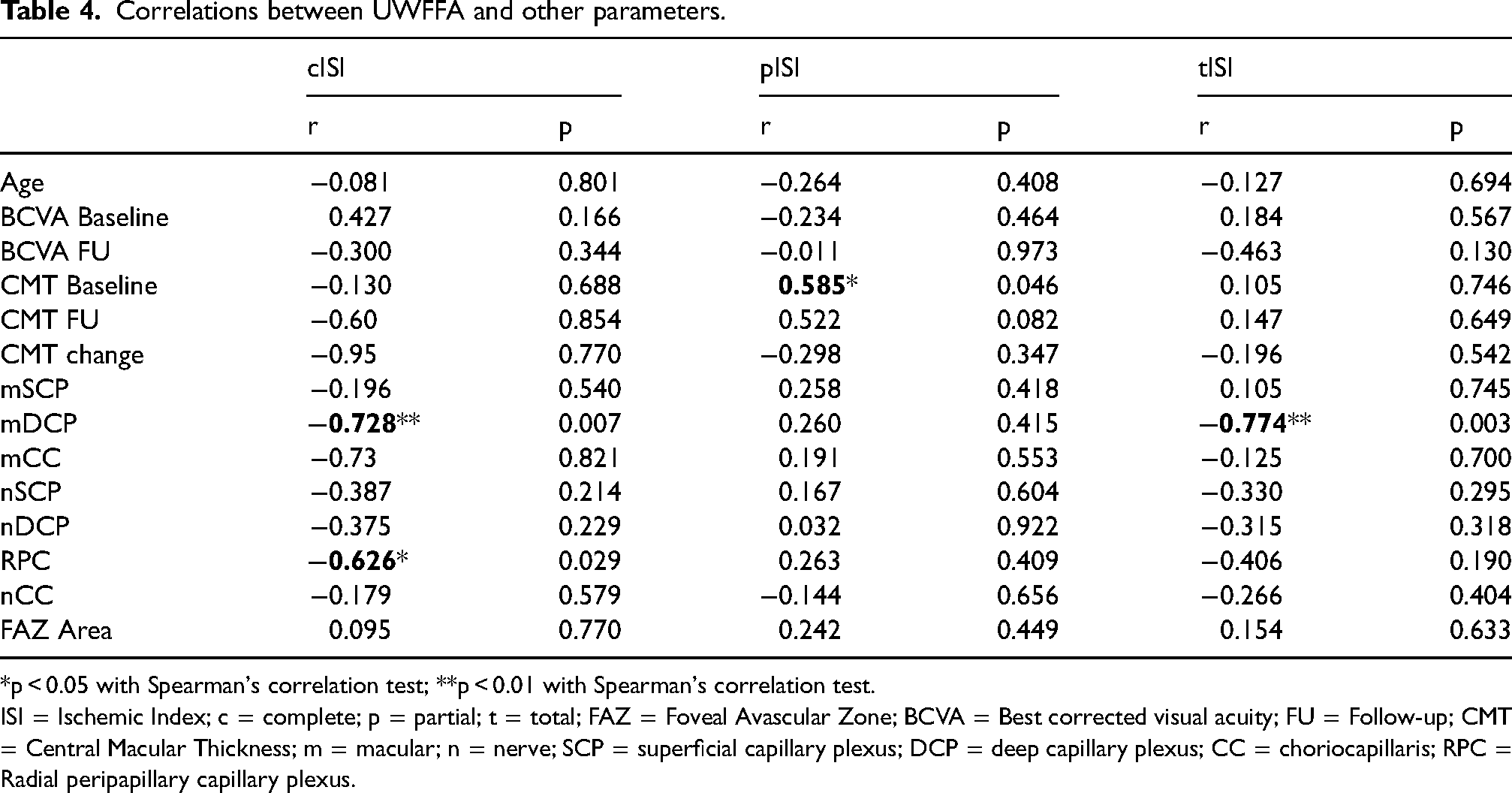
*p < 0.05 with Spearman's correlation test; **p < 0.01 with Spearman's correlation test.
ISI = Ischemic Index; c = complete; p = partial; t = total; FAZ = Foveal Avascular Zone; BCVA = Best corrected visual acuity; FU = Follow-up; CMT = Central Macular Thickness; m = macular; n = nerve; SCP = superficial capillary plexus; DCP = deep capillary plexus; CC = choriocapillaris; RPC = Radial peripapillary capillary plexus.
Discussion
PCN-P characterizes specific RVO sub-forms. In particular, BRVO showing PCN-P has been reported as representing about two-thirds of cases. 8 Nevertheless, the extension of PCN-P was assessed by standard FA which cannot examine the far periphery of the retina. In addition, its definition was based on the terminology used in the CRVO and BRVO studies, which defined RVOs as ischemic when PCN-P of at least 10 disc areas in CRVO, and 5 disc areas in BRVO was present.9,10
The advent of UWFFA has revolutionized the PCN-P assessment introducing the ISI, which is calculated by dividing the area of PCN-P per the total visible fundus area. 11 ISI has been reported to correlate with several clinical and OCTA parameters, such as FAZ area, VD, CMT, BCVA and treatment response.4,12 In our study, we subdivided PCN-P in areas of partial and complete ischemia, according to the classification introduced by Ryu et al. 7
In our investigation, we analyzed 12 patients affected by BRVO by calculating pISI, cISI and ISI, based on partial, complete and total PCN-P areas and analyzed their relationship with BCVA, CMT (as a surrogate measurement for macular edema) and OCTA parameters.
In our cohort, average pISI, cISI and tISI were 25.2%, 6.3% and 31.5%, respectively. Prior research on BRVO found that the average ISI varied between 8% and 22%, although that range depended on the retinal area that was taken into account and on the calculation method adopted. Indeed, previous studies’ results only considered the area that we identified as complete ischemia.3–5,11
Our data reveal that ISI does not correlate with FAZ and BCVA in BRVO eyes. While these association are well-established in CRVO, their existence is debated in BRVO. 11 Similar findings were observed in previous research, which found that ISI and BCVA were only correlated when PCN-P was present in specific retinal subregions. Additionally, there was no direct relationship between FAZ area and ISI, although a cut-off was found to identify patients with larger FAZ.5,7
In terms of the effect of ISI on CMT, our data suggest that, in contrast to complete ischemia, only partial ischemia correlates with an increased CMT in BRVO eyes. However, in our study we could not find an association between the amount of pCNP and the response to anti-VEGF treatment in terms of CMT reduction. Our findings align with the results obtained by Ryu et al, who reported that only partial ischemia showed significant correlation with CMT and the aqueous levels of VEGF-A, as well as many other cytokines, while complete ischemia was not associated with these parameters. 7 They advanced the hypothesis that complete PCN-P is equal to complete loss of cells producing cytokines in response to hypoperfusion, whereas in regions of partial PCN-P, cells are presumably still alive and susceptible to respond to the ischemic insults with the production of cytokines, which ultimately leads to increased permeability and edema development.
Moving to OCTA parameters, we found VD to be reduced in almost all layers in BRVO, except for mCC and mSCP. An impairment of the mSCP has been variably reported by prior studies.4,6,13,14 In addition, a recent analysis conducted by Kim and coworkers unveiled a more severe reduction of the mDCP when compared to the mSCP. 14
Of note, RPC was also reduced in comparison to healthy subjects. Chen et al. firstly described a reduction in RPC, while Fan and colleagues found it to be also reduced in fellow eyes of BRVO patients, suggesting a contribution of systemic factors.13,15 A VD reduction of the RPC could represent a biomarker of ONH perfusion, but it has also been associated with a reduction in retinal nerve fiber layer thickness, although these results are yet to be confirmed. Remarkably, we found a statistically significant correlation between RPC and cISI, suggesting that complete ischemia is related to the perfusion status of the ONH. If these findings are supported by future research, VD of the ONH might be an additional biomarker of PCN-P, indicating the necessity to perform FA to investigate the presence of large ischemic areas in BRVO patients.
Finally, cISI and tISI were negatively correlated with mDCP. These findings are consistent with previous descriptions of a negative association between ISI and mDCP in the literature, but they also suggest that the regions that contribute significantly to reduce mDCP are those of complete ischemia. 4
We are aware that the present investigation is affected by several limitations. First of all, our study has a limited sample size, being the number of patients examined scant. Secondly, ISI calculation may be difficult, being affected by image quality and patient's cooperation. Also, we calculated ISI on central UWFFA images only, although a recent study clarified that such images still provide reliable measurements. 16 Moreover, OCTA parameters are prone to artifacts and their applicability on eyes affected by RVO is not standardized yet. Even though our study is burdened by several limitation, we believe that our findings could add to the interpretation of PCN-P and its correlation with anatomical and functional outcomes. A better characterization of the spectrum of retinal ischemia and its individual implications may be clinically important in the future to develop new treatment strategies and alternatives for RVOs based on the prevalent type of non-perfusion.
In summary, our study provides preliminary data on the role of PCN-P of different severities on OCTA. We confirmed that the entity of partial retinal non-perfusion was correlated with the severity of macular edema in BRVO, and that mDCP configures itself as a good biomarker of PCN-P. Moreover, mDCP seems more linked to complete ischemia, rather than partial ischemia. This last finding deserves further investigation to understand if the mechanisms that lead to macular edema and VD reduction should be considered as separated entities in BRVO. In conclusion, the relation between UWFFA and OCTA findings should be further explored, and other longitudinal studies on this topic are recommended to confirm our findings.
Footnotes
Acknowledgements
None.
Authorship
All authors attest that they meet the current ICMJE criteria for Authorship.
Conflict of interest: All authors have no conflict of interest. Prof. Francesco Bandello is the Editor in Chief of EJO but he was not involved in the evaluation procedure of the present study.
Declaration of conflicting interests
Prof. Francesco Bandello is the Editor in Chief of European Journal of Ophthalmology, but he was not involved in the evaluation procedure of the present study. All other authors have no conflict of interest.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Financial disclosure
Francesco Bandello consultant for: Zeiss (Dublin, USA), Farmila-Thea (Clermont-Ferrand, France), Alimera Sciences (Alpharetta, Georgia, USA), Allergan Inc (Irvine, California, USA), Alcon (Fort Worth, Texas, USA), NovagaliPharma (Évry, France), Bausch And Lomb (Rochester, New York, USA), Hoffmann-La-Roche (Basel, Switzerland), Thrombogenics (Heverlee, Belgium), Novartis (Basel, Switzerland), Sanofi-Aventis (Paris, France), Genentech (San Francisco, California, USA),Bayer Shering-Pharma (Berlin, Germany). All other authors do not have any disclosures to declare
Patient consent
The patient was informed and consented to the use his medical records and data for research purposes.
